Page 665
28—
Recommendations on Diet, Chronic Diseases, and Health
The committee's overall recommendations on diet, chronic diseases, and health are presented in this chapter along with a discussion of the criteria, the process, and the factors considered in formulating them. There is also a discussion of the nature of the recommendations and the target populations and comparisons with recommendations of other expert groups in the United States and abroad. In addition, this chapter includes an assessment and some quantitative estimates of the potential benefits and adverse consequences of dietary modifications as they relate to chronic disease risk and recommendations for research to increase knowledge in this area.
Criteria and Process for Formulating Dietary Recommendations
Absolute proof is difficult to obtain in any branch of science. As evidence accumulates, however, it often reaches the point of proof in an operational sense, even though proof in an absolute sense may be lacking. In law, proof beyond a reasonable doubt is generally accepted as a standard for making decisions and taking action. The degree of evidence as well as the severity of the crime are the bases for the relative intrusiveness of legal actions taken, e.g., issuing a warning for a misdemeanor compared to the imposition of severe penalties for a felony. A similar paradigm can be applied to evidence on dietary patterns and associated health risks. For example, public education might be sufficient to warn against the potential hazard of excess caffeine intake, whereas evidence on the toxicity and carcinogenicity of aflatoxin warrants government regulation to curtail aflatoxin contamination of grains and milk. The strength of the evidence might not be the only relevant criterion for determining the course of action; other factors include the likelihood and severity of an adverse effect, potential benefits of avoiding the hazard, and the feasibility of reducing exposure.
The Committee on Diet and Health adopted this approach of gearing dietary recommendations—the proposed level of action—to such critical features as the level of certainty, the potential for public health benefit, and the likelihood of minimal risk. Thus, although much remains to be learned before firm conclusions and recommendations can be made regarding the total impact of diet on chronic disease risk, in the committee's judgment it would be derelict to ignore the large body of evidence while waiting for absolute proof of benefit from dietary change. The committee concluded that the overall evidence regarding a relationship between certain dietary patterns (e.g., a diet high in saturated fat and total fat) and chronic diseases (e.g., cardiovascular diseases or certain cancers) supports (1) a comprehensive
Page 666
effort to inform the public about the likelihood of certain risks and the possible benefits of dietary modification and (2) the use of technological and other means (e.g., production of leaner meat) to facilitate dietary change.
The process of arriving at dietary recommendations, rather than the recommendations themselves, previously has received little attention. One relevant attempt is the development of the Public Health Objectives for the Nation by the Office of Disease Prevention and Health Promotion of the U.S. Department of Health and Human Services (DHHS, 1983). That office proposed 17 priority objectives for improving nutrition during the 1990s as well as an implementation plan for meeting these objectives. A midcourse review of the status of these objectives documented the process of developing the objectives and suggested that substantial progress has been made in achieving certain nutrition-related objectives (DHHS, 1986). The logic, criteria, and philosophy for formulating dietary recommendations are also discussed in reports by the Health Education Council in the United Kingdom (NACNE, 1983), the American Heart Association in its Dietary Guidelines for Healthy American Adults (AHA, 1986), the National Research Council's Committee on Diet, Nutrition, and Cancer (NRC, 1982), and a Food and Nutrition Board report entitled Toward Healthful Diets (NRC, 1980b).
Several individual attempts to define or analyze the process of developing dietary recommendations also provide insights into the philosophy underlying recommendations issued in different countries (e.g., Grobstein, 1983; Langsford, 1979; Molitor, 1979; Palmer, 1983). The committee hopes to contribute to this nascent field through the discussions that follow.
A special feature of the present study is its attempt to develop recommendations and strategies for risk reduction across the entire spectrum of major diet-related chronic diseases. Several factors were considered in this process: risks and benefits; the advantages of making recommendations by nutrient, by food, or by dietary pattern; the basis for proposing quantitative as opposed to qualitative recommendations; recommendations for individuals as opposed to populations; and the feasibility of implementation. These are discussed in the following sections.
Assessment of Risks and Benefits
To develop dietary recommendations for reducing the overall risk of diet-related chronic diseases, it is essential to analyze and compare recommendations pertaining to individual diseases. For example, recommendations to increase calcium intake to provide possible protection against osteoporosis might in isolation be viewed as conflicting with recommendations for coronary heart disease (CHD) prevention, because dairy products—which contribute the most calcium to the U.S. diet—are also major sources of saturated fatty acids (SFAs), which are known to increase plasma cholesterol levels and CHD risk. Thus, recommendations for maintaining adequate bone mass and for preventing CHD would both have to stress consumption of low-fat dairy products.
Other important considerations are dietary interactions and their synergistic or antagonistic effects. For example, the potential benefits of enhanced trace element intake for certain cancers might be offset by increasing the intake of vegetables and cereals in an attempt to reduce risk for colon cancer, because such foods are also high in fiber, which could in principle initially inhibit intestinal absorption of certain trace elements.
As exemplified systematically at the end of this chapter, the committee considered such potential risks as well as dietary interactions and dose-response relationships in assessing the probable impact of dietary modification on risk factors across the range of chronic diseases. To some extent, this task was simplified by the inherent concordance in dietary risk and protective factors. For example, a recommendation to lower fat intake would be consistent with evidence that low-fat intake may reduce the risk of certain cancers and with stronger evidence that decreased SFA and cholesterol intakes reduce cardiovascular disease risk.
Recommendations by Nutrients, Foods, or Dietary Patterns
The committee discussed whether to base its recommendations on individual nutrients, single foods or food groups, or the overall pattern of dietary intake. Nutrient-based recommendations (e.g., fluoridation of water for the general population or iron fortification to reduce the risk of iron deficiency) might be easy for public health personnel to interpret and implement (e.g., through supplementation or food fortification); however, they may fail to take into account needs that arise from interactions among nutrients (e.g., increased selenium requirements for those on a high-vitamin C diet or enhanced iron absorption in the presence of vitamin C). Furthermore, such recommenda-
Page 667
tions may be difficult for the public to interpret or translate into diets, e.g., understanding how to plan diets to obtain at least 800 mg of calcium—the Recommended Dietary Allowance (RDA) per day. Thus, recommendations pertaining to nutrient intake would usually need to be translated by professionals into guidance about food choices for the public.
Recommendations based on single foods or food groups are easier to implement when only a few foods serve as the major sources of an essential dietary component (e.g., dairy products, which are the primary source of calcium in the U.S. diet). However, such guidance can be misleading. Rich sources of nutrients are not necessarily good dietary sources unless the food is eaten frequently or in large amounts and the nutrient is bioavailable. For example, although the calcium content of spinach is higher than that of dairy products, dairy products are better sources of calcium because of greater bioavailability and more frequent consumption. Furthermore, such recommendations may ignore food group commonalities (i.e., foods with similar nutrient profiles can be exchanged for each other).
As summarized later in this chapter, guidelines issued by other expert groups, including the American Diabetes Association (1987), the American Heart Association (AHA, 1988), the National Research Council's Committee on Diet, Nutrition, and Cancer (NRC, 1982), the U.S. Department of Agriculture and the Department of Health and Human Services (USDA/DHHS, 1985), and the U.S. Surgeon General (DHHS, 1988), are in general based on overall dietary patterns. Furthermore, epidemiologic evidence on chronic diseases pertains more often to foods or diets and less often to single nutrients or other nonnutritive substances (e.g., coffee and tea). Therefore, nutrient-based recommendations must be derived often from the epidemiologic data on dietary patterns. For example, the statement that diets with a high plantfood and low fat content are associated with reduced rates of certain cancers more accurately reflects present knowledge than do conclusions that diets high in selenium or isothiocyanates are likely to reduce cancer risk. The latter requires an inference about cause and effect that is not yet justified by the data.
Recommendations about overall dietary patterns may be difficult to implement, however, if they are too general, devoid of quantification, or provide quantitative information that the average person cannot interpret. For example, the basic five food groups recommended by the USDA are represented in the average fast-food cheeseburger, but not in the desirable proportions (i.e., only a small proportion from the fruit and vegetable group, but high proportions of salt and fat). Alternatively, few people would be able to translate a recommendation to consume a ''lower-fat" diet or only "30% of calories from fat" into appropriate food choices. In light of these considerations, the committee concluded that dietary guidelines to prevent chronic diseases and improve the health of the general U.S. population should emphasize overall dietary patterns but should also incorporate relevant information about food groups, foods, and nutrients.
Quantitative Versus Qualitative Recommendations
The committee considered the extent to which its recommendations could be quantified. In general, its decisions were based on the strength of the evidence. The need for quantification also depended on whether dietary effects have a threshold and whether the effects seem to be linear or curvilinear in nature. Quantitative guidelines can take into account nutrient interactions, they are less susceptible to misinterpretation when translated into food choices, and they can be presented as single numbers or as ranges. Furthermore, they are more likely to result in dietary modification because they provide specific targets.
The committee weighed these advantages against the possibility that specifying quantities might in some cases give the appearance of greater certainty than is justified by the evidence. Overall, the committee found the arguments for quantification compelling.
Recommendations for Individuals as Opposed to Populations
There are two approaches to reducing dietary risk factors for chronic diseases: the first is the individual-based approach aimed at identifying and treating individuals at high risk and the second a more global population-based or public health approach aimed at the general population (Blackburn and Jacobs, 1984; Goldbourt, 1987; Olson, 1986). These two approaches are complementary to each other (Rose, 1985; WHO, 1982).
Recommendations tailored to special needs of individuals based on age, sex, physiological status (e.g., pregnancy and lactation), genetic background, and body build, as well as to special conditions such as occupational exposures and
Page 668
metabolic defects, would be ideal. Recommendations to individuals or special population subgroups could also take into consideration thresholds for nutrient requirements (e.g., upper limits or ranges of nutrient intake set to avoid deficiency or toxicity) or specify an optimal average nutrient intake over time. Recommendations suited to individual needs are desirable because every person is genetically unique, and genetic determinants influence the etiology and pathogenesis of practically all chronic diseases associated with nutritional factors. For example, high blood pressure, obesity, hyperlipidemia and atherosclerosis, and certain cancers appear to aggregate in families because of interaction of genetics and a shared environment. Public health recommendations to modify undesirable dietary patterns are unlikely to apply equally to everyone because genetic-environmental interactions as well as dietary exposures contribute to the outcome in specific individuals.
For conditions such as the hyperlipidemias, we can identify some persons at high risk and concentrate specific preventive efforts in this subpopulation. For other conditions, where specific tests are lacking, a strong family history of the disease may suggest that special preventive approaches are needed. It is usually not feasible, however, to identify people at high risk or to screen the entire population. Moreover, people at only moderate or slightly increased risk—e.g., those with borderline-high blood cholesterol levels—will also benefit greatly from the dietary recommendations given to high-risk individuals (National Cholesterol Education Program, 1988).
For most diseases, we are prevented from making individually based recommendations because of a lack of knowledge about susceptible genotypes or risks to particular individuals and about the distribution of dietary requirements in the population. Nevertheless, dietary recommendations aimed at reducing the risk in the general population can have a major benefit for the nation's health. This is because even a relatively small reduction in risk for a disease that occurs in a large number of people who are at moderate risk could lead to a larger reduction in risk for the total population than a large reduction in risk for a smaller number of people at higher risk. For example, the majority of CHD deaths occurs not among those at high risk because of high serum cholesterol levels, but in people who have only moderate elevations in serum cholesterol (i.e., <240 mg/dl; National Cholesterol Education Program, 1988). Thus, any reduction in the intake of saturated fatty acids, total fat, and cholesterol in this segment of the population could result in a large absolute decrease in CHD deaths. Similarly, for the general population, decreased salt intake may substantially reduce the risk of hypertension and a reduced fat intake may curtail the risk of certain cancers, although the effects on many individuals may be small or absent. Furthermore, although genetic factors can affect individual susceptibility, they appear to account for only a small part of the observed variation in disease incidence among populations, as exemplified by the tendency of migrants to acquire the disease rates of their adoptive countries (see Chapter 5).
Thus, a major focus of any preventive strategy should be to shift the distribution of risk factors (including adverse dietary exposures) in the entire population, thereby decreasing overall disease risk. This is best accomplished through recommendations for the general population. This public health approach requires special strategies, including support of the media, the food industry, nutritionists, public health personnel, the medical profession, educators, and government. Such a policy has many merits if it is feasible to implement without harm to individuals, since it may benefit many people, is simpler to implement, and the overall costs to society are usually low. Examples of such policies in other arenas are mass vaccinations against poliomyelitis despite a wide range of genetic susceptibility to paralysis, fluoridation of the entire water supply to prevent caries despite differences in caries susceptibility (see Chapters 14 and 26), or iron fortification of cereals, even though only children and adult women are at risk of iron deficiency and such fortification may adversely affect those few with hemochromatosis (see Chapters 4 and 14). With advances in knowledge of genetic variability and its interaction with the environment, in the future we will be increasingly able to supplement general recommendations for the population with more sophisticated, individually based dietary intervention.
The committee also considered the relationship between public health goals and dietary recommendations aimed at individuals. Dietary recommendations for individuals are derived almost entirely from data on benefit or risk in certain populations and thus require considerable discretion and clinical judgment in their application. Goals or guidelines for the general population attempt to consider the wide variation in the distribution of dietary or nutrient requirements in the population, but they fail to consider individual
Page 669
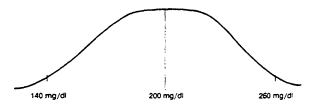
FIGURE 28-1
Hypothetical distribution of serum total cholesterol levels (mean ± 2 SD)
in a population associated with a public health goal of 200 mg/dl.
needs and are therefore not identical to guidelines for the individual.
For example, the recommendation that individuals limit SFA intake to less than 10% of total calories derives mainly from evidence that populations with mean intakes of less than 10% of calories as SFA have low mean serum total cholesterol levels and are relatively free of atherosclerotic diseases. However, this recommended goal for individuals is different from the goal for a population. Figures 28-1 and 28-2 illustrate the different bases of recommendations for individuals and for the population as a whole. In the hypothetical example in Figure 28-1, serum cholesterol levels in a population range from 140 to 260 mg/dl with a mean of 200 mg/dl. This distribution—i.e., the mean ± 2 standard deviations (SD)—is compatible with a goal of 200 mg/dl for the general population (National Cholesterol Education Program, 1988). In contrast, Figure 28-2 shows the population serum cholesterol distribution that might be associated with a recommendation that all individuals lower their serum total cholesterol to 200 mg/dl or less. To achieve this goal (i.e., where very few individuals would have levels above 200 mg/dl) would require a much lower population average of serum total cholesterol levels (i.e., approximately 150 mg/dl).
The dietary recommendations in the following section are directed to individuals, but they incorporate public health goals for the general population as well.
Feasibility of Implementation
Should the feasibility of implementation affect dietary recommendations? For example, if an expert committee concludes that the population would be healthier if fat consumption were reduced from an average of 40% to no more than 10% of total calories, should it consider not only the feasibility of designing nutritionally balanced diets with only 10% of calories from fat but also the
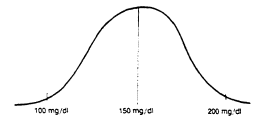
FIGURE 28-2
Hypothetical distribution of serum total cholesterol levels
(mean ± 2 SD) in a population associated with a public health
goal that all individuals lower their serum total cholesterol to
200 mg/dl or less. The range of cholesterol levels is assumed
to be narrower than that shown in Figure 28-1.
feasibility of achieving such dietary change? If such a recommendation would fit within a balanced diet, it could be made in principle, despite the recognition that fat consumption would decline gradually at best and that a more readily attainable goal may encourage more change.
The committee carefully considered the feasibility of designing nutritionally balanced diets based on its recommendations and, to a limited extent, the factors involved in the implementation of its recommendations. In general, however, its recommendations are based on the scientific principles described above.
The Committee's Dietary Recommendations
The dietary recommendations of the Committee on Diet and Health, given below, are directed to healthy, North American adults and children. Wherever evidence permits, the committee attempts to identify the special dietary needs of population subgroups at high risk for specific diseases or with different dietary requirements because of age, sex, or physiological status. The special dietary needs of the elderly are largely unknown.
As discussed above, the quantities proposed in the committee's recommendations are goals for intake by individuals. To achieve these goals, the mean intake by the population (the public health goal) would have to be higher or lower than the recommended intake for individuals, depending on the direction of the proposed dietary modification. For example, a recommendation that all individuals should reduce their fat intake to 30% or less of calories can be expected to lead to a population mean intake substantially below 30% of calories from fat. Similarly, a recommendation that individuals increase their carbohydrate intake to more
Page 670
than 55% of total calories can be expected to lead to a population mean intake clearly above 55% of calories from carbohydrates. Thus, the guidelines for individuals differ somewhat from the public health (population) goals, which need to be more stringent in order to achieve the goals for individuals.
The extent to which the public health goal for a nutrient differs from the goal for individuals in the population will depend on the distribution of intake for that nutrient in the population. In most cases, however, the variation in nutrient intakes in the population is not well known.
The recommendations in this report are the product of a systematic and extensive analysis of the literature by a multidisciplinary committee that considered the criteria and the process for arriving at recommendations and documented the extensive literature on which they are based. They are generally in agreement with the advice provided by other expert panels in the United States and abroad, although in most cases they include more specific quantitative recommendations. These recommendations are appropriate for current patterns of dietary intake and disease morbidity and mortality in the United States and are based on conclusions regarding the association of dietary factors with the entire spectrum of chronic diseases. They take into account competing risks for different diseases as well as nutrient interactions. These recommendations should be reexamined as new knowledge is acquired and as the patterns of morbidity and mortality change over the next decades.
The committee's recommendations are presented in a logical sequence that also reflects a general order of importance. For example, all dietary macrocomponents are addressed first. Among these, highest priority is given to reducing fat intake, because the scientific evidence concerning dietary fats and other lipids and human health is strongest and the likely impact on public health the greatest. Lower priority is given to recommendations on other dietary components, because they are derived from weaker evidence or because the public health impact is likely to be comparatively less. Where the evidence is strongest, the committee presents quantitative recommendations. It recognizes that setting specific quantitative goals is somewhat arbitrary and is based on informed judgment rather than on scientifically derivable formulas; however, quantification facilitates translation of goals into dietary patterns and food choices. Goals are needed to develop and evaluate programs aimed at achieving dietary changes and serve as the basis for regulatory actions such as those relating to food labeling and the validity of health claims for foods and nutrients.
The committee's recommendations derive from an assessment of the evidence on chronic diseases, but should be used in combination with the RDAs to achieve an optimal and highly desirable dietary pattern for the maintenance of good health. In the committee's judgment, these recommendations have the potential for a substantial reduction in the risk of diet-related chronic diseases in the general population.
· Reduce total fat intake to 30% or less of calories. Reduce saturated fatty acid intake to less than 10% of calories and the intake of cholesterol to less than 300 mg daily. The intake of fat and cholesterol can be reduced by substituting fish, poultry without skin, lean meats, and low- or nonfat dairy products for fatty meats and whole-milk dairy products; by choosing more vegetables, fruits, cereals, and legumes; and by limiting oils, fats, egg yolks, and fried and other fatty foods.
A large and convincing body of evidence from studies in humans and laboratory animals shows that diets low in saturated fatty acids and cholesterol are associated with low risks and rates of atherosclerotic cardiovascular diseases. High-fat diets are also linked to a high incidence of some types of cancer and, probably, obesity. Thus, reducing total fat and saturated fatty acid intake is likely to lower the rates of these chronic diseases. Fat intake should be reduced by curtailing the major sources of dietary fats rather than by eliminating whole categories of foods. For example, by substituting fish, poultry without skin, lean meats and low- or nonfat dairy products for high-fat foods, one can lower total fat and saturated fatty acid intake while ensuring an adequate intake of iron and calcium—two nutrients of special importance to women. Dietary fat can also be reduced by limiting intake of fried foods, baked goods containing high levels of fat, and spreads and dressings containing fats and oils.
Different types of fatty acids have different effects on health. SFAs and dietary cholesterol tend to increase total and LDL serum cholesterol and, consequently, the risk of cardiovascular disease. The extent of this activity differs among SFAs; palmitic, myristic, and lauric acids have the greatest cholesterol-raising effect. The main dietary sources of these cholesterol-raising SFAs are dairy and meat products and some vegetable oils, such as coconut, palm, and palm-kernel oils. Dietary cholesterol is found mainly in egg yolks, certain
Page 671
shellfish, organ meats, and, to a lesser extent, in other meats and dairy products. Thus, the intake of these foods should be curtailed. MUFAs are found in a variety of foods but are especially abundant in olive oil and canola oil. PUFAs are of two types—omega-6 and omega-3; both are essential nutrients and cannot be synthesized endogenously. Omega-6 PUFAs are common in several plant oils, including corn, safflower, soybean, and sunflower oils. Omega-3 PUFAs are found in coldwater marine fish (such as salmon and mackerel) and in some plant oils (e.g., soybean and canola oils). Omega-6 PUFAs and MUFAs (and carbohydrates) lower LDL cholesterol when substituted for saturated fatty acids. Omega-3 PUFAs also lower LDL cholesterol when substituted for SFAs, but they are more effective in lowering elevated serum triglyceride levels. Although consumption of fish one or more times a week has been associated with a reduced risk of CHD, the committee does not recommend the use of concentrated fish oil supplements, because there is insufficient evidence that they are beneficial and the absence of long-term adverse effects has not been established.
The evidence linking high-fat diets to increased cancer risk is less persuasive than that associating saturated fatty acids and dietary cholesterol to CHD, but the weight of evidence indicates that high-fat diets are associated with a higher risk of several cancers, especially of the colon, prostate, and breast. Most evidence from studies in humans suggests that total fat or saturated fatty acids adversely affect cancer risk. No studies in humans have yet examined the benefits of changing to low-fat diets; however, such evidence exists from experiments in animals. The combined evidence from epidemiologic and laboratory studies suggests that reduction of total fat is likely to reduce the risk of these cancers.
Epidemiologic data on the possible association of low serum cholesterol levels with an increased incidence of and mortality from cancer in general or colon cancer in men in particular are inconsistent and do not suggest a causal association. Rather, they indicate that the lower serum cholesterol levels in some of these studies were in part the consequence of undetected cancers. The overall evidence indicates that dietary modification to lower serum total cholesterol and CHD risk is likely to reduce the risk of colon cancer without increasing the risk of other cancers.
Animal studies also suggest that high-fat diets may lead to obesity, possibly because dietary fat is converted to body fat more efficiently than are other sources of calories. Short-term clinical studies in humans indicate that a substantial reduction in fat intake may be accompanied by weight loss; however, reduced caloric intake was observed in some of these reports and although not specifically noted is likely to have occurred in others. This indicates that a substantial reduction in fat intake may result in overall caloric reduction, perhaps because of the caloric density of dietary fat. From a public health perspective, this phenomenon may be important, regardless of whether fat reduction per se results in weight loss or whether weight loss results from an overall reduction in caloric intake.
In the committee's judgment, concerns that reduced fat intake may curtail intake of meats and dairy products and thus limit intakes of adequate iron and calcium in women and children or that young children on reduced-fat diets might not obtain adequate calories to support optimal growth and development are not justified. Fat intake can be reduced to approximately 30% of calories without risk of nutrient deficiency, and this level of fat intake after infancy has not been associated with any detrimental effects. Furthermore, adequate caloric intake can readily be maintained in children on diets containing 30% of calories from fat.
Although the committee recommends that the total fat intake of individuals be 30% or less of calories, there is evidence that further reduction in fat intake may confer even greater health benefits. However, the recommended levels are more likely to be adopted by the public because they can be achieved without drastic changes in usual dietary patterns and without undue risk of nutrient deficiency. Furthermore, they permit gradual adaptation to lower-fat diets as more lower-fat foods become available on the market. The committee recommends that people who should not lose weight should compensate for the caloric loss resulting from decreased fat intake by consuming greater amounts of foods containing complex carbohydrates (e.g., vegetables, certain fruits, legumes, and whole-grain cereal products).
Although the committee recommends that SFA intake be maintained at less than 10% of total calories by individuals, it is highly likely that further reduction, to 8 or 7% of calories or lower, would confer greater health benefits. Such further reductions can best be achieved by substituting additional complex carbohydrates and MUFAs for SFAs in the diet. Larger reductions in cholesterol intakes—e.g., to 250 to 200 mg or even less per day—may also confer health benefits.
The committee recommends that the PUFA
Page 672
intake of individuals not exceed 10% of total calories and that PUFA intake in the population be maintained at current levels in the U.S. diet, i.e., an average of approximately 7% of total calories. (The requirement for omega-6 PUFAs can be met by 1 to 2% of calories as linoleic acid.) Concern that an increase in PUFA intake may increase risk of certain cancers derives primarily from studies of animals on very-high-PUFA diets. Given the absence of human diets naturally very high in total PUFAs and the lack of information about the long-term consequences of high PUFA intake (see Chapter 7), it seems prudent to recommend that PUFA intake not be increased above the current average in the U.S. population. However, since most of the PUFAs in the current U.S. diet are of the omega-6 rather than the omega-3 type, and since the committee's recommendation is directed mainly at omega-6 PUFAs, any increase in total PUFA resulting from an increase in foods containing omega-3 PUFAs (e.g., by eating more fish containing such fatty acids) is reasonable.
· Every day eat five or more servings* of a combination of vegetables and fruits, especially green and yellow vegetables and citrus fruits. Also, increase intake of starches and other complex carbohydrates by eating six or more daily servings of a combination of breads, cereals, and legumes.
The committee recommends that the intake of carbohydrates be increased to more than 55% of total calories by increasing primarily complex carbohydrates. Fats and carbohydrates are the two major sources of calories in the diet. National food consumption surveys indicate that the content of the average U.S. diet is high in fat and low in complex carbohydrates (e.g., starches, vegetables, legumes, breads, cereals, and certain fruits). Green and yellow vegetables, fruits, especially citrus fruits, legumes, and whole-grain cereals and breads, which constitute a small portion of the present U.S. diet, generally contain low levels of fat; thus, they are good substitutes for fatty foods and good sources of several vitamins, minerals, complex carbohydrates, and dietary fiber. The recommended number of servings is derived from experience in planning nutritionally balanced diets that would meet the committee's dietary recommendations. The amounts recommended would facilitate an increase in the total carbohydrate and complex carbohydrate content of the diet, make up for the calorie deficit due to fat reduction, and supply sufficient quantities of essential vitamins and minerals. The committee does not recommend increasing the intake of added sugars, because their consumption is strongly associated with dental caries and although they are a source of calories for those who may need additional calories, they provide no nutrients. Furthermore, foods high in added sugars (e.g., desserts and baked goods) are generally also high in fat.
Studies in various parts of the world indicate that people who habitually consume a diet high in plant foods have low risks of atherosclerotic cardiovascular diseases, probably largely because such diets are usually low in animal fat and cholesterol, both of which are established risk factors for atherosclerotic cardiovascular diseases. Some constituents of plant foods, e.g., soluble fiber and vegetable protein, may also contribute—to a lesser extent—to the lower risk of atherosclerotic cardiovascular diseases. The mechanism for the link between frequent consumption of vegetables and fruits, especially green and yellow vegetables and citrus fruits, and decreased susceptibility to cancers of the lung, stomach, and large intestine is not well understood because the responsible agents in these foods and the mechanisms for their protective effect have not been fully determined. However, there is strong evidence that a low intake of carotenoids, which are present in green and yellow vegetables, contributes to an increased risk of lung cancer. Fruits and vegetables also contain high levels of fiber, but there is no conclusive evidence that the dietary fiber itself, rather than other nutritive and nonnutritive components of these foods, exerts a protective effect against these cancers. The committee does not recommend the use of fiber supplements.
Vegetables and fruits are also good sources of potassium. A diet containing approximately 75 mEq of potassium (i.e., approximately 3.5 g of elemental potassium) daily may contribute to reduced risk of stroke, which is especially common among blacks and older people of all races. Potassium supplements are neither necessary nor recommended for the general population.
· Maintain protein intake at moderate levels.
Protein is an essential nutrient, and protein-containing foods are important sources of essential amino acids in the diet. However, because there are no known benefits and possibly some risks in consuming diets with a high animal protein content, the committee recommends that protein
*An average serving is equal to a half cup for most fresh or cooked vegetables, fruits, dry or cooked cereals and legumes; one medium piece of fresh fruit; one slice of bread; or one roll or muffin.
Page 673
intake not be increased to compensate for the caloric loss that would result from the recommended reduction in fat intake. In general, average protein intake by adults in the United States considerably exceeds the RDA, which is 0.8 g/kg of desirable body weight for adults.
The committee recommends maintaining total protein intake at levels lower than twice the RDA for all age groups (e.g., less than 1.6 g/kg body weight for adults).
Increased risks of certain cancers and CHD have been associated in some epidemiologic studies with diets high in meat and, as a consequence, in animal protein and with high protein intake alone in laboratory studies. It is not known whether these adverse effects are due solely to the usually high total-fat, saturated-fatty acid, and cholesterol content of diets that are rich in meat or animal protein, or to what extent protein per se or other factors also contribute. High protein intake may also lead to increased urinary calcium loss.
The committee is aware of concerns among some scientists that animal protein restriction might curtail the ability of some population subgroups with habitually lower protein intakes (e.g., women and the elderly) to meet the RDA for certain other essential nutrients such as iron. However, the recommendation to maintain intake below twice the RDA for all age groups would require no reduction of current average intakes in the United States. The committee does not recommend against eating meat; rather, it recommends consuming lean meat in smaller and fewer portions than is customary in the United States.
· Balance food intake and physical activity to maintain appropriate body weight.
Excess weight is associated with an increased risk of several chronic disorders, including NIDDM, hypertension, CHD, gallbladder disease, osteoarthritis, and endometrial cancer. The risks appear to decline following a sustained reduction in weight. Increased abdominal fat carries a higher risk for these disorders than do comparable fat deposits in the hips and thighs. New standards for healthy body composition take into account such differences in regional body fat distribution as well as weight-to-height ratios. Neither large fluctuations in body weight nor extreme restrictions in food intake are desirable.
In the U.S. population and other westernized societies, body weight and body mass index are increasing while the overall caloric intake of the population is decreasing. These trends as well as the association of moderate, regular physical activity with reduced risks of heart disease lead to the committee's recommendation that the U.S. population increase its physical activity level and that all healthy people maintain physical activity at a moderately active level, improve physical fitness, and moderate their food intake to maintain appropriate body weight. For adult men and women of normal weight, .this will also allow the ingestion of adequate calories to meet all known nutrient needs. Overweight people should increase their physical activity and reduce their caloric intake, and people with a family history of obesity should avoid calorically dense foods and select low-fat foods.
· The committee does not recommend alcohol consumption. For those who drink alcoholic beverages, the committee recommends limiting consumption to the equivalent of less than 1 ounce of pure alcohol in a single day. This is the equivalent of two cans of beer, two small glasses of wine, or two average cocktails. Pregnant women should avoid alcoholic beverages.
Excessive alcohol drinking increases the risk of heart disease, high blood pressure, chronic liver disease, some forms of cancer, neurological diseases, nutritional deficiencies, and many other disorders. Even moderate drinking carries some risk in circumstances that require neuromotor coordination and judgment, e.g., driving vehicles, working around machinery, and piloting airplanes or boats. Consumption of even small amounts of alcohol can lead to dependence. Approximately 10% of those who consume alcoholic beverages in the United States are alcoholics. Pregnant women and women who are attempting to conceive should avoid alcoholic beverages because there is a risk of damage to the fetus and no safe level of alcohol intake during pregnancy has been established.
Although several studies show that moderate alcohol drinking is associated with a lower CHD risk, it would be unwise to recommend moderate drinking for those who do not drink because, in the committee's judgment, a causal association has not been established and because even moderate drinking poses certain other risks, including the risk of alcohol addiction.
· Limit total daily intake of salt (sodium chloride) to 6 g or less. Limit the use of salt in cooking and avoid adding it to food at the table. Salty, highly processed salty, salt-preserved, and salt-pickled foods should be consumed sparingly.
Studies in human populations in different parts of the world show that a diet containing more than
Page 674
6 g of salt per day is associated with elevated blood pressure, and many Americans habitually exceed this level. It is probable that susceptibility to salt-induced hypertension (salt sensitivity) is genetically determined, but no reliable genetic marker has yet been identified. Thus, those who are most susceptible to developing salt-induced hypertension, and therefore likely to benefit most from this recommendation, cannot yet be identified. In salt-sensitive people, the recommended level of salt intake is unlikely to contribute to blood pressure elevation and may even lead to blood pressure reduction. In the general population, the recommended level will have no detrimental effect. The committee is aware that a greater reduction in salt intake (i.e., to 4.5 g or less) would probably confer greater health benefits than its present recommendation, but chose 6 g as an initial goal that can be achieved more readily. This does not preclude a subsequent recommendation for further reduction.
The evidence linking salt intake per se to stomach cancer is less persuasive than that for salt and hypertension. There is consistent evidence, however, that frequent consumption of salt-preserved or salt-pickled foods increases the risk of stomach cancer. The specific causative agents in those foods have not been identified.
· Maintain adequate calcium intake.
Calcium is an essential nutrient; it is necessary for adequate growth and skeletal development. Certain segments of the population, especially women, because of their low caloric intake, and adolescents, because of their higher nutrient requirements, need to make careful food choices to obtain adequate calcium from the food supply. The committee recommends consumption of low- or nonfat dairy products and dark-green vegetables, which are rich sources of calcium and can assist in maintaining calcium intake at approximately RDA levels. Although low calcium intake is associated with a higher frequency of fractures and possibly with high blood pressure, the potential benefits of calcium intakes above the RDAs to prevent osteoporosis or hypertension are not well documented and do not justify the use of calcium supplements.
· Avoid taking dietary supplements in excess of the RDA in any one day.
A large percentage of the U.S. population consumes some vitamin or mineral supplement daily. The supplements are often self-prescribed and not based on known nutrient deficiencies. It is not known what, if any, benefits or risks accrue to individuals or the general population from taking small doses of supplements. Some population subgroups (e.g., those suffering from malabsorption syndromes) may require supplements, but they should take them only under professional supervision. A single daily dose of a multiple vitamin-mineral supplement containing 100% of the RDA is not known to be harmful or beneficial; however, vitamin-mineral supplements that exceed the RDA and other supplements (such as protein powders, single amino acids, fiber, and lecithin) not only have no known health benefits for the population but their use may be detrimental to health. The desirable way for the general public to obtain recommended levels of nutrients is by eating a variety of foods.
Thus, the committee supports the general scientific opinion and the opinions of several other expert panels that have recently commented specifically on supplement use. It emphasizes, however, that the long-term health effects (risks and benefits) of supplements have not been adequately studied.
· Maintain an optimal intake of fluoride, particularly during the years of primary and secondary tooth formation and growth.
There is convincing evidence that consumption of optimally fluoridated water (i.e., 0.7 to 1.2 ppm fluoride, depending on ambient temperature) significantly reduces the risk of dental caries in people of all ages, especially in children during the years of primary and secondary tooth formation and growth. There is no evidence that such fluoride concentrations have any adverse effects on health, including cancer risk. In the absence of optimally fluoridated water, the committee supports the use of dietary fluoride supplements in the amounts generally recommended by the American Dental Association, the American Academy of Pediatrics, and the American Academy of Pediatric Dentistry.
Implications of Recommendations for Food Choices
What do the committee's recommendations imply with regard to selection of foods and food groups? To some extent, this issue is addressed under each recommendation. Therefore, only a synthesis is provided here. Principles of food selection will also be explained in more detail in the committee's forthcoming report to the general public.
Page 675
In summary, the diet recommended by the committee should contain moderately low levels of fat, with special emphasis on restriction of saturated fatty acids and cholesterol; high levels of complex carbohydrates; only moderate levels of protein, especially animal protein; and only low levels of added sugars. Caloric intake and physical activity should be balanced to maintain appropriate body weight. The recommendation to maintain total fat intake at or below 30% of total caloric intake and saturated fatty acid intake at less than 10%, combined with the recommendation to maintain protein intake only at moderate levels, means that for most North Americans it will be necessary to select leaner cuts of meat, trim off excess fat, remove skin from poultry, and consume fewer and smaller portions of meat and poultry. Fish and many shellfish are excellent sources of low-fat protein. By using plant products (e.g., cereals and legumes) instead of animal products as sources of protein, one can also reduce the amount of saturated fatty acids and cholesterol in the diet.
Dairy products are an important source of calcium and protein, but whole milk, whole-milk cheeses, yogurt, ice cream, and other milk products are also high in saturated fatty acids. Therefore, low-fat or skim milk products should be substituted. Furthermore, it is desirable to change from butter to margarine with a low SFA content, to use less oils and fats in cooking and in salad dressings, and to avoid fried foods.
For most people, the recommended restriction of fat intake, coupled with the recommendation for moderation in protein intake, implies an increase in calories from carbohydrates. These calories should come from an increased intake of whole-grain cereals and breads rather than from foods or drinks containing added sugars. For example, bakery goods, such as pies, pastries, and cookies, although they provide complex carbohydrates also tend to contain high levels of total fat, saturated fatty acids, and added sugars, all of which need to be curtailed to meet the committee's recommendations.
In general, vegetables and fruits are unlikely to contribute substantially to caloric intake but are major sources of vitamins, minerals, and dietary fiber. The committee places special emphasis on increasing consumption of green and yellow vegetables as well as citrus fruits, particularly since their consumption in North America is relatively low. The committee's recommendations would lead to a substantial increase in consumption frequency and portion sizes, especially of vegetables, for the average person. Thorough washing of fresh vegetables (especially leafy ones) and fruits will minimize the consumption of pesticide residues in the diet.
The need for restriction of certain dietary components—such as egg yolks; salt; salty, smoked, and preserved foods; and alcoholic beverages—is clearly explained in the recommendations. Further considerations include methods of preparation, cooking, and processing, which can have important effects on the composition of foods. The committee emphasizes the need to read the labels on prepared, formulated, and other processed foods to identify their contribution of nutrients in general and of salt, fats and cholesterol, and sugars in particular. With regard to the risk of chronic diseases, maximum benefit can be attained and any unknown, potentially harmful effects of dietary constituents minimized by selecting a variety of foods from each food group, avoiding excessive caloric intake (especially excessive intake of any one item or food group), and engaging regularly in moderate physical exercise.
Comparison of the Committee's Recommendations with those by Other Expert Groups
Recommendations to the General Population
In the recent history of dietary recommendations for overall health, an expert group from Sweden, Norway, and Finland was among the first to propose in 1968 that the general population should avoid excessive caloric intake, reduce fat intake from 40 to 25-30% of calories, reduce saturated fatty acid intake while increasing dietary polyunsaturated fatty acids, reduce consumption of sugar and sugar-containing foods, and increase the consumption of vegetables, potatoes, skim milk, fish, lean meat, and cereal products (Anonymous, 1968). The next two decades were characterized by a proliferation of dietary recommendations by authoritative groups in the United States, Canada, many western European countries, Japan, Australia, and New Zealand.
In the past decade alone, more than a dozen expert committees, voluntary health organizations, and government agencies in the United States have issued dietary guidelines to promote good health in general or to lower the risk of specific chronic diseases (see Table 28-1). The recommendations for general health mainte-
Page 676
nance include Dietary Goals for the United States, issued in 1977 by a select committee of the U.S. Senate (1977); the Surgeon General's report on Health Promotion and Disease Prevention in 1979 (DHEW, 1979); a joint statement by the American Medical Association and the Food and Nutrition Board in 1979 (Council on Scientific Affairs, 1979); Dietary Guidelines for Americans, issued jointly by the Departments of Agriculture and Health and Human Services in 1980 and revised in 1985 (USDA/DHEW, 1980, 1985); and the Surgeon General's Report on Nutrition and Health (DHHS, 1988). Tables 28-1 and 28-2 summarize recent recommendations for overall health maintenance by official bodies in the United States and several other industrialized countries.
Many expert groups have focused on specific diseases. In the early 1960s, the American Heart Association was the first U.S. organization to recommend dietary modifications for reducing cardiovascular disease risk (Page et al., 1961). The AHA has periodically revised its recommendations, most recently in 1988 (AHA, 1988). The Inter-Society Commission for Heart Disease Resources (1970, 1984) has also periodically proposed dietary recommendations to lower the risk of heart disease in the United States. More recently, a Consensus Conference of the National Institutes of Health resulted in recommendations to lower blood cholesterol (NIH, 1985). Recent recommendations on diet and atherosclerotic cardiovascular diseases in the United States and abroad are summarized in Table 28-3.
Guidelines to lower cancer risk in the United States were first issued by the National Cancer Institute in 1979 and revised by that institute in 1984 and 1987 (NCI, 1984a,b, 1987; Upton, 1979). The National Research Council's Committee on Diet, Nutrition, and Cancer and the American Cancer Society also proposed interim dietary guidelines aimed at lowering cancer risk (ACS, 1984; NRC, 1982). Dietary guidelines on cancer risk in the United States and abroad are summarized in Table 28-4.
Several voluntary health organizations and other expert groups have periodically issued other disease-specific recommendations. For example, the American Diabetes Association (1987) has made recommendations aimed at dietary management of noninsulin-dependent diabetes mellitus (NIDDM), and the National Institutes of Health have recommended weight reduction for overweight individuals and those with obesity-related chronic conditions (NIH, 1984a) and have also proposed dietary modification to prevent osteoporosis (NIH, 1984b).
Tables 28-1 to 28-4 show that there are many similarities among dietary recommendations in the United States and other industrialized countries. Most sets of recommendations deal with the type and amount of fat and cholesterol in the diet; body weight and exercise; complex carbohydrates, fiber, and refined sugars; sodium, salt, or salty foods; alcoholic beverages; and variety in the diet. Some also address avoidance of toxic substances, and two recent statements specifically focus on the intake of dietary supplements (Callaway et al., 1987; Council on Scientific Affairs, 1987). Some of the recommendations specify quantities (e.g., percentage of calories from fat or grams of salt per day), whereas others are general in nature, suggesting that people should eat more of or avoid too much of some dietary component. Most recommendations are directed to the general population, although several expert groups (e.g., the National Cholesterol Education Program, 1988) also highlight the needs of certain high-risk population subgroups. Other organizations (e.g., Council on Scientific Affairs, 1979; NRC, 1980b) have cautioned against aiming broad, sweeping dietary recommendations at the general population.
The general agreement among dietary recommendations from different sources is striking. The vast majority of expert panels have recommended maintenance of appropriate body weight, and on the basis of actuarial data, some have also proposed weight/height standards. These recommendations are aimed at curtailing the prevalence of obesity—a major contributor to several chronic disorders, including hypertension, NIDDM, hyperlipidemia, cardiovascular disorders, some hepatobiliary diseases, and some types of cancer. New standards for health with regard to height, weight, and body composition take into account differences in regional body fat distribution as well as weight/height ratios.
The committee supports the recommendation to maintain appropriate body weight, made by practically all organizations listed in Tables 28-1 to 28-4, and it emphasizes that physical activity and food intake should be balanced in order to avoid obesity. The recommendation to avoid frequent fluctuations in weight and extreme dieting is in accord with similar recommendations from the American Dietetic Association (ADA, 1986).
Perhaps the most common and consistent recommendation for the general population is to limit
Page 677
the intake of total fat, usually to approximately 30% of total calories. This is usually intended to reduce the risk of cardiovascular diseases, certain cancers, and possibly obesity. Most expert panels also suggest a reduction in saturated fatty acid intake, usually to £10% of total calories (see, e.g., AHA, 1986, 1988; Department of National Health and Welfare Canada, 1977; DHEW, 1979; NCI, 1984a,b, 1987; NIH, 1985; USDA/DHHS, 1985; WHO, 1982). There is less general agreement about the proportional intake of PUFAs. The American Heart Association has previously recommended that PUFAs partially replace saturated fatty acids in the diet to make up about 10% of total calories (AHA, 1982); however, their recent guidelines (AHA, 1986, 1988) and those of the National Institutes of Health (NIH, 1985) suggest instead that PUFAs should not exceed 10% of total calories.
Recommendations on dietary cholesterol are also inconsistent, although the most widely accepted recommendation is to limit cholesterol intake to £300 mg/day. Recent suggestions that cholesterol intake be limited to £100 mg/1,000 kcal per day (e.g., AHA, 1986; WHO, 1982) have been reviewed recently by the American Heart Association, which has again recommended that cholesterol intake should be less than 300 mg/day (AHA, 1988)—a dietary goal that can be readily achieved by U.S. adults.
The committee's quantitative limits on the intake of total fat, saturated fatty acids, and cholesterol are consistent with advice from other expert panels in the United States as well as international expert groups on heart disease and cancer (e.g., ACS, 1984; AHA, 1988; Department of National Health and Welfare, Canada, 1977; DHSS, 1984; ECP/IUNS, 1986; NIH, 1985; NRC, 1982; WHO, 1982). The committee points out, however, that the recommended diet would only be ''moderately" low in fat, whereas evidence indicates that further reductions in fat, saturated fat, and cholesterol intake might confer additional benefits; for PUFAs, however, it proposes maintaining intake at the average levels currently consumed by the U.S. population.
Most organizations have also advised increasing complex carbohydrate intake, and some have specified dietary fiber (e.g., Commonwealth Department of Health/National Health and Medical Research Council, 1983; Department of National Health and Welfare, Canada, 1982; NACNE, 1983; National Advisory Committee, New Zealand, 1982; NCI, 1984a,b, 1987), usually with a concomitant decrease in consumption of refined sugars. These guidelines generally stem from concern about diabetes, obesity, dental caries, or cancer. However, they are less often stated in quantitative terms, perhaps because the evidence linking these components to specific diseases is (with the exception of sugars and dental caries) less clear or convincing than for fats. Complex carbohydrates are generally recommended in preference to refined sugars, even though there is only minimal evidence linking sugar intake per se to specific health problems (except for dental caries). Addition of refined sugars to the diet contributes calories without providing any essential nutrients. As discussed in Chapter 24, recent studies have focused on the glycemic index of different foods in subjects with NIDDM, but no clear and clinically significant conclusions can yet be drawn from such studies, especially for individuals without the disease.
Recommendations on dietary fiber intake are less consistent within the United States, although as shown in Table 28-3, increased fiber intake has been recommended by expert groups from the United Kingdom, Canada, Australia, and New Zealand. In the United States, recommendations on fiber range from suggestions to increase intake to 20 to 35 g/day (LSRO, 1987; NCI, 1984a,b, 1987) to recommendations simply to consume more fiber (USDA/DHHS, 1985) or to increase consumption of high-fiber vegetables, fruits, and whole-grain cereal products (NRC, 1982). In some cases, dietary fiber is subsumed under complex carbohydrates. The absence of definitive data has precluded recommendations on specific types of dietary fibers (e.g., soluble and insoluble).
The Committee on Diet and Health agrees with most other expert groups in proposing that the intake of vegetables, fruits, and other sources of complex carbohydrates should be increased and that the intake of added sugars should be limited (e.g., ACS, 1984; AHA, 1988; DHEW, 1979; DHSS, 1984; NIH, 1985; NRC, 1982; USDA/ DHHS, 1985). The committee's recommendations extend beyond those of most other groups because they specify the minimum number of servings per day and propose a quantitative goal for total carbohydrate intake. However, unlike some expert panels (e.g., LSRO, 1987; NCI, 1984a,b, 1987), the committee believes that the strength of the evidence does not justify making specific recommendations pertaining to dietary fiber at this time. The committee's recommendation to emphasize the consumption of vegetables, fruits, and other sources of complex carbohydrates would, however,
Page 678
| TABLE 28-1 Dietary Recommendations to the U.S. Public, 1977 to 1989 | |||||||||||
| Type of Recommendation Reference | Maintain Appropriate Body Weight, Exercise | Limit or Reduce Total Fat (%kcal) | Reduce Saturated Fatty Acids (%kcal) | Increase Polyunsat -urated Fatty Acids (%kcal) | Limit Cholesterol (mg/day) | Limit Simple Sugars | Increase Complex Carbohydrates (% kcal from total carbohydrates) | Increase Fiber | Restrict Sodium Chloride(g) | Moderate Alcohol Intake | Other Recommendations |
| General Health Maintenance | |||||||||||
| U.S. Senate | Yes | 27-33 | Yes | Yes | 250-350 | Yes | Yes | Yes | 8 | Yes | Reduce additives processed foods |
| Council on | Yes | No | No | No | No | Yes | NC | NC | 12 | Yes | Consider high-risk |
| DHEW (1979) | Yes | Yes | Yes | NS | Yes | Yes | Yes | NS | Yes | Yes | More fish, poultry |
| NRC (1980b) | Yes | For weight reduction only | No | No | No | For weight reduction only | No | No | 3-8 | For weight | Variety in diet; consider high-risk groups |
| USDA/DHHS (1980; 1985) | Yes | Yes | Yes | No | Yes | Yes | Eat adequate starch and fiber | Yes | Yes | Yes | Variety in diet; consider high-risk groups |
| DHHS (1988) | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | Fluoridation of water; adolescent girls and women increase intake of calcium-rich foods; children, adolescents and women of childbearing age increase intake of iron-rich foods |
Page 679
| Type of Recommendation Reference | Maintain Appropriate Body Weight, Exercise | Limit or Reduce Total Fat (% kcal) | Reduce Saturated Fatty Acids (%kcal) | Increase Polyun- saturated Fatty Acids (%kcal) | Limit Cholesterol (mg/day) | Limit Simple Sugars | Increase Complex Carbohydrates (% kcal | Increase | Restrict Sodium Chloride (g) | Moderate Alcohol Intake | Other Recommendations | |||
| Diet and | Balance energy intake and expenditure | £30 | <10 for individuals and 7-8 population mean | Up to 10 for individuals and ~7 population mean | <300 | Yes | (At least 55); >five daily servings of vegetables and fruits; >six daily servings of cereals, breads, and legumes | Directly through vegetables, fruits, and cereals | £6 g/day with a goal of 4.5 g/day | If you drink, limit to < 1.0 oz alcohol or <2 drinks/day | Avoid dietary supplements, especially in excess of RDAs; drink fluoridated water; limit protein intake to moderate levels (less than twice the RDA) | |||
| Heart Disease | ||||||||||||||
| Inter-Society | Yes | <30 | 8 | 10 | <250 | NC | Increase to make up caloric deficit | NC | 5 g/day | NC | NS | |||
| NIH (1985) | Yes | <30 | <10 | Up to 10 | 250-300 | Endorsed Recommendations of AHA (1982 and Inter-Society Commission for Heart Disease Resources (1984) | NC | NC | Specific recommendations for high-risk groups; also physicians, public, and food industry | |||||
| AHA (1988) | Yes | <30 | <10 | Up to 10 | <300 | NS | (50 or more) | NS | £3 g/day | 1-2 oz | Protein to make up remainder of calories; wide variety of foods | |||
| Cancer | ||||||||||||||
| NRC (1982) | NC | ~30 | Yes | No | NC | NC | Through whole grains, fruits and vegetables | NS | By limiting intake of salt-cured, pickled, smoked foods | Yes | Emphasize fruits and vegetables; avoid high doses of supplements; pay attention to cooking methods | |||
| ACS (1984) | Yes | ~30 | Yes | No | NC | NC | Same as NRC (1982) | Yes | Same as NRC (1982) | Yes | Same as NRC (1982) | |||
| NCI (1987) | Yes | Yes | Yes | No | NC | NC | Yes, more whole grains, fruits, and vegetables | To 20-35 g | NC | Yes | Variety in diet; avoid fiber supplements | |||
Page 680
| TABLE 28-1 Continued | |||||||||||
| Type of Recommendation Reference | Maintain Appropriate Body Weight, Exercise | Limit or Reduce Total Fat (%kcal) | Reduce Saturated Fatty Acids (%kcal) | Increase Polyunsa-turated Fatty Acids (%kcal) | Limit Cholesterol (mg/day) | Limit Simple Sugars | Increase Complex Carbohydrates (%kcal from total carbohydrates) | Increase Fiber | Restrict Sodium Chloride (g) | Moderate Alcohol Intake | Other Recommendations |
| Osteoporosis | |||||||||||
| NIH (1984b) | Exercise | NC | NC | NC | NC | NC | NC | NC | NC | NC | Raise calcium to mg/day (premenopausal), 1,500 mg/day(postmenopausal); use calcium supplements if needed; use vitamin D for calcium absorption |
| Diabetes | |||||||||||
| American | Yes | <30 | Yes | No | <300 | Yes | (55-60) | Yes | Yes | Yes | Nonnutritive sweeteners permitted but not recommended; limit protein to RDA level; avoid supplements except in special cases |
| NOTE: NC = No Comment; NS = Not Specified | |||||||||||
Page 681
indirectly result in increased consumption of dietary fiber.
Recommendations on protein intake have seldom been included among dietary guidelines by expert groups in the United States, and protein intake per se has received little attention compared to calories, fats, or carbohydrates. However, an expert panel in Ireland (Department of Health, Ireland, 1984) proposed reducing protein intake to 1 g/kg body weight—i.e., approximately the RDA level (NRC, 1980a)—and a panel in the Netherlands suggested that only 30 to 50% of protein should come from animal sources (Food and Nutrition Council, Netherlands, 1983-1984). Furthermore, protein-containing foods have been highlighted by several international expert panels who suggest selection of lean meats, more poultry and fish, and foods with more vegetable and less animal protein (e.g., Department of Health, Ireland, 1984; Food and Nutrition Council, Netherlands, 1983-1984; National Advisory Committee, New Zealand, 1982; WHO, 1982). In the United States, an earlier Surgeon General's Report (DHEW, 1979) recommended consumption of less red meat and more poultry and fish, while the 1988 report (DHHS, 1988) recommends selection of lean meats in addition to poultry and fish.
The Committee on Diet and Health proposes maintaining protein intake at moderate levels (i.e., <1.6 g/kg body weight for adults). This reflects its judgment that there is no benefit from consuming amounts of protein that are higher than the RDA and that there is some evidence that diets excessively high in animal protein may be harmful to health.
With few exceptions, experts recommend a reduction in salt intake generally or to a specific level to reduce the risk of hypertension in the population. Several expert groups concerned with cancer risk also suggest limiting salt-cured and salt-pickled foods to lower the risk of stomach cancer (ACS, 1984; NRC, 1982; Panel on Nutrition and Prevention of Diseases, 1983). The Panel on Nutrition and Prevention of Diseases (1983) in Japan singled out salt as a possible causative agent for stomach cancer. No concrete recommendations have been made concerning calcium, magnesium, or chloride to reduce the risk of hypertension.
The committee's recommendation to limit salt intake to 6 g/day or less is similar to the recommendations of other expert groups and pertains both to hypertension and to stomach cancer. However, the committee specifically acknowledges the existence of genetic predisposition to salt-induced hypertension and also makes a specific quantitative recommendation for potassium intake.
Even though consumption of alcoholic beverages has been addressed by only about half the expert groups, their recommendations are fully consistent. There is general agreement that excessive alcohol intake should be avoided; moderation is usually recommended for those who drink, but it is often not defined. This recommendation stems from concern about the risk of chronic liver disease, hypertension, some forms of cancer, and cardiovascular diseases.
The committee's overall recommendation on alcoholic beverages is in agreement with others (e.g., ACS, 1984; DHHS, 1988; NACNE, 1983; NCI, 1984a,b, 1987; NRC, 1982; Swedish National Food Administration, 1981; USDA/DHHS, 1985). It makes a specific mention of the need to avoid alcohol intake in pregnancy—an issue still not fully resolved in the judgment of some experts (NIAAA, 1986). The committee supports the general opinion that a recommendation that would encourage moderate drinking for the general population to lower the risk of coronary events would not be prudent, since the data do not establish a causal association (Castelli, 1979; Hennekens et al., 1979).
Nutrient adequacy has been primarily the focus of the RDAs, which are developed by the Food and Nutrition Board (NRC, 1980a). The USDA/ DHHS Dietary Guidelines for Americans (USDA/ DHHS, 1985) addressed adequate nutrient intakes in its recommendation to "Eat a variety of foods." The American Dietetic Association's recommendations for women emphasized the need for adequate consumption of calcium and, during the years of menstruation, also of iron (ADA, 1986). The statement on osteoporosis issued by the NIH Consensus Development Conference recommends intake of 1,000 to 1,500 mg of calcium daily, which exceeds the current RDA of 800 mg (NIH, 1984b). Most discussions of nutrient adequacy continue to use the RDAs as the standard for adequate nutrient intakes.
The Committee on Diet and Health does not specifically address nutrient adequacy in its report; however, in its overall recommendations, it takes into account the adequacy of certain nutrients whose intake might be curtailed (e.g., calcium or iron) or greatly exceeded (e.g., protein) as a result of the recommendations. Furthermore, it emphasizes that in planning optimal diets to attain
Page 682
| TABLE 28.2 General Dietary Recommendations in Other Industrialized Countries, 1978-1987 | |||||||||||
| Country (Reference) | Maintain Appropriate Body Weight | Limit or Reduce Total Fat(% kcal) | Reduce Saturated Fatty Acids (%kcal) | Increase Polyunsatur-ated Fatty Acids (%kcal) | Limit Cholesterol (mg/day) | Limit Simple Sugars | Increase Complex Carbohydrates (%kcal from total carbohydrates) | Increase Fiber | Restrict Sodium Chloride | Moderate Alcohol Intake | Other Recommendations |
| Sweden (Swedish National Food Administration, 1981; Expert Group for Diet and Health, 1985) | Yes | 25-35 | Yes | P/S= 0:5a | Yes | < 10% of energy | Yes (50-60) | >30 g/day | ~7-8 g/day | Yes | Varied diet; exercise; regular meals |
| France (Dupin et al., 1981) | Yes | 30-35 | Yes | NS | NS | Yes | (50-55) | Yes | Yes | <10% kcal | Water fluoridation |
| Norway (Royal Ministry of Health and Social Services, 1981-1982) | NC | <35 | Yes | P/S = 1:2 | NS | < 10% of energy | Yes (50-60) | Yes | NC | NC | Maintain adequate |
| Canada (Department of National Health and Welfare, 1982) | Yes | 35 | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Exercise |
| New Zealand (National Advisory Committee, 1982) | Yes | Yes | Yes | NS | NS | Yes | Yes | Yes | Yes | Yes | Variety; less animal protein; |
| Australia (Commonwealth Department of Health/ National Health and Medical Research Council, 1983, 1987) | Yes | 33 | NC | NC | NC | <12% of | Indirectly | To 30 g/day | To 100 mmol/day | <5% kcal/day | Promote breastfeeding; |
| Year 2000 targets | |||||||||||
Page 683
| TABLE 28-2 Continued | |||||||||||
| Country (Reference) | Maintain Appropriate Body Weight | Limit or Reduce Total fat (% kcal) | Reduce Saturated Fatty Acids (% kcal) | Increase Polyunsat-urated Fatty Acids (%kcal) | Limit Cholesterol (mg/day) | Limit Simple Sugars | Increase Complex Carbohydrates (% kcal from total carbohydrates) | Increase Fiber | Restrict Sodium Chloride | Moderate Alcohol Intake | Other |
| Netherlands (Food and Nutrition Council, 1983-1984) | Yes | 30-35 | Yes | Max. 10% | Yes | Yes | NS | NC | NC | Yes | Variety |
| United Kingdom (NACNE, 1983) | Yes | 30 | 10 | NS | No | To 20 kg/year | Through whole grains, vegetables, and fruits | To 30 g/day | Decrease by 3 g/day | £4% of calories | Exercise; food labeling; nutrition education |
| Federal Republic of Germany (German Society of Nutrition, 1985) | Yes | Yes | NS | NS | NS | Avoid excess | Fresh fruits and vegetables, whole-grain cereals | Yes | Yes | Yes | Variety; small, frequent meals; proper cooking; sufficient protein |
| Ireland (Department of Health, 1984) | Yes | £35 | Yes | NC | NC | Moder | Yes | To 20-35 g/day | <9 g/day | <5% kcal | Reduce protein to 1 g/kg body weight; more vegetable protein |
| Japan (Japanese Ministry of Health and Welfare, 1985) | Yes | 20-25 | Yes | Use vegetable and fish oils | NC | NC | NC | NC | < 10 g/day | NC | Varied diet (at least 30 foods daily); home cooking; pleasant eating environment |
| a Ratio of polyunsaturated to saturated fatty acids. | |||||||||||
| NOTE: NC = No comment; NS = Not specified. | |||||||||||
Page 684
maximal benefit, it is advisable to use the RDAs in combination with its dietary recommendations.
The absence of supportive data precluded a specific recommendation about the need for variety in-the diet or the number of meals per day. Nevertheless, the committee supports the concepts of eating a variety of foods to ensure nutrient adequacy and eating meals regularly in a pleasant environment as proposed by the Japanese Ministry of Health and Welfare (1985).
In the United States, three recent statements have specifically addressed the use of vitamin-mineral supplements (ADA, 1987; Callaway et al., 1987; Council on Scientific Affairs, 1987). In general, these groups and others listed in Tables 28-1 through 28-4 consider supplementation to be warranted only under special conditions when nutrient needs cannot be or are not being met by diet alone. These conditions include nutrient malabsorption (resulting, for example, from gastrointestinal tract damage or drug-nutrient interactions), nutrient depletion (e.g., in chronic diarrhea), or increased physiological requirements (e.g., during pregnancy and lactation). These same organizations usually warn against megadoses of supplements (although megadoses are seldom defined), usually because of the risk of toxicity from fat-soluble vitamins and the more recently recognized toxicity of certain water-soluble vitamins (e.g., pyridoxine). The committee supports these recommendations. It stresses, however, that although the acute toxicity of many nutrients is well documented, the long-term health effects (risks or benefits) of low levels of supplements have not been adequately studied (see Chapter 18). The committee supports fluoridation of water to prevent dental caries.
In summary, the few differences of opinion on dietary recommendations stem largely from incomplete data on diet and chronic diseases. The absence of clearly defined and universally accepted criteria for interpreting the evidence and formulating dietary recommendations to the public has also hampered the achievement of consensus. Expert groups also sometimes differ about the target population, i.e., whether recommendations should be directed to the general population or only to high-risk groups (e.g., Council on Scientific Affairs, 1979; DHEW, 1979; NRC, 1980b). Sometimes a comparison of recommendations tends to highlight inconsistencies, because not all expert panels address all dietary components or diseases and their recommendations may be focused on a single chronic disease such as cancer or heart disease rather than on overall health (e.g., AHA, 1988; NRC, 1982; USDA/DHHS, 1985). Furthermore, there is often a difference of opinion about the importance of diet in comparison to other environmental and genetic risk factors for specific chronic diseases and, consequently, about the potential impact of dietary modification on these risk factors. The Committee on Diet and Health recognizes the importance of genetic variation for dietary recommendations. Its recommendations are intended to improve the health of the total population without harming anyone, although not every individual may benefit equally.
Recommendations Pertaining to Age, Sex, and Physiological Status
Most of the dietary recommendations summarized in Tables 28-1 through 28-4 are directed to the general population (i.e., to adults), although several expert groups have also commented on their applicability to children, the elderly, and women (e.g., ADA, 1986; NIH, 1985). Because nutrient and dietary needs often vary by age, sex, and physiological status, there is often a question about whether one set of dietary recommendations can be justified for the whole population. Following are the specific reasons for concern:
· Are the data pertaining to the pediatric diet and the subsequent risk of adult chronic diseases complete or convincing enough to justify modifying diet in childhood? (See Chapters 7, 19, and 20.)
· Will fat-restricted or calorie-restricted diets curtail growth and lead to protein or micronutrient deficiency in young children? (See Chapter 7.)
· Do the general recommendations address the special needs of all women or of pregnant and lactating women in particular? (See following section, Potential Adverse Consequences of Dietary Recommendations.)
· Will restriction of dietary fats, calories, and other nutrients place elderly people, whose caloric intake is often low, at special risk of nutrient deficiency? (See following section, Potential Adverse Consequences of Dietary Recommendations.)
The-Inter-Society Commission for Heart Disease Resources (1970) was the first to recommend that infants and children should also modify their diets with the objective of preventing atherosclerotic diseases in later life. The American Academy of Pediatrics (AAP, 1983) believed that the rela-
Page 685
tionship of childhood arterial lesions to clinically significant lesions in adults had not been proven, that the effectiveness of dietary modification in preventing CHD had not been established, and that it might be hazardous to tamper with a diet that has been successful in promoting growth and preventing other diseases in children. However, the AAP agreed that children at high risk, usually defined as those with more than 230 mg/dl serum total cholesterol, should be advised to modify their diets or possibly to begin drug therapy (AAP, 1983).
In the 1970s, evidence increasingly indicated that U.S. children had higher plasma cholesterol levels than did children in other countries and that they might thus be at higher risk of CHD in adulthood. In 1983, the American Heart Association recommended that all children over 2 years of age reduce total fat intake to 30% or less of calories, with 10% or less from saturated fatty acids and not more than 10% from polyunsaturated fatty acids and that they should reduce cholesterol intake to 100 mg/1,000 kcal (AHA, 1983). Similar recommendations were made by the American Health Foundation (1983) and at the NIH Consensus Development Conference in 1984 (NIH, 1985). The AAP Committee on Nutrition stated, however, that "current dietary trends in the United States toward a reduced consumption of saturated fats, cholesterol and salt and an increased intake of polyunsaturated fats should be followed with caution. Diets that avoid extremes are safe for children" (AAP, 1983).
The recent recommendations of these expert groups are remarkably similar, despite the sharp division in opinion in previous years about the appropriateness of fat-modified diets for children. In the United States, dietary intakes of fat and cholesterol by children and adults have declined in recent years; continued reductions would bring actual intakes very close to those recommended by the American Heart Association (AHA, 1983). Thus, the only major difference between the recommendations of the American Heart Association, the American Health Foundation, and the National Institutes of Health and those of the American Academy of Pediatrics is the absence of quantitative targets in the recent American Academy of Pediatrics' statement (AAP, 1983). These issues are discussed in more detail in Chapter 7.
Relatively little attention has been given to the role of the pediatric diet in modifying the risk of such other diseases in adults as hypertension and obesity. In general, short-term intervention trials have not provided impressive data to suggest that sodium intake affects blood pressure in normotensive children, but the data from observational studies concerning sodium intake and blood pressure are more consistent and more impressive. It is well established that populations that maintain low sodium intake from birth do not experience a rise in blood pressure with age, nor do they develop clinical hypertension. It is not clear, however, whether there is a threshold for the effect of salt on clinical hypertension. In general, populations consuming 1,200 mg of sodium or less per day (£ 3 g of salt) have very low rates of hypertension, whereas salt intakes above 3 g/day from a young age appear to show a direct, linear relationship with the risk of hypertension in adults (MacGregor, 1985). There is less convincing evidence about the effect of childhood intakes of potassium, calcium, and polyunsaturated fatty acids on hypertension in adulthood (Miller et al., 1987, 1988).
Data on the effects of diet in infancy or early childhood on the development of cancer in adults are extremely limited. Therefore, no specific dietary recommendations have been aimed at reducing cancer risk from childhood. On the basis of the overall evidence on dietary factors and carcinogenesis, however, particularly the changes observed in migrant populations (see Chapter 22), it is reasonable to conclude that childhood eating patterns are important determinants of adult risk of certain diet-related cancers, most notably breast cancer and stomach cancer. This important area requires additional study.
Considerably more is known about the correlation between diet in infancy and childhood and the development of obesity in adults (see Chapters 6 and 21). It is generally recognized that overeating and obesity in infancy are not good predictors of obesity in adulthood but that the correlation between the two improves with age and that adiposity in later childhood is an increasingly better predictor of obesity in adolescence and adulthood (Garn and LaVelle, 1985; Shapiro et al., 1984).
There is little doubt about the importance of dietary patterns (especially patterns of sugar consumption) in children and the development of dental caries (see Chapter 26). On the other hand, there is little information pertaining to childhood eating patterns and NIDDM in adults.
The committee's review of the limited evidence on the role of the pediatric diet in predisposition to chronic diseases in adulthood suggests that its dietary recommendations to the general public are
Page 686
| TABLE 28-3 Dietary Recommendations to Lower Coronary Heart Disease Risk in the United States and Abroad | |||||||||||
| Country (Reference) | Target Populationa | Body Weight/ | Total fat (% kcal) | Saturated Fatty Acids (% kcal) | Polyun- | Cholesterol (mg/day) | Complex Carbohydrates and Fiber | Simple Sugars | Sodium Chloride | Alcohol Intake | Other Recommendations |
| Sweden, Finland, Norway(Anonymous, 1968) | GP | Reduce calories to avoid obesity; exercise | Reduce to 25-35 | Reduce | Increase | NC | Increase vegetables, fruits, potatoes | Decrease | NC | NC | 10-12% of calories from protein, of which 30-50% should be of animal origin |
| United States (American Health Foundation, 1972) | GP | Avoid obesity | Reduce to 35 | Isocaloric amounts of SFAs, PUFAs, and MUFAs | 300 | Increase | NC | Reduce to 5 g/day | NC | NC | |
| Netherlands (Netherlands Nutrition Council, 1973) | GP | Maintain appropriate body weight | 33 | Restrict | 10-13 | 250-300 | Increase to make up caloric needs | Use little | NC | NC | NC |
| Federal Republic of Germany (Pahlke, 1975) | GP | NC | Reduce | Reduce | Increase | Reduce | NC | NC | NC | NC | NC |
| New Zealand (National Heart Foundation of New Zealand, 1976) | GP HR | Maintain appropriate body weight | 35 | Reduce, especially for HR | HR should substitute for SFA | Reduce | NC | Restrict to reduce weight | NC | Restrict to reduce weight | NC |
| Canada (Department of National Health and Welfare, 1977) | GP | Maintain appropriate body weight | Reduce to 35 | 10 | 10 | NC | Increase | NC | Restrict | NC | Variety of foods |
| Australia (National Heart Foundation of Australia, 1979) | HR | Avoid obesity | Reduce to 30-35 | P:Sb =1:0 | Restrict | Eat enough | Use less | Restrict | Moderation | Focus on HR food labeling | |
| United Kingdom (Ad Hoc Working Group on Coronary Prevention, 1982) | GP | Avoid obesity; increase exercise | 30 | <10 | NC | NC | Increase | NC | NC | NC | Special attention to children |
| Wold Health Organization (WHO, 1982) | GP | Avoid obesity | Reduce to 20-30 | <10 | Up to 10 | < 300 | Increase | NC | < 5 g/day | Drink less | Emphasis on foods, fish, lean meats, dairy products, and fewer whole eggs |
Page 687
| Country (Reference) | Target Populationa | Body Weight/ | Total fat (% kcal) | Saturated Fatty Acids (% kcal) | Polyunsat-urated Fatty Acids (% kcal) | Cholesterol (mg/day) | Complex Carbohydrates and Fiber | Simple Sugars | Sodium Chloride | Alcohol Intake | Other Recommendations |
| Japan (Panel on Nutrition and Prevention of Diseases, 1983) | GP | NC | 20-25 | NC | Cook with vegetable oil | NC | Increase | Reduce | Limit to < 10 g/day | Avoid too much | Variety; eat enough protein, half from vegetables and half from animal sources; eat enough potassium, especially from green, leafy vegetables. Eat lean meat and fish; eat fewer confections |
| United Kingdom (DHSS, 1984) | GP | Avoid obesity; exercise | Reduce to 35 | Reduce to 15 | NS; P/S ~0.45 | NS | Increase breads, cereals, fruits, vegetables | NC | Decrease | <90 ml/day for males; <65 ml/day for females | Special Recommendations to government, professionals, industry |
| United States (Inter-Society Commission for Heart Disease Resources, 1984) | GP | Control obesity | <30 | 8 | 10 | <250 | Increase to make up caloric loss | NC | 5 g/day | NC | NS |
| United States (NIH, 1985) | GP HR | Maintain appropriate body weight | <30 | <10 | Up to 10 | 250-300 | Endorsed earlier recommendations of AHA (1982) and the Inter-Society Commission groups; for Heart Disease Resources(1984) | NC | NC | Special recommendations | |
| Finland (Finnish Heart Association, 1987) | GP HR | Avoid excess weight; exercise | <30 | Reduce | P/S >0.5 | Reduce | NC | NC | Reduce for HR <5 g/day | Moderation | Avoid trace element deficiencies; food labeling; focus on HR groups |
| Canada (Canadian Consensus Conference on Cholesterol, 1988) | GP | Adjust caloric intake and expenditure | <30 | <10 | <10 | Restrict through less organ meats and egg yolks; for HR <300 mg | Increase | NC | Limit | Limit | Focus on HR groups limit protein |
| United States (AHA, 1988) | GP | Maintain appropriate body weight | <30 | <10 | Up to 10 | <300 | Increase to derive >50% kcal from total carbohydrates | NS | £3 g/day of sodium | 1-2 oz ethanol/day | Protein to make up remainder of calories; wide variety of foods |
| a GP = General population; HR = High-risk population. | |||||||||||
Page 688
| TABLE 28-4 Dietary Recommendations to Lower Cancer Risk in the United States and Abroad | ||||||||||
| Country | Main- | Limit | Modify | Emphasize Fruit | Increase | Restrict | Food | Food | Alcohol Intake | Other Recommendations |
| United States | NC | To ~30 | NC | Especially citrus fruits, green and yellow and cruciferous vegetables | Whole-grain products | Indirectly | Minimize cured, pickled, and smoked foods | Monitor, test, and reduce exposure | Drink less, if at all | Monitor and test mutagens and carcinogens; recommendations made to government, scientists, and industry |
| Japan (Panel on Nutrition and Prevention of Diseases, 1983) | NC | Avoid excess | NC | Especially green and yellow vegetables, oranges, carotene, and fungi | Unrefined cereal, seaweed, fiber-rich legumes | Yes | Avoid hot drinks and burned food | NC | Same as NRC (1982) | Varied diet; chew food well |
| United States | Yes | To ~30 | NC | Especially vitamin A- and C-rich foods and cruciferous vegetables | High-fiber foods, whole-grain cereals | NS | Same as NRC (1982) | NS | Same as NRC (1982) | NC |
| Canada | Yes | Reduce | Decrease saturated fatty acids and cholesterol | Yes | More fiber-containing foods | NS | Same as | Same as | Two or fewer drinks per day, if any | NC |
| Europe | Yes | To <30 | NC | Yes | Yes | To<5 g/day | Same as NRC (1982) and NCI (1987) | Same as NRC (1982) and NCI (1987) | Same as NRC (1982) | Varied diet; recommendations made to government, scientists, and industry |
| United States | Yes | To ~30 | NC | Vitamin A-rich green and yellow and cruciferous vegetables, citrus fruits | Whole-grain products; eat 20-30 g fiber/day | NS | Same as NRC (1982); avoid frying and high-temperature cooking | NC | Same as NRC (1982) | Balanced diet; read labels; follow USDA/DHHS (1985) guidelines |
Page 689
| TABLE 28-5 Studies Demonstrating an Inverse Relationship Between Serum Cholesterol and Cancer Mortalitya | |||||||||
| Number in Study | Age (years) | Years | Site-Specific | Variables | Mean Cholesterol | Comments | |||
| Study, Year (Reference) | Male | Female | Male | Female | |||||
| Six studies pooled, 1974 | 36,211 | — | 35-64 | — | 5-23 | Colonb | NR | NR | Study of colon cancer only (90 colon cancer deaths) |
| Evans County, Georgia, 1980 (Kark et al., 1980) | 948c | 970c | 15-74 | 15-74 | 12-14 | All except pancreas, ovary, and basal cell | Age, race, overweight, social class, smoking | White male: 213 | Statistical significance of inverse relationships in males only; low serum cholesterol correlated with low vitamin A levels (166 cancer cases; 103 cancer deaths) |
| Honolulu Heart Study, 1980 (Kagan et al., 1981) | 8,006 | — | 45-64 | — | 9 | Colonb | Age, systolic blood pressure, cigarette smoking, alcohol, relative weight | 218 (survivors) | Greatest risk at cholesterol £ 180 |
| Paris Prospective Study | 7,603 | — | 43-52 | — | 6.6 | All except bronchus and lungs | NR | 223 (survivors) | Study suggests low cholesterol levels secondary to preexisting disease (134 cancer deaths) |
| New Zealand Maoris, | 319 | 311 | 25-74 | 25-74 | 11 | NR | Age, systolic blood pressure, Quetelet body mass index | Male: 225 | Effect of preexisting disease considered; numbers small; |
| Puerto Rico Heart | 9,824 | — | 45-64 | — | 8 | NR | Relative weight, heart rate, physical activity, hematocrit, education, cigarette smoking | Rural: 196 | After multivariate analysis, inverse relationship only in rural men; greatest risk at serum cholesterol £ 165 (179 cancer deaths) |
| Whitehall Study, 1980 | 17,716 | — | 40-64 | — | 7.5 | Lung, | NR | 197 (plasma) | Study suggests low cholesterol levels secondary to preexisting disease (353 cancer deaths) |
| Framingham Heart | 2,336 | 2,873 | 35-64 | 35-64 | 24 | Men: colon and all other sites combinede | Age, alcohol, cigarette smoking, | Male: 235 | Inverse relationship only in males; greatest risk at serum cholestrol £ 190; inverse relationship for LDL cholesterol and cancer (691 incident cancers) |
| a Adapted from Sidney and Farquhar, 1983. | NOTE: NR = Not reported | ||||||||
| b p < .05. | |||||||||
| c White. | |||||||||
| d Black. | |||||||||
| e p < .01. | |||||||||
Page 690
also suitable for children after infancy. It is well recognized that there are critical stages in life when eating habits are formed. Although additional research is needed to clarify the interrelationship between childhood eating patterns and most chronic diseases in adults, there is sufficient basis for assuming that the proposed recommendations will be beneficial to children and unlikely to adversely affect their growth and development.
Potential Adverse Consequences of Dietary Recommendations
The committee considered the potential benefits (see next section on Public Health Impact) and adverse consequences of its dietary recommendations by using several approaches: examining concordance among trends in life expectancy and the rates and trends of mortality from cardiovascular disease, cancer, and other major causes of death, both within and among countries; assessing concordance between dietary patterns and mortality rates; estimating risk in the population attributable to dietary factors; examining concordance of the habitual diet with diet-related risk factors; estimating the potential for nutrient deficiency or toxicity in some population subgroups or individuals at the ranges of intake recommended for the general population; and examining the evidence on clustering of diseases, risk factors, and precursors of diseases in the same individuals.
Concordance Between Life Expectancy and Causes of Death
Concordance between death rates for cardiovascular and noncardiovascular chronic diseases (including cancer) would provide evidence that a common environmental factor, such as habitual diet, might influence both these major causes of death. Discordant death rates would suggest that an environmental variable (e.g., dietary pattern) that promotes one disease might inhibit another and, for example, that dietary contributors to certain cancers and cardiovascular diseases are not the same. Similarly, concordance of diet with diet-related risk factors or disease precursors (e.g., between a diet low in total fat and saturated fat and low serum cholesterol levels or reduced prevalence of colonic polyps, or among energy intake, relative body weight, and blood pressure) would also suggest possible common dietary risk factors for several diseases and, thus, little likelihood of adverse effects from a recommended action, for example, to lower blood cholesterol levels in the population. In contrast, lack of concordance would lead to concerns about increasing the susceptibility of population subgroups to one disease while decreasing the susceptibility to other chronic conditions.
The same logic applies to parallel time trends in incidence or mortality rates and to clustering of several major diseases, risk factors, or high-risk behaviors. For example, it would be important to learn whether people with cardiovascular diseases also often have precursor states for cancer (e.g., bronchial metaplasia).
Similarly, concordance between longer life expectancy and low death rates from cardiovascular diseases and cancer would indicate that effective prevention of one or the other major causes of death has no hidden adverse consequences for the population. In fact, countries having among the lowest death rates from cardiovascular diseases (i.e., Japan and Greece) have substantially greater life expectancy at all ages compared to countries with the highest CHD death rates (i.e., the United Kingdom, Finland, and the United States) (WHO, 1987).
Patterns of Mortality from Major Chronic Diseases
A thorough review of the evidence presented in Chapters 7, 19, and 22 suggests that there is concordance between mortality from heart diseases and certain cancers and that high fat intake is a risk factor for both diseases. Furthermore, dietary fat is not established as a protective factor for any major cause of death or for any of the chronic diseases examined in this report. Cited below are examples (from Chapter 7) indicating that the committee's recommendation to reduce intake of total fat and SFAs should lead to a reduction in the incidence of heart disease as well as certain cancers.
In many countries, correlational data indicate parallel trends in mortality from heart disease and cancers of several sites, including the colon and breast. Sidney and Farquhar (1983) demonstrated a positive ecological correlation (R = .74) between death rates from CHD and colon cancer for 49 countries (Figure 28-3) that reported such data to the World Health Organization. Similarly, T. Thom (National Heart, Lung, and Blood Institute, personal communication, 1989) plotted change in mortality from heart disease, stoke, and cancer in 27 countries from 1970 to 1983 and showed that heart disease, stroke, and total cancer deaths (other than from lung cancer) declined in parallel
Page 691
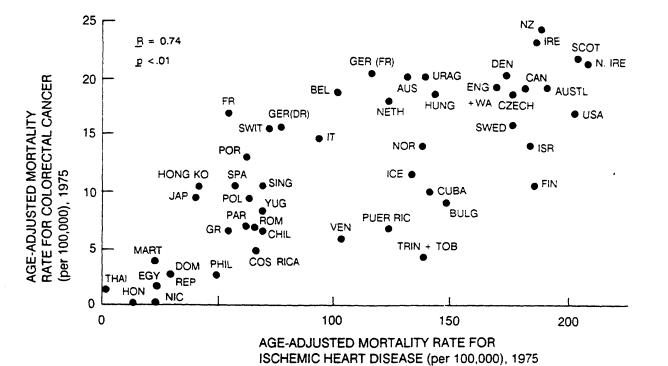
FIGURE 28-3
International comparison of 1975 age-adjusted mortality rates from ischemic heart
disease and colorectal cancer, 49 countries. From Sidney and Farquhar (1983).
in the majority of countries surveyed, also presumably due to some common environmental risk factors.
Comparisons of deaths from heart disease and certain cancers require further consideration, however. For example, the substantial decline in CHD mortality from 1970 to 1983 observed in these 27 countries by T. Thom and the decline in CHD incidence observed in several large cohorts, as well as data from other sources, indicate that improved treatment methods as well as a reduction in risk factors account for these effects. During the same period, however, although mortality from colon cancer has decreased in some countries, its incidence has remained largely unchanged—probably reflecting improved therapy, early diagnosis, or both. If dietary fat exerts a major influence on the risk of both CHD and colon cancer, the lack of concordance in the incidence (but not the mortality) might be due to the long latency period for colon cancer and the finding in several epidemiologic studies that a diet high in total fat (both saturated and unsaturated) rather than saturated fat alone is associated with high colon cancer risk. This interpretation is further supported by dietary survey data (see Chapter 3), which indicate that, although over the last few decades saturated fat intake in the United States has declined substantially, the intake of total fat has remained stable or increased somewhat. Nevertheless, there is no increase in the incidence of colon cancer.
Finally, the U.S. vital statistics (DHHS, 1987) show clear parallels in death rates for all the major chronic diseases for men and women in the United States. Between 1950 and 1978, for example, all major causes of death (heart disease, cerebrovascular disease, and cancers other than lung) declined in parallel, whereas lung cancer death rates rose steeply during that period. This observation is consistent with other evidence suggesting that certain dietary components are common risk factors for several major causes of death but are not the primary risk factors for lung cancer. Although cigarette smoking is a risk factor for many diseases, it is a much more powerful contributor to lung cancer risk than to the risk of other diseases.
Dietary Fat Intake, Serum Cholesterol Levels, and Mortality from Cardiovascular Diseases and Cancer
A major goal of the committee's recommendation to reduce the intake of total fat, SFAs, and dietary cholesterol is to lower the population mean and distribution of serum total and low-density
Page 692
| TABLE 28-6 Studies Not Demonstrating an Inverse Relationship Between Serum Cholesterol and Cancer Mortalitya | ||||||
| Study, Year (Reference) | Number in Study | Age (years) | ||||
| Male | Female | Male | Female | Years Followed | Mean Cholesterol Level of Study Population (mg/dl) | |
| Norwegian workers, 1972 | 3,751 | — | 40-49 | — | 10 | 270 |
| American Heart Association | 8,503 | — | 30-65+ | — | 8.3-12.0 | 235 |
| Chicago Heart Association Detection Project in Industry, 1980 (Dyer et al., 1981) | 6,890 | 5,750 | 45-64 | 45-64 | 5 (average) | 214 |
| Chicago Peoples Gas Study, 1980 (Dyer et al., 1981) | 1,233 | — | 40-59 | — | 18 | 236 |
| Chicago Western Electric Company, 1980 (Dyer et al., 1981) | 1,899 | — | 40-55 | — | 17 | 248 |
| WHO Clofibrate Trial, 1980 (Oliver et al., 1978, 1980) | 10,414 | — | 30-59 | — | 9.6 (average) | Group II: 247 Group III: 181 |
| Yugoslavia Cardiovascular Disease Study, 1980 (Kozarevic et al., 1981) | 11,121 | — | 35-62 | — | 7 | 205 |
| Israel Ischemic Heart Disease Study, 1981(Yaari et al., 1981) | 10,059 | — | 40-64 | — | 7 | 209 |
| a From Sidney and Farquhar (1983). | ||||||
lipoprotein (LDL) cholesterol. In several prospective studies, however, serum cholesterol levels at entry were observed to be inversely related to subsequent risk of colorectal cancer in men (Table 28-5), but this relationship was not found in other studies (Table 28-6) (Sidney and Farquhar, 1983). Subjects in some studies that showed a statistically significant inverse association had intrinsically low blood cholesterol levels, despite their consumption of a relatively high-fat diet. In some studies, the relationship was no longer significant after excluding those who died a short time after entry into the study, i.e., subjects with a low serum total cholesterol presumably due to preclinical cancer. In some other studies, the inverse association disappeared when other risk characteristics were taken into consideration (McMichael and Potter, 1984; Sidney and Farquhar, 1983).
The evidence reviewed in Chapter 7 does not support a causal relationship between low serum cholesterol level and colon cancer. Nevertheless, the committee considered a worst-case estimate of the effect of reducing dietary SFAs and cholesterol and consequently serum cholesterol, using data from 18 years of follow-up in the Framingham study (Williams et al., 1981). A downward shift of 10% in serum cholesterol levels in each category of men was associated with a 6% estimated increase in colorectal cancer incidence. If the men in the Framingham study during the 1960s and 1970s are assumed to be representative of all U.S. men, a serum cholesterol decrease of 10% would mean an additional 2,840 colon cancer cases in addition to 105,000 cases estimated for the United States in 1988 (Silverberg and Lubera, 1988). As noted above, however, this extreme estimate of colon cancer risk is not supported by the detailed review of evidence presented in Chapter 7. Furthermore, as discussed later in this chapter, a conservative estimate of the number of CHD deaths prevented (approximately 100,000) in the population from a 10% reduction in serum cholesterol levels suggests that the net effect of serum cholesterol reduction would be a major benefit.
In fact, many comparisons within and among populations (reviewed in Chapter 7) suggest that reduced intakes of saturated fatty acids and total fat to <10% and <30% of calories, respectively,
Page 693
would lead to a decrease in the incidence of several cancers, including colon cancer. For example, a case-control study by Jain et al. (1980) indicated a population-attributable risk of 42%, suggesting that a notable reduction in colon cancer incidence might result from reducing fat intake to the lowest level found in that study (<30% of calories daily). Even when the hypothetical, and unlikely, adverse effects of a downward shift in serum cholesterol levels are considered, the overall evidence indicates a net reduction in colon cancer rates. Moreover, ecological studies in 20 countries show that per capita intake of total fat and saturated fatty acids is directly correlated with mortality from colon cancer and all cancer sites (Sidney and Farquhar, 1983). Despite their limitations, data from such studies provide no support for a causal relationship between a low-fat diet, low serum cholesterol, and cancer.
Further evidence is provided by Sidney and Farquhar (1983), who plotted the mean total serum cholesterol against cancer mortality in seven countries (Keys, 1980) geographically remote from each other. These data show a highly positive correlation (R = .73) between the average serum cholesterol levels and cancer mortality in the population. Phillips (1975) reported that in Seventh-Day Adventists, who consume vegetarian diets (i.e., low-fat, high-carbohydrate diets), the rates of cardiovascular disease and all cancers, including colon cancer, are low as are their average serum cholesterol levels.
Thus, several lines of evidence indicate that lowering total fat, SFA, and cholesterol intake and a resultant decrease in mean serum cholesterol levels would not increase cancer risk. Other assessments of competing risks, described below, also indicate that reduced intake of total fat, SFAs, and cholesterol is associated with overall reduction in the risk of both cardiovascular diseases and certain cancers.
Commonality in Risk and Protective Factors for Major Chronic Diseases
The literature reviewed in this report provides strong evidence that major diet-related chronic diseases have common environmental causes and thus justify a common approach to prevention. Other evidence comes from the application of risk profiles derived from longitudinal studies of one disease to predict the risk of another. For example, the profile for CHD risk in the Seven Countries Study accurately predicted the long-term risk of stroke, cancer, and all causes of death (Farchi et al., 1987). Such commonality can also be discerned in the protective factors for major diseases. For example, the Alameda County Index of ''seven healthy daily habits" correlated positively with a lower risk of CHD, cancer, and other major causes of death (Breslow and Enstrom, 1980). In the Göteborg Study, several of the same social attributes were related to the risk of mortality from all causes (Wilhelmsen et al., 1986). In the United Kingdom, an inverse gradient was found between social class of civil servants and mortality from CHD and other major causes of death (Marmot et al., 1978). The evidence reviewed in Chapter 14 suggests that a low selenium intake may be a risk factor for heart disease as well as for cancer.
Long-term intervention trials, especially those using dietary modification, also provide evidence of commonality in risk and protective factors for the major causes of death and suggest that the dietary changes recommended by the committee are unlikely to have adverse health effects. In some of the cholesterol-lowering trials, there was a tendency for an increase in mortality from neoplasms in the groups treated with diet and drugs; however, this finding was not confirmed in other trials and was not statistically significant in any trial or when data from all trials were combined (R. Peto, University of Oxford, personal communication, 1987). A few studies noted an increase in the rates of death due to trauma in the treated groups when compared to the control groups. However, a statistical summary of all the trials suggests that although there is a tendency toward increased mortality, there is no real excess of trauma deaths in the treated groups. Furthermore, there is no plausible mechanism to explain why interventions that reduce serum cholesterol levels would increase the risk of trauma. Similarly, in the North Karelia community intervention program involving dietary modification throughout the 1970s, mortality from cardiovascular diseases and cancer tended to decrease in parallel (Tuomilehto et al., 1986).
Low Serum Total Cholesterol and the Risk of Stroke in Hypertensives
As discussed in Chapters 7 and 19, epidemiologic observations in Japan and Honolulu (Reed et al., 1986) and Framingham (Kannel and Wolf, 1983), as well as findings from the large cohort screened in the Multiple Risk Factor Intervention Trial (MRFIT) (Iso et al., 1988), show a consistent pattern of increased deaths from hemorrhagic
Page 694
stroke among hypertensives who have low serum cholesterol values. In contrast, as the ability to distinguish hemorrhagic and thrombotic stroke has improved, a linear, positive relationship has been found consistently between serum total cholesterol and thrombotic stroke risk.
Hemorrhagic stroke risk is concentrated among those with the lowest cholesterol levels, usually below 160 to 170 mg/dl, and the excess risk is largely confined to hypertensive individuals, i.e., those with greater than 90 mm Hg diastolic pressure (Iso et al., 1988). The strength, consistency, and temporal nature of the relationship between serum cholesterol levels and cerebral hemorrhage suggest causality, but no plausible pathophysiological mechanism has been established for such an effect, and confounding factors such as low dietary and plasma protein, high salt intake, alcohol consumption, liver disease, and bleeding disorders have not been ruled out. Even if the association were causal, it would not indicate that reduction of the relatively high serum cholesterol levels in most industrial societies would increase the risk of hemorrhagic stroke in the population. Moreover, it would be possible to identify high-risk people by their combined high blood pressure and low serum cholesterol values and to reduce their risk by controlling their hypertension.
In contrast, the estimated reduction in thrombotic stroke and coronary disease risk in the population from reducing serum cholesterol levels would vastly counterbalance any small (and thus far entirely hypothetical) possibility that the risk of hemorrhagic stroke would be increased. Furthermore, the committee's recommendations to control weight, avoid or moderate alcohol intake, reduce the intake of sodium chloride, and increase potassium intake are likely to reduce the number of hypertensives in the population and, thus, the number of those at increased risk for stroke associated with low serum cholesterol (if in fact low serum cholesterol levels among hypertensives are causally associated with the risk of stroke).
Decreased Saturated Fatty Acid and Cholesterol Consumption
Evidence from epidemiologic, clinical, and metabolic studies reviewed in Chapter 7 indicates that SFA and cholesterol intake are the major dietary determinants of serum total and LDL cholesterol levels in populations and, thereby, of CHD risk. The committee's recommendation to reduce SFA intake to less than 10% of calories along with reducing cholesterol intake is therefore likely to reduce serum cholesterol levels and, consequently, CHD risk in the population. The few epidemiologic studies on dietary fat and cancer that have distinguished among the effects of specific types of fat suggest that reduction of SFA intake to the levels recommended by the committee will also lead to a reduction in the incidence of and mortality from cancers of the colon, prostate, and breast. The committee found no evidence to suggest that the recommended reduction in SFA intake will increase the risk of any other chronic disease.
Increased Polyunsaturated Fatty Acid Consumption
The committee's dietary recommendations would not increase the average intake of PUFAs in the U.S. population (now approximately 7% of calories). Animal studies consistently show an increase in colon or mammary cancers at very high PUFA intake (see Chapter 7). Observations in human populations and in animal experiments in which PUFAs were partially substituted for SFAs suggest that PUFA intake of up to 10% of calories does not increase the population risk of cancer. However, human populations have seldom been observed to increase their PUFA consumption dramatically, and few populations regularly consume high levels (>10% of calories) of PUFAs. Thus, the current U.S. average PUFA intake combined with the committee's recommended decrease in total fat and SFA consumption is likely to lead to an overall decrease in the risk of diet-related cancers.
Increased Monounsaturated Fatty Acid Consumption
The committee's recommendations on saturated, polyunsaturated, and total fats might indirectly result in a relative increase in the consumption of MUFAs. Evidence within populations is not strong but suggests that substitution of MUFAs for SFAs may decrease cancer risk. For example, a case-control study of colorectal cancer showed a lower risk in those with a high intake of olive oil (Macquart-Moulin et al., 1986). Cross-cultural population studies suggest that an increased intake of MUFAs should reduce rates of colorectal cancer when SFA and total fat consumption are also reduced. For example, low colon cancer rates are found in southern Europe where olive oil is a staple but where SFA intake is low in comparison to
Page 695
western or northern Europe (Keys, 1980; Waterhouse et al., 1982).
Increased Carbohydrate Consumption
A substantial amount of data indicates that diets with high levels of plant foods and complex carbohydrates are associated with reduced risk of several chronic diseases, but a positive association between carbohydrate intake and gastric cancer risk reported in two studies (Hakama and Saxen, 1967; Risch et al., 1985) may raise questions about the consequences of increasing carbohydrate intake in the U.S. diet. Since other studies have not found increased gastric cancer risk, it is likely that' the association is attributable to the frequent consumption of such dietary components as salted, pickled, and smoked foods, which is common in some populations on high-carbohydrate diets (Miller, 1982). In contrast, Seventh-Day Adventists, who generally consume high-carbohydrate diets that are low in salted or pickled foods, have a low cancer risk (Phillips, 1975). In the committee's judgment, any hypothetical increase in gastric cancer risk from high complex carbohydrate intake would be substantially less than the overall reduction in risk likely to occur with decreases in fat and nitrite intake and increases in vegetable and vitamin C consumption. The net effect of the committee's recommendations is likely to be a reduction in gastric and colon cancer rates.
Increased Consumption of Vegetables and Other Sources of b-Carotene
The evidence reviewed in Chapter 11 indicates that low consumption of carotenoid-containing foods is consistently associated with a higher risk of several cancers, especially lung cancer, although some evidence suggests an increased risk of prostate cancer in elderly men who consume higher levels of carotenoids. However, prostate cancer risk has been much more consistently associated with high-fat than with high-carotenoid consumption. Nevertheless, the committee does not recommend use of carotene supplements.
Pesticide Residues on Vegetables and Fruits
Increased consumption of vegetables and fruits can be expected to result in increased ingestion of residues of herbicides and pesticides used in agriculture. Therefore, the committee emphasizes the need to wash all raw fruits and vegetables thoroughly. Although some of these chemicals are carcinogenic in animals, there are very few studies pertaining to their carcinogenicity in humans. A few epidemiologic studies of agricultural workers and others exposed to phenoxyacetic acid and herbicides have reported increased risk of non-Hodgkin's lymphoma and possibly soft tissue sarcomas (Hardell et al., 1981; Hoar et al., 1986). Inhalation was the route of exposure in those studies, however, and limited data suggest that no adverse effects result from the ingestion of small amounts of these agents in foods. Furthermore, the potential small increased risk of these somewhat uncommon tumors that might result from increased exposures in the general population would be greatly outweighed by the potential benefits (i.e., reduced risk of cancers of the lung, stomach, colorectum, and other sites and reduced risk of other chronic diseases) to be expected from greater fruit and vegetable consumption. Thus, the committee concluded that the recommendation to consume liberal amounts of fruits and vegetables is appropriate and poses no undue competing risk.
Alcoholic Beverages and Human Health
Would the committee's decision not to recommend alcohol for those who do not drink deprive some people who are at risk of myocardial infarction of any potential benefits of alcohol? The association between moderate alcohol intake and lower CHD risk is consistent, but not strong, and not established as causal. Furthermore, the potential benefits of moderate alcohol intake itself have not been differentiated from the effects of other healthy behaviors generally found among people who control their alcohol intake. The relationship also appears to be independent of the absolute amount of alcohol intake. Even if very moderate alcohol intake were shown to be causally associated with lower CHD risk, the potential benefits of recommending alcohol for nondrinkers would be far outweighed by the well-established health risks and accidents associated with alcohol consumption.
Potential for Nutrient Deficiency or Toxicity
The use of optimal nutrient thresholds offers another approach to assessing public health benefits or risks of dietary modification. What is the impact of the committee's recommendations on
Page 696
the adequacy of nutrient intakes, especially for population subgroups that may be at risk of deficiency or toxicity? The effects of most, if not all, of the dietary factors examined by the committee vary directly and continuously with the level of intake; some relationships are curvilinear. Recommended nutrient thresholds are therefore arbitrary, and arbitrary cutpoints are proposed with the aim of reducing the population risk and facilitating individual choices. They are not true thresholds below or above which benefit or risk is absent or great.
Nutrient requirements vary among individuals. Thus, a recommended range of nutrient intake that meets most people's requirements may exceed a toxic threshold for a few. For example, the recommended intake of iron may lead to iron deficiency anemia in a small segment of the population at one end of the spectrum and hemochromatosis at the other. In general, however, the recommendations take into account the dietary needs of most individuals and are likely to be beneficial to the general population without posing significant risks. For example, could decreased red-meat consumption, which is likely to result from attempts to lower fat intake, lead to decreased iron intake among those vulnerable to iron deficiency (i.e., women in their reproductive years and children)? The committee recommends that fatty meats be replaced with lean meats, poultry (skin removed), fish, and sources of plant protein, such as dried beans. This recommended dietary pattern would continue to furnish adequate sources of heme iron, which is more readily absorbed than inorganic iron in plant foods. The committee also advocates increased consumption of vegetables and fruits (sources of vitamin C), which improve absorption of inorganic iron when consumed at the same time. Furthermore, the relatively low iron intake of women in their reproductive years is due partly to their low caloric intakes; increased energy expenditure through more physical exercise would permit a higher caloric intake without resulting in obesity (if exercise and caloric intake are properly balanced) and would increase the intake of many nutrients, including iron.
The committee's recommendation to balance physical activity and food intake in such a way as to maintain appropriate body weight should not result in nutrient deficiencies, which might occur if caloric intakes were substantially reduced. In fact, increased activity and caloric intake should improve the nutrient quality of the diet, if calories are provided by a variety of nutrient-dense foods.
The committee recommends limiting, not eliminating, egg yolks. Would decreasing the intake of eggs result in a decline in protein intake among children and the elderly? In the 1977-1978 Nationwide Food Consumption Survey (USDA, 1984), the mean percentage of protein intake from eggs was 4% in the adult population in contrast to 3% supplied by nuts, seeds, and legumes as a group. Eggs furnished an average of 4.3% of the protein intake from infancy to 5 years of age and 2.4% for children between the ages of 6 and 8. For men and women 65 to 74 years old, eggs furnished an average of 5 and 4% of the protein intake, respectively. For men and women 75 years and over, they supplied 6 and 4.3%, respectively. A recent survey by the U.S. Department of Agriculture indicated that children 1 to 5 years of age obtained 2.7% of their protein from eggs (USDA, 1987). Therefore, eggs do not appear to be a major protein source for any sex-age group in the U.S. population.
Similarly, decreased salt intake (and consequently decreased iodized salt intake) should not be detrimental to iodine status because the average U.S. diet is considered to be excessively high in iodine content. As discussed in Chapters 3 and 14, a National Research Council committee in 1980 recommended that steps be taken to lower dietary sources of iodine (NRC, 1980a).
The Committee on Diet and Health recommends increased consumption of foods such as whole grains, legumes, vegetables, and fruits—a practice that would increase dietary fiber intake. Is increased dietary fiber intake likely to result in decreased absorption of calcium and other minerals? A recent review indicates that mineral absorption and metabolism are not adversely affected when total dietary fiber, provided by a variety of traditional foods, is as high as 35 g/day (Kelsay, 1986). The committee does not advocate increasing dietary fiber intake by adding purified components of fiber, such as bran or guar gum. Many communities have adapted well to high fiber intakes without apparent detrimental effects on mineral status (Jenkins, 1988). Although continued research on the influence of dietary fiber on mineral absorption is needed, current evidence does not indicate that the general public will experience adverse effects (that might counteract the anticipated beneficial effects) from the kind of diet recommended by the committee.
Page 697
Public Health Impact
(Potential Benefits) of Dietary Recommendations
What would be the impact on public health if the committee's dietary recommendations are fully adopted? Data on diet and disease risk for individuals are appropriate for estimating the effects in the population under certain conditions—when the observations are population-based, extensive, and long term so that population-attributable risk can be calculated; when the congruence of evidence permits a strong inference of causality; and when the observations are reasonably current. These conditions are especially relevant to studies of the relationship between dietary and serum total cholesterol and CHD risk and experimental reduction in serum total cholesterol and subsequent CHD risk. The excess of coronary events attributable to elevated serum cholesterol can be calculated from data on several populations. Moreover, the Hegsted and Keys equations (Hegsted, 1986; Keys, 1984) described in Chapter 7 can be used to predict the downward shift in the population mean and distribution of serum cholesterol that might result from large-scale implementation of the committee's recommendations. The population risk attributable to elevated serum cholesterol could then be used to estimate the number of cases of CHD prevented or the percentage reduction in disease rates.
Lower Serum Cholesterol and Estimated Reduction in CHD Mortality
Amler and Dull (1987) report that the population-attributable risk fraction (PARF) for cardiovascular diseases due to elevated serum total cholesterol levels (>220 mg/dl) is approximately 10% and that reduction of these levels to below 220 mg/ dl could prevent more than 100,000 deaths annually. A widespread reduction in other diet-related risk factors (e.g., reduced blood pressure and improved glucose tolerance in the population in addition to lower serum cholesterol levels) could lead to an even greater reduction in mortality. These rough estimates are based on single-factor correlations within populations that have a high CHD incidence and may underestimate the potential for reducing atherosclerosis and other cardiovascular diseases through relatively modest downward shifts in the population mean and distribution of major risk factors, particularly in the levels of atherogenic serum lipoproteins.
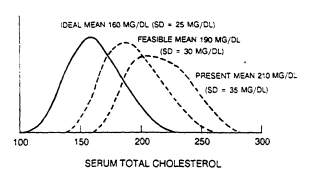
FIGURE 28-4
These idealized smoothed curves portray the present distributions of serum total cholesterol
found in samples of the U.S. population (right); distributions believed to be attainable by
a continuation of current changes in U.S. eating patterns over the next 10 years (middle);
and distributions believed to be ideal for reducing the large population burden of
atherosclerotic cardiovascular diseases (left). These curves also display the phenomena
that skewness and the relative excess of individuals having high values tend to diminish
as the population mean is lowered. From the American Health Foundation (1979).
Figure 28-4 shows three distribution curves for total serum cholesterol—one represents the U.S. adult population during the late 1970s with a mean of 210 mg/dl and is associated with the relatively high CHD mortality of that period; another represents populations with a mean of 160 mg/dl in which the incidence of atherosclerosis is low and CHD is rare; the intermediate curve, with a mean serum cholesterol of approximately 190 mg/dl, represents a feasible reduction of about 10% in average serum cholesterol values for the U.S. adult population (i.e., from the current mean of 210 mg/ dl). This corresponds to distributions found in populations (e.g., in southern Europe) that have substantially lower cardiovascular disease rates than the United States. Thus, a reduction of approximately 10% in mean serum cholesterol levels for the whole population to approximately 190 mg/dl could lead to a large reduction in coronary disease rates (American Health Foundation, 1979). Moreover, populations that have 10 to 20% lower average serum cholesterol levels than the current U.S. average consistently are found to have extremely low rates of CHD. These observations indicate that there is a potential for substantial reduction of atherosclerotic CHD and stroke in the entire population and for a continued favorable downward trend in the United States.
The reduction in all-cause mortality and CHD mortality can be roughly estimated by applying the committee's dietary recommendations for reduced intake of total fat, saturated fatty acids, and cho-
Page 698
lesterol and using 6-year death rates in men from the MRFIT study (Iso et al., 1988). On the basis of the Keys equation (Keys, 1984), one could estimate that the committee's recommendations—i.e., a 4% reduction in calories from saturated fatty acids (from 14 to 10% of calories with no change in PUFA intake) and a reduction in dietary cholesterol from 420 to 300 mg daily (a reduction of 120 mg, or 40 mg/1,000 kcal, assuming an intake of 3,000 calories/day)—may lead to a 20-mg/dl reduction in mean serum cholesterol levels. The reduction in 6-year mortality in MRFIT screenees could then be estimated to be approximately 21% for CHD, approximately 16% for all cardiovascular diseases, and approximately 2% for all deaths. These would be underestimates of the effects of overall dietary modification because they do not consider the independent effects of reducing dietary cholesterol on CHD risk or the effects of reduced salt intake and reduced body weight on hypertension.
Similarly, the proportionate reduction in CHD incidence that would result from a reduction in serum cholesterol can be estimated from the graded risk observed in very-long-term cohort studies, i.e., an approximately 3% reduction in incidence for each 1% difference in the average serum cholesterol level at entry (R. Peto, University of Oxford, personal communication, 1987). Such estimates are reasonable in light of the reduced mean serum cholesterol levels in the population and the decline in coronary deaths documented in the United States over the past 20 years, as well as results of clinical trials among high-risk people.
All these estimates have severe limitations. For example, the data on disease risk are based on the level of risk at entry and relatively short periods of observation. There are no appropriate models for considering postponed rather than prevented events; some people saved from early cardiovascular deaths will surely die from other causes. Also, continuous changes in multiple risk factors affect people of different ages, sex, and cultures in different ways.
Diet-Related Risk Factors and CHD Risk
As suggested above, systematic population data on the decline in diet-related risk factors (e.g., blood cholesterol or blood pressure) and the observed decline in deaths from cardiovascular diseases over the past 20 years in the United States can serve as one basis for estimating the public health impact of a recommended dietary change. Estimates based on such data suggest that a reduction in blood cholesterol alone may have been responsible for approximately 25 to 30% of the overall decline in reported CHD deaths in the United States since 1967 (Byington et al., 1979; Goldman and Cook, 1984). Because the average population blood cholesterol levels are determined predominantly by the composition of the average diet, the approximately 10% reduction in average serum cholesterol levels in the United States since the 1960s is comparable to the change that might be anticipated from large-scale implementation of the committee's recommendations. A further substantial decline in CHD mortality is therefore possible.
Other limitations of these estimates stem from the uncertainties in the cross-sectional data on which they are based, i.e., misclassification of causes of death; failure to consider cohort effects; lack of data on true incidence in the population; lack of systematic, parallel determinations of serum cholesterol data in population samples during the same period as the observed decline in coronary deaths; and confounding due to changes in the levels of other risk factors, especially blood pressure and cigarette smoking.
Variations in Dietary Lipid Profiles and Estimated CHD Risk
Another basis for estimating the effects of dietary change are data from comparative studies of different populations, especially the Seven Countries Study (Keys, 1980), which over 15 years included systematic observations of a wide range of dietary intakes in several countries, some intakes comparable to the current U.S. diet, and others comparable to that now recommended by the committee. In such comparisons, numerous confounding factors may contribute to differences in disease incidence among populations. Nevertheless, in the Seven Countries Study, differences in dietary composition and in average blood cholesterol explained a major part of the population variance in coronary disease rates (Keys, 1980). Without exception, populations consuming the levels of saturated fatty acids recommended by the committee—i.e., <10% of calories—have had little burden of atherosclerotic disease (see Chapter 7). These observations suggest that atherosclerotic diseases could be confined to a much smaller and older segment of the population. Such a projection is also supported by the observed 30 to 50% decline (depending on age, sex, and race) in U.S. coronary death rates in the past 20 years.
Page 699
Dietary Intervention and Estimated Reduction in CHD Risk
Data from intervention trials to lower serum cholesterol by diet alone or by a combination of diet and drugs strongly confirm the long-term observations reported above and reviewed in detail in Chapter 7. These data indicate that CHD incidence is related proportionately to reduced serum cholesterol levels and the duration of exposure to low serum cholesterol levels. They also show a relatively rapid effect on coronary disease risk, i.e., a reduction of risk after approximately 2 years of reduction in blood lipoprotein levels. Moreover, when the data from the cholesterol-lowering trials are taken together, there is no statistically significant excess of neoplastic or all-cause mortality among the treated groups.
Dietary Modification and Potential Reduction in Cancer Risk
As discussed in Chapter 7, there have been few long-term observations and few intervention trials for cancer and other noncardiovascular causes of death. Thus, there is much less certainty about the public health impact of dietary recommendations for reducing risk of these diseases than for reducing risk of CHD. Nonetheless, estimates have been made of the proportion of cancer incidence attributable to diet and, by extrapolation, the potential effect of dietary recommendations in reducing cancer rates. Higginson and Muir (1979) estimated the proportion of cancers related to various environmental factors. They stated that although cancer incidence due to diet could not be precisely estimated, dietary factors are among the general "lifestyle" factors estimated to be responsible for approximately 90% of all cancers. Wynder and Gori (1977) were more specific. On the basis of international and national comparisons of cancer incidence, reported differences between U.S. mortality rates and the lowest reported worldwide mortality rates for each cancer site, and results of case-control studies, they concluded that a little more than 40% of cancers in men and almost 60% of cancers in women in the United States could be attributed to dietary factors.
Using a similar approach, Doll and Peto (1981) were somewhat more cautious. They agreed that a substantial proportion of cancers in both sexes in the United States was likely to be attributable to dietary factors, but from a survey of the literature, they provided a wide range of estimates (i.e., 10 to 70%) for the proportion of cancer deaths that could be reduced by practical dietary means. They stated that it might not be possible to achieve a large reduction in the near future but suggested that dietary modifications might eventually result in a 35% reduction of cancer deaths in the United States. This reduction was estimated to include a 90% reduction in deaths from cancers of the stomach and large bowel; a 50% reduction in deaths from cancers of the endometrium, gallbladder, pancreas, and breast; a 20% reduction. in deaths from cancers of the lung, larynx, bladder, cervix, mouth, pharynx, and esophagus; and a 10% reduction in deaths from cancer at other sites. These investigators placed a greater degree of confidence in the projected 35% reduction in overall mortality than in the estimated contribution of diet to specific cancer sites. More recently, the National Cancer Institute's Committee on Prevention suggested that of NCI's goal of a 50% reduction in cancer mortality, about 8% might be achieved by dietary modification (Greenwald and Sondik, 1986).
Two case-control studies of dietary factors and cancer in Canada, which were based on reasonably representative population controls, enabled the authors to estimate the proportion of the cancers that might be attributable to dietary factors. One of the studies pertained to breast cancer and showed a weak positive association with total dietary fat. On the basis of those data, Miller (1978) estimated that 27% of the breast cancer risk for these women might be attributable to total dietary fat intake. The second study showed a moderately increased risk for colorectal cancer associated with a high saturated fatty acid intake in both men and women. On the basis of those data, Jain et al. (1980) estimated that 41% of the risk for males and 44% of the risk for females might be attributable to saturated fatty acid intake. Both estimates, which were based on the observed degrees of association in these representative studies, may be low because artifacts in the dietary data tend to lead to low estimates of relative risk (Marshall et al., 1981). This is particularly true for breast cancer, because estimated effects of dietary factors based on current intake are likely to be substantially below the true effect for a factor that is operational earlier in life, possibly during adolescence.
Amler and Dull (1987) estimated that a 20% reduction in both colon cancer and breast cancer rates could result from changes in the habitual diet; they considered this to be a conservative estimate.
Page 700
| TABLE 28-7 Health Impact of Major Cancers Associated with Dietary and Other Interventions in the United States in 1980a | |||
| Cancer Sites | Risk Factor | Total Number of | Number of Cancer Deaths in 1980 Attributed to the Risk Factorc |
| Lung | Smoking (75.9) | 67,140 | 50,959 |
| Occupation (12) | 10,615 | 1,274 | |
| Colon and Rectum | Diet (20) | 11,444 | 2,289 |
| Breast | Diet (20) | 7,504 | 1,501 |
| Pancreas | Smoking (25.8) | 5,931 | 1,530 |
| Bladder | Smoking (39.0 M) | ||
| (16.4 F) | 4,347 | d | |
| Occupation (23) | 2,530 | 582 | |
| Larynx | Smoking (74) | 2,552 | 1,888 |
| Alcohol (16.9) | 583 | 99 | |
| Cervix | Smoking (24.1) | 1,320 | 318 |
| Total | 113,966 | ||
| % of all cancers | 28 | ||
| a Adapted from Amler and Dull (1987). | |||
| b AR = attributable risk. | |||
| c Number of attributable deaths in 1980 = attributable risk (as a percentage) x total number of cancer deaths in 1980. | |||
| d Cannot calculate using combined male and female deaths. | |||
Table 28-7 provides estimates (column 2), by cancer site, of the percentage of total risk attributable to major risk factors. Multiplying these attributable risks by the total number of 1980 cancer deaths (column 3) gives the number of cancer deaths for each site (column 4) attributable to each risk factor. Although attributable risk estimates are only approximate, Table 28-7 suggests that dietary recommendations similar to those of the Committee on Diet and Health could prevent more than 2,000 deaths from colorectal cancer and approximately 1,500 from breast cancer annually. These calculations also probably underestimate the real potential of dietary change, because these apparently diet-related tumors are very rare in some populations.
All these estimates about the extent of cancer attributable to diet should be interpreted cautiously, since they are based on data that are subject to considerable error and require making a number of assumptions about which opinions might reasonably differ.
Overview and Summary of Risks and Benefits of Dietary Modification
In summary, the committee used several approaches and various lines of evidence to assess possible adverse consequences of its dietary recommendations for the general population. For example, it examined the degree of concordance in death rates and mortality trends among the major diet-related causes of death (i.e., coronary heart disease and cancers) to determine the commonality in dietary risk factors and protective characteristics. It also analyzed the possible consequences of reducing the intake of total fat, SFAs, and cholesterol—actions that would reduce serum cholesterol and CHD risk but that in some studies are also associated with increased risk of colon cancer mortality. Furthermore, it considered the effect of reducing serum total cholesterol in the population on the risk of hemorrhagic stroke in hypertensives, the possible adverse effects of increased PUFA or MUFA intake, increased carbohydrate intake, increased intake of vegetables and carotene, possible increased exposure to pesticides, moderate alcohol intake versus avoidance, and the potential for nutrient deficiency or toxicity among population subgroups. Using worst-case scenarios, the committee concluded that the potential for adverse effects (e.g., increased colon cancer risk due to a reduction in the population mean for serum total cholesterol) is minimal at best and is far outweighed by the many potential benefits. Various lines of evidence indicate that risk factors and protective factors for the major diet-related chronic diseases and causes of death run in parallel and that,
Page 701
in general, dietary intervention to reduce the risk of one disease (e.g., CHD) is likely also to reduce the risk of other diseases (e.g., several cancers).
Central to the committee's deliberations was the extent to which the overall risk of chronic diseases in the U.S. population might be reduced by dietary modification. Because the extent to which dietary factors are involved in the etiology of different chronic diseases varies considerably (see Chapter 27), the impact of dietary modification on the risk of different diseases will also vary.
The committee used several approaches for developing quantitative estimates of the expected public health impact if its dietary recommendations were to be fully adopted by the public. The accuracy of such an estimate is determined by the availability of strong, consistent, and congruent evidence from a variety of sources, especially from extensive, long-term observations of dietary interventions in human populations. Such data are most extensive for serum cholesterol levels and the risk of CHD and much less extensive for dietary factors and CHD, cancer, and other major causes of death.
Estimates for the reduction in CHD risk were derived by extrapolating the effects of a downward shift in average serum cholesterol levels, by comparing CHD risk in populations with substantially different diets and mean serum cholesterol levels, and by examining the results of cholesterol-lowering trials on cardiovascular disease incidence. There are many drawbacks to using any of these approaches, as explained above. Taken together, however, these approaches strongly suggest that following the committee's recommendations for reducing intake of SFAs, cholesterol, and total fats and a consequent modest (at least 10%) reduction in serum cholesterol levels should lead to at least a 20% reduction in CHD risk in the United States beyond the 1987 levels. More stringent dietary modification provides the potential for even greater reduction in coronary disease in the future. This underestimates the benefits of dietary modification because it only focuses on certain lipids and does not take into account the potential benefits of reductions in body weight and blood pressure in the population.
The picture is less clear for the risk of cancer. The committee's conclusions are generally in agreement with those of the National Research Council's Committee on Diet, Nutrition, and Cancer, which in 1982 concluded that cancers of most major sites are influenced by dietary patterns (NRC, 1982). The data are not sufficient, however, to quantitate the contribution of diet to overall cancer risk or to determine the quantitative reduction in risk that might be achieved by dietary modifications. The committee notes that several countries (e.g., Mediterranean countries) with dietary patterns similar to those recommended here have about half the U.S. rates for diet-associated cancers (see Chapter 22). This suggests that the committee's dietary recommendations could also have a substantial impact on reducing the risk of cancers in the United States.
For the other chronic diseases and conditions considered in this report (i.e., hypertension, obesity, osteoporosis, diabetes mellitus, hepatobiliary disease, and dental caries), the magnitude of risk reduction expected through full implementation of the committee's guidelines on diet and health cannot be reliably estimated due to limitations in the data. Nevertheless, the committee concluded that implementation of its dietary recommendations through readily available natural diets is likely to result in considerable reductions in the overall risk of these chronic diseases without a discernible increase in the risk of any cause of death or disability.
The committee also categorized dietary factors according to the strength of the evidence relating each to the risk of chronic diseases and the potential public health impact of dietary modification. In the committee's judgment, modification of the total diet along the lines of its recommendations is necessary to achieve the maximum public health benefit, and among dietary factors, modifications in the intake of total fat, SFAs, and dietary cholesterol are likely to have the greatest impact.
Implementation of Dietary Recommendations
What strategies are needed to implement the committee's dietary recommendations, and what are their implications for society? These questions are the subject of a separate study by the Food and Nutrition Board. Therefore, these issues are considered only briefly in this report.
As summarized in Tables 28-1 through 28-4, a comparison of dietary guidelines from diverse, authoritative sources in the United States and abroad suggests that scientists and public health agencies now widely agree on general nutrition principles to promote good health, but the best way to implement these principles has not been determined. It is apparent to the committee and the Food and Nutrition Board that if one of our
Page 702
national goals is to reduce the risk of chronic diseases and if dietary modification is likely to assist in achieving that goal, then various sectors of society need to collaborate in implementing dietary recommendations. The committee is aware that a number of efforts to implement dietary recommendations are already under way both within and outside the U.S. government. The U.S. Department of Health and Human Services, for example, has developed implementation plans to coincide with 17 priority objectives for improving nutrition during the decade 1980 to 1990. These plans include measures to improve health, reduce risk factors, increase public and professional changes in the macronutrient composition of the awareness, and improve services and surveillance(DHHS, 1983), and many of them are consistent with implementing dietary changes. Voluntary health organizations, health professionals, and the food industry are also taking actions that pertain to implementation of nutrition policies. Nevertheless, the committee wishes to draw special attention to the following general issues pertaining to implementation.
A concerted effort will be needed to make changes in the food supply and in nutrition policy average U.S. diet. and programs to increase the availability of low- fat, low-saturated fat, and low-salt foods in super- markets and in public eating facilities such as school cafeterias and restaurants. Consideration may need to be given to the most effective means of achieving such modification: through technological changes, massive public education efforts, legislative measures such as food labeling, or a combination of such strategies. Although the committee's report to the public, which will follow this report, will explain its major conclusions and recommendations in lay terms, leaders in government agencies, the health professions, the food industry, and the mass media face the challenge of interpreting the committee's nine dietary recommendations for the general public and their implications for high-risk groups. They will need to convey in practical terms the concept of certainty or uncertainty of benefit, competing risks, dietary interactions, and target populations. There is a need to develop adequate educational tools and to identify the best means of educating and motivating the public. Health professionals, government agencies, and the food and agriculture industries must also undertake additional research to identify ways of effecting dietary change.
Health professionals specifically need to under- take more definitive research to determine the suitability of traditional nutrition education tools such as the Basic Four Food Guide (Page and Phipard, 1957) for use with the current recommendations and to consider new food guidance systems, such as the ones discussed by Cronin et al. (1987), that take into account the proposed The food industry has traditionally exerted a major influence on eating patterns. Although producers of meat, poultry, fats, and oils have in the past taken issue with certain dietary recommendations, they have been increasingly responsive to dietary guidance. For example, there is an increasingly wide variety of diet menus in restaurants (Burros, 1985), and the food industry has undertaken research that attempts to implement current recommendations (e.g., the production of leaner animals) and has voluntarily adopted measures to control additives and contaminants of concern. The challenge to the private sector now is to undertake more scientifically based advertising, to develop suitable educational materials, and to make more nutritionally desirable and affordable foods more widely available in grocery stores, restaurants, hospitals, and other public eating facilities.
Food marketing research suggests that the public is now better informed and more intensely interested in matters pertaining to diet, chronic diseases, and health and that it actively seeks nutrition guidance (Jones and Weimer, 1981; Louis Harris & Associates, Inc., 1978, 1979; Mark Clements Research, Inc., 1980). However, food marketing surveys also demonstrate that the general public does not necessarily apply the advice it seeks. The multiple forces that compete for the public's attention in the marketplace and the absence of criteria for separating fact from fallacy underscore the need for a coordinated approach to implementing dietary recommendations—a strategy that involves cooperation among government agencies, professionals, and the private sector.
It is apparent to the Food and Nutrition Board and its Committee on Diet and Health that many actions within and outside the federal government directly or indirectly influence the development and implementation of dietary recommendations. However, these actions appear fragmented, often pertain to a single disease or a single dietary recommendation, and are not necessarily consistent. Furthermore, their effectiveness is unclear. In view of these concerns, another Food and Nutrition Board committee is developing a strategy for implementing the dietary recommendations proposed in this report.
Page 703
The committee is confident that it is feasible to implement its recommendations within the framework of the current U.S. lifestyle, and it is encouraged by knowledge that dietary habits in the United States already have changed markedly—in many ways that are consistent with current recommendations. Thus, it seeks the collaboration of government agencies, the food industry, health professionals (physicians, nutritionists, dietitians, and public health personnel), educational institutions, leaders in mass media, and the general public in interpreting and implementing the proposed dietary modifications.
Research Directions
Fundamental scientific discoveries generally occur in completely unexpected ways. Thus it is impossible to predict where the major discoveries will be made or which research directions will prove to be the most fruitful. Therefore, the committee does not wish to stifle creativity by specifying experimental protocols or directing research. Nevertheless, it is possible and desirable to propose a scheme for organizing research to seek more definitive data on the associations between diet and chronic diseases. The committee's conclusions and dietary recommendations reflect its assessment of current knowledge and actions justified now; they can be made more definitive only through additional research of the kind recommended below.
The seven categories of research proposed below are not presented in order of priority. Rather, taken together, they reflect a conceptual framework for interdisciplinary collaborative research that encompasses different kinds of investigations: short- and long-term experiments in vitro and in vivo, food consumption surveys, food composition analyses, descriptive and analytical epidemiologic studies, metabolic studies and clinical trials in humans, and social and behavioral research. More detailed and specific research recommendations are summarized in Chapters 4 and 6 through 26.
Identification of Foods and Dietary Components That Alter the Risk of Chronic Diseases
and Elucidation of Their Mechanisms of Action
Much needed research falls in this category. Many dietary constituents are already known to play a role in the etiology of chronic diseases, but additional and more specific knowledge, especially concerning mechanisms of action, will lead to more definitive conclusions and provide more precise guidance about the ways to reduce the risk of different chronic diseases.
With regard to macroconstituents, the committee recommends that additional research focus on the following issues.
· Separating the effects of energy intake per se from those of specific sources of calories, e.g., fats, on disease risk, especially the risk of certain cancers, obesity, and noninsulin-dependent diabetes mellitus (NIDDM).
· The effects of increasing the proportion of carbohydrates in the diet on CHD morbidity and mortality among individuals with diabetes.
· The mechanism for regional fat accumulation, the feedback signals for regulation of fat stores, the means to modify body fat distribution, and the relative risks associated with regional fat deposits.
· The role of postprandial lipoproteins and their remnants in atherogenesis and in the risk of coronary heart disease and their relationship to dietary fat intakes.
· The nature and the regulation (including regulation by dietary intake) of heterogeneity within each major class of lipoproteins and the role of different lipoprotein subclasses in atherosclerosis and CHD.
· The major dietary determinants of plasma HDL and the role of HDL in preventing coronary heart disease.
· The mechanism whereby the type and amount of dietary fat influence different stages of carcinogenesis, e.g., PUFA (omega-3 and omega-6) and cancer risk, or MUFA intake and breast cancer risk.
· The relative importance of different types of proteins (animal and vegetable) compared to different types and amounts of fats in chronic disease etiology and their mechanisms of action (e.g., in coronary heart disease, different cancers, hypertension, and stroke).
· The relative effects of different types and amounts of fibers in chronic disease etiology and the mechanisms whereby they may affect serum lipid levels, CHD, different cancers, NIDDM, and gallstones.
· The influence of dietary factors other than fats on serum lipids, the atherosclerotic process, and cardiovascular diseases.
· The nutritional, environmental, behavioral, and genetic factors in the etiology of obesity associated with NIDDM.
Page 704
· The potential link between the intake of total carbohydrates, different types of carbohydrates, and stomach cancer.
· Further identification of eating patterns that are protective against dental caries and the contributory role of sugars in the pathogenesis of caries versus the effect of fluoride in caries prevention.
· The mechanisms whereby chronic alcohol ingestion increases the risk of hypertension and possibly that of breast cancer.
With regard to research directions for foods and their microconstituents, the committee wishes to draw attention to the following topics.
· Further identification of the constituents in plant foods (vegetables, whole-grain products, and citrus fruits) that may modify the risk of different chronic diseases and elucidation of their mechanisms of action.
· The specific dietary and other environmental factors associated with vegetarian lifestyles and their relative contribution to the overall maintenance of health and reduction of the risk of specific chronic diseases.
· The mechanisms whereby various ions (e.g., sodium, potassium, chloride, and possibly calcium) affect blood pressure.
· The potential role of specific B vitamins in carcinogenesis and of carotenoids as potential chemopreventive agents for specific neoplasms.
· The mechanism whereby vitamin E deficiency combined with a high PUFA intake may enhance carcinogenesis.
· The mechanisms, other than nitrosamine-inhibition, whereby vitamin C may influence carcinogenesis and the specific effects of vitamin C versus those of other substances in plant foods that are associated with a lower cancer risk.
· The potential role of calcium and vitamin D in the etiology and prevention of osteoporosis.
· The relative role of different types of coffee and constituents of coffee and tea in altering cancer risk and in affecting serum cholesterol levels and heart disease risk.
· Further identification of nutritive and nonnutritive dietary constituents that may cause, or protect against, various chronic diseases.
· Evaluation of the carcinogenic potential of suspect carcinogens in common foods, e.g., certain mycotoxins, polycyclic aromatic hydrocarbons, and naturally occurring constituents such as flavonoids.
· The effect of diet on the endogenous formation of mutagens, such as nitrosamines and fecal and urinary mutagens, and the carcinogenicity of such mutagens.
Improvement of the Methodology for Collecting and Assessing Data on the Exposure of Humans to Foods
and Dietary Constituents That May Alter the Risk of Chronic Diseases
Methodological shortcomings limit the interpretation of data and often prevent the derivation of precise conclusions about the association of diet and chronic diseases. Thus, the committee recommends that high priority be given to the following types of research.
· Development of better methods to monitor and quantify dietary exposures in human populations. This includes improvement in food composition data for both nutritive and nonnutritive substances (especially fiber and microconstituents), methods for more frequent and long-term monitoring of dietary intake, and better methods to quantify dietary intake, especially for energy and alcohol. In particular, the methodology of USDA's Nationwide Food Consumption Surveys and the National Center for Health Statistics' Health and Nutrition Examination Surveys should be improved to permit assessment of the long-term health effects of dietary factors, both nutritive and nonnutritive.
· Development of better methods for data analysis from epidemiologic studies, for example, statistical methods that take into account collinearity and multiple interactions among dietary variables and that permit simultaneous analysis of the association between specific foods, food classes and food constituents, and disease end points.
· Additional techniques for assessing the mutagenic effects of chemicals on human cells in vivo and application of such techniques to assess mutagenicity of diets that are believed to present a high or a low risk for cancer.
Identification of Markers of Exposure and Early Indicators of the Risk of Various Chronic Diseases
This category of research is designated for two purposes: first, to circumvent the shortcomings of using the disease itself as the sole end point, i.e., because of the long latency period of many chronic diseases, evidenced by the delay between dietary exposure and disease expression; and second, to circumvent problems of exposure misclassification
Page 705
when dietary recall methods are used. In the committee's judgment, there is a pressing need to identify biochemical/biological markers of dietary exposure, early biological markers that can forecast the emergence of clinical disease, and genetic markers that can identify high-risk subgroups in the population. In addition, the committee proposes further use of molecular biology techniques to study gene-nutrient interactions that can help characterize individual variability in nutrient requirements and susceptibility to various chronic diseases. The following are examples of specific topics that deserve attention.
· Additional and better biochemical markers of exposure to dietary fats and early biological markers of neoplasia.
· Genetic control of response to dietary fats, the interaction of genetic factors and dietary fats, and their impact on specific chronic diseases, especially cardiovascular diseases, cancer, and gallbladder disease.
· The role of gene-nutrient interactions in the etiology of NIDDM, alcohol dependence, hypertension, osteoporosis, certain cancers, food intake and obesity, and dental caries.
· Simpler methods for identifying high-risk groups.
Quantification of the Adverse and Beneficial Effects of Diet and Determination of the Optimal Ranges
of Intake of Dietary Macro- and Microconstituents That Affect the Risk of Chronic Diseases
Although most dietary constituents are known to have some effect on the risk of certain chronic diseases, much less is known about the magnitude of this effect. The committee believes that there is a strong need to quantify these effects in order to estimate the contribution of diet to the risk of chronic diseases. These efforts should include a study of nutrient interactions, competing risks, and dose-response relationships. The ultimate aim of such research should be to determine the optimal ranges of intake of various dietary components for health maintenance, keeping in mind the desirability of identifying their effects and the shape of the dose-response curve. The following are examples of specific areas that deserve attention.
· More discriminating data on the effect of the type and amount of fat on the risk of cardiovascular diseases and cancers of the breast, colon, and prostate and on the levels of fat intake associated with the maximum risk reduction. Special attention is needed to determine the effects on cancer and cardiovascular disease risk of very high intakes of polyunsaturated fats (e.g., of the kind found in fish oils) and to determine the optimal proportion of polyunsaturated, monounsaturated, and saturated fatty acids in the diet.
· The optimal range of protein intake by identifying the effects of the amounts and types of protein on chronic diseases including atherosclerosis, certain cancers, hypertension and stroke, and osteoporosis.
· The long-term effects of excessive protein intake on renal function in humans and its relationship to the risk of end-stage renal disease.
· The role of specific amino acids or combinations of amino acids in augmenting chronic disease risk.
· The nature of interaction between protein and different carcinogens in experimentally induced carcinogenesis.
· The long-term effects of increasing the proportion of complex carbohydrates (starches and fibers) in the diet on the risk of, and biochemical markers for, several diseases, especially stomach and pancreatic cancers, NIDDM, and atherosclerotic cardiovascular diseases, and the specific roles of individual fibers in disease onset.
· The potential beneficial or adverse effects of mild to moderate alcohol consumption on coronary heart disease risk.
· The optimal range of intake of water-soluble vitamins for prevention of chronic diseases, especially cancer and liver disease at all stages of the life cycle.
· Dose-response curves for trace elements with the potential for reducing chronic disease risk (e.g., selenium and copper).
· Interactions among nutrients or among nutrients and other environmental risk factors at ranges of exposure that have the potential for modifying chronic disease risk. These would include interactions of physical activity, fat intake, and obesity; alcohol and vitamin A or alcohol and the B vitamins and cancer; fiber and micronutrients such as calcium, zinc, or vitamin C and various diseases; vitamin E, polyunsaturated fatty acids, and CHD; vitamin E, selenium, and cancer; sodium, potassium, and their anions, alcohol, lipids, proteins, and hypertension, or dietary electrolytes and calcium and hypertension; fluoride, the spectrum of carbohydrate intake, and dental caries; diet, phys-
Page 706
ical fitness, and blood pressure; and synergistic and antagonistic interactions among food additives, contaminants, nutrients, and cancer risk.
Through Intervention Studies, Assessment of the Potential for Chronic Disease Risk Reduction
Carefully designed intervention studies should be conducted to assess the public health impact of dietary modification. Although many such studies have been conducted for heart disease, hypertension, dental caries, and obesity, and a few have focused on osteoporosis, no such long-term studies have yet been completed for cancer. The committee has considered whether priority should be given to large-scale trials or whether current knowledge is sufficient to undertake interventions in the population and subsequently to assess their effectiveness by careful monitoring of trends in disease incidence and mortality.
Intervention trials should be undertaken only when a substantial body of data indicates a high likelihood of benefit without discernible risk. A few such trials (e.g., fat-reduction for breast cancer risk; a trial to examine multiple risk factors to test multiple disease end points; a trial with sodium restriction, potassium supplementation, and weight control for hypertension; b-carotene supplements for the risk of cancers of the lung, gastrointestinal tract, and cervix; increased dietary fiber for the risk of colon cancer; and especially trials that can simultaneously measure the impact of dietary modification on multiple disease end points) might be justified to obtain more definitive data, but they should not be used as a basis for delaying prudent dietary modifications warranted by current knowledge. Any intervention studies should be accompanied by effective monitoring to assess disease incidence, prevalence, and mortality rates.
Application of Knowledge About Diet and Chronic Diseases to Public Health Programs
Social and behavioral research should be undertaken to achieve a better understanding of factors that motivate people to modify their food habits. This knowledge is indispensable for designing effective public health programs to reduce the risk of chronic diseases. Furthermore, improved technologies are needed to enhance the availability of foods that conform to the committee's dietary recommendations. Examples of the type of research are listed below.
· Comparisons of the behavior and motivations of people who have changed their food habits with those who have not.
· Natural history of dietary change in humans to identify periods of vulnerability to change in eating habits.
· Methods for reducing obesity and maintaining weight loss.
· Methods for controlling alcohol abuse and alcohol dependence.
· Methods for monitoring and evaluating the impact of dietary recommendations on chronic disease risk.
· Ethnic and cultural differences in response to dietary modification and means of incorporating these differences in strategies for risk reduction.
· Animal husbandry and food technology research to produce leaner animals, plant foods with less pesticide or toxic chemical residues, and a greater variety of processed foods with less fat, modified fatty acid composition, less salt, more complex carbohydrates, and less refined sugars.
Expansion of Basic Research in Molecular and Cellular Nutrition
The six categories described above focus on research to enhance knowledge of the interrelationship among dietary factors, chronic diseases, and health, and this research includes an understanding of the underlying mechanisms. The committee emphasizes the need for such fundamental research to further advance our knowledge of basic cellular and molecular mechanisms. Research in disciplines ranging from the physical sciences to biochemistry, physiology, applied biology, nutrition, medicine, epidemiology, biophysics, cellular and molecular biology, and genetics is needed to fill the gaps in our understanding of how dietary, environmental, and genetic factors interact to influence the risk of chronic diseases.
References
AAP (American Academy of Pediatrics). 1983. Toward a prudent diet for children. Pediatrics 71:78-80.
ACS (American Cancer Society). 1984. Nutrition and Cancer: Cause and Prevention. American Cancer Society Special Report. American Cancer Society, New York. 10 pp.
ADA (American Dietetic Association). 1986. The American Dietetic Association's nutrition recommendations for women. J. Am. Diet. Assoc. 86:1663-1664.
Page 707
ADA (American Dietetic Association). 1987. Recommendations concerning supplement usage: ADA statement. J. Am. Diet. Assoc. 87:1342-1343.
Ad Hoc Working Group on Coronary Prevention. 1982. Prevention of coronary heart disease in the United Kingdom. Lancet 1:846-847.
AHA (American Heart Association). 1982. Rationale of the diet-heart statement of the American Heart Association: Report of Nutrition Committee. Circulation 65: 839A-854A.
AHA (American Heart Association). 1983. Diet in the healthy child: task force committee of the Nutrition Committee and the cardiovascular disease in the young council of the American Heart Association. Circulation 67: 1411A-1414A.
AHA (American Heart Association). 1986. Dietary guidelines for healthy American adults: a statement for physicians and health professionals by the Nutrition Committee, American Heart Association. Circulation 74:1465A-1468A.
AHA (American Heart Association). 1988. Dietary guidelines for healthy American adults: a statement for physicians and health professionals by the Nutrition Committee, American Heart Association. Circulation 77:721A-724A.
American Diabetes Association. 1987. Nutritional recommendations and principles for individuals with diabetes mellitus: 1986. Diabetes Care 10:126-132.
American Health Foundation. 1972. Position statement on diet and coronary heart disease. Prev. Med. 1:255-286.
American Health Foundation. 1979. Conference on the health effects of blood lipids: optimal distributions for populations. Prev. Med. 8:580-759.
American Health Foundation. 1983. Summary and recommendations of the conference on blood lipids in children: optimal levels for early prevention of coronary artery disease. Prev. Med. 12:728-740.
Amler, R.W., and H.B. Dull, eds. 1987. Closing the Gap: The Burden of Unnecessary Illness. Oxford University Press, New York. 210 pp.
Beaglehole, R., M.A. Foulkes, I.A.M. Prior, and E.F. Eyles. 1980. Cholesterol and mortality in New Zealand Maoris. Br. Med. J. 280:285-287.
Blackburn, H., and D. Jacobs. 1984. Sources of the diet-heart controversy: confusion over population versus individual correlations. Circulation 70:775-780.
Breslow, L., and J.E. Enstrom. 1980. Persistence of health habits and their relationship to mortality. Prev. Med. 9: 469-483.
Burros, M. 1985. Dining choices for healthier food. New York Times, May 11, p. 52.
Byington, R., A.R. Dyer, D. Garside, K. Liu, D. Moss, J. Stamler, and Y. Tsong. 1979. Recent trends of major coronary risk factors and CHD mortality in the United States and other industrialized countries. Pp. 340-380 in R.J. Havlik, M. Feinleib, T. Thom, B. Krames, A.R. Sharrett, and R. Garrison, eds. Proceedings of the Conference on the Decline in Coronary Heart Disease Mortality. DHEW Publ. No. (NIH) 79-1610. National Heart, Lung, and Blood Institute, National Institutes of Health, Public Health Service, Department of Health, Education, and Welfare, Bethesda, Md.
Callaway, C.W., K.W. McNutt, R.S. Rivlin, A.C. Ross, H.H. Sandstead, and A.P. Simopoulos. 1987. Statement on vitamin and mineral supplements. The Joint Public Information Committee of the American Institute of Nutrition and the American Society for Clinical Nutrition. J. Nutr. 117:1649.
Cambien, F., P. Ducimetiere, and J. Richard. 1980. Total serum cholesterol and cancer mortality in a middle-aged male population. Am. J. Epidemiol. 112:388-394.
Canadian Cancer Society. 1985. Facts on Cancer & Diet: Your Food Choices May Help You Reduce Your Cancer Risk. Canadian Cancer Society, Toronto. 23 pp.
Canadian Consensus Conference on Cholesterol. 1988. Preliminary Report. A Conference on the Prevention of Heart and Vascular Disease Through Altering Serum Lipids and Lipoprotein Risk Factors, March 9-11, 1988. Government Conference Centre, Ottawa, Ontario, Canada. 16 pp.
Castelli, W.P. 1979. How many drinks a day? J. Am. Med. Assoc. 242:2000.
Commonwealth Department of Health/National Health and Medical Research Council. 1983. Nutrition Policy Statements. C.J. Thompson, Commonwealth Government Printer, Canberra, Australia. 39 pp.
Council on Scientific Affairs. 1979. American Medical Association concepts of nutrition and health. J. Am. Med. Assoc. 242:2335-2338.
Council on Scientific Affairs. 1987. Vitamin preparations as dietary supplements and as therapeutic agents. J. Am. Med. Assoc. 257:1929-1936.
Cronin, F.J., A.M. Shaw, S.M. Krebs-Smith, P.M. Marsland, and L. Light. 1987. Developing a food guidance system to implement the dietary guidelines. J. Nutr. Educ. 19:281-302.
Department of Health, Ireland. 1984. Guidelines for Preparing Information and Advice to the General Public on Healthy Eating. Food Advisory Committee, Department of Health, Dublin, Ireland. 26 pp.
Department of National Health and Welfare, Canada. 1977. Recommendations for Prevention Programs in Relation to Nutrition and Cardiovascular Disease. Report of the Committee on Diet and Cardiovascular Diseases, Bureau of Nutritional Sciences, Health Protection Branch, Ottawa, Ontario, Canada. 46 pp.
Department of National Health and Welfare, Canada. 1982. Canada's Food Guide Handbook (revised). Report of the Committee on Diet and Cardiovascular Diseases. Ottawa Supply and Services, Ottawa, Ontario, Canada. 52 pp.
DHEW (U.S. Department of Health, Education, and Welfare). 1979. Healthy People: the Surgeon General's Report on Health Promotion and Disease Prevention. DHEW (PHS) Publ. No. 79-55071. Office of the Assistant Secretary for Health and Surgeon General, Public Health Service, U.S. Department of Health, Education, and Welfare. U.S. Government Printing Office, Washington, D.C. 177 pp.
DHHS (U.S. Department of Health and Human Services). 1983. Public health service implementation plans for attaining the objectives for the nation: improved nutrition, summary of the problem. Public Health Reports 98:132-155.
DHHS (U.S. Department of Health and Human Services). 1986. The 1990 Health Objectives for the Nation: A Midcourse Review. Office of Disease Prevention and Health Promotion, Public Health Service. U.S. Government Printing Office, Washington, D.C. 253 pp.
DHHS (U.S. Department of Health and Human Services). 1987. Monthly Vital Statistics Report, Vol. 36: The Advance Report of Final Mortality Statistics, 1985. DHHS Publ. No. (PHS) 87-1120. National Center for Health
Page 708
Statistics, Public Health Service, U.S. Department of Health and Human Services, Hyattsville, Md. 48 pp.
DHHS (U.S. Department of Health and Human Services). 1988. The Surgeon General's Report on Nutrition and Health. DHHS (PHS) Publ. No. 88-50210. Public Health Service, U.S. Department of Health and Human Services. U.S. Government Printing Office, Washington, D.C. 712 pp.
DHSS (Department of Health and Social Security). 1984. Diet and Cardiovascular Disease. Report on Health and Social Subjects No. 28. Report of the Panel on Diet in Relation to Cardiovascular Disease, Committee on Medical Aspects of Food Policy. Her Majesty's Stationery Office, London. 32 pp.
Doll, R., and R. Peto. 1981. The causes of cancer: quantitative estimates of avoidable risks of cancer in the United States today. J. Natl. Cancer Inst. 66:1191-1308.
Dupin, H., et al. 1981. Apports Nutritionnels Conseillés pour la population française. Technique et Documentation, Lavoisier, France. 101 pp.
Dyer, A.R., J. Stamler, O. Paul, R.B. Shekelle, J.A. Schoenberger, D.M. Berkson. M. Lepper, P. Collette, S. Shekelle, and H.A. Lindberg. 1981. Serum cholesterol and risk of death from cancer and other causes in three Chicago epidemiological studies. J. Chronic Dis. 34:249-260.
ECP/IUNS (European Organization for Cooperation on Cancer Prevention Studies/International Union for Nutritional Sciences). 1986. Proceedings of a joint ECP-IUNS workshop on diet and human carcinogenesis (Arhus, Denmark; June 1985). Nutr. Cancer 8:1-40.
Farchi, G., A. Menotti, and S. Conti. 1987. Coronary risk factors and survival probability from coronary and other causes of death. Am. J. Epidemiol. 126:400-408.
Finnish Heart Association. 1987. Prevention of Coronary Heart Disease in Finland. National Board of Health, National Public Health Institute, Finnish Cardiac Society. Finnish Heart Association, Helsinki, Finland. 96 pp.
Food and Nutrition Council, Netherlands. 1983-1984. Food Policy Note (Nota Voedingsbeleid). Ministry of Health, Welfare, and Culture, Ministry of Agriculture, and the Ministry of Economics. The Hague. 94 pp.
Garcia-Palmieri, M.R., P.D. Sorlie, R. Costas, Jr., and R.J. Havlik. 1981. An apparent inverse relationship between serum cholesterol and cancer mortality in Puerto Rico. Am. J. Epidemiol. 114:29-40.
Garn, S.M., and M. LaVelle. 1985. Two-decade follow-up of fatness in early childhood. Am. J. Dis. Child. 139:181-185.
German Society of Nutrition. 1985. Ten Guidelines for Sensible Nutrition. Deutsche Gesellschaft für Ernährung e.V. Frankfurt, Federal Republic of Germany. 6 pp.
Goldbourt, U. 1987. High risk versus public health strategies in primary prevention of coronary heart disease. Am. J. Clin. Nutr. 45 suppl. 5:1185-1192.
Goldman, L., and E.F. Cook. 1984. The decline in ischemic heart disease mortality rates. An analysis of the comparative effects of medical interventions and changes in lifestyle. Ann. Intern. Med. 101:825-836.
Greenwald, P., and E.W. Sondik, eds. 1986. Cancer control objectives for the nation: 1985-2000. J. Natl. Cancer Inst. Monogr. 2:1-105.
Grobstein, C. 1983. Should imperfect data be used to guide public policy? Science 83 4:18.
Hakama, M., and E.A. Saxén. 1967. Cereal consumption and gastric cancer. Int. J. Cancer 2:265-268.
Hardell, L., M. Eriksson, P. Lenner, and E. Lundgren. 1981. Malignant lymphoma and exposure to chemicals, especially organic solvents, chlorophenols and phenoxy acids: a case-control study. Br. J. Cancer 43:169-176.
Hegsted, D.M. 1986. Serum-cholesterol response to dietary cholesterol: a re-evaluation. Am. J. Clin. Nutr. 44:299-305.
Hennekens, C.H., W. Willett, B. Rosner, D.S. Cole, and S.L. Mayreut. 1979. Effects of beer, wine, and liquor in coronary deaths. J. Am. Med. Assoc. 242:1973-1974.
Higginson, J., and C.S. Muir. 1979. Environmental carcinogenesis: misconceptions and limitations to cancer control. J. Natl. Cancer Inst. 63:1291-1298.
Hoar, S.K., A. Blair, F.F. Holmes, C.D. Boysen, R.J. Robel, R. Hoover, and J.F. Fraumeni, Jr. 1986. Agricultural herbicide use and risk of lymphoma and soft-tissue sarcoma. J. Am. Med. Assoc. 256:1141-1147.
Inter-Society Commission for Heart Disease Resources. 1970. Primary prevention of the atherosclerotic diseases. Circulation Suppl. 42:A55-A95.
Inter-Society Commission for Heart Disease Resources. 1984. Optimal resources for primary prevention of atherosclerotic diseases. Circulation 70:153A-205A.
Iso, H., D.R. Jacobs, Jr., D. Wentworth, J.D. Neaton, and J. Cohen. 1988. Relationship of serum cholesterol to risk of different types of stroke: 28th conference on cardiovascular disease epidemiology. CVD Epidemiol. Newsletter (AHA) 43:40.
Jain, M., G.M. Cook, F.G. Davis, M.G. Grace, G.R. Howe, and A.B. Miller. 1980. A case-control study of diet and colo-rectal cancer. Int. J. Cancer 26:757-768.
Japanese Ministry of Health and Welfare. 1985. Dietary Guidelines for Health Promotion, Vol. 29. Health Promotion and Nutrition Division, Health Services Bureau. Ministry of Health and Welfare, Tokyo. 6 pp.
Jenkins, D.J.A. 1988. Carbohydrates (B) dietary fiber. Pp. 52-71 in M.E. Shils and V.R. Young, eds. Modern Nutrition in Health and Disease, 7th ed. Lea & Febiger, Philadelphia.
Jones, J.L., and J. Weimer. 1981. Health-related food choices. Fam. Econ. Rev. Summer:16-19.
Kagan, A., D.L. McGee, K. Yano, G.G. Rhoads, and A. Nomura. 1981. Serum cholesterol and mortality in a Japanese-American population: the Honolulu Heart Program. Am. J. Epidemiol. 114:11-20.
Kannel, W.B., and P.A. Wolf. 1983. Epidemiology of cerebrovascular disease. Pp. 1-24 in R.W.R. Russell, ed. Vascular Disease of the Central Nervous System, 2nd ed. Churchill Livingstone, Edinburgh.
Kark, J.D., A.H. Smith, and C.G. Hames. 1980. The relationship of serum cholesterol to the incidence of cancer in Evans County, Georgia. J. Chronic Dis. 33:311-322.
Kelsay, J.L. 1986. Update on fiber and mineral availability. Pp. 361-372 in G.V. Vahouny and D. Kritchevsky, eds. Dietary Fiber: Basic and Clinical Aspects. Plenum Press, New York.
Keys, A. 1968. Official Collective Recommendation on Diet in the Scandinavian Countries. Nutr. Rev. 26:259-263.
Keys, A. 1980. Pp. 345-359 in Seven Countries: A Multivariate Analysis of Death and Coronary Heart Disease. Harvard University Press, Cambridge, Mass.
Keys, A. 1984. Serum cholesterol response to dietary cholesterol. Am. J. Clin. Nutr. 40:351-359. Kozarevic, D., D. McGee, N. Vojvodic, T. Gordon, Z. Racic, W. Zukel, and T. Dawber. 1981. Serum cholesterol and
Page 709
mortality: the Yugoslavia Cardiovascular Disease Study. Am. J. Epidemiol. 114:21-28.
Langsford, W.A. 1979. A food and nutrition policy. Food Nutr. Notes Rev. 36:100-103.
Louis Harris & Associates, Inc. 1978. Health Maintenance. Pacific Mutual Life Insurance Co., Newport Beach, Calif. 88 pp.
Louis Harris & Associates, Inc. 1979. The Perrier Study: Fitness in America. Great Waters of France, Inc., New York. 59 pp.
LSRO (Life Sciences Research Office). 1987. Physiological Effects and Health Consequences of Dietary Fiber. Federation of American Societies for Experimental Biology, Bethesda, Md. 236 pp.
MacGregor, G.A. 1985. Sodium is more important than calcium in essential hypertension. Hypertension 7:628-640.
Macquart-Moulin, G., E. Riboli, J. Cornée, B. Charnay, P. Berthezène, and N. Day. 1986. Case-control study on colorectal cancer and diet in Marseilles. Int. J. Cancer 38: 183-191.
Mark Clements Research, Inc. 1980. Trends in Nutrition, I. The Benchmark Survey, February, 1980. Self Magazine, New York. (various pagings)
Marmot, M.G., A.M. Adelstein, N. Robinson, and G.A. Rose. 1978. Changing social-class distribution of heart disease. Br. Med. J. 2:1109-1112.
Marshall, J.R., R. Priore, S. Graham, and J. Brasure. 1981. On the distortion of risk estimates in multiple exposure level case-control studies. Am. J. Epidemiol. 113:464-473.
McMichael, A.J., and J.D. Potter. 1984. Parity and death from colon cancer in women: a case-control study. Comm. Health Study 8:19-25.
Miller, A.B. 1978. An overview of hormone-associated cancers. Cancer Res. 38:3985-3990.
Miller, A.B. 1982. Risk factors from geographic epidemiology for gastrointestinal cancer. Cancer 50 suppl. 11:2533-2540.
Miller, J.Z., M.H. Weinberger, and J.C. Christian. 1987. Blood pressure response to potassium supplementation in normotensive adults and children. Hypertension 10:437-442.
Miller, J.Z., M.H. Weinberger, S.A. Daugherty, N.S. Fineberg, J.C. Christian, and C.E. Grim. 1988. Blood pressure response to dietary sodium restriction in healthy normotensive children. Am. J. Clin. Nutr. 47:113-119.
Molitor, G.T. 1979. National nutrition goals: how far have we come? Pp. 135-141 in M. Chou and D.P. Harmon, Jr., eds. Critical Food Issues of the Eighties. Pergamon Press, New York.
NACNE (National Advisory Committee for Nutrition Education). 1983. A Discussion Paper on Proposals for Nutritional Guidelines for Health Education in Britain. Health Education Council, London. 40 pp.
National Advisory Committee, New Zealand. 1982. Nutrition goals for New Zealanders. Health 34:11-12.
National Cholesterol Education Program. 1988. Report of the National Cholesterol Education Program Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Arch. Intern. Med. 148:36-69.
National Heart Foundation of Australia, Committee on Diet and Heart Disease. 1979. Diet and coronary heart disease: a review. Med. J. Aust. 2:294-307.
National Heart Foundation of New Zealand. 1976. Coronary Heart Disease: A Progress Report, 1976. Report by a Committee Convened by the Scientific Committee of the National Heart Foundation of New Zealand. National Heart Foundation of New Zealand, Dunedin, New Zealand. 132 pp.
NCI (National Cancer Institute). 1984a. Cancer Prevention: Good News, Better News, Best News. NIH Publ. No. 842671. National Institutes of Health, Public Health Service, U.S. Department of Health and Human Services. U.S. Government Printing Office, Washington, D.C. 20 pp.
NCI (National Cancer Institute). 1984b. Diet, Nutrition, and Cancer Prevention: A Guide to Food Choices. NIH Publ. No. 85-2711. National Institutes of Health, Public Health Service, U.S. Department of Health and Human Services. U.S. Government Printing Office, Washington, D.C. 52 pp.
NCI (National Cancer Institute). 1987. Diet, Nutrition, and Cancer Prevention: A Guide to Food Choices. NIH Publ. No. 87-2878. National Institutes of Health, Public Health Service, U.S. Department of Health and Human Services. U.S. Government Printing Office, Washington, D.C. 39 pp.
NHLBI (National Heart, Lung, and Blood Institute). 1980. Summary Report of the NHLBI Cholesterol Workshop, February 26-27, 1980. Division of Heart and Vascular Disease, National Institutes of Health. U.S. Government Printing Office, Washington, D.C.
NIAAA (National Institute on Alcohol Abuse and Alcoholism). 1986. Toward a National Plan to Combat Alcohol Abuse and Alcoholism: A Report to the United States Congress. National Institutes of Health, Public Health Service, U.S. Department of Health and Human Services, Rockville, Md. 81 pp.
NIH (National Institutes of Health). 1984a. Health Implications of Obesity: National Institutes of Health Consensus Development Conference Statement. Ann. Intern. Med. 103:1073-1077.
NIH (National Institutes of Health). 1984b. Osteoporosis: Consensus Development Conference Statement, Vol. 5. Publ. No. 421-132:4652. National Institute of Arthritis, Diabetes, and Digestive and Kidney Diseases and the Office of Medical Applications of Research. U.S. Government Printing Office, Washington, D.C. 6 pp.
NIH (National Institutes of Health). 1985. Lowering blood cholesterol to prevent heart disease: consensus conference. J. Am. Med. Assoc. 253:2080-2086.
NRC (National Research Council). 1980a. Recommended Dietary Allowances. 9th ed. A Report of the Committee on Dietary Allowances, Food and Nutrition Board, Assembly of Life Sciences, National Academy of Sciences. National Academy Press, Washington, D.C. 185 pp.
NRC (National Research Council). 1980b. Toward Healthful Diets. Report of the Food and Nutrition Board, Division of Biological Sciences, Assembly of Life Sciences. National Academy of Sciences, Washington, D.C. 24 pp.
NRC (National Research Council). 1982. Diet, Nutrition, and Cancer. Report of the Committee on Diet, Nutrition, and Cancer, Assembly of Life Sciences, National Academy Press, Washington, D.C. 496 pp.
Oliver, M.F., J.A. Heady, J.N. Morris, and J. Cooper. 1978. A co-operative trial in the primary prevention of ischaemic heart disease using clofibrate: report from the Committee of Principal Investigators. Br. Heart J. 40:1069-1118.
Oliver, M.F., J.A. Heady, J.N. Morris, and J. Cooper. 1980. W.H.O. cooperative trial on primary prevention of ischaemic heart disease using clofibrate to lower serum cho-
Page 710
lesterol: mortality follow-up. Report of the Committee of Principal Investigators. Lancet 2:379-385.
Olson, R.E. 1986. Mass intervention vs screening and selective intervention for the prevention of coronary heart disease. J. Am. Med. Assoc. 255:2204-2207.
Page, I.H., E.V. Allen, F.L. Chamberlain, A. Keys, J. Stamler, and F.J. Stare. 1961. Dietary fat and its relation to heart attacks and strokes. Circulation 23:133-136.
Page, L., and E.F. Phipard. 1957. Essentials of an Adequate Diet. Home Economics Research Report No. 3. Agricultural Research Service, U.S. Department of Agriculture. U.S. Government Printing Office, Washington, D.C. 21 pp.
Pahlke, G. 1975. Dietary fat and degenerative vascular diseases. Nutr. Metab. 18:113-115.
Palmer, S. 1983. Diet, nutrition, and cancer: the future of dietary policy. Cancer Res. 43 suppl. 5:2509s-2514s.
Panel on Nutrition and Prevention of Diseases. 1983. Dietary guidelines and nutrition policies in Japan. Ministry of Health and Welfare, Public Health Bureau. Japan Dietetic Association, Tokyo. 168 pp.
Phillips, R.L. 1975. Role of life-style and dietary habits in risk of cancer among Seventh-Day Adventists. Cancer Res. 35: 3513-3522.
Reed, D., K. Yano, and A. Kagan. 1986. Lipids and lipoproteins as predictors of coronary heart disease, stroke, and cancer in the Honolulu Heart Program. Am. J. Med. 80: 871-878.
Risch, H.A., M. Jain, N.W. Choi, J.G. Fodor, C.J. Pfeiffer, G.R. Howe, L.W. Harrison, K.J. Craib, and A.B. Miller. 1985. Dietary factors and the incidence of cancer of the stomach. Am. J. Epidemiol. 122:947-959.
Rose, G. 1985. Sick individuals and sick populations. Int. J. Epidemiol. 14:32-38.
Rose, G., and M.J. Shipley. 1980. Plasma lipids and mortality: a source of error. Lancet 1:523-526.
Rose, G., H. Blackburn, A. Keys, H.L. Taylor, W.B. Kannel, O. Paul, D.D. Reid, and J. Stamler. 1974. Colon cancer and blood-cholesterol. Lancet 1:181-183.
Royal Ministry of Health and Social Affairs. 1981-1982. On the Follow-up of Norwegian Nutrition Policy. Report No. 11 to the Storting (1981-1982). Oslo. 79 pp.
Shapiro, L.R., P.B. Crawford, M.J. Clark, D.L. Pearson, J. Raz, and R.L. Huenemann. 1984. Obesity prognosis: a longitudinal study of children from the age of 6 months to 9 years. Am. J. Public Health 74:968-972.
Sidney, S., and J.W. Farquhar. 1983. Cholesterol, cancer, and public health policy. Am. J. Med. 75:494-508.
Silverberg E., and J.A. Lubera. 1988. Cancer statistics, 1988. CA Mag. 38:5-22.
Swedish National Food Administration. 1981. Swedish Nutrition Recommendations. National Food Administration, Uppsala. 11 pp.
Tuomilehto, J., J. Geboers, J.T. Salonen, A. Nissinen, K. Kuulasmaa, and P. Puska. 1986. Decline in cardiovascular mortality in North Karelia and other parts of Finland. Br. Med. J. 293:1068-1071.
Upton, A.C. 1979. Statement on Diet, Nutrition, and Cancer. Hearings of the Subcommittee on Nutrition of the Senate Committee on Agriculture, Nutrition, and Forestry, October 2, Washington, D.C.
U.S. Senate. 1977. Dietary Goals for the United States, 2nd ed. Report of the Select Committee on Nutrition and Human Needs. Stock No. 052-070-04376-8. U.S. Government Printing Office, Washington, D.C. 83 pp.
USDA (U.S. Department of Agriculture). 1984. Nationwide Food Consumption Survey. Nutrient Intakes: Individuals in 48 States, Year 1977-78. Report No. 1-2. Consumer Nutrition Division, Human Nutrition Information Service, Hyattsville, Md. 439 pp.
USDA (U.S. Department of Agriculture). 1987. Nationwide Food Consumption Survey. Continuing Survey of Food Intakes by Individuals. Women 19-50 Years and Their Children 1-5 Years, 4 Days, 1985. Report No. 85-4. Nutrition Monitoring Division, Human Nutrition Information Service, U.S. Department of Agriculture, Hyattsville, Md. 182 pp.
USDA/DHHS (U.S. Department of Agriculture/Department of Health and Human Services). 1980. Nutrition and Your Health: Dietary Guidelines for Americans. Home & Garden Bulletin No. 228. U.S. Department of Agriculture and Department of Health and Human Services, Washington, D.C. 20 pp.
USDA/DHHS (U.S. Department of Agriculture/Department of Health and Human Services). 1985. Nutrition and Your Health: Dietary Guidelines for Americans, 2nd ed. Home & Garden Bulletin No. 228. U.S. Government Printing Office, Washington, D.C. 24 pp.
Waterhouse, J., C. Muir, K. Shanmugaratnam, and . Powell, eds. 1982. Cancer Incidence in Five Continents, Vol. IV. International Agency for Research on Cancer, Lyon, France. 812 pp.
Westlund, K., and R. Nicolaysen. 1972. Ten-year mortality and morbidity related to serum cholesterol. Scand. J. Clin. Lab. Invest. 30 suppl. 127:1-24.
WHO (World Health Organization). 1982. Prevention of Coronary Heart Disease. Report of a WHO Expert Committee. Technical Report Series No. 678. World Health Organization, Geneva. 53 pp.
WHO (World Health Organization). 1987. World Health Statistics Annual 1987. World Health Organization, Geneva. 455 pp.
Wilhelmsen, L., G. Berglund, D. Elmfeldt, G. Tibblin, H. Wedel, K. Pennert, A. Vedin, C. Wilhelmsson, and L. Werkö. 1986. The multifactor primary prevention trial in Göteborg, Sweden. Eur. Heart J. 7:279-288.
Williams R.R., P.D. Sorlie, M. Feinleib, P.M. McNamara, W.B. Kannel, and T.R. Dawber. 1981. Cancer incidence by levels of cholesterol. J. Am. Med. Assoc. 245:247-252.
Wynder, E.L., and G.B. Gori. 1977. Contribution of the environment to cancer incidence: an epidemiologic exercise. J. Natl. Cancer Inst. 58:825-832.
Yaari, S., U. Goldbourt, S. Even-Zohar, and H.N. Neufeld. 1981. Associations of serum high density lipoprotein and total cholesterol with total, cardiovascular, and cancer mortality in a 7-year prospective study of 10,000 men. Lancet 1:1011-1015.














































