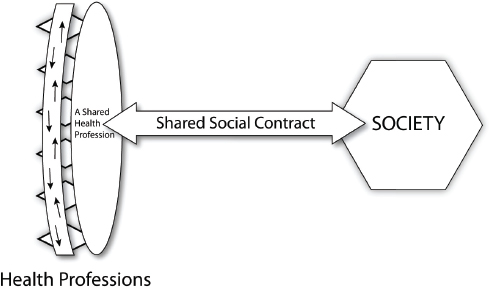
FIGURE II-3 Transdisciplinary professionalism.
SOURCE: Belar, 2013.
a problem. The Global Forum’s convening mechanism is an opportunity to go where Forum members have not gone before; we cannot predetermine its outcome. That depends on the views of the participants who represent numerous professions and perspectives. Will it be possible to develop a shared social contract with society for the next generation of health professionals? If so, how will it be modeled, and how will it be taught? This workshop may only be an initial step.
II.2 PROFESSIONALISM AND MEDICINE’S SOCIAL CONTRACT1
Richard L. Cruess, M.D., and Sylvia R. Cruess, M.D.
Centre for Medical Education, McGill University
Paul Starr appears to have been the first to describe the relationship between medicine and society as contractual. In his 1982 book, he wrote that the contract between medicine and society was being redrawn in
________________
1 This paper is based in part on work previously published in Perspectives in Medicine and Biology 51:579–598 (2008).
response to dramatic changes in health care and that the changes were “subjecting medical care to the discipline of politics or markets or reorganizing its basic institutional structure” (Starr, 1982, p. 380). Subsequently, many observers, including social scientists (e.g., Pescosolido et al., 2000; Stevens, 2001; Hafferty, 2003; Sullivan, 2005), lawyers (e.g., Rosenblatt et al., 1997), policy analysts (e.g., Iglehart, 2005), bioethicists (e.g., Bloom, 2002; Kurlander et al., 2004; Williams-Jones and Burgess, 2004; World Medical Association, 2005; Wynia, 2008), and physicians (e.g., Inui, 1992; Cruess, 1993; Rettig, 1996; Ludmerer, 1999; Gillon et al., 2001; Benson, 2002; Barondess, 2003; Davies and Glasspool, 2003; Gruen et al., 2004; Smith, 2004; Wells, 2004; Cruess and Cruess, 2008), turned to the historical concept of the “social contract” as being a useful and accurate description of the relationship. The idea that the relationship between medicine and society involved reciprocity has been extant in the United Kingdom for some time. In discussing the establishment of the UK National Health Service (NHS), Klein (1983) proposed that a “bargain” had been struck in which the medical profession preserved its autonomy and privileged position in return for supporting the new health care system. Following this, others have used the term “implicit bargain,” particularly during recent years, because, they pointed out, the bargain appeared to have broken down. Two new terms have recently emerged as Ham and Alberti (2002) and others (Edwards et al., 2002; Rosen and Dewar, 2004) called the relationship an “implicit compact” and the Royal College of Physicians of London refers to a “moral contract” (2005). None of these terms has roots in either philosophy or political science.
The Changing Nature of Health Care, Professionalism, and the Social Contract
The social contract between medicine and society that existed until the middle of the 20th century was relatively simple (Starr, 1982; Krause, 1996). Medicine was practiced by solo practitioners treating individual patients who were generally responsible for paying for the services received. There were many opportunities to demonstrate altruism because of the large numbers of medically-indigent patients whom physicians often treated for free. Accountability rested with the patient, with minimal accountability for the wider society. Individual physicians and the medical profession were trusted and had unquestioned authority. As medicine became a “mature” and established profession, it became inherently conservative and often defended what it regarded as the substance of its professionalism based on an understanding of the social contract of that era. Hafferty and Castellani (2010) have labeled this “nostalgic professionalism” and pointed out that it is not applicable to the contemporary practice of medicine. They also
propose that the basis of the current social contract is being pushed toward different forms of professionalism, including “lifestyle” and/or “entrepreneurial” professionalism. What is eminently clear is that the social contract of the early 21st century is very different from that of 50 years ago.
The Social Contract—Its Origins and Evolution
The early philosophers who developed the concept of the social contract did so in response to the injustices that existed in a time of hereditary monarchs (Gough, 1957; Crocker, 1968; Masters and Masters, 1978; Bertram, 2004). It sought to explain the origins of the state and society and to delineate their relationship. A contemporary definition of the term “social contract” is
a basis for legitimating legal and political power in the idea of a contract. Contracts are things that create obligations, hence if we can view society as organized “as if” a contract has been formed between the citizen and the sovereign power, this will ground the nature of the obligations, each to the other. (Blackburn, 1996, p. 335)
Although not all philosophers or social scientists endorse the application of the term “social contract” to the field of health care, there is a respected and influential group that does (Rawls, 1999, 2003; Bertram, 2004; Daniels, 2008). Rawls proposed that the organizing principle in society should be justice based on fairness. Although he did not classify health as a “social primary good,” he did believe health is necessary for individuals to be “normal and fully cooperating members of society over a complete life” (Rawls, 2003, p. 174) and that this constitutes an entitlement to health services. Daniels (2008) endorsed this point of view and expanded it by stating that health care was essential as a means of access to “fair equality of opportunity in society.”
It is important to emphasize that no formal contract exists in the legal sense. Rather, as stated by Gough, the rights and duties of the parties to the contract “are reciprocal and the recognition of this reciprocity constitutes a relationship which by analogy can be called a social contract” (Gough, 1957, p. 245). Contemporary interpretation of contract theory leans heavily on the idea of “legitimate expectations” as being fundamental to mutual understanding (Rawls, 2003; Bertram, 2004). Obviously, a failure of one party to meet the legitimate expectations of the other has consequences in the attitudes and hence the responses of the other.
In placing health care in the context of the social contract, it can be located within what has been labeled a “macro” contract (Donaldson and Dunfee, 1999, 2002), which includes all essential services required
by citizens. Another approach suggests that there are a series of “micro” contracts that apply to individual services that must conform to the “moral boundaries” laid down by a macro contract (Donaldson and Dunfee, 1999, 2002). Health care could be included in the overall relationship, as Rawls and others have suggested, or, given its importance to the well-being of both individuals and society, it could be governed by its own micro contract. It appears to us that this latter approach better describes the reality of the relationship. It has the further advantage of allowing health care issues to be addressed in isolation from other issues in society within the context of the overall macro contract.
Finally, it is obvious that the details of the social contract between medicine and society differ substantially between countries, being influenced by cultural, economic, and political factors. Although there are many documented commonalities, there are also significant differences in the funding and organization of health care (Ferlie and Shortell, 2001; Schoen et al., 2004; Anderson et al., 2005), in how professionalism is expressed, and in the expectations of the general public (Vogel, 1986; Hafferty and McKinley, 1993; Krause, 1996; Tuohy, 1999; Cruess et al., 2010; Hodges et al., 2011). What probably does not differ is the role of the healer, which has been present as long as mankind has existed and which answers a basic human need in times of illness (Kearney, 2000). Those elements of the social contract that refer to the healer’s role will therefore be relatively constant across national and cultural boundaries, while those that refer to how the services of the healer are organized, funded, and delivered will vary (Cruess and Cruess, 1997).
Medicine’s Social Contract
Although it is clear that no written social contract exists between individual physicians and the medical profession and society, it is apparent that the contract is a mixture of the written and the unwritten. The written portions are numerous, and many impose legal obligations on the profession and its members. These include licensing laws and documents mandating the organizations responsible for self-regulation, including licensing, certifying, and accrediting bodies, as well as the medical education establishment. Codes of ethics are publicly available documents governing the behavior of physicians. The laws outlining the nature of the health care system in every country are explicit expressions of important parts of the social contract in that country.
These legally binding portions of the contract are very important. However, of extreme importance to both patients and physicians are those portions of the social contract that cannot be legislated or imposed. They spring from the inherent moral nature of the medical act (Pellegrino, 1990). Care,
compassion, altruism, and commitment are an essential part of the professional identity of every practicing physician, and they clearly represent fundamental expectations of patients and the public. Expressing them must spring from a sense of who physicians are, rather than just what they do.
A frequent statement in the literature is that “a social contract exists between medicine and society,” implying that each side is monolithic. This is not true. We have proposed an outline of the nature of the social contract between medicine and society (see Figure II-4), one that differs from the only other published outline of which we are aware (Ham and Alberti, 2002). As can be seen, the medical profession consists of individual physicians and the many institutions that represent them, including national and specialty associations and regulatory bodies. Within the circle chosen to represent the medical profession are found a myriad of firmly held opinions, vested interests, and political orientations. Individual physicians often dis-
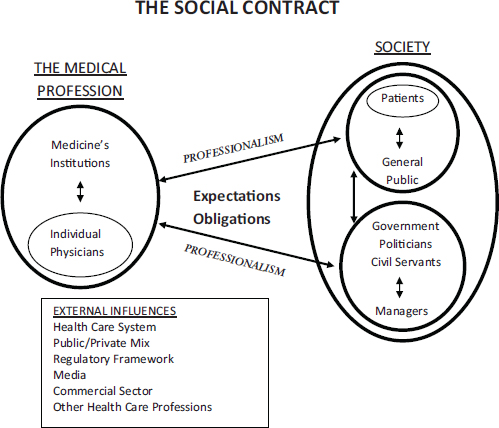
FIGURE II-4 A schematic representation of medicine’s social contract with society.
SOURCE: Cruess and Cruess, 2008.
agree with the associations that represent them, generalists and specialists may have different approaches, and there are often regional differences in opinion. Nevertheless, in most countries, some form of consensus emerges within the medical profession when it is negotiating the details of its social contract, although this term is almost never invoked to describe the process.
A democratic society is even more complex. It consists of citizens and those whom they chose to govern them. When one focuses on health care, citizens can be designated as patients and members of the general public. Obviously, members of the general public have a clear and personal interest in the relationship with the medical profession, because virtually every citizen will eventually need the services of the healer. For patients, the need is immediate. Although there may be tension between patients and patients’ groups and the wider public, their needs and desires are generally not dissimilar as they approach the negotiations.
As health care in most countries has come to be regarded as a right, governments have become responsible for ensuring that minimal levels of care are available to their citizens, thus giving them a major and often determining role in setting the terms of the social contract. However, governments are not monolithic, and there are many vested and often conflicting interests within them. Elected politicians are answerable to their constituents, civil servants are responsible for the proper functioning of the system, and managers in the field have their own responsibilities and desires. Government policy results from a dialogue among these hierarchically organized parties, with elected politicians being ultimately accountable.
Within the circle representing society, the relationship between patients and the public and government is primarily political, with the public in democratic societies expressing its satisfaction or dissatisfaction with government policy in health through the electoral process. It is reminiscent of the original meaning of the social contract.
Professionalism has been defined as “a set of values, behaviors, and relationships that underpins the trust that the public has in doctors” (Royal College of Physicians of London, 2005, p. 14). Trust is absolutely essential if the social contract is to function (Sullivan, 1995; Goold, 2002). Society’s expectations of both individual physicians and the medical profession are based on both trust and understanding of these values and behaviors. This explains why professionalism is the basis of medicine’s social contract with society. Society expects physicians to behave professionally in return for their privileged position. If they fail to do so, society will alter the contract.
Mediators of the Social Contract
Although the primary social contract for medicine involves the profession and society, there are structures and powerful stakeholders with
legitimate and vested interests in the overall health care system who have a profound impact on medicine’s social contract (Rosen and Dewar, 2004). The nature of the national health care system is undoubtedly the most powerful. Other structures and stakeholders include the regulatory system, the commercial sector, other health professions, and the media.
The current social contract between medicine and society represents the “bargain” that has been established. It is based in part on historical practices and in part on direct negotiations between medicine and society and is heavily influenced by the input of the many stakeholders who have legitimate vested interests in how health care is organized and delivered. Because both health care and society are in a period of rapid change, how this contract will change and how it will be renegotiated becomes important.
The Negotiations Leading to Expectations and Obligations
Norman Daniels in Just Health (2008) discusses the process of “social negotiation,” which determines the nature of physician’s obligations and powers. He states that negotiation consists of “various forms of interaction between professional organizations and broader political institutions. It may lead to … specific legal arrangements … or there may be broader understandings that emerge from public debate about specific issues” (p. 225). He points out that there is a socially negotiated ideal of “the good physician” and that at any given point in time physician behavior is constrained by the nature of this ideal. Upon joining the profession, an individual must accept this concept and is not free to pick and choose among the obligations which result from it. However, the concept of the good physician is not immutable and is being constantly renegotiated as “conditions inside and outside medicine change.” For example, the paternalistic model of the doctor–patient relationship has gradually altered as the patients’ rights movement firmly established the principle of patient autonomy in decision making (Emanuel and Emanuel, 1992; Truog, 2012). The negotiations that led to this change took place in a decentralized fashion over many decades.
Other changes can occur more precipitously. The introduction of national health plans in the United Kingdom (Klein, 1995) and Canada (Marchildon, 2006) changed medicine’s social contract the moment the legislation was enacted. In both instances, prolonged negotiations involving the profession preceded the change. Recently, the perception of both the general public and the government in the United Kingdom that the medical profession had failed to exercise the authority delegated to them to self-regulate caused the government to withdraw some of that authority. The regulatory framework in the United Kingdom is now substantially different, and as a result the nature of the social contract, and of the substance of medical professionalism, has changed (Secretary of State for Health, 2007).
It should be stressed that at any moment in time, negotiations are taking place that will lead to an alteration in medicine’s social contract with society.
Who Negotiates the Social Contract?
As should be clear, there are a host of issues that, together, make up medicine’s social contract. The nature and substance of the health care system itself is without doubt the most tangible expression of this social contract, and it imposes the distinctive characteristics that are found in different countries and cultures (Hafferty and McKinley, 1993; Krause, 1996). Because professionalism in any given country is based on the social contract, it is not surprising that differences are found in the nature of professionalism across national and cultural lines (Cruess et al., 2010; Ho, 2011).
With one prominent country serving as an exception, the negotiations that result in the social contract are carried out at national or regional negotiating tables. Society is usually represented by members of the government or an organization mandated to act on the government’s behalf, a situation that has been present because most countries in the developed world established national health plans. Medicine is usually represented by a national or regional medical association. In Canada, where responsibility for health is a fiercely protected provincial jurisdiction, each province or territory has its own health care system which, while adhering to national standards, can accommodate differing regional needs (Marchildon, 2006). The provincial medical associations are either unions or quasi-unions and are mandated to negotiate on behalf of the medical profession. In Europe, medical unions are the norm. Although the term “social contract” is almost never used during the negotiations, fundamental aspects of the social contract are negotiated directly between the medical profession and government.
The exception to the rule is of course the United States, which until recently had not introduced a true national health plan. As pointed out by Stevens (2001, pp. 329–330), in the United States “there has been no similar concentration of responsibility for universal health insurance at national, state, or local levels and no single government agency responsible for delegating formal power to medical organizations in relation to organized payment and service systems,” a situation that still appears to be true. With its long history, the American Medical Association (AMA) would appear to have the mandate to represent medicine, but well under one-third of practicing physicians belong to the AMA. The AMA therefore lacks credibility in attempting to speak for the medical profession (Wolinsky and Brune, 1994). Most physicians are more comfortable being represented by their specialty associations. The lack of a national health plan has led to the absence of a central negotiating table at which the social contract can be addressed.
Negotiations in United States are carried out at many levels, with the commercial sector having substantial input into the nature of the contract. Of course, this does not mean that a social contract does not exist in the United States. The contract that does exist, as pointed out by Hafferty and Castellani (2010), is less well defined, because it is impacted by the many pressures found in American society. The contract, and the professionalism derived from it, stresses individualism and individual responsibility and must accommodate the necessity for practicing physicians to function as entrepreneurs in a competitive marketplace. Medicine is often treated as a commodity, and physicians have been described as often serving as double agents, with fiduciary duties to patients conflicting with legal obligations to employers or insurers (Angell, 1993; Schlesinger, 2002). As has been noted, a social contract implies reciprocity, with rights and privileges accompanied by obligations for the other parties to the contract. The impact of the commercial sector results in a social contract in which there are tensions between patients’ expectations and physicians’ complex obligations.
The Expectations of Medicine and Society: “Each to the Other”
All contracts impose obligations on the parties to the contract, and social contracts, in spite of their amorphous nature, are no different. The expectations of one party to the contract lead to the obligations of the other party. It thus becomes important that all parties to the contract understand the expectations of the other parties. If medicine fails to meet the legitimate expectations of society, society will wish to change the contract. On the other hand, if what individual physicians and the medical profession regard as their legitimate expectations are not met, they will respond by either attempting to alter the contract or perhaps by changing their own behavior.
In a previous publication we proposed an outline of the obligations between physicians and medicine and patients and the general public, between physicians and medicine and government, and between government and patients and the general public (Cruess and Cruess, 2008). This analysis was based on a review of the literature. Patients’ expectations of individual physicians and of medicine are well documented. They want accessible care within the context of a health care system that is value-laden, equitable, and adequately funded and staffed. They want their physicians to be competent, caring, and compassionate, to listen to them, to be accountable, and to demonstrate qualities that lead to trust. They want to be able to preserve their own dignity and autonomy in decision making. Finally, they want some input into public policy. Government expectations, although less explicitly documented, are made known. They make assumptions upon which public policy is grounded, and these assumptions serve as the basis of their expectations of medicine (Le Grand, 2003). As long as the privilege of self-
regulation is granted to the medical profession, they expect the profession to assure the competence of its members. They require compliance with laws related to health care and also expect that members of the medical profession will be trustworthy. They believe that professions should serve as a source of objective advice—even if this advice is often ignored—and they believe that because of the privileged position of the medical profession, the profession and its members must be devoted to the public good. Finally, they require new levels of accountability (Wynia et al., 1999) and want the profession to practice team health care, expectations that have become much more important in recent times.
It is interesting that the expectations of individual physicians and of medicine as a whole are rarely made explicit in a coherent fashion. This is somewhat surprising, because it is quite legitimate for physicians to have expectations of patients, of the general public, and of governments. However, one can infer these expectations from the negotiating stances of the profession and from surveys of physicians that document levels of satisfaction and dissatisfaction (Cruess and Cruess, 2008). An important expectation of medicine is sufficient autonomy for physicians to exercise independent judgment in giving advice to patients. Physicians also expect to be trusted, because the role of the healer requires such trust. Because of their expertise, physicians expect a role in forming public policy in health. There is also considerable evidence that physicians, like patients, want a health care system that is value-laden, equitable, adequately funded and staffed and with reasonable freedom within the system. Although this is rarely articulated, physicians clearly want the monopoly granted to them through licensure laws to be maintained. In many parts of the world, the profession’s ability to self-regulate remains a significant expectation. The recent changes in the United Kingdom will certainly alter expectations in that country, and, in this global world, other countries may well re-examine self-regulation. Finally, physicians expect rewards—both financial and non-financial. Several surveys indicate that autonomy and respect rather than increased remuneration are important to physicians.
Significance
One might legitimately ask why it is necessary or desirable to invoke the concept of the social contract in describing the relationship between contemporary medicine and society. What are the benefits to medicine or society?
There is consensus that events of the past few decades have resulted in a situation in which neither medicine nor society is satisfied with the relationship (Dunning, 1999; Sullivan, 2005). There is also agreement that medicine’s professionalism is under threat, with the threats coming from two well-documented but separate sources (Starr, 1982; Krause, 1996;
Freidson, 2001; Sullivan, 2005). The first series of threats arises from the failure of the medical profession to meet some of the legitimate expectations of both patients and society in areas over which the profession exercises independent authority. Self-regulation and the belief that physicians are not as altruistic as were their forefathers are examples (Freidson, 2001; Jones, 2002). Because these issues lie within medicine’s control, direct action by the profession is necessary, and, indeed, the profession has reacted. Regulatory procedures are becoming more rigorous and transparent. Maintenance of competence, re-licensure, and/or re-validation are being considered or implemented throughout the world (Irvine, 2003). Attempts are being made to inform physicians of their obligations through educational programs whose purpose is the explicit teaching of professionalism (Cohen, 2006; Cruess and Cruess, 2006).
A second series of threats arises from the society that the profession serves and the health care systems within which medicine must function. Society and the health care system can either support or subvert professional values, and in many instances the latter appears to be true (Cohen et al., 2007). Obviously, medicine has no direct control over society or the health care system. An obvious recourse is to negotiate for a health care system that actually supports professional values, a direction that can benefit both medicine and society (Wynia et al., 1999; Sullivan, 2005; Cohen et al., 2007). Framing the discussion in terms of negotiating medicine’s social contract has several advantages.
First, the very use of the word contract implies negotiation. Second, it recognizes the principle of reciprocity. The central idea included in the discourse in the social sciences—that medicine was granted a privileged position on the understanding that it would behave in ways that benefited society—is both legitimized and formalized. In this way, medicine’s professional obligations become both logical and understandable. Third, it implies that there will be consequences if the terms of the contract are not met. If medicine fails to meet legitimate societal expectations, society will wish to change the contract, perhaps withdrawing some of medicine’s privileges, as happened in the United Kingdom. However, the converse is true. If physicians feel that their legitimate expectations are not met, individual physicians and the profession will react. One possible response is a change in physician behavior. For example, the physician entrepreneur may emerge (Hafferty and Castellani, 2010).
Finally, the concept of the social contract can be beneficial in teaching professionalism to current students, trainees, and practitioners who no longer respond to obligations framed as “thou shall” or “thou shall not” (Twenge, 2009). They wish to know why they must behave in a certain way, and framing the discourse terms of a social contract provides a logical answer.











