7
Partners in Promoting Health Equity in Communities
Effective partnerships are essential for community-based solutions for advancing health equity by making it a shared vision and value, increasing the community’s capacity to shape outcomes, and fostering multi-sector collaboration. Many different stakeholders can lead or participate in championing and implementing such solutions. These include organizations with a health mission, such as public health agencies, hospitals, or federally qualified health centers. In some communities these traditional partners are joined by public- and private-sector partners, including community-based organizations, faith-based organizations, businesses (from Fortune 1,000 to small employers), the education sector and academia, philanthropy, housing, justice, planning and land use, public safety, and transportation agencies.
Partners are able to deploy unique skills and access resources to serve a variety of roles in community-based solutions for health equity. A partner, such as a public health agency or a congregation, may serve as the convener of coalitions as a source of data and analysis (e.g., the local hospital, university, or school district), as a funder (a foundation or community development financial institution), or all of the above. As philanthropy and other partners engage in actions and interventions that address the underlying or “upstream” causes of health inequity (Mitchell, 2016), innovative ideas from the private sector are being brought to bear in addressing health inequities.
The concepts of disruption, innovation, paradigm shift, and design thinking have become guiding principles for engaging in this emerging
collaborative cross-sector work. Systems have functioned in silos for decades for good reason: efficiency, expertise, and logistics have all kept programs moving down the same course. However, the outcomes that result from those systems need to improve, and to get to the improved outcomes will require novel ways of both defining the challenges and thinking about how cross-sector partners can come together, leverage work from other fields, and work effectively as a team.
Human-centered design is an approach that places communities and individuals at the center of the solution. Particularly for health equity, community engagement plays a central role in finding solutions. Different models have used design thinking for place-based initiatives as well as solutions aimed at improving other social determinants of health. More of these partnerships with various cross-sector groups are likely to arise in the coming years (Active Living By Design, 2016).
In addition to new ways to bring cross-sector partners together across levels, new forums will likely emerge. These could include combining professional education, joint conferences, new educational tracks within professional schools, and new positions within institutions that span multiple skill sets—for example, a planner embedded in a health department and a health worker embedded in a planning department. In the following sections, different health equity actors are highlighted, with their unique roles in promoting health equity outcomes described and various examples offered of how they have been able to create partnerships to advance progress toward health equity. Innovative approaches to fostering multi-sector collaboration to achieve health equity will require participation from many different partners. Research on community engagement initiatives suggests that these partnerships generate benefits at both the individual and community levels (Attree et al., 2011). The remainder of this chapter is dedicated to describing these different stakeholders and the roles they may assume in supporting community interventions, ending with a discussion of cross-sector collaboration.
FINANCE
In recent years, the array of funding sources and financing structures for community-based efforts to address social, economic, and environmental factors that shape health has greatly expanded. In addition to federal government programs such as Promise Neighborhoods and the Sustainable Communities Partnership and foundations that support community work (e.g., the California Endowment’s Building Healthy Communities, the multi-partner Build Health Challenge), the funding landscape now includes the community development sector, led by the Federal Reserve Bank of San Francisco and others, for-profit financial
institutions, social investors, and others. Emerging financing structures include pay-for-success arrangements and private equity real estate funds (NASEM, 2016a; Super Church, 2015). The role of hospitals and health system as sources of financing—for example, through community benefit investments—is discussed in the section on anchor institutions.
Although the range of potential funders of efforts to advance community well-being and to address the roots of health inequity has expanded, the ongoing need to secure adequate and sustainable funding even in the face of constraints (e.g., both ongoing and acute, such as economic recession) is a fact of life. Partnerships need to be creative and cannot view their work in a silo; identifying leverage points and co-benefits is vital. Funding from the transportation, infrastructure improvement, development, climate resilience, and health sectors needs to be leveraged collaboratively to garner a synergistic effect. The Strong, Prosperous, and Resilient Communities Challenge (SPARCC) is an example that highlights this paradigm shift from silo to overlapping circles, from isolation to synergy. With a $20 million investment and additional capital, six regions will serve as pilot sites for learning about collaborative approaches at the regional level. The partners engaged will include “leaders from the for-profit, nonprofit, philanthropic, and government organizations working across diverse issue areas such as transportation, community development, racial equity, climate resiliency, and health,” with a goal of promoting integrated outcomes and building capacity to effect systems change (SPARCC, n.d.). Existing funding programs can be leveraged with health and equity principles as a way to award and prioritize funding. For example, California has a cap-and-trade program as one of several strategies to reduce greenhouse gases, and a California legislative requirement allocates a certain amount of funding for disadvantaged communities (CalEPA, n.d.). This type of investment from a climate change program has the direct benefit of promoting health equity.
Role of Philanthropy
The philanthropy sector can use different tools to support communities as they design, implement, and evaluate interventions to achieve health equity. In broad categories, these tools include convening, leadership and capacity development, model testing, topic studies and reports, project and program funding, advocacy support, and social movement building.
Convening is a core strategy for foundations, which may serve the role of a trusted, neutral host in bringing together individuals and organizations from different sectors and disciplines. Most foundations aspire to achieve balance and inclusivity across the broad landscape of community
members and other stakeholders and to support engaging across differences to achieve a common goal.
Leadership development and capacity building is another commonly used philanthropic tool that helps address gaps, especially within the nonprofit sector, though other private and public sectors can and do take advantage of these foundation programs. In the case of community interventions that are inclusive of multiple sectors and the affected community, funding both the capacity of all participants to fully engage and the development of new leaders within communities is essential to creating enduring change that will outlast the funding duration.
Model testing refers to smaller-scale, innovative interventions that, while based on robust theories and other inputs, may not have the evidence base to attract other funding sources such as local, state, and federal government agencies. Foundations can take risks with innovative programming, fund appropriate evaluation, and create the evidence that others require to address the issues of scale and sustainability. For most of the philanthropic sector, this is as close as philanthropy gets to funding empirical research.
Foundations do fund studies of specific topics: specifically, studies that review and synthesize existing knowledge, projects, or data and create reports, position papers, media, and other products that are intended to support and inspire other work. In fact, this report is an example of what foundations can do to promote community interventions.
Another core foundation strategy for community work involves grants made for explicit projects or programs. Such philanthropic grant making can be responsive (involving a cyclical review of unsolicited grants that advance the mission of the foundation) or directive (usually involving a request-for-proposals process where agencies such as community nonprofits apply to complete a scope of work created by the foundation). Some foundations are also using novel approaches involving community engagement to distribute decision making for program and project funding to the communities themselves.
Advocacy funding may present challenges for certain foundations for which funding issue-specific advocacy strategies, such as lobbying, is prohibited by federal tax law. Nevertheless, such foundations can support advocacy groups with general operating funds (as distinguished from program-specific funds) that can be used to lobby, as long as the foundation is not involved with decision making about what issues the advocacy group chooses to take on. Foundations can also support social movement building by providing support for organizations that use community organizing to address important social issues. However, many (if not most) foundations choose not to offer funding in the advocacy and policy arenas, despite the opportunities to create significant, sustainable
change in health equity issues. This pattern may change over time, however, as foundations look for enduring upstream changes in areas that address their mission.
Another area for foundation support is civil rights law. A 2001 report to The Rockefeller Foundation on racial justice with findings and recommendations for funders that are relevant in considering community solutions to achieve health equity suggests that
- Foundation support is needed to expand civil rights and racial justice lawyering to take on injustice while deepening public understanding of the nature and causes of exclusion, including the complexities of race, ethnicity, and class.
- Civil rights and racial justice lawyering can be a powerful tool to strengthen philanthropic efforts across a range of programs. Creative approaches can help create broader constituencies in various foundation areas, including health, education, and community revitalization.
- Funding for organizational capacity is needed to permit the creation of broad networks and the development of sophisticated techniques.
- Strategic funding of national, regional, and local groups can have a substantial impact. Local groups can work for community solutions around the country while connecting with the broader national civil rights community. Support for problem-solving legal strategies can build trust, build partnerships, and empower community leaders speak for themselves. Lawyers can facilitate access to unresponsive institutions and provide legal leverage against unfair practices. Marginalized communities can use local democracy to challenge structures that isolate and impoverish them (Hair, 2001).
Through greater investments in communities of color and low-income communities, foundations can build on the civil rights movement and advance social justice through advocacy and organizing for structural change (Hansen, 2012; Skocpol, 2013). As an example, while strategic foundation support has enabled the success of the environmental justice movement, funding constraints have made it difficult to build organizational infrastructure, community organizing, leadership development, and effective participation in the policy and legal arenas. Reliable, predictable, and flexible multiyear core support for health, environmental justice, and racial equity organizations is necessary for them to carry out their mission, respond to new challenges and opportunities, and serve their communities (Bullard and Garcia, 2015; Joassart-Marcelli, 2010;
Joassart-Marcelli et al., 2011). For a community example of an environmental justice organization that successfully leverages foundation support to build healthier and more equitable communities, see the discussion of WE ACT for Environmental Justice in Chapter 5.
The California Endowment’s Building Healthy Communities initiative offers a noteworthy example of a philanthropic multi-sector intervention to achieve health equity. This 10-year, 14-community strategy has, at its 5-year mark, achieved improved health coverage for the underserved, as grantees and partners fought for and supported the successful implementation of the Patient Protection and Affordable Care Act (ACA) and the expansion of Medicaid in California. There has been a stronger health coverage policy for undocumented residents as grantees and partners successfully crafted and led the #Health4All Campaign,1 paving the way for state-supported health coverage for undocumented children. There have been school climate, wellness, and equity improvements as grantees, partners, and youth have led or supported efforts across the state to reform harsh school discipline and suspension policies, and they continue to work to successfully implement school equity funding formulas. Foundation grantees and partners have lent advocacy support for health- and prevention-oriented justice system reform; a key objective of justice reinvestment is to channel savings from a reduced need for prisons into prevention strategies. Grantees have joined with other coalitions supporting outcome improvement work in young men of color, bringing improved public policy and civic attention to the issue and resulting in the creation of a Select Committee on the Status of Boys and Men of Color in the state legislature. Finally, the Building Healthy Communities initiative has helped grantees in their efforts to enact more than 100 local policies and system changes, ultimately promoting a culture of health in local jurisdictions that emphasizes such community resources as more walkable neighborhoods, fresh food access, park space, and access to safe drinking water.
Recommendation 7-1: Foundations and other funders should support community interventions to promote health equity by:
- Supporting community organizing around important social determinants of health;
- Supporting community capacity building;
- Supporting education, compliance, and enforcement related to civil rights laws; and
___________________
1 For more information, see http://www.calendow.org/prevention/health4all (accessed December 19, 2016).
- Prioritizing health equity and equity in the social determinants of health through investments in low-income and minority communities.
Reliable, predictable, and flexible multiyear core support for health, environmental justice, and racial equity organizations is necessary for them to carry out their missions, respond to new challenges and opportunities, and serve their communities. With available tools, philanthropy can play an important role in supporting community interventions to achieve health equity and should be considered as an important potential partner in this work.
Role of Business
The U.S. business community has a significant stake in correcting health inequities as a strategy for stabilizing and strengthening the U.S. economy. Business contributes positively (or negatively) to health and healthy conditions in several ways: as payers offering their employees health care benefits; as employers who have a role in ensuring workplace health and safety; as producers of goods and services that may have implications for health and well-being; as creators of externalities (e.g., causing environmental impacts through such things as the production of greenhouse gases) or promoters of sustainable technology; and through their philanthropic efforts, as funders of a range of activities that may contribute to improving public health. The various ways that businesses can affect health and well-being also illustrate the multiple pathways for business involvement in promoting health equity: through a focus on health care; through workplace wellness and safety; through corporate social responsibility (e.g., sustainability programs, impact investing of education, and other determinants of health); and through philanthropic endeavors.
Several major U.S. organizations that have addressed employee health for decades, including the U.S. Chamber of Commerce and the National Business Group on Health (NBGH), have in the past several years begun to consider the potential for a wider role for business, beyond workplace wellness and health care insurance, in addressing the social determinants of health and achieving health equity. Analogous to the gradual shift from focusing primarily on health care benefits and how their growing cost affects the corporate “bottom line,” to achieving a better quality of care and better value—including by addressing inequities in health care—there has been an evolution in thinking about worker health and wellness to a greater consideration of the social determinants of health and ways for business to expand opportunity in communities.
Examples of the former include the NBGH Innovation in Advancing Health Equity Award (formerly called the Innovation in Reducing Health Care Disparities Award) and its development of a health disparities cost impact tool and an employer’s guide to reducing racial and ethnic disparities in the workplace (Dan et al., 2011). In 2014 a U.S. Chamber of Commerce event entitled Innovations in Workplace and Community Wellness: Navigating the New Terrain included a session titled The Business Case for Equity of Care, in which Kenneth Thorpe spoke about how gaps in equity present “large human and economic costs” and how non-health factors, including community environments, affect health outcomes and the deep inequities among them.
Examples of the latter—the move toward considering what shapes health beyond the factory or office walls—include several high-profile efforts and reports published over the past 2 years. In a report making the business case for racial equity in Michigan, the author writes of the experience of America’s Edge and ReadyNation, among other business-oriented efforts to expand opportunity, and concludes that “racially-based obstacles to the success of today’s younger generation threaten our economy and security. Tackling these obstacles is not only the right thing to do; it can be a significant driver of our collective social and economic wellbeing” (Turner, 2015). One company that has taken on wellness outside of the office walls is the Rosen Hotels and Resorts, which has shifted its benefits for employees to include college tuition and the construction of a medical center for employees. Rosen has also contributed to funding for a local preschool in a community that was suffering from low graduation rates and high rates of violence.
In 2015 the Vitality Institute published a report that provided support for business leaders’ interest in engaging with communities and others to improve health beyond the company walls. The report illuminated the links between an unhealthy workforce and conditions in their communities of residence. It echoed other research in asserting that the limited investment in disease prevention and social programs and services and heavy investment in treatment has contributed to disparities in outcomes. The authors concluded that “investments in community health have substantial potential to impact the health of the workforce in these sectors, to narrow occupation-related health disparities among working-age Americans, and to reduce the risk that non-communicable diseases pose to the economic vitality of the nation” (Oziransky et al., 2015). Notably, the report called for employer–community partnerships and recommended that employers “engage in strategic philanthropy and use market-driven solutions to create shared value and address health disparities” (Oziransky et al., 2015). Box 7-1 briefly describes a business–community partnership that seeks to improve community health.
Another development in the business sector that can be deployed to engage community-based partners on the topic of collaborative action to improve well being and economic vitality, if not explicitly health equity, is the notion of the triple bottom line (The Economist, 2009): profit, people, planet or achieving balance or harmony among financial, social, and environmental impacts. This notion is conceptually linked with the increasingly popular business sector definition of shared value (Porter and Kramer, 2011) as balancing profit with sustainability and social benefit and the evidence against viewing them as trade-offs (see Chapter 4).
In Capitalism at Risk: Rethinking the Role of Business, Harvard Business School professors highlighted chief executive officer remarks from a series of symposia on capitalism’s greatest challenges (Bower et al., 2011). These include executives’ concern about societal risks that tear the fabric of public trust, such as income and wealth inequality and its effects—exploitation and political and financial instability. Bower and colleagues observed that “health care costs affect the competitiveness of U.S. businesses but also constitute the leading cause of personal bankruptcy, contributing significantly to the burden of low income,” and they added that, in light of these costs, “it is surprising that business has on the whole been so little engaged with the question” (Bower et al., 2011). Business leaders at all levels understand that poor health reduces business
profits, and although they are not necessarily focused on health equity, they are thinking about health and its implications. Bower and colleagues point out that “it is not hard to imagine individual companies, industry associations, or international groups joining in some kind of program to drive widespread attention to these three aspects [smoking, obesity, and substance abuse] of improved health” (Bower et al., 2011). This attention is aligned with acknowledging that smoking, obesity, and drug abuse are the result of health inequities and that in addition to reducing profitability, these inequities widen economic and opportunity inequalities and political polarization that can lead to gridlock and prevent democracy from solving national problems.
To engage local, regional, and national business leaders in addressing health inequities, one effective approach is to discuss the challenges in terms that permit the leaders to participate as partners. This might involve talking about health inequity as weakening workforce productivity, increasing operating costs and hurting profits, and worsening inequality and political polarization. These approaches enable business people to become involved in matters that matter to most to them. Improving health equity enhances the reputations of those businesses involved. If such efforts are pursued constructively and systematically, business leaders will want to be publicly associated with these efforts because they are viewed as being “good for business.” If community leaders and business leaders who are actually concerned about employee productivity, company profitability, and political stability work together effectively, the result will be meaningful improvements that help achieve health equity.
ANCHOR INSTITUTIONS
Many cities in the United States face significant challenges—such as high rates of poverty, high unemployment, and substandard schools—stemming from disinvestment, deindustrialization, globalization, and the related negative impacts on the manufacturing-based economies on which these cities previously relied. Over the past three decades, discussion has evolved on the role of institutions of higher education and medical centers in the economic, cultural, and social fabric of cities (Harkavy et al., 2014; Netter Center for Community Partnerships, 2008). These are only a few of what have been described as anchor institutions.2 Anchor institutions were first described in 2001 (Harkavy et al., 2014) and sub-
___________________
2 Key anchor institutions within a local community include educational, health care, and infrastructure. Additional anchor institutions include local government entities; faith-based organizations; and cultural institutions, such as museums, arts centers, or sports venues (Rubin and Rose, 2015).
sequently “emerged as [a] new paradigm for understanding the role that place-based institutions could play in building successful communities and local economies” (Taylor and Luter, 2013, p. 4). While there are many definitions of anchor institutions, Taylor and Luter note three agreed-upon features of anchor institutions: “anchors are large, spatially immobile, mostly nonprofit organizations that play an integral role in the local economy” (Taylor and Luter, 2013, p. 8). Because anchor institutions are “firmly rooted in their locales” (Norris and Howard, 2015, p. 8) and therefore are considered “sticky capital”—that is, they have “an economic self-interest in helping ensure that the communities in which they are based are safe, vibrant, and healthy” (Serang et al., 2013, p. 4).
Citing arguments by Hodges and Dubb (Hodges and Dubb, 2012), a report by Serang and colleagues defines an anchor mission as “a commitment to consciously apply their long-term, place-based economic power of the institution, in combination with its human and intellectual resources, to better the long-term welfare of the communities in which the institution is anchored” (Serang et al., 2013, p. 5).
Anchor institutions such as universities and hospitals have significant economic, social, and cultural impacts in their surrounding communities (ICIC, 2011). Their relevance for cities is particularly noteworthy: of the 100 largest city cores in the United States, 66 have an anchor institution as the largest employer, and 1 in 8 (about 925) U.S. colleges and universities and 1 in 15 (about 350) hospitals are based in such areas (ICIC, 2011).
Universities and hospitals are powerful local economic engines; they have significant holdings in real estate and expenditures related to procurement for goods and services, endowments, and employment (Norris and Howard, 2015). As shown in Figure 7-1, hospitals in the United States have annual expenditures of nearly $800 billion and nearly $350 billion in purchasing alone, and they employ 5.5 million individuals annually (Norris and Howard, 2015). Annually, the 4,100 universities in the United States educate 21 million students, employ 4 million people, and have more than $400 billion in endowments and $460 billion in economic activity (Harkavy et al., 2014; Snyder and Dillow, 2015). Together hospitals and universities employ 8 percent of the U.S. labor force and account for more than 7 percent of U.S. gross domestic product (Norris and Howard, 2015). Their economic, intellectual, and human capital places anchor institutions in a unique position to improve and enrich surrounding communities in partnership with other key place-based stakeholders from sectors such as government, business, faith, and community-based organizations and local residents. Yet, the economic and social impacts of universities, colleges, and hospitals in their local and surrounding communities can vary, are often undocumented, and contribute to the quality of relationships between such anchors and local residents. A number of scholars
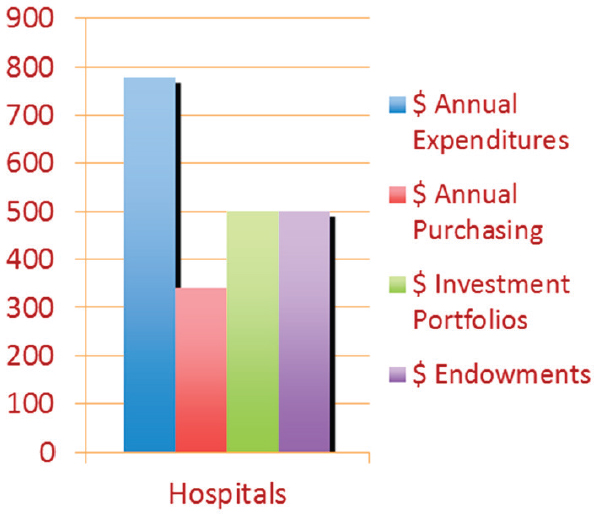
SOURCE: Norris and Howard, 2015.
have written about the often-conflicting relationships between such large organizations and local communities, particularly when local residents do not perceive their communities to be directly benefiting from the presence of such institutions (Martin et al., 2005; Miller and Rivera, n.d.; O’Mara, 2012). Rubin and Rose (2015) have noted that “[m]any anchors have a history of being distant from grassroots communities or of wielding their power and influence in ways that advance their immediate agenda but not that of nearby residents or the broader public” (Rubin and Rose, 2015, p. 2): for example, in terms of their human resources and procurement practices and real estate investments.
Consensus is growing regarding the benefits of such an anchor role. Harkavy and colleagues note that such institutions (1) are affected by their local environment and, as such, have a stake in the health of surrounding communities; (2) have a moral and ethical responsibility to contribute to the well-being of surrounding communities because they can make a difference; and (3) when involved in solving real-world local problems, they are more likely to advance learning, research, teaching, and service (Harkavy et al., 2014).
Becoming an “engaged anchor” (Rubin and Rose, 2015, p. 2) and adopting an anchor mission to implement and assess impacts on local communities requires a conscious and intentional approach in governance (Harkavy et al., 2014). For example, this includes the involvement of leadership from universities and hospitals, including the board of trustees, senior administration, and faculty in developing an operational strategy and new organizational structures in order to produce meaningful change.
Recent initiatives by the National Task Force on Anchor Institutions (NTFAI) (NTFAI, 2010) and the Democracy Collaborative (Democracy Collaborative, n.d.-a) have focused on leveraging the economic power of anchor institutions that reside within or next to low-income communities to improve community conditions and the health and well-being of local residents. While many universities and hospitals have community programs as part of their community engagement and community benefit efforts, the NFTAI-proposed anchor institution approach is different. It focuses on altering traditional anchor institution business practices in order to deploy anchor institutions’ economic power locally to help improve the underlying conditions that shape health. The premise is that hospitals and universities have a unique responsibility and role, along with other anchor institutions (e.g., community foundations, local governments, and key infrastructure services), in helping solve local problems, including those affecting the health of local residents, and that they are uniquely positioned to use their vast economic knowledge and human resources to contribute to the improvement of the quality of life in their local communities. Furthermore, Birch and colleagues “suggest that the entire topic of the university as an engaged, anchor institution is a strategic element of the modern academy (Gaffikin and Perry, 2009) embedded in the practices of university leadership” (Birch et al., 2013).
Using the social determinants of health framework, the NTFAI and the Democracy Collaborative developed a framework, approach, and metrics that universities and hospitals can use to increase their economic investment in the local neighborhoods where they reside and to improve living conditions and quality of life (Dubb et al., 2013). Findings from interviews with anchor institution leaders, partnership directors, staff, and a broad range of representatives from national association and community development groups reveal the influential factors that led to the adoption of an anchor mission and strategy and the challenges related to this. Most importantly, the report outlines a set of equity and community benefits indicators and metrics with which anchor institutions can track their contributions and progress toward goals related to improving community well-being and wealth. A data dashboard was developed that allows anchors to use a shared metric for assessing such progress. The
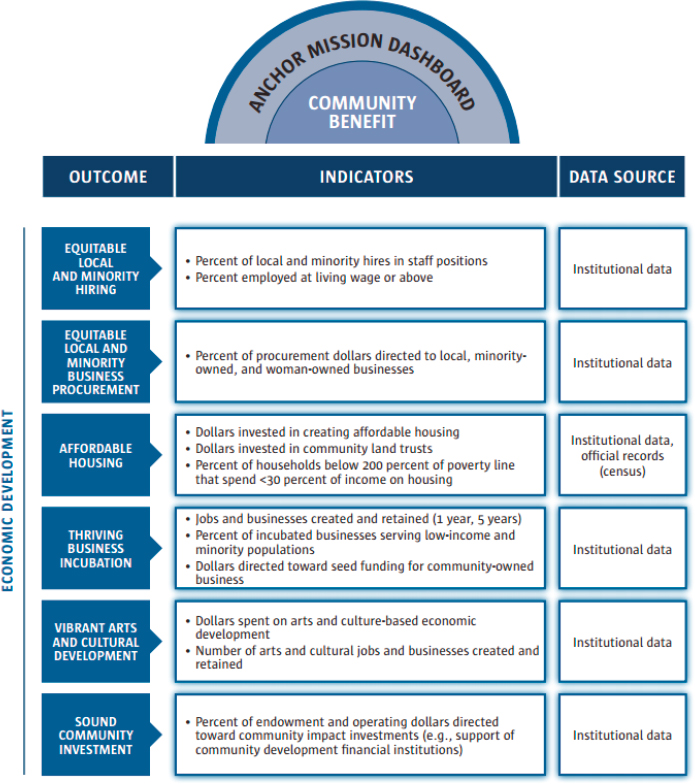
SOURCE: Democracy Collaborative, 2014.
dashboard identifies the desired outcome, indicators, and data sources for community benefits. As shown in Figure 7-2, these are couched in the social determinants of health framework and are highly consistent with the role of multi-sector collaboration and the critical role of community residents. Furthermore, the report highlights the importance of shared value and self-interest as motivating forces for anchor institutions to play an active and strategic role in improving conditions in their surrounding communities.
Six universities (Cleveland State University, Drexel University, the University of Memphis, the University of Missouri–St. Louis, Rutgers University–Newark, and SUNY Buffalo State) are participating in the Learning Cohort to pilot the Anchor Institution Mission and Metrics Dashboard (Democracy Collaborative, 2014). This effort is expected to lead to the identification of lessons learned and evidence-based strategies using a shared framework.
Examples of Anchor Institution Strategies
There are numerous examples of how universities and hospitals have implemented an anchor institution strategy to improve conditions in their local communities, particularly with a focus on the social determinants of health (Rooney and Gittleman, 2015; Rubin and Rose, 2015; Zuckerman, 2013). These new anchor institution approaches (Andrews and Erickson, 2012; Harkavy and Zuckerman, 1999) share a number of the features noted in the model discussed in this report (see Figure 1-3). For example, their focus is well aligned with upstream approaches relevant to the social determinants of health, such as the creation of workforce training and living-wage jobs with good benefits to increase employment among local residents; building wealth and reducing debt among community residents; creating and improving existing affordable housing; increasing community safety and access to safe green space and parks and affordable healthy food; enriching the presence of and participation in the arts; building advocacy and action capacity among community residents and community-based organizations; and engaging multiple private and public sectors in partnerships.
This new paradigm for anchor institution commitment to improve conditions in their local communities differs from past failed efforts. Such past efforts commonly relied only or primarily on government and foundation grants to universities to develop time-limited projects with their cities and communities without any real integration of the work into their institutional mission, culture, and organizational structure (Taylor and Luter, 2013). Treated as an add-on, these projects were not sustainable and are thought to have contributed little to improving local community conditions (Taylor and Luter, 2013).
For example, the Community–Campus Partnerships for Health (CCPH) is a nonprofit membership organization established in 1997 that promotes health equity and social justice through partnerships between communities and academic institutions (CCPH, n.d.). Members view health broadly as physical, mental, emotional, social, and spiritual wellbeing and emphasize partnership approaches to health that focus on changing the conditions and environments in which people live, work,
study, pray, and play. By mobilizing knowledge, providing training and technical assistance, conducting research, building coalitions, and advocating for supportive policies, CCPH helps to ensure that the reality of community engagement and partnership matches the rhetoric (CCPH, 2007, 2012).
As noted in the examples below, anchor institutions can and are playing an important role in uplifting community conditions through a series of multilevel strategies and economic investment. However, an anchor institution approach is not a panacea, especially if it is not combined with an equitable approach to economic development that meaningfully uplifts the living conditions of long-term, poor residents. Without intentional attention paid to equitable benefits from economic development, such efforts risk contributing to gentrification and the displacement of existing poor residents. Thus, at the crux of anchor institution efforts is the challenge of how to improve community conditions without displacement but instead with observable and measureable indicators that living conditions have improved for the individuals and families living in these neighborhoods prior to reinvestment. The following are community examples of anchor institution approaches to improving community conditions and improving health outcomes. Box 7-2 highlights a few examples of institutions applying the anchor approach.
Role of Academic Research Centers
One federal strategy to promote the more rapid adoption of clinical research was the establishment of the Clinical and Translational Science Award (CTSA) program, which initially funded 12 institutions (NCATS, n.d.-a). The CTSA program, has grown and evolved over time to more than 60 organizations, but while funding support for community engagement efforts has decreased over the past few years, engaging patients and communities in every phase of the process of translating research into practice remains a program goal. Members of the CTSA consortium
collaborated in the publication of community engagement principles (ATSDR, 2011) as well as other products that may be useful to communities, such as logic models (Eder et al., 2013) and suggested measures. A 2013 Institute of Medicine (IOM) report reinforced the critical role of community engagement in all phases of research, from basic research to clinical practice and community and public health research, and concluded that these partnerships with patients, family members, health care providers, and other community stakeholders need to be preserved, nurtured, and expanded (IOM, 2013).
Many CTSA program awardees make resources available to community-based organizations and community members through their community engagement activities. The Irving Institute, funded through Columbia University’s CTSA, includes a freestanding community engagement center, the CCPH. From the perspective of university researchers, CCPH supports community-engaged research as well as recruitment and data collection at a convenient place in the primarily Latino community of Washington Heights/Inwood in New York City. However, CCPH also offers resources and services, including free blood pressure screening and meeting space for community-based organizations. (See the description of the community example WE ACT for Environmental Justice in Chapter 5 for information on other Columbia University programs that have fostered local engagement in community research in marginalized neighborhoods of northern Manhattan in New York City.)
Academic organizations funded through the CTSA program (NCATS, n.d.-b) have developed and made available resources that can be used to promote community-based solutions for health equity, such as a health literacy review service and computers for community members to use. The Partnership of Academicians and Communities for Translation (PACT) of the Colorado Clinical & Translational Science Institute includes the PACT Council, which comprises 18 members with equal representation from the university and community, with participants from more than 20 ethnic, geographic, and self-identified communities facing a range of health disparities (Westfall et al., 2013). Two activities are particularly relevant for community-based solutions to achieve health equity. First, more than $200,000 per year is awarded in pilot grants for innovative programs that address health disparities identified by the community. Second, there is a robust educational program aimed at graduate students, researchers, and community members. This includes a seminar series on community engagement as well as the Colorado Immersion Training program, which provides an intensive longitudinal experience for researchers to develop and sustain community-engaged research, including a placement in a local community.
As noted in Chapters 3 and 4, respectively, transdisciplinary research approaches are needed to produce more of the evidence necessary to inform work on health equity, and the knowledge base that communities can draw on today to design solutions to reduce health inequities is not well matched to the challenge (i.e., randomized controlled trials are not a good fit for generating evidence on approaches that address the social, economic, environmental, and structural factors that shape health). An increased knowledge base could inform and guide communities in applying the promising strategies needed to shed light on systems and how to change them, to increase the understanding of complex and interacting initiatives aimed at population-wide change, and to support the work of continuing adaptation to improve outcomes. Yet, longstanding traditions and institutional arrangements have favored a narrow swath of research—research using controlled experimental methods to identify circumscribed programs that have been found to be effective in controlled settings. Therefore, based on the committee’s expertise and its examination of the available evidence, the committee recommends the following:
Recommendation 7-2: A number of actions to improve the knowledge base for informing and guiding communities should be taken, including
- Public and private research funders should support communities and their academic partners in the collection, analysis, and application of evidence from the experience of practitioners, from leaders of community-based organizations, and from traditionally underrepresented participants who are typically left out of such partnerships.
- Universities, policy centers, and academic publications should modify current incentive3 structures to encourage and reward more research on the social distribution of risks and resources and the systematic generation and dissemination of the evidence needed to guide the complex, multi-faceted interventions that are most likely to reduce inequities in health outcomes.4
___________________
3 Such incentives may include funding, publication standards, and rules governing tenure.
4 SQUIRE (Standards for Quality Improvement Reporting Excellence) is an example of concerted efforts by leaders in one sector—health care—to change powerful incentives. The SQUIRE guidelines provide an explicit framework for reporting new knowledge about system-level work to improve the quality, safety, and value of health care in the hope of shifting the emphasis and rewards from a near-exclusive emphasis on experimental findings to examining interventions closely, carefully, and in detail; generating important new knowledge about systems of care; and learning about how best to change those systems (Davidoff and Batalden, 2005).
- Academic programs should promote the development of and dialogue on theory, methods, and the training of students to create a more useful knowledge base in the next generation of researchers on how to design, implement, and evaluate place-based initiatives to improve community health.
Regarding the final bullet in Recommendation 7-2, such programs would contribute to preparing population health researchers and practitioners to advance knowledge that leads to improved population health science. These future researchers will need to address several questions, such as
- Through which modifiable mechanisms do community-level factors affect health directly and indirectly? And for which populations and what health conditions?
- Which policy and community-level levers are the most powerful, feasible, and sustainable for improving health in varied community settings—and for what health conditions?
- What have been promising approaches for place-based interventions, and what methodological challenges have they faced in documenting change at the population level and scaling up?
- What is the role of social capital, collective efficacy, community organizing, and the empowerment of community residents as agents of change for improving community conditions in place-based interventions? And what effective or promising approaches have been used?
- How and under what circumstances can researchers and community-based organizers best partner with each other, and what are the most effective community organizing strategies to promote health equity?
- What is the role of anchor institution policies and practices, including for colleges and universities, within poor neighborhoods in contributing to improving community conditions and fostering health equity? What are the pros and cons of various campus-community partnership models? What evidence exists regarding the efficacy and impact of these partnerships on the factors that affect health and health outcomes among local poor communities? (Smedley and Amaro, 2016)
Hospitals and Health Systems
Hospitals and health care systems share in the responsibility to improve health equity. The American College of Healthcare Executives,
the American Hospital Association (AHA), America’s Essential Hospitals, the Association of American Medical Colleges, and the Catholic Health Association of the United States have urged all hospitals to “take the #123forEquity Pledge to Eliminate Health Care Disparities” (AHA, n.d.-a). The AHA provides a tool kit (AHA, 2015) and other resources (AHA, n.d.-b) for hospitals that pursue the #123forEquityPledge.
In a review of the literature and interviews with leaders of health care organizations, the Institute for Healthcare Improvement (IHI) outlines practical steps and a conceptual framework for guiding health care organizations that want to begin a journey to improved health equity. The IHI stresses the importance of “making health equity a strategic priority at every level of an organization, especially at the top” (IHI, 2016, p. 4) and outlines a number of concrete ways for health care systems to get started. The paper offers a framework for change and a self-assessment tool for health care organizations to assess their current state on each component of the IHI framework. In the IHI and AHA materials, hospitals are urged to start their health equity journey by looking at practices within their own institutions, with the stated goal of “dismantling the institutional racism and implicit biases that hold us back” (IHI, 2016). The AHA equity-of-care tool kit highlights the steps that hospitals can take—starting with leadership—including better collection and use of data on race and ethnicity, cultural competency training, and increasing diversity in governance and leadership (AHA, 2015). Key components of the IHI framework are outlined below:
- Begin quality improvement work by considering the needs and issues faced by populations experiencing worse health outcomes and the greatest disparities in the social determinants of health.
- Tailor quality improvement efforts to meet the needs of marginalized populations across the continuum of social determinants of health.
- Include traditionally disenfranchised people in health care transformation efforts and in advisory positions.
- Use the required community health needs assessment (CHNA) as an opportunity to pursue health equity issues in a more coordinated approach with other hospitals and diverse stakeholders committed to advancing health equity (see Box 7-3 for a brief overview of CHNA for charitable hospitals).
- Provide cultural competency education within the institution and in the community.
- Procure supplies and services from women- and minority-owned businesses and use hiring practices that promote diversity and
- Increase access to health care and human services which includes, among other things, building health care facilities in underserved communities.
inclusion; increasing diversity in hospital leadership and governance is especially important.
Hospitals also need to commit to looking beyond the walls of their institutions to address the root causes of poor health that are situated outside hospitals; the primary causes of growing health disparities in the United States do not begin in a doctor’s office, and place heavily influences health (see Chapters 2 and 3). To truly advance health equity in the community, hospitals must also have a strong focus on improving the places where people live and work and where children learn and play.
Hospitals are well positioned to help lead multi-sector work aimed at advancing health equity. For example, hospitals are often trusted health leaders in the communities they serve. Nonprofit hospitals are already required to conduct CHNAs (see Chapter 6), a task that could be conducted with a health equity focus. For example
- Bon Secours in Baltimore and Virginia has partnered with community organizations to develop low-income housing.
- Catholic Health Initiatives, a health care system based in Denver, requires all of its hospitals to address one community-identified issue related to violence prevention.
- Our Lady of the Lake Hospital in Baton Rouge has a robust program of school health clinics that includes physical, dental, and mental health. The purpose of the program is to improve school attendance and to ensure that children are ready to learn.
- Presence Health in Chicago is partnering with Catholic Charities and others in the community to form an accountable health community and will be identifying and addressing issues related to social determinants.
- Innovations in the use and sharing of data are increasingly used to bring partners together across the social determinants of health to highlight connections, create a common language, and monitor progress across various sectors (e.g., see the Camden Coalition of Healthcare Providers5).
Moreover, as anchor institutions, hospitals are deeply rooted economic engines in the communities they serve, holding significant social capital and controlling vast amounts of real estate and other financial investments (see the section on the role of anchor institutions in this chapter). By leveraging their economic power, good will, and human resources, hospitals can make significant advancements in health equity. The role of hospitals is explored further in the discussion of anchor institutions below.
Community health centers and federally qualified health centers (FQHCs) have long played a role in providing primary care services to underserved populations, including uninsured and underinsured individuals and families (for a summary of the first rural FQHC, Delta Health Center, see Chapter 5). A 2010 report on FQHC partnerships with local health departments described “promoting health equity and eliminating health disparities” as one goal of such partnerships (Zakheim et al., 2010).
In 2015 the National Association of Community Health Centers (NACHC) implemented the Protocol for Responding to and Assessing Patients’ Assets, Risks, and Experiences (PRAPARE), a national effort to help health centers and other providers collect the data needed to better understand and take action on their patients’ social determinants
___________________
5 For more information, see https://www.camdenhealth.org (accessed December 19, 2016).
of health.6 The PRAPARE Core Measures include, in addition to race, ethnicity, and education, housing status and housing stability, migrant and seasonal farm worker status, material security, transportation, social integration and support, and stress. The PRAPARE tool is being used with different electronic health record systems and in different settings (NACHC, n.d.-b).
Anchor Institution Approaches
Anchor institutions, including universities, hospitals, and other entities discussed earlier in this chapter, that are located in low-income communities have an important role to play in improving local economies and the community conditions that affect health. The anchor institution approach of an articulated mission, strategies, and metrics to improve community conditions has gained increasing attention and buy-in in a number of major metropolitan areas. Such organizations have made significant investment, usually with a number of other anchor partners, including city government and, often, private investors. Data on how such efforts have improved the living conditions of long-term and poor residents are not yet available.
Yet, a number of the anchor investment areas have evidenced gentrification and displacement, and often local residents question whether long-term and poor residents have benefited compared to the benefits gained by anchor partners and wealthier residents who have moved into the areas. Thus, while anchor investment areas are promising, a major remaining challenge for anchor institutions is whether in fact they can improve the quality of life for low-income residents in their surrounding neighborhoods. This will require keeping a careful eye on the development of community initiatives that equitably benefit long-term and poor residents of their surrounding communities.
An alternative to the traditional approach to economic development described by the Democracy Collaborative focuses on community wealth building (Kelly and McKinley, 2015). Figure 7-3 shows the drivers of community wealth and the differences between traditional and community wealth-building approaches to economic development. Figure 7-4 shows six strategies for the wealth-building approach. The wealth-building approach does not assume that economic development will result in “trickle down” benefits to local residents and instead employs and builds
___________________
6 “PRAPARE has been a multi-year effort between NACHC, the Association of Asian Pacific Community Health Organizations, the Oregon Primary Care Association, and the Institute for Alternative Futures, along with a group of pioneer health centers and health center networks in Hawaii, Iowa, New York, and Oregon” (NACHC, n.d.-a).
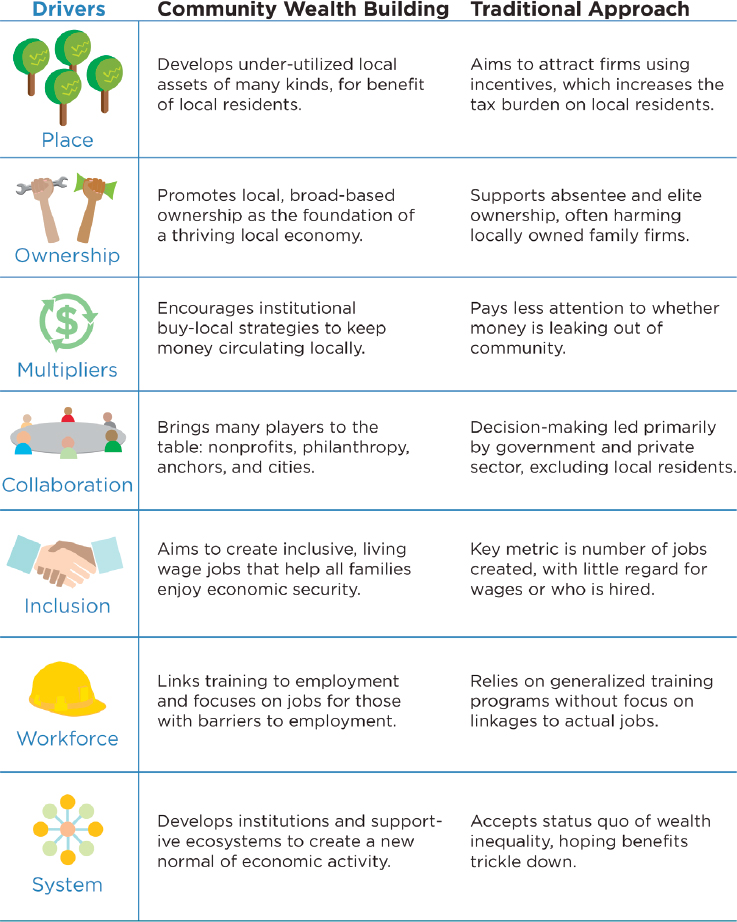
SOURCE: Kelly and McKinley, 2015.
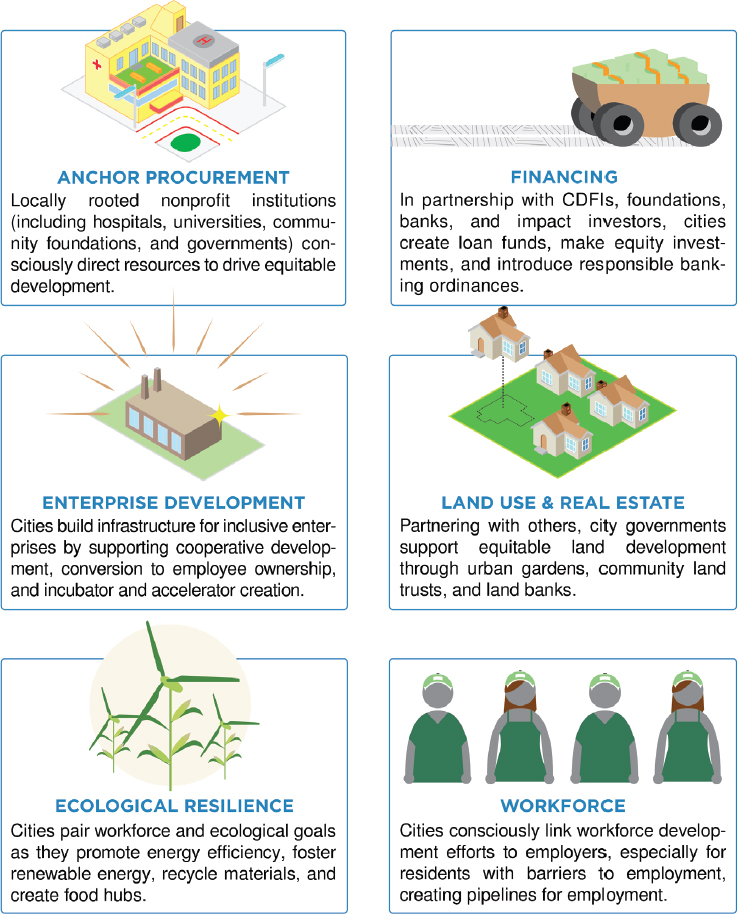
NOTE: CDFI = community development financial institution.
SOURCE: Kelly and McKinley, 2015.
on existing assets within the local community to build sustainable ecosystems that promote equity and provide direct benefit to local residents. This is the real distinction between wealth-building and more prevalent market-driven approaches that can be part of more traditional anchor approaches to development.
The concept of shared value discussed above also offers another approach to the traditional anchor approaches to community and/or economic development. Porter (2010) has described how anchor institutions should view community viability as a critical driver of an anchor’s long-term success in workforce hiring, recruitment, and quality of life, and asserted that when anchors make progress working with communities with the greatest need, that can help create “the greatest shared value” (Porter, 2010).
Conclusion 7-1: Based on its judgment and its review of community-based efforts to promote health equity or address the determinants of health, the committee concludes that community-based innovations are often most effective when they build on efforts of various community entities (e.g., foundations, anchor institutions) with an existing foundation or body of work and a strong presence in the community.
Recommendation 7-3: The committee recommends that anchor institutions (such as universities, hospitals, and businesses) make expanding opportunities to promote health equity in their community a strategic priority. This should be done by:
- Deploying specific strategies to address the multiple determinants of health on which anchors can have a direct impact or through multi-sector collaboration; and
- Assessing the negative and positive impacts of anchor institutions in their communities and how negative impacts may be mitigated.7
The literature on institutional racism and implicit bias and effects on health equity is generally focused on health care organizations and settings. Little or no evidence is available for other kinds of anchor institutions (aside from scholarship on racism and bias in academia, although not as anchor institutions or in the context of the production of health inequities). Based on the evidence and examples available from health care, however, and with the support of emerging tools on equity, diversity, and inclusion,8 anchor institutions could develop a structure and
___________________
7 See, for example, McNeely and Norris (2015).
8 See examples outlined in NASEM, 2016b.
processes to identify and decrease institutional racism and implicit bias within their own institutions to enable them to evaluate their roles and engage with communities more effectively.
OTHER COMMUNITY-BASED PARTNERS
The Role of Faith Organizations
Faith organizations are often a key partner in advocating for and developing or providing health care services as well as in addressing the social determinants of health. Faith organizations are often the entities where issues are first identified at a point when they can be dealt with at a much earlier and resolvable stage. A community of caring and competent volunteers can be mobilized to address the community’s needs and to advocate for appropriate legislation and the use of civic resources—including food, shelter, pregnancy care, child care, respite, elderly care, and addiction care—to address health equity (e.g., see a summary of work by ISAIAH, a faith-based community organization, in Box 7-4). Health care providers can be a partner and resource for the many faith communities in their service area. Whether for dental care, opioid addiction, advanced care planning, or domestic abuse, partnering with faith communities can be invaluable, as they often have the most confidence of and credibility with their communities (Schroepfer, 2016). Examples of faith organizations engaging in work to achieve health equity in their communities include the Health Ministries Association, Inc. (HMA, n.d.), the Maryland Faith Health Network (Health Care for All, n.d.), and the Methodist Healthcare Center of Excellence in Faith & Health (Methodist Healthcare, n.d.).
Almost all faith organizations are clear that in addition to preaching the doctrines of their faith, a critical call is to provide service for those in need and those most vulnerable. With their unique position in the community, they have the ability to be invaluable in achieving health equity.
Community Development Corporations
Community development corporations (CDCs) are nonprofit, community-based organizations focused on revitalizing the areas in which they are located, which are typically low-income, underserved neighborhoods that have experienced significant disinvestment (Democracy Collaborative. n.d.-b). The CDC movement is 45 years old, and the Democracy Collaborative reports that more than 4,000 CDCs across the United States engage in a variety of communities, including those with high proportions of racial and ethnic minorities (Democracy Collaborative, n.d.-b). Historically, the emphasis of CDCs has been housing, but today the functions and
services of CDCs vary widely, with some also offering direct health services. The work of the Thunder Valley CDC, for example, is summarized in Chapter 4. Additional examples below highlight the variety of CDC activities taking place.
Chicanos Por La Causa, Inc. (CPLC) is one of the largest Hispanic CDCs in the United States (CPLC, n.d.). For more than 40 years, CPLC has focused on building stronger, healthier communities by providing the political and economic empowerment that supports individuals to learn the skills and develop the resources necessary to become self-sufficient. Funded through a grant from the Helios Education Foundation, a new program in Arizona focuses on helping 2,000 Hispanic parents develop literacy and advocacy skills related to education and health services. Through the Northern New Mexico Food Hub, Siete Del Norte, a subsidiary of CPLC, is working with community partners to assist local farmers to access commercial markets and make local produce more readily
available in rural New Mexico. Health services are provided through multiple CPLC components.
Since 1975 the East Bay Asian Local Development Corporation (EBALDC) has invested more than $200 million in assets in Oakland and the greater San Francisco East Bay area with a primary emphasis on housing options, social supports, and income and wealth (EBALDC, n.d.). Recently, EBALDC has developed and implemented a healthy neighborhood framework for assessing each potential project, program, and partnership for its potential to bring resources and opportunities that will enable the people who live there to make choices that lead to healthy and vibrant lives. This healthy neighborhood framework also informs assessments of the needs of particular communities as well as the particular approaches to be applied. While the primary emphasis areas remain consistent across activities, special attention is focused on other needs of the community, based on the assessment. EBALDC’s work will be complemented by collaboration with local businesses on nearby commercial corridors to improve the business environment, create good jobs, and support business development in the neighborhood.
The Quitman County Development Organization (QCDO) was established in 1977 by a group of African American community activists with a history of engagement in the civil rights movement (QCDO, n.d.). Toward the overall goal of improving the quality of life in northwest Mississippi, QCDO has developed affordable housing, owns a community credit union, provides grants to churches for economic development projects, and engages in a variety of child care social services programs and micro-enterprise lending. A number of activities target early childhood. For example, the Raising a Reader program targets children 3 to 5 years of age to assist with early language development. In addition, the program equips parents with the skills and knowledge to successfully support their children’s growth in reading and language through monthly parent meetings, monthly classroom readings, the provision of books for reading to the child, and parental tracking of books read to the child.
ROLE OF GOVERNMENT
Policy Makers and Elected Officials
Policy makers may be elected officials such as members of city councils or of municipal, county, or school boards; state legislators; mayors and governors; members of Congress; and the president of the United States. Policy makers also include policy and other staff at different jurisdictional levels and in different types of agencies and departments. Policy makers
in a specific sector range from the local (e.g., zoning) to the national policy level (e.g., implementers of the Fair Housing Act).
Local policy decisions may have untoward effects that create conditions that contribute to health inequities. The IOM identified the role of policy as a determinant of health in its report For the Public’s Health: Revitalizing Law and Policy to Meet New Challenges (IOM, 2011). The report provides examples of various policy decisions across sectors that can have impacts on health. For example, land use decisions can shape the physical environment (e.g., building freeways that divide neighborhoods) and agricultural policy can impact the food environment (e.g., corn subsidies contributing to poor diets) (IOM, 2011). There is also research that suggests that policy decisions can have a disproportionate impact on underserved populations. Fullilove and Wallace (2011) examine historical policies such as segregation, redlining, and urban renewal and their effects on minority populations. The displacement of these groups has been linked with violence, family disintegration, substance abuse, sexually transmitted diseases, and stress (Fullilove and Wallace, 2011). The committee finds that policy makers, discussed throughout the report, can play a significant leadership role to promote health equity.
Recommendation 7-4: The committee recommends that local policy makers assess policies, programs, initiatives, and funding allocations for their potential to create or increase health inequities in their communities.
Policy makers and government executives can help spur innovations in connecting the dots for health equity, as in the case of geospatial data that can highlight associations. As an example, the city of Fresno, California, facilitates the collaborative Fresno Community Health Improvement Partnership to build a Health Priority Index, which looks at places that bear the highest burden of disease and serves as a starting point to think about policy, systems, and environmental change. This multi-sector network uses data as a point of conversation for shared priorities and decision making, bringing together city staff, the public health department, community members, planners, and community-based organizations.9
Centers for Medicare & Medicaid Services
Addressing unmet needs in the social determinants of health, such as food, housing, and social services, has gained momentum and interest among payers. For example, the Centers for Medicare & Medicaid
___________________
9 For more information, see http://www.fchip.org (accessed December 21, 2016).
Services recently developed an innovation project, “accountable health communities,” that required screening patient populations for unmet needs and referring them for services. Participating health care institutions were required to demonstrate linkages with local resources and joint planning. As part of the program, a common screening tool will be developed. A broad social-determinants-of-health lens would require comprehensive screening across many areas, including housing, food security, employment, transportation, and education. It would also elicit consumers’ desire for assistance. Various tools along these lines have been developed in pediatrics.
Some evidence-based models exist that rely on screening and referral. In addition, there are pediatric models that embed intervention services related to social determinants of health (reading, early childhood education, and advocacy) within clinical settings. At times the referral is combined with dedicated staff, such as community health workers, patient navigators, or case managers, who refer and also facilitate linkage with available community programs (Shah et al., 2014). One challenge with broad screening programs is that they require maintaining up-to-date program and contact information for local private and public agencies. Another is the need to provide training at the screening site concerning sensitive screening, avoiding stigma, and broadening knowledge across the areas of need. Finally, screening programs can fail if resources in the community are not available to address identified needs, leading the screening to be both inefficient and ethically questionable.
Public Health Agencies
Public health agencies throughout the United States are focusing attention and resources on addressing health equity (e.g., the theme of the 2016 National Association of County and City Health Officials’ [NACCHO’s] annual meeting, “Cultivating a Culture of Health Equity,” and the 2016 Association of State and Territorial Health Officials President’s Challenge, “Advancing Health Equity and Achieving Optimal Health for All”). Addressing health equity will require the intentional investment of resources and support in the communities and populations with the greatest need. This approach is not new to state and local public health agencies accustomed to using infectious disease data to guide their investments in prevention and treatment measures to the highest risk individuals and communities. As an example, the number of newly diagnosed HIV infections decreased 19 percent from 2005 to 2014 (CDC, 2014), and reductions in the morbidity, mortality, and health care costs associated with vaccine-preventable diseases from 2000 to 2010 have been included among the top 10 public health achievements for the decade
(CDC, 2011). Public health agencies are working to adapt such approaches to address the non-health factors that shape health outcomes, including education, transportation, housing, and employment opportunities, and to exchange data with the traditional and nontraditional partners that are primarily responsible for addressing these social and economic factors. In addition, public health agencies will need to access other, nontraditional public health data sources on the social determinants of health as they continue to work in this area. Data on indicators such as high school graduation rates, poverty levels, affordable housing availability, median family income, unemployment rates, and limited English proficiency could be considered core public health data.
Public health agencies have the unique ability to use population-based health data to identify health priorities and health disparities; to inform and help mobilize the community and stakeholders to address health priorities; and to evaluate and monitor the health effects of new policies, programs, and changes to the built environment. Several public health agencies have prioritized addressing health equity in their community health plans (City of Chicago, 2016; OpenData KC, 2016). In March 2016, the Chicago Department of Public Health launched Healthy Chicago 2.0, a citywide plan that was developed and will be implemented in collaboration with representatives of more than 130 organizations across a broad range of sectors with the primary goal of achieving health equity (City of Chicago, 2016). NACCHO has developed a health equity and social justice program10 to build the capacity of local health departments in confronting the root causes of health inequity, including resources such as a tool kit and a Web-based course for the public health workforce (NACCHO, 2016).
Because of existing relationships, public health agencies may be the natural conveners of certain health equity stakeholders, including health care systems, community organizations, and health insurance companies. They can also be partners with or conveners of community development organizations, faith-based organizations, businesses, and other governmental agencies (e.g., transportation, housing, education) because public health agencies have the data needed to link nontraditional partners’ work and interests to health and to share with them evidence-based approaches. Box 7-5 highlights a few examples of public health agencies as conveners or partners. In recent years, due in to part to the evolution of public health accreditation standards (PHAB, 2013), many public health agencies have invested in the staff and training required to support community engagement for addressing acute or emerging health issues as
___________________
10 For more information, see http://www.naccho.org/programs/public-health-infrastructure/health-equity (accessed October 21, 2016).
well as ongoing public health priorities. Some innovative public health agencies have even invested in staff who can provide capacity building assistance to communities too.
As organizations initiate efforts to address health equity, public health agencies should be engaged in the early phases of plan development. Public health agencies can contribute data, epidemiologic expertise, partnerships, and community engagement capacity in addition to commitments to achieving health equity.
Public health agencies can hire staff who have community development knowledge and experience. In addition, public health agencies and health care systems should tap into the expertise of community development organizations (e.g., community development organizations, community development financing institutions) when creating their community health plans.
As local jurisdictions start to come together to address the underlying social determinants of health, many of the legacy structures that continue
to influence social issues will need to change, and change, although disruptive, can lead to greater effectiveness. In both Boulder, Colorado, and San Diego, California, housing and health departments have come together in recognition that health equity is difficult to achieve if homelessness or housing insecurity is a major issue (Quinn, 2016). Creating new ways to provide services is not only achievable through merging departments to create a more efficient system; it can also happen through how funding is allocated toward improving conditions related to the social determinants of health. Lead poisoning, poor housing conditions that exacerbate asthma, and physical risk from poor housing structures are physical environment factors that directly affect health and that disproportionately affect the health of vulnerable populations. The funding streams available to remediate such a problem can be complicated to apply for, and often there is a need to go through several funding sources and applications. Although there are co-benefits from retrofitting a house (e.g., energy efficiency, better health from addressing asthma triggers), funds are separated even if the retrofit achieves multiple benefits. The Green and Healthy Homes Initiative has been able to braid funding from federal, state, private, and philanthropic partners to address housing and health issues in a more holistic way (GHHI, n.d.). For a community example that addresses housing and health with a multi-sectoral approach, see the discussion of People for Sustainable Housing in Chapter 5.
In early 2016 the Governance Institute convened the first in a series of intensive trainings as part of Alignment of Governance & Leadership in Healthcare: Building Momentum for Transformation. The training, which will recur, was designed to orient health care delivery system executives to the potential of interfacing and partnering with the community development sector. Moreover, the Build Healthy Places Network, the Center on Social Disparities in Health, and the Robert Wood Johnson Foundation (RWJF) have put forward “Making the Case for Linking: Community Development and Health,” a brief highlighting multiple models and examples of health and development sector partnerships from around the country (Edmonds et al., 2015).
Recommendation 7-5: The committee recommends that public health agencies and other health sector organizations build internal capacity to effectively engage community development partners and to coordinate activities that address the social and economic determinants of health. They should also play a convening or supporting role with local community coalitions to advance health equity.
The Role of the Educational System
Schools and school systems have not typically thought of public health and health care professionals as potential partners in their efforts to confront the nonacademic aspects of low educational achievement, especially in the context of their required efforts to conduct needs assessments and develop school improvement plans. However, there are many potential stakeholders on which schools could rely for advice and support. Public health departments, managed care organizations, public health–focused community organizations, and others can serve as partners in assessing health needs and have an influence on educational success. Schools can go further by engaging both district-employed and contracted specialized instructional support personnel, union officials, and other community-based organizations as part of their efforts to assess and meet student needs, especially those related to health and wellness.
Community engagement and the partnerships that may emerge as a result are likely to affect educational outcomes as well. There are numerous examples of schools where well-conceived and well-coordinated partnerships appear to have affected both the physical and the mental health needs of student and academic achievement (Frankl, 2016). Although the strength of the evidence underlying these examples varies widely, as does the scale of these partnerships, there is reason to believe that the observed positive educational effects are related to the care with which these partnerships have been built (Freudenberg and Ruglis, 2007). High-quality community engagement is essential across all grade levels—early childhood, elementary grades, and high schools (ICF International, 2010; Legters and Balfanz, 2010; Sigler, 2016). Engaging low-income families is challenging for a variety of reasons, not the least of which is that all too often these are people who have had negative experiences with schools and school systems (Mitchell, 2008). Other factors range from logistical issues associated with the parents’ or guardians’ ability to get to schools, to social and cultural factors having to do with their ability to effectively navigate the organizational dynamics of schools, especially for schools that are not deliberately focused on family involvement (Hornby and Lafaele, 2011). See the description of the Eastside Promise Neighborhood in Chapter 5 for an example of a low-income community that seeks to improve both health and educational outcomes.
Another approach to the role of schools in health equity interventions is to address education and health disparities by focusing on health problems that are widely present in communities, for which there are strong linkages to academic success, and for which community-based intervention is possible. Basch suggests that it is important to think in terms of causal pathways, plausible explanations for why a particular health problem would cause a negative educational outcome (Basch, 2011). He
identifies a variety of educationally relevant health factors, ranging from vision impairment, asthma, and dental disease to aggression and violence, nutrition and obesity, and sexual health issues, which taken together are likely to negatively affect educational opportunities and learning outcomes.
Collecting data on health determinants and health indicators as part of local needs assessments would help in the identification of health problems that affect student learning and achievement. The Every Student Succeeds Act11 is a new federal mandate that requires school-level needs assessments, although access to quality data may persist as a barrier. A forthcoming health impact assessment conducted by the Health Impact Project (a joint initiative of the RWJF and The Pew Charitable Trusts) highlights the need to collect student-, household-, and community-level data on social determinants of health that influence student achievement (Morley, 2016). Unfortunately, not all schools have good data on chronic absenteeism, for example (Balfanz and Byrnes, 2012). Nor is information on school climate and neighborhood or on the community factors that affect learning widely available. The Health Impact Project’s health impact assessment discusses that data on some community factors already being collected by local public health departments, hospitals, and other agencies and organizations can be examined as part of school-level needs assessments (Morley, 2016). Inclusion of such data in the development of school improvement plans can help to identify and build community partnerships beyond school settings to further improve student health and academic achievement as well as school performance (Morley, 2016). See Chapter 6 for a recommendation (Recommendation 6-2) on state department guidance for student health needs assessments.
Household and community factors figure prominently in educational outcomes and could be addressed through community-based education efforts. Neighborhood and household poverty have effects on the social, emotional, and physical resources available to children. Research indicates that violence gives rise to higher risks of posttraumatic stress and negative effects on school functioning (McGill et al., 2014). Housing instability creates attendance problems as well as affects the ability for sustained exposure to specific teachers and schools. Child welfare policies often exacerbate discontinuities in schooling. Other factors being equal, the more these neighborhood and household factors can be understood and addressed in concert with school efforts, the more likely it is that both health and educational outcomes will improve.
___________________
11 S.1177—Every Student Succeeds Act. Public Law 114-95 (December 10, 2015), 114th Cong.
Mounting evidence suggests that focusing on measures of student engagement—especially those that have to do with sense of self, self-regulation, social awareness, and self-efficacy—both foster a sense of wellbeing in students and promote learning (see Dweck et al., 2014; Miyake et al., 2010). However, schools will need to broaden how they currently think about success for these measures to make sense. Schools might also have to adopt new data collection strategies, such as student and parent surveys, to generate this type of information. The CORE districts, a network of urban school districts in California, have developed such an instrument to collect data on factors they view as important indicators of student success (CORE, 2016).
Focusing on measures of school conditions may be another way to generate information about emotional well-being and learning. The research base about school climate and culture is substantial and suggests that in addition to leadership and instructional coherence, strong and trusting relationships among adults and between adults and students matter greatly to school and student success (Bryk et al., 2010). This, too, might require extra effort for school officials, but, given the evidence, it offers great potential in terms of improving the conditions for learning and student well-being. A School Quality Review Guide for the New York City Public Schools includes survey data on New York City schools’ climate and culture (NYC Department of Education, 2016).
Measuring suspension and expulsion rates would give schools a sense of whether their disciplinary policies are excluding students from learning opportunities. Similarly, collecting and analyzing data on absenteeism is an important way to examine opportunities for students to learn. Given the emerging evidence, better data on absenteeism may be critical to addressing health and learning. Irregular attendance is often a function of underlying health factors and is correlated with credit accumulation in middle and high schools (Balfanz and Byrnes, 2012). Children who are chronically absent in the early grades are much less likely to read at grade level, and whether a young child reads at grade level in turn predicts academic performance at the middle and high school levels (Chang and Balfanz, 2016; Ginsburg et al., 2014). See Chapter 6 for more on the role of education at the federal and state levels.
Recommendation 7-6: Given the strong effects of educational attainment on health outcomes and their own focus on equity (ED, 2016), the U.S. Department of Education Institute for Educational Science and other divisions in the department should support states, localities, and their community partners with evidence and technical assistance on the impact of quality early childhood education programs, on interventions that reduce
disparities in learning outcomes, and on the keys to success in school transitions (i.e., pre-K and K–12 or K–12 postsecondary).
Providing federal assistance to advance early childhood education programs is likely to provide many benefits for health equity because the evidence shows that disparities in development and achievement emerge early in the life course (Heckman, 2011), and thus this is a critical phase at which to intervene (Conti et al., 2011). Furthermore, this would leverage an already existing effort, as the U.S. Department of Education has committed to promoting the use of data to advance equity in the fiscal year 2017 (ED, 2016). There are potential limitations with the availability of evidence on reducing disparities in learning outcomes beyond early childhood and elementary levels. Additionally, the state of evidence on racial and ethnic minorities for whom English is not the first language needs to be taken into consideration. Otherwise, efforts to promote equity could unintentionally be hindered.
Role of Law Enforcement and the Justice System
It is increasingly clear that an important focus for community interventions should be building trust between law enforcement and local communities. The final report of The President’s Task Force on 21st Century Policing highlights trust as the cornerstone for just and efficient law enforcement and community safety (The President’s Task Force on 21st Century Policing, 2015). Yet, concerns about police brutality, bias, and a lack of accountability severely undermine trust in law enforcement, especially among racial and ethnic minority communities. Partnering with law enforcement agencies is essential to building trust between law enforcement and local communities.
One mechanism for building trust between law enforcement and local communities is community policing, which is based on the philosophy that police departments can join forces with the communities they serve to determine problems and identify solutions aimed at prevention and intervention (Skogan, 2006). In theory, proactive strategies that are implemented with a community policing approach address the proximal conditions that engender public safety issues such as crime, social disorder, and fear of crime (Bureau of Justice Statistics, 2016). Community policing can lead to greater permeability and interdependence between departments and communities (Gill et al., 2014). Building sufficient trust for effective community policing requires that police get to know residents, which can be achieved through police–resident social events, community gatherings, and public hearings.
The National Academies’ Committee on Proactive Policing–Effects on Crime, Communities, and Civil Liberties in the United States12 is conducting a study that reviews the evidence on the effects of various forms of proactive policing, including community policing. The review includes an assessment of proactive policing approaches and their effects on crime and disorder, discriminatory application, legality, and community receptiveness.
Specific strategies for community policing vary. One strategy to improve community oversight is the civilian review board, a mechanism by which community members can review police conduct (Finn, 2001). Although civilian review boards were a major focus of the civil rights movement, only some communities successfully convinced local governments to pass legislation establishing civilian review boards, which differ markedly from one another in form, structure, potency, and level of authority (Dunn, 2010; Harris, 2005).
Another approach to community policing is to achieve racially and ethnically representative police departments. Research suggests that communities have greater levels of trust in law enforcement when police demographics mirror the community (DOJ, 2015, 2016). This is rarely the case, however, as the proportion of sworn officers who are white is typically much higher than the proportion for the communities they serve (DOJ, 2015, 2016).
The predominant theory for why some communities have more violence than others centers on the differing capacity of communities to come together to control crime (Sampson, 2012). Communities experience different organizing against crime: some are able to come together and use their resources to control unwanted criminal elements, while others are less effective. Typically, able communities have greater financial resources and are relatively stable (i.e., residents have lived in the community for a long time and thus tend to know each other and have a vested stake in the community). These structural conditions—resources and stability—create conditions under which residents are more likely to agree on what constitutes a crime problem and under which they can work together to control crime via informal and formal means. Formally, residents will call the police when crimes are witnessed and otherwise work to develop positive relations with the police. Informally, they rely on healthy social capital and networks to transfer information and social control. For example, in a neighborhood where a resident knows his or her neighbors and feels a sense of belonging and attachment, he or she is more likely to recognize unwanted behavior as suspicious (e.g., a group of teenagers lurking in an
___________________
12 Report forthcoming in 2017. For more information, see http://sites.nationalacademies.org/DBASSE/CLAJ/CurrentProjects/DBASSE_167718 (accessed December 2, 2016).
alleyway), notify other residents, or call the police. This is an example of collective efficacy: communities using their relationships, shared norms, trust, and social cohesion to come together to control crime.
Not all communities benefit from the same degree of collective efficacy (Sampson et al., 1997). In some communities, some neighbors may not know who is “suspicious,” and different neighbors may not perceive the same individuals as “suspicious.” Some neighbors may not alert other neighbors because they do not know or trust these neighbors. They may doubt that anything will be done about the issue and think it is a frequent occurrence. Witnesses may fear the police themselves and be reluctant to call. Such communities lack the collective efficacy to come together and address crime, and such places are often characterized by poverty and residential instability (where residents are not attached to neighborhoods).
One possible strategy to build and improve collective efficacy is to identify and obtain the resources necessary to improve the physical condition of neighborhoods. Various grant programs (such as the Seattle Department of Neighborhood’s Neighborhood Matching Fund13 and other Hope grants14) provide resources to communities that propose their own solutions (Ramey and Shrider, 2014). These community-driven approaches have been shown to increase attachment to place, reduce violence, and improve mental health (see work, for example, by Charles Branas at the University of Pennsylvania Urban Health Lab) (Culyba et al., 2016; University of Pennsylvania, 2013). Another approach to building collective efficacy involves improving the relationships between community and “external” actors who broker resources for the community, such as banks, politicians, and law enforcement (Vélez, 2001). Communities with stronger ties among these actors are more able to hold these actors accountable. Other potential strategies include creating community watch organizations and block groups, which can facilitate social cohesion; strengthening neighborhood institutions such as neighborhood associations, schools, churches, businesses, and community centers; and facilitating the ability of residents to own their homes, fostering a stronger attachment to their community. Community policing approaches are thus fundamentally multi-sectoral because they promote organizational strategies that facilitate collaborative relationships among various community stakeholders.
___________________
13 For more information on the Neighborhood Matching Fund, see http://www.seattle.gov/neighborhoods/programs-and-services/neighborhood-matching-fund (accessed November 23, 2016).
14 For more information on the HOPE VI Program, see http://portal.hud.gov/hudportal/HUD?src=/program_offices/public_indian_housing/programs/ph/hope6 (accessed November 23, 2016).
As noted earlier, the final report of The President’s Task Force on 21st Century Policing highlights the importance of building and maintaining trust between law enforcement and local communities (The President’s Task Force on 21st Century Policing, 2015). Recent events illustrate the crisis of trust and accountability that is taking place in many communities across the country. Concerns about police brutality, bias, and procedural injustice severely undermine the efficacy and legitimacy of law enforcement. This is especially acute among racial and ethnic minority communities. The committee supports the recommendations of The President’s Task Force on 21st Century Policing that direct law enforcement agencies and communities toward the creation and maintenance of public safety
CROSS-SECTOR COLLABORATION—HEALTH IN ALL POLCIES
The term “health in all policies” (HIAP) refers to the use of a social-determinants-of-health approach to solutions and structures that breaks down the siloed nature of government to advance collaboration. In 2006 Sihto and colleagues defined HIAP as “a horizontal, complementary policy-related strategy with a high potential to contributing to population health,” at the core of which is the examination of “determinants of health, which can be influenced to improve health but are mainly controlled by policies of sectors other than health” (Sihto et al., 2006, p. 4). HIAP may be more accessibly described as the act of applying a health lens to decisions, policies, practices, and investments in other sectors, including in business (NASEM, 2016a).
Although the term has particular resonance for people working in the health field, it fits in a broader space of cross-sector collaboration which may include working across government agencies responsible for different aspects of the economy (e.g., the federal Sustainable Communities Partnership among the U.S. Department of Transportation [DOT], the U.S. Department of Housing and Urban Development [HUD], and the U.S. Environmental Protection Agency [EPA]) or at the intersection between the public and private sectors.
HIAP “engages diverse governmental partners and stakeholders to work together to promote health, equity, and sustainability, and simultaneously advance other goals such as promoting job creation and economic stability, transportation access and mobility, a strong agricultural system, and educational attainment” (Rudolph et al., 2013, p. 6). “There is no one ‘right’ way to implement a Health in All Policies approach, and there is substantial flexibility in process, structure, scope, and membership” (Rudolph et al., 2013, p. 17). Health in All Policies: A Guide for State and Local Governments outlines five key elements of HIAP, which are (1) promote
health, equity, and sustainability; (2) support inter-sectoral collaboration; (3) benefit multiple partners (i.e., achieve “co-benefits”); (4) engage stakeholders; and (5) create structural or process change (Rudolph et al., 2013). HIAP approaches can prevent unintended negative consequences for health, potentially avoiding higher health care costs and other challenges.
There are numerous examples of unintended consequences that have surfaced when policy making did not consider the health implications of a policy (e.g., the use of antibiotics in agriculture or automobile-centered land use and planning). HIAP or cross-sector collaborative initiatives can use different tools to consider the health implications of new policies and programs. A health impact assessment (HIA) is sometimes used to systematically examine the likely effects of a policy decision, such as new infrastructure (see Chapter 8 for a more detailed discussion of the use of HIA to advance health equity). For example, transportation, planning, and health departments can collaborate to implement health impact assessments to ensure that new transportation projects are evaluated based on their health implications (such as walkability and safety) in addition to more traditional transportation metrics. The Minnesota Department of Health founded the Healthy Minnesota Partnership, a multi-sector coalition (specifically, transportation, education, and community organizations) to inform the development and implementation of a statewide health assessment and community health improvement plan. In 2014 the department released Advancing Health Equity in Minnesota: Report to the Legislature (MDH, 2014), a publication used as a resource by state and local coalitions in a range of policy initiatives, including the effort to advocate for an increase in the minimum wage (ASTHO, 2014).
The NACCHO website offers several HIAP resources, including success stories of local health departments working in cross-sector coalitions (NACHHO, n.d.). These include the county council in Prince George’s County, Maryland, passing an ordinance in 2011 that requires the planning board to refer site, design, and master plan proposals to the Prince George’s County Health Department for an HIA of the proposed development on the community and the distribution of potential effects within the population and to recommend design components that increase positive health outcomes and minimize adverse health outcomes for the community. In another example, the Mid-Ohio Regional Planning Commission passed a complete-streets policy mandating that all projects funded by the commission accommodate all users, including pedestrians, bicyclists, users of mass transit, people with disabilities, and older adults.
Governance for “Health in All Policies” or Cross-Sector Collaboration
State policies in such areas as education, development, and land use have clear parallels to federal policy and can significantly shape how communities respond to health disparities. There are several state-level examples of cross-sector collaboration intended to improve health and health equity. In 2010 the State of California created a Health in All Policies Task Force—representing 19 state agencies, departments, and offices—under the auspices of the state’s Strategic Growth Council, aiming to build interagency partnerships across state government and to address issues of health, equity, and environmental sustainability. This is the first formal state-level body of its kind. Its goals describe a broad definition of health which includes air and water quality, natural resources and agricultural lands, the availability of affordable housing, infrastructure systems, public health, sustainable communities, and climate change. Such HIAP approaches and governance structures have also been adopted at the community level.
Several regions, including Seattle–King County (Washington state), Nashville, and Atlanta, have implemented cross-sector public sector and public–private partnership approaches to addressing challenges to the well-being of local communities by including a social justice and equity lens in all policies and collaborating to change the local conditions for health (King County, n.d.-a; Minyard et al., 2016; T4A, n.d.). The Nashville Metropolitan Planning Organization, for example, increased the percentage of projects that incorporate safe walking and biking elements from 2 percent in 2005 to 70 percent in its 2010 plan (Nashville Area Metropolitan Planning Organization, 2010). Although the plan does not use the term “health equity,” its monitoring of performance and impacts is framed by Title VI of the Civil Rights Act of 1964 and by the 1994 Executive Order on Environmental Justice, and the overall planning process is informed by transportation equity principles. Specifically, the project evaluation factors described in the plan include questions on health and environment, such as: “Does the project aid/harm the advancement of social justice and equity opportunity to destinations throughout the region?” and “How can the project be scoped to mitigate any negative impacts to predominantly low-income or minority communities or persons with a disability?” (Nashville Area Metropolitan Planning Organization, 2010).
National Initiatives
Several national initiatives have served to further cross-sector partnerships to improve health, livability, and economic development. In 2015, NACCHO funded three HIAP demonstration sites (Houston,
Baltimore city, and San Diego) with funding from the National Center for Environmental Health and the Agency for Toxic Substances and Disease Registry, both of the U.S. Centers for Disease Control and Prevention (CDC). In September 2014, the CDC provided support for the 3-year Plan4Health initiative, jointly led by the American Public Health Association (APHA) and the American Planning Association (APA) and implemented through 18 local coalitions, which include APHA and APA local affiliates. Plan4Health coalitions “incorporate equity into many aspects of their work to increase opportunities for active living and access to health foods” (Norcross, 2016). However, “getting to the root issues of why inequities exist can be complex, time consuming, and takes the buy-in and contributions of traditional and non-traditional cross-sector partners” (Makara, 2016). Plan4Health has assembled a collection of resources to support coalitions in this vital work, including A Refresher on Health Equity and the Transportation and Health Tool developed by the DOT and the CDC (Hartig, 2015; Makara, 2016). In 2016 the Association of Collegiate Schools of Architecture and the Association of Schools and Programs of Public Health (ASPPH) held their first-ever joint conference, titled Building for Health and Well-being: Structures, Cities, Systems. One conference track focused on what it called Acupunctural Urbanism: Advocacy, Equity, and Community Based Initiatives. In 2014 the American Institute of Architects held a summit on health and design, keynoted by the acting U.S. Surgeon General, and launched the Design and Health Research Consortium in 2015 (of which ASPPH has become a member). The consortium’s inaugural proceedings included a session on resilience and equity which concluded that ethnic and racial minorities are disproportionately exposed to harmful environmental factors and that “resilience in the context of health and environment must engage questions of race, ethnicity, income, and institutionalized prejudice” (AIA and ACSAAF, 2015). Such efforts—interprofessional, interdisciplinary, and cross-sectoral—enhance opportunities for fruitful collaboration to promote health equity in the practice of public health, architecture, and planning.
Financing and other support for a range of built environment and economic development projects comes from community development organizations. Community development corporations and community development financial institutions manage “billions in housing, real estate and small business assets and investments” and build community wealth and expand opportunities by increasing affordable housing access and building “green” affordable housing (Phillips, 2006).
Federal Government Initiatives on Health Equity
Over the past decade, there has been significant federal effort to coordinate actions aimed at advancing health equity. Below, the committee describes the considerable infrastructure for health equity that has been constructed within the federal government. As discussed earlier in this chapter, similar efforts to create a public-sector infrastructure for equity more generally or health equity specifically exist in some states and even some local jurisdictions.
The National Partnership for Action to End Health Disparities (NPA) has been a key driver. Its stakeholders are the Federal Interagency Health Equity Team (FIHET), the offices of minority health at the U.S. Department of Health and Human Services (HHS), regional health equity councils, and health equity champions. Federal leadership for NPA is provided by FIHET, whose mission is to convene federal leaders to end health inequities by building capacity for equitable policies and programs, cultivating strategic partnerships, and sharing relevant models for action (FIHET, 2016). The partnership includes leaders from the Consumer Product Safety Commission and the departments of agriculture, commerce, defense, education, housing and urban development, justice, labor, transportation, veterans affairs, and health and human services. The ACA mandated the establishment of offices of minority health within six agencies of HHS: the Agency for Healthcare Research and Quality, the CDC, the Centers for Medicare & Medicaid Services (CMS), Health Resources and Services Administration, Substance Abuse and Mental Health Services Administration, and the U.S. Food and Drug Administration. The 10 regional health equity councils are independent, nongovernmental organizations comprising leaders and stakeholders from both nonfederal public (e.g., state government) and private sectors (e.g., academia, community-based organizations, health systems, health insurers) from within that region. The health equity champions program further extends the NPA’s reach through pledges of support from organizations, advocacy groups, foundations, academic institutions, technical or subject matter experts, and community members.
The NPA has produced two major products to date. The National Stakeholder Strategy (NSS) for Achieving Health Equity laid out five goals and associated strategies in the areas of awareness, leadership, health system and life experience, cultural and linguistic competency, and data, research, and evaluation (NPA, 2016b). Within the NSS, the priorities for action and associated progress are to
- Educate and facilitate outreach on the Patient Protection and Affordable Care Act of 2010 (ACA): The Office of Minority Health is supporting implementation of the ACA by helping connect
-
minority consumers and communities of color with information about affordable health insurance options and partnering with CMS and other federal agencies and private-sector organizations to support to outreach efforts.
- Support the implementation of the National Standards for Culturally and Linguistically Appropriate Services in Health and Health Care: The Think Cultural Health website (HHS, n.d.) includes resources as well as an interactive map for monitoring activities by state.
- Educate youth and emerging leaders about health inequities and the social determinants of health so that they become champions for health equity: The youth National Partnership for Action to End Health Disparities priority area was developed in response to this need and is preparing young people to become future leaders and practitioners by educating them about health inequities and the social determinants of health and engaging youth in health equity work (NPA, 2016a).
- Strengthen the nation’s network of community health workers, who play a key role in disease prevention and health promotion: NPA activities primarily focus on supporting the integration of community health workers into clinical and preventive care workforces through the regional health equity councils (RHECs) (NPA, n.d.).
- Promote the integration of health equity into policies and programs: Activities include a “health equity mapping” pilot to work collaboratively with volunteer FIHET organizations to map the relationship between their priorities and core functions and the attainment of health equity; FIHET has partnered with the Democracy Collaborative to convene federal and nonfederal leaders from health, community economic development, and other sectors to identify key conditions needed to drive strategic cross-sector collaboration to promote health equity; RHECs have published regional blueprints and health equity report cards; and NPA has collaborated with nongovernmental partners who are key conveners of decision makers at the local and state levels (e.g., the National Indian Health Board and the Association of State and Territorial Health Officials) (NPA, 2016c).
The complementary HHS Action Plan to Reduce Racial and Ethnic Health Disparities includes an HHS commitment to an ongoing assessment of the effectiveness of policies and programs related to reducing racial and ethnic health inequities and accountability for increasing health insurance coverage, improving quality, building data capacity, preventing disease, and strengthening cultural competency to create a nation free
of inequities in health and health care (HHS, 2011). Box 7-6 summarizes an Office of Minority Health report on the federal government’s role in health equity.
Finally, CMS is implementing several activities that will provide opportunities for partnering across sectors in the community. Its quality strategy details agency priorities for health care quality improvement and identifies the elimination of disparities as a foundational principle along with enabling local innovations, strengthening infrastructure and data systems, and fostering learning organizations (CMS, 2016). The CMS Equity Plan for Medicare will affect change through several unique CMS levers (CMS, 2015). These include quality improvement networks and quality improvement organizations, CMS programs, policy, data, access to stakeholders, and communication tools. The plan focuses on Medicare populations that experience disproportionately high burdens of disease, worse quality of care, and barriers to accessing care.
Guided by a framework that includes three interconnected domains—better understanding and awareness of inequities, identifying and creating solutions based on that understanding, and accelerating the implementation of measurable actions to achieve health equity—the CMS Equity Plan for Medicare has six priority areas. Three focus on meeting the needs of diverse populations through enhanced language access, physical access, and community health worker training. The other three center on data collection, reporting, and analysis; evaluating impact and integrating solutions across CMS programs; and the development and dissemination of promising approaches to reduce health disparities.
The current state of health disparities is both deeply troubling and a call to action to stem the high human and economic cost of health inequity. Clearly, considerable support for addressing health equity has been established in HHS and across the executive branch through the Federal Interagency Health Equity Taskforce. Sustaining and elevating this cross-government effort will be important in helping to galvanize a national effort toward promoting health equity and encouraging ongoing efforts around the country.
In November 2016, the president signed an executive order establishing a community solutions council charged with fostering “collaboration across agencies, policy councils, and offices to coordinate actions, identify working solutions to share broadly, and develop and implement policy recommendations that put the community-driven, locally led vision at the center of policymaking” (The White House, 2016).
The council builds on the foundation of earlier efforts, including a 2010 executive order, and it seems to signal attention at the highest level of government to the notion of helping all communities to successfully confront their challenges “including crime, access to care, opportunities
to pursue quality education, lack of housing options, unemployment, and deteriorating infrastructure” (The White House, 2016).
Recommendation 7-7: The committee recommends that key federal government efforts, such as the Community Solutions Council, that are intended to support communities in addressing major challenges, consider integrating health equity as a focus.
A health equity focus could mean undertaking such efforts as
- Determining how government decisions in health and non-health sectors could affect low-income and minority populations, including unintended negative consequences.
- Convening key stakeholders to explore financing structures through which companies, philanthropy, and government can together fund key health equity initiatives, including efforts to generate better, timelier, and more locally relevant data.
The importance of considering the unintended consequences of government policies is evident. For example, Chapter 3 outlines several examples of historical government policies that shaped government investment, land use, transportation planning, and other features of communities with disproportionately negative effects on access to housing, safety, social cohesion, family stability, and health outcomes in low-income and minority populations (Freeman and Braconi, 2002; IOM, 2003; Levy et al., 2006; Prevention Institute, 2011; Vélez, 2001; Zuk et al., 2015). Weighing the consequences on health outcomes, however, will require access to more varied and meaningful sources of data and may demand resources for analysis and assessment. The unique circumstances and context of each community (e.g., defined by census tract or zip code) may make it difficult to undertake such an assessment of potential consequences in a way that considers their full scope.
Public–private partnerships offer opportunities for innovation and alignment of resources that can achieve greater efficiency and effectiveness. Examples include pay-for-success financing models to support early childhood development and other programs, the Sustainable Communities federal partnership that brought together public- and private-sector actors to align their efforts, and clean energy financing arrangements (IOM, 2015a; PolicyLink, n.d.; Probst, 2014).
The language of the Executive Order (excerpted in Box 7-7) demonstrates recognition of the importance of equity (not explicitly health equity) and the determinants of health and well-being: for example,
“Place is a strong determinant of opportunity and well-being. Research shows that the neighborhood in which a child grows up impacts his or her odds of going to college, enjoying good health, and obtaining a lifetime of economic opportunities” (The White House, 2016). This executive order builds on and revokes Executive Order 13560 of December 14, 2010, which had previously established a “community solutions council” within the Corporation for National and Community Service, a federal agency, and was intended to be comprised solely of 30 members from outside the federal government and charged “to support the social innovation and civic participation agenda of the Domestic Policy Council” (The White House, 2010). The new executive order also references the Community Solutions Task Force, created in 2015 and which the new Council is intended to replace. Since 2015, the Community Solutions Task Force, comprising executive departments, offices, and agencies across the federal government, has served as the primary interagency coordinator of agency work to engage with communities to deliver improved outcomes. This order builds on recent work to facilitate interagency and community-level collaboration to meet the unique needs of communities in a way that reflects these communities’ local assets, economies, geography, size, history, strengths, talent networks, and visions for the future. The distinguishing feature of the new council is that it is to be located in the White House and be cochaired by an Assistant to the President or the
Director of the Office of Management and Budget, as designated by the President and by one of several cabinet secretaries identified in the order (e.g., DOJ, HHS, HUD).
The Executive Order also calls on the council to conduct outreach to “representatives of nonprofit organizations, civil rights organizations, businesses, labor and professional organizations, start-up and entrepreneurial communities, State, local, and tribal government agencies, school districts, youth, elected officials, seniors, faith and other community-based organizations, philanthropies, technologists, other institutions of local importance, and other interested or affected persons with relevant expertise in the expansion and improvement of efforts to build local capacity, ensure equity, and address economic, social, environmental, and other issues in communities or regions” (The White House, 2016).
The committee hopes that the council could build on the foundations of health equity work presented in this report and elsewhere and take action toward solutions, including cross-sector, community-driven, and public–private partnerships. It needs to be more than merely a symbol to avoid a disempowering effect on communities. Furthermore, there is a large power differential between a group of such high profile actors and communities and community members. The committee hopes that council engagement of community members will be conducted in the spirit of respect and authentic partnership. As outlined in this report, communities are where change takes place, and the members of communities are best equipped to know what is needed to effect change in their community.
CONCLUDING OBSERVATIONS
There are many potential multi-sector partners that can come together in creating community interventions to promote health equity, and multiple examples of effective approaches exist. Regardless of the sectors and organizations that make up these partnerships, a key element of success is the authentic engagement of members of the affected community. Partners will vary based on the target of the intervention, from the education sector (schools) and criminal justice (law enforcement) to the private sector (businesses, health care systems, and payers) and local, state, and federal government agencies (including public health). Anchor institutions can play key partner and leadership roles by virtue of their stable presence and economic resource power. Regardless of the participants, effective and enduring interventions depend on collaboration across multiple sectors. Cross-sector collaborations, as modeled by approaches aiming to achieve co-benefits (e.g., expanded employment and improved health status; increased energy efficiency and decreased asthma rates), bring together the partners discussed in this chapter to address the social determinants of health and achieve health equity.
REFERENCES
Active Living By Design. 2016. Finding common ground with human-centered design. http://activelivingbydesign.org/finding-common-ground-with-human-centered-design (accessed October 19, 2016).
AHA (American Hospital Association). 2015. Equity of care: A toolkit for eliminating health care disparities. http://www.hpoe.org/Reports-HPOE/equity-of-care-toolkit.pdf (accessed October 20, 2016).
AHA. n.d.-a. #123forequity pledge to eliminate health care disparities. http://www.equityofcare.org/pledge/index.shtml (accessed October 20, 2016).
AHA. n.d.-b. Equity of care: Resources. http://www.equityofcare.org/resources/index.shtml (accessed October 20, 2016).
AIA and ACSAAF (American Institute of Architects and the Association of Collegiate Schools of Architecture and Architects Foundation). 2015. Pulse on progress: Proceedings of the inaugural meeting of the aia design & health research consortium. Princeton, NJ: The American Institute of Architects and the Association of Collegiate Schools of Architecture and Architects Foundation.
Andrews, N. O., and D. J. Erickson. 2012. Investing in what works for America’s communities: Essays on people, place & purpose. Federal Reserve Bank of San Francisco and Low Income Investment Fund.
ASTHO (Association of State and Terriorial Health Officials). 2014. Minnesota Department of Health changes the narrative on health with the healthy Minnesota partnership. http://www.astho.org/Health-Equity/MN-Health-Equity-in-All-Policies-Story (accessed October 20, 2016).
ATSDR (Agency for Toxic Substances and Disease Registry). 2011. Principles of community engagement (second edition). NIH Publication No. 11-7782. http://www.atsdr.cdc.gov/communityengagement (accessed October 19, 2016).
Attree, P., B. French, B. Milton, S. Povall, M. Whitehead, and J. Popay. 2011. The experience of community engagement for individuals: A rapid review of evidence. Health & Social Care in the Community 19(3):250–260.
Balfanz, R., and V. Byrnes. 2012. Chronic absenteeism: Summarizing what we know from nationally available data. Baltimore, MD: Johns Hopkins University Center for Social Organization of Schools.
Basch, C. E. 2011. Healthier students are better learners: A missing link in school reforms to close the achievement gap. Journal of School Health 81(10):593–598.
Bhaskaran, S. 2016. Pinklining: How Wall Street’s predatory products pillage women’s wealth, opportunities, & futures. http://isaiahmn.org/newsite/wp-content/uploads/2016/06/Pinkling-June-2016.pdf (accessed October 19, 2016).
Birch, E., D. C. Perry, and H. L. Taylor. 2013. Universities as anchor institutions. Journal of Higher Education Outreach and Engagement 17(3):7–15.
Bower, J. L., H. B. Leonard, and L. S. Paine. 2011. Capitalism at risk: Rethinking the role of business. Boston, MA: Harvard Business Review Press.
Bryk, A. S., P. B. Sebring, E. Allensworth, S. Luppescu, and J. Q. Easton. 2010. Organizing schools for improvement: Lessons from Chicago. Chicago, IL: University of Chicago Press.
Bullard, R. D., and R. Garcia. 2015. Diversifying mainstream environmental groups is not enough. Parks & Recreation. http://www.parksandrecreation.org/2015/July/Diversifying-Mainstream-Environmental-Groups-Is-Not-Enough (accessed October 19, 2016).
Bureau of Justice Statistics. 2016. Community policing. http://www.bjs.gov/index.cfm?ty=tp&tid=81 (accessed December 1, 2016).
CalEPA (California Environmental Protection Agency). n.d. Greenhouse gas-reduction investments to benefit disadvantaged communities. http://www.calepa.ca.gov/EnvJustice/GHGInvest (accessed October 19, 2016).
Campbell’s Soup Company. 2015. Campbell’s healthy communities taking shape in Camden. https://www.campbellsoupcompany.com/newsroom/news/2015/03/23/campbells-healthy-communities-taking-shape-in-camden (accessed October 21, 2016).
CCPH (Community–Campus Partnerships for Health). 2007. Community-campus partnerships for health: Celebrating a decade of impact. Community-Campus Partnerships for Health. https://ccph.memberclicks.net/assets/Documents/10annivreportfinal.pdf (accessed November 16, 2016).
CCPH. 2012. Creating the space to ask “why?” Community-campus partnerships as a strategy for social justice. https://ccph.memberclicks.net/assets/Documents/conf12-draftpaper.pdf (accessed October 20, 2016).
CCPH. n.d. Community-campus partnerships for health. https://ccph.memberclicks.net (accessed October 20, 2016).
CDC (U.S. Centers for Disease Control and Prevention). 2011. Ten great public health achievements—United States, 2001-2010. Morbidity and Mortality Weekly Report 60(19):619–623.
CDC. 2014. Diagnoses of HIV infection in the United States and dependent areas, 2014. HIV Surveillance Report (26). https://www.cdc.gov/hiv/pdf/library/reports/surveillance/cdc-hiv-surveillance-report-us.pdf (accessed September 12, 2016).
Chang, H., and R. Balfanz. 2016. Preventing missed opportunity: Taking collective action to confront chronic absence. Attendance Works and Everyone Graduates Center. http://www.attendanceworks.org/research/preventing-missed-opportunity (accessed October 19, 2016).
Chetty, R., and N. Hendren. 2015. The impacts of neighborhoods on intergenerational mobility: Childhood exposure effects and county-level estimates. http://www.equality-of-opportunity.org/images/nbhds_paper.pdf (accessed October 20, 2016).
City of Chicago. 2016. Healthy Chicago 2.0: Partnering to improve health equity 2016–2020. Chicago, IL: Chicago Department of Public Health.
CMS (Centers for Medicare & Medicaid Services). 2015. The CMS equity plan for improving quality in Medicare. Baltimore, MD: Centers for Medicare & Medicaid Services, Office of Minority Health.
CMS. 2016. CMS quality strategy. Baltimore, MD: Centers for Medicare & Medicaid Services.
Conti, G., J. Heckman, and S. Urzua. 2011 (unpublished). Early endowments, education, and health. Chicago, IL: University of Chicago.
CORE. 2016. Student, staff, parent culture-climate survey. Sacramento, CA: John W. Gardner Center for Youth and their Communities.
CPLC (Chicanos Por La Causa). n.d. Chicanos por la causa. http://www.cplc.org (accessed October 20, 2016).
Culyba, A. J., S. F. Jacoby, T. S. Richmond, J. A. Fein, B. C. Hohl, and C. C. Branas. 2016. Modifiable neighborhood features associated with adolescent homicide. JAMA Pediatrics 170(5):473–480.
Dan, D., R. Finch, D. Harrison, and D. Kendall. 2011. An employer’s guide to reducing racial & ethnic health disparities in the workplace. Washington, DC: National Business Group on Health.
Davidoff, F., and P. Batalden. 2005. Toward stronger evidence on quality improvement. Draft publication guidelines: The beginning of a consensus project. Quality & safety in health care 14(5):319–325.
Democracy Collaborative. 2014. Press release: Six universities partner with the democracy collaborative to develop and share best practices for measuring community impact. http://democracycollaborative.org/content/press-release-six-universities-partner-democracy-collaborative-develop-best-practices (accessed October 20, 2016).
Democracy Collaborative. n.d.-a. Anchor institutions. http://democracycollaborative.org/democracycollaborative/anchorinstitutions/Anchor%20Institutions (accessed October 20, 2016).
Democracy Collaborative. n.d.-b. Community development corporations (CDCs). http://community-wealth.org/strategies/panel/cdcs/index.html (accessed November 1, 2016).
DOJ (U.S. Department of Justice). 2015. Diversity in law enforcement: A literature review. http://www.cops.usdoj.gov/pdf/taskforce/Diversity_in_Law_Enforcement_Literature_Review.pdf (accessed October 19, 2016).
DOJ. 2016. Advancing diversity in law enforcement. https://www.justice.gov/crt/case-document/file/900761/download (accessed October 18, 2016).
Doucet, B. 2015. Detroit’s gentrification doesn’t address poverty. Portside. http://portside.org/2015-02-18/detroits-gentrification-doesnt-address-poverty (accessed October 20, 2016).
Dubb, S., S. McKinley, and T. Howard. 2013. Achieving the anchor promise: Improving outcomes for low-income children, families and communities. Democracy Collaborative.
Dunn, R. A. 2010. Race and the relevance of citizen complaints against the police. Administrative Theory And Praxis 32(4):557–577.
Dweck, C. S., G. M. Walton, and G. L. Cohen. 2014. Academic tenacity: Mindsets and skills that promote long-term learning. Bill and Melinda Gates Foundation.
EBALDC (East Bay Asian Local Development Corporation). n.d. East Bay Asian Local Development Corporation. http://www.ebaldc.org (accessed October 19, 2016).
ED (U.S. Department of Education). 2016. The fiscal year 2017 budget: Promoting greater use of evidence and data as a lever for advancing equity. In Homeroom: The Official Blog of the U.S. Department of Education. Washington, DC: U.S. Department of Education.
Eder, M. M., L. Carter-Edwards, T. C. Hurd, B. B. Rumala, and N. Wallerstein. 2013. A logic model for community engagement within the clinical and translational science awards consortium: Can we measure what we model? Academic Medicine 88(10):1430–1436.
Edmonds, A., P. Braveman, E. Arkin, and D. Jutte. 2015. Making the case for linking community development and health: A resource for those working to improve low-income communities and the lives of the people living in them. http://www.buildhealthyplaces.org/resources/making-the-case-for-linking-community-development-and-health (accessed October 24, 2016).
FIHET (Federal Interagency Health Equity Team). 2016. Federal interagency health equity team. http://minorityhealth.hhs.gov/npa/templates/browse.aspx?lvl=1&lvlid=36 (accessed December 1, 2016).
Finn, P. 2001. Citizen review of police: Approaches & implementation. https://www.ncjrs.gov/pdffiles1/nij/184430.pdf (accessed October 19, 2016).
Frankl, E. 2016. Community schools: Transforming struggling schools into thriving schools. https://populardemocracy.org/news/publications/community-schools-transforming-struggling-schools-thriving-schools (accessed October 19, 2016).
Freeman, L., and F. Braconi. 2002. Gentrification and displacement. The Urban Prospect 8(1).
Freudenberg, N., and J. Ruglis. 2007. Reframing school dropout as a public health issue. Preventing Chronic Disease 4(4).
Fullilove, M. T., and R. Wallace. 2011. Serial forced displacement in American cities, 1916–2010. Journal of Urban Health 88(3):381–389.
Gaffikin, F., and D. C. Perry. 2009. Discourses and strategic visions: The U.S. research university as an institutional manifestation of neoliberalism in a global era. American Educational Research Journal 46(1):115–144.
Gehlert, H. 2015. Advancing health equity: Case studies of health equity practice in four award-winning California Health Departments. Berkeley, CA: Berkeley Media Studies Group.
GHHI (Green and Healthy Homes Initiative). n.d. What is GHHI?http://www.greenandhealthyhomes.org/about-us/what-ghhi (accessed October 19, 2016).
Gill, C., D. Weisburd, C. W. Telep, Z. Vitter, and T. Bennett. 2014. Community-oriented policing to reduce crime, disorder and fear and increase satisfaction and legitimacy among citizens: A systematic review. Journal of Experimental Criminology 10:399–428.
Ginsburg, A., P. Jordan, and H. Chang. 2014. Absences add up: How school attendance influences student success. Attendance Works. http://www.attendanceworks.org/research/absences-add (accessed October 19, 2016).
Governing. n.d. Cleveland gentrification maps and data. http://www.governing.com/gov-data/cleveland-gentrification-maps-demographic-data.html (accessed October 20, 2016).
Hair, P. D. 2001. Louder than words: Lawyers, communities and the struggle for justice. http://www.racialequitytools.org/resourcefiles/hair.pdf (accessed October 19, 2016).
Hansen, S. 2012. Cultivating the grassroots: A winning approach for environment and climate funders. https://www.ncrp.org/files/publications/Cultivating_the_grassroots_final_lowres.pdf (accessed October 19, 2016).
Harkavy, I., and H. Zuckerman. 1999. Eds and meds: Cities’ hidden assets. Washington, DC: The Brookings Institution Center on Urban and Metropolitan Policy.
Harkavy, I., M. Hartley, R. A. Hodges, A. Sorrentino, and J. Weeks. 2014. Effective governance of a university as an anchor institution: University of Pennsylvania as a case study. Leadership and Governance in Higher Education 2.
Harris, D. A. 2005. Good cops: The case for preventive policing. New York: New Press.
Hartig, E. 2015. Explore the transportation and health tool. http://plan4health.us/explore-the-transportation-and-health-tool (accessed October 20, 2016).
Health Care for All. n.d. Maryland faith health network. http://healthcareforall.com/getinvolved/maryland-faith-community-health-network (accessed October 20, 2016).
Heckman, J. 2011. The economics of inequality: The value of early childhood education. American Educator 31–47.
Henry Ford Health System. n.d. About Henry Ford Health System. https://henryford.referrals.selectminds.com/info/page1 (accessed October 20, 2016).
HHS (U.S. Department of Health and Human Services). 2011. HHS action plan to reduce racial and ethnic health disparities. Washington, DC: U.S. Department of Health and Human Services.
HHS. n.d. Think cultural health. https://www.thinkculturalhealth.hhs.gov (accessed October 20, 2016).
HMA (Health Ministries Association). n.d. Health Ministries Association, Inc.http://hmassoc.org/about-us/what-we-do (accessed October 20, 2016).
Hodges, R. A., and S. Dubb. 2012. The road half traveled: University engagement at a crossroads.
Hornby, G., and R. Lafaele. 2011. Barriers to parental involvement in education: An explanatory model. Educational Review 63(1):37–52.
ICF (Inner City Fund) International. 2010. Communities in schools national evaluation: Five year summary report. Fairfax, VA: ICF International.
ICIC (Initiative for a Competitive Inner City). 2011. Inner city, anchor institutions and urban economic development: From community benefit to shared value. Inner City Highlights 1(2). http://community-wealth.org/content/inner-city-anchor-institutions-and-urban-economic-development-community-benefit-shared-value (accessed October 20, 2016).
IHI (Institute for Healthcare Improvement). 2016. Achieving health equity: A guide for health care organizations. Cambridge, MA: Institute for Healthcare Improvement.
IOM (Institute of Medicine). 2003. Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: The National Academies Press.
IOM. 2011. For the public’s health: Revitalizing law and policy to meet new challenges. Washington, DC: The National Academies Press.
IOM. 2013. The CTSA program at NIH: Opportunities for advancing clinical and translational research. Washington, DC: The National Academies Press.
IOM. 2014. Supporting a movement for health and health equity: Workshop summary. Washington, DC: The National Academies Press.
IOM. 2015a. Financing population health improvement: Workshop summary. Washington, DC: The National Academies Press.
IOM. 2015b. The role and potential of communities in population health improvement: Workshop summary. Washington, DC: The National Academies Press.
ISAIAH. n.d. Vision. http://isaiahmn.org/vision-3 (accessed October 19, 2016).
Joassart-Marcelli, P. 2010. Leveling the playing field? Urban disparities in funding for local parks and recreation in the Los Angeles region. Environment and Planning A 42(5):1174–1192.
Joassart-Marcelli, P., J. Wolch, and Z. Salim. 2011. Building the healthy city: The role of nonprofits in creating active urban parks. Urban Geography 32(5):682–711.
Kelly, M., and S. McKinley. 2015. Cities building community wealth. Democracy Collaborative.
King County. n.d.-a. Equity and social justice. http://www.kingcounty.gov/elected/executive/equity-social-justice.aspx (accessed October 20, 2016).
King County. n.d.-b. Public health—Seattle & King County. http://www.kingcounty.gov/healthservices/health.aspx (accessed October 20, 2016).
Legters, N., and R. Balfanz. 2010. Do we have what it takes to put all students on the graduation path? New directions for youth development 2010(127):11–24.
Levy, D. K., J. Comey, and S. Padilla. 2006. In the face of gentrification: Case studies of local efforts to mitigate displacement. Washington, DC: Urban Institute.
Makara, M. 2016. A refresher on health equity. http://plan4health.us/a-refresher-on-health-equity (accessed October 20, 2016).
Martin, L. L., H. Smith, and W. Phillips. 2005. Bridging ‘town & gown’ through innovative university-community partnerships. The Innovation Journal: The Public Sector Innovation Journal 10(2). http://www.innovation.cc/volumes-issues/martin-u-partner4final.pdf (accessed October 20, 2016).
McGill, T. M., S. R. Self-Brown, B. S. Lai, M. Cowart-Osborne, A. Tiwari, M. Leblanc, and M. L. Kelley. 2014. Effects of exposure to community violence and family violence on school functioning problems among urban youth: The potential mediating role of posttraumatic stress symptoms. Front Public Health 2:8.
McNeely, E., and G. Norris. 2015. Shine summit 2015: Innovating for netpositive impact: Summary report. Boston, MA: Sustainability and Healthy Initiative for NetPositive Enterprise.
MDH (Minnesota Department of Health). 2014. Advancing health equity in Minnesota: Report to the legislature. St. Paul: Minnesota Department of Health.
Methodist Healthcare. n.d. Community. http://www.methodisthealth.org/about-us/faithand-health/community/ (accessed October 20, 2016).
Miller, D. S., and J. D. Rivera. n.d. Town and gown: Understanding the past to improve the future. International Journal of the Humanities 3(8):215–224.
Minyard, K., K. Lawler, E. Fuller, M. Wilson, and E. Henry. 2016. Reducing health disparities in Atlanta. Stanford Social Innovation Review. https://ssir.org/articles/entry/reducing_health_disparities_in_atlanta (accessed October 20, 2016).
Mitchell, C. 2008. Parental involvement in public education: A literature review. Research for Action. http://www.researchforaction.org/wp-content/uploads/2016/02/Mitchell_C_Parent_Involvement_in_Public_Education.pdf (accessed October 19, 2016).
Mitchell, F. 2016. Innovations in health equity and health philanthropy. Stanford Social Innovation Review. https://ssir.org/articles/entry/innovations_in_health_equity_and_health_philanthropy (accessed October 19, 2016).
Miyake, A., L. E. Kost-Smith, N. D. Finkelstein, S. J. Pollock, G. L. Cohen, and T. A. Ito. 2010. Reducing the gender achievement gap in college science: A classroom study of values affirmation. Science 330:1234–1237.
Morley, R. 2016. Re: Comments on title i, § 200.21(c) school-level needs assessment; proposed rule. Docket ID: Ed-2016-oese-0032 title i, § 200.21(c). http://www.pewtrusts.org/~/media/assets/2016/10/health-impact-project-comments-20021c/hip-comments-20021c.pdf (accessed November 18, 2016).
NACCHO (National Association of County and City Health Officials). 2016. Health equity and social justice. http://www.naccho.org/programs/public-health-infrastructure/health-equity (accessed October 19, 2016).
NACCHO. n.d. Resources. http://archived.naccho.org/topics/environmental/HiAP/resources (accessed October 20, 2016).
NACHC (National Association of Community Health Centers). n.d.-a. Prapare. http://nachc.org/research-and-data/prapare (accessed October 20, 2016).
NACHC. n.d.-b. Research and data. http://nachc.org/research-and-data (accessed October 20, 2016).
NASEM (National Academies of Sciences, Engineering, and Medicine). 2016a. Applying a health lens to business practices, policies, and investments: Workshop summary. Washington, DC: The National Academies Press.
NASEM. 2016b. Framing the dialogue on race and ethnicity to advance health equity: Proceedings of a workshop. Washington, DC: The National Academies Press.
Nashville Area Metropolitan Planning Organization. 2010. 2035 Nashville area regional transportation plan.http://www.nashvillempo.org/docs/lrtp/2035rtp/Docs/2035_Doc/2035Plan_Complete.pdf (accessed March 8, 2016).
NCATS (National Center for Advancing Translational Sciences). n.d.-a. Clinical and translational science awards (ctsa) program. http://www.ncats.nih.gov/ctsa (accessed October 19, 2016).
NCATS. n.d.-b. CTSA program hubs. http://www.ncats.nih.gov/ctsa/about/hubs (accessed October 19, 2016).
Neavling, S. 2013. ‘Bring on more gentrification,’ declares Detroit’s economic development czar. Motor City Muckraker. http://motorcitymuckraker.com/2013/05/16/bring-on-more-gentrification-declares-detroits-economic-development-czar-george-jackson (accessed December 2, 2016.
Netter Center for Community Partnerships. 2008. Anchor institutions toolkit: A guide for neighborhood revitalization. Philadelphia: University of Pennsylvania.
Norcross, A. 2016. Health equity and planning. http://plan4health.us/health-equity-and-planning (accessed October 20, 2016).
Norris, T., and T. Howard. 2015. Can hospitals heal America’s communities? “All in for mission” is the emerging model for impact. Democracy Collaborative. http://democracycollaborative.org/content/can-hospitals-heal-americas-communities-0 (accessed October 20, 2016).
NPA (National Partnership for Action to End Health Disparities). 2016a. Education youth and emerging leaders about the social determinants of health and health disparties through the youth national partnership to action to end health disparities (YNPA). http://minorityhealth.hhs.gov/npa/templates/content.aspx?lvl=1&lvlid=38&ID=356 (accessed October 20, 2016).
NPA. 2016b. National stakeholder strategy for achieving health equity. Rockville, MD: National Partnership for Action to End Health Disparities, U.S. Department of Health and Human Services, Office of Minority Health.
NPA. 2016c. Promoting the integration of equity in all policies & programs. http://minorityhealth.hhs.gov/npa/templates/content.aspx?lvl=1&lvlid=38&ID=355 (accessed December 1, 2016).
NPA. n.d. Regional health equity councils. http://minorityhealth.hhs.gov/npa/templates/browse.aspx?lvl=1&lvlid=42 (accessed December 1, 2016).
NTFAI (National Task Force on Anchor Institutions). 2010. Anchor institutions task force. http://www.margainc.com/files_images/general/anchor_task_force_statement.pdf (accessed October 20, 2016).
NYC (New York City) Department of Education. 2016. Quality review. http://schools.nyc.gov/Accountability/tools/review/default.htm (accessed December 19, 2016).
NYSDOH (New York State Department of Health). 2016. Supportive housing initiatives. https://www.health.ny.gov/health_care/medicaid/redesign/supportive_housing_initiatives.htm (accessed October 20, 2016).
O’Mara, M. P. 2012. Beyond town and gown: University economic engagement and the legacy of the urban crisis. Journal of Technology Transfer 37(2):234–250.
OpenData KC. 2016. Kansas City, MO., community health improvement plan 2011 through 2016. https://data.kcmo.org/Health/KCMO-CHIP-2011-2016/gunq-ki6v (accessed October 20, 2016).
Oziransky, V., D. Yach, T. Tsu-Yu, A. Luterek, and D. Stevens. 2015. Beyond the four walls: Why community is critical to workforce health. New York: Vitality Institute.
PHAB (Public Health Accreditation Board). 2013. Public health accreditation board standards & measures. Alexandria, VA: Public Health Accreditation Board.
Phillips, R. 2006. Interview of Ron Phillips, CEO of Coastal Enterprises, Inc. (CEI) of Maine, edited by S. Dubb. Washington, DC: Democracy Collaborative.
PolicyLink. n.d. Center for infrastructure equity: Sustainable communities. http://www.policylink.org/focus-areas/infrastructure-equity/sustainable-communities (accessed December 1, 2016).
Porter, M. E. 2010. Anchor institutions and urban economic development: From community benefit to shared value. Presented at Inner City Economic Forum Summit San Francisco, CA.
Porter, M. E., and M. R. Kramer. 2011. Creating shared value. Harvard Business Review 89(1-2):62–77.
Prevention Institute. 2011. Fact sheet: Links between violence and health equity. Oakland, CA: Prevention Institute.
Probst, C. S. 2014. Private sector financing and public-private partnerships for financing clean energy. Research Program on Sustainability Policy and Management, Earth Institute, Columbia University.
Providence Hospital. n.d. Community health assessment. http://www.provhosp.org/aboutus/community-health-assessment (accessed December 1, 2016).
Purciel-Hill, M., F. Santiago, L. Farhang, A. Tesfai, K. Ito, and K. H. Pace. 2016. Drowning in debt: A health impact assessment of how payday loan reforms improve the health of Minnesota’s most vulnerable. http://isaiahmn.org/newsite/wp-content/uploads/2016/03/PaydayLendingHIA-FinalReport41616.pdf (accessed October 19, 2016).
QCDO (Quitman County Development Organization). n.d. Quitman County Development Organization. http://www.qcdo.org (accessed October 20, 2016).
Quinn, M. 2016. Boulder County, CO.: Blueprint for merging health and housing under one roof. Governing. http://www.governing.com/topics/health-human-services/govhousing-health-mergers-boulder.html (accessed October 19, 2016).
Ramey, D. M., and E. A. Shrider. 2014. New parochialism, sources of community investment, and the control of street crime. Criminology & Public Policy 13(2):193–216.
Rooney, J. D., and J. Gittleman. 2005. A new era of higher education-community partnerships: The role and impact of colleges and universities in greater Boston today. The Boston Foundation and the University College of Citizenship and Public Service at Tufts University.
Rubin, V., and K. Rose. 2015. Strategies for strengthening anchor institutions’ community impact. Oakland, CA: PolicyLink.
Rudolph, L., J. Caplan, K. Ben-Moshe, and L. Dillon. 2013. Health in all policies: A guide for state and local governments. Washington, DC, and Oakland, CA: American Public Health Association and Public Health Institute.
RWJF (Robert Wood Johnson Foundation). 2015a. From vision to action: A framework and measures to mobilize a culture of health. Princeton, NJ: Robert Wood Johnson Foundation.
RWJF. 2015b. Kansas City, MO: 2015 culture of health prize winner. http://www.rwjf.org/en/library/articles-and-news/2015/10/coh-prize-kansas-city-mo.html (accessed October 20, 2016).
Sampson, R. J. 2012. Great American city: Chicago and the enduring neighborhood effect. Chicago; London: The University of Chicago Press.
Sampson, R. J., S. W. Raudenbush, and F. Earls. 1997. Neighborhoods and violent crime: A multilevel study of collective efficacy. Science 277(5328):918–924.
Schrantz, D. 2016. PowerPoint presentation to the Committee on Community-Based Solutions to Promote Health Equity in the United States in Washington, DC, April 27, 2016. http://www.nationalacademies.org/hmd/~/media/Files/Activity%20Files/PublicHealth/COH_Community%20Based%20Solutions/April%20Meeting/Schrantz%20D.pdf (accessed October 18, 2016).
Schroepfer, E. 2016. A renewed look at faith community nursing. MEDSURG Nursing 25(1):61–66.
Serang, F., J. P. Thompson, and T. Howard. 2013. The anchor mission: Leveraging the power of anchor institutions to build community wealth. Takoma Park, MD: The Democracy Collaborative.
Shah, M. K., M. Heisler, and M. M. Davis. 2014. Community health workers and the Patient Protection and Affordable Care Act: An opportunity for a research, advocacy, and policy agenda. Journal of health care for the poor and underserved 25(1):17–24.
Sigler, M. K. 2016. Expanding transition: Redefining school readiness in response to toxic stress. Voices in Urban Education (Annenberg Institute for School Reform)(43):37–45.
Sihto, M., E. Ollila, and M. Koivusalo. 2006. Principles and challenges of health in all policies. In Health in all policies: Prospects and potentials, edited by T. Ståhl, M. Wismar, E. Ollila, L. E. and K. Leppo. Helsinki, Finland: Finland Ministry of Social Affairs and Health and the European Observatory on Health Systems and Policies.
Skocpol, T. 2013. Naming the problem: What it will take to counter extremism and engage Americans in the fight against global warming. http://www.scholarsstrategynetwork.org/sites/default/files/skocpol_captrade_report_january_2013_0.pdf (accessed October 19, 2016).
Skogan, W. G. 2006. Police and community in Chicago: A tale of three cities. Oxford; New York: Oxford University Press.
Smedley, B., and H. Amaro. 2016. Advancing the science and practice of place-based intervention. American Journal of Public Health 106(2):197.
Snyder, T. D., and S. A. Dillow. 2015. Digest of educational statistics 2013. Washington, DC: U.S. Department of Education, National Center for Education Statistics, Institute of Education Sciences.
SPARCC (Strong, Prosperous, and Resilient Communities Challenge). n.d. Strong, prosperous, and resilient communities challenge. http://sparcchub.org (accessed October 19, 2016).
Super Church, M. 2015. Using data to address health disparities and drive investment in healthy neighborhoods. Washington, DC: National Academy of Medicine. https://nam.edu/wp-content/uploads/2015/12/SuperChurch.pdf (accessed July 16, 2016).
T4A (Transportation for America). n.d. Transportation for America. http://t4america.org (accessed October 20, 2016).
Taylor, H. L., and G. Luter. 2013. Anchor institutions: An interpretative review essay. New York: Anchor Institutions Task Force.
The Economist. 2009. Triple bottom line: It consists of three ps: Profit, people and planet. http://www.economist.com/node/14301663 (accessed December 1, 2016).
The President’s Task Force on 21st Century Policing. 2015. Final report of the president’s task force on 21st century policing. Washington, DC: Office of Community Oriented Policing Services.
The White House. 2010. Executive order 13560—White House council for community solutions. https://www.whitehouse.gov/the-press-office/2010/12/14/executive-order-13560-white-house-council-community-solutions (accessed December 1, 2016).
The White House. 2016. Executive order—establishing a community solutions council. https://www.whitehouse.gov/the-press-office/2016/11/16/executive-order-establishing-community-solutions-council (accessed December 1, 2016).
Trinity Health. n.d. Trinity health. http://www.trinity-health.org (accessed October 20, 2016).
Turner, A. 2015. The business case for racial equity in Michigan. Washington, DC: Altarum Institute.
University of Pennsylvania. 2013. Urban health lab. http://www.urbanhealthlab.org (accessed December 2, 2016).
Vélez, M. B. 2001. Role of public social control in urban neighborhoods: A multi-level analysis of victimization risk. Criminology 39(4):837–864.
Viveiros, J., and L. Sturtevant. 2016. The role of anchor institutions in restoring neighborhoods: Health institutions as a catalyst for affordable housing and community development. Washington, DC: National Housing Conference.
Westfall, J. M., K. Nearing, M. Felzien, L. Green, N. Calonge, F. Pineda-Reyes, G. Jones, M. Tamez, S. Miller, and A. Kramer. 2013. Researching together: A CTSA partnership of academicians and communities for translation. Clinical and Translational Science 6(5):356–362.
Woods, A. 2014. Detroit doesn’t need hipsters to survive, it needs black people. The Huffington Post. http://www.huffingtonpost.com/2014/03/10/saving-detroit-thomas-sugrue-hipsters_n_4905125.html (accessed October 20, 2016).
Wright, W., K. W. Hexter, and N. Downer. 2016. Cleveland University’s circle initiative: An anchor-based strategy for change. Takoma Park, MD: Democracy Collaborative.
Zakheim, M., K. McNamara, and J. Joseph. 2010. Partnerships between federally qualified health centers and local health departments for engaging in the development of a community-based system of care. Bethesda, MD: National Association of Community Health Centers.
Zuckerman, D. 2013. Hospitals building healthier communities: Embracing the anchor mission. College Park: The Democracy Collaborative at the University of Maryland.
Zuckerman, D., D. V., and K. Parker. 2015. Cross-sector collaboration and resource alignment strategies to achieve health equity. Washington, DC: Democracy Collaborative.
Zuk, M., A. H. Bierbaum, K. Chapple, K. Gorska, A. Loukaitou-Sideris, P. Ong, and T. Thomas. 2015 (unpublished). Gentrification, displacement, and role of public investment: A literature review. San Francisco, CA: Federal Reserve Bank of San Francisco.
































































