7
Potassium Dietary Reference Intakes: Risk Characterization and Special Considerations for Public Health
The final two steps of the Dietary Reference Intake (DRI) organizing framework provide public health context for the revised or newly established reference values. One of the hallmarks of these steps is to compare the DRI values to intake distributions in the United States and Canada for the nutrient of interest, to assess whether population intakes are likely to be adequate, and to determine if the population is at risk due to excessive intake. Use of biochemical and clinical measures, if available, can also supplement this risk characterization. With the expansion of the DRI model, this step now also examines intakes in relevant populations in relation to the Chronic Disease Risk Reduction Intake (CDRR), if established. This information is then used to describe the public health implications of the established DRI values. This chapter provides the committee’s risk characterization and special considerations for public health as they relate to the potassium DRI values established in this report.
RISK CHARACTERIZATION BASED ON POTASSIUM INTAKE LEVELS IN THE U.S. AND CANADIAN POPULATIONS
Adequate Intakes (AIs) are usually established when the evidence is not sufficient to derive Estimated Average Requirements and Recommended Dietary Allowances. The potassium AIs were derived using the highest median usual potassium intakes across two nationally representative surveys among children and normotensive male and female adults. For infants, the potassium AIs were derived by estimating potassium intake of breastfed infants.
Because the committee lacked information as to how AIs relate to actual requirements, caution is needed in use and interpretation of the AI values (IOM, 2000, 2003). The potassium AIs were derived using median intakes of apparently healthy groups of people within the U.S. and Canadian populations. Therefore, “similar groups with mean intakes at or above the AI can be assumed to have a low prevalence of inadequate intakes. When mean intakes of groups are below the AI, it is not possible to make any assumptions about the extent of intake inadequacy” (IOM, 2000, p. 12).
The sections that follow compare the potassium AI values established in this report to current potassium intakes in the U.S. and Canadian populations. Appendix G provides methodological details about the surveys used for this comparison, namely the U.S. National Health and Nutrition Examination Survey (NHANES), Canadian Community Health Survey–Nutrition 2015 (CCHS Nutrition 2015), and the Feeding Infants and Toddlers Study 2016 (FITS 2016). Data are presented by sex and age groups, as provided in these data sources. Details regarding the bias of using 24-hour dietary recalls to estimate distributions of usual intake compared to 24-hour urinary potassium excretions are presented in Chapter 3 (see Figure 3-1). Supplementary figures for select comparisons are provided in Appendix H.
Characterization by DRI Age, Sex, and Life-Stage Groups
Infants 0–12 Months of Age
The committee was provided with evidence on the distribution of usual potassium intake of U.S. infants (see Table 7-1). Among NHANES 2009–2014 infants 0–6 months of age who did not consume breast milk, estimated median potassium intake was 763 mg/d (20 mmol/d). Among FITS 2016 infants, which include both infants who did and did not consume breast milk, estimated median potassium intake was 625 mg/d (16 mmol/d). These median potassium intakes exceed the AI, which was derived by estimating potassium intake of breastfed infants and assumes an average breast milk potassium concentration of 515 mg/L. The committee notes that its estimate of breast milk potassium concentration may be lower than the value used to estimate intakes in FITS 2016 (see Chapter 4 and Appendix F).
Intake estimates for infants 7–12 months of age include potassium intakes from either breast milk, formula, or other milks in addition to complementary foods. Median usual potassium intakes among infants 7–12 months of age ranged from approximately 900–1,300 mg/d (23–33 mmol/d) and varied by whether infants included in the analyses consumed breast milk (see Table 7-2). Slightly more than half of infants who consumed some breast milk and more than 75 percent of infants who
TABLE 7-1 Usual Potassium Intake Among U.S. Infants 0–6 Months of Age, as Compared to the Potassium Adequate Intake
| Comparison Data Source | Age Range (Months) | Breastfeeding Status of Infants | Adequate Intake (mg/d) | Mean (mg/d)a | Percentile | ||
|---|---|---|---|---|---|---|---|
| 25th (mg/d) | 50th (mg/d) | 75th (mg/d) | |||||
| NHANES 2009–2014 | 0–6 | Not BF | 400 | 801 (16) | 618 | 763 | 941 |
| FITS 2016 | 0–5.9 | All | 400 | 659 (10) | 487 | 625 | 793 |
NOTES: Bold indicates the value is higher than the Adequate Intake for the DRI age, sex, and life-stage group. Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. No analyses were identified that estimated usual potassium intake distribution for breastfed infants 0–6 months of age. FITS 2016 = Feeding Infants and Toddlers Study 2016; mg/d = milligrams per day; NHANES = National Health and Nutrition Examination Survey; Not BF = analysis of infants who did not consume breast milk.
aPresented as intake (standard error).
SOURCES: Bailey et al., 2018; NHANES 2009–2014 (unpublished).
did not consume breast milk in this age group exceed the potassium AI. Infants who did not consume breast milk had higher potassium intakes than breastfed infants. This difference may reflect both the lower potassium content of breast milk compared to infant formula, and higher energy intakes in infants who are not breastfed with concomitant higher potassium intakes (Heinig et al., 1993; Whitehead, 1995).
Children and Adolescents 1–18 Years of Age
The 50th and 75th percentiles from the estimated distributions of usual potassium intakes among U.S. and Canadian children and adolescents are summarized in Table 7-3. The potassium AIs for children and adolescents 1–18 years of age were established using the highest median usual intakes in the U.S. and Canadian population within each DRI group. Therefore, the 50th percentiles approach or meet the AI values within the DRI groups for children and adolescents. Because it is unknown how the AI value relates to actual requirements, interpretation of intakes below the AI in terms of inadequacy cannot be made.
Adults 19 Years of Age and Older
The 75th percentile of usual potassium intake exceeds the potassium AI for most adult DRI age, sex, and life-stage groups, indicating that between
TABLE 7-2 Usual Potassium Intake Among U.S. Infants 7–12 Months of Age, as Compared to the Potassium Adequate Intake
| Comparison Data Source | Age Range (months) | Breastfeeding Status of Infants | Adequate Intake (mg/d) | Mean (mg/d)a | Percentile | ||
|---|---|---|---|---|---|---|---|
| 25th (mg/d) | 50th (mg/d) | 75th (mg/d) | |||||
| NHANES 2009–2014 | 7–12 | Not BF | 860 | 1,305 (32) | 1,039 | 1,263 | 1,526 |
| NHANES 2003–2010 | 7–11 | Not BF | 860 | 1,257 (26) | 1,051 | 1,212 | 1,418 |
| 7–11 | BFb | 860 | 901 (41) | 742 | 892 | 1,042 | |
| FITS 2016 | 6–11.9 | All | 860 | 1,125 (13) | 855 | 1,074 | 1,342 |
| NHANES 2003–2010 | 7–11 | All | 860 | 1,168 (21) | 963 | 1,133 | 1,334 |
| NHANES 2009–2012 | 6–11 | Allc | 860 | 1,119 (21) | 844 | 1,068 | 1,336 |
NOTES: Bold indicates the value is higher than the Adequate Intake for the DRI age, sex, and life-stage group. Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. BF = analysis of infants who consumed breast milk; FITS 2016 = Feeding Infants and Toddlers Study 2016; mg/d = milligrams per day; NHANES = National Health and Nutrition Examination Survey; Not BF = analysis of infants who did not consume breast milk.
aPresented as intake (standard error).
bConsumption of at least some breast milk, as reported on the 24-hour dietary recall.
cEstimated 23.9 ± 3.3 percent of this sample reported consuming any breast milk. SOURCES: Ahluwalia et al., 2016; Bailey et al., 2018; NHANES 2009–2014 (unpublished); Tian et al., 2013.
one-quarter and one-half of U.S. and Canadian adults exceed the AI (see Table 7-4). Median usual potassium intakes of the general U.S. and Canadian populations are lower than the observed median intakes in the normotensive population used to establish the potassium AI values. There were two adult DRI life-stage groups in which usual potassium intakes at the 75th percentiles were below the potassium AI: females 19–30 years of age in the United States and males older than 70 years of age in the United States and Canada. Because it is unknown how the AI relates to actual requirements, interpretation of intakes below the AI in terms of inadequacy cannot be made.
Characterization by Sex
On average, males had higher usual potassium intakes than females. As noted in Chapter 3, potassium intake is highly correlated with energy intake, leading to higher intakes of potassium with greater energy intakes.
TABLE 7-3 50th and 75th Percentiles of Usual Potassium Intake Among U.S. and Canadian Children and Adolescents 1–18 Years of Age, as Compared to the Potassium Adequate Intakes
| DRI Group | AI (mg/d) | 50th Percentile (mg/d)a | 75th Percentile (mg/d)a | Percent > AI |
|---|---|---|---|---|
| Both sexes, 1–3 years | ||||
| U.S., both sexes | 2,000 | 1,944 (24) | 2,279 (32) | 45 |
| Canada, males | 2,000 | 2,042 (45) | 2,450 (49) | 53 |
| Canada, females | 2,000 | 1,934 (51) | 2,324 (58) | 45 |
| Both sexes, 4–8 years | ||||
| U.S., both sexes | 2,300 | 2,094 (19) | 2,432 (24) | 33 |
| Canada, males | 2,300 | 2,349 (49) | 2,764 (56) | 53 |
| Canada, females | 2,300 | 2,134 (45) | 2,509 (54) | 37 |
| Males, 9–13 years | ||||
| U.S. | 2,500 | 2,331 (38) | 2,734 (55) | 38 |
| Canada | 2,500 | 2,516 (44) | 3,007 (55) | 50 |
| Males, 14–18 years | ||||
| U.S. | 3,000 | 2,628 (52) | 3,123 (74) | 30 |
| Canada | 3,000 | 2,984 (77) | 3,680 (97) | 49 |
| Females, 9–13 years | ||||
| U.S. | 2,300 | 2,050 (33) | 2,392 (53) | 30 |
| Canada | 2,300 | 2,263 (44) | 2,683 (55) | 47 |
| Females, 14–18 years | ||||
| U.S. | 2,300 | 1,914 (43) | 2,267 (53) | 23 |
| Canada | 2,300 | 2,255 (49) | 2,747 (58) | 47 |
NOTES: Bold indicates the value is higher than the Adequate Intake for the DRI age, sex, and life-stage group. Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. AI = Adequate Intake; mg/d = milligrams per day; U.S. = United States.
aPresented as intake (standard error). SOURCES: CCHS Nutrition 2015 (unpublished); NHANES 2009–2014 (unpublished).
The difference in intakes between males and females informed the committee’s decision to stratify potassium AIs by sex for individuals 9 years of age and older. Although no statistical comparisons were carried out to explore differences, the percent of the population with intakes above the AI was relatively similar in males and females in each of the DRI age groups.
Characterization by Country
Although no statistical comparisons were carried out to explore differences, median and 75th percentile of potassium intakes are relatively comparable between the United States and Canada for many DRI age,
TABLE 7-4 50th and 75th Percentiles of Usual Potassium Intake Among U.S. and Canadian Adults 19 Years of Age and Older, as Compared to the Potassium Dietary Reference Intake Values
| DRI Group | AI (mg/d) | 50th Percentile (mg/d)a | 75th Percentile (mg/d)a | Percent > AI |
|---|---|---|---|---|
| Males, 19–30 years | ||||
| U.S. | 3,400 | 2,825 (40) | 3,475 (62) | 27 |
| Canada | 3,400 | 2,973 (87) | 3,540 (117) | 30 |
| Males, 31–50 years | ||||
| U.S. | 3,400 | 3,098 (31) | 3,703 (50) | 36 |
| Canada | 3,400 | 2,945 (59) | 3,618 (204) | 32 |
| Males, 51–70 years | ||||
| U.S. | 3,400 | 3,065 (32) | 3,709 (66) | 35 |
| Canada | 3,400 | 2,927 (51) | 3,576 (69) | 30 |
| Males, > 70 years | ||||
| U.S. | 3,400 | 2,783 (35) | 3,324 (56) | 22 |
| Canada | 3,400 | 2,615 (46) | 3,169 (57) | 17 |
| Females, 19–30 years | ||||
| U.S. | 2,600 | 2,119 (31) | 2,509 (44) | 20 |
| Canada | 2,600 | 2,296 (73) | 2,771 (125) | 32 |
| Females, 31–50 years | ||||
| U.S. | 2,600 | 2,366 (19) | 2,845 (30) | 36 |
| Canada | 2,600 | 2,404 (44) | 2,744 (80) | 34 |
| Females, 51–70 years | ||||
| U.S. | 2,600 | 2,425 (25) | 2,899 (33) | 40 |
| Canada | 2,600 | 2,418 (35) | 2,900 (41) | 39 |
| Females, > 70 years | ||||
| U.S. | 2,600 | 2,312 (27) | 2,805 (38) | 34 |
| Canada | 2,600 | 2,179 (41) | 2,652 (48) | 27 |
| Pregnant | ||||
| U.S. | 2,600/2,900b | 2,533 (87)c | 3,090 (116)c | 32c |
| Canada | 2,600/2,900b | 2,876 (134)c | 3,294 (175)c | 48c |
| Lactating | ||||
| U.S. | 2,500/2,800d | 2,675 (104)e | 3,079 (110)e | 41e |
| Canada | 2,500/2,800d | 2,814 (111)e | 3,211 (158)e | 51e |
NOTES: Bold indicates the value is higher than the AI for the DRI age, sex, and life-stage group. Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. AI = Adequate Intake; mg/d = milligrams per day.
aPresented as intake (standard error).
bPotassium AI presented by age groups, pregnant females 14–18 years of age/pregnant females 19 years of age and older.
cIntakes are compared to the AI for pregnant females 19 years of age and older.
dPotassium AI presented by age groups, lactating females 14–18 years of age/lactating females 19 years of age and older.
eIntakes are compared to the AI for lactating females 19 years of age and older.
SOURCES: CCHS Nutrition 2015 (unpublished); NHANES 2009–2014 (unpublished).
sex, and life-stage groups (see Tables 7-3 and 7-4). An exception was the group of Canadian males 14–18 years of age, who reported a higher usual intake of potassium than the corresponding group in the United States. The difference for this group was more than 340 mg/d (9 mmol/d). Methods for collecting 24-hour dietary recalls, nutrient databases, and statistical methods used to estimate intakes were similar between the U.S. and Canadian surveys, and therefore would not be expected to explain these differences (CDC/NCHS, 2019; Statistics Canada, 2017; and see Appendix G for details of the methodology). Because it is unknown how the AI relates to actual requirements, and because there is no Tolerable Upper Intake Level (UL) for potassium, the implications of the differences cannot be inferred.
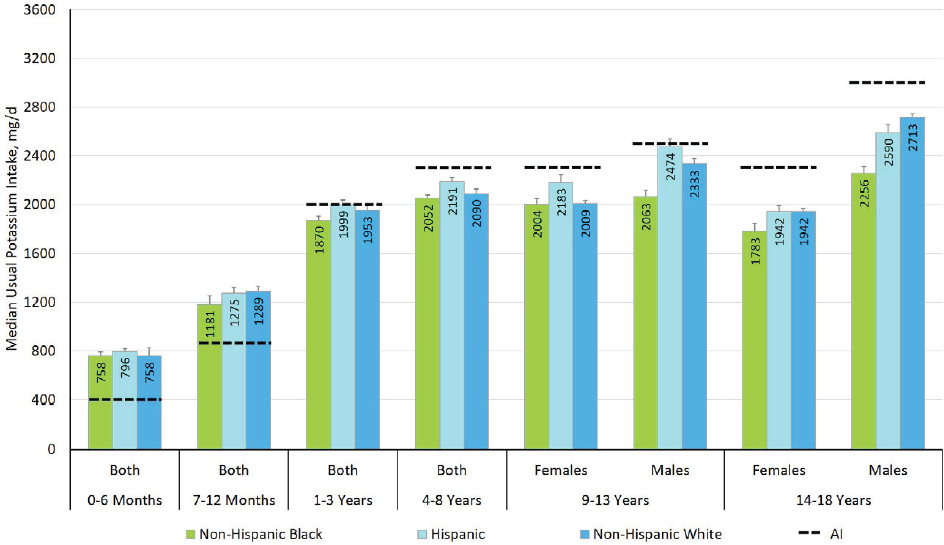
Characterization by Race and Ethnicity Groups
For the United States, distributions of the usual potassium intake were estimated by three race/ethnicity categories: non-Hispanic white, non-Hispanic black, and Hispanic (see Figures 7-1 and 7-2). Although no statistical comparisons were made, the median intakes were lowest for non-Hispanic blacks in each of the DRI age, sex, and life-stage groups. For some DRI groups, the differences were quite small (e.g., for females 19–30 years of age median intakes differed by 51 mg/d between non-Hispanic blacks and non-Hispanic whites); for other DRI groups, differences in median intakes were larger (e.g., for males older than 70 years of age, median intakes differed by more than 700 mg/d between non-Hispanic blacks and non-Hispanic whites). Almost all adult groups and children 14–18 years of age among Hispanics and among non-Hispanic blacks had usual daily intakes of potassium that are 500 mg/d or more below the AI. Although it is not known how the AI relates to requirements, these groups ought to be encouraged to increase their potassium intake to meet the AI. A comparable stratified analysis was not available for Canada.
Risk Characterization by Hypertension Status
Although the apparently healthy population used to derive the adult potassium AIs were normotensive, there is no indication that the AIs cannot be applied to hypertensive individuals, with the exception of those taking medications that may interfere with blood potassium levels (see Special Considerations section below).
For the United States and Canada, distributions of the usual potassium intakes were stratified by hypertension status. In the Canadian distributions, hypertension status was self-reported and stratified into two catego-
SOURCE: NHANES 2009–2014 (unpublished).

NOTES: Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. AI = Adequate Intake; mg/d = milligrams per day.
SOURCE: NHANES 2009–2014 (unpublished).
ries, based on the question “Do you have high blood pressure?” (Statistics Canada, 2017). In the U.S. distributions, hypertension status was stratified into three categories—normotensive, elevated blood pressure, and hypertensive. Hypertension status was defined using the 2017 American College of Cardiology and the American Heart Association guidelines for adults (Whelton et al., 2018), based on the mean of up to three consecutive blood pressure measurements or use of hypertensive medications. In both analyses, individuals who self-reported having a history of cardiovascular disease were excluded.1 For comparability between the United States and Canada, the elevated blood pressure group from the NHANES 2009–2014 data is omitted from this section.
In some DRI life-stage groups, median usual potassium intakes were higher in normotensive individuals compared to individuals with hypertension, particularly for males 51–70 years of age and females 51 years of age and older (see Figure 7-3). It is difficult to know why these groups differ. Possible explanations for the difference might be that those with higher potassium intakes have lower blood pressure, and/or those with hypertension taking angiotensin-converting enzyme inhibitors (ACE-Is), angiotensin II receptor blockers (ARBs), or renin inhibitor medications avoid potassium-rich food sources and potassium supplements because of the potassium-sparing effects of these drugs. Populations taking such medications are described below as a special consideration. Because it is unknown how the AI relates to actual requirements, and because there is no potassium UL, the implications of the differences cannot be inferred.
SOURCES OF POTASSIUM IN THE DIET
Various cycles of NHANES data have been used to characterize leading contributors of potassium intake (Hoy and Goldman, 2012; NIH/NCI, 2018b; O’Neil et al., 2012, 2018) (see Tables 7-5 through 7-8). The age-stratified analyses provide evidence that there are certain foods that commonly contribute a sizeable proportion of potassium intake in the diets of children, adolescents, and adults, including milk, white potatoes, and fruit. The age-stratified analyses also provide evidence of variation in relative contribution and some differences in top food contributors across age groups. Furthermore, the tables highlight how different approaches to grouping foods can lead to different rankings of the top contributors to
___________________
1 The NHANES usual potassium intake distribution stratified by hypertension status excluded anyone who had reported that a doctor or other health professional had ever told them they had a stroke or heart attack (myocardial infarction). The CCHS Nutrition 2015 usual potassium intake distribution stratified by hypertension status excluded anyone who had reported that a health professional had ever told them they had heart disease. Participants who answered that they did not know or refused to answer were also excluded.
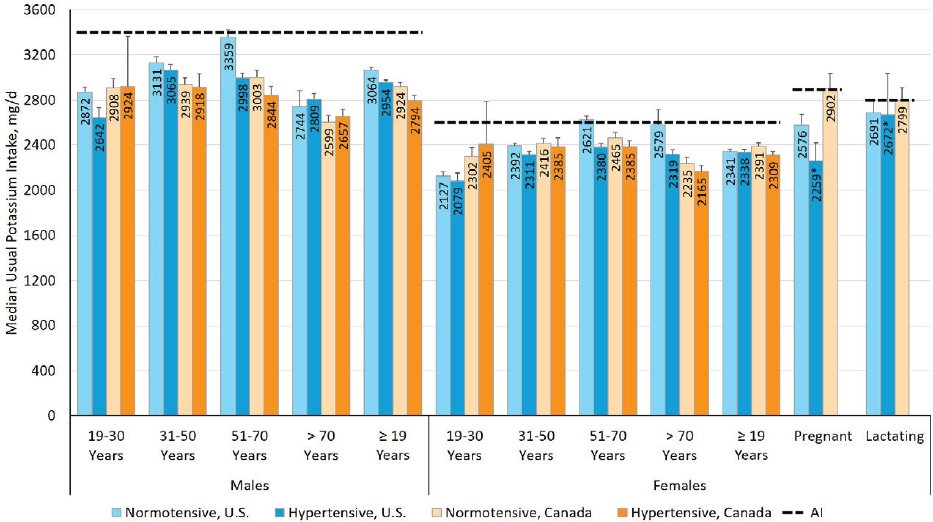
NOTES: Intake values are presented in milligrams. To convert the milligram value to mmol, divide the intake level by 39.1. * = estimate statistically unstable; AI = Adequate Intake; mg/d = milligrams per day. This note was revised since the prepublication release.
SOURCES: CCHS Nutrition 2015 (unpublished); NHANES 2009–2014 (unpublished).
potassium intake. Fruits, for instance, are broadly grouped in two of the analyses and appear among the top contributors across the age-stratified analyses (O’Neil et al., 2012, 2018). In contrast, the analysis in which fruits do not appear among the top contributors to potassium intake used several, more narrowly defined fruit groups (e.g., bananas, citrus fruits, grapes) (NIH/NCI, 2018a,b).
Table 7-9 presents foods with the highest amounts of potassium per standard food portion. Synthesizing this information with the evidence presented in Tables 7-5 through 7-8 shows that the foods that are among the highest in potassium content are not necessarily the top contributors to potassium intake in the diet. Foods with lower potassium content per standard portion can contribute to a substantial proportion of total potassium intake when such foods are consumed commonly and in large quantities. Similarly, foods that are high in potassium may not make a substantial contribution to total potassium intake if the food is not commonly consumed or is consumed only in small quantities.
Food fortification and dietary supplements contribute minimally to total potassium intake. An analysis of NHANES 2003–2006 data reported that, of 2,616 mg/d (67 mmol/d) potassium consumed among individuals
TABLE 7- 5 Percent Contribution of Food Categories to Potassium Intake—National Health and Nutrition Examination Survey, 2009–2010
| Food Categories | Individuals Reporting (%)a | Contribution to Potassium (%) |
|---|---|---|
| Fruits and vegetables | 81 | 20 |
| Milk and milk drinksb | 55 | 11 |
| Meats and poultry | 66 | 10 |
| Grain-based mixed dishesc | 50 | 10 |
| Coffee and tea | 55 | 7 |
| 100 percent juices | 25 | 5 |
| Meat/poultry mixed dishesd | 18 | 4 |
| Plant-based protein foodse | 27 | 4 |
| Savory snacksf | 45 | 3 |
NOTE: Data are from What We Eat In America, National Health and Nutrition Examination Survey 2009–2010, day 1 dietary intake data, weighted, excluding breastfed infants.
aPercent of individuals reporting the foods in the category at least once on the reporting day.
bIncludes milk (all fat levels), flavored milk, milk substitutes, and milkshakes.
cIncludes pasta mixed dishes, macaroni and cheese, rice mixed dishes, pizza, sandwiches, burritos, tacos, and tamales.
dIncludes dishes in which meat or poultry is the main ingredient with grain and/or vegetables, gravies, or sauces.
eIncludes beans or peas, mixed dishes with beans or peas, nuts and seeds, and soy products. fIncludes chips, crackers, popcorn, and pretzels.
SOURCE: Hoy and Goldman, 2012.
TABLE 7-6 Top 10 Food Categories Contributing to Potassium Intake Among U.S. Persons 2 Years of Age and Older, Ranked by Percent Contribution—National Health and Nutrition Examination Survey, 2005–2006 (N = 8,549a)
| Rank | Food Category | Percent Contributionb |
|---|---|---|
| 1 | Reduced-fat milk | 5.9 |
| 2 | Coffee | 5.2 |
| 3 | Chicken and chicken mixed dishes | 4.5 |
| 4 | Beef and beef mixed dishes | 3.6 |
| 5 | 100 percent orange/grapefruit juice | 3.4 |
| 6 | Fried white potatoes | 3.3 |
| 7 | Potato/corn/other chips | 3.2 |
| 8 | Whole milk | 2.9 |
| 9 | Other white potatoes | 2.9 |
| 10 | Pasta and pasta dishes | 2.7 |
aThis number was revised since the prepublication release.
bMean potassium intake for this analysis was 2,617 mg/d (67 mmol/d).
SOURCE: Adapted from NIH/NCI, 2018b.
TABLE 7-7 Top 10 Food Categories Contributing to Potassium Intake Among U.S. Persons 2–18 Years of Age, Ranked by Percent Contribution—National Health and Nutrition Examination Survey, 2011–2014 (N = 5,876)
| Rank | 2–5 Years of Age (n = 1,511) | |
|---|---|---|
| Food Group | Percent Contributiona | |
| 1 | Milk | 21.1 |
| 2 | Fruits | 9.6 |
| 3 | 100 percent fruit juice | 8.5 |
| 4 | Flavored milk | 5.1 |
| 5 | Vegetablesd | 3.9 |
| 6 | White potatoes | 3.9 |
| 7 | Grain-based mixed dishes | 3.7 |
| 8 | Poultry | 3.5 |
| 9 | Savory snacks | 3.1 |
| 10 | Sweetened beverages | 3.0 |
NOTES: Food groups are from the 47 subgroups defined by the What We Eat In America food category classification system. The percent contributions reflected in the table were adjusted to disaggregate dairy intake from nondairy foods (e.g., mixed dishes) and reallocate them to the milk, cheese, and yogurt subgroups, as appropriate.
aMean potassium intake for this group was 1,982 mg/d (51 mmol/d).
bMean potassium intake for this group was 2,198 mg/d (56 mmol/d).
TABLE 7-8 Top 10 Food Categories Contributing to Potassium Intake Among U.S. Persons 19 Years of Age and Older, Ranked by Percent Contribution—National Health and Nutrition Examination Survey, 2003–2006 (N = 9,490)
| Rank | 19–50 Years of Age (n = 5,429) | |
|---|---|---|
| Food Group | Percent Contributiona | |
| 1 | Milk | 9.7 |
| 2 | Coffee, tea, other nonalcoholic beverages | 7.0 |
| 3 | White potatoes | 6.9 |
| 4 | Tomatoes, tomato/vegetable juice | 6.1 |
| 5 | Beef | 5.7 |
| 6 | Fruit juice | 5.2 |
| 7 | Fruit | 4.5 |
| 8 | Poultry | 4.4 |
| 9 | Crackers, popcorn, pretzels, chips | 4.1 |
| 10 | Other vegetables | 3.4 |
NOTES: Food groups were defined by the U.S. Department of Agriculture Dietary Sources Nutrient database, which were collapsed into 51 categories for the analysis.
aMean potassium intake for this group was 2,783 mg/d (71 mmol/d).
bMean potassium intake for this group was 2,659 mg/d (68 mmol/d).
| 6–11 Years of Age (n = 2,193) | 12–18 Years of Age (n = 2,172) | ||
|---|---|---|---|
| Food Group | Percent Contributionb | Food Group | Percent Contributionc |
| Milk | 15.6 | Milk | 15.0 |
| Fruits | 7.3 | White potatoes | 6.1 |
| Flavored milk | 5.7 | Fruits | 5.6 |
| 100 percent juice | 5.3 | 100 percent fruit juice | 4.6 |
| White potatoes | 4.5 | Poultry | 4.5 |
| Savory snacks | 4.0 | Vegetablesd | 4.1 |
| Poultry | 3.9 | Savory snacks | 4.0 |
| Pizza | 3.7 | Mexican mixed dishes | 3.9 |
| Grain-based mixed dishes | 3.7 | Grain-based mixed dishes | 3.7 |
| Mexican mixed dishes | 3.6 | Meats | 3.7 |
cMean potassium intake for this group was 2,308 mg/d (59 mmol/d).
dExcludes white potatoes.
SOURCE: Adapted from O’Neil et al., 2018. Reprinted with permission under the Creative Commons Attribution (CC BY) license (http://creative-commons.org/licenses/by/4.0) (accessed January 18, 2019).
| ≥ 51 Years of Age (n = 4,061) | |
|---|---|
| Food Group | Percent Contributionb |
| Coffee, tea, other nonalcoholic beverages | 10.8 |
| Milk | 9.5 |
| Fruit | 8.0 |
| White potatoes | 6.4 |
| Tomatoes, tomato/vegetable juice | 5.5 |
| Fruit juice | 4.8 |
| Beef | 4.4 |
| Other vegetables | 3.5 |
| Poultry | 3.2 |
| Yeast breads and rolls | 3.1 |
SOURCE: Adapted from O’Neil et al., 2012. Reprinted with permission under the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0) (accessed January 18, 2019).
TABLE 7-9 Food Sources Ranked by Amount of Potassium per Standard Portions, as Presented in the 2015 Dietary Guidelines Advisory Committee Report
| Food | Potassium (mg) | ||
|---|---|---|---|
| Standard Portion | Per Standard Portion | Per 100 grams | |
| Potato, baked, flesh and skin | 1 medium | 941 | 544 |
| Prune juice, canned | 1 cup | 707 | 276 |
| Carrot juice, canned | 1 cup | 689 | 292 |
| Passion-fruit juice, yellow or purple | 1 cup | 687 | 278 |
| Tomato paste, canned | ¼ cup | 669 | 1,014 |
| Beet greens, cooked from fresh | ½ cup | 654 | 909 |
| Adzuki beans, cooked | ½ cup | 612 | 532 |
| White beans, canned | ½ cup | 595 | 454 |
| Plain yogurt, nonfat | 1 cup | 579 | 255 |
| Tomato puree | ½ cup | 549 | 439 |
| Sweet potato, baked in skin | 1 medium | 542 | 475 |
| Salmon, Atlantic, wild, cooked | 3 ounces | 534 | 628 |
| Clams, canned | 3 ounces | 534 | 628 |
| Pomegranate juice | 1 cup | 533 | 214 |
| Plain yogurt, low-fat | 1 cup | 531 | 234 |
| Tomato juice, canned | 1 cup | 527 | 217 |
NOTES: This table presents an excerpt from the 2015 Dietary Guidelines Advisory Committee Report of food sources with ≥ 500 mg potassium per standard portion. The data were cited as being from the U.S. Department of Agriculture National Nutrient Database for Standard Reference, Release 27. Potassium contents are presented in milligrams. To convert the milligram value to mmol, divided by 39.1. mg = milligrams.
SOURCE: Adapted from DGAC, 2015.
2 years of age and older, an average of 20 mg/d (0.5 mmol/d) came from fortification (Fulgoni et al., 2011). Potassium from fortification has been reported to contribute 0.2 to 0.6 percent of total potassium intake among children 2–18 years of age (Berner et al., 2014). Multivitamin and mineral supplements provide similarly small amounts of potassium. An analysis of NHANES 2007–2010 data of individuals 4 years of age and older found that multivitamin/mineral supplements provide approximately 11 mg/d (0.3 mmol/d) potassium to the overall estimated usual potassium intake of 2,606 mg/d (67 mmol/d) (Wallace et al., 2014). Use of multivitamin/mineral supplements containing potassium among adults 20 years of age and older appears to be declining. In 2011–2012, 18 percent [95% confidence interval (CI): 16, 19] of adults reported using a potassium-containing multivitamin/mineral supplement in the previous 30 days; the prevalence in 1999–2000 was estimated to be 28 percent [95% CI: 26, 30] (Kantor et al., 2016). Potassium-containing supplement use appears to be low among
older adults, with an estimated 1.7 percent of adults 60 years of age and older reported using a potassium-containing dietary supplement in the previous 30 days (Gahche et al., 2017).
PUBLIC HEALTH IMPLICATIONS AND SPECIAL CONSIDERATIONS
To interpret the findings from the risk characterization analysis presented above, consideration is given to the meaning and use of AIs. AIs are recommended average daily nutrient intake levels that are established when the intake distribution of requirements could not be established. To that end, an AI, including the potassium AIs established in this report, does not necessarily reflect requirements, but rather reflects the best estimate of intakes assumed to be adequate. Despite the uncertainties that exist with the potassium AIs, the values presented in this report reflect intake levels that are intended to be broadly applicable to the U.S. and Canadian populations. Nevertheless, there are certain situations and subpopulations in which potassium intakes may need to differ from the AI. Such special considerations are described below, and followed by a discussion of the implications of the updated potassium DRI values.
Special Considerations
Excessive Sweat Losses
Individuals who are exposed to high temperatures or those who engage in high levels of physical activity, especially at high temperatures, may require potassium intakes higher than the AI because of higher than usual losses of potassium through elevated sweat levels, ranging from 390–2,300 mg/d (10–60 mmol/d) (Consolazio et al., 1963; Costill et al., 1982; Malhotra et al., 1976, 1981). Typically, potassium concentrations in sweat in adults at ambient temperature and moderate levels of physical activity range from 100–300 mg/L (3–7 mmol/L) sweat, with total losses estimated to be approximately 78–137 mg/d (2–4 mmol/d) (EFSA NDA et al., 2016; IOM, 2005). Additionally, potassium sweat concentrations can increase up to 500 mg/L (14 mmol/L) sweat at high temperatures (Fukumoto et al., 1988), but they are less elevated in heat-acclimatized individuals exposed to high temperatures (40°C [104°F]), being approximately 200 mg/L (5 mmol/L) (Malhotra et al., 1976). Even in heat-acclimatized individuals exposed to high temperatures, total potassium sweat loss is still greater, at approximately 2,300 mg/d (60 mmol/d), owing to 20-fold greater sweat production of approximately 8 L/d (Malhotra et al., 1976).
Individuals Taking Medications That Affect Potassium Retention and Excretion
Recent major hypertension guidelines have recommended more intensive blood pressure lowering targets for individuals with hypertension; ACE-Is and ARBs are recommended among first-line pharmaceutical agents for hypertension treatment (Whelton et al., 2018). Using a systolic blood pressure threshold for treatment of ≥ 130 mm Hg, the proportion of the U.S. population that may require pharmacological antihypertensive therapy is estimated to be 36 percent (Muntner et al., 2018). ACE-Is and ARBs are also used frequently in heart failure populations; these individuals typically have high serum potassium concentrations, and are likely to have a higher risk of potassium toxicity.
Persons taking medications that alter regulation of potassium homeostasis through increased retention or excretion of potassium represent a special population for whom the applicability of the potassium AI is uncertain. For example, persons taking ACE-Is or ARBs may have a higher risk of developing hyperkalemia on a diet enriched with potassium (Cappuccio et al., 2016). Similar consideration needs to be given to persons taking other medications that influence potassium homeostasis, such as potassium-sparing diuretics. Conversely, many non-potassium-sparing diuretics induce urinary loss of potassium and can lower serum potassium concentrations in some individuals. Such individuals may require greater potassium intake. Some studies suggest that repletion of potassium in this setting may enhance the antihypertensive effects of these medications (Kaplan et al., 1985). In these cases and under the guidance of a health care provider, intakes that deviate from the AI may be warranted.
Heart failure is estimated to affect 5.7 million adults in the United States (Mozaffarian et al., 2016). Treatment for heart failure often includes treatment with ACE-Is/ARBs and diuretics; certain diuretic classes can cause hypokalemia or hyperkalemia (Pitt et al., 1999). These medications are often used in combination, and balancing the specific medications and their doses is often guided by serum potassium concentrations. Thus, it is uncertain if the potassium AI is applicable to individuals with heart failure.
Adrenal Insufficiency
Adrenal insufficiency is a rare condition; nonetheless, this disease is characterized by mineralocorticoid hormone levels below homeostatic requirements. Individuals with this condition are characterized by hyperkalemia. The potassium AI may not be appropriate in individuals with this condition.
Chronic Kidney Disease
Impaired renal potassium excretion commonly leads to hyperkalemia in patients with chronic kidney disease (CKD). On the other hand, use of potassium-wasting diuretics and restriction of potassium-rich foods, such as fruits and vegetables, in patients with CKD can lead to hypokalemia (Gilligan and Raphael, 2017; Kovesdy et al., 2017). Although hyperkalemia is a well-recognized complication of CKD, the prevalence of hyperkalemia (14 to 20 percent) and hypokalemia (12 to 18 percent) is similar in CKD patients (Gilligan and Raphael, 2017). Both hyperkalemia and hypokalemia are independently associated with increased risk of cardiovascular disease, hospitalization, and all-cause deaths among patients with CKD (Hoppe et al., 2018; Luo et al., 2016). In 3,939 patients with CKD from the Chronic Renal Insufficiency Cohort Study, the highest quartile of urinary potassium excretion (≥ 2,624 mg/d [≥ 67 mmol/d]) was significantly associated with increased risk of CKD progression but not all-cause mortality (He et al., 2016). A post-hoc analysis including 812 participants from the Modification of Diet in Renal Disease Study, however, reported higher baseline urinary potassium level being associated with a lower risk of all-cause mortality but not kidney failure (Leonberg-Yoo et al., 2017). Patients with CKD need to consult with their health care providers about individualized potassium intake recommendation, because of variations in the severity of kidney function decline, comorbidities, and use of medications such as ACE-I.
Type 2 Diabetes
The prevalence of type 2 diabetes is high and increasing in the general population. In 2011–2012, the estimated prevalence of diabetes was 12 to 14 percent among U.S. adults, depending on the criteria used (Menke et al., 2015). General population studies demonstrate that the presence of type 2 diabetes is associated with hyperkalemia (Hughes-Austin et al., 2017). This is likely attributable to the wide use of ACE-I/ARB and a higher prevalence of CKD among persons with type 2 diabetes. However, even among individuals with type 2 diabetes who do not have kidney disease and are not taking ACE-I/ARBs, hyperkalemia may be more common because of hyporeninemic hypoaldosteronism and other comorbidities or cotreatments (Dojki and Bakris, 2018). These data suggest that persons with diabetes may have an elevated risk of hyperkalemia and associated adverse health consequences if potassium intake is too high. However, higher potassium intake has also been associated with the slower decline of kidney function and lower incidence of cardiovascular complications in type 2 diabetic patients with normal renal function (Araki et al., 2015). Thus, the applica-
bility of the potassium AIs for persons with type 2 diabetes is uncertain, and its application will likely need to be individualized in consultation with a health care provider, with consideration of the individual’s kidney function, medication use, and serum potassium concentrations.
Implications of the Potassium DRI Values in Context of the Previous Values and the Expanded DRI Model
The potassium DRI values in this report reflect the committee’s synthesis of a broad range of evidence on adequate and safe levels of potassium intake and the relationship between potassium and chronic disease. To contextualize the public health implications, the committee provides comment on each of the DRI categories.
The potassium AIs, as with all AIs, are intake levels that do not necessarily reflect requirements, but rather are the best estimates for intake levels in apparently healthy individuals. The potassium AIs established in this report are almost all lower than the values established in the Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate (2005 DRI Report) (IOM, 2005). This change is underpinned by several factors. More rigorous data analysis methodologies for synthesizing data, for instance, have emerged and are now incorporated in the DRI process. This committee had available for its use a prepared systematic review that assessed risk of bias and strength of the evidence. Furthermore, this committee reviewed the evidence using an expanded DRI model, in which consideration of chronic disease risk reduction was separate from consideration of adequacy. The evolution of the data, processes, and DRI model led the committee to use the median intake of groups of apparently healthy people to derive the potassium AI values. The potassium AI values are no longer informed by evidence from potassium supplement trials on blunting the effects of salt-sensitive rise in blood pressure, which was the case with the levels established in the 2005 DRI Report. Food pattern modeling evidence from the 2015 Dietary Guidelines Advisory Committee revealed that, for many energy levels, it was not possible to meet the potassium AI established in the 2005 DRI Report while meeting intake requirement for other nutrients (DGAC, 2015). Given the basis of the potassium AIs in this report, potassium intakes at or above the AI through dietary intake alone are more feasible than the potassium AIs established in the 2005 DRI Report.
There was insufficient evidence of toxicological risk to establish a potassium UL, aligned with what was concluded in the 2005 DRI Report. The committee notes that the lack of a UL does not necessarily reflect a lack of risk, but rather a lack of evidence of risk. As noted above, there are select population groups in whom retention and excretion of potassium
are altered, which may put them at risk of hyperkalemia. At present, the available evidence suggests that dietary potassium intakes in the ranges currently consumed in the United States and in Canada appear to be safe and reflect little or insubstantial contribution from food fortification and dietary supplements.
The committee’s inability to establish a potassium DRI based on chronic disease reflects limitations in the evidence. Although there was evidence that potassium supplements decreased blood pressure, notably in individuals with hypertension, an intake–response relationship could not be established and the heterogeneity across studies could not be explained. The committee was further limited in its ability to consider blood pressure a qualified surrogate marker, in context of potassium intake, as evidence on the independent effect of potassium intake on cardiovascular disease risk is lacking. Pursuant to the guidance and recommendations offered in the Guiding Principles for Developing Dietary Reference Intakes Based on Chronic Disease (NASEM, 2017), the committee did not establish a potassium DRI based on chronic disease. The committee recognizes that higher potassium intakes are related to blood pressure reductions, particularly among hypertensive adults. Although this relationship could not, for the reasons stated, be used to develop a potassium DRI based on chronic disease, or could not otherwise be quantified, it nevertheless suggests that higher potassium intake through the diet will likely benefit populations with elevated blood pressure. In the absence of quantitative intake–response data for the potassium and blood pressure relationship, all persons (except the at-risk subpopulations described above), and particularly hypertensive adults, might benefit from achieving intakes at the level of the AI and to consult with health care providers as to whether higher intakes might be needed.
REFERENCES
Ahluwalia, N., K. A. Herrick, L. M. Rossen, D. Rhodes, B. Kit, A. Moshfegh, and K. W. Dodd. 2016. Usual nutrient intakes of US infants and toddlers generally meet or exceed Dietary Reference Intakes: Findings from NHANES 2009-2012. American Journal of Clinical Nutrition 104(4):1167-1174.
Araki, S., M. Haneda, D. Koya, K. Kondo, S. Tanaka, H. Arima, S. Kume, J. Nakazawa, M. Chin-Kanasaki, S. Ugi, H. Kawai, H. Araki, T. Uzu, and H. Maegawa. 2015. Urinary potassium excretion and renal and cardiovascular complications in patients with type 2 diabetes and normal renal function. Clinical Journal of the American Society of Nephrology 10(12):2152-2158.
Bailey, R. L., D. J. Catellier, S. Jun, J. T. Dwyer, E. F. Jacquier, A. S. Anater, and A. L. Eldridge. 2018. Total usual nutrient intake of US children (under 48 months): Findings from the Feeding Infants and Toddlers Study (FITS) 2016. Journal of Nutrition 148(9S):1557S-1566S.
Berner, L. A., D. R. Keast, R. L. Bailey, and J. T. Dwyer. 2014. Fortified foods are major contributors to nutrient intakes in diets of US children and adolescents. Journal of the Academy of Nutrition and Dietetics 114(7):1009-1022.
Cappuccio, F. P., L. A. Buchanan, C. Ji, A. Siani, and M. A. Miller. 2016. Systematic review and meta-analysis of randomised controlled trials on the effects of potassium supplements on serum potassium and creatinine. BMJ Open 6(8):e011716.
CDC/NCHS (Centers for Disease Control and Prevention/National Center for Health Statistics). 2019. National Health and Nutrition Examination Survey. https://www.cdc.gov/nchs/nhanes/index.htm (accessed February 12, 2019).
Consolazio, C. F., L. O. Matoush, R. A. Nelson, R. S. Harding, and J. E. Canham. 1963. Excretion of sodium, potassium, magnesium and iron in human sweat and the relation of each to balance and requirements. Journal of Nutrition 79:407-415.
Costill, D. L., R. Cote, and W. J. Fink. 1982. Dietary potassium and heavy exercise: Effects on muscle water and electrolytes. American Journal of Clinical Nutrition 36(2):266-275.
DGAC (Dietary Guidelines Advisory Committee). 2015. Scientific report of the 2015 Dietary Guidelines Advisory Committee: Advisory report to the Secretary of Health and Human Services and the Secretary of Agriculture. Washington, DC: U.S. Department of Agriculture, Agricultural Research Service.
Dojki, F. K., and G. L. Bakris. 2018. Blood pressure control and cardiovascular renal outcomes. Endocrinology and Metabolism Clinics of North America 47(1):175-184.
EFSA NDA (European Food Safety Authority Panel on Dietetic Products, Nutrition and Allergies), D. Turck, J.-L. Bresson, B. Burlingame, T. Dean, S. Fairweather-Tait, M. Heinonen, K. I. Hirsch-Ernst, I. Mangelsdorf, H. McArdle, M. Neuhäuser-Berthold, G. Nowicka, K. Pentieva, Y. Sanz, A. Siani, A. Sjödin, M. Stern, D. Tomé, H. Van Loveren, M. Vinceti, P. Willatts, P. Aggett, A. Martin, H. Przyrembel, A. Brönstrup, J. Ciok, J. Á. Gómez Ruiz, A. de Sesmaisons-Lecarré, and A. Naska. 2016. Dietary reference values for potassium. EFSA Journal 14(10).
Fukumoto, T., T. Tanaka, H. Fujioka, S. Yoshihara, T. Ochi, and A. Kuroiwa. 1988. Differences in composition of sweat induced by thermal exposure and by running exercise. Clinical Cardiology 11(10):707-709.
Fulgoni, V. L., 3rd, D. R. Keast, R. L. Bailey, and J. Dwyer. 2011. Foods, fortificants, and supplements: Where do Americans get their nutrients? Journal of Nutrition 141(10):1847-1854.
Gahche, J. J., R. L. Bailey, N. Potischman, and J. T. Dwyer. 2017. Dietary supplement use was very high among older adults in the United States in 2011-2014. Journal of Nutrition 147(10):1968-1976.
Gilligan, S., and K. L. Raphael. 2017. Hyperkalemia and hypokalemia in CKD: Prevalence, risk factors, and clinical outcomes. Advances in Chronic Kidney Disease 24(5):315-318.
He, J., K. T. Mills, L. J. Appel, W. Yang, J. Chen, B. T. Lee, S. E. Rosas, A. Porter, G. Makos, M. R. Weir, L. L. Hamm, and J. W. Kusek. 2016. Urinary sodium and potassium excretion and CKD progression. Journal of the American Society of Nephrology 27(4):1202-1212.
Heinig, M. J., L. A. Nommsen, J. M. Peerson, B. Lonnerdal, and K. G. Dewey. 1993. Energy and protein intakes of breast-fed and formula-fed infants during the first year of life and their association with growth velocity: The DARLING Study. American Journal of Clinical Nutrition 58(2):152-161.
Hoppe, L. K., D. C. Muhlack, W. Koenig, P. R. Carr, H. Brenner, and B. Schottker. 2018. Association of abnormal serum potassium levels with arrhythmias and cardiovascular mortality: A systematic review and meta-analysis of observational studies. Cardiovascular Drugs and Therapy 32(2):197-212.
Hoy, M. K., and J. D. Goldman. 2012. Potassium intake of the U.S. Population, What We Eat In America, NHANES 2009–2010 Food Surveys Research Group Dietary Data Brief No. 10. http://ars.usda.gov/Services/docs.htm?docid=19476 (accessed October 22, 2018).
Hughes-Austin, J. M., D. E. Rifkin, T. Beben, R. Katz, M. J. Sarnak, R. Deo, A. N. Hoofnagle, S. Homma, D. S. Siscovick, N. Sotoodehnia, B. M. Psaty, I. H. de Boer, B. Kestenbaum, M. G. Shlipak, and J. H. Ix. 2017. The relation of serum potassium concentration with cardiovascular events and mortality in community-living individuals. Clinical Journal of the American Society of Nephrology 12(2):245-252.
IOM (Institute of Medicine). 2000. Dietary Reference Intakes: Applications in dietary assessment. Washington, DC: National Academy Press.
IOM. 2003. Dietary Reference Intakes: Applications in dietary planning. Washington, DC: The National Academies Press.
IOM. 2005. Dietary Reference Intakes for water, potassium, sodium, chloride, and sulfate. Washington, DC: The National Academies Press.
Kantor, E. D., C. D. Rehm, M. Du, E. White, and E. L. Giovannucci. 2016. Trends in dietary supplement use among US adults from 1999-2012. JAMA 316(14):1464-1474.
Kaplan, N. M., A. Carnegie, P. Raskin, J. A. Heller, and M. Simmons. 1985. Potassium supplementation in hypertensive patients with diuretic-induced hypokalemia. New England Journal of Medicine 312(12):746-749.
Kovesdy, C. P., L. J. Appel, M. E. Grams, L. Gutekunst, P. A. McCullough, B. F. Palmer, B. Pitt, D. A. Sica, and R. R. Townsend. 2017. Potassium homeostasis in health and disease: A scientific workshop cosponsored by the National Kidney Foundation and the American Society of Hypertension. Journal of the American Society of Hypertension 11(12):783-800.
Leonberg-Yoo, A. K., H. Tighiouart, A. S. Levey, G. J. Beck, and M. J. Sarnak. 2017. Urine potassium excretion, kidney failure, and mortality in CKD. American Journal of Kidney Diseases 69(3):341-349.
Luo, J., S. M. Brunelli, D. E. Jensen, and A. Yang. 2016. Association between serum potassium and outcomes in patients with reduced kidney function. Clinical Journal of the American Society of Nephrology 11(1):90-100.
Malhotra, M. S., K. Sridharan, and Y. Venkataswamy. 1976. Potassium losses in sweat under heat stress. Aviation Space and Environmental Medicine 47(5):503-504.
Malhotra, M. S., K. Sridharan, Y. Venkataswamy, R. M. Rai, G. Pichan, U. Radhakrishnan, and S. K. Grover. 1981. Effect of restricted potassium intake on its excretion and on physiological responses during heat stress. European Journal of Applied Physiology and Occupational Physiology 47(2):169-179.
Menke, A., S. Casagrande, L. Geiss, and C. C. Cowie. 2015. Prevalence of and trends in diabetes among adults in the United States, 1988-2012. JAMA 314(10):1021-1029.
Mozaffarian, D., E. J. Benjamin, A. S. Go, D. K. Arnett, M. J. Blaha, M. Cushman, S. R. Das, S. de Ferranti, J. P. Despres, H. J. Fullerton, V. J. Howard, M. D. Huffman, C. R. Isasi, M. C. Jimenez, S. E. Judd, B. M. Kissela, J. H. Lichtman, L. D. Lisabeth, S. Liu, R. H. Mackey, D. J. Magid, D. K. McGuire, E. R. Mohler, 3rd, C. S. Moy, P. Muntner, M. E. Mussolino, K. Nasir, R. W. Neumar, G. Nichol, L. Palaniappan, D. K. Pandey, M. J. Reeves, C. J. Rodriguez, W. Rosamond, P. D. Sorlie, J. Stein, A. Towfighi, T. N. Turan, S. S. Virani, D. Woo, R. W. Yeh, and M. B. Turner. 2016. Heart disease and stroke statistics-2016 update: A report from the American Heart Association. Circulation 133(4):e38-e360.
Muntner, P., R. M. Carey, S. Gidding, D. W. Jones, S. J. Taler, J. T. Wright, Jr., and P. K. Whelton. 2018. Potential U.S. population impact of the 2017 ACC/AHA high blood pressure guideline. Journal of the American College of Cardiology 71(2):109-118.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Guiding principles for developing Dietary Reference Intakes based on chronic disease. Washington, DC: The National Academies Press.
NIH/NCI (National Institutes of Health/National Cancer Institute). 2018a. Figure 1. List of specific foods: Result of grouping like foods reported in 2003-2006 NHANES. https://epi.grants.cancer.gov/diet/foodsources/potassium/figure1.html (accessed October 22, 2018).
NIH/NCI. 2018b. Table 1a. Mean intake of potassium, mean intake of energy, and percentage potassium contribution of various food among U.S. population, by age, NHANES 2005-06. https://epi.grants.cancer.gov/diet/foodsources/potassium/table1a.html (accessed October 22, 2018.
O’Neil, C. E., D. R. Keast, V. L. Fulgoni, and T. A. Nicklas. 2012. Food sources of energy and nutrients among adults in the US: NHANES 2003-2006. Nutrients 4(12):2097-2120.
O’Neil, C. E., T. A. Nicklas, and V. L. Fulgoni, 3rd. 2018. Food sources of energy and nutrients of public health concern and nutrients to limit with a focus on milk and other dairy foods in children 2 to 18 years of age: National Health and Nutrition Examination Survey, 2011(–)2014. Nutrients 10(8):1050.
Pitt, B., F. Zannad, W. J. Remme, R. Cody, A. Castaigne, A. Perez, J. Palensky, and J. Wittes. 1999. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. New England Journal of Medicine 341(10):709-717.
Statistics Canada. 2017. Canadian Community Health Survey–Nutrition (CCHS). http://www23.statcan.gc.ca/imdb/p2SV.pl?Function=getSurvey&SDDS=5049 (accessed October 23, 2018).
Tian, N., Z. Zhang, F. Loustalot, Q. Yang, and M. E. Cogswell. 2013. Sodium and potassium intakes among US infants and preschool children, 2003–2010. American Journal of Clinical Nutrition 98(4):1113-1122.
Wallace, T. C., M. McBurney, and V. L. Fulgoni, 3rd. 2014. Multivitamin/mineral supplement contribution to micronutrient intakes in the United States, 2007-2010. Journal of the American College of Nutrition 33(2):94-102.
Whelton, P. K., R. M. Carey, W. S. Aronow, D. E. Casey, Jr., K. J. Collins, C. Dennison Himmelfarb, S. M. DePalma, S. Gidding, K. A. Jamerson, D. W. Jones, E. J. MacLaughlin, P. Muntner, B. Ovbiagele, S. C. Smith, Jr., C. C. Spencer, R. S. Stafford, S. J. Taler, R. J. Thomas, K. A. Williams, Sr., J. D. Williamson, and J. T. Wright, Jr. 2018. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APHA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. Hypertension 71(6):e13-e115.
Whitehead, R. G. 1995. For how long is exclusive breast-feeding adequate to satisfy the dietary energy needs of the average young baby? Pediatric Research 37(2):239-243.






















