2
Population Health in the United States
The symposium opened with an overview of population health in the United States. Eileen Crimmins, the AARP Professor of Gerontology at the University of Southern California, reviewed current trends in U.S. health and mortality compared to other high-income countries. David Williams, the Florence Sprague Norman and Laura Smart Norman Professor of Public Health and professor of African and African American studies and sociology at Harvard University, discussed racial, ethnic, and socioeconomic disparities in population health and their causes. The session was moderated by Robert Hummer, the Howard W. Odum Professor of Sociology at the University of North Carolina. Highlights of this session are presented in Box 2-1.
RECENT TRENDS IN POPULATION HEALTH
Relative Mortality as an Indicator of National Health
As a baseline, Crimmins referred participants to three reports published in 2010, 2011, and 2013 that assessed key differences in health and mortality between the United States and other high-income countries (NRC, 2010, 2011; NRC and IOM, 2013). Although life expectancy at birth for both men and women in the United States increased between 1980 and 2008, the data show that Americans live shorter lives relative to men and women in economically comparable countries. Over the past decade, U.S. life expectancy relative to other countries has continued to decline, she said.
Where U.S. life expectancy actually ranks globally depends on the countries included in the comparison. For example, a 2016 analysis from the World Bank that excluded a number of small island nations ranked the United States as 36th for life expectancy. Had the excluded nations been included, Crimmins explained, the United States would have been ranked in the range of 40th to 42nd. Crimmins also pointed out that several countries including Chile, Korea, Lebanon, and Singapore that once ranked below the United States have made significant gains and now rank above the United States.
Trends in Absolute Mortality
Over the past 2 years, Crimmins said, the absolute life expectancy in the United States has unexpectedly decreased, albeit by a very small
amount. Some demographic groups are faring worse than others, and inequalities are generally growing. The life expectancy of men is increasing more than that of women. The life expectancy of people with higher education has increased more than that of those with lower levels of education. One positive trend is a closing of the gap in life expectancy between white and black populations, as black life expectancy has increased more than white life expectancy in recent years. The largest increases in life expectancy have been among black men. Despite these gains, major gaps persist between black and white life expectancy. At every educational level, white individuals have a life expectancy that is 2 to 4 years longer than black individuals with the same level of education (Sasson, 2016).
Place matters, too, as trends in mortality for women, which are influenced by social cohesion and economic factors, also vary widely by state (Montez et al., 2016). In some U.S. counties, current life expectancy for women is actually lower than it was 30 years ago, which Crimmins said “is really quite shocking.”
Explaining Differences in Mortality Rates
A variety of explanations have been offered to account for the differences in mortality rates between the United States and other economically comparable countries. Contributing factors include smoking history, obesity, access to medical care, policies that are not supportive of health, and a lack of social safety nets. Crimmins highlighted obesity in particular as affecting U.S. life expectancy relative to other countries. She pointed out that many of these factors affect people before age 50, not in old age. The 2013 National Research Council and Institute of Medicine report U.S. Health in International Perspective: Shorter Lives, Poorer Health found that among 17 comparable countries, the United States ranked worst (16th or 17th) for mortality at most ages, up until after age 70, after which point the United States ranks among the best (NRC and IOM, 2013).
Case and Deaton (2015) have studied the rising mortality rates of middle-aged white men and women in the United States and suggest that “deaths of despair” are a large contributor, Crimmins said (see Figure 2-1). Deaths of despair include deaths related to drug and alcohol poisoning, suicide, and chronic liver disease. Such deaths rose significantly in the United States after 2000 to a level far above that of economically comparable countries. Drug overdose deaths have been increasing, particularly among people with low levels of education, and most strikingly among the non-Hispanic/white population with limited education (Ho, 2017). Adverse midlife mortality trends are apparent in a range of groups across the U.S. population (Woolf et al., 2018). Crimmins added that the United States has the highest rate of maternal mortality in the developed world
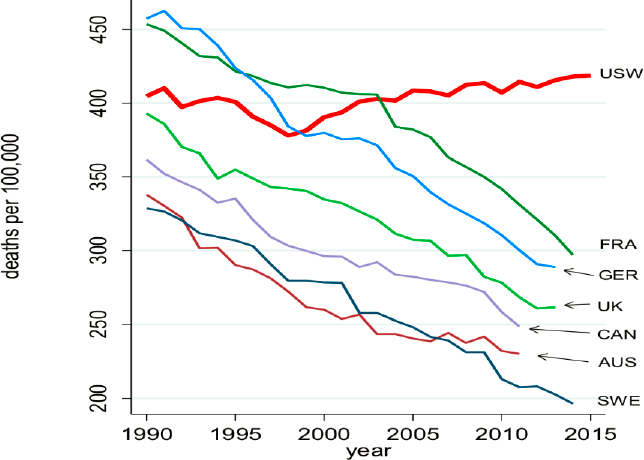
NOTE: AUS = Austria; CAN = Canada; FRA = French; GER = Germany; SWE = Sweden; UK = United Kingdom; USW = US whites.
SOURCES: Crimmins presentation, October 3, 2018; Case and Deaton, 2015, Figure 1.
(GBD, 2016). In addition, while cardiovascular mortality has continued to decline, the rate of the decline has decreased (Ma et al., 2015).
In a study of 18 countries economically comparable to the United States, Ho and Hendi (2018) found that the majority of countries had a decline in life expectancy in 2014–2015, but subsequently recovered that lost life expectancy and even experienced gains. Life expectancy in the United States, however, has continued to decline, and this has been attributed to midlife so-called deaths of despair (e.g., suicide and drug overdose) and other external causes. The decline in European peer countries was attributed to increased deaths in old age from chronic conditions. Another study of the effect of the 2008 economic crisis found no change in the declining mortality rate trend among people in Western Europe with low levels of education (Mackenbach et al., 2018). This is in contrast to the increased inequality and unfavorable mortality trends observed in the United States following the 2008 crisis.
Root Causes and Proposed Solutions
Health and mortality in the United States continue to worsen relative to economically comparable countries, Crimmins summarized. Many
inequalities are increasing, and some populations are experiencing deterioration in multiple aspects of health. Some of the proximate causes of increased mortality (e.g., the opioid epidemic, poor mental health, maternal mortality) are amenable to interventions, she said. It is the root causes of adverse mortality trends that differentiate the United States from economically comparable countries, she said. Macroeconomic change has led to job losses in some sectors and stagnant income for many people. Families are stressed, and there is a lack of supportive social policies. A national strategy to increase life expectancy is needed, Crimmins said, if the United States is to achieve levels of health that are comparable to those enjoyed by peer countries. She emphasized the need to recognize that individuals and families have a right to health care, to health, to jobs, and to support if they cannot work. In closing, Crimmins noted that she expected legislation on a life expectancy strategy to be proposed in the coming days.1
RACIAL, ETHNIC, AND SOCIOECONOMIC STATUS DISPARITIES IN HEALTH
Racial disparities in health have persisted over time, Williams said, and in his remarks he shared his perspective on priority areas to address this challenge. He reiterated the point made by Crimmins that the gap in life expectancy between white and black populations is much smaller today than it was in 1950, but there is still a gap. He emphasized the importance of applying an intersectional lens as there are complexities that can be missed when only considering overall life expectancy. For example, black women have had a longer life expectancy than white males since 1970 (NCHS, 2017). Since 1950, black women have had the largest gain in life expectancy of all groups, which Williams said was a result of policies stemming from the Civil Rights movement.
Intersection of Migration and Socioeconomic Status
Williams noted the need to consider the extent to which the narrowing of the black–white health gap over the past two decades is a function of changes in the black population as a result of black migration. Regardless of origin, these immigrants tend to have better health than their native-born counterparts (Hamilton and Green, 2018). Black migration from Africa has outpaced migration from the Caribbean since 2000, and African immigrants experience a smaller decline in their health with increasing length of stay in the United States than their Caribbean peers (Hamilton
___________________
1 The National Strategy to Increase Life Expectancy Act of 2018, or H.R. 7035, was introduced on October 5, 2018. Information about the legislation may be found at https://www.congress.gov/bill/115th-congress/house-bill/7035 (accessed December 23, 2020).
and Green, 2018). In addition, black immigrants from Africa are twice as likely as whites to have a college degree, Williams said. It is estimated that nearly 20 percent of the black population in the United States are immigrants (Hamilton and Green, 2018). This demonstrates the importance of disaggregating data to better understand trends, and to better elucidate the effect of the changing composition of the black population versus improved outcomes for the historic black population in the United States.
Disaggregated data are also needed to better understand the health stresses facing Hispanic populations and Asian populations in the United States, Williams stated. For example, the health of Mexican immigrants in the decade after arrival in the United States is similar to that of the U.S.born white population; however, their health profile changes negatively over their years of residence in the United States and becomes similar to that of the U.S.-born black and Mexican American populations (Kaestner et al., 2009). Similarly, hypertension profiles are different for U.S.-born and foreign-born Hispanic residents (Dominguez et al., 2015). As above, these nuances would not be apparent from simply analyzing data for Latinos in the United States. Williams also noted the need to consider the heterogeneity of the Hispanic population beyond ethnicity. For example, he said that about 5 percent of immigrants from Mexico have a college degree or higher compared to 50 percent of immigrants from Venezuela. It is necessary to understand how this combination of immigration and socioeconomic status affects health status, he said.
Interrelationship of Race, Ethnicity, and Socioeconomic Status and Their Combined Effect on Health
The National Longitudinal Mortality Study 1988–1998 found that, overall, there is a 5-year gap in life expectancy at age 25 between white and black populations in the United States. When education is taken into account, there is a 6.4-year gap in life expectancy between white individuals with a college degree versus those with a high school education or less. There is a 5.3-year gap in life expectancy of black Americans with a college degree versus those with a high school education or less. Williams pointed out that the education-based life expectancy gap within each racial and ethnic group is greater than the overall variation between the racial and ethnic populations. When considered by level of education, Williams said that black individuals with a college degree have lower life expectancy than white individuals with only a high school diploma. He added that similar patterns are observed relative to income. He encouraged health systems to more routinely collect and report data by race and socioeconomic status together, rather than by race only.
Data on All Populations, Including Very Small Populations
To illustrate the value of data on small populations Williams described a study of workplace discrimination by the American Psychological Association. The study gathered national data and also oversampled specific populations, including Native Americans. Survey data collected from white, black, Hispanic, Asian, and Native American individuals found that Native Americans reported the highest levels of discrimination for three indicators of job discrimination: unfairly fired, unfairly denied promotion, and unfairly not hired for a job (APA, 2016). When asked about everyday discrimination, more Native Americans surveyed reported experiencing discrimination at least once per week than any other population (Native American, 34 percent; black, 23 percent; Hispanic, 19 percent; white, 11 percent; and Asian, 11 percent). This information about the Native American experience would be unknown if population-specific data were not collected, he said (APA, 2016).
Research on Life-Course and Transgenerational Sources of Inequities
Williams shared several examples of the effect life course has on health inequities. A study in Sweden found that preconception stress (stressors in the life of the mother that occur in the 6 months prior to conception) is associated with a 53 percent higher risk of infant mortality (Class et al., 2013). Another study conducted in the United States found an association between preconception stress and low birth weight. Childhood abuse of the mother has been suggested to predict depressive symptoms in her children in adolescence and young adulthood (Roberts et al., 2015). Finally, a study conducted by Brody and colleagues (2014) found that perceived discrimination against black adolescents in Georgia (age 16 to 18) was associated with a higher allostatic load at age 20 (higher levels of stress hormones, and increased systolic and diastolic blood pressure, inflammation, and body mass index). This shows systematic biological dysregulation linked to stress exposure during their teens. Williams emphasized the need to better understand how these life-course factors and outcomes vary across racial and ethnic status and contribute to inequities in health.
Cost of Resilience
Another study by Brody and colleagues (2013) assessed the cost of resilience. The study followed black teens from low socioeconomic circumstances who had high levels of self-control and self-regulation, which predicts higher academic success and emotional stability in their 20s. These young adults are likely to go on to college and have lower rates of
drug and alcohol use. However, they have greater obesity, higher blood pressure, higher stress hormones, and higher levels of epigenetic aging than both low socioeconomic status peers who have low self-control and higher socioeconomic status peers. Their success seems to come at a cost, and Williams noted the need to better understand what drives this and what can be done to address it.
Effect of the Social Environment on Child and Adolescent Health
Shortly after the 2016 election, a survey of 2,000 K–12 teachers about their classroom environment found that 67 percent had students who expressed fears about what would happen to their family; one-third reported observing increased anti-Muslim or anti-immigrant sentiment among students; and more than half said there was an increase in uncivil political discourse in the classroom (SPLC, 2016). Teachers reported that “some students were emboldened to use slurs and name calling and say bigoted and hostile things,” Williams relayed. This hostile environment has been growing since the election, and Williams said there has been an increase in hate crimes and harassment. In fact, he said, since the election, primary and secondary schools currently rank as the number one site of hostility and hate crimes in the United States.
A better understanding of the health effect of the social environment on young people is needed, Williams said. He cited a study of more than 2,500 11th-grade students in Los Angeles assessing their level of concern about increasing hostility and discrimination because of a person’s race, ethnicity, sexual identity, immigrant status, religion, or disability. Students were interviewed in spring 2016, and again in spring 2017, and each time more than 40 percent said they were very or extremely concerned about increasing discrimination. In 2016, students that reported higher levels of concern also reported increased smoking and use of alcohol and marijuana, and increased symptoms of depression and attention-deficit/hyperactivity disorder (Leventhal et al., 2018). Some associations were more prevalent among Hispanic and black students. These data suggest that the current environment is affecting health behaviors and potentially mental health among teens, Williams said. The American Psychological Association has found that the current political climate is a “very significant or somewhat significant source of stress” for many Americans across age and racial groups (APA, 2017).
Williams described one of many recent studies that document the health effects of hostility in the current environment. Leitner and colleagues (2016) studied the association between circulatory disease-related deaths and racial prejudice against black residents in more than 1,800 counties. The results show that death rates are higher in counties with
high levels of explicit prejudice. He added that similar findings have been demonstrated for the lesbian, gay, bisexual, transgender, queer, and/or questioning population. There is a consistent pattern across a broad range of outcomes and measures of prejudice at the community level that needs to be better understood, he said.
Current Issues Affecting the Health of Immigrants
Arizona’s Support Our Law Enforcement and Safe Neighborhoods Act (SB 1070) authorizes police to stop anyone suspected of being in the United States illegally and to detain those without proper documentation. Williams and colleagues studied pairs of young mothers and their mother figures (their own mothers, grandmothers, aunts) for their use of public assistance and preventive routine care for their children before and after passage of the law. The data show a decline in the use of health and social services for the children after the law was enacted (Toomey et al., 2014). Interestingly, the decline was steepest among U.S.-born Mexican American mothers who, Williams pointed out, were U.S. citizens and therefore not at risk.
The health effect of immigration raids has also been studied. The largest single-site immigration raid in U.S. history (at the time) took place in Postville, Iowa, in 2008. Nearly 400 persons were detained until their immigration status could be confirmed. Families were separated, and ultimately, 300 people were deported. The community was extremely fearful, and some slept in churches instead of their homes. One study found an increased risk of low birth weight for infants born to Latina mothers in the Postville area during the year after the raid (Novak et al., 2017). Williams added that there was no change in birth weight of infants born to non-Hispanic white mothers during this time.
Creating Resilient Environments
Much of the work on resilience has been focused on individual resilience, Williams said, but policy interventions are also needed that can create resilience at the societal level. Such interventions could help to buffer the effects of childhood poverty, for example. The United States currently ranks 34th in a ranking of child poverty in 35 economically comparable countries (UNICEF, 2012). When the level of child poverty is considered both before and after taxes and transfers (i.e., the effect of the economic system of the country on child poverty), it becomes apparent that many other countries’ economic policies help to reduce child poverty, while U.S. economic policies do not appear to greatly benefit children in poverty (see Figure 2-2).
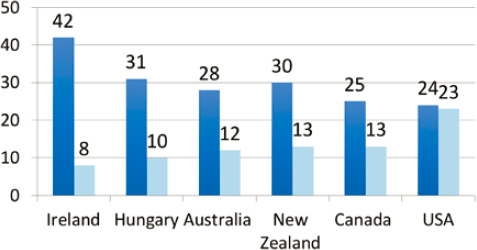
SOURCES: Williams presentation, October 3, 2018; adapted from UNICEF, 2012, Figure 8.
Williams added that “poverty is not randomly distributed in the United States” where a greater proportion of black (31 percent), Hispanic (27 percent), and Native American (34 percent) children live in poverty compared to their Asian and white counterparts (both at 10 percent). Williams emphasized the role of the social safety net as a “resilience resource,” and said that keeping the safety net in place is a strategy for societal resilience.
Williams offered the Omnibus Budget Reconciliation Act in 1981 as an example of the negative effect that U.S. economic policies can have on health (Mundinger, 1985). Funding cuts to health and social services during the Reagan administration resulted in 500,000 people losing their eligibility for Aid to Families with Dependent Children, 1 million people losing eligibility for food stamps, 600,000 people becoming no longer eligible for Medicaid, and the closing of numerous community health centers. “A broad range of negative effects occurred when the safety net was harmed,” Williams said. For example, as more people had reduced access to care, there were increases in the incidence of low birth weight newborns, pregnant women with anemia, preventable childhood diseases, lead poisoning in children, and chronic diseases in adults. Williams reiterated the need to secure the safety net and emphasized the importance of monitoring policy changes and studying their effect on health, including health inequities. These data are needed to inform advocacy efforts for strengthening the safety net.
Understanding and Addressing Deeply Embedded Racism
One of the many ways that racism manifests is through negative stereotyping, Williams said. In a recent study, Williams and colleagues
found that 52 percent of white individuals who work or volunteer with children perceived black adults as being prone to violence. With regard to other populations, 43 percent of these white adults endorsed this negative stereotype toward Hispanic adults, 29 percent toward American Indian adults, 29 percent toward Arab American adults, 10 percent toward Asian adults, and 22 percent toward other white adults (Priest et al., 2018). These white adults who work or volunteer with children were also asked about their beliefs regarding the tendency for violence by young children and teens of different races and ethnicities. Fewer of these white adults endorsed this stereotype for children. For example, 23 percent believed that black children under the age of 10 were prone to violence (16 percent toward Hispanic children, and fewer toward other subgroups). Williams shared a quote from an 1899 book by W. E. B. Du Bois in which Du Bois identifies an empathy gap, specifically, the indifferent attitude of the general population regarding the health and well-being of the black population as the single biggest challenge concerning racial inequities in health. A recent study suggests that this lack of empathy persists and is evident in early life (Dore et al., 2014).
Moving Forward
It is necessary to raise awareness of the inequities in society and health, Williams said, adding that research is needed to identify ways to “reduce the perception of inequities as politically contentious and polarizing.” The stories of the disadvantaged need to be told in a compelling way that resonates with the public and fosters empathy. Finally, a strong science base is needed to make the case for addressing inequities in health and to garner the political will to effect change (Williams and Purdie-Vaughns, 2017).
DISCUSSION
The discussion period included several questions and comments about data—from exceptions from national life expectancy trends to the effects of the Patient Protection and Affordable Care Act (ACA) on life expectancy—and about structural factors and systems that affect population health trends.
A participant asked whether there are data to suggest that particular states or counties have been able improve on the life expectancy trends seen nationwide. Crimmins responded that there are regions that are outliers relative to the national trends. She referred participants to the work of Christopher Murray at the Institute for Health Metrics and Evaluation, who has identified “eight Americas” based on geographic and sociodemographic characteristics (see Murray et al., 2006). Areas that buck the
trend tend to be wealthier or have better health or health behaviors. She suggested that the difference in trends is more related to different social and economic characteristics of an area and less to policies. As another resource for data on health and the determinants of health across all states, Williams referred participants to the work of Brian Smedley, Steven Woolf, and others with the Health Opportunity and Equity Initiative.2
Whitney Robinson of the University of North Carolina at Chapel Hill reiterated the point made by Williams about the importance of viewing the data through an intersectional lens. There are insights to be gained, for example, by considering immigrant versus nonimmigrant populations. She asked about variables by which to stratify the data (beyond sex/gender, race/ethnicity) in order to include intersectionality when evaluating these trends. Williams added that socioeconomic status and nativity status are also important to consider, and Crimmins noted that data on educational attainment are similarly valuable.
John Auerbach from Trust for America’s Health noted that the passage of the ACA and the subsequent drastic reduction in the number of uninsured Americans was expected to improve health. He asked about data on health relative to whether a state chose to expand Medicaid under the ACA. Crimmins suggested that, based on the maps she discussed, the states that did not expand Medicaid appear to also be those that are the worst with regard to life expectancy. Williams agreed, but noted that a dramatic change in health would not necessarily be expected, even if the use of preventive services was improved. Access to quality care is essential, but medical care alone cannot solve the range of population health issues.
Based on the presentations, a participant said she understood that maternal outcomes were changing across all populations, and that she believed that biases in society were actually affecting all populations. She asked what agencies might do to demonstrate that what happens in some populations affects all populations over time. She also said that the connections between child health and adult health outcomes need to be communicated more effectively. Crimmins responded that research is being done on the link between early, mid, and late life, trying to better understand how early life shapes one’s life course and aging trajectory. Williams added that both negative and positive early-life exposures affect biological functioning later in life. It is important to try to understand how these exposures accumulate over time to affect health outcomes. “Early-life exposures do affect adult health for all individuals, but they are not randomly distributed,” he said, and he reiterated that health patterns are influenced by race, ethnicity, socioeconomic status, and immigrant status.
___________________
2 See http://www.nationalcollaborative.org/our-programs/hope-initiative-project (accessed December 23, 2020).












