1
Introduction
In response to the coronavirus disease 2019 (COVID-19) pandemic and the societal disruption it has brought, national governments and the international community have invested vast sums of money in the development of a safe and effective vaccine. Although subject to myriad uncertainties, mass vaccination against this novel coronavirus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), offers the possibility of significantly reducing transmission and severe morbidity and mortality beyond what might be accomplished solely through non-pharmaceutical interventions, better diagnostic tests, and improved therapies.
The goal of protecting the public’s health is intertwined with the goal of protecting society’s socioeconomic well-being, which in turn has an impact on the public’s overall health. Even if one or more safe and effective COVID-19 vaccines from those under development are tested and quickly approved for use, they are unlikely to be available immediately in amounts sufficient to vaccinate the entire population, despite plans to begin large-scale production of promising vaccines even before trials are completed. As a result, at the outset and in the months to follow, a COVID-19 vaccine will almost certainly be available only in limited supplies. In this context, scarce vaccines will need to be allocated in ways that reduce morbidity and mortality and reduce SARS-CoV-2 transmission in order to protect the public’s health and its socioeconomic well-being.
This chapter presents the study charge and approach and lays out the report’s organization. The chapter also examines the ways in which race and ethnicity and health equity are intertwined with the impact of COVID-19, the populations that are at increased risk of severe illness or
death from COVID-19, and the current landscape of COVID-19 vaccines at the time of this writing—all of which have significant implications when planning for the equitable allocation of COVID-19 vaccine. This chapter concludes with a description of a national COVID-19 vaccine program that builds on the solid and tested national vaccine program that has existed in this country for more than half a century.
STUDY CHARGE
To meet the anticipated high demand for a COVID-19 vaccine in the early stages of availability, guidance is urgently needed to plan for equitably distributing a limited vaccine supply. To address this urgent need, the Centers for Disease Control and Prevention (CDC) and the National Institutes of Health (NIH) asked the National Academies of Sciences, Engineering, and Medicine (the National Academies), in partnership with the National Academy of Medicine, to convene an ad hoc committee to develop an overarching framework for COVID-19 vaccine allocation in order to assist policy makers in the domestic and global health communities. This framework could later inform the work of national health authorities and additional advisory bodies, including CDC’s Advisory Committee on Immunization Practices (ACIP), during the development of national and local guidelines.
The full charge to the committee is in Box 1-1. The committee was comprised of 18 members with academic backgrounds and professional expertise in fields including public health, epidemiology, medicine, bioethics, law, public policy, economics, occupational health, health insurance, geriatrics, and global health. Biographies of the committee members are provided in Appendix B.
ABOUT THIS REPORT
Study Approach and Scope
In developing this report, the framework, and recommendations herein, the committee deliberated for approximately 2.5 months (mid-July 2020 through September 2020), and held eight virtual meetings. Three of these meetings included sessions open to the public (all public meeting agendas can be found in Appendix A).
Soliciting Public Comments on the Discussion Draft of the Preliminary Framework for the Equitable Allocation of COVID-19 Vaccine
Importantly, as part of its study process, the committee made available a discussion draft of its framework, Discussion Draft of the Preliminary
Framework for Equitable Allocation of COVID-19 Vaccine,1 to obtain input from members of the public, especially groups disproportionately affected by COVID-19, to inform the committee’s final report (see Appendix
___________________
1 See https://www.nap.edu/catalog/25914 (accessed September 15, 2020).
A for additional details on the process). Between September 1 and 4, 2020, the committee conducted its public comment period which consisted of written and oral comment opportunities. The public comment period served to convey the inclusiveness of the committee’s process to foster trust and engagement around the final report and to ensure that the framework reflects the realities and concerns of those dealing with COVID-19 on the ground. Beyond the formal public comment period, members of the public were able to submit comments through a link on the study webpage2 or through a designated email address for the duration of the study.
The committee hosted a public listening session where more than 2,000 members of the public attended and more than 50 individuals were able to formally address the committee. During this public listening session, the committee heard from stakeholders from minority communities, state and local government representatives, health and medical professional organizations, those representing older adults, those representing occupations at risk, and stakeholders from special populations, such as those representing incarcerated individuals, as well as individuals experiencing homelessness.
The committee also accepted written comments through an online form. The written comment opportunity elicited more than 1,400 written comments. A summary of comments and how the committee responded to these suggestions is described in Appendix A. All materials and comments received through the online form were placed in the committee’s Public Access File, and are available by request through the National Academies’ Public Access Records Office.
Study Scope
As specified in the committee’s Statement of Task (see Box 1-1), the committee was charged with assisting policy makers in planning for the equitable allocation of vaccines against COVID-19. This report focuses primarily on the allocation of one or more COVID-19 vaccines and the best way to do so equitably without further exacerbating—and to the extent possible, mitigating—existing health inequities. The report also addresses implementation issues necessary to ensure equitable allocation. The committee notes that it chose not to consider three issues:
- Political context: The committee appreciates that decisions about the public’s health are made in the context of existing political realities and those are not static.
___________________
2 See https://www.nationalacademies.org/our-work/a-framework-for-equitable-allocation-of-vaccine-for-the-novel-coronavirus (accessed September 15, 2020).
- Legal, regulatory, and public health changes: The committee recognizes that the allocation of COVID-19 vaccine could be changed by regulatory or public health requirements (e.g., mask mandates, greater spacing of workers in food processing facilities). Should these occur, they will affect some individuals’ risks of getting sick or transmitting infection if they do. As a result, they will affect the operation of the allocation procedure and require adaptive implementation, which the proposed framework is designed to make possible. It is crucial that these other protective measures not be prematurely abandoned. A full discussion of other legal and regulatory issues that could impact allocation is generally beyond the scope of this study. They include, but are not limited to, the process of vaccine approval, distribution, and reimbursement at the federal level; the potential intersection of allocation criteria with federal and state anti-discrimination laws; variability in state vaccination mandates aimed at schoolchildren and employees in certain sectors, such as patient care; professional licensing and scope of practice rules; recognition of out-of-state provider licenses when additional professionals are needed; payment and reimbursement provisions and processes for the varying public and private insurers within states; provider and manufacturer exposure to liability; and state-based surveillance and privacy protections.
- Advances in medical treatment and therapeutic agents: The committee recognizes the vast, creative efforts made to improve medical treatment and develop therapeutic agents for COVID-19. As they succeed, they should reduce the risk of disease severity and death and may reduce the risk of transmission of infection. Here, too, the adaptability of the allocation procedure can accommodate changes in risk.
The guidance offered through the committee’s allocation framework is intended to inform the work of the federal government, ACIP, and that of state, tribal, local, and territorial (STLT) authorities in their COVID-19 vaccine allocation planning. Throughout the report, there are key terms that are routinely used in the public health field that may contain nuance or depend on the particular context and user. Box 1-2 shows the committee’s definitions for these key terms.
Report Audiences and Uses
In developing this report, the committee recognized the need for clear, transparent, and unified messaging at the federal level. While the National Academies cannot implement these phases or recommendations, the intention is for this report to guide those who can. Key audiences who can ben-
efit from and be informed by this report include the federal government and STLT authorities, as well as groups such as ACIP as they create and implement national and/or local guidelines for COVID-19 vaccine allocation.
Organization of the Report
The organization of this report closely follows the Statement of Task (see Box 1-1). Chapter 2 provides lessons learned from previous situations in which scarce resources were allocated and it describes other COVID-19 vaccine allocation efforts currently under way at the national and international levels.
Chapter 3 describes the committee’s framework for the equitable allocation of COVID-19 vaccine and lays out the foundational principles that inform the vaccine allocation framework, the goal of the framework, the risk-based allocation criteria used to apply the principles, and the resulting allocation phases. Chapter 3 also contains the rationale behind the inclusion of the groups listed in each phase. Chapter 4 explores the application of the framework in different scenarios, such as those in which the number and timing of vaccine doses is variable, when vaccine uptake may be lower than expected, or under changing social, economic, and legal contexts.
The remaining chapters highlight key implementation considerations. Chapter 5 examines issues of program administration and monitoring and evaluation to ensure effectiveness and equity, and challenges related to vaccination costs. Chapter 6 focuses on risk communication and community engagement. Chapter 7 addresses vaccine acceptance, including the landscape of vaccine hesitancy and mistrust and strategies for vaccine promotion. Chapter 8 discusses the role of U.S. participation in global vaccine allocation. Finally, Appendix A describes in detail the methods of the study process, and Appendix B presents biographical sketches of the committee members and staff.
COVID-19 AND HEALTH EQUITY CONSIDERATIONS
In the United States and worldwide, the COVID-19 pandemic has magnified the intersectional and pervasive impacts of social and structural inequities in society. COVID-19 is having a disproportionate impact on people who are already disadvantaged by virtue of their race and ethnicity, age, health status, residence, occupation, socioeconomic conditions, and/or other contributing factors (Williams and Cooper, 2020). In public health crises, certain populations are often falsely accused of being the cause of an outbreak, further worsening stigma and discrimination. The current moment of ethical reckoning playing out around race in the United States reveals the disproportionate impact of the COVID-19 pandemic on racial and ethnic minorities and other vulnerable and marginalized groups through cultural and political discourse across the country (Yancy, 2020). Given the legacies of inequality, injustice, and discrimination that have undermined the health and well-being of certain populations in the United States for centuries, considerations of equity should factor into plans for allocating and distributing COVID-19 treatments and vaccines to the population at large (Essien et al., 2020).
Racial and Ethnic Equity
An increasing body of evidence indicates that in the United States, certain racial and ethnic groups including Black, Hispanic or Latinx, American Indian and Alaska Native, and Native Hawaiian and Pacific Islander communities have been disproportionately affected by COVID-19 (Cohen, 2020b; Johnson and Buford, 2020). This is evident in the overrepresentation of these groups in the daily number of reported cases3 and in their
___________________
3 According to CDC data, among cases where race and ethnicity are reported, 33 percent are Hispanic, 22 percent are Black, and 1.3 percent American Indian and Alaska Native (AI/AN). This impact is disproportionate because Hispanics make up 18 percent of the U.S. population, Blacks make up 13 percent, and AI/AN make up 0.7 percent (CDC, 2020a).
increased risk of severe clinical outcomes, hospitalization, and death (Gold et al., 2020; Killerby et al., 2020; Millett et al., 2020; Price-Haywood et al., 2020; Stokes et al., 2020). In Chicago, for example, both the number of COVID-19 cases per 100,000 persons and the mortality rates are higher among Hispanic and Black populations than among White populations. Similarly, age-adjusted COVID-19 (cause-specific) mortality rates are higher among Hispanic and Black populations (Webb Hooper et al., 2020).
American Indian and Alaska Native individuals had a cumulative incidence of laboratory-confirmed COVID-19 cases that was 3.5 times greater than that among non-Hispanic White individuals, according to data from 23 states as of July 2020 (Hatcher et al., 2020). Pacific Islander communities have experienced mortality from COVID-19 at a rate up to five times their proportion of the population compared to the general population (Wong, 2020). Due to COVID-19, Native Hawaiians have experienced mortality rates that are three times higher than the proportion of the population in Hawaii (Wong, 2020).
CDC has compiled data by race and ethnicity on the rates of COVID-19 cases, age-adjusted hospitalizations, and death (CDC, 2020b,d). Compared to non-Hispanic Whites, American Indian and Alaska Native persons had a case rate that was 2.8 times higher, a hospitalization rate that was 4.6 times higher, and a death rate that was 1.4 times higher (CDC, 2020b,d). Hispanic or Latinx persons had a case rate that was 2.8 times higher, a hospitalization rate that was 4.7 times higher, and a death rate that was 1.1 times higher (CDC, 2020b,d). Black and African American persons had a case rate that was 2.6 times higher, a hospitalization rate that was 4.7 times higher, and a death rate that was 2.1 times higher (CDC, 2020b,d).
Intertwined inequities and disparities in the social determinants of health—which CDC defines as “conditions in the places where people live, learn, work, and play that affect a wide range of health and quality-of-life risks and outcomes” (CDC, 2020j)—tend to impact racial and ethnic minority groups disproportionately (CDC, 2020c; Cohen, 2020b). Chronic conditions that are associated with worse COVID-19 outcomes—for example, diabetes mellitus, asthma, hypertension, kidney disease, and obesity—are more common in Black and Hispanic or Latinx populations than in White populations (Arasteh, 2020; Hatcher et al., 2020; Kirby, 2020). In the United States, the Native Hawaiian and Pacific Islander community is one of the highest-risk populations for cardiometabolic diseases, including diabetes mellitus, obesity, and hypertension (Mau et al., 2009). American Indians and Alaska Natives also tend to have higher rates of diabetes mellitus, obesity, hypertension, and other chronic conditions compared to the White population in the United States (Adakai et al., 2018; Poudel et al., 2018).
In addition to experiencing higher incidence and prevalence rates of chronic medical conditions, racial and ethnic minority populations tend to have limited access to health care, are less likely to be insured, and are more likely to live and work in conditions that worsen health outcomes (Tai et al., 2020). Minority groups also comprise a greater percentage of essential workers—only 20 percent of African Americans are able to work from home, for example—and many rely on public transportation to travel to work, which increases their likelihood of exposure to SARS-CoV-2 (Kirby, 2020; Tai et al., 2020). In New York City, 75 percent of frontline workers are people of color and 40 percent of transit workers are African American. Native Hawaiian and Pacific Islander populations are also disproportionately represented in essential workers groups in areas such as the hospitality industries, family businesses, and low-paying health care occupations; they are also more likely to live in congregate living settings (Wong, 2020), increasing their risk for SARS-CoV-2 infection. CDC has identified several categories of risk factors that are associated with COVID-19 illness, hospitalization, and death in racial and ethnic minority communities (CDC, 2020c) (see Box 1-3), all of which tie back to the historical impact of systemic racism and the social determinants of health. An increasing body of evidence demonstrates that racism and discrimination, through the biological impacts of stress, poverty, and other negative outcomes, play a direct role in the health of communities of color (RWJF, 2020; Williams, 2020).
These points are important, and the committee has taken great pains to emphasize them not only because of the moral and ethical implications of this disproportionate experience with COVID-19 by these individuals, but also because in our highly interconnected world, for the reasons previously noted, the challenges experienced by particular subpopulations have an effect on us all. If we have learned anything from this pandemic, it is that we are inevitably all in this together.
Historical Gap in Immunization Coverage
Historical precedent for the current disparities in COVID-19 morbidity and mortality is reflected in the gaps in routine and 2009 H1N1 influenza immunization coverage between non-Hispanic White and racial and ethnic minority populations. Non-Hispanic Whites have had higher coverage for routine immunizations compared to racial and ethnic minority groups (Walker et al., 2014). A nationally representative survey indicated that 2009 H1N1 influenza vaccine uptake was greater for White and Hispanic respondents than for Black respondents; the same trend was present for seasonal influenza vaccine (42.6 percent versus 32.2 percent) (Uscher-Pines et al., 2011). Another study found that Black and Hispanic populations were significantly less likely than White populations to receive influenza vaccine
regularly (Crouse Quinn et al., 2011). The 2009 H1N1 influenza vaccine coverage generally was higher among non-Hispanic Whites than among non-Hispanic Blacks. Vaccination coverage among Black health care workers was also lower, indicating that access to care was not the only barrier to vaccination (CDC, 2010). Black and Hispanic survey respondents also tend to be less likely than White respondents to agree that vaccines are “safe in general” (Uscher-Pines et al., 2011). Data from a program of dispensing free H1N1 influenza vaccinations at public clinics in Los Angeles County in 2009 showed that African Americans had the lowest rates of vaccination uptake compared to other racial and ethnic groups. A major challenge encountered during this immunization drive was community messaging and discourse that was at odds with the government messaging in the area. In response, county public health officials pursued audience-specific advertising, contracted local organizations to support accurate messaging, and engaged in outreach to community leaders and partners (Plough et al., 2011), demonstrating the need for targeted messages delivered by trusted messengers, particularly for groups marginalized within our medical systems.
Additional Health Equity Considerations
The full extent of COVID-19 on people’s health and well-being will likely not be fully understood for years, but long-term effects are anticipated to span multiple dimensions, including behavioral, developmental, social, emotional, mental health, educational, and economic impacts. These impacts are felt around the globe, spanning all populations and regions; however, certain groups are at an increased risk of suffering from the multifaceted impacts of COVID-19. Table 1-1 provides an overview of key data available thus far on the impact of COVID-19 on these populations.
TABLE 1-1 Key Data on the Impact of COVID-19 on Certain Populations
| Population | Key Impact Data |
|---|---|
| Black |
|
| Hispanic/Latinx |
|
| American Indian and Alaska Native |
|
| Population | Key Impact Data |
|---|---|
| Native Hawaiian and Pacific Islander |
|
| Older adults (≥65 years) |
|
| Older adults (>80 years) |
|
| People with underlying or comorbid conditions |
|
| People who live and/or work in congregate settings |
|
| Sex |
|
| Children |
|
| People who are pregnant or breastfeeding |
|
NOTE: The following groups are omitted from the table due to a lack of COVID-specific epidemiological data: people who are undocumented, people with mental and physical disabilities, and people experiencing homelessness.
Special Populations at an Increased Risk from COVID-19
Differential health impacts are also experienced by certain populations who tend to experience worse outcomes if they contract COVID-19. Like racial and ethnic minority groups, many of these populations face underlying social and structural disparities that intersect to exacerbate health inequities.
Older Adults
Older people who contract COVID-19 are at a greater risk of developing severe disease and dying (UN, 2020b). This risk is likely exacerbated by the fact that many elderly people have underlying health conditions or live in congregate settings, such as long-term care facilities, where transmission of SARS-CoV-2 can occur readily (Cohen, 2020b). In the United States, adults aged 65 years and older account for approximately 8 out of 10 reported deaths related to COVID-19 (CDC, 2020f). Among those 65 years of age and older, the risk of severe COVID-19 disease and mortality increases sharply with age (see Figure 1-1, which shows cumulative hospitalization rates per 100,000 persons stratified by age groups). In the United States, people aged 85 and older are experiencing an “overwhelming percentage” of severe outcomes due to COVID-19 (Nikolich-Zugic et al., 2020). Worldwide, estimates suggest that people aged >80 years are experiencing a mortality rate from COVID-19 that is about five times the average mortality rate (UN, 2020b). A global modeling study suggests that around two-thirds of people aged ≥70 years have at least one underlying health condition, which compounds their risks of COVID-19 infection, severe disease, and death (Sanyaolu et al., 2020). Compared to people below the age of 65, the population-level COVID-19 mortality risk for people aged 65 years and older is estimated to be 16-fold to 52-fold higher in the United States (based on data from 13 U.S. states) and 30-fold to 100-fold higher in Europe and Canada (based on data from 10 European countries) (Ioannidis et al., 2020). Because of the significantly greater likelihood that older people with COVID-19 will die—particularly those with underlying conditions that enhance their risk—protecting this vulnerable group should be a key consideration in managing the pandemic (Ioannidis et al., 2020). This group also presents a growing challenge over time, as the United Nations estimates that by 2050 there will more than twice as many people over age 65 as there will be children under 5, and the cohort of adults older than 65 will exceed the cohort of individuals who are 15–25 years old (Koff and Williams, 2020).
People with Underlying Conditions or Comorbid Conditions
The risk of severe disease and death due to COVID-19 is greater among people with underlying conditions or comorbid conditions. These conditions include cancer, chronic kidney disease, chronic obstructive pulmonary disease, an immunocompromised state or weakened immune system from solid organ
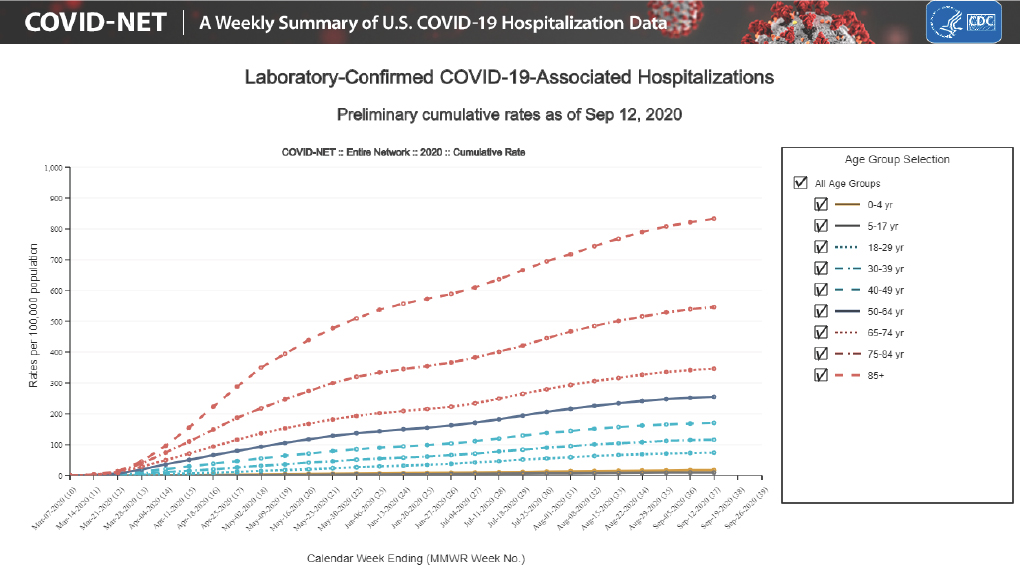
NOTES: The Coronavirus Disease 2019 (COVID-19)-Associated Hospitalization Surveillance Network (COVID-NET) conducts population-based surveillance for laboratory-confirmed COVID-19-associated hospitalizations in children and adults. The current network covers nearly 100 counties in the 10 Emerging Infections Program states, and 4 additional states through the Influenza Hospitalization Surveillance Project (14 states in total). The network represents approximately 10 percent of the U.S. population.
SOURCES: CDC, 2020f,i.
transplant, obesity, serious heart conditions, sickle cell disease, and type 2 diabetes mellitus (CDC, 2020g). Modeling estimates suggest that roughly 20 percent of people worldwide may be at an increased risk of severe COVID-19 disease due to their underlying health conditions. This risk also increases substantially with age, because both older adults and people with underlying health conditions tend to experience severe health outcomes if they contract COVID-19 (CDC, 2020a; UN, 2020b). According to CDC’s surveillance data for March 2020, people with COVID-19 who had underlying health conditions—most commonly hypertension, obesity, cardiovascular disease, diabetes mellitus, and chronic lung disease—were six times as likely to be hospitalized and 12 times as likely to die from the disease as those without underlying health conditions (CDC, 2020a; Sanyaolu et al., 2020). Although older people are more likely to have one or more comorbid conditions, people of any age with underlying health conditions are at greater risk of severe COVID-19 (Sanyaolu et al., 2020). CDC’s data suggest that about one-third of patients aged 18–49 who are diagnosed with COVID-19 have underlying chronic lung disease, such as asthma (Sanyaolu et al., 2020). CDC has developed a list of medical conditions that increase the risk of severe COVID-19 illness, which is updated on an ongoing basis (see Box 1-4).
People Who Live and/or Work in Congregate Settings
People who live or work (or both) in congregate settings, such as nursing homes or group residential homes, are at higher risk of acquiring COVID-19 and developing severe disease. Approximately 1,347,000 people in the United States live in nursing homes, 811,000 reside in assisted living facilities, and approximately 75,000 live in intermediate-care facilities—in addition to more than 3 million people who work in nursing or residential care facilities (CDC, 2020e,j; Chidambaram, 2020; True et al., 2020). Older adults residing in senior living facilities are at a high risk of severe COVID-19 due to the burden of chronic illness and their exposure to the virus while to living in congregate housing (Nikolich-Zugic et al., 2020). In a sample of 23 states with publicly reported death data as of April 23, 2020, more than 10,000 deaths—or 27 percent of all deaths due to COVID-19 in the sample—occurred among people living in long-term care facilities. Across Colorado, Delaware, Massachusetts, Oregon, Pennsylvania, and Utah, more than half of all COVID-19 deaths occurred among residents of long-term care facilities (Chidambaram, 2020).
Older people living in congregate settings tend to have one or more underlying health conditions. However, many people without such underlying conditions are at increased risk of SARS-CoV-2 infection due to living or working in congregate settings: for example, prisoners, meat packers, soldiers, and grocery store workers (Cohen, 2020b). People who are in-
carcerated tend to have multiple risk factors that can increase their risk of contracting SARS-CoV-2 infection and experiencing worse outcomes upon developing COVID-19. The United States incarcerates more individuals than any other country, with nearly 2.2 million people living in prisons and jails at the end of 2016 (Akiyama et al., 2020). The nature of incarceration makes it difficult or impossible to maintain adequate social distance, thus increasing transmission of SARS-CoV-2 (Hawks et al., 2020). For instance, at Rikers Island prison in New York, more than 200 additional infections were diagnosed within just 2 weeks after the first case was detected in the
facility (Hawks et al., 2020). At San Quentin prison in California, more than 1,600 infections have been diagnosed (Maxmen, 2020). Age and comorbid conditions can also exacerbate the risk of COVID-19 among people who are incarcerated. Due to longer sentences, the average age of the prison population in the United States has increased. Between 1993 and 2013, the number of people aged >55 years in prisons increased by nearly 400 percent (Hawks et al., 2020), and the U.S. Department of Justice reports that 81,600 persons who are incarcerated are aged >60 years (Akiyama et al., 2020). Half of the people who are incarcerated in state prisons have at least one chronic condition—for example, heart disease (10 percent) and asthma (15 percent)—at prevalence rates that are higher than those in the general population, even when age is taken into account (Hawks et al., 2020). Furthermore, some population groups are more likely to be disproportionately incarcerated, including racial ethnic minorities, people with unstable housing, and people with substance use disorders or mental illness (Akiyama et al., 2020). Despite their heightened risk of acquisition and transmission of infection, people who are incarcerated may also face barriers in accessing health care. For instance, the 2009 H1N1 vaccine roll-out exposed the failure to incorporate prisons into planning efforts (Akiyama et al., 2020). On the other hand, long-term carceral settings may facilitate easier deployment of a multi-dose vaccine.
People Experiencing Homelessness
The United States has a large number of people experiencing homelessness, who also may experience greater risks related to COVID-19. Between 2007 and 2019, the United States had approximately 500,000 individuals experiencing homelessness on any given night (Tsai and Wilson, 2020). People aged <65 years experiencing homelessness have an all-cause mortality rate that was already 5–10 times higher than that in the general population before the arrival of COVID-19; this disparity in mortality could be further widened by the pandemic (Tsai and Wilson, 2020). Homelessness can exacerbate conditions that drive SARS-CoV-2 transmission, including crowded shelters/housing and limited access to basic hygiene, such as hand-washing facilities (Tsai and Wilson, 2020). Homeless individuals often have less access to health care, which can limit their access to COVID-19 testing, quarantine, and treatment (Tsai and Wilson, 2020). Additionally, the transient and geographically mobile nature of populations experiencing homelessness could undermine efforts to track infection and prevent transmission (Tsai and Wilson, 2020).
People with Mental and Physical Disabilities
Having a disability, in and of itself, does not put individuals at a higher risk for SARS-CoV-2 infection or severe COVID-19 illness—according to CDC, the key factor lies in the likelihood of having serious underlying comorbid conditions (CDC,
2020h). However, adults with disabilities are three times more likely to have conditions such as heart disease, stroke, diabetes mellitus, or cancer when compared to adults without disabilities (CDC, 2020h), which puts them at a higher risk of severe illness from COVID-19. In addition, some groups experience an increased risk due to the living conditions necessitated by their disability. For example, some individuals with limited mobility will frequently come into unavoidable close contact with others, such as caregivers (CDC, 2020h). Additionally, millions of people with developmental disabilities live in group homes as a direct result of court mandates requiring depopulating institutions. Some people with disabilities who may have trouble understanding information or engaging in safe behavior—such as social distancing or hand washing—are also at increased risk (CDC, 2020h), and those who may not be able to communicate or convey the symptoms they experience from COVID-19 can lead to an increased risk of infecting others or having unrecognized illness (CDC, 2020h).
Differential Impact Across Sex and Gender
Current evidence suggests that men and women have similar rates of COVID-19 disease. However, men who contract COVID-19 are at greater risk for severe outcomes and death, regardless of age. In one public data set, the proportion of men who died from COVID-19 was 2.4 times that of women (Jin et al., 2020). However, the broader social and economic impacts of COVID-19 are intensified for women and girls because of their gender (UNWomen, 2020). These impacts are being amplified in many contexts where social cohesion has been undermined and institutional capacity and services have been limited. The impacts of women’s and girls’ generally lower economic status have been compounded by COVID-19, and the disruption of services for children and older persons has created an additional burden of unpaid care work on women and girls. Deepening economic and social stress, restricted movement, and social isolation measures have led to exponential increases in gender-based violence (Kofman and Garfin, 2020), as many women have been forced to “lockdown” with their abusers while support services for survivors of abuse have become inaccessible (Usher et al., 2020).
Differential Impact Across Geographic Regions
Across geographic regions within the United States, different trends have emerged. As of September 14, 2020, 31 out of 50 states are classified as COVID-19 hot spots (KFF, 2020). Hot spots are defined as states where (1) cases have increased by more than 5 percent over the last 2 weeks; (2) the 7-day rolling average positivity rate exceeds 10 percent or has increased by more than 1 percent over the last 2 weeks; and (3) per 1 million persons, new daily cases are more than 100 (KFF, 2020). Differences also exist across states based on policies such as social distancing requirements (e.g., non-essential business
closures, stay-at-home orders, large gathering bans), removal of barriers to testing and treatment (e.g., paid sick leave), and whether the states are reporting data regarding illness and mortality in long-term care facilities (KFF, 2020), a key factor contributing to the differential burden of COVID-19 across jurisdictions.
People Who Are Undocumented
People who are undocumented or otherwise living without clear legal status may also experience higher risks due to COVID-19. Although the populations of Hispanic immigrant communities tend to be relatively young and healthy, the prevalence of diabetes mellitus—a risk factor for more severe COVID-19 disease—is 22 percent among people who are Hispanic, which is the highest prevalence in any racial ethnic group in the United States (Page et al., 2020). Additionally, many undocumented immigrants work in service industries and are unable to isolate at home (Page et al., 2020). Health care system and access problems also compound the inequities faced by this population. The Patient Protection and Affordable Care Act does not provide health insurance coverage eligibility to undocumented individuals; as a result, an estimated 7.1 million undocumented immigrants lack health insurance and are prevented from accessing health care (Page et al., 2020). Under the Public Health Service Act, the United States can provide free COVID-19 care, but it is unclear how this has applied in the current pandemic situation. Out-of-pocket fees will likely limit COVID-19 testing and provision of appropriate care; even those who can and do access health care, whether in person or via telehealth, may struggle with limited English and may rely on outdated or incorrect health information available online (Page et al., 2020).
Children
More research is needed to understand the impact of SARS-CoV-2 infection on children. According to data compiled by the American Academy of Pediatrics (AAP) as of September 10, 2020, children and adolescents account for 10 percent of COVID-19 cases and less than 0.3 percent of deaths (AAP and CHA, 2020). Most children diagnosed with COVID-19 experience mild symptoms, most commonly fever and cough (NASEM, 2020). Although children tend to experience mild infections, a study of 582 children aged <18 years in 21 countries found that 62 percent of those with COVID-19 were admitted to the hospital, 8 percent required intensive care unit (ICU) admission, and 4 percent required mechanical ventilation (Gotzinger et al., 2020). Research on multisystem inflammatory syndrome in children, a rare but severe pediatric disease that is temporally associated with COVID-19, is ongoing (Ahmed et al., 2020), and consistent with observations previously described, children who are Black, Hispanic or Latinx, American Indian and Alaska Native, or who have certain underlying conditions (e.g., obesity, lung disease) are at increased risk of hospitalization or
death due to COVID-19 (Bixler et al., 2020; Kim et al., 2020). One study found that, among adolescent (under the age of 21) COVID-19-related deaths reported to CDC from mid-February through the end of July 2020, 78 percent were Black, Hispanic or Latinx, or American Indian and Alaska Native individuals (Bixler et al., 2020). Overall, AAP has reported that as of September 10, 2020, 1.8 percent of all child COVID-19 cases resulted in hospitalization (AAP and CHA, 2020). The COVID-19 pandemic will likely shape the worldview, hygiene habits, and consumer behavior of children, and it remains to be seen how profoundly the pandemic interferes with children’s development, education, and long-term relationships. Some children may face permanent life alterations or developmental impairments, such as through the effects of acute malnutrition, exposure to toxic stress, family breakdown, child labor, or teenage pregnancy (UN, 2020a). Increasing joblessness associated with the COVID-19 pandemic will likely have long-term consequences for child poverty. Furthermore, the longer schools remain closed, the less likely children will be able to catch up in terms of both education and life skills (UN, 2020a). Current COVID-19 vaccine trials do not include children, a gap that must be filled to ensure safety and efficacy of COVID-19 vaccine in pediatric populations (Branswell, 2020).
People Who Are Pregnant or Breastfeeding
Emerging evidence suggests that pregnant women may be at an increased risk of developing severe COVID-19 disease that requires ICU admission and mechanical ventilation (Cohen, 2020b; Ellington et al., 2020). Moreover, Black and Hispanic women who are pregnant appear to be disproportionately affected by SARS-CoV-2 infection during pregnancy (Ellington et al., 2020), and factors such as increased maternal age, high body mass index, chronic hypertension, and pre-existing diabetes have been associated with severe COVID-19 during pregnancy (Allotey et al., 2020). In addition, infants born to women who are infected with SARS-CoV-2 during pregnancy appear to be at an increased risk for adverse outcomes, including preterm birth and admission to a neonatal intensive care unit (Allotey et al., 2020). People breastfeeding infants while infected with SARS-CoV-2 does not appear to put the infants at risk (Chambers et al., 2020). Pregnant women are not generally prioritized to receive new vaccines, given the potential for fetal harm (Cohen, 2020b). Pregnant women have been excluded from COVID-19 vaccine clinical trials, leaving deployment of any COVID-19 vaccine in this group without evidence as to their safety and efficacy (LaCourse et al., 2020).
COVID-19 VACCINE LANDSCAPE
The development and widespread allocation and distribution of a safe and effective COVID-19 vaccine is the cornerstone of establishing
community-level protection and suppressing the COVID-19 pandemic (O’Callaghan et al., 2020). The global scope of the COVID-19 pandemic and the urgent need for widespread vaccination—perhaps of up to 60 percent of the worldwide population—has created an unparalleled scenario in which the timeline for vaccine development is being compressed from what has typically been 1–2 decades to just 1–2 years or less (Graham, 2020; Lurie et al., 2020; O’Callaghan et al., 2020; Steenhuysen and Kelland, 2020). Developing an effective vaccine against a newly discovered viral pathogen in such a short time frame is unprecedented, but efforts around the world have now generated multiple promising candidates that are entering various stages of clinical trials. However, the successful development of a vaccine will give rise to another host of unprecedented logistical challenges related to manufacturing, purchasing, distribution, allocation, and uptake. These challenges are compounded and intensified by the need to rapidly manufacture and equitably distribute billions of doses of vaccine concurrently across the globe.
Vaccine Development
A COVID-19 vaccine could be effective in two ways: either by preventing people from getting infected or by reducing the severity of disease if a person does become infected (Chen, 2020). Candidate vaccines are tested in three phases (see Table 1-2 for more detail) of clinical trials focusing on (1) safety, a primary concern through every phase of testing; (2) the
TABLE 1-2 Explanation of Phases of Vaccine Trials
| Phase | Name | Explanation |
|---|---|---|
| Phase I | Safety Trials | The vaccine is given to a small number of people. Dosage, safety, and stimulation of the immune system are tested. This is the first trial in humans. |
| Phase II | Expanded Trials | The vaccine is given to hundreds of people across different population groups to see how and if the vaccine behaves differently in them. These test further the safety and stimulation of the immune system. |
| Phase III | Efficacy Trials | The vaccine is given to thousands of people to monitor how many become infected or develop the disease in comparison to a placebo control group. This helps establish whether or not the vaccine can protect against the virus, and additional safety monitoring is conducted as well. (A COVID-19 vaccine will have to protect at least 50 percent of those who received the vaccination in order to be deemed effective by the U.S. Food and Drug Administration.) |
SOURCES: Corum et al., 2020; FDA, 2018; Lurie et al., 2020.
induction of an immune response; and (3) efficacy in an ideal setting, prior to assessing real-world effectiveness in post-marketing Phase IV trials (Chen, 2020). A key indicator of vaccine efficacy is a robust and durable immunogenic response (O’Callaghan et al., 2020). Fortunately, the genetic sequence of SARS-CoV-2 appears to be relatively stable thus far, which is promising for a vaccine’s ability to provide durable protection and to match currently circulating variants of the virus (Chen, 2020; Dearlove et al., 2020). In order to be authorized for use, the U.S. Food and Drug Administration (FDA) guidance indicates that a COVID-19 vaccine will need to be at least 50 percent efficacious in placebo-controlled trials (Craven, 2020; FDA, 2020).
Major Ongoing Development Efforts
According to the World Health Organization (WHO), 149 COVID-19 vaccines are currently in pre-clinical development and 38 candidate vaccines are undergoing evaluation in clinical trials in the United States, Europe, and China (Lee et al., 2020; WHO, 2020a). As of early September 2020, the Regulatory Affairs Professionals Society (Craven, 2020) vaccine tracker is currently tracking 45 vaccine candidates, many of which are in Phase I–III trials and some of which are promising candidates in the preclinical stages of research and development (Craven, 2020). Globally to date, only one vaccine has been approved, from the Gamaleya Research Institute of Epidemiology and Microbiology in Moscow, Russia; however, it has not yet undergone Phase III clinical trials so its efficacy is unknown, and it has only been approved in Russia (Craven, 2020). Domestically, the U.S. government has homed in on six COVID-19 vaccine candidates, with four currently in Phase III trials: the Johnson & Johnson JNJ-78436735, the Moderna/NIAID mRNA 1273, the University of Oxford/AstraZeneca AZD1222, and the Pfizer and BioNTech BNT162 (Craven, 2020). More details follow about all six vaccine candidates currently funded through Operation Warp Speed (OWS). Other major candidates (several of which are also being funded by the Coalition for Epidemic Preparedness Innovations) include vaccines being developed by Clover Biopharmaceuticals, the University of Queensland, Sinovac, the Wuhan Institute of Biological Products/Sinopharm, CanSino Biologics, and the University of Melbourne and Murdoch Children’s Research Institute (Craven, 2020).
Operation Warp Speed
In May 2020, the U.S. Department of Health and Human Services (HHS) launched OWS as a public–private partnership with the objective of delivering 300 million doses of a safe and effective COVID-19 vaccine by
January 2021 (HHS, 2020a). OWS is a collaboration that involves multiple federal entities (HHS and its agencies and the U.S. Department of Defense—with additional involvement by the U.S. Departments of Agriculture, Energy, and Veterans Affairs) and NIH’s partnerships with 18 biopharmaceutical companies working to develop a COVID-19 vaccine (HHS, 2020a).
As of early September 2020, OWS has publicly announced six contracts supporting vaccine development, each including a clause that guarantees a supply of COVID-19 vaccine to the U.S. government should a vaccine receive approval and licensure from FDA (HHS, 2020a). The vaccine candidates included span four platform technologies: mRNA, replication-defective vector, subunit protein adjuvanted, and live-attenuated vector (Slaoui, 2020). It is anticipated that OWS may pursue one additional agreement to complete its portfolio, potentially under the live-attenuated vector platform. The six vaccine candidates currently supported under OWS include those being developed by:
- AstraZeneca and the University of Oxford (replication-defective vector)—OWS is providing up to $1.2 billion in support, and at least 300 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
- GlaxoSmithKline and Sanofi (protein adjuvanted)—OWS is providing up to $2 billion in support, and at least 100 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
- Johnson & Johnson (Janssen) (replication-defective vector)—OWS is providing up to $1 billion in support, and at least 100 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
- Moderna (mRNA)—OWS is providing up to $1.5 billion in support, and at least 100 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
- Novavax (protein adjuvanted)—OWS is providing up to $1.6 billion in support, and at least 100 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
- Pfizer and BioNTech (mRNA)—OWS is providing up to $1.95 billion in support, and at least 100 million doses of vaccine are guaranteed to the U.S. government (HHS, 2020a).
From among these six candidates, four vaccine candidates are furthest along in development, all of which aim to induce antibodies against the receptor-binding domain of the surface spike protein of SARS-CoV-2 (O’Callaghan et al., 2020). The four candidates span two categories:
- Messenger RNA (mRNA) vaccines: Moderna (mRNA-1273) and Pfizer/BioNTech (BNT 162)
- Adenovirus replication-defective vectored vaccines: AstraZeneca and the University of Oxford (AZD1222) and Johnson & Johnson (JNJ-78436735)
Categories of the OWS Candidate COVID-19 Vaccines Currently in Phase III Trials
An mRNA vaccine uses a novel method for inducing the production of a robust immune response that does not require introducing SARS-CoV-2 itself. It delivers mRNA coding for the SARS-CoV-2 antigen into human cells, where antigen can be produced (O’Callaghan et al., 2020). This type of vaccine would be easier to produce in mass quantities than would other categories of COVID-19 vaccine, but an mRNA vaccine has never before been approved for commercial use to prevent infections. Both Moderna’s and Pfizer and BioNTech’s versions of this type of vaccine are currently being tested in Phase III studies and will require two doses (28 days between doses for Moderna’s vaccine and 21 days between doses for Pfizer and BioNTech’s vaccine) to provide adequate immune response and clinical protection (Jackson et al., 2020; Pfizer, 2020).
Adenovirus replication-defective vectored vaccine candidates use different vectors to deliver recombinant SARS-CoV-2 spike protein genes—derived from the surface of the virus—to human cells and induce an immune response (O’Callaghan et al., 2020). AstraZeneca and the University of Oxford developed a replication-defective simian adenovirus vector-based COVID-19 vaccine candidate that recently resumed Phase III trials outside the United States after they were paused to allow for a safety review following a suspected adverse event (trials remain paused in the United States); the candidate is being tested for use with either one or two doses (AstraZeneca, 2020). Johnson & Johnson’s adenovirus vector-based COVID-19 vaccine candidate leverages the company’s AdVac technology, which was also used for its Ebola vaccine that has been approved for use by the European Commission; the candidate being tested in Phase III trials uses a one-dose regimen (Johnson & Johnson, 2020). Johnson and Johnson’s candidate is anticipated to remain stable at –20 degrees Celsius, with similar requirements for the AstraZeneca and University of Oxford vaccine candidate. For the two COVID-19 vaccine candidates using mRNA technology, cold chain requirements are among the highest concerns for manufacturing, with ultra-cold storage (–80 degrees Celsius) potentially required (Slaoui, 2020; Taylor, 2020).
Expediting Vaccine Development
Given the urgency of the pandemic, multiple strategies are being employed or considered to help expedite the COVID-19 vaccine development
process. Some vaccine developers are conducting vaccine immunogenicity and efficacy trials in parallel, instead of sequentially, and liaising with multiple regulatory bodies to expedite the path to approval and licensure (Steenhuysen and Kelland, 2020). Human challenge trials offer the possibility of expediting this process by approving a vaccine based on its expected benefit, if the antibody levels in trial participants are similar to those observed in people infected in the real world (Chen, 2020). Human challenge trials have also been suggested to expedite vaccine development, but in addition to serious ethical concerns related to infecting healthy participants to test a vaccine, such trials necessarily involve very small sample sizes that are insufficient to assess safety (Chen, 2020; Cohen, 2020a). To facilitate large-scale clinical trial testing of COVID-19 vaccine candidates (and monoclonal antibodies), NIH’s National Institute of Allergy and Infectious Diseases (NIAID) established the COVID-19 Prevention Trials Network in July 2020 (Cohen, 2020a) by merging four existing NIAID-funded clinical trial networks: the HIV Vaccine Trials Network, the HIV Prevention Trials Network, the Infectious Diseases Clinical Research Consortium, and the AIDS Clinical Trials Group.
In the United States, regulatory requirements have been adjusted to expedite authorization and clinical trials, and FDA is encouraging studies on the use of COVID-19 vaccines among pregnant women as well as the enrollment of racial and ethnic minorities disproportionately affected by the disease (Chen, 2020). Trials including children are anticipated to occur eventually and will be necessary to establish safety and efficacy in pediatric populations (Branswell, 2020). Other countries have existing emergency use provisions that allow for the use of a candidate vaccine among people at high risk of disease while Phase III trials are ongoing (Edmond, 2020). From the perspective of regulatory bodies, however, accelerating vaccine development increases the risk that adverse events will not be detected prior to widespread distribution, given smaller Phase III trial enrollment and shorter follow-up time with participants (GAO, 2020). Rapid development and testing may also give rise to concerns about vaccine safety and exacerbate vaccine hesitancy among the general public, which could impact vaccine uptake when distribution of a vaccine begins (Schaffer DeRoo et al., 2020).
Vaccine Manufacturing
When a successful COVID-19 vaccine has been approved, fulfilling the global demand will require the rapid production of an unprecedented number of doses. The required number of vaccine doses and the necessary manufacturing infrastructure and facilities will depend on the type of vaccine candidate(s) that is (are) successful (Khamsi, 2020). Inevitably,
this demand will create major manufacturing-related challenges, including insufficient capacity, material shortages, and bottlenecks. The current global supply chain for vaccines is characterized by a small number of large companies with the capacity to manufacture large quantities of vaccine doses, but those companies are already operating at or near capacity producing other critical vaccines for seasonal influenza and other infectious diseases (e.g., measles), which they must continue to produce (Edmond, 2020; Furlong, 2020; Khamsi, 2020). Some pharmaceutical companies are planning to manufacture different components of a COVID-19 vaccine at different sites worldwide (Furlong, 2020). However, travel restrictions are making it difficult for companies to deploy experts to oversee production sites and technology transfers in other countries (Chen, 2020).
A major limiting factor in vaccine manufacturing could be shortages in automated filling and finishing capacity—this involves the vaccine being placed into vials or syringes, sealed, and packed for shipping (Chen, 2020). Further manufacturing bottlenecks could be caused by shortages of raw materials and adjuvants for subunit vaccines, plus, vials, stoppers, and supplies for labels and package inserts (Chen, 2020; Khamsi, 2020). Vaccine manufacturing also requires a skilled workforce, which can prevent smaller manufacturers or those in low-resource settings from entering the market. This inequity has the potential to impede access to effective vaccines outside of wealthier nations (Anderson, 2020; Furlong, 2020).
Various strategies could help address these manufacturing challenges. For example, the adoption of platform technologies for manufacturing different types of vaccines using the same production process in a single facility could help solve problems of scale-up and speed (Furlong, 2020). However, platform technologies have not yet been used to produce mRNA-based vaccines (Furlong, 2020) and they do not enable single-dose vials to be filled at the same rapid speed at which doses are produced. Process intensification—which involves densification of equipment and chaining to ensure continuous or semi-continuous processing—could increase production volume, reduce costs, and enable smaller facilities in lower-resource settings with less access to skilled workers to enter the supply chain (Anderson, 2020).
Financing and Purchasing
From a financing perspective, developing and manufacturing vaccines is inherently risky and hugely costly, even in normal circumstances. Only about 6 percent of vaccine candidates ultimately make it to market (Steenhuysen and Kelland, 2020), and setting up a production facility in the United States can cost US$50–$500 million for a monovalent vaccine and up to US$700 million for a polyvalent vaccine (Anderson, 2020). Produc-
tion of a COVID-19 vaccine is projected to cost in the billions of dollars, which far exceeds current public and private financing commitments (Khamsi, 2020).4 The current pandemic situation has required concurrent investment in developing candidate vaccines of unknown benefit and in scaling up vaccine-specific manufacturing capacity and supply chains—capacity that might never be used if that candidate proves unsafe or ineffective (Furlong, 2020; Khamsi, 2020). Some of this enormous financial risk is being mitigated by advance-purchase agreements with countries for promising vaccine candidates (Furlong, 2020). However, a major concern is the emergence of vaccine nationalism, whereby governments hoard supplies, buy up large amounts of future doses, and seek to manufacture vaccines domestically to maintain control (Furlong, 2020). Manufacturing “at risk” can expedite the distribution process through upfront investment to begin mass production of a vaccine while it is still undergoing clinical trials (Chen, 2020; Steenhuysen and Kelland, 2020). If clinical trials demonstrate that a vaccine is safe and effective, then huge numbers of doses will already be available for distribution to populations at greatest risk. The inherent risk is the loss of that investment if the candidate vaccine is unsuccessful.
Vaccine Distribution
If and when a sufficient number of doses of COVID-19 vaccine are manufactured, they must reach the people who need them. Distribution of the vaccine will present its own set of complex challenges related to cost, access, logistics, and allocation/prioritization of the limited number of doses that will be available in the early stages if a vaccine is successful, as well as mitigating concerns about vaccine safety. Some vaccines may require two doses to produce immunity, creating further complexity in distribution, although administering multiple doses might be easier in institutional settings (Chen, 2020). The global supply chain is untested in operating at this scale, and any breakdown could have serious consequences for effective vaccine deployment (Chen, 2020; Steenhuysen and Kelland, 2020). Lack of capacity for cold storage and insufficient cold supply chains could pose major barriers to global vaccine distribution. Some vaccines (e.g., mRNA vaccines) may require storage and shipping at an ultra-cold temperature (–80 degrees Celsius), which can cause glass vials to shatter (Chen, 2020), but companies developing mRNA vaccines are exploring ways to make the vaccines stable at higher temperatures (Chen, 2020). Broken cold chains are a major cause of vaccine wastage and could limit access to vaccines in
___________________
4 Some large funders are investing in large companies with an established track record in vaccine development, regulatory approval, and production at scale, while others are investing in smaller entities with promising candidates but less experience in approval and production (Steenhuysen and Kelland, 2020).
regions of the world where breakdowns in the cold supply chain are already frequent.5 Massive numbers of new vials, syringes, and needles will also be needed to deliver billions of vaccine doses to the people who need them (Chen, 2020). Potential solutions include innovations such as prefilled plastic syringes,6 plastic vials with glass linings,7 and multi-dose bags or vials that contain larger numbers of doses, which can be filled more quickly and are easier to store (Furlong, 2020). However, it is important to note that such novel solutions will require testing to ensure no interaction between the vaccine and storage materials, such as plastic.
Moving beyond supply concerns and onto demand side considerations, broad vaccine acceptance will be key to successful vaccine uptake as well. Already, surveys indicate that more work is needed to promote a potential COVID-19 vaccine and ensure public trust in a vaccine and the processes involved in its delivery. Chapter 7 of this report, focused on vaccine acceptance, discusses these issues at length.
Last, vaccine distribution, although essential, is but one part of a pandemic response and one tool for responding to the COVID-19 pandemic. Other efforts to mitigate the transmission of COVID-19, such as social distancing, testing, diagnostic testing, contact tracing, and wearing masks all continue to be of vital importance especially during the early phases of vaccinations. Continued guidance on these practices remains an important reality, including discussions of optimal strategies for leveraging these interventions in combination. The introduction of a COVID-19 vaccine would be a valuable addition to the pandemic response, but must be a part of a multi-pronged public health response to COVID-19.
CONTEXTUALIZING COVID-19 VACCINATION EFFORTS IN THE CURRENT SYSTEM
In conducting its work, the committee assumed that the national COVID-19 vaccine program will build on the solid and tested national vaccine program that has existed for 65 years and has evolved and improved over the years. The program started in 1955 with the development of an effective poliomyelitis inactivated vaccine. Over the years, it expanded to include a score of vaccines leading to major public health improvements. Polio was eliminated from the United States and measles transmission was
___________________
5 Furthermore, cold chains are also very energy intensive and require refrigerants that contribute to global warming (Furlong, 2020).
6 HHS and the U.S. Department of Defense are supporting efforts to increase capacity for manufacturing up to half a billion pre-filled plastic syringes by 2021, but this could be delayed by the need for FDA approval for the technology (Chen, 2020).
7 However, larger vials that contain 5–20 doses can lead to potential waste if all of the doses are not used within 24 hours after the vial is opened (Chen, 2020).
interrupted, appearing now only as the result of importations of the virus. Mumps, rubella, Haemophilus influenzae B meningitis, and other diseases have become a memory and are likely to be unknown by new parents.
The United States national vaccine program is a coalition of seamless components, and OWS recently released a figure demonstrating anticipated plans for distribution of a COVID-19 vaccine that reflects the relationship between various partners (see Figure 1-2). FDA determines the safety and efficacy of new vaccines, and has the regulatory authority to license them for use in the United States. ACIP provides consultation to CDC on how to use the vaccines. CDC in turn develops guidelines on age groups, the routine immunization schedule, and the need for boosters, and it monitors the provision of the vaccines based on state needs. Within the framework of federal guidelines, STLT authorities have had the flexibility to adapt the system to their own needs. Over the years, some STLT authorities have developed strong programs using health care providers (e.g., pediatricians, family practitioners, registered nurses) to administer a vaccine—while other states have used public health clinics. For many years, varied systems for tracking vaccinated children could not communicate, but over time, even this difficulty has been addressed.
However, the vaccination program goes beyond this. States can request a CDC field assignee from the Program Operations Branch in the Immu-
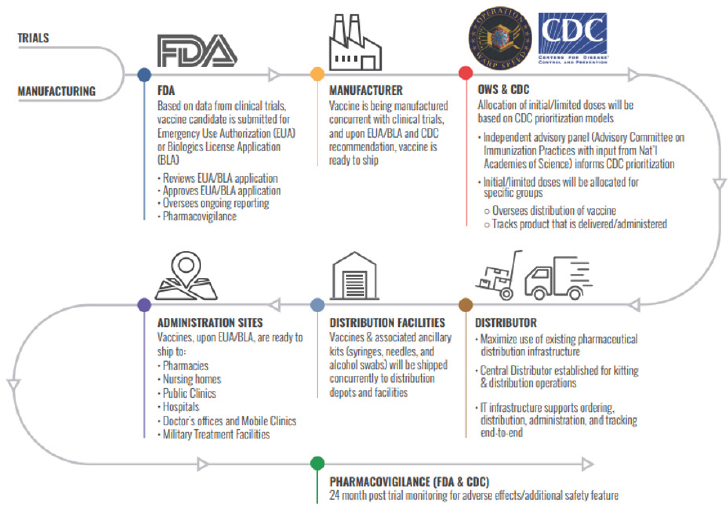
SOURCE: HHS, 2020b.
nization Services Division of the National Center for Immunization and Respiratory Diseases to help in the delivery of vaccines (there are currently approximately 70 assignees managed under this program) (CDC, 2015). Over the decades, the vast majority of states have made use of that provision, providing a strong bond between the federal government and the states. Surveillance and assessment guidelines are developed by CDC with state input. Unusual problems such as adverse reactions, unexplained deaths in those vaccinated, failure to protect, and a host of other problems result in immediate assistance from CDC due to this unusual federal–state relationship. Assignees are supervised in their daily activities by the state rather than by CDC. The state health officer then coordinates with every county and city in the state to oversee the provision of vaccines, surveillance, and assessment. The coalition of federal, state, county, and city health workers focused on immunization activities has been historically very strong.
However, the existing national vaccine program will require significant modifications to address the challenges posed by the delivery of new COVID-19 vaccines. Early COVID-19 vaccines may require ultra-cold storage not needed for other vaccines. States will have to arrange for these vaccines to be given in settings with special capabilities, such as medical facilities.
The need for real-time information on people vaccinated by age, sex, occupation, etc., as well as the need for rapid information on adverse events following immunization (equivalent to a Phase IV study) will require augmentation of the current surveillance/assessment system, probably involving training programs and new assignees to the vaccination program. Flexibility and agility will be important, and opportunities to embed the national COVID-19 vaccine program within current vaccination program activities must be sought. The basic approach of federal guidelines and close federal/state administration of programs will continue to be crucial.
REFERENCES
AAP (American Academy of Pediatrics) and CHA (Children’s Hospital Association). 2020. Children and COVID-19: State data report. American Academy of Pediatrics and Children’s Hospital Association. https://downloads.aap.org/AAP/PDF/AAP%20and%20CHA%20-%20Children%20and%20COVID-19%20State%20Data%20Report%208.6.20%20FINAL.pdf (accessed September 17, 2020).
Adakai, M., M. Sandoval-Rosario, F. Xu, T. Aseret-Manygoats, M. Allison, K. J. Greenlund, and K. E. Barbour. 2018. Health disparities among American Indians/Alaska Natives—Arizona, 2017. Morbidity and Mortality Weekly Report 67(47):1314.
Ahmed, M., S. Advani, A. Moreira, S. Zoretic, J. Martinez, K. Chorath, S. Acosta, R. Naqvi, F. Burmeister-Morton, F. Burmeister, A. Tarriela, M. Petershack, M. Evans, A. Hoang, K. Rajasekaran, S. Ahuja, and A. Moreira. 2020. Multisystem inflammatory syndrome in children: A systematic review. EClinicalMedicine. doi: 10.1016/j.eclinm.2020.100527.
Akiyama, M. J., A. C. Spaulding, and J. D. Rich. 2020. Flattening the curve for incarcerated populations—COVID-19 in jails and prisons. The New England Journal of Medicine 382:2075–2077. doi: 10.1056/NEJMp2005687.
Allotey, J., E. Stallings, M. Bonet, M. Yap, S. Chatterjee, T. Kew, L. Debenham, A. C. Llavall, A. Dixit, D. Zhou, R. Balaji, S. I. Lee, X. Qiu, M. Yuan, D. Coomar, M. van Wely, E. van Leeuwen, E. Kostova, H. Kunst, A. Khalil, S. Tiberi, V. Brizuela, N. Broutet, E. Kara, C. R. Kim, A. Thorson, O. T. Oladapo, L. Mofenson, J. Zamora, and S. Thangaratinam. 2020. Clinical manifestations, risk factors, and maternal and perinatal outcomes of coronavirus disease 2019 in pregnancy: Living systematic review and meta-analysis. BMJ 370:m3320. doi: 10.1136/bmj.m3320.
Anderson, T. 2020. Intensifying vaccine production. Bulletin of the World Health Organization 98:302–303. doi: 10.2471/BLT.20.020520.
Arasteh, K. 2020. Prevalence of comorbidities and risks associated with COVID-19 among Black and Hispanic populations in New York City: An examination of the 2018 New York City community health survey. Journal of Racial and Ethnic Health Disparities. doi: 10.1007/s40615-020-00844-1.
AstraZeneca. 2020. COVID-19 vaccine AZD1222 showed robust immune responses in all participants in Phase I/II trial. https://www.astrazeneca.com/media-centre/press-releases/2020/covid-19-vaccine-azd1222-showed-robust-immune-responses-in-all-participants-in-phase-i-ii-trial.html (accessed September 17, 2020).
Bixler, D., A. D. Miller, C. P. Mattison, et al. 2020. SARS-CoV-2–associated deaths among persons aged <21 years—United States, February 12–July 31, 2020. Morbidity and Mortality Weekly Report. https://www.cdc.gov/mmwr/volumes/69/wr/mm6937e4.htm (accessed September 17, 2020).
Branswell, H. 2020. Will COVID-19 vaccines be safe for children and pregnant women? The data, so far, are lacking. STAT. https://www.statnews.com/2020/08/19/will-covid-19-vaccines-be-safe-for-children-and-pregnant-women-the-data-so-far-are-lacking/#:~:text=Outside%20of%20the%20U.S.%2C%20two,12%20to%2065%20to%20enroll (accessed September 15, 2020).
CDC (Centers for Disease Control and Prevention). 2010. Interim results: Influenza A (H1N1) 2009 monovalent vaccination coverage—United States, October–December 2009. Morbidity and Mortality Weekly Report 59(02):44–48. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5902a4.htm (accessed September 17, 2020).
CDC. 2015. Immunization Services Division (ISD). Atlanta, GA: CDC. https://www.cdc.gov/ncird/isd.html (accessed September 21, 2020).
CDC. 2020a. Coronavirus disease 2019 case surveillance—United States, January 22–May 30, 2020. 69(2). Morbidity and Mortality Weekly Report 69(24):759–765. https://www.cdc.gov/mmwr/volumes/69/wr/mm6924e2.htm (accessed September 17, 2020).
CDC. 2020b. COVIDview Weekly Summary. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covidview/index.html (accessed September 15, 2020).
CDC. 2020c. COVID-19: Health equity considerations and racial and ethnic minority groups. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/race-ethnicity.html (accessed September 17, 2020).
CDC. 2020d. COVID-19: Hospitalization and death by race/ethnicity. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/investigations-discovery/hospitalization-death-by-race-ethnicity.html (accessed September 17, 2020).
CDC. 2020e. COVID-19: Nursing home care. Atlanta, GA: CDC National Center for Health Statistics. https://www.cdc.gov/nchs/fastats/nursing-home-care.htm (accessed September 17, 2020).
CDC. 2020f. COVID-19: Older adults. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/older-adults.html (accessed September 17, 2020).
CDC. 2020g. COVID-19: People with certain medical conditions. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html (accessed September 17, 2020).
CDC. 2020h. COVID-19: People with disabilities. Atlanta, GA: CDC. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-disabilities.html (accessed September 17, 2020).
CDC. 2020i. COVID-NET: A weekly summary of U.S. COVID-19 hospitalization data. Atlanta, GA: CDC. https://gis.cdc.gov/grasp/COVIDNet/COVID19_3.html (accessed September 15, 2020).
CDC. 2020j. Residential care communities. Atlanta, GA: CDC National Center for Health Statistics. https://www.cdc.gov/nchs/fastats/residential-care-communities.htm (accessed September 17, 2020).
CDC. 2020k. About social determinants of health (SDOH). Atlanta, GA; CDC. https://www.cdc.gov/socialdeterminants/about.html (accessed September 21, 2020).
Chambers, C., P. Krogstad, K. Bertrand, D. Contreras, N. H. Tobin, L. Bode, and G. Aldrovandi. 2020. Evaluation for SARS-CoV-2 in breast milk from 18 infected women. JAMA. Published online August 19, 2020. doi: 10.1001/jama.2020.15580.
Chen, C. 2020. How—and when—can the coronavirus vaccine become a reality? ProPublica. https://www.propublica.org/article/how-and-when-can-the-coronavirus-vaccine-become-a-reality (accessed September 17, 2020).
Chidambaram, P. 2020. State reporting of cases and deaths due to COVID-19 in long-term care facilities. Kaiser Family Foundation. https://www.kff.org/coronavirus-covid-19/issue-brief/state-reporting-of-cases-and-deaths-due-to-covid-19-in-long-term-care-facilities (accessed September 17, 2020).
Cohen, J. 2020a. Controversial “human challenge” trials for COVID-19 vaccines gain support. Science. July 20, 2020. doi: 10.1126/science.abd9203.
Cohen, J. 2020b. The line is forming for a COVID-19 vaccine. Who should be at the front? Science. June 29, 2020. doi: 10.1126/science.abd5770.
Corum, J., S.-L. Wee, and C. Zimmer. 2020. Coronavirus vaccine tracker. The New York Times. https://www.nytimes.com/interactive/2020/science/coronavirus-vaccine-tracker.html (accessed September 17, 2020).
Craven, J. 2020. COVID-19 vaccine tracker. Rockville, MD: Regulatory Affairs Professionals Society. https://www.raps.org/news-and-articles/news-articles/2020/3/covid-19-vaccine-tracker (accessed September 17, 2020).
Crouse Quinn, S., S. Kumar, V. S. Freimuth, D. Musa, N. Casteneda-Angarita, and K. Kidwell. 2011. Racial disparities in exposure, susceptibility, and access to health care in the US H1N1 influenza pandemic. American Journal of Public Health 101(2):285–293. doi: 10.2105/AJPH.2009.188029.
Dearlove, B., E. Lewitus, H. Bai, Y. Li, D. B. Reeves, M. G. Joyce, P. T. Scott, M. F. Amare, S. Vasan, N. L. Michael, K. Modjarrad, and M. Rolland. 2020. A SARSCoV-2 vaccine candidate would likely match all currently circulating variants. Proceedings of the National Academy of Sciences 117(38):23652–23662. doi: 10.1073/pnas.2008281117.
Edmond, C. 2020. 3 challenges in creating a coronavirus vaccine—and how they are being overcome. The World Economic Forum COVID Action Platform. 14 May 2020. https://www.weforum.org/agenda/2020/05/coronavirus-covid-19-vaccine-industry (accessed September 17, 2020).
Ellington, S., P. Strid, V. Tong, K. Woodworth, R. Galang, L. Zambrano, J. Nahabedian, K. Anderson, and S. Gilboa. 2020. Characteristics of women of reproductive age with laboratory-confirmed SARS-CoV-2 infection by pregnancy status—United States, January 22–June 7, 2020. Morbidity and Mortality Weekly Report 69(25):769–775.
Essien, U. R., N. D. Eneanya, and D. C. Crews. 2020. Prioritizing equity in a time of scarcity: The COVID-19 pandemic. Journal of General Internal Medicine 35:2760–2762. doi: 10.1007/s11606-020-05976-y.
FDA (U.S. Food and Drug Administration). 2018. What are the different types of clinical research? Silver Springs, MD: FDA. https://www.fda.gov/patients/clinical-trials-what-patients-need-know/what-are-different-types-clinical-research (accessed September 15, 2020).
FDA. 2020. Development and licensure of vaccines to prevent COVID-19: Guidance for industry. Silver Springs, MD: FDA. https://www.fda.gov/media/139638/download (accessed September 17, 2020).
Furlong, A. 2020. Europe’s challenge of a lifetime: Manufacturing enough coronavirus vaccines. Politico.
GAO (U.S. Government Accountability Office). May 26, 2020. Science & tech spotlight: COVID-19 vaccine development. GAO Science, Technology Assessment, and Analytics. Washington, DC: GAO. https://www.gao.gov/products/GAO-20-583SP (accessed September 17, 2020).
Gold, J., K. Wong, C. Szablewski, P. Patel, J. Rossow, J. Da Silva, P. Natarajan, S. Bamrah Morris, R. Neblett Fanfair, J. Rogers-Brown, B. Bruce, S. Browning, A. Hernandez-Romieu, N. Furukawa, M. Kang, M. Evans, N. Oosmanally, M. Tobin-D’Angelo, C. Drenzek, D. Murphy, J. Hollberg, J. Blum, R. Jansen, D. Wright, W. Sewell III, J. Owens, B. Lefkove, F. Brown, D. Burton, T. Uyeki, S. Bialek, and B. Jackson. 2020. Characteristics and clinical outcomes of adult patients hospitalized with COVID-19—Georgia, March 2020. Morbidity and Mortality Weekly Report 69(18):545–550. doi: 10.15585/mmwr.mm6918e1.
Gotzinger, F., B. Santiago-Garcia, A. Noguera-Julian, M. Lanaspa, L. Lancella, F. Calo Carducci, N. Gabrovska, S. Velizarova, P. Prunk, V. Osterman, U. Krivec, A. Lo Vecchio, D. Shingadia, A. Soriano-Arandes, S. Melendo, M. Lanari, L. Pierantoni, N. Wagner, A. L’Huillier, U. Heininger, N. Ritz, S. Bandi, N. Krajcar, S. Roglic, M. Santos, C. Christiaens, M. Creuven, D. Buonsenso, S. Welch, M. Bogyi, F. Brinkmann, and M. Tebruegge. 2020. COVID-19 in children and adolescents in Europe: A multinational, multicentre cohort study. The Lancet Child & Adolescent Health 4(9):P653–P661. doi: 10.1016/S2352-4642(20)30177-2.
Graham, B. 2020. Rapid COVID-19 vaccine development. Science 368(6494):945–946. doi: 10.1126/science.abb8923.
Hatcher, S. M., C. Agnew-Brune, M. Anderson, L. D. Zambrano, C. E. Rose, M. A. Jim, A. Baugher, G. S. Liu, S. V. Patel, and M. E. Evans. 2020. COVID-19 among American Indian and Alaska Native persons—23 states, January 31–July 3, 2020. Morbidity and Mortality Weekly Report 69(34):1166–1169. doi: 10.15585/mmwr.mm6934e1.
Hawks, L., S. Woolhandler, and D. McCormick. 2020. COVID-19 in prisons and jails in the United States. JAMA Internal Medicine 180(8):1041–1042. doi: 10.1001/jamainternmed.2020.1856.
HHS (U.S. Department of Health and Human Services). 2020a. Fact sheet: Explaining Operation Warp Speed. Washington, DC: HHS. https://www.hhs.gov/about/news/2020/06/16/fact-sheet-explaining-operation-warp-speed.html (accessed September 17, 2020).
HHS. 2020b. Trump administration releases COVID-19 vaccine distribution strategy. Washington, DC: HHS. https://www.hhs.gov/about/news/2020/09/16/trump-administrationreleases-covid-19-vaccine-distribution-strategy.html (accessed September 22, 2020).
Ioannidis, J., C. Axfors, and D. G. Contopoulos-Ioannidis. 2020. Population-level COVID-19 mortality risk for non-elderly individuals overall and for non-elderly individuals without underlying diseases in pandemic epicenters. Environmental Research 188(September 2020):10980. doi: 10.1016/j.envres.2020.109890.
Jackson, L., E. Anderson, N. Rouphael, P. Roberts, M. Makhene, R. Coler, M. McCullough, J. Chappell, M. Denison, L. Stevens, A. Pruijssers, A. McDermott, B. Flach, N. DoriaRose, K. Corbett, K. Morabito, S. O’Dell, S. Schmidt, P. Swanson, M. Padilla, J. Mas-cola, K. Neuzil, H. Bennett, W. Sun, E. Peters, M. Makowski, J. Albert, K. Cross, W. Buchanan, R. Pikaart-Tautges, J. Ledgerwood, B. Graham, and J. Beigel. 2020. An MRNA vaccine against SARS-CoV-2—preliminary report. The New England Journal of Medicine. doi:10.1056/NEJMoa2022483.
Jin, J.-M., P. Bai, W. He, F. Wu, X.-F. Liu, D.-M. Han, S. Liu, and J.-K. Yang. 2020. Gender differences in patients with COVID-19: Focus on severity and mortality. Frontiers in Public Health 8(29 April 2020). doi: 10.3389/fpubh.2020.00152.
Johnson, A., and T. Buford. 2020. Early data shows African Americans have contracted and died of coronavirus at an alarming rate. ProPublica. http://wallstreetwindow.com/2020/04/early-data-shows-african-americans-have-contracted-and-died-of-coronavirus-at-an-alarming-rate-akilah-johnson-and-talia-buford-propublica-04-06-2020 (accessed September 17, 2020).
Johnson & Johnson. 2020. Johnson & Johnson initiates pivotal global phase 3 clinical trial of Janssen’s COVID-19 vaccine candidate. https://www.jnj.com/johnson-johnson-initiates-pivotal-global-phase-3-clinical-trial-of-janssens-covid-19-vaccine-candidate (accessed September 25, 2020).
KFF (Kaiser Family Foundation). 2020. State data and policy actions to address coronavirus. https://www.kff.org/coronavirus-covid-19/issue-brief/state-data-and-policy-actions-to-address-coronavirus (accessed September 17, 2020).
Khamsi, R. 2020. If a coronavirus vaccine arrives, can the world make enough? Nature 580. https://www.nature.com/articles/d41586-020-01063-8 (accessed September 17, 2020).
Killerby, M., R. Link-Gelles, S. Haight, C. Schrodt, L. England, D. Gomes, M. Shamout, K. Pettrone, K. O’Laughlin, A. Kimball, E. Blau, E. Burnett, C. Ladva, C. Szablewski, M. Tobin-D’Angelo, N. Oosmanally, C. Drenzek, D. Murphy, J. Blum, J. Hollberg, B. Lefkove, F. Brown, T. Shimabukuro, C. Midgley, J. Tate, and CDC COVID-19 Response Clinical Team. 2020. Characteristics associated with hospitalization among patients with COVID-19—Metropolitan Atlanta, Georgia, March–April 2020. Morbidity and Mortality Weekly Report 69(25):790–794. doi: 10.15585/mmwr.mm6925e1.
Kim, L., M. Whitaker, A. O’Halloran, et al. 2020. Hospitalization rates and characteristics of children aged <18 years hospitalized with laboratory-confirmed COVID-19—COVID-NET, 14 states, March 1–July 25, 2020. Morbidity and Mortality Weekly Report 69(32):1081–1088. doi: 10.15585/mmwr.mm6932e3.
Kirby, T. 2020. Evidence mounts on the disproportionate effect of COVID-19 on ethnic minorities. The Lancet Respiratory Medicine 8(6):547–548. doi: 10.1016/S2213-2600(20)30228-9.
Koff, W., and M. Williams. 2020. COVID-19 and immunity in aging populations—a new research agenda. The New England Journal of Medicine 383:804–805. doi: 10.1056/NEJMp2006761.
Kofman, Y. B., and D. R. Garfin. 2020. Home is not always a haven: The domestic violence crisis amid the COVID-19 pandemic. Psychological Trauma: Theory, Research, Practice, and Policy 12(S1):S199–S201. doi: 10.1037/tra0000866.
LaCourse, S., G. John-Stewart, and K. Adams Waldorf. 2020. Importance of inclusion of pregnant and breastfeeding women in COVID-19 therapeutic trials. Clinical Infectious Diseases 71(15):879–881. doi: 10.1093/cid/ciaa444.
Lee, G. M., B. P. Bell, and J. R. Romero. 2020. The Advisory Committee on Immunization Practices and its role in the pandemic vaccine response. JAMA 324(6):546–547. doi: 10.1001/jama.2020.13167.
Lurie, N., M. Saville, R. Hatchett, and J. Halton. 2020. Developing COVID-19 vaccines at pandemic speed. The New England Journal of Medicine 382(21):1969–1973. doi: 10.1056/NEJMp2005630.
Mau, M. K., K. Sinclair, E. P. Saito, K. N. Baumhofer, and J. K. Kaholokula. 2009. Cardiometabolic health disparities in native Hawaiians and other Pacific Islanders. Epidemiologic Reviews 31(1):113–129. doi: 10.1093/ajerev/mxp004.
Maxmen, A. 2020. California’s San Quentin Prison declined free coronavirus tests and urgent advice—now it has a massive outbreak. Nature 583:339–340. doi: 10.1038/d41586-020-02042-9.
Millett, G., A. Jones, D. Benkeser, S. Baral, L. Mercer, C. Beyrer, B. Honermann, E. Lankiewicz, L. Mena, J. Crowley, J. Sherwood, and P. Sullivan. 2020. Assessing differential impacts of COVID-19 on black communities. Annals of Epidemiology 47:37–44. doi:10.1016/j.annepidem.2020.05.003.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2020. Reopening K–12 schools during the COVID-19 pandemic: Prioritizing health, equity, and communities. Washington, DC: The National Academies Press.
Nikolich-Zugic, J., K. Knox, C. Tafich Rios, B. Natt, D. Bhattacharya, and M. Fain. 2020. SARS-CoV-2 and COVID-19 in older adults: What we may expect regarding pathogenesis, immune responses, and outcomes. GeroScience 42:505–514. doi: 10.1007/s11357-020-00193-1.
O’Callaghan, K. P., A. M. Blatz, and P. A. Offit. 2020. Developing a SARS-CoV-2 vaccine at warp speed. JAMA (324(5):437–438. doi: 10.1001/jama.2020.12190.
Page, K. R., M. Venkataramani, C. Beyrer, and S. Polk. 2020. Undocumented U.S. immigrants and COVID-19. The New England Journal of Medicine 382(21):e62. doi: 10.1056/NEJMp2005953.
Pfizer. 2020. Pfizer and Biontech announce early positive data from an ongoing phase 1/2 study of MRNA-based vaccine candidate against SARS-CoV-2. Pfizer News. https://www.pfizer.com/news/press-release/press-release-detail/pfizer-and-biontech-announce-early-positive-data-ongoing-0 (accessed September 17, 2020).
Plough, A., B. Bristow, J. Fielding, S. Caldwell, and S. Khan. 2011. Pandemics and health equity: Lessons learned from the H1N1 response in Los Angeles County. Journal of Public Health Management and Practice 17(1):20–27. doi: 10.1097/PHH.0b013e3181ff2ad7.
Poudel, A., J. Y. Zhou, D. Story, and L. Li. 2018. Diabetes and associated cardiovascular complications in American Indians/Alaskan Natives: A review of risks and prevention strategies. Journal of Diabetes Research 2018:2742565. doi: 10.1155/2018/2742565.
Price-Haywood, E., J. Burton, D. Fort, and L. Seoane. 2020. Hospitalization and mortality among black patients and white patients with COVID-19. The New England Journal of Medicine 382:2534–2543. doi: 10.1056/NEJMsa2011686.
RWJF (Robert Wood Johnson Foundation). 2020. Race, racism, and health. Princeton, NJ: RWJF. https://www.rwjf.org/en/library/collections/racism-and-health.html (accessed September 21, 2020).
Sanyaolu, A., C. Okorie, A. Marinkovic, R. Patidar, K. Younis, P. Desai, Z. Hosein, I. Padda, J. Mangat, and M. Altaf. 2020. Comorbidity and its impact on patients with COVID-19. SN Comprehensive Clinical Medicine 2:1069–1076. doi: 10.1007/s42399-020-00363-4.
Schaffer DeRoo, S., N. J. Pudalov, and L. Y. Fu. 2020. Planning for a COVID-19 vaccination program. JAMA 323(24):2458–2459. doi: 10.1001/jama.2020.8711.
Slaoui, M. 2020. Operation Warp Speed. Presentation at Committee on Equitable Allocation of Vaccine for the Novel Coronavirus Public Workshop.
Steenhuysen, J., and K. Kelland. 2020. Vaccine makers face biggest medical manufacturing challenge in history. Yahoo! News. https://news.yahoo.com/vaccine-makers-face-biggest-medical-110231019.html (accessed September 17, 2020).
Stokes, E. K., L. D. Zambrano, K. N. Anderson, E. P. Marder, K. M. Raz, S. El Burai Felix, Y. Tie, and K. E. Fullerton. 2020. Coronavirus disease 2019 case surveillance—United States, January 22–May 30, 2020. Morbidity and Mortality Weekly Report 69(24):759–765. doi: 10.15585/mmwr.mm6924e2.
Tai, D. B. G., A. Shah, C. A. Doubeni, I. G. Sia, and M. L. Wieland. 2020. The disproportionate impact of COVID-19 on racial and ethnic minorities in the United States. Clinical Infectious Diseases ciaa815. doi: 10.1093/cid/ciaa815.
Taylor, N. P. 2020. J&J starts COVID-19 vaccine phase 3, eyes early 2021 approval. Fierce Biotech. September 23, 2020. https://www.fiercebiotech.com/biotech/j-j-starts-covid-19-vaccine-phase-3-eyes-early-2021-approval (accessed September 22, 2020).
True, S., J. Cubanski, R. Garfield, M. Rae, G. Claxton, P. Chidambaram, and K. Orgera. 2020. COVID-19 and workers at risk: Examining the long-term care workforce. Kaiser Family Foundation. https://www.kff.org/medicaid/issue-brief/covid-19-and-workers-at-risk-examining-the-long-term-care-workforce (accessed September 17, 2020).
Tsai, J., and M. Wilson. 2020. COVID-19: A potential public health problem for homeless populations. The Lancet Public Health 5(4). doi: 10.1016/S2468-2667(20)30053-0.
UN (United Nations). 2020a. UN Secretary-General’s policy brief: The impact of COVID-19 on children. New York: UN. https://unsdg.un.org/resources/policy-brief-impact-covid-19-children (accessed September 17, 2020).
UN. 2020b. UN Secretary-General’s policy brief: The impact of COVID-19 on older persons. New York: UN. https://www.un.org/development/desa/ageing/news/2020/05/covid-19-older-persons (accessed September 17, 2020).
UNWomen. 2020. UN Secretary-General’s policy brief: The impact of COVID-19 on women. New York: UNWomen. https://www.unwomen.org/en/digital-library/publications/2020/04/policy-brief-the-impact-of-covid-19-on-women (accessed September 17, 2020).
Uscher-Pines, L., J. Maurer, and K. M. Harris. 2011. Racial and ethnic disparities in uptake and location of vaccination for 2009-H1N1 and seasonal influenza. American Journal of Public Health 101(7):1252–1255. doi: 10.2105/AJPH.2011.300133.
Usher, K., N. Bhullar, J. Durkin, N. Gyamfi, and D. Jackson. 2020. Family violence and COVID 19: Increased vulnerability and reduced options for support. International Journal of Mental Health Nursing 29(4). doi: 10.1111/inm.12735.
Walker, A. T., P. J. Smith, and M. Kolasa. 2014. Reduction of racial/ethnic disparities in vaccination coverage, 1995–2011. MMWR Supplements 63(1):7–12.
Webb Hooper, M., A. M. Nápoles, and E. J. Pérez-Stable. 2020. COVID-19 and racial/ethnic disparities. JAMA 323(24):2466–2467. doi: 10.1001/jama.2020.8598.
WHO (World Health Organization). 2020a. Draft landscape of COVID-19 candidate vaccines. Geneva, Switzerland: WHO. https://www.who.int/publications/m/item/draft-landscape-of-covid-19-candidate-vaccines (accessed September 22, 2020).
WHO. 2020b. Health equity. Geneva, Switzerland: WHO. https://www.who.int/topics/health_equity/en (accessed September 15, 2020).
Williams, D. R. 2020. Stress was already killing black Americans. COVID-19 is making it worse. The Washington Post. https://www.washingtonpost.com/opinions/2020/05/13/stress-was-already-killing-black-americans-covid-19-is-making-it-worse (accessed September 21, 2020).
Williams, D. R., and L. A. Cooper. 2020. COVID-19 and health equity—a new kind of “herd immunity.” JAMA 323(24):2478–2480. doi: 10.1001/jama.2020.8051.
Wong, W. 2020. Presented at Equitable Allocation of COVID-19 Vaccine: Public Listening Session. Washington, DC: National Academies of Sciences, Engineering, and Medicine. https://www.nationalacademies.org/event/09-02-2020/public-listening-session-discussion-draft-of-the-preliminary-framework-for-equitable-allocation-of-covid-19-vaccine (accessed October 28, 2020).
Yancy, C. W. 2020. COVID-19 and African Americans. JAMA 323(19):1891–1892. doi: 10.1001/jama.2020.6548.




































