4
Reimagining Behavioral and Public Health Systems to Support Children and Families
In addition to reimagining economic systems, the workshop also centered discussions around creating improved, antiracist behavioral and public health systems following the pandemic to better support children and families. This chapter presents background in understanding the ways that racism impacts the health of children and families and explores potential systemic solutions. Short- and long-term goals for reimagining systems were also identified as stakeholders strive to move the field forward.
UNDERSTANDING THE IMPACT OF RACISM ON HEALTH
To create systems that are equitable and effective for all children, we need to understand the complex ways that racism impacts health, said Maxine Hayes, former state health officer for the Washington State Department of Health. She introduced the panel topic with a perspective that emphasized the narratives behind health disparities. Joseph Wright, senior vice president and chief medical officer of Capital Region Health within the University of Maryland Medical System, spoke on the importance of truth and reconciliation within organizations to move toward antiracist systems.
Highlighting Stories Behind Disparities
There is a dual pandemic happening in our nation—COVID-19 and racism—stated Hayes. The opportunities for reform as a result of the COVID-19 pandemic could result in a wiser and better nation, and Hayes challenged participants to envision a day in America where no health
inequities existed. Health and well-being, Hayes said, are essential requirements for a quality life, as well as a thriving economy. She referred to the World Health Organization’s definition of health1—not only the absence of disease and disability, but a state of positive physical, mental, social, and spiritual well-being—and asked where the responsibility lies for the health of the American citizen. She argued that all levels of government—federal, state, tribal, and local—are responsible for public health. She also emphasized the need to “put the public back in public health,” saying that public support is necessary to generate the political will to build capacity and implement public health work.
Connecting the Narratives
In 1988, the Institute of Medicine assigned three core functions to the future of public health: assessment, assurance, and process development (Institute of Medicine, 1988). While these functions are still relevant, Hayes acknowledged that more could be done in terms of assessment and connecting statistics to narratives that will move people to action.
The COVID-19 pandemic has pulled back the curtain on racial disparities within the health system. While we have utilized telemedicine to integrate clinical care, behavioral health, public health, and social and community services, Hayes said, we have failed in terms of health equity, and it should not be surprising that Black Americans face the worst COVID-19 outcomes due to generations of racism, sexism, poverty, and injustices of all kinds. This profile can also be applied to Native American and Hispanic American populations. The stories behind each COVID-19 death need to be told, Hayes said. The deaths are a reflection of a wide array of preventable chronic diseases and social determinants of health such as poverty, toxic unremitting stress, food insecurity, violence, trauma, police brutality, poor housing, toxic environments, and poor access to opportunities for meeting basic needs.
Because racism has been declared the number one determinant of racial/ethnic disparities in health, we should assume the presence of racism in public health system policies, practices, and norms, and it should be questioned, said Hayes. When practicing as a pediatrician and public health advocate, Hayes said that she always addresses complex problems by attending to the root cause first. The root cause can occur long before adulthood, she said, and even prior to conception. Taking an integrative, lifespan approach to addressing problems can ensure health and well-being from “womb to tomb.” To improve the health of the African
___________________
1 “Health is a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity” (World Health Organization, 1946).
American community, for example, the services provided at child-bearing ages should be examined, suggested Hayes. When babies are born, the priorities should include home visits, screening for poverty, assessing stress, mental health, relational health, and connecting families to community-based family support services.
In closing, Hayes presented pictures of posters made by her kindergarten-age granddaughter supporting the Black Lives Matter movement. She made a special note of one that read, “The future is watching” and challenged participants to have the moral courage to do the right thing today as it would impact future generations to come.
Confronting the Impacts of Toxic Stress on Children from Racism
Wright spoke to the influence of stress on child health and development and the components needed to move toward a more equitable health future. He began by providing an actionable definition of “equity”:
The fair treatment, access, opportunity, and advancement for all people, while striving to identify and eliminate barriers that have prevented the full participation of some groups. Improving equity involves increasing justice and fairness within the procedures and processes of institutions or systems, as well as in the distribution of resources. Tackling equity issues requires an understanding of the root causes of outcome disparities within our society (Coates Library, 2021).
A root cause of inequity is racism, which manifests itself in many forms: internalized, interpersonal, institutional, and structural, explained Wright. The effects of racism on children are toxic and the relationship between environment, ecology, biology, and child health development is incontrovertible, he argued.
Physiological Impacts of Childhood Stress
The impact of early toxic stress has neuroendocrine and neurobiological impacts that affect brain structure if not addressed, Wright stated. As Figure 4-1 shows, there is a cyclical relationship between early toxic stress and brain development. These impacts are known as physiological weathering and worsen over the life course. Wright explained that this happens as environmental exposures influence DNA methylation2 and the incorporation of epigenetic3 factors at the level of chromosomal replication.
___________________
2 DNA methylation is the main way gene activity is adjusted during life, especially during early development (Law and Jacobson, 2012).
3 Epigenetics is the study of gene expression (King, Stansfield, and Mulligan, 2006).
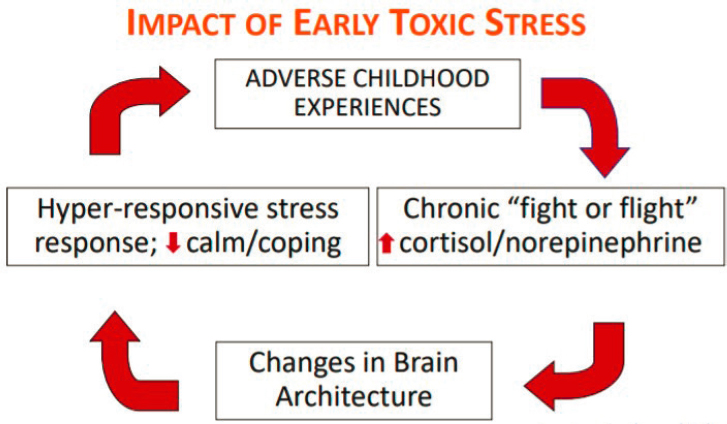
SOURCE: Joseph Wright presentation, September 14, 2020.
Specifically, the effects of exposure to early adversity spark neuronal signaling, which through the production of regulatory proteins and enzymatic impact on epigenetic markers can influence the turning-on or turning-off of gene expression. This results in inheritable and intergenerational impacts. From a life-course perspective, the causal factors of chronic disease result from childhood and preconception circumstances and are fueled by environmental and social stressors. These then manifest through physiologic mechanisms such as hypothalamic-pituitary-adrenal axis4 dysregulation, chronic inflammation, and altered immunity. He demonstrated the relationship between perceived racism and disease risk through a conceptual model (see Figure 4-2).
Creating an Equity Agenda
The American Academy of Pediatrics (AAP) has begun to create an equity agenda in the organized medicine5 field. Wright pointed to equity as the guiding principle but said an internal emphasis is also being placed on
___________________
4 The hypothalamic-pituitary-adrenal axis (HPA) is a neuroendocrine system essential for stress management (Kinlein, Wilson, and Karatsoreos, 2015).
5 Organized medicine consists of groups of physicians, including (1) practicing physicians, (2) young physicians, and (3) residents and medical students (Kahn, Baum, and Ellis, 2019).
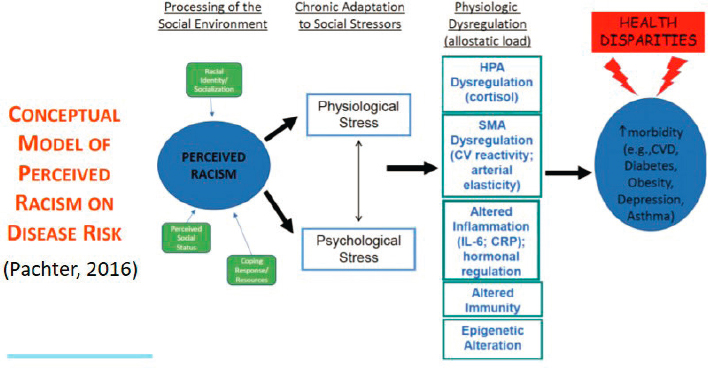
SOURCE: Joseph Wright presentation, September 14, 2020. Reprinted with permission from L.M. Pachter.
the organization to act as a societal player. For the AAP to address bias and discrimination in a way that is impactful to children and families, for example, there must be understanding, transparency, and accountability about the organization’s history as well as its present state. To continue moving the equity agenda forward, the organization has focused on building policy and workforce development, while emphasizing the critical aspects of diversity, inclusion, and advocacy.
Continuing in the vein of transparency, Wright reviewed the racist history of AAP, which denied membership to Dr. Roland B. Scott, the first African American to pass the pediatric board exam. A long-overdue apology was eventually issued by the organization for the racism Dr. Scott and his mentor faced as well as the inequities that other pediatricians have also endured. Since the apology, AAP has added specific language in its bylaws and constitution that clearly states that the organization does not discriminate on the basis of race, ethnicity, religion, sexual orientation, gender identification, or country of origin. Wright discussed AAP’s history to demonstrate the importance of acknowledging previous negative practices as part of reconciliation and the advancement toward an equitable health agenda.
EXPLORING SOLUTIONS
Discussions continued on how to move forward and restructure systems of care with possible solutions. Neal Horen, director of the Early
Childhood Division at Georgetown University, discussed the foundations of successful systems and the various factors that are needed to create an explicitly antiracist system. Michael Warren, associate administrator at the Maternal and Child Health Bureau, provided a framework for focused, collaborative efforts to improve child health outcomes. Finally, Riana Elyse Anderson, assistant professor of Health Behavior and Health Education at the University of Michigan’s School of Public Health, examined the relationship between basic and applied research and the way that these relationships provide opportunities for collaboration to restructure health systems.
Embedding Antiracism and Mental Health into Early Childhood Care
To create successful solutions to systemic racism, we must understand the systems that created them, said Horen. He highlighted this in his presentation and discussed the factors that must be taken into consideration when designing new systems of care so that they address racism in more direct ways. Horen described the fundamental components that he views as essential for a successful system of care: groundwork, labor force, infrastructure, and sustainability.
The framework includes a core system of care values, cultural awareness, interagency collaboration, and the provision of individualized services and support in existing settings. Horen acknowledged that while these were once viewed as strengths of the system, more is needed if a framework is to be successfully applied to realistic scenarios. The model does not explicitly address racism, disparities, equity, or inclusion, for example. Horen pointed out that it is necessary to address these factors directly instead of merely implying them through the inclusion of cultural awareness. Another point of contention is the provision of services and support in natural settings. Once thought to be a successful approach, Horen stated that it is neither sufficient nor successful when applied to real life situations.
To develop systems that directly address racism, an intersectional lens must be applied to strategic planning, implementation, workforce development, and financing, Horen argued. He posed the question: Who are we building systems for, and how are they a part of making those decisions? Using an intersectional lens as an element of the design template, systems can be developed to be directly antiracist, said Horen. To advance the existing landscape, it needs to be reworked through evidence-based practices for promotion and prevention, choosing the appropriate interventions, direct and indirect funding, workforce, partnerships, and existing infrastructure. Leaders designing and implementing interventions must ensure that interventions (1) reach their intended audiences, (2) are implemented effectively by a highly competent workforce, (3) are sustainable, and (4) address disparities, equity, and inclusion throughout the design. To reach these goals,
leaders must be transparent, aware of where others are in their journey, and willing to address systemic racism.
A New Paradigm for Improving Maternal and Child Health at the National Level
Warren began by highlighting the recent 85th anniversary of the signing of Title V under the Social Security Act, which made Title V maternal and child health services block grants available to the states. These grants have served as a foundation of the U.S. public health system for mothers, children, and families and are often used for essential public health infrastructure, improving access to care, and direct services in preventative and primary care. In fiscal year 2018, the block grant reached 99 percent of all infants, 91 percent of pregnant women, and 55 percent of children, including children with special health care needs (Health Resources and Services Administration, 2020).
Accelerating Upstream Together
Despite the successes of Title V in the past 85 years, there are still opportunities for improvement. Warren explained that the Maternal and Child Health Bureau is using the Accelerate Upstream Together Framework to guide the efforts to improve maternal and child health over the next 15 years leading up to Title V’s 100th anniversary.
The “accelerate” aspect of the framework encourages a faster rate of progress. Warren presented a systems-based example regarding the medical home approach to pediatric and primary care. The term “medical home” originated as a concept of a central place where records were stored for children with special health care needs and has since grown to incorporate a system of care with multiple components: continuous, comprehensive, coordinated, culturally appropriate, accessible care. The most recent national survey of children’s health reported that only 48 percent of all children and 43 percent of children and youth with special health care needs were receiving care in a medical home (Health Resources and Services Administration, 2020). Warren continued with an outcomes-based example on infant mortality, saying that while the overall rate of infant mortality in the past 30 years has been cut in half, the improvements have not been equal across populations, as noted previously. The infant mortality rate for Black infants in 2017 is equal to the infant mortality rate of White infants in 1980, a 37-year delay in achieving the same survival rate. The data on medical home care and infant mortality rates exemplifies the need for an accelerated change of pace, he stated.
Second, to increase the pace of change, we must think “upstream,” Warren said. This approach focuses on prevention to keep negative
outcomes from happening in the first place. Clinical care is often the center of the conversation, but as Warren points out, clinical care only accounts for about 10 to 20 percent of a person’s overall health and well-being. This means the conversation needs to be expanded to think more broadly about other determinants of health: behavioral patterns, social circumstances, community factors, and policy. A life-course approach is also needed because early experiences exert such powerful influence on trajectories well into adulthood and can even influence future generations, Warren stated.
As Hayes noted previously, preconception and the mother’s overall health must be factored into the approach of addressing infant mortality. This approach must begin in early childhood and emphasizes the need for a comprehensive public health systems approach. The three core functions of public health services—assessment, assurance, and policy development—must be used beyond clinical care to think broadly about all partners that need to be incorporated to improve population health outcomes.
The final facet of the framework Warren discussed is “together.” This reminds us that children’s health and well-being outcomes cannot be thought of in isolation, he explained. He highlighted the socio-ecological model, which embodies various levels of influence when it comes to child outcomes and places children and families at the forefront of discussions and initiatives. He pointed out that improvement efforts cannot be carried out in isolation. Partners at every level—local, state, and federal—must work together toward progress.
Racial Socialization and Capitalizing on Momentum
Anderson presented systemic reform solutions to address racial discrimination. She posed a question to participants to set the stage for reimagining a system of care through behavioral and public health approaches: Are we aiming to habituate or innovate?
Racial discrimination is associated with and responsible for a myriad of negative outcomes in children, she explained. These include but are not limited to psychological well-being, insulin resistance, posttraumatic stress symptoms, alcohol consumption, and poor academic engagement. To solve the systemic problems that perpetuate racism in our society, we need systemic solutions, Anderson said. While barriers exist to implementing large-scale, systemic solutions such as lack of time, money, resources, and expertise, the most serious barrier is perhaps the lack of empathy. A shift in perspective and a challenge to the status quo is needed to truly address the system of oppression that is in place against Black people in America, she argued.
Instead of simply dwelling on all of the ways Black Americans are doing poorly due to structural racism and systems, Anderson suggested flipping
the framing to think more about interpersonal solutions and systems to understand what Black families and communities are doing well, the cultural strengths being used, and what can be learned from them. With empathy for Black people and support at an all-time high, she offered a solution for “expediting clinical trials for the virus of racism.”
Reflecting a statement made by David Williams, Anderson pointed out that the COVID-19 pandemic and robust support for the Black Lives Matter movement have created an opportune moment for dismantling systemic racism. She shared a model she created in collaboration with Howard Stevenson, director of the Racial Empowerment Collaborative at the University of Pennsylvania: the Racial Encounter Coping Appraisal and Socialization Theory (see Figure 4-3) (Anderson and Stevenson, 2019). It combines common stress and coping models to create a model that is specific to racism.
To further the application of the RECAST model, Anderson shared the Embrace, Managing, and Bonding through Race program, which can be applied to identify specific stressor targets, program targets, and program outcomes (see Figure 4-4). She highlighted a scene from the movie “Black Panther” as an analogy, saying that she would love to see all of the negative discrimination and kinetic energy that is thrown at Black children be taken in and capitalized on as they engage in interpersonal and systemic buffering before bringing it back to the system to enact positive change.
Moving forward, racism-based interventions could benefit from more support on various levels. Anderson advocated for more funding in Phase II and Phase III clinical trials, going beyond just basic research about how racism and discrimination negatively affect children. She also called for a mentorship model as an avenue of support and communication for those working toward solutions at different points in their careers. In addition to

SOURCE: Anderson and Stevenson (2019).
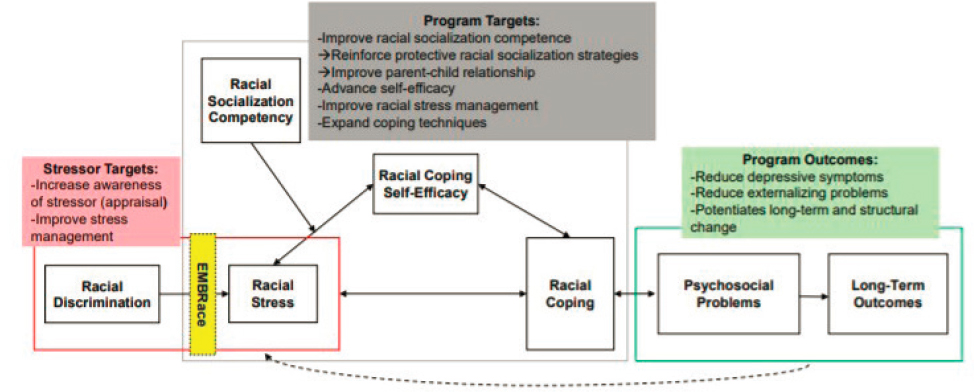
SOURCE: Anderson, McKenny, and Stevenson (2018).
connecting those at different points in their careers, Anderson said, there is a need to build connections among those working within the different stages of research to increase communication and increase awareness of not only where we are now but of where we want to be. This can be done by incentivizing connections between basic and applied researchers. All of these interventions are pertinent to the current COVID-19 pandemic and the fissures it has created in our society, she concluded.
ENSURING EQUITY IN A NEW SYSTEM
Harolyn Belcher, chief diversity officer and director for the Office of Health, Equity, Inclusion, and Diversity at Johns Hopkins University, led the panel in a discussion based on questions posed by workshop participants. The first question asked the panelists to respond to why the United States has not been able to provide free health care in the way that has been done in Canada. Warren replied by saying that while access to health care is an important piece of a child’s overall health and well-being, it is only one factor. Hayes reinforced the idea that health is more than just health care. The social determinants outside of clinical care have a significant impact on one’s health, and the narrative needs to change to be inclusive of all influential factors, she concluded.
Continuing the discussion, a participant pointed to a 2018 study that showed medical homes may not be as effective for Black and Hispanic families (Guerrero, Zhou, and Chang, 2018) and inquired about strategies to change this. In response, Warren emphasized the importance of incorporating equity into measurement systems to analyze outcomes between populations. Additionally, medical home data must be broken down to reveal the disparities that need to be addressed.
The discussion shifted to exploring how community strength could be integrated into research questions. To bridge this gap, there must be a shift in perspective from integrating “them” to integrating “us,” said Anderson. She said her choice to live in Detroit instead of closer to the University of Michigan is rooted in this concept of integrating herself more fully into the community where she centers her work. This allows her to be more aware of the unique characteristics and strengths of the community.
Wright concluded by discussing the future path of AAP. While the organization has been on the path of truth and reconciliation for a while, he said, it still has a lot of work to do. The current efforts to validate and codify the wrongdoings of the organization’s past is a big step but still leaves room for deliberate and intentional efforts regarding diversity and inclusion in the leadership ranks.
Operationalizing Reimagined Antiracist Behavioral and Public Health Systems
The six small groups reconvened and reported out on ways to restructure the system to move toward antiracist behavioral and public health systems. A summary of themes from the discussions is below.
Policy
A few of the groups highlighted a need for policy change to create a system that ensures sustainable antiracist efforts. Matt Lyons, director of policy and research at the American Public Human Services Association, reported that his group discussed the need for an outward-facing plan at every level of care from families and children to leadership. This type of outward policy approach would ensure accountability and increase transparency, he said. Suzanne Le Menestrel, director of the Forum for Children’s Well-Being at the National Academies of Sciences, Engineering, and Medicine, stated that policy makers need to take an antiracist approach to creating decision-making frameworks to ensure that all decisions are addressed in this way.
Workforce
Lyons also discussed the various ways in which the workforce could be reformed to create antiracist work environments and outcomes. He proposed possible interventions such as providing antiracism training to those who work with young children, specifically early childhood educators. Another approach would be to recruit diverse individuals to fill positions in the behavioral and public health workforce. By diversifying the workforce, he said, the communities they are serving would be better represented.
Community Level
There was also discussion on reforms that could take place at the community level. Lyon’s group discussed community development investments such as infrastructure being structured into equitable public health investments. They also suggested incorporating family voices and the lived experiences of individuals into reform conversations to increase the trust between communities and the care systems. A way to do this would be through a greater emphasis on community health workers who are integrated into the communities they are serving. Carlos Santos, associate professor in the Luskin School of Public Affairs at the University of California, Los Angeles, also stressed the importance of community health workers and their potential contributions to a diversified health care workforce.
Funding
Increasing funding of behavioral and public health systems to create new programs and expand existing ones was a common theme among the groups. Lyon’s group called for more funding for prevention work specifically within the mental health system. His group also discussed the need for a restructured incentive system to address social determinants of health. This would bring more attention to long-term issues, he said. Reflecting on the importance of Title V as discussed in an earlier presentation, Deborah Klein Walker, adjunct professor at the Boston University of Public Health and Tufts University School of Medicine, reported that her group called for expanded funding, noting that Title V is currently funded at less than $1 billion. Expanding the budget to $1.5 billion could create more opportunity to include family voices and more funding at the community level. Walker’s group agreed that health care system funding needs to be sufficient to support a system that is both accessible and affordable. As Le Menestrel said, “A child’s well-being should not be tied to whether their parent or caregiver is employed.”












