1
Introduction
The U.S. Social Security Administration (SSA) provides financial assistance to people with disabilities through the Social Security Disability Insurance (SSDI) (Title II of the Social Security Act) and Supplemental Security Income (SSI) (Title XVI of the Social Security Act) programs. The SSDI program, established in 1956, provides benefits to eligible adults with disabilities who have paid into the Disability Insurance Trust Fund, as well as to certain family members. The SSI program, created in 1972, is a means-tested program based on income and financial resources that pays benefits to eligible adults and children with disabilities, individuals who are blind, and adults aged 65 and older. In December 2020, approximately 9.54 million individuals were receiving SSDI benefits as “disabled workers” (85.5 percent), “disabled widow(er)s” (2.5 percent), or “disabled adult children” (12.1 percent), and about 6.8 million individuals classified as blind or disabled were receiving SSI benefits (SSA, 2021a, pp. 11, 21; 2021b).
CONTEXT FOR THIS STUDY
To receive SSDI or SSI disability benefits, an individual must meet the statutory definition of disability. For adults, disability is defined as an “inability to engage in any substantial gainful activity [SGA] by reason of any medically determinable physical or mental impairment which can be expected to result in death or which has lasted or can be expected to last
for a continuous period of not less than 12 months.”1 Children under the age of 18 who are not engaged in SGA are considered disabled if they have “a medically determinable physical or mental impairment or combination of impairments that causes marked and severe functional limitations, and that can be expected to cause death or that has lasted or can be expected to last for a continuous period of not less than 12 months.”2
SSA uses a five-step process based on medical–vocational evaluations to determine whether an adult meets the definition of disability. After SSA determines an applicant’s administrative eligibility and the presence of a medical impairment of sufficient duration and severity in steps 1 and 2 of this process, it assesses, in step 3, whether the applicant’s impairment meets or medically equals the criteria listed for a condition in SSA’s Listing of Impairments-Adult Listings (listings) (SSA, n.d.-a). The Adult Listings are organized by major body system and describe impairments that SSA considers to be sufficiently severe to prevent an applicant from performing any gainful activity, regardless of age, education, or work experience. Step 3 is used as a “screen-in” step. If an impairment is severe but does not meet or medically equal any listing, SSA assesses in step 4 whether the applicant’s physical or mental residual functional capacity (RFC) allows the person to perform past relevant work. Applicants who are able to perform past relevant work are denied benefits, while those who are unable to do so proceed to step 5. At step 5, SSA considers, in combination with the applicant’s RFC, such vocational factors as age, education, and work experience, including transferable skills, in determining whether the individual can perform other work in the national economy. Applicants determined to be unable to adjust to performing other work are allowed benefits, while those determined able to adjust are denied.
Disability determinations in children follow a three-step sequential evaluation process. After determining administrative eligibility and the presence of a medical impairment of sufficient duration and severity, SSA assesses in step 3 whether the impairment(s) meets, medically equals (is equivalent in severity to), or functionally equals (i.e., the impairment[s] results in functional limitations equivalent in severity to) the criteria in SSA’s Child Listings (SSA, n.d.-b).3 If a child’s impairment or combination of impairments “does not meet or medically equal any listing, [SSA] will
___________________
1 42 U.S.C. 423(d)(1); 42 U.S.C. 416(i); see also 20 CFR 404.1505; 20 CFR 416.905; “Substantial gainful activity” is work activity involving significant physical or mental activities for pay or profit (20 CFR 416.972). Someone earning more than a specified monthly amount ($1,310 after deduction of impairment-related work expenses for a nonblind individual in 2021) ordinarily is considered to be engaging in SGA (SSA, 2022).
2 20 CFR 416.906; see also 42 U.S.C. 1382(c).
3 20 CFR 416.926; 20 CFR 416.926a.
decide whether it results in limitations that functionally equal the listings.”4 Functional equivalence refers to functionally equaling the listings: SSA’s technique for determining functional equivalence is a “whole child” approach that “accounts for all of the effects of a child’s impairments singly and in combination—the interactive and cumulative effects of the impairments—because it starts with a consideration of actual functioning in all settings” (SSA, 2009).
For both adults and children, disability claims related to heritable disorders of connective tissue (HDCTs) are evaluated under listings for the affected body systems. With the exception of Marfan syndrome (MFS), which is identified under the cardiovascular listing 4.10 (aneurysm of aorta or major branches), HDCTs are not specified in the listings.
STUDY CHARGE AND SCOPE
In 2020, SSA requested that the Health and Medicine Division of the National Academies of Sciences, Engineering, and Medicine convene a committee of relevant experts to review the current state of medical knowledge and practice regarding selected HDCTs. The Committee on Selected Heritable Disorders of Connective Tissue was charged with determining the latest standards of care, technology for understanding disease processes, treatment modalities, and science demonstrating the effect of these disorders on the health and functional capacity of adults and children (see Box 1-1 for the committee’s statement of task). The 16-member committee comprised experts in general medicine, immunology, orthopedics, neurology, cardiology, hematology, ophthalmology, psychiatry, rehabilitation, pain management, and genetics.
STUDY APPROACH
Definition of Disability
The concept of disability has evolved over the past several decades from a medical to a biopsychosocial model. In the medical model, disability is viewed as a feature of a person that is caused by injury, disease, or other health condition and managed through medical treatment or modification of an individual’s behavior (IOM, 1991; Kaplan, 2000; WHO, 2001, 2002). In contrast, the biopsychosocial model, exemplified by the World Health Organization’s International Classification of Functioning, Disability and Health (ICF), portrays disability as “the interaction between an individual (with a health condition) and that individual’s contextual factors
___________________
4 20 CFR 416.926a.
(environmental and personal factors)” (WHO, 2001). The ICF model recognizes functioning in three domains (middle tier of Figure 1-1): (1) body functions and structures, which encompass physiological functions of the body, including psychological functions, as well as the functioning of body structures (e.g., movement of limbs, cardiac function); (2) activities, which are actions or tasks (e.g., running, problem solving); and (3) participation, which is the performance of tasks in a societal context (e.g., participation in school or organized sports). The ICF model refers to deficits in body functions and structures as impairments, deficits in completing activities as limitations, and reductions in participation as restrictions. It should be noted that such accommodations as assistive technologies and environmental modifications are environmental contextual factors that act on the ICF domains to enhance an individual’s activity and participation.
As noted above, SSA’s definition of disability in adults is “inability to engage in any SGA by reason of any medically determinable physical or mental impairment which can be expected to result in death or which has lasted or can be expected to last for a continuous period of not less than 12 months.”5 SGA is work activity that “involves doing significant and productive physical or mental duties” or activity that “is done (or intended) for
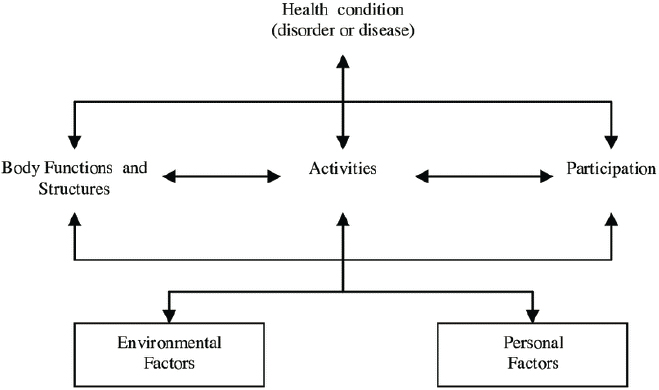
SOURCE: WHO, 2001. Reproduced from International Classification of Functioning, Disability and Health, World Health Organization, Introduction: 5. Model of Functioning and Disability, p. 18, copyright 2001.
___________________
5 42 U.S.C. 423(d)(1); 42 U.S.C. 416(i); see also 20 CFR 404.1505; 20 CFR 416.905.
pay or profit,” regardless of whether a profit is realized.6 In the SSA context, “disability” in adults refers to work disability—an inability to participate in work “in an ordinary work setting, on a regular and continuing basis, and for 8 hours per day, 5 days per week, or an equivalent work schedule” (SSA, 2021c).
This report focuses on those physical; vision, hearing, and speech; and mental activities the committee determined to be most relevant to SSA based on the information SSA collects about applicants and the information the U.S. Bureau of Labor Statistics collects about the physical and mental demands of jobs for inclusion in the Occupational Information System. SSA classifies jobs as sedentary, light, medium, heavy, and very heavy based on the level of physical exertion required for the work.7 SSA distinguishes between two types of limitations: exertional and nonexertional. Exertional limitations relate to the strength demands of jobs (sitting, standing, walking, lifting, carrying, pushing, and pulling) and are classified by level (sedentary, light, medium, heavy, and very heavy). All other limitations (e.g., mental limitations, sensory limitations, environmental intolerance) are considered nonexertional (SSA, 1999).
SSA incorporates function into its definition of disability for children, stating that a child’s qualifying impairment(s) must cause “marked and severe functional limitations.”8 SSA considers a number of factors when evaluating the effects of an impairment or combination of impairments on a child’s functioning.9 These factors include but are not limited to
- how well the child can initiate and sustain activities, how much extra help he or she needs, and the effects of structured or supportive settings (see § 416.924a(b)(5));
- how the child functions in school (see § 416.924a(b)(7)); and
- the effects of the child’s medications or other treatment (see § 416.924a(b)(9)).10
SSA considers “how appropriately, effectively, and independently” the child performs their activities (everything they do at home, at school, and in the community) “compared to the performance of other children [their] age who do not have impairments.”11 In particular, SSA considers functioning in six domains:
___________________
6 20 CFR 404.1510; 20 CFR 404.1572.
7 20 CFR 416.967.
8 20 CFR 416.906.
9 20 CFR 416.924a.
10 See 20 CFR 416.926a.
11 20 CFR 416.926a.
- acquiring and using information,
- attending and completing tasks,
- interacting and relating with others,
- moving about and manipulating objects,
- caring for [oneself], and
- health and physical well-being.12
Selection of Heritable Disorders of Connective Tissue
HDCTs are a heterogeneous group of inherited disorders that affect the body’s connective tissue. As directed in its statement of task, the committee addressed in particular the Ehlers-Danlos syndromes (EDS) and MFS, two of the most prevalent HDCTs. The EDS are a group of 13 disorders characterized by joint hypermobility and tissue fragility (Malfait et al., 2017). MFS is an autosomal-dominant disorder that affects multiple organ systems, with cardiovascular, ocular, and skeletal features being most prominent (Loeys et al., 2010). In addition, the committee identified for inclusion in this report hypermobility spectrum disorders (HSD) and several other hereditary aortopathies (Loeys-Dietz syndrome, congenital contractural arachnodactyly [also known as Beals-Hecht syndrome], and Shprintzen-Goldberg syndrome) because of the features they share with hypermobile EDS (hEDS, the most prevalent EDS type) and MFS, respectively.
Terminology
Secondary Impairments
The committee was tasked with describing, to the extent possible, secondary impairments that result from the HDCTs or their treatments. Because there is not always a known or clear causal link between the disorder and all of its manifestations, the committee understands “secondary impairments” to mean physical and mental manifestations (medical diagnoses, syndromes, or comorbid and other health conditions) that are either associated with or may result from an HDCT. Many of these are not specific to HDCTs and can also occur in other individuals. Use of this term thus defined does not mean that any of the physical or mental manifestations seen in individuals with HDCTs are not core elements of the disorders. Rather, the primary impairment is the underlying genetic disorder (e.g., EDS, MFS), and the secondary impairments encompass all of the physical and mental manifestations of that disorder.
___________________
12 20 CFR 416.926a.
Because connective tissues are found throughout the body, HDCTs manifest in multiple body systems. The symptoms and secondary impairments associated with HDCTs vary widely, as do the severity of the manifestations experienced by different individuals and the timing of their appearance. The committee considers the number, types, and severity of the physical and mental secondary impairments experienced by individuals—which may develop and vary in severity (wax and wane) over time—to be of particular importance with regard to the functional implications of HDCTs.
Treatment and Management
The committee was tasked with addressing several issues related to the treatment of HDCTs. For the purposes of this report, the committee distinguishes between “treatment” and “management”: whereas treatment focuses on curing or mitigating a specific disease, in this case an HDCT, management focuses on caring for the person as a whole, which requires a multidisciplinary team and extends throughout the life course. Although no curative treatments currently are available for EDS and MFS, these disorders can be managed through surveillance and treatment of associated secondary impairments.
Severity
The committee was tasked with describing the severity of HDCTs. For the purposes of this report, the terms “severe” and “severity” are used as they typically would be in clinical or medical care settings. When the terms reflect SSA’s program definition (i.e., an impairment of such severity as to be the basis of a finding of an inability to engage in any SGA), their usage is specified as such.
Information Gathering
The committee conducted an extensive review of the literature pertaining to heritable disorders of connective tissue and work-related functioning. This review began with a search of online databases for U.S. and international English- and Spanish-language literature from 2006 through 2021. This search encompassed PubMed and Scopus, as well as websites including those of the International Consortium on Ehlers-Danlos Syndromes & Hypermobility Spectrum Disorders, the EDS & HSD Community Coalition (formerly “the EDS Comorbidity Coalition”), The Ehlers-Danlos Society, The Marfan Foundation, and SSA. Committee members and project staff identified additional salient literature and information using traditional
academic research methods and online searches throughout the course of the study.
The committee used a variety of resources to supplement its review of the literature. Meeting virtually six times, the committee held two public workshops to hear from invited experts in areas pertinent to its charge (see Appendix A). Speakers at the workshops included experts in HDCT-associated gastrointestinal conditions, mental health conditions, and orthostatic intolerance. Additionally, the committee participated in a panel discussion with patient advocates and commissioned a paper on the functional impact of orthostatic intolerance in EDS (Appendix B). The committee’s work was further informed by several previous reports of the National Academies: Cardiovascular Disability: Updating the Social Security Listings (IOM, 2010), The Promise of Assistive Technology to Enhance Activity and Work Participation (NASEM, 2017), Functional Assessment for Adults with Disabilities (NASEM, 2019), and Childhood Cancer and Functional Impacts across the Care Continuum (NASEM, 2021).
REPORT ORGANIZATION
Chapter 2 provides an overview of the history, etiology, diagnosis, and management considerations common to all HDCTs. Chapter 3 addresses the diagnosis and management of MFS and several other hereditary aortopathies and the secondary impairments associated with these disorders. Chapter 4 does the same for EDS and HSD. Chapter 5 includes more information on physical and mental secondary impairments associated with the selected HDCTs and their potential effects on functioning, with particular focus on activities of interest to SSA (e.g., for adults, work-related activities and demands, and for children, other activities). Chapter 6 contains the report’s overall conclusions.
REFERENCES
IOM (Institute of Medicine). 1991. Disability in America: Toward a national agenda for prevention. Edited by A. M. Pope and A. R. Tarlov. Washington, DC: The National Academies Press. https://doi.org/10.17226/1579.
IOM. 2010. Cardiovascular disability: Updating the Social Security listings. Washington, DC: The National Academies Press. https://doi.org/10.17226/12940.
Kaplan, D. 2000. The definition of disability: Perspective of the disability community. Journal of Health Care Law & Policy 3(2). https://digitalcommons.law.umaryland.edu/jhclp/vol3/iss2/5/.
Loeys, B. L., H. C. Dietz, A. C. Braverman, B. L. Callewaert, J. De Backer, R. B. Devereux, Y. Hilhorst-Hofstee, G. Jondeau, L. Faivre, D. M. Milewicz, R. E. Pyeritz, P. D. Sponseller, P. Wordsworth, and A. M. De Paepe. 2010. The revised Ghent nosology for the Marfan syndrome. Journal of Medical Genetics 47(7):476-485. https://doi.org/10.1136/jmg.2009.072785.
Malfait, F., C. Francomano, P. Byers, J. Belmont, B. Berglund, J. Black, L. Bloom, J. M. Bowen, A. F. Brady, N. P. Burrows, M. Castori, H. Cohen, M. Colombi, S. Demirdas, J. De Backer, A. De Paepe, S. Fournel-Gigleux, M. Frank, N. Ghali, C. Giunta, R. Grahame, A. Hakim, X. Jeunemaitre, D. Johnson, B. Juul-Kristensen, I. Kapferer-Seebacher, H. Kazkaz, T. Kosho, M. E. Lavallee, H. Levy, R. Mendoza-Londono, M. Pepin, F. M. Pope, E. Reinstein, L. Robert, M. Rohrbach, L. Sanders, G. J. Sobey, T. Van Damme, A. Vandersteen, C. van Mourik, N. Voermans, N. Wheeldon, J. Zschocke, and B. Tinkle. 2017. The 2017 international classification of the Ehlers-Danlos syndromes. American Journal of Medical Genetics Part C: Seminars in Medical Genetics 175(1):8-26. https://doi.org/10.1002/ajmg.c.31552.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. The promise of assistive technology to enhance activity and work participation. Edited by A. M. Jette, C. M. Spicer, and J. L. Flaubert. Washington, DC: The National Academies Press. https://doi.org/10.17226/24740.
NASEM. 2019. Functional assessment for adults with disabilities. Edited by P. A. Volberding, C. M. Spicer, and J. L. Flaubert. Washington, DC: The National Academies Press. https://doi.org/10.17226/25376.
NASEM. 2021. Childhood cancer and functional impacts across the care continuum. Edited by P. A. Volberding, C. M. Spicer, T. Cartaxo, and L. Aiuppa. Washington, DC: The National Academies Press. https://doi.org/10.17226/25944.
SSA (U.S. Social Security Administration). 1999. DI 24515.063 Exertional and nonexertional limitations. http://policy.ssa.gov/poms.nsf/lnx/0424515063 (accessed January 24, 2022).
SSA. 2009. SSR 09-1p: Title XVI: Determining childhood disability under the functional equivalence rule—The “whole child” approach. https://www.ssa.gov/OP_Home/rulings/ssi/02/SSR2009-01-ssi-02.html#fn4 (accessed May 26, 2022).
SSA. 2021a. Annual statistical report on the Social Security Disability Insurance program, 2020. SSA Publication No. 13-11826. Washington, DC: SSA. https://www.ssa.gov/policy/docs/statcomps/di_asr/index.html (accessed May 23, 2022).
SSA. 2021b. Annual statistical supplement, 2021—Supplemental Security Income: Summary (7.A). https://www.ssa.gov/policy/docs/statcomps/supplement/2021/7a.html (accessed January 26, 2022).
SSA. 2021c. DI 24510.057 Sustainability and the residual functional capacity (RFC) assessment. http://policy.ssa.gov/poms.nsf/lnx/0424510057 (accessed January 26, 2022).
SSA. 2022. Substantial gainful activity. https://www.ssa.gov/OACT/COLA/sga.html (accessed January 26, 2022).
SSA. n.d.-a. Listing of impairments—Adult listings (Part A). https://www.ssa.gov/disability/professionals/bluebook/AdultListings.htm (accessed January 26, 2022).
SSA. n.d.-b. Listing of impairments—Childhood listings (Part B). https://www.ssa.gov/disability/professionals/bluebook/ChildhoodListings.htm (accessed January 26, 2022).
WHO (World Health Organization). 2001. International classification of functioning, disability and health. Geneva, Switzerland: WHO. https://apps.who.int/iris/handle/10665/42407 (accessed July 22, 2022).
WHO. 2002. Towards a common language for functioning, disability and health: ICF. Geneva, Switzerland: WHO. https://www.who.int/publications/m/item/icf-beginner-s-guide-towards-a-common-language-for-functioning-disability-and-health (accessed July 22, 2022).












