Proceedings of a Workshop
| IN BRIEF | |
|
February 2022 |
Providing Health Literate Virtual Health Services
Proceedings of a Workshop—in Brief
The COVID-19 pandemic led to a dramatic increase in health services being conducted by telephone or video. While this change may have important benefits to patients, such as increasing access to care, it may also pose challenges for those with low health literacy. To explore the challenges that virtual or telehealth services may pose to those with low health literacy, as well as the opportunities for increasing access to care, the National Academies of Sciences, Engineering, and Medicine’s Roundtable on Health Literacy held a virtual public workshop on September 23, 2021. The workshop examined the experiences that individuals with low health literacy have with using virtual or telehealth services; best practices for ensuring that individuals with low health literacy are able to obtain, process, understand, and act upon health information and services provided virtually or through telehealth; and health system and provider strategies for ensuring the delivery of health literate virtual health services that benefit patients and practitioners alike.
The following sections of the Proceedings of a Workshop—in Brief present summaries of each of the workshop’s three presentations and the panel discussion that followed them. The planning committee’s role was limited to planning the workshop, and the Proceedings of a Workshop—in Brief was prepared by the workshop rapporteurs as a factual summary of what occurred at the workshop. Statements, recommendations, and opinions expressed are those of individual presenters and participants and are not necessarily endorsed or verified by the National Academies. They should not be construed as reflecting any group consensus.
To begin the webinar, Lawrence Smith, executive vice president and physician in chief at Northwell Health and dean of the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell, welcomed attendees. He then introduced the first moderator of the day, Olayinka Shiyanbola, associate professor at the University of Wisconsin-Madison School of Pharmacy.
THE PROMISE AND CHALLENGES OF PROVIDING HEALTH LITERATE VIRTUAL HEALTH SERVICES
Shiyanbola introduced the first presenter of the day, Marina Serper, assistant professor at the University of Pennsylvania Perelman School of Medicine. Serper presented on what her research team has learned about telehealth use among older adults and what the Penn Medicine health system is doing to overcome some health literacy challenges.
Serper began her presentation by reviewing the changes in the telehealth landscape during the COVID-19 pandemic. While telehealth had been growing gradually over the past decade, video-enabled telehealth exploded during the pandemic when shelter-in-place orders first went into effect in March 2020. At their peak, telehealth outpatient claims nationwide grew 78-fold from prepandemic levels, and they have since stabilized at 38-fold greater than before
![]()
the pandemic.1 Practices serving Medicare beneficiaries increased their offerings to older adults from 18 percent of visits prior to the pandemic to 64 percent during the pandemic (Koma et al., 2021). Serper noted, however, that not all Medicare beneficiaries possess the technology they need to access telehealth appointments, and the trends also reveal inequities in access. For example, fewer than half of Black and Hispanic Medicare beneficiaries say they own a computer, while Medicare beneficiaries who live in rural areas or who are 75 years or older are less likely than urban or younger Medicare beneficiaries to own a computer or smartphone (Koma et al., 2021).
Serper then shared information about her research, in which she and her collaborators have been able to examine the attitudes and beliefs of older adults during the COVID-19 pandemic and gain some idea about the uptake and acceptability of telehealth in this cohort (Bailey et al., 2020; Wolf et al., 2020). They did this by using five ongoing National Institutes of Health studies of kidney transplant recipients and older adults with chronic comorbidities that had collected detailed sociodemographic, psychosocial, and health literacy information. Serper shared a few key data about the sample of her add-on study:
- 673 adults
- Approximately half had limited health literacy (as measured by the Newest Vital Sign; Weiss et al., 2006)
- Nearly one-third of the study participants were Black
- 21.5 percent were Hispanic
- 11.3 percent had limited English proficiency
- 29.4 percent were living below the poverty level
Between December 2020 and March 2021, her study’s participants reported they had two to three telehealth visits during the previous 4 months. Analyses found that there was no difference in the number of visits by literacy status, age, English proficiency, race, ethnicity, or self-reported health. There were, however, notable differences in the participants’ use and perceptions of video telehealth, said Serper (Figure 1). Participants with low or marginal health literacy were less likely to have a primary care video visit or specialty care video visit, more likely to have difficulty recall
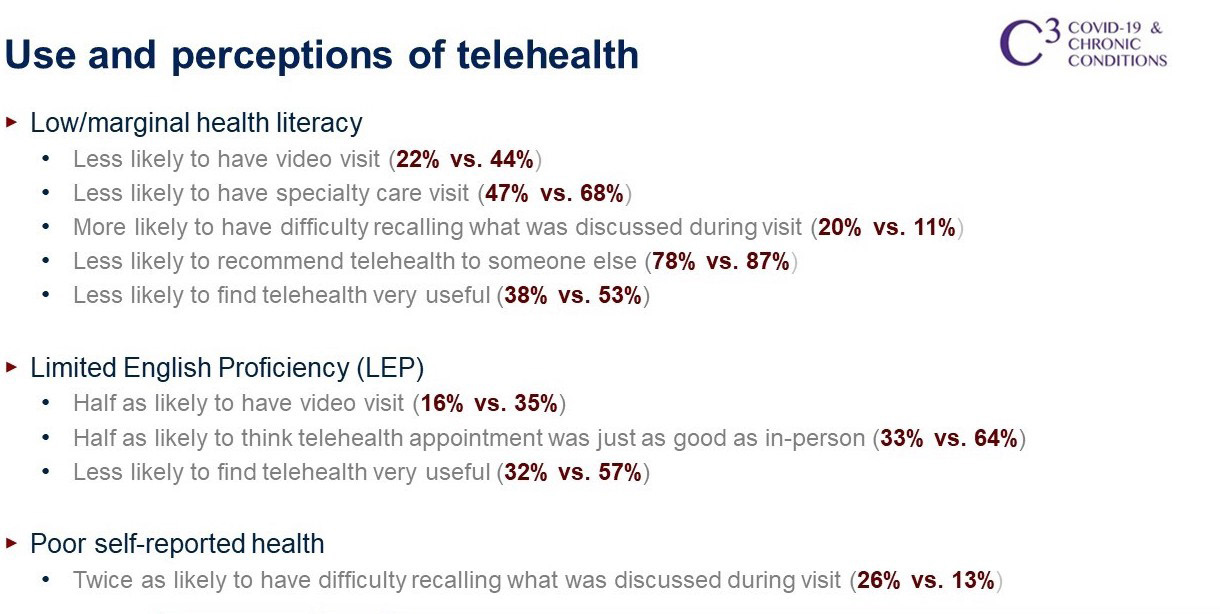
NOTE: C3 is an ongoing cohort study with several associated publications.
SOURCES: Workshop presentation by Serper on September 23, 2021; Bailey et al., 2020; Wolf et al., 2020.
___________________
1 Includes cardiology, dental/oral, dermatology, endocrinology, ENT medicine, gastroenterology, general medicine, general surgery, gynecology, hematology, infectious diseases, neonatal, nephrology, neurological medicine, neurosurgery, oncology, ophthalmology, orthopedic surgery, poisoning/drug tox./comp. of TX, psychiatry, pulmonary medicine, rheumatology, substance use disorder treatment, urology. Also includes only evaluation and management visits; excludes emergency department, hospital inpatient, and psychiatry inpatient claims; excludes certain low-volume specialties (see https://www.mckinsey.com/industries/healthcare-systemsand-services/our-insights/telehealth-a-quarter-trillion-dollar-post-covid-19-reality [accessed December 16, 2021]).
ing what they discussed during the visit, and less likely to find telehealth useful or recommend telehealth to someone else. Those with limited English proficiency were half as likely to have a video visit or to think a telehealth appointment was as good as an in-person visit, and they were less likely to find telehealth useful. In addition, individuals with poor self-reported health were twice as likely to have difficulty recalling what they discussed during their visit.
With those data as background, Serper discussed how her health system, Penn Medicine, adapted to this rapidly changing landscape, addressed some of the barriers to telehealth, and worked toward promoting equity in telehealth services. Serper explained that prior to the pandemic, Penn Medicine’s telehealth programs were “boutique,” in that specialty clinics such as genetics, neurology, and nephrology were the primary users of telehealth. In total, the health system, which serves 6.7 million patients, was conducting fewer than 100 telehealth visits a day using proprietary software on dedicated telemedicine workstations. “It was a complex workflow that only a few providers knew how to do,” said Serper, “and we were missing key features such as interpreter services and direct patient messaging about how to log into the visit.”
Once the pandemic hit and shelter-in-place orders went into effect, noted Serper, Penn Medicine had to figure out how to conduct 70 percent or more of its visits virtually, with some clinics at the height of the pandemic conducting 90 percent of their visits virtually. This rapid transition started by hiring a new telehealth vendor and deploying its BlueJeans telehealth platform systemwide over 1 weekend. Key to the rapid and successful rollout of this new system, said Serper, was Penn Medicine’s decade long investment in telehealth and the expertise housed in its Center for Connected Care and Center for Network Telemedicine. The new system included a telemedicine command center staffed by Penn Medicine’s electronic health record (EHR) transformation team and dozens of volunteer medical students to support both patients and clinicians.
Penn Medicine’s in-house staff also developed a wraparound telehealth platform to address workflow and user experience needs that the BlueJeans platform did not meet. The wraparound system, called Switchboard, integrates patient messaging with the EHR and its scheduling function. “This allowed us to automatically message the patient and the provider and conduct inpatient and outpatient visits more seamlessly without having a person call everybody and give them their specific video link,” explained Serper.
There are several ways that the system aims to simplify the process for patients. The automated function sends out a reminder email 3 days before a scheduled visit that includes a visit guide, eliminating the need for patients to log into a patient portal to learn how to connect to their telehealth visit. Ten minutes before the visit, the system sends out another reminder with a direct link to the appointment so the patient does not have to download software to access care. Serper noted that the system can automatically switch patients from an in-person to a telehealth visit should the need arise as the pandemic ebbs and flows. Building in language translation services was challenging, but the system now enables on-demand, two-way text translation for 65 languages. It can also access a live, third-party video interpreter when needed.
Penn Medicine polled over 500 of its providers to get their input on important principles for successful telemedicine visits. This feedback identified 14 principles, which are presented in Box 1.
Additionally, Serper explained that the gastroenterology and liver clinics surveyed their patients to gauge their perceptions of telemedicine during the first 4 weeks of using BlueJeans and Switchboard (see select results in Figure 2). They found that, in general, patients thought their visits were of high quality and that the technology was easy to use. However, she did highlight a few potential disparities among the findings. For example, Serper noted that a lower percentage of Black patients surveyed, compared to white patients, reported that the telehealth technology was easy to use (77 percent of Black respondents versus 82 percent of white respondents, P < 0.5 in bivariate comparisons); a lower percentage of patients who are over age 60 reported that a telehealth visit was as good or better than meeting face to face (61 percent of respondents over age 60, compared to 73 percent of respondents under age 60, P < 0.5 in bivariate comparisons). Younger patients and those individuals enrolled in Penn Medicine’s patient portal were more likely to report they had a high-quality visit, which she said was not surprising given that these individual were likely to be more comfortable using digital technology.
When asked for the top words or phrases that came to mind about telemedicine, patients almost uniformly expressed positive responses, which Serper attributed to patients being grateful they could access care and appreciative that the health system was able to pivot so quickly and efficiently from in-person to telehealth care.
Serper and her colleagues also surveyed the system’s practitioners to identify their biggest concerns after the first 4 weeks of making the switch to telehealth. The top issues in the minds of Penn Medicine’s practitioners were that their patients would not be accepting of telehealth, that there might be problems with the technology, that they could not conduct a physical exam, and that there might be workflow and scheduling issues. Though Penn Medicine has shifted many of its visits back to being in person, telehealth visits still average over 1,000 a day, with up to 2,000 on some days. Serper noted that the health system can scale its telehealth capabilities as needed.
She concluded her presentation by cautioning that the ways that health systems are currently operating telehealth programs may place some patients at risk of experiencing less than optimal telehealth visits, especially patients with low health literacy, low English proficiency, and multiple health issues, as well Black, Indigenous, and people of color (BIPOC) communities, and older individuals. Health systems and payers, said Serper, should operationalize telehealth best practices, engage patients and caregivers, make sure that integrated interpreter services are available,
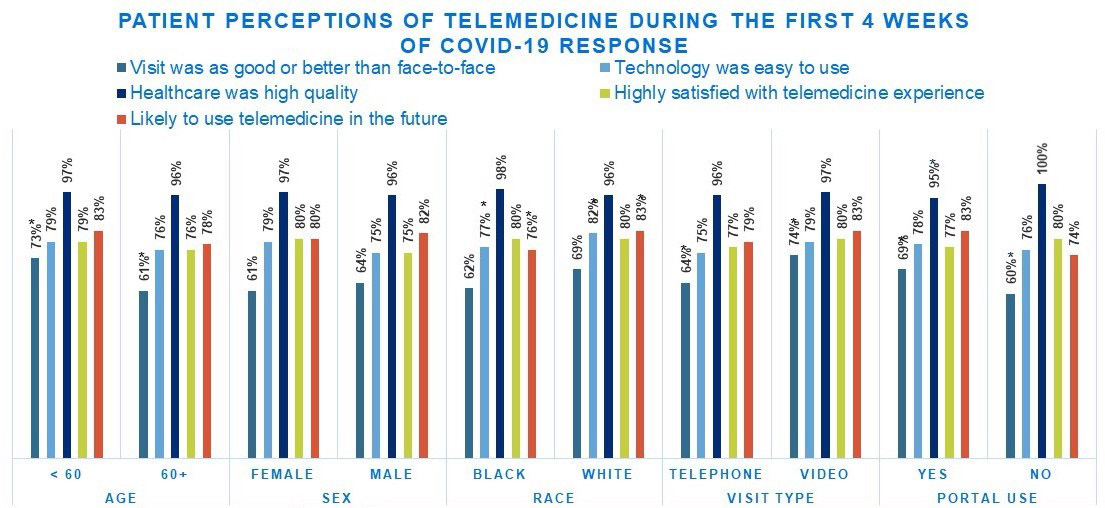
NOTES: Electronic health record data in an academic setting, over 4 weeks; N = 788. P < 0.05 in bivariate comparisons.
SOURCES: Workshop presentation by Serper on September 23, 2021; Serper et al., 2020.
simplify technology and workflows, offer training and support to patients and staff, and continuously monitor the quality of services to ensure access and equity in telehealth.
Session moderator Olayinka Shiyanbola, University of Wisconsin, Madison, asked Serper to comment as a provider on how she and her colleagues might benefit if health systems focused on health literacy in virtual services (Box 2). First, Serper replied, health systems should provide clear, health literate instructions for how to schedule and prepare for a visit. She suggested that she and other providers like herself should bear the responsibility of better helping patients reconcile medications and provide clearer electronic instructions at the end of the visit. For both virtual and in-person services, she suggested, patients should be provided with the written information they need without having to be responsible for recalling instructions. She noted that in her opinion, there is still a ways to go in terms of improving after-visit summaries or guides, and wondered how to ensure that the things discussed in the visit are imparted to the patient and incorporated in the EHR. Serper said, “We do have a patient instructions field [in the EHR], and it is in the patient portal, but I am sure there are ways that we can do this where it is more adapted to reading level and so that it can be translated.” She said that the result of adding such health literate practices to services would be to increase efficiency for patients and providers alike.
ENSURING ACCESS FOR ALL TO HEALTH LITERATE VIRTUAL HEALTH SERVICES
The second moderator of the day, Gem Daus, is a health policy analyst with the Office of Health Equity at the Health Resources and Services Administration (HRSA). Daus introduced the next presenter, Lisa Bothwell, program analyst at the Administration for Community Living (ACL). Bothwell’s presentation explained what the law requires around accessibility in telehealth services, as well as what is known about the actual experience of the disabled community with telehealth. In so doing, this talk explored what added challenges those with disabilities may face in achieving health literacy, and what different strategies health systems may need to apply to provide health literate services to the disabled community.
She began by explaining that ACL is an operational division within the U.S. Department of Health and Human Services (HHS) created around “the fundamental principle that all people, regardless of age or disability, should be able to live independently and fully participate in their communities.”2 Nine different pieces of federal legislation—including the Older Americans Act, the Rehabilitation Act, and the Developmental Disability Act—authorize ACL to issue grants and provide support to grantees and nonprofit organizations that support people with disabilities and older adults, as well as those organizations that conduct research on these populations.
Bothwell stated that one ACL program, Assistive Technology State Grants, is particularly relevant to this workshop in that it provides funds to enable all 56 U.S. states and territories to improve access to and acquisition of assistive technology to individuals with disabilities of all ages. Assistive technology includes items, devices, or pieces of equipment such as joysticks, large-print keyboards, and screen readers.3 Some of these state-level assistive technology programs are able to offer trainings for users with disabilities on the use of accessible telehealth technology. These programs have worked with states and other entities to use Coronavirus Aid, Relief, and Economic Security (CARES) Act funding to provide assistive technology to increase disability access.
___________________
2 See https://acl.gov (accessed November 18, 2021).
3 Bothwell shared that these resources are available at the national website, sorted by state and territory, at https://www.at3center. net (accessed November 16, 2021).
Bothwell explained that three laws—the American with Disabilities Act (ADA), Section 504 of the Rehabilitation Act, and Section 1557 of the Patient Protection and Affordability Act of 2010—together state that individuals who identify with disabilities may not be “excluded from participation in or denied the benefits of services, programs, or activities; or be subjected to discrimination” on the basis of disability by any covered entity (HHS Office for Civil Rights, 2016).
Covered entities under the ADA include professional offices for health care providers, hospitals, social service centers, insurance offices, and pharmacies. Section 504 can apply to entities receiving Medicare or Medicaid reimbursement, while the Affordable Care Act applies to any health program or activity, any part of which is receiving federal financial assistance, or under any program or activity that is administered by any entity established under Title I of the Affordable Care Act or its amendments. Local and state requirements may also apply.
In addition, covered entities may not provide any aid, benefit, or service to persons with disabilities “that is not as effective in affording equal opportunity to obtain the same result, to gain the same benefit, or to reach the same level of achievement as that provided to others” without disabilities (HHS Office for Civil Rights, 2016). Though there is a waiver for these requirements—if they are to cause an undue financial or administrative burden to the organization or cause it to fundamentally alter the program or activity—covered entities are still obligated to act to the maximum extent possible to ensure that people with disabilities receive the benefits or services that the entity provides, said Bothwell.
Covered entities, she noted, must ensure that communication with people with disabilities be as effective as communication with other individuals. This applies not just with people with disabilities but can also apply to that person’s family members, friends, or associates. Effective communication may also require providing what are called auxiliary aids and services at no charge. The appropriate type of auxiliary aid and services required for effective communication will depend on the type of communication used by the person with disability, by the complexity of their communication, and the context in which that communication is happening, said Bothwell.
Bothwell elaborated on the role that interpretation services can play in ensuring “effective communication” with individuals with disabilities. For example, individuals who are blind or have low vision may need the services of a qualified reader, while those who are deaf or hard of hearing may require captioning provided by what are known as communication access real-time translation services. In the previous presentation, Serper had mentioned that her health system’s telehealth technology includes access to an interpreter; Bothwell explained that a qualified interpreter is trained “to interpret effectively, accurately, and impartially, both receptively and expressively, using any necessary specialized vocabulary” (HHS Office for Civil Rights, 2016). This definition, she explained, is generally similar for qualified readers and qualified speech-to-speech transliterators—specialists who are trained to understand unclear speech and repeat it again clearly. She cautioned against relying on untrained adults, such as a relative or friend, as interpreters, given that they are often unable to remain neutral during an appointment and may not be familiar with medical language.
Regarding electronic information technology, the three laws dictate that “covered entities must offer people with disabilities full and equal access to the electronic information technology they employ.” This must be the case unless the covered entity provides “reasonable accommodations or reasonable modifications that permit those individuals to receive all the benefits provided by the electronic information technology in an equally effective manner” (HHS Office for Civil Rights, 2016).
Bothwell said that the HHS Office for Civil Rights issued guidance prior to the COVID-19 pandemic on accessibility requirements (HHS Office for Civil Rights, 2016), calling it “a great resource to review if you are looking at building out your telehealth system and processes.” She noted, too, that when Congress passed the ADA, it did so with foresight into the fact that requirements might need to change in the future; it included language that requires covered entities to provide accommodations and services that keep pace with rapidly changing technology.
Bothwell offered a few suggestions in addition to the minimum requirements of the law. When it comes to providing accessible telehealth services, Bothwell suggested using a telemedicine platform with the capacity to add a third party, such as an interpreter for someone who is deaf or hard of hearing or a remote care provider for a patient with an intellectual disability. She also suggested that health systems consider modifying their pre-telemedicine appointment practices to allow for additional time needed to provide a patient with a visual or intellectual disability extra assistance with using the video platform technology; some of the programs Bothwell mentioned earlier are able to serve as a resource and provide that training. Various design standards for developing accessible websites exist, including the Web Content Accessibility Guidelines,4 and published literature that discusses the ability to personalize telehealth options for individuals with a disability and older adults (Valdez et al., 2021).
___________________
4 See https://www.w3.org/TR/WCAG21 (accessed December 2, 2021).
To conclude her presentation, Bothwell provided some relevant statistics from two recent studies. The Flatten Inaccessibility Survey of adults who are blind or have low vision found that 30 percent of the 988 participants reported meeting with their health care provider using telehealth and of those, 21 percent reported that the telehealth platform was not accessible (Rosenblum et al., 2020). A second study Bothwell highlighted surveyed readiness for a video visit among older adults. The study found that 25 percent of adults ages 65 to 74, 44 percent of those ages 75 to 84, and 72 percent of adults who were 85 years or older met criteria for being unready for a video visit. The reasons for their unreadiness included:
- difficulty hearing
- difficulty communicating
- trouble reading small print
- dementia
- issues with lack of Internet access, lack of email, or texting ability (Lam et al., 2020).
She noted that approximately 20 percent of people with disabilities are likely to not have access to a computer, tablet, or smartphone that would enable them to access a telehealth platform (Noel and Ellison, 2020).
Session moderator Gem Daus, of HRSA, asked Bothwell how health systems, as they seek to improve their telehealth services, might work to engage the disability community in a way that is informative but without putting any additional burdens on those individuals. Bothwell suggested reaching out to aging and disability networks and asking them how best to provide trainings and to see if they would be willing to engage their members to conduct usability testing.5 She added that it is crucial to include people with disabilities in the workflow process—from the time that person makes a phone call to the health care provider, all the way through to the end of their treatment or care. As a person with a disability, she has found it important when a provider thinks not just about how to schedule a visit with her, but how she can be integrated into the workflow from start to finish. She noted that the U.S. Justice Department has an ADA informational hotline that care professionals and practitioners can contact to receive help for meeting ADA requirements.6
RESOURCES FOR PROVIDING HEALTH LITERATE VIRTUAL SERVICES
The final moderator of the workshop was Jay Duhig, director of patient integration and patient safety at AbbVie, Inc. Duhig introduced the final presenter, Whitney Wiggins, public health analyst at the HRSA Office for the Advancement of Telehealth (OAT). Wiggins’s presentation focused on the resources and strategies that are available to providers and patients for improving the health literacy of virtual health services.
Wiggins opened by noting that HRSA has awarded over 1,300 grants that include a telehealth component. She began by providing an overview of the types of telehealth-related activities that take place across HRSA, and which her office oversees. Telehealth-related activities across HRSA include programs that provide support for distance learning and workforce development, direct clinical care, infrastructure development, and research. Her office links together HHS’s telehealth efforts, and coordinates with other federal partners to create programs that improve access to health care using telehealth, enhance telehealth outcomes, and support both clinicians and patients through the process. OAT also promotes the use of telehealth technologies for health care delivery, education, and for providing health information services. It provides funding for direct services, research, and technical assistance with telehealth. In addition to these more programmatic roles, OAT is responsible for monitoring policy and research that relates to providing telehealth services.
Wiggins then highlighted specific telehealth-related programs with which OAT is involved. OAT’s resource centers program supports the delivery of technical assistance to programs around the country that provide telehealth services. In 2020, these centers fielded over 10,000 technical assistance inquiries, a 350 percent increase over 2019. It also reached 200,000 participants through 2,716 outreach events, a 200 percent increase over 2019.
The continuum of grant programs that OAT funds includes Telehealth Centers of Excellence, the Evidence-Based Telehealth Network grant program, the Rural Telehealth Research Center, and the Telehealth Network grant program. The Centers of Excellence program monitors the clinical effectiveness and cost-effectiveness of telehealth visits compared to in-person visits and helps build the evidence base in support of telehealth. Together with the Rural
___________________
5 See https://acl.gov/programs/aging-and-disability-networks (accessed November 11, 2021).
6 See https://www.ada.gov/infoline.htm (accessed October 29, 2021).
Telehealth Research Center, it focuses on rural and medically underserved areas with high rates of chronic disease and poverty. The Telehealth Research Center analyzes, publishes, and disseminates telehealth research.
The Evidence-Based Telehealth program, which Wiggins oversees, funds research to develop and compare common quality measures used for telehealth services and in-person services. One project this program funded used telehealth networks to increase access to behavioral health care services in rural and frontier communities.7 Evaluation of this program’s work will establish an evidence base to assess the effectiveness of telebehavioral health care for patients, providers, and patients. During 2019 and 2020, this program served nearly 3,100 patients and saved nearly 734,000 miles in travel for care. In 2021, the Evidence-Based Telehealth program is aiming to improve direct-to-consumer telehealth services in rural and frontier communities by using telehealth networks; the program also includes evaluations of its efforts, which can help to create an evidence base for assessing the effectiveness of other direct-to-consumer telehealth care for patients, providers, and payers. A new effort, the telehealth broadband pilot program, is a joint effort between Wiggins’ office, the Federal Communications Commission, HHS, and the U.S. Department of Agriculture. This 3-year program will assess existing gaps in broadband coverage in Alaska, Michigan, Texas, and West Virginia and then connect communities in these states to broadband resources.
The Telehealth Network grant program, also overseen by OAT, aims to demonstrate the use of telehealth networks to improve health care services for medically underserved populations in urban, rural, and frontier communities. In fiscal year 2020, this program focused on using telehealth to deliver emergency services with an emphasis on expanding emergency services for stroke, cardiology, and psychiatry. In 2020, the Telehealth Networks saved nearly 3.8 million miles in travel for care, up from 3.2 million miles in 2019 and 1.6 million miles in 2017.
Having laid out the many telehealth-related programs within HRSA, Wiggins then shifted her attention to a discussion of the importance of inclusion and access to telehealth, especially in rural communities. In 2020, the HHS Office of the Assistant Secretary for Planning and Evaluation examined Medicare beneficiary use of telehealth visits during the COVID-19 pandemic and concluded that Medicare’s new telehealth flexibilities around reimbursement played a critical role in helping to maintain access to primary health care services (Bosworth et al., 2020). Telehealth services also played a primary role in helping rural communities access care during the pandemic.
Wiggins then discussed the concept of digital inclusion, which she considers to be an important component of health equity. According to the National Digital Inclusion Alliance, digital inclusion refers to the activities necessary to ensure that “all individuals and communities, including the most disadvantaged, have access to and use of information and communication technologies.” The five elements of digital inclusion that they highlight are:
- affordable, robust broadband Internet service;
- Internet-enabled devices that meet the needs of the user;
- access to digital literacy training;
- quality technical support; and
- applications and online content designed to enable and encourage self-sufficiency, participation, and collaboration.8
Wiggins noted that rural communities in particular often experience barriers to digital inclusion. Broadband access, in particular, is a common challenge. Wiggins shared that HRSA’s Telehealth Network grant program has worked to provide resources to help overcome some of these challenges. As an example, Wiggins said that one awardee, the Marshfield Clinic, recently joined the Wisconsin governor’s task force on broadband. The task force designed surveys and focus groups to understand patient challenges, and created a list of organizations that were providing digital literacy classes and providing tech support. One recommendation that the task force issued was to establish a statewide digital equity fund that would “fund, strengthen, and support digital inclusion activities and ideas that lead to all Wisconsin residents having the information capacity needed to fully participate in society.”9
___________________
7 The U.S. Department of Agriculture’s Economic Research Service explains that “frontier and remote” communities are considered a subset of rural areas, “characterized by some combination of low population size and high geographic remoteness.” https://www.ers.usda.gov/data-products/frontier-and-remote-area-codes (accessed December 16, 2021).
8 For greater detail on each of these elements of digital inclusion, see https://www.digitalinclusion.org/definitions (accessed November 18, 2021).
9 See https://psc.wi.gov/Documents/broadband/2021%20Governors%20Task%20Force%20on%20Broadband%20Access.pdf (accessed November 18, 2021).
Program grantees have reported that having one of these grants enabled them to be leaders in their organizations during the pandemic-triggered transition from in-person to telehealth appointments. At the start of the transition, clinicians reported they were spending more time providing technology support to their patients, which limited the time they spent on addressing medical concerns. Grantees were able to assume that support role, as well as serve as a specific point of contact that patients and providers could contact to answer questions and address technology issues. Grantees also established procedures for doing preappointment technology checks with patients and recommending applications that are easily accessible for patients.
Wiggins said that many of HRSA’s grantees, across their telehealth-related programs, found that digital navigators, patient coordinators, and community health workers proved to be valuable resources during the pandemic, helping to improve the digital skills of underconnected or unconnected populations in a manner that was culturally competent. A survey by a grantee at the University of Kansas Health Services found that having a digital navigator or coordinator was key to patients’ high satisfaction with telehealth services.
Some sites, said Wiggins, developed promotional resources for their telehealth services as a means of helping patients understand and learn more about telehealth services at their convenience. For health systems contemplating preparing such resources, she noted that such resources should explain what telehealth is and the health service being provided, what can and cannot be done through telehealth services, answer common questions such as how to schedule an appointment and access telehealth services, and be culturally competent and available in the languages spoken in a given community. Wiggins also shared a video on accessing telehealth services that the Texas A&M University Medical Center developed and posted on YouTube for other health systems to use.10 She also discussed a new resource, Telehealth.HHS.gov, which she described as a “trusted website and resource for both patients and providers” to promote access and use of telehealth services.
Session moderator Jay Duhig, of AbbVie, Inc., asked Wiggins to comment on efforts her office made to assist individuals who did not have access to broadband connectivity during the COVID-19 pandemic. She replied that some of her office’s programs worked directly with patients, while others coordinated with community-based resources, such as libraries, schools, and Indian Health Service clinics that were providing broadband access in their parking lots.
DISCUSSION
Shiyanbola opened the discussion by asking Serper if patients in her health system receive instructions ahead of time to find a location from which to do their telehealth visit that would afford them privacy and comfort. Serper replied that the previsit guide patients receive does suggest they find a quiet place to have their visit; but in the real world, many patients have their visit during work breaks or while they were driving.
Duhig then asked the three speakers if they could address some of the current research gaps that have emerged as programs respond to the COVID-19 pandemic. Serper responded that it remains to be seen what “dose” of telemedicine is best for patients with chronic illnesses; in other words, there are research gaps around identifying the optimal balance of telehealth and in-person clinical visits for such patients. Wiggins suggested that research be conducted to better understand clinicians’ needs; this would allow for them to be provided with more resources before they begin using telehealth. She has also heard from grantees that there is a need to identify what resources caregivers want and need that would help them to support their patients with telehealth appointments. Bothwell suggested conducting more research exploring how best to communicate through telehealth with communities in which English is not the preferred language. As an example, she said that there are different forms of sign language used in America (e.g., Black American Sign Language) and wondered how those differences manifest in health care and accessibility.
Daus asked for the panelists’ thoughts on whether telehealth visits will continue once the pandemic is over, or how that might vary by appointment type (e.g., follow-up visits as opposed to initial visits). Serper said her experience as a clinician is that follow-up appointments best lend themselves readily to telehealth. She said it is nice to establish an initial in-person connection with a patient, but that follow-up telehealth visits do not seem to impair that connection. She acknowledged that this might not be the case with all areas of medicine, such as psychotherapy.
In her final question, Shiyanbola asked for ideas on how to encourage health systems, providers, and other organizations to address health literacy and accessibility barriers as they provide virtual health services. Wiggins said her programs have found involving care coordinators in the telehealth workflow to be a great asset. Doing so takes some of the burden off of the clinician as far as making connections with resources that can address health literacy and accessibility. ◆◆◆
___________________
10 Available at https://www.youtube.com/watch?v=tAqAdNxRUrM (accessed December 2, 2021).
REFERENCES
Bailey, S. C., M. Serper, L. Opsasnick, S. D. Persell, R. O’Conor, L. M. Curtis, J. Y. Benavente, G. Wismer, S. Batio, M. Eifler, P. Zheng, A. Russell, M. Arvanitis, D. P. Ladner, M. J. Kwasny, T. Rowe, J. A. Linder, and M. S. Wolf. 2020. Changes in COVID-19 knowledge, beliefs, behaviors, and preparedness among high-risk adults from the onset to the acceleration phase of the U.S. outbreak. Journal of General Internal Medicine. 35(11):3285-3292. https://doi.org/10.1007/s11606-020-05980-2.
Bosworth, A., J. Ruhter, L. W. Samson, S. Sheingold, C. Taplin, W. Tarazi, and R. Zuckerman. 2020. Medicare beneficiary use of telehealth visits: Early data from the start of the COVID-19 pandemic. Washington, DC: Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services. https://aspe.hhs.gov/sites/default/files/migrated_legacy_files//198331/hp-issue-brief-medicare-telehealth.pdf (accessed December 16, 2021).
HHS Office for Civil Rights. 2016. Guidance and resources for electronic information technology: Ensuring equal access to all health services and benefits provided through electronic means. https://www.hhs.gov/sites/default/files/ocr-guidance-electronic-information-technology.pdf (accessed December 16, 2021).
Koma, W., J. Cubanski, and T. Neuman. 2021. Medicare and telehealth: Coverage and use during the COVID-19 pandemic and options for the future. Kaiser Family Foundation issue brief. https://www.kff.org/medicare/issue-brief/medicare-and-telehealth-coverage-and-use-duringthe-covid-19-pandemic-and-options-for-the-future (accessed December 16, 2021).
Lam, K., A. D. Lu, Y. Shi, and K. E. Covinsky. 2020. Assessing telemedicine unreadiness among older adults in the United States during the COVID-19 pandemic. JAMA Internal Medicine 180(10):1389-1391. https://doi.org/10.1001/jamainternmed.2020.2671.
Noel, K., and B. Ellison. 2020. Inclusive innovation in telehealth. NPJ Digital Medicine 3(89). https://doi.org/10.1038/s41746-020-0296-5; https://www.nature.com/articles/s41746-020-0296-5 (accessed December 16, 2021).
Rosenblum, L. P., P. Chanes-Mora, C. R. McBride, J. Flewellen, N. Nagarajan, R. Nave Stawaz, and B. Swenor. 2020. Flatten inaccessibility: Impact of COVID-19 on adults who are blind or have low vision in the United States. American Foundation for the Blind. https://static.afb.org/legacy/media/AFB_Flatten_Inaccessibility_Report_Accessible_FINAL.pdf?_ga=2.258125450.1441867718.1633723294-1731864937.1633723294 (accessed December 16, 2021).
Serper, M., F. Nunes, N. Ahmad, D. Roberts, D. C. Metz, and S. J. Mehta. 2020. Positive early patient and clinician experience with telemedicine in an academic gastroenterology practice during the COVID-19 pandemic. Gastroenterology 159(4):1589-1591. e1584. https://doi.org/10.1053/j.gastro.2020.06.034.
Valdez, R. S., C. C. Rogers, H. Claypool, L. Trieshmann, O. Frye, C. Wellbeloved-Stone, and P. Kushalnagar. 2021. Ensuring full participation of people with disabilities in an era of telehealth. Journal of the American Medical Informatics Association 28(2):389-392. https://doi.org/10.1093/jamia/ocaa297. PMID: 33325524; PMCID: PMC7717308.
Weiss, B. D., M. Z. Mays, W. Martz, K. M. Castro, D. A. DeWalt, M. P. Pignone, J. Mockbee, and F. A. Hale. 2006. Quick assessment of literacy in primary care: The newest vital sign. Annals of Family Medicine 3(6):514-22. https://doi.org/10.1370/afm.405. Erratum in: Annals of Family Medicine 2006 4(1):83.
Wolf, M. S., M. Serper, L. Opsasnick, R. M. O’Conor, L. Curtis, J. Y. Benavente, G. Wismer, S. Batio, M. Eifler, P. Zheng, A. Russell, M. Arvanitis, D. Ladner, M. Kwasny, S. D. Persell, T. Rowe, J. A. Linder, and S. C. Bailey. 2020. Awareness, attitudes, and actions related to COVID-19 among adults with chronic conditions at the onset of the U.S. outbreak: A cross-sectional survey. Annals of Internal Medicine 173(2):100-109. https://doi.org/10.7326/M20-1239.
DISCLAIMER: This Proceedings of a Workshop—in Brief was prepared by Rose Marie Martinez, Kelly McHugh, and Joe Alper as a factual summary of what occurred at the meeting. The statements made are those of the rapporteurs or individual workshop participants and do not necessarily represent the views of all workshop participants; the planning committee; or the National Academies of Sciences, Engineering, and Medicine.
*The National Academies of Sciences, Engineering, and Medicine’s planning committees are solely responsible for organizing the workshop, identifying topics, and choosing speakers. The responsibility for the published Proceedings of a Workshop—in Brief rests with the institution. Workshop planning committee members are Gem Daus, Health Resources and Services Administration; James (Jay) Duhig, AbbVie, Inc.; and Olayinka Shiyanbola, University of Wisconsin, Madison.
REVIEWERS: To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Christopher Trudeau, University of Arkansas—Little Rock, and Joanne G. Schwartzberg, Accreditation Council for Graduate Medical Education. Leslie Sim served as the review coordinator.
SPONSORS: The Roundtable on Health Literacy, under which this workshop was organized, is supported by AbbVie, Inc., California Dental Association, U.S. Department of Health and Human Services, Eli Lilly and Company, Health Literacy Media, Health Literacy Partners, Health Resources and Services Administration (HHSH25034011T), Merck & Co., National Institutes of Health (HHSN263201800029I /HHSN26300012), Northwell Health, and Pfizer, Inc.
For additional information regarding the workshop, visit https://www.nationalacademies.org/our-work/providing-health-literate-virtual-health-services-a-workshop.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2022. Providing health literate virtual health services: Proceedings of a workshop—in brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/26490.
Health and Medicine Division

Copyright 2022 by the National Academy of Sciences. All rights reserved.











