Nursing Home Environment and Resident Safety
Nursing home residents have diverse needs, which can be viewed within the framework of Maslow’s hierarchy of needs (as discussed in Chapter 4 and detailed in Table 4-1). This chapter of the report explores two key areas that are critical to residents’ quality of care and quality of life: resident safety and the physical environment in which nursing home residents live and receive care and services. These two topics are located within the second level of Maslow’s hierarchy—safety and security—as depicted in Figure 4-1.
ENSURING THE SAFETY OF NURSING HOME RESIDENTS
Patient safety is an essential component of high quality care (IOM, 2001). Given the large share of nursing home residents who are frail, vulnerable, and have chronic medical conditions, keeping residents safe from harm is critically important and particularly challenging. As reinforced throughout this report, a nursing home provides care to residents, while also serving as a place to live. Because of this dual function as well as the health characteristics of their residents, nursing homes must balance safety with residents’ preferences for autonomy and quality of life (Brauner et al., 2018).
Preventable adverse events constitute more than half of all harms experienced by nursing home residents (OIG, 2014a). The most common of these are falls, infections, and adverse events related to medications. While medical errors, such as providing the wrong medication to a resident, are a common source of patient harm, failure to provide care also results in patient harm (Simmons et al., 2016). Omissions of care, also referred to as missed care, are a key patient safety issue in nursing homes (Ball and
Griffiths, 2018), and have a negative impact on resident outcomes as well as the quality of care in nursing homes (Ogletree et al., 2020).
This chapter discusses some of the more common safety-related areas of focus in nursing homes including improving medication safety, resident falls, preventing elder abuse, improving communication during transitions of care, enhancing infection control, and strengthening emergency planning, preparedness and response.
Improving Medication Safety
All certified nursing homes are required by statute to provide pharmaceutical services to ensure that all drugs needed to meet each resident’s needs are dispensed and administered properly.1 Regulations revised in 2016 require a licensed pharmacist review each resident’s drug regimen as well as their medical record on a monthly basis (Barlas, 2016).2
Given the prevalence of nursing home residents with multiple chronic conditions, ongoing symptoms (e.g., chronic pain), and acute problems (e.g., infections), polypharmacy—defined as taking five or more medications per day—is common. Research indicates that 91 percent of nursing home residents take more than 5 medications per day, while 65 percent of residents take more than 10 medications per day (Spinewine et al., 2021). Polypharmacy is associated with a high risk of negative clinical outcomes, including cognitive impairments, falls, fractures, adverse drug events (ADEs),3 and drug interactions (Bernsten et al., 2001; Hoel et al., 2021; NIA, 2021; Wang et al., 2015).
Medication errors, which can occur at any step of the medication use process (prescribing, purchasing, ordering, delivery, storage, preparation, administration, or monitoring), affect between 16 and 27 percent of all nursing home residents (Spinewine et al., 2021). Research shows that approximately 40 percent of medication errors occur at care transitions (Hughes, 2008; Redmond et al., 2018). Poor communication during these transitions can
___________________
1 CMS Requirements for Long-Term Care Facilities—Pharmacy Services, 42 CFR § 483.45 (2016).
2 Concerns over conflict of interest were raised in relation to cases where pharmacists were seen to lack independence from and were thus unduly influenced by pharmaceutical companies (Barlas, 2012). Several cases were filed under the whistleblower provisions of the False Claims Act alleging that nursing home pharmacies accepted kick-backs from drug manufacturers in exchange for prescribing that manufacturers’ prescription drugs (CANHR, 2009; DOJ, 2015). Other cases involved a company offering consultant pharmacist services to nursing homes at below market value in exchange for the pharmacist prescribing that drug manufacturer’s products (McCrystal et al., 2010). However, the revised rules did not contain any specific requirements to address these concerns (Barlas, 2016).
3 An adverse drug event (ADE) is an injury resulting from medical intervention related to a drug. This includes medication errors, adverse drug reactions, allergic reactions, and overdoses (ODPHP, 2021).
also lead to adverse drug events (Branch et al., 2021). Thus, ensuring the appropriate use of medications is crucial to ensuring resident safety, preventing unnecessary harm, and improving the quality of care in nursing homes.
Efforts to improve medication safety involve regular, formal pharmacist reviews of medications combined with an enhanced integration of the pharmacist with the interdisciplinary care team. One review found that the introduction of pharmacists into nursing homes contributed positively to reducing the number of drugs taken by nursing home residents (Lee et al., 2019). Earlier studies revealed that interventions by pharmacists in nursing home settings generally reduced inappropriate prescribing and improved the knowledge base of nursing home staff (Verrue et al., 2009).
Another initiative targeting medication safety is deprescribing, which refers to the process of reducing, discontinuing, or withdrawing of medications. Deprescribing has been found to have an impact on improving health outcomes, reducing the number of potentially inappropriate medications, decreasing the number of older people who had falls, and lowering mortality rates (Kua et al., 2019). Approaches to deprescribing medications that are no longer needed or that have more potential for harm than good include, for example, efforts to substitute nonpharmacologic management for psychoactive medications in persons with dementia (O’Mahony et al., 2014; Sloane et al., 2021; Welsh et al., 2020).
Among the quality improvement strategies focused on medication safety are efforts to minimize the adverse effects of potentially inappropriate prescribing, overprescribing, and drug interactions. Approaches to optimize prescribing include the development of and adherence to prescribing guidelines, such as the Beers Criteria4 for potentially inappropriate medication use in older persons (American Geriatrics Society, 2019). Other approaches include improving communication within the care team and with residents and families about medication issues (e.g., potentially inappropriate antibiotics) and tailoring medication prescribing to resident characteristics and needs (Desai et al., 2011). As one of the four components of age-friendly health systems, effective medication management emphasizes the key role of regular care plan meetings with the interdisciplinary care team (as discussed in Chapter 4) to ensure alignment with “what matters” to the individual nursing home resident and their families (Edelman et al., 2021). For a nursing home resident’s perspective on medication safety, see Box 6-1.
Health information technology applications such as electronic medication administration records (eMARs) hold the potential to improve medication safety—particularly in terms of reducing medication errors—in nursing home settings. Such eMARs enable the automatic documentation of medication into the electronic medical record. Nursing home settings have not
___________________
4 For more information, see https://dcri.org/beers-criteria-medication-list (accessed November 3, 2021).
adopted this technology as broadly as other health care settings, which may be due to a lack of financial support (Spinewine et al., 2021). The integration of eMARs with clinical decision-making would help to improve the safety of medication delivery, the tracking of residents’ allergies, and the monitoring of residents’ response to medication (Poon et al., 2010; Truitt et al., 2016).
Antipsychotic Medications
A serious patient safety and quality issue in nursing homes is the use of antipsychotic medications. Such medications are used to treat mental health conditions such schizophrenia. The Food and Drug Administration released information about cardiac fatalities in 2005 and issued black box warnings about the association of antipsychotic medications with an increased risk of death when used to treat elderly patients with dementia-related psychosis (Narang et al., 2010).5 The Office of the Inspector General (OIG) raised concerns about the high use of antipsychotic medications among nursing home residents more than 10 years ago, based on an examination of claims for atypical antipsychotic drugs6 for nursing home residents. OIG found
___________________
5 Drug companies charged with off-label marketing of antipsychotic drugs for nursing home residents paid large penalties in settlements under the False Claims Act. See https://www.justice.gov/opa/pr/johnson-johnson-pay-more-22-billion-resolve-criminal-and-civil-investigations (accessed February 16, 2022).
6 Atypical antipsychotics—also known as second-generation antipsychotics and serotonin-dopamine antagonists—are a type of psychotropic drug that the Food and Drug Administration has approved to treat medical conditions such as schizophrenia, Tourette’s syndrome, Huntington’s disease, and bipolar disorder (OIG, 2021).
that nearly 90 percent of claims for atypical antipsychotic drugs were associated with a condition listed in the black box warning (OIG, 2011). In an effort to advance person-centered care and promote the use of nonpharmacologic treatments for nursing home residents with dementia, the Centers for Medicare & Medicaid Services (CMS) launched the National Partnership to Improve Dementia Care in Nursing Homes in 2012 (discussed in Chapter 4). An initial focus of the Partnership was on reducing use of antipsychotic medications for nursing home residents with dementia.
More recently, the OIG conducted an examination of the way in which CMS monitors the use of antipsychotic medication use in nursing homes (OIG, 2021). CMS uses a quality measure to track the number of long-stay nursing home residents who received antipsychotic medication. OIG concluded that CMS’s reliance on nursing homes’ self-reported data through the Minimum Data Set (MDS) as the only source of information on antipsychotic drug use in nursing homes has resulted in an inaccurate measurement of the full extent of such medication use. The OIG analyzed Medicare claims and found that 5 percent of all Part D beneficiaries who were long-stay residents age 65 and older had a Part D claim in 2018 for an antipsychotic medication, but the MDS did not report those residents as having received an antipsychotic drug in the same quarter in which they had a Part D claim (OIG, 2021). Moreover, the OIG found that nearly one in three of all nursing home residents who had schizophrenia diagnoses documented in the MDS did not have any Medicare service claims for that diagnosis—in other words, there was no documented evidence that the resident received treatment for their schizophrenia diagnosis. Importantly, CMS excludes residents with MDS-reported diagnoses of schizophrenia, Huntington’s disease, or Tourette’s syndrome from inclusion in its quality measure of antipsychotic drug use. Finally, OIG found that even for the residents whose antipsychotic drug use was captured in the MDS, the MDS does not capture critically important details such as the particular antipsychotic drug prescribed, specific dosage, and duration of use.
Based on its findings, OIG recommended that CMS take steps to improve the accuracy of MDS reports by developing automatic comparisons of Medicare Part D claims and MDS information to identify inconsistencies. OIG also recommended that CMS consider supplementing MDS information with Part D data to facilitate the effective monitoring of medication use in nursing homes (OIG, 2021).
Having an effective electronic health record (EHR) system (discussed in Chapter 9) that is highly integrated with medication prescribing and administration processes, for example, could enable nursing homes to run automated comparisons of MDS survey data and pharmacy data (part of Medicare Part D claims), which may improve oversight and associated prescribing practices for chronic illnesses such as dementia. In the case of
nursing home residents with dementia, combining these data sources could improve accuracy of identifying cases of dementia, and reduce errors of omission and commission that might result in inappropriate prescribing and administration practices for the treatment of nursing home residents with dementia (Lin et al., 2010).
Falls Prevention
The prevention of physical injury, including resident harm from falling, is a prominent safety issue in nursing home settings, and preventing falls is a major focus for quality improvement efforts. Approximately half of all nursing home residents fall every year (AHRQ, 2019). Moreover, falls resulting in significant injury represented nearly 1 out of 10 adverse events experienced by Medicare skilled nursing facility residents (OIG, 2014a). Falls are very common occurrences in nursing homes due to the high prevalence of gait, balance, and muscle strength problems among residents (Chang et al., 2010). Systematic reviews have identified a number of factors associated with an elevated risk of falls, including previous falls, whether a resident uses a cane or other assistive walking device, wandering, Parkinson’s disease, dizziness, polypharmacy, and the use of sedatives, antipsychotics, or antidepressants (Cameron et al., 2018a; Deandrea et al., 2013; Muir et al., 2012). In addition, residents with cognitive impairment or acute conditions may make errors in judgment that lead to falls (Brauner et al., 2018; Fischer et al., 2014; Meuleners et al., 2016). Thus, falls are associated with a range of issues, including medication management, mobility, and the cognitive state of the resident (Edelman et al., 2021).
The role of medication in falls has been well studied. A number of drugs, aptly referred to as fall-risk increasing drugs, are associated with a significant risk of falls. In particular, the use of psychotropic, cardiac, and analgesic drugs in the older population is associated with higher risk of falls (Leipzig et al., 1999a,b). A 2009 study analyzed nine unique drug classes: antihypertensive agents, diuretics, β blockers, sedatives and hypnotics, neuroleptics and antipsychotics, antidepressants, benzodiazepines, narcotics, and nonsteroidal anti-inflammatory drugs (Woolcott et al., 2009). The authors presented a significant association between falls and the use of sedatives and hypnotics, antidepressants, and benzodiazepines, and noted that the use of antidepressants had the strongest association with falls. Other drug classes have also been associated with an increased fall risk, such as neuroleptics and antipsychotics, and nonsteroidal anti-inflammatory drugs (Woolcott et al., 2009). The most successful fall-prevention strategies are multifactorial, containing elements that address the physical environment, medication prescribing, and physical exercise. Successful efforts also include a focus on education and training, mobility assistance, balance and strength
training, reductions in the number of prescribed medications, and increases in staffing levels (Cameron et al., 2018a; Clemson et al., 2012; Leland et al., 2012; Vlaeyen al., 2015). The Agency for Healthcare Research and Quality (AHRQ) developed an interdisciplinary falls management program to reduce falls in nursing homes.7
Efficacy trials have demonstrated that multicomponent interventions can reduce the occurrence of falls by as much as one-third. Fall-reduction rates in clinical practice, however, are much lower (Gulka et al., 2020). It is important to recognize that falls in the nursing home setting might be associated with positive changes, such as increased mobility as a result of physical therapy and a resident’s ability to get up and walk around rather than being confined to a bed or a chair. This increased resident autonomy, which can be viewed as an improvement in the resident’s quality of life, can increase the residents’ risk of falling at the same time. Thus, the occurrence of a fall in a nursing home setting may not necessarily be an indicator of poor care, but rather a reflection of the high-risk status of the population, coupled with the importance of promoting independence among residents with the goal of improving quality of life (Cameron et al., 2018b). Certain videogame-based exercises show promise in contributing to reducing the risk of falling in nursing home settings. Such exercises work to enhance older adults’ gait, balance, and overall physical performance (Bateni, 2012; Lee et al., 2019; Tay et al., 2018).
Preventing Elder Abuse in the Nursing Home Setting
Despite these protections enshrined in federal legislation, elder abuse in nursing homes continues to represent a serious threat to residents’ safety and quality of life. Though a standard or universal definition of elder abuse does not exist (Braaten and Malmedal, 2017), CMS defines abuse as
the willful infliction of injury, unreasonable confinement, intimidation, or punishment with resulting physical harm, pain or mental anguish. Abuse also includes the deprivation by an individual, including a caretaker, of goods or services that are necessary to attain or maintain physical, mental and psychosocial well-being.8,9
___________________
7 For access to the AHRQ Fall Program, see https://www.ahrq.gov/patient-safety/settings/long-term-care/resource/injuries/fallspx/man1.html (accessed February 7, 2022).
8 CMS Survey and Certification of Long-Term Care Facilities—Definitions, 42 CFR § 488.301 (2017).
9 Other definitions are found in the literature. For example, according to the Centers for Disease Control and Prevention, “Elder abuse is an intentional act or failure to act that causes or creates a risk of harm to an older adult. An older adult is someone age 60 or older. The abuse often occurs at the hands of a caregiver or a person the elder trusts” (CDC, 2021).
Elder abuse can take many forms, including physical, psychological, financial, sexual, and spiritual abuse10 as well as neglect. In the nursing home setting, abuse of residents can be perpetrated by staff, family members, or other residents (Myhre et al., 2020; NCEA, 2021a).
The Nursing Home Reform Act of 1987, passed as part of the Omnibus Budget Reconciliation Act of 1987 (OBRA 87), established quality-of-life rights for nursing home residents, including freedom from abuse, mistreatment, and neglect and the ability to voice grievances without fear of discrimination or reprisal (Wiener et al., 2007). Physical restraints, the use of which had previously been common in nursing homes, were allowed only under very narrow circumstances, and strict requirements were established limiting the amount of time that residents could be restrained.11 OBRA 87 also expanded the rights of nursing home residents to communicate with regulators and specified that residents have access to a state long-term care ombudsman.12
As emphasized throughout this report, many nursing home residents have physical or mental impairments, and their dependency on others for care amplifies their vulnerability to abuse (Braaten and Malmedal, 2017; Lindbloom et al., 2007). Older adults with Alzheimer’s disease and related dementias (ADRD) represent a growing share of the nursing home population and, given their cognitive impairments, are at even greater risk for abuse. Moreover, ADRD can also lead to behavior that may be aggressive and challenging for nursing home staff to manage, which may in turn lead to incidents of abuse of residents by staff (Berridge et al., 2019; Braaten and Malmedal, 2017; IOM and NRC, 2014; Myhre et al., 2020).
Although staff use of physical restraints on residents has significantly declined since OBRA 87, nursing home staff use psychotropic medications to control the symptoms of certain diseases. According to Human Rights Watch, U.S. nursing facilities administer antipsychotic medications to thousands of residents, most of whom have Alzheimer’s disease or some other form of dementia with associated symptoms such as agitation, restlessness, and aggression. Not only do these residents not have a diagnosis for which these drugs are approved for use, but antipsychotic drugs are very
___________________
10 An element of elder abuse, spiritual abuse refers to efforts to intimidate, pressure, or control a person using religion, faith, or beliefs. Examples include using scripture or beliefs to humiliate a person, and force a person into doing things (e.g., giving money) against their will, or not allowing residents to attend religious ceremonies.
11 The series of reforms included the requirement that nursing home residents have “the right to be free” from physical and chemical restraints not required to treat their medical symptoms. Viewed as harmful to residents’ health and quality of life, the restraints used included physical restraints such as hand mitts, vests that tie residents to chairs or beds, and restrictive chairs that limit mobility as well as chemical restraints such as psychoactive drugs used to affect a resident’s mood and behavior (OIG, 2019).
12 Specifically, OBRA 87 mandated that nursing facility residents have “direct and immediate access to ombudspersons when protection and advocacy services become necessary.”
dangerous for older people with dementia, significantly increasing their risk of heart problems, infections, and falls. These drugs are often given to residents without their consent (HRW, 2018). Moreover, research indicates that nursing homes are diagnosing residents as having schizophrenia to justify the use of antipsychotic drugs to render residents more compliant. An investigation of Medicare data by the New York Times found that the percentage of nursing home residents diagnosed with schizophrenia has risen 70 percent since 2012. Currently, one in nine nursing home residents have a diagnosis of schizophrenia (Thomas et al., 2021). Thus, there is increasing concern that while physical restraints may no longer be in use in nursing home settings, they have been replaced by chemical restraints and that the use of such medications without the resident’s consent constitutes a form of abuse (HRW, 2018).
Other medical conditions common among nursing home residents can cause agitation, confusion, and aggression and thus increase the risk of abuse of residents by staff (Braaten and Malmedal, 2017). Finally, not only is the population aging, but it is becoming increasingly diverse. Little is known, however, about racial or ethnic differences in elder abuse. Available evidence points to a significantly higher prevalence of financial and psychological abuse in African American adults than in White adults (Dong et al., 2014).
Scope of Abuse in Nursing Homes
Abuse in the nursing home setting could take a variety of forms, including physical neglect and depriving residents of their dignity (e.g., not changing their dirty clothes); limiting their choice over daily activities; intentionally providing inadequate care (e.g., neglecting to change their position to avoid pressure sores); and physical, psychological/emotional, sexual, and financial abuse. Research on the prevalence of abuse of residents in nursing home settings is limited, and studies often yield very different prevalence estimates.
Yon et al. conducted a systematic review and meta-analysis of self-reports of abuse by nursing home residents. According to the study’s estimates, psychological abuse was the most common, with one-third of respondents reporting incidents of psychological abuse. The next most common forms of abuse were physical abuse (14 percent), financial abuse (14 percent),13 and neglect (nearly 12 percent) (Yon et al., 2019). The lived experience of one nursing home resident is found in Box 6-2 below.
___________________
13 Examples of financial abuse in the nursing home setting include forging a resident’s signature, cashing residents’ checks without permission, theft or misuse of a resident’s funds or possessions, and forcing a resident to sign financial documents (Nursing Home Abuse Guide, 2021).
Staff are not the only perpetrators of abuse in nursing homes. One study of more than 2,000 residents in 10 nursing homes revealed that 20 percent of residents experienced at least one incidence of resident-to-resident abuse over the course of one month (Lachs et al., 2016; see also Lachs et al., 2021). Moreover, while the subject has received less attention, research reveals the pervasive nature of resident-to-staff aggression in nursing homes, particularly aggression against certified nursing assistants, who provide most of the direct care to and interact most closely with residents (Brophy et al., 2019; Lachs et al., 2013). A study of nursing home staff found that 15.6 percent of residents had exhibited aggressive behaviors toward staff during a 2-week period. Though verbal abuse (e.g., being screamed at) was the most prevalent, physical abuse of staff was common (Lachs et al., 2013). Resident-to-staff aggression may be due to a number of factors, ranging from resident frustration and aggravation to resident response to aggressive behavior or maltreatment by staff (Lachs et al., 2013). Resident abuse of staff may in turn lead staff to abuse and neglect residents as a reaction to, or out of frustration with, residents’ aggressive behavior, thus fueling a dangerous cycle of abuse. Staff who experience abuse may also feel higher levels of burnout, helplessness, self-doubt, and loneliness (Isaksson et al., 2009; Kristiansen et al., 2006) or react by avoiding contact with aggressive residents, which may result in a negative impact on the quality of care they receive (Lachs et al., 2013). One study found significant relationships among abuse and factors such as number of staff, workplace strain, and stress (Gates et al., 2003).
Research indicates that the prevalence of abuse (regardless of perpetrator) in nursing homes is significantly underestimated (Pillemer et al., 2016) and that many incidents of abuse are not reported (Storey, 2020).
Nursing home residents may fear retaliation if they report abuse, may be embarrassed or ashamed to report the incident, or may be unable to report abuse due to physical or cognitive impairments (Baker et al., 2016; Lindbloom et al., 2007). Moreover, conditions typically associated with abuse, such as being withdrawn and uncommunicative, may be easy to conflate with the common symptoms of dementia (Dong et al., 2014). Similarly, staff may not report abuse by residents out of concern about losing their job (Lachs et al., 2013).
Elder abuse is often unnoticed, ignored, and disregarded by nursing home staff. For example, one study of sexual abuse against older nursing home residents involved focus groups with nursing home staff. Interviews revealed that the staff found it difficult to imagine that acts of sexual abuse against nursing home residents could actually take place, which in turn made it very difficult for them to believe that any such abuse had actually happened. Such perceptions by staff make it more challenging to not only discover abuse, but adds to the residents’ feeling of vulnerability and heightens their hesitancy to report abuse, based on the fear they will not be believed (Iversen et al., 2015). A 2015 literature review on the state of knowledge of sexual abuse against nursing home residents revealed that both older women and men were victims of sexual abuse, which was perpetrated primarily by nursing home staff and other residents. The study emphasized the need for further research and called for effective reporting systems as one important component of a broader approach to addressing sexual abuse against older persons (Malmedal et al., 2015).
Sexual abuse allegations are not tracked on a national or state level as they are often not categorized apart from other forms of abuse. An analysis of inspection reports by CNN revealed that more than 1,000 nursing homes had been cited for mishandling or failing to prevent sexual assault and sexual abuse cases between 2013 and 2016; many facilities received multiple citations over the time period (Ellis and Hicken, 2017). Ongoing media reports and congressional testimony underscore the urgency of addressing sexual abuse in nursing homes (Fedschun, 2019; U.S. Congress, 2019).
Oversight of Elder Abuse in Nursing Homes
Federal, state, and local agencies as well as individual nursing homes all have a role to play in oversight and investigation of elder abuse in nursing homes. CMS regulations stipulate the specific processes for the reporting and investigation of incidents of abuse. Nursing homes are required to ensure that abuse is reported to state survey agencies; these agencies are in turn required to report incidents to CMS (see Table 6-1). Certain individuals (including nursing home owners, operators, and employees) are required by law to immediately report any incident to the state survey agency as well
TABLE 6-1 Reporting and Investigating Elder Abuse in Nursing Homes
| NURSING HOMES | STATE SURVEY AGENCY |
|---|---|
| Reporting Abuse | |
|
Nursing homes must ensure that allegations of elder abuse are reported to the state survey agency immediately. If the allegation involves serious bodily injury, nursing homes must report it no later than 2 hours after the allegation is made. If the incident does not involve serious bodily injuries, it must be reported within 24 hours. Federal law requires certain covered individuals at the nursing homes to report incidents immediately to law enforcement in addition to the state survey agency if there is a reasonable suspicion that a crime has occurred. Such covered individuals include nursing home owners, operators, and employees. |
State survey agencies must report to the Centers for Medicare & Medicaid Services (CMS) all complaints and certain facility-reported incidents of abuse through a computer-based complaint and incident tracking system. State survey agencies must immediately alert CMS regional offices when an especially significant or sensitive incident occurs that attracts public or broad media attention. State survey agencies are required to enter into CMS’s tracking system all complaint information gathered as part of the agency’s federal survey and certification responsibilities, as well as all facility-reported incidents that require a federal onsite survey. There is no federal requirement for state survey agencies to notify law enforcement until the state survey agency has substantiated a suspected crime. The U.S. Government Accountability Office (GAO) found that this led to delays in referring suspected crime to law enforcement. In an effort to avoid such delays, GAO recommended that CMS require state survey agencies to refer any suspected crime to law enforcement immediately. |
| Investigating Abuse | |
|
CMS requires nursing homes to have written policies and procedures for conducting internal investigations of suspected elder abuse. CMS requires nursing homes to submit findings from these investigations to the state survey agency within 5 business days of the incident. Federal law requires nursing homes to establish policies for ensuring that law enforcement is notified of elder abuse that occurs in their facilities. |
CMS requires state survey agencies to assess reports of elder abuse in nursing homes and assign a priority investigation status based on the seriousness of the allegations: Immediate jeopardy requires the agency to start onsite investigation within 2 business days of receipt. Non-immediate jeopardy high priority requires onsite investigation within 10 days of prioritization. Non-immediate jeopardy medium requires onsite survey to be scheduled (no time frame specified). Non-immediate jeopardy low requires investigation during the next survey. CMS policy requires state survey agencies to notify law enforcement of substantiated findings of elder abuse that occur in nursing homes. |
SOURCE: GAO, 2019a.
as to law enforcement if there is a reasonable suspicion that a crime has been committed (GAO, 2019a).14
Additionally, other state and local agencies may be involved in investigating abuse in nursing homes. Each state has an adult protective services (APS) program. APS jurisdiction and standards of practice vary from state to state. State and local APS work closely with local law enforcement if criminal abuse is suspected (Ramsey-Klawsnik, 2018). CMS regulations give the nursing home survey agency primary jurisdiction for allegations of abuse of residents by staff, resident-to-resident abuse, and abuse of staff by residents in nursing homes.15 In contrast, APS has jurisdiction in cases where someone from outside the facility committed abuse against a resident, such as a family member who might commit abuse during a visit (Ramsey-Klawsnik, 2018).
As an indication of increased concern about elder abuse in nursing homes, the U.S. Government Accountability Office (GAO) and OIG at the U.S. Department of Health and Human Services have released a number of investigative reports over the past several years (GAO, 2019a,b,c; OIG, 2019). GAO’s investigations revealed that the number of abuse deficiencies in nursing homes cited by state survey agencies more than doubled (from 430 to 875) between 2013 and 2017, with the most common form of abuse being physical and mental or verbal abuse. The increasing number and severity of abuse amplifies concerns about the safety of nursing home residents (GAO, 2019a).
GAO recommended that CMS develop guidance on abuse information that nursing homes should self-report and require state survey agencies to submit data on abuse and perpetrator type (GAO, 2019c). GAO also recommended that actions be taken to refer incidents of abuse to law enforcement in a timely manner; to track abuse referrals; to clarify that evidence exists to support the allegation of abuse; and to share information with law enforcement.
The OIG analyzed high-risk hospital emergency room Medicare claims for treatment and found that one in five claims was due to potential abuse or neglect of nursing home residents (OIG, 2019). OIG’s analysis revealed significant failures within each step of the process, showing that nursing homes had failed to report many instances of abuse or neglect to the state survey agencies and that several survey agencies had failed to report abuse to local law enforcement.
___________________
14 Mandated reporting laws for elder abuse require individuals such as nursing home staff, doctors, and nurses—referred to as “mandated reporters”—to contact authorities about any concerns related to elder abuse. Laws in eight states require any person who suspects elder abuse to report it to authorities (Nursing Home Abuse Justice, 2021).
15 CMS Requirements for Long-Term Care Facilities—Resident Rights, 42 CFR § 483.10 (2016).
To address the breakdown of reporting at every level, OIG recommended that CMS work with survey agencies to improve training on how to identify and report incidents of potential abuse and neglect of nursing home residents and to work to enhance existing guidance with examples of incidents of potential abuse and neglect (OIG, 2019). OIG also recommended that CMS require state survey agencies to record and track all incidents of potential abuse and neglect in nursing homes and referrals made to local law enforcement and other agencies. Finally, OIG recommended that CMS monitor the survey agencies’ reporting of findings of substantiated abuse to local law enforcement.
CMS’ quality reporting system, Care Compare (see Chapter 3), includes an alert icon to help potential residents and their families gain a better understanding of the quality of care provided by specific nursing homes, including citations for resident abuse.16
Preventing Elder Abuse
Elder abuse in general, and particularly in the nursing home setting, is not well understood or recognized. Research on elder abuse in nursing homes is still in its early stages, particularly compared with other forms of interpersonal violence (Lindbloom et al., 2007; Myhre et al., 2020; Yon et al., 2019). The nature, origins, and causes of abuse in nursing homes are associated with a complex web of personal, social, and organizational factors (Myhre et al., 2020). Research focused on recognizing and detecting abuse as well as research on strategies to address and prevent abuse of nursing home residents are both limited (Braaten and Malmedal, 2017; Myhre et al., 2020). In particular, research is needed in order to be able to better design intervention strategies and approaches and to clearly establish the linkages between intervention activities and changes in the prevalence of elder abuse (Baker et al., 2016; Kennedy and Will, 2021; Shen et al., 2021).
Nursing homes can be challenging places to work, with staff citing workforce shortages and time pressures as the key sources of stress (Brophy et al., 2019). Research reveals that staff who self-report that they have abused a nursing home resident characterize themselves as “emotionally exhausted” (Yon et al., 2019). Thus, it is important to focus on staffing and staff competence as part of elder abuse prevention strategies. This includes training on identifying abuse and risk factors, effective communication
___________________
16 Consumer organizations have been quick to warn consumers that “the absence of an abuse icon on Nursing Home Compare does not necessarily indicate the absence of abuse,” noting, “Federal reports over the last few decades have documented that state survey agencies (health inspectors) have missed problems and failed to cite violations. Moreover, violations indicating the existence of abuse or potential abuse may be cited under other federal tags, resulting in their exclusion from this initiative” (CMA, 2019).
and teamwork, creating a work environment that encourages and supports openness and discussion of challenges, and implementation of a person-centered care approach (Braaten and Malmedal, 2017).
Improvement strategies derived from the culture change model for nursing homes (see Chapter 4 and later in this chapter) have been proposed as effective approaches to reduce elder abuse in nursing homes. Characterized by the core elements of staff empowerment, consistent staff assignment, resident-directed care and activities, decentralized decision making, and the creation of home-like living environments, culture change is viewed as an effective approach for promoting the safety of residents (Berridge et al., 2019). The delivery of person-centered care, a hallmark of the model, can ensure that the resident feels seen and recognized by staff as a person (rather than staff focusing on their medical condition or disease state), which can help support stronger bonds between staff and residents (Braaten and Malmedal, 2017).
Successful approaches to intervening in resident abuse incidents, particularly resident-to-resident aggression, include the development of inter-professional protocols with clinical staff in the nursing home for dealing with such situations (Bonifas, 2015). Research has shown that nurse–social work collaborative teams are an effective staffing approach with which to address elder abuse (Bonifas, 2015). Preventive measures to reduce resident-to-resident aggression include preadmission screening for aggressive behaviors, the development of a person-centered approach to providing care based on the screening assessment, and an intentional (in other words, nonrandom) approach to roommate selection (Bonifas, 2015). Other potential approaches to reducing elder abuse include consistent assignment (discussed in Chapter 5), which involves a resident receiving care from the same nursing assistants, who would know the resident well and be more aware of any changes in condition that might be related to potential instances of abuse.
Interventions designed to address residents’ aggressive behavior toward staff include training programs such as Bathing Without a Battle, which has been found to be an effective means of improving the bathing experience of residents with dementia in nursing homes (Gozalo et al., 2014). Other interventions include creating awareness on the part of staff as to which residents should not interact during mealtimes or activities; distraction of residents who show escalating aggression; and mediating disagreements among residents to ensure they do not lead to aggressive behavior. Further study is needed to prevent resident abuse of staff and the negative impact on residents and on staff safety, job satisfaction, morale, and turnover (Lachs et al., 2013).
One potential intervention to detect and prevent elder abuse that has become increasingly common is the deployment of surveillance cameras in nursing homes. Seven states have enacted legislation to permit private
individuals to use cameras in residents’ room in nursing homes, and other states have proposed similar legislation (Levy et al., 2019). The use of cameras carries with it serious ethical concerns and risks to residents as well as nursing home staff members. For residents, concerns include the impact on residents’ privacy and dignity, whereas for staff the concerns focus on whether cameras may undermine workers’ sense of being responsible for the residents (Levy et al., 2019).
Despite enactment of legislation allowing the use of cameras and the associated ethical and legal concerns (e.g., privacy, dignity), research is limited as to the prevalence, efficacy, or effects of the use of cameras in nursing homes (Berridge et al., 2019). Nursing homes are both places of work and places where people live, and as such they “are a complex space for regulating privacy because they are simultaneously public and private spaces” (Berridge et al., 2019).
Elder abuse prevention strategies need to include efforts on a broad societal level using public awareness campaigns to elevate the importance of understanding and recognizing the dangers of elder abuse. World Elder Abuse Awareness Day, for example, is recognized internationally and serves as a global platform to call attention to the problem (NCEA, 2021b). Another public awareness effort is the National Council on Elder Abuse’s Reframing Elder Abuse Project.17
It is clear that a constellation of measures will be needed to combat elder abuse. These range from high-quality research to identify the most effective prevention strategies to staff training and education about effective clinical interventions, the implementation of the culture change model for nursing homes, and creating public awareness of the problem of elder abuse more broadly.
Care Transitions
Many nursing home residents have multiple, complex medical conditions and require transitions between the nursing home and the hospital. Poor communication between nursing homes and hospitals is one of the key barriers to safe and effective care transitions (Gillespie et al., 2010). Nine out of 10 nursing home residents arrive in the emergency department (ED) missing critical patient information—such as medication lists and reason for transfer to the ED—necessary to provide safe and efficient care (Terrell and Miller, 2006). Poor-quality communication has also been shown to impact resident care when residents are discharged from the hospital with poor-quality information about ED diagnosis, tests and treatments provided, and
___________________
17 For more information, see https://ncea.acl.gov/resources/reframing.aspx (accessed November 3, 2021).
treatment recommendations (Terrell and Miller, 2006). Missing, inaccurate, or conflicting information is a key barrier to effective transitions between nursing homes and hospitals, which contribute to the risk of rehospitalization and inappropriate care for residents (King et al., 2013).
Research highlights the importance of high-quality communication among health care professionals including effective use of EHRs as well as in-person communication to facilitate care transitions (Scott et al., 2017). The use of EHRs in nursing homes is discussed further in Chapter 9 of this report.
Infection Control
A major patient safety concern in nursing homes is infections, with nearly 2 million infections occurring in nursing homes each year (Mody et al., 2015; Montoya et al., 2016; Strausbaugh and Joseph, 2000). Urinary tract infection (UTI) is one of the most common infections among nursing home residents, with many UTIs associated with the use of catheters (Dwyer et al., 2013; Mody et al., 2017). Diagnoses of UTI among nursing home residents present specific challenges as older adults with a UTI may show signs of confusion or agitation rather than pain (Wegerer, 2017). This is particularly problematic for nursing home residents with dementia as signs of confusion and agitation may be interpreted to be related to their dementia or advanced age rather than an indication of a UTI (D’Agata et al., 2013; Hodgson et al., 2011). Moreover, many illnesses present with similar symptoms to UTI and residents with dementia may not be able to verbalize their symptoms. These challenges often lead to diagnostic errors as well as misuse of antimicrobials (D’Agata et al., 2013; Mitchell, 2021).
CMS expanded infection control conditions for nursing homes in its updated 2016 requirements.18 Existing and updated federal requirements were designed to address a broad range of issues in nursing homes, including strict infection control needs during food preparation, housekeeping, and daily care; influenza prophylaxis, surveillance, and response; norovirus prevention and response; Clostridioides difficile detection and response; surveillance for rare but potentially deadly outbreaks such as legionella pneumonia and Candida auris; potentially inappropriate overuse of antibiotics for such diagnoses as viral bronchitis and asymptomatic bacteriuria; and the growing prevalence of colonization with and infection by multidrug-resistant organisms (Jump et al., 2018; Montoya and Mody, 2011; Strausbaugh et al., 2003).
___________________
18 CMS Requirements for Long Term Care Facilities—Infection Control, 42 CFR § 483.80 (2016).
Lack of Expertise in Infection Control Practices
Infection control has been a long-standing requirement of nursing homes and an area in which many shortcomings were noted by state survey agencies well in advance of the COVID-19 pandemic. Among the new 2016 federal requirements, which were to be implemented over a 2-year period (2017–2019), nursing homes were directed to initiate antibiotic stewardship programs; develop policies and procedures related to identification, reporting, investigation, and control of communicable diseases and infections among residents, staff, and visitors; and employ a staff member who is an infection preventionist. CMS and the Centers for Disease Control and Prevention (CDC) developed a free online training program for infection preventionists in March 2019 to assist nursing homes to prepare for this new staff position (CMS, 2019a). (See Chapter 5 for discussion of the infection preventionist role in nursing homes.)
Given the relatively recent implementation of the new requirements, most nursing homes were unprepared to deal with the wave of infections from the novel coronavirus. Studies found that nearly 75 percent of facilities did not have adequate staffing or infection control measures in place prior to the pandemic (Chapman and Harrington, 2020; Geng et al., 2019). Indeed, GAO found that 82 percent of nursing homes had deficiencies in infection prevention and control between 2013 and 2017; infection prevention and control was the most common reason for deficiencies cited by nursing home surveyors prior to the pandemic. Moreover, approximately two-thirds of nursing homes with infection prevention and control deficiencies had been cited multiple times (GAO, 2020). A 2020 Kaiser Health News analysis found that even among five-star facilities (see Chapter 3 for more on the CMS star rating system), 4 in 10 have been cited for infection control deficiencies (Rau, 2020).
The COVID-19 pandemic was unprecedented in scope and overwhelmed all sectors of the health care system. Nursing homes have increasingly been identified as high-risk settings for the transmission of infectious diseases, and this was confirmed by the devastating impact of the pandemic. The extremely high mortality levels among nursing home residents and staff during the early phases of the public health emergency underscored the extent to which the lack of robust infection prevention and control programs rendered nursing homes extremely vulnerable in the face of a highly transmissible novel pathogen (Andersen et al., 2021). High rates of transmission of the virus were facilitated by the composition of the resident population, which included large numbers of chronically ill, often immunocompromised individuals as well as the physical design of nursing homes: congregate living in multiple-occupancy rooms and with multiple-user bathrooms. Moreover, residents are brought together regularly for congregate indoor meals and activities, and multiple staff have very close contact with residents multiple times a day (Ouslander and Grabowski, 2020).
The pandemic revealed that there was a significant lack of the expertise and experience in infection control practices necessary to limit the introduction and spread of the coronavirus within nursing homes. While nursing homes are required to assign an individual staff member to infection control, this was not typically a full-time position; persons with infection control responsibilities had many other responsibilities as well (Andersen et al., 2021).19 Efforts to isolate or group those infected or quarantine those exposed were often delayed or inadequate and sometimes nonexistent, resulting in rapid spread of the virus throughout facilities (Blain et al., 2020; Giri et al., 2021).
During the early phases of the pandemic, nursing homes’ attempts to contain the spread of the SARS-CoV-2 virus occurred against the backdrop of a lack of prioritization of nursing homes in federal and state responses to the pandemic (Laxton et al., 2020). While CMS, CDC, state departments of health and human services, and provider organizations issued infection-control guidance, the volume and frequently changing nature of the guidance posed significant challenges to nursing home administrators and directors of nursing who struggled to interpret, keep up with, and adapt to the latest guidance. Quality Improvement Organizations have historically lacked both the resources and the expertise to provide assistance to nursing homes to address quality problems, which was made clear during the pandemic (GAO, 2007; Harrington et al., 2017; IOM, 1986; Laxton et al., 2020; Musumeci and Chidambaram, 2020; Spanko, 2020). Assistance often came instead from either local hospital-affiliated health systems or from county or state health departments (Laxton et al., 2020).
The federal government, states, and localities deployed strike teams20 and, in some cases, the National Guard to provide assistance to nursing homes to handle infection prevention and control (Andersen et al., 2021; CMS, 2021). In addition, the Institute for Healthcare Improvement,21 PHI,22 and the Agency for Healthcare Research and Quality’s Nursing Home COVID-19 Action Network23 provided useful resources to bolster nursing homes’ responses to the pandemic. CDC published guidance on
___________________
19 CMS Requirements for Long Term Care Facilities—Infection Control, 42 CFR § 483.80 (2016).
20 Federal strike teams deployed nationally to assist nursing homes with significant COVID-19 outbreaks consisted of infection prevention specialists, epidemiologists, Public Health Service officers from CDC, CMS, and the Office of the Assistant Secretary of Health, while local and state public health officials joined when available. In addition, a number of states created state strike teams to provide support to nursing homes (Andersen et al., 2021).
21 For more information, see http://www.ihi.org/Topics/COVID-19/Pages/default.aspx (accessed November 3, 2021).
22 For more information, see https://phinational.org/ (accessed November 3, 2021).
23 For more information, see https://www.ahrq.gov/nursing-home/index.html (accessed November 3, 2021).
antibiotic stewardship (CDC, 2020) and developed a 20-hour training course for infection preventionists (CDC TRAIN, 2020).
Inadequate Supply of PPE
Adequate access to personal protective equipment (PPE)—including masks, gowns, goggles, gloves, and hand sanitizer—did not exist early in the pandemic (McGarry et al., 2020). In addition, nursing home staff were not adequately trained in the appropriate use of PPE. Staff had not been fit-tested for use of N95 respirators or trained in their appropriate use, nor were they trained in the correct donning and doffing of PPE, including gowns, gloves, and respirators or masks, or in which PPE to use in which situations (Denny-Brown et al., 2020; GAO, 2020). One report indicated that as late as August 2020, shortages of PPE, including N95 respirators and medical gowns, had actually intensified rather than diminished. Nearly half of all nursing homes reported that they had less than a week’s supply of at least one type of PPE at some point between May and August 2020. A week’s supply of PPE is considered the minimum acceptable amount and less than that is considered a “critical shortage”; however, during a major infectious disease outbreak, a nursing home can use up that limited supply in a day or two and should ideally have access to much more (Murray and Friedman, 2020). Another study also found more than one in five nursing homes reported severe PPE shortages of less than a 1-week supply in July 2020 (McGarry et al., 2020). The severe shortages represented “an extremely limited capacity to respond to a COVID-19 outbreak” (McGarry et al., 2020, p. 1813). The CMS Coronavirus Commission on Safety and Quality in Nursing Homes recommended that nursing homes procure and sustain a 3-month supply of PPE, working with federal and state agencies to ensure adequate supply of PPE for nursing homes (MITRE, 2020). One nursing home resident’s perspective on the impact of PPE shortages is provided in Box 6-3.
Access to Testing and Timeliness of Results
Early in the pandemic, when availability of testing was very limited, nursing homes depended on symptom screening of staff and residents to protect residents from infection. Unfortunately, symptom screening alone did not identify many of those who were infected and able to transmit the virus. The testing of staff was as important as testing of residents. Staff often were exposed to people infected with the virus in the community, because of their need to use public or shared transportation, because their low wages often led them to work more than one job, and because they and others near them were unable to self-isolate and work from home by the very nature of their jobs (Denny-Brown et al., 2020; Shen, 2020; True et al., 2020).
Another factor that contributed to the rapid transmission of the virus in nursing home settings was the delay in recognizing the importance of asymptomatic infection in disease transmission, with early reports claiming that there was little or no asymptomatic transmission of the virus (CNBC, 2020). It has now been well documented that asymptomatic or presymptomatic infection was often the way the virus was introduced into, and spread within, nursing homes. Overall, inadequate access to testing for COVID-19 to identify those infected, either residents or staff, whether symptomatic or asymptomatic, limited nursing homes’ ability to effectively contain the spread of the virus (Ouslander and Grabowski, 2020). The amount of time between COVID-19 testing and results proved to be a significant issue during the pandemic. According to one study, 6 months after the first COVID cases in U.S. nursing homes, less than 15 percent of staff and 10 percent of residents experienced a test turnaround time of less than 1 day (McGarry et al., 2021). Timeliness of receipt of test results is critical to containing the viral spread in both nursing homes and the community (McGarry et al., 2021).
Lockdown of Facilities as Infection Control Response
In an effort to protect residents and staff, in March 2020, CMS directed nursing homes to severely limit or not allow any visitation from family members and loved ones, with a significant impact on residents in the form of social isolation and loneliness (discussed in Chapters 2 and 8). The importance of telehealth and other technologies to help combat social isolation among nursing home residents is discussed in Chapter 9. Moreover, many families of nursing home residents found communication of information concerning COVID-19 infections in the facilities to be inadequate (Hado and Friss Feinberg, 2020; HRW, 2021; National Consumer Voice, 2021). Some states have considered ways to ensure that such isolation does not occur in future public health emergencies (Jaffe, 2021).
One strategy to strengthen infection control in nursing homes in the future would be to address the training requirements and accountability of nursing home infection preventionists as specified in the 2016 updated requirements (Stone et al., 2018). Other potential strategies include encouraging nursing homes to form alliances with hospital-based infectious disease specialists; strengthening infection and antibiotic reporting requirements, including having regular feedback comparing performances of nursing homes with their peers and requiring influenza and coronavirus immunizations for staff (Pugh, 2020); and requiring an increased role for local and state health departments in assisting with nursing home infection control (CMS and CDC, 2020; Laxton et al., 2020).
NURSING HOME EMERGENCY PLANNING, PREPAREDNESS, AND RESPONSE
Another vital safety-related challenge for nursing homes that was revealed in the starkest of terms during the pandemic is planning, preparing, and implementing an effective response to a wide array of public health emergencies to protect residents from harm while also ensuring that residents are cared for during and after an emergency (Powell et al., 2012). The 2016 CMS Medicare and Medicaid requirements for participation (discussed in more detail in Chapter 8) require long-term care facilities to maintain a comprehensive emergency preparedness program, based on a thorough risk assessment, with written policies and procedures in place specific to their population.24 Additionally, regulations expanded emergency plan requirements to consider items such as sewage disposal, supplies, emergency lighting, and evacuation procedures with a resident/staff tracking system, and more.25 Beyond having such written plans in place, nursing home staff need to review and audit the plans on a regular basis to ensure that the plans are robust, that nursing home staff can locate supplies, and that there is accurate documentation of participation in emergency management planning discussions and exercises.
Frequent life-threatening events ranging from the COVID-19 pandemic to weather-related disasters such as hurricanes, tornadoes, floods, and wildfires clearly underscore the urgent need for nursing homes to plan and prepare for a broad range of public health emergencies. Weather-related emergencies, with their associated damage resulting from strong winds and flooding, have had a devastating impact on the staff and residents of nursing homes and resulted in higher rates of morbidity, mortality, and
___________________
24 CMS Requirements for Long Term Care Facilities—Emergency Preparedness, 42 CFR § 483.73 (2016).
25 Ibid.
hospitalization than among other members of the community (Lane and McGrady, 2018). Thus it is essential for nursing homes to prepare for serious weather events most likely to occur in the part of the United States in which they are located (i.e., hurricanes on the East Coast, tornadoes in the Midwest and South, severe snowstorms in the West and Midwest, floods in sites near rivers and lakes, and drought-fueled wildfires on the West Coast).
Although evacuation is a significant risk for nursing home residents, who tend to be frail, have multiple medical conditions, and become disoriented in new surroundings, evacuation may still be necessary when disasters pose an immediate risk to a facility and its residents (Brown et al., 2012; Cacchione et al., 2011). Experience during disasters such as hurricanes Katrina, Sandy, and Ida, for example, revealed that nursing home facilities often lacked clear guidance for evacuation procedures, despite calls by experts to develop flexible planning and protocols (IOM, 2012; Powell et al., 2012). Nursing homes house distinct vulnerable populations, such as those with cognitive impairments, vision and hearing impairments, and disabilities, which require specific evacuation planning considerations (Hyer et al., 2010; IOM, 2012).
Research emphasizes the importance of nursing home staff training in psychological first aid (PFA) and general emergency preparedness. Local emergency management’s review of nursing home facilities’ emergency plans has also been found to be critical. One study indicated that nursing homes may consider including some residents in emergency preparedness staff training efforts (Pierce et al., 2017).
Studies have noted that during disasters and emergencies the emphasis is on physical safety and provision of medical care, and not on nursing home residents’ mental health needs. PFA was developed in response to residents’ needs immediately following a disaster to reduce distress and promote residents’ ability to function. PFA does not require a highly trained licensed mental health provider, and nursing home staff could be trained to provide such care (Brown et al., 2009). The availability of PFA operating manuals for nursing home staff has contributed to the broad application of PFA as an effective tool for disaster intervention (Wang et al., 2021).
Including Nursing Homes in Federal Emergency Preparedness and Response
The Federal Emergency Management Agency (FEMA), an agency of the U.S. Department of Homeland Security, is responsible for the coordination of federal government resources to ensure that communities are prepared for, and capable of effectively responding to, disasters (FEMA, 2021). To facilitate coordination of resources, FEMA created the National Response Framework, which provides an overarching organizational structure for
15 emergency support functions (ESFs) ranging from transportation and communication, firefighting, and search and rescue to public safety and security. The ESFs specify the most critical resources and capabilities needed to respond to a national emergency (FEMA, 2020).
ESF 8 includes specific considerations related to public health and medical services in the context of federal emergency support, and it provides a mechanism for the coordination of federal assistance to support state, tribal, and local officials in response to a disaster, emergency, or incident that may lead to a public health, medical, behavioral, or human service emergency (FEMA, 2016a). ESF 8 outlines the federal government’s role in coordinating public health infrastructure and health care delivery to minimize or prevent health emergencies. The Department of Health and Human Services (HHS) coordinates ESF 8 through the Assistant Secretary for Preparedness and Response (ASPR). Core functions that ESF 8 supports include26
- Public information and warning (e.g., coordinating public health messaging);
- Critical transportation (e.g., resources to assist the movement of at-risk/medically fragile populations to shelter areas);
- Mass care services (e.g., technical expertise and guidance on the public health issues of the medical needs population, advocacy services, etc.); and
- Public health, health care, and emergency medical services (e.g., health surveillance, triage in the event of a health care surge, assessment of the public health needs of a health care system or facility, technical assistance, etc.) (FEMA, 2016a).
In addition, ESF 15—external affairs—requires government, community organizations, and private-sector authorities to provide accurate, coordinated, timely, and accessible information necessary to develop, coordinate, and deliver messages in the event of an emergency to affected audiences, including the media and local populations. The Department of Homeland Security works closely with HHS as the respective leads for ESF 8 and ESF 15 during a public health emergency (FEMA, 2016b).27
The key focus of ESF 8 is on supporting the response to public health and medical disasters. For example, resources for patient care during public health and medical emergencies are directed to “support prehospital triage and treatment, inpatient hospital care, outpatient services,
___________________
26 For a complete list of the core capabilities of ESF 8, see FEMA (2016a).
27 For a complete list of core capabilities of ESF 15, see FEMA (2016b).
behavioral healthcare, medical-needs sheltering, pharmacy services, and dental care to victims with acute injury/illnesses or those who suffer from chronic illnesses/conditions” (FEMA, 2016a). ESF 8, however, does not specify nursing homes among the list of facilities, nor does it designate nursing home residents and staff as a specific vulnerable population. Similarly, ESF 15 also does not specifically include residents of nursing homes in the list of community members (FEMA, 2016b). Clarification of nursing homes in the list of community members is particularly relevant given the inclusion of behavioral health care among the list of services, in light of the prevalence of behavioral health needs among nursing home residents (discussed in Chapter 4) and the importance of providing PFA to nursing home residents in the aftermath of an emergency, as discussed above.
The devastating impact of COVID-19 on nursing home staff and residents described above demonstrates the urgent need to explicitly ensure that long-term care settings such as nursing homes are included in the broad range of emergency planning, preparedness, and response activities for health care settings similar to what is done for acute-care settings. In order to ensure the same level of preparedness and response accorded other health care settings, it is critical to include nursing homes explicitly in federal emergency response protocols, such as ESF 8 and ESF 15.
Partnering with Local and State Emergency Management and Public Health
As discussed above, nursing homes have not been well integrated into federal planning and response efforts. For example, a lack of federal–state integration left individual states responsible for PPE distribution resulting in wide variation in the prioritization and inclusion of nursing homes to receive supplies (Abbasi, 2020; Cohen and Rodgers, 2020; McGarry et al., 2020; Murray and Friedman, 2020). This is also the case for state and local disaster planning and response efforts (Hyer et al., 2010). A federal program, the Hospital Preparedness Program (HPP),28 directed by ASPR, provides financial support to states, localities, and territories to develop regional coalitions of health care organizations that collaborate on emergency planning, preparedness, and response. Regional coalitions are required to include at least two acute care hospitals, emergency medical services, emergency management, and public health agencies. On average, nearly 90 percent of hospitals belonged to a health care coalition in 2017; in 17
___________________
28 See https://www.phe.gov/Preparedness/planning/hpp/Pages/default.aspx (accessed February 4, 2022).
states every hospital was a member of a coalition. An OIG report called on ASPR to encourage those who receive HPP funding to “prioritize exercises for communities and health care coalitions that include hospitals, long-term care facilities, EMS, emergency management, public health, and other essential partners” (OIG, 2014b, p. 22).
Improved coordination with emergency management officials across all levels could enhance the effectiveness of nursing home emergency planning and preparedness (Lane and McGrady, 2016). It is essential that nursing homes be included in state and local emergency planning sessions and drills. Ideally, these state and local agencies would have staff members with expertise, knowledge, and training in long-term care populations and programs. Forging effective partnerships with local emergency management is particularly critical to establishing evacuation standards, plans, sites, and routes as well as ensuring that the nursing home facility is aware of the most up-to-date state and local emergency planning regulations (Andersen et al., 2021; Casey et al., 2020; Lane and McGrady, 2016, 2018; OIG, 2012; U.S. Senate Committee on Finance, 2018).
In addition to coordinating with emergency management for disaster planning, preparedness, and response, nursing home emergency planning efforts should be integrated with those of local public health and local health care facilities for infection control, the need for which was made clear during the COVID-19 pandemic (Andersen et al., 2021; Powell et al., 2012). State and local public health departments, including State Health Department health care–associated infection programs first established in 2009, serve as vital partners for providing technical assistance, education, and training to nursing homes on infection prevention and control (Andersen et al., 2021). Moreover, as discussed above, shortages of essential supplies, such as PPE, for nursing homes during the pandemic underscores the importance of ensuring nursing homes are included in federal and state emergency planning, preparedness, and response measures and initiatives.
Public health plays other key roles during emergencies, providing necessary resources as well as essential expertise concerning food safety, environmental protection, and infection control. Health care facilities will be stressed during emergency events and thus limited in their ability to care for additional patients. Nursing home planning and preparedness efforts therefore need to be closely coordinated with those of public health departments, health and social care organizations, and other health care facilities and emergency services. In this way, an integrated network of care among hospitals, nursing homes, and local and state community services can be established to ensure that nursing home residents’ health care needs can be met during emergencies (Harnett et al., 2020).
THE PHYSICAL ENVIRONMENT
The physical environment of the nursing home plays a crucial role in supporting resident health and function, promoting quality of life, enabling staff to provide needed care, and supporting family satisfaction (Wood et al., 2020). Due to the unique dual role of nursing homes as places to live as well as sites in which care is provided, increased attention is being paid to ways to create a nursing home environment that is more like home rather than a health care institution in which people also happen to live (van Hoof et al., 2016a). Indeed, the degree to which residents feel at home may be critical to the success of providing person-centered care and may contribute to the overall quality of care in nursing homes (Edvardsson et al., 2010; van Zadelhoff et al., 2011). Moreover, COVID-19, with its associated disease incidence and visitor/group gathering restrictions, has underlined the importance of the particular design of the nursing home physical environment for resident well-being and quality of life (Anderson et al., 2020).
Key elements of the physical nursing home environment include sensory-related elements such as light, sound, odor, and touch; air flow and temperature control; environmental aspects specifically related to personal care provision and staff function; the building’s overall design; room layout and configuration; and indoor and outdoor spaces. These aspects of the physical environment are important to consider in constructing, renovating, and evaluating nursing homes and in planning the nursing home of the future, and are discussed further below.
Sensory-Related Elements of the Physical Environment
It is through the senses of sight, hearing, smell, taste, and touch that one experiences and communicates with the world. Those experiences can be pleasant or unpleasant, depending on how sensory stimulation is provided and regulated. Many nursing home residents have limitations or needs related to one or more senses, and those needs will vary depending on the individual. Therefore, support for positive sensory perception and minimization of unpleasant sensory experiences are critical elements of quality nursing home environments, as summarized in Table 6-2 below.
Building Layout
Many nursing homes were developed using design features adapted from hospitals constructed in the 1960s and 1970s (Eijkelenboom et al., 2017; Schwarz, 1997). These features, which include large units with long corridors, large activity and dining spaces, shared rooms and bathrooms,
TABLE 6-2 Importance of Sensory Perceptions in the Nursing Home Setting
| Sense | Key Issues to Consider for Sensory Perceptions in the Nursing Home Setting |
|---|---|
| Sight | Lighting design issues in nursing homes are complex because common aging changes in the eye cause older persons to need higher light intensities, while at the same time they are also more sensitive to glare and to differences in the consistency of lighting. For this reason, lighting design must take many factors into consideration, including |
| The use of indirect rather than direct lighting sources, including overhead illumination and diffusers for skylights. | |
| The promotion of evenness of lighting within rooms, such as by having daylight sources from more than one side of a room, to achieve a ratio no larger than 3:1 from lightest to darkest areas of a room. | |
| Adequate illumination in bedroom task areas for reading. | |
| Design features and policies that reduce glare, for example, from shiny floor surfaces and lighting fixtures. | |
| Full-spectrum bright light during the day (ideally by exposure to direct or indirect sunlight) to entrain circadian systems, improving sleep and possibly relieving depression. | |
| Motion-activated systems to provide illumination for nighttime activity, including trips to the bathroom, thereby helping promote safety and prevent falls. | |
| Sound | Most nursing home residents have some degree of hearing loss, including aging-related changes that impair speech discrimination and increase sensitivity to background noise. Noise is common in many nursing homes, due to environmental factors such as poor sound absorbency of surfaces; loud sounds generated by staff communication, meal service, housekeeping, and maintenance; resident vocalization; electronic systems such as televisions, radios, and computers; and alarms. Unwanted noise can reduce sleep and increase agitation, and desired sounds (such as personalized music) can enhance the quality of life. |
| Issues to consider in providing optimal sound stimulation include | |
| Smaller nursing home functional units, such as wards and common areas, as noise increases with the number of residents and staff. | |
| Private bedrooms, which eliminate distracting sounds of roommates and their care. | |
| Noise-absorbent materials on walls and ceilings of common rooms and hallways. | |
| Policies and procedures that limit loud staff communication. | |
| Use of headphones or other personal communication/listening devices by residents with significant hearing impairment when individualized activities, including resident–staff communication, take place in common areas. | |
| Touch | Many nursing home residents have mobility issues that confine them largely or wholly to beds and chairs, often resulting in them remaining in the same place for hours or longer. In addition, conditions such as advanced dementia, visual impairment, and hearing loss mean that awareness of the immediate environment is mainly by touch. Many residents with significant mobility limitations are unable to reposition themselves when they are uncomfortable, placing them at risk not only for chronic discomfort but also for skin breakdown and pressure ulcers. Among the issues to consider are |
| Different individuals can have widely different preferences in terms of ambient temperature; individual room thermostats are an important element of person-centered care. |
| Bed, wheelchair, and other seating surfaces play an important role in a resident’s physical comfort. Cushioning designed to provide comfort, facilitate positioning, and prevent pressure ulcers are essential for persons with mobility limitations. | |
| Exposure to sunlight, soft blankets, pets (if desired), and other pleasant and stimulating tactile sensations can add to a resident’s quality of life. | |
| Smell | The reduction and elimination of noxious odors is an elementary element of nursing home quality. Beyond the absence of negative odors, environmental quality should provide access to pleasantly stimulating odors as well. |
| Examples include | |
| Cooking-related odors, such as bread baking or brewing coffee. | |
| Fresh flowers. | |
| Aromatherapy with scents that have been associated with positive impact on mood, such as lavender in relieving anxiety. |
SOURCES: Dichter et al., 2021; Donelli et al., 2019; Figueiro et al., 2014; Forbes et al., 2014; Hickman et al., 2007; Joosse, 2011; Martin and Ancoli-Israel, 2008; Meyer et al., 1992; Riemersma-van der Lek et al., 2008; Schnelle et al., 1999; Sloane et al., 2002, 2007a; Wu et al., 2015.
and lack of ready access to outdoors (Brawley, 2005; Eijkelenboom et al., 2017), are now considered to be detrimental to the residents’ quality of life, infection control, and effective staff function in caring for nursing home residents. Newer evidence and experience-based principles of environmental design for older persons have led to the identification of a range of best practices for optimal nursing home design, which are described below.
Air Flow and Filtration
The COVID-19 pandemic has led to building designers giving much greater consideration to the role that air flow and filtration can play in minimizing the cross-contamination of aerosolized droplets that can occur through stagnation in public areas and transmission through ventilation systems. Moreover, there is a greater interest in filtration systems that can capture and eliminate aerosolized viral particles from circulation.
The need to care for residents with active, airborne/droplet infections such as COVID-19 in the nursing home setting has raised the possibility of mandating that nursing homes have some negative pressure rooms, with separate systems to ventilate air outdoors to the facility roof. Lessons learned through the COVID-19 experience underscore the importance of incorporating new air circulation standards in future nursing home design (Lynch and Goring, 2020; Reiling et al., 2008; TROPOS, 2020). Consideration should also be given to the use of air cleaners with upper-room ultraviolet disinfection and air purifiers with high-efficiency particulate
absorbing filters as an additional measures, though with the understanding that such purifiers cannot replace the supply of fresh air (TROPOS, 2020; University of Nebraska–Lincoln, 2021).
Facilitation of Staff Activity
The design of a nursing home should also consider issues related to staff convenience and function, such as ensuring ready access to supplies by locating supply closets close to areas where the supplies will be used and by placing personalized resident supplies and, when possible, medications in locked cabinets in resident rooms. In addition, the design layout should include attention to incorporating enhanced infection control practices (e.g., accessible handwashing stations for staff that are integrated with workflow and the use of bacterial resistant surfaces and improved waste disposal). Furthermore, it is important to design bathing areas that facilitate resident transfer and care, prevent infection, keep residents warm, and do not overheat staff (Sloane et al., 1995, 2007b). Moreover, resident monitoring devices, such as motion sensors in bedrooms, are important possibilities to consider as a way to facilitate staff activity (Woodbridge et al., 2018).
Access to Outdoors
Ready access to safe, stimulating outdoor space is important to residents’ health and quality of life, but most nursing homes do not provide this amenity (Cutler and Kane, 2006). The average nursing home resident spends little if any time outdoors, even in good weather, despite evidence that exposure to sunlight can raise vitamin D levels, promote better sleep, and improve one’s mood (van den Berg et al., 2019). Well-designed outdoor spaces provide opportunity for activities that promote dignity and important personal expression for many older persons (Connell et al., 2007; Martin and Ancoli-Israel, 2008; Sandvoll et al., 2020). Barriers to the use of outdoor space include the nontherapeutic design of many outdoor spaces, difficult access to the outdoors, the need for most residents to have staff or family assistance when they are outdoors, and the need for staff to plan and conduct or monitor activities outdoors. For nursing homes located in areas where the weather presents a barrier to outdoor activities, interior designs should include windows, not only to ensure a sufficient amount of natural light, but also to enable residents to experience the outdoors visually.
Given the important association between access to the outdoors and residents’ health, the thoughtful design of outdoor space is an important element of nursing home planning, construction, and use (van den Berg et al., 2019).
Important elements of outdoor space design for nursing homes to consider include
- One outdoor area for each functional unit of the nursing home, both for infection control and to facilitate the oversight of residents;
- Ready access to outdoor space on the ground level, without locks or thresholds, and with easy doorway visibility for residents and ability of staff to monitor the activity of residents from common areas;
- Security by way of a safe, visually appealing barrier at the limits of the area;
- Circular paths to facilitate movement;
- Plantings that are visually pleasant, provide visual and olfactory stimulation, and are nonpoisonous;
- Areas that provide sun and areas that provide shade, with seating availability in each; and
- Opportunities for visual stimulation and activity, such as raised and ground-level gardens, bird feeders, whirligigs, and space for outdoor games (van den Berg et al., 2019; Wrublowsky, 2018).
Private Rooms and Bathrooms
Having one’s own private bedroom and bathroom is important for addressing nursing home residents’ needs such as privacy, dignity, relationship considerations (e.g., family visitation), and sensory control (e.g., temperature and television noise). It also provides private space for personal expression (e.g., a resident’s own furniture and mementos or intimate interactions) (Calkins and Cassella, 2007; Nygaard et al., 2020; van Hoof et al., 2016b). A large body of research has demonstrated the benefits of single occupancy rooms in terms of patient safety, effectiveness and quality of care, and promotion of person-centered care. Private rooms have been shown to reduce the risk of acquiring and spreading infections in hospital settings (Chaudhury et al., 2004; Cohen et al., 2017; Munier-Marion et al., 2016; Stiller et al., 2016; Zhu et al., 2022). Research also shows that single rooms are associated with improved sleep patterns and reduced agitation in people with dementia, fewer medication errors, and fewer adverse outcomes in hospitals (Silow-Carroll et al., 2021). Moreover, research has revealed higher resident satisfaction and family preference for single occupancy rooms (Nakrem et al., 2013; Nguyen Thi et al., 2002; Reid et al., 2015). Overall, the benefits of private rooms include shorter hospital stays, greater privacy for the patient, reduced noise levels and traffic in and out of patient’s rooms, contributing to reduced stress on the part of patients, and space for family members to visit and support the individual’s healing process (Chaudhury et al., 2004). A family member’s perspective is captured in Box 6-4 below.
Moreover, it is clear from the COVID-19 experience and from research on colonization of multidrug-resistant bacteria that private rooms and bathrooms promote infection control (Brown et al., 2021; Mody et al., 2021; Siegel et al., 2017). On the other hand, a limited number of nursing home residents will prefer to share a bedroom, for example, with a spouse, partner, or close friend. Therefore, while it is better for the residents if most nursing home rooms and bathrooms are private, reserving a small number of double-occupancy rooms for those who prefer to share a room is important. For a family member’s perspective on the importance of having a private room, see Box 6-5.
Impact of the COVID-19 Pandemic and Physical Design of Nursing Homes
The devastating impact of the COVID-19 pandemic on nursing homes, combined with the specific ways in which the physical design of nursing homes facilitated the spread of the virus, has renewed interest in alternative nursing home designs (Sabatino and Harrington, 2021). Many of the recommended features of updated physical environments take into account the factors discussed in the preceding sections of this chapter, including expanded resident living spaces with private rooms and bathrooms, improved ventilation and air circulation, and outdoor areas and room to exercise, along with other physical, environmental, and safety features to improve quality of life for residents (Anderson et al., 2020).
Indeed, the lessons learned during the COVID-19 pandemic, particularly the key factors that contributed to the spread of the virus in nursing home settings, are critical to anyone reimagining nursing homes for the future (see Box 6-6). Central among these factors was the size of the nursing home facility. In 2019, the median capacity of a nursing home facility was 100 beds, although average facility size varied significantly by geographic location as well as by ownership type (MedPAC, 2021; Sabatino and Harrington, 2021). Research has shown nursing home size to be a major predictor of infection rates (Abrams et al., 2020; Figueroa et al., 2020; Harrington et al., 2020; Stall et al., 2020).
Another key factor related to density in facilities is room sharing; most nursing home residents live multi-occupancy rooms, with two to four beds per room and shared bathrooms. Multi-occupancy rooms are standard in nursing homes, as Medicare and Medicaid will only pay for semi-private rooms; residents who want a single room must pay private rates (CMS, 2019b).29 Reducing the density of all resident spaces with spacious living areas and more single-occupancy rooms (even without reducing total capacity and size) has been shown to reduce transmission of infectious diseases, such as COVID-19 (Zhu et al., 2022).
Innovative Physical Design of Nursing Homes
This chapter has discussed key safety and environmental aspects that influence nursing home quality of care and which have a direct impact on residents’ quality of life. The culture in nursing homes has long mirrored an acute-care model in terms of its esthetics, restrictions, and medical focus. Many residents, however, prefer a model that is less institutional and more
___________________
29 CMS Requirements for Long-Term Care Facilities—Admission, Transfer, and Discharge Rights, 42 CFR § 483.15 (2016).
reflective of the homes in which they once lived, which commonly includes private rooms and bathrooms (Roubein, 2021; Waters, 2021). Small-scale30 nursing home environments eliminate disorienting long corridors and large public spaces, reduce unpleasant noise, create a more “home-like” feel, and can promote staff cohesion (Abrams et al., 2020; Kane et al., 2007; Passini
___________________
30 Though there is no formal definition of what constitutes a small nursing home, a common limit is 20 or fewer residents (Sabatino and Harrington, 2021).
et al., 2000; Waters, 2021). Key features in the small household model of nursing home care are depicted in Figure 6-1.
Interest in reconfiguring large, institution-like traditional nursing homes as smaller, more home-like settings is not new; innovative approaches such as the Eden Alternative31 and the Green House Project32 have been around for more than 25 years in this country. As discussed in Chapter 4, creating a more home-like atmosphere is a key element of the culture change movement in nursing homes. For one family member’s perspective on a more home-like atmosphere for nursing homes, see Box 6-7.
Small-scale home-like environments have been developed in other nations, such as the Netherlands, Denmark, and Norway (de Boer et al., 2018; Kane et al., 2007; Rabig et al. 2006; Regnier, 2018; Verbeek et al., 2009; Waters, 2021), as well as “clustered neighborhood designs” where groups of 8–12 residents have their own rooms yet share living and dining space (Eijkelenboom et al., 2017). Other innovative approaches include nursing home models in the Netherlands that serve to bring together both ends of the age spectrum through a combination of child care and long-term care (Werner et al., 2020).
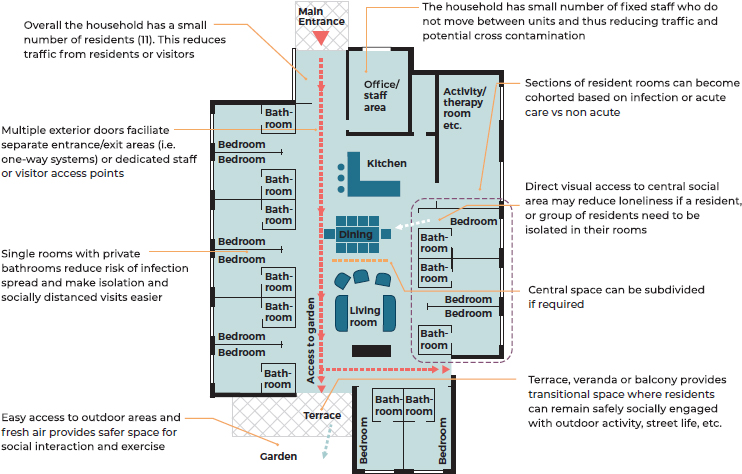
SOURCE: Anderson et al., 2020.
___________________
31 For more information, see https://www.edenalt.org (accessed December 2, 2021).
32 For more information, see https://thegreenhouseproject.org (accessed December 2, 2021).
Another example of an alternate approach to traditional nursing home care that has been in place for nearly 20 years is TigerPlace. Launched in 200433 as a state demonstration project, TigerPlace was designed to maximize older adults’ independence and function throughout the end of life (Lane et al., 2019; Rantz et al., 2008, 2014a).34 Though the main service provided is housing (meals, housekeeping, and maintenance are also included), interdisciplinary professional health care team members (e.g., full-time registered nurses, social workers, licensed practical nurses, certified nursing assistants, and consulting advanced practice registered nurse faculty) provide services to residents. TigerPlace was designed as a “living laboratory” for research and development of a wide range of interdisciplinary innovations, such as evaluation of aging in place and of the effectiveness of care coordination (Rantz et al., 2014b, 2015); the development of technology to enhance aging independently (Mishra et al., 2020; Rantz et al., 2005); environmental sensors to detect early illness, automated fall risk, and fall detection (Skubic et al., 2015; Stone et al., 2015; Su et al., 2018); electronic health record data mining (Mishra et al., 2020; Popejoy et al.,
___________________
33 The passage of state legislation in 1999 and 2001 enabled a facility with apartments to be built to nursing home standards, licensed as an intermediate care facility (facilitating the use of long-term care insurances by residents). TigerPlace operates as independent housing through waivers granted to enable its innovative approach to providing services to older adults.
34 A public–private partnership was formed with Americare Systems, Inc., which built, owns, and operates the housing component, with the care delivery provided by a home health agency of the Sinclair School of Nursing, University of Missouri. For more information, see https://agingmo.com/tiger-place-institute (accessed December 3, 2021).
2015), longitudinal functional health and cost-of-care measurement (Rantz et al., 2011, 2014a); and social engagement or other research activities of interest to older adults, faculty, and students (Demiris et al., 2008, 2009; Galambos et al., 2013, 2019). Evaluations of TigerPlace have consistently shown that residents and families prefer TigerPlace’s innovative approach. Financial analyses reveal that the total cost of care (beginning at the point when residents would qualify for nursing home placement through the end of life) is less than traditional care (Rantz et al., 2011, 2014a).
Redesigning Nursing Home Environments to Support Quality Care
As noted above, a number of innovative models reflect the preference for less institutional, more home-like settings, including Green House homes. Launched in 2003 with initial funding from the Robert Wood Johnson Foundation (RWJF),35 a total of approximately 300 independently owned Green House homes operate in 32 states and serve approximately 3,200 older adults. The large majority of Green House homes—more than 80 percent—are owned by nonprofit companies (Waters, 2021).
Research has identified the benefits of the Green House model as including higher quality of life, lower Medicare spending, and reduced staff turnover as compared with traditional nursing homes (Green House Project, 2012; Waters, 2021). Studies have found that, compared with traditional nursing home residents, those living in Green House homes had lower rates of hospitalization, and were 45 percent less likely to need catheters, 38 percent less likely to have pressure ulcers, and 16 percent less likely to be bedridden (Zimmerman et al., 2016). Earlier studies demonstrated that residents and families were more satisfied with Green House homes than traditional nursing homes (Kane et al., 2007; Lum et al., 2008).
Despite the positive impact they have on a range of resident health outcome measures and the enhanced quality of life they provide, Green Houses represent less than 2 percent of all nursing homes and provide care to less than 1 percent of all nursing home residents. A significant limiting factor is their relatively high costs of construction and operation compared with traditional nursing homes. Although costs vary by location, daily rates in Green Houses range from approximately $250 to $500 per day. Medicaid reimbursement rates for nursing home care vary by state (discussed in Chapter 7), but overall, given the higher costs of Green Houses relative to other nursing home settings, residents tend to be primarily White, middle- or upper-income private paying individuals. This raises equity concerns
___________________
35 RWJF awarded the Green House Project a 5-year, $10 million grant to pay for technical assistance, support for architects, and evaluations (Waters, 2021).
about the ability of individuals on Medicaid to access high-quality care such as that provided in Green House settings (Waters, 2021).
The pandemic highlighted another benefit of the Green Home model in that nursing homes using this model had significantly lower rates of coronavirus infection. The infection rates in large traditional nursing homes (with 50 or more residents) were nine times higher than the rates in Green House nursing homes. The median mortality rate in Green Houses was 24 for every 100 COVID-19 cases, as compared with 80 per 100 cases in small traditional homes and 53 per 100 cases in large traditional nursing homes. The lower rates of COVID-19 cases and mortality among Green House residents were likely due to residents having private rooms and to the fact that fewer people live and work in Green Houses than in traditional nursing homes (Zimmerman et al., 2021).
A range of incentives and supports will be needed to facilitate the shift to smaller, more home-like designs for nursing homes with features that would enhance patient safety by lessening the impact of a future public health emergency, while improving resident quality of life. Transition to a new model of care will require significant financial investment by the U.S. Congress, as well as a number of regulatory changes, including allowing Medicare and Medicaid to pay for private rooms for residents; private rooms are currently only paid for by CMS if deemed medically necessary (CMS, 2019b).
Federal agencies such as the U.S. Department of Housing and Urban Development (HUD), the Internal Revenue Service, and CMS could help promote the development of smaller nursing homes with private rooms by providing incentives for new construction of smaller homes or renovations for smaller units within larger homes (Sabatino and Harrington, 2021). An existing source of financing assistance to support rehabilitation or construction of smaller nursing home facilities is HUD’s Section 232 program, which guarantees mortgages of nearly 2,400 nursing homes across the country.36 HUD has been criticized, however, for inadequate oversight of the program and for discontinuing its physical inspections of nursing homes that received HUD-backed mortgages, many of which have received one- or two-star ratings under the CMS Five Star rating system (Goldstein and Gebeloff, 2019). The U.S. Department of Agriculture operates a loan program to provide affordable financing to develop essential community facilities in rural areas of the country. Funding can be used to purchase, build, or improve community facilities, which include nursing homes.37
___________________
36 See https://www.hud.gov/program_offices/housing/mfh/progdesc/procsec232_223f (accessed February 7, 2022).
37 See https://www.rd.usda.gov/programs-services/community-facilities/community-facilities-direct-loan-grant-program (accessed February 7, 2022).
Clearly, the COVID-19 pandemic has served as the catalyst underscoring the urgency of transforming the nursing home built environment (Werner et al., 2020). The design of nursing homes going forward will need to take into account all the myriad factors discussed in this chapter in order to ensure the highest quality of life for residents and to answer resident, family, and staff safety concerns—on a daily basis as well as in times of future public health emergencies. Such necessary changes will require a collaborative approach that brings together health care leaders, nursing home architects and builders, state and federal agencies, and local communities (Anderson et al., 2020).
KEY FINDINGS AND CONCLUSIONS
- Resident safety is a key aspect of quality of care in nursing homes. Because of the dual role of nursing homes as care settings as well as places to live, nursing homes must balance resident safety with resident autonomy and quality of life.
- Even before the pandemic, infection control issues were the most common reason for citation deficiencies by nursing home surveyors.
- Nursing homes are not well integrated into federal, state, county, and local emergency management planning, preparedness, and response.
- Nursing home emergency management needs to be conducted in partnership with state and local emergency management departments as well as with local public health and health care facilities.
- The physical environment of the nursing home plays a large and important role in supporting or inhibiting resident function and in promoting or detracting from residents’ quality of life. This became particularly evident during the COVID-19 pandemic.
- Features such as large units, long corridors, massive activity and dining spaces, shared rooms and bathrooms, and a lack of ready access to outdoor areas are now considered to be detrimental to resident quality of life, infection control, and effective staff function.
- Small nursing homes had fewer COVID-19 infections and lower mortality compared with nursing homes with 50 or more beds.
- Research demonstrates the positive impact of single occupancy rooms and private bathrooms on resident health, safety, and quality of life. However, CMS does not reimburse for private rooms in nursing homes other than in cases of medical necessity.
- COVID-19 affected high-quality nursing homes as well as low-quality nursing homes. The overwhelming impact of the pandemic on nursing homes shines a light on existing, universal, deep-rooted
- problems that require systemic solutions across the nursing home industry.
REFERENCES
Abbasi, J. 2020. “Abandoned” nursing homes continue to face critical supply and staff shortages as COVID-19 toll has mounted. JAMA 324(2):123–125.
Abrams, H. R., L. Loomer, A. Gandhi, and D. C. Grabowski. 2020. Characteristics of U.S. nursing homes with COVID-19 cases. Journal of the American Geriatrics Society 68(8):1653–1656.
AHRQ (Agency for Healthcare Research and Quality). 2019. Falls. https://psnet.ahrq.gov/primer/falls (accessed February 4, 2022).
American Geriatrics Society. 2019. Updated AGS Beers criteria® for potentially inappropriate medication use in older adults. Journal of the American Geriatrics Society 67(4):674–694.
Andersen, L. E., L. Tripp, J. F. Perz, N. D. Stone, A. H. Viall, S. M. Ling, and L. A. Fleisher. 2021. Protecting nursing home residents from COVID-19: Federal strike team findings and lessons learned. NEJM Catalyst: Innovations in Care Delivery 2(3). https://doi.org/10.1056/CAT.21.0144.
Anderson, D. C., T. Grey, S. Kennelly, and D. O’Neill. 2020. Nursing home design and COVID-19: Balancing infection control, quality of life, and resilience. Journal of the American Medical Directors Association 21(11):1519–1524.
Baker, P. R. A., D. P. Francis, N. N. Hairi, S. Othman, and W. Y. Choo. 2016. Interventions for preventing abuse in the elderly. Cochrane Database of Systematic Reviews 2016(8):CD010321.
Ball, J., and P. Griffiths. 2018. Missed nursing care: A key measure for patient safety. https://psnet.ahrq.gov/perspective/missed-nursing-care-key-measure-patient-safety (accessed February 7, 2022).
Barlas, S. 2012. Medicare wants only ‘independent’ consultant pharmacists in nursing homes. Pharmacy and Therapeutics 37(1):6.
Barlas, S. 2016. Medicare adds new long-term-care pharmacy rules: Agency passes again on pharmacist independence requirements. Pharmacy and Therapeutics 41(12):762–764.
Bateni, H. 2012. Changes in balance in older adults based on use of physical therapy vs the Wii Fit gaming system: A preliminary study. Physiotherapy 98(3):211–216.
Bernsten, C., I. Björkman, M. Caramona, G. Crealey, B. Frøkjaer, E. Grundberger, T. Gustafsson, M. Henman, H. Herborg, C. Hughes, J. McElnay, M. Magner, F. van Mil, M. Schaeffer, S. Silva, B. Søndergaard, I. Sturgess, D. Tromp, L. Vivero, and A. Winter-stein. 2001. Improving the well-being of elderly patients via community pharmacy-based provision of pharmaceutical care: A multicentre study in seven European countries. Drugs and Aging 18(1):63–77.
Berridge, C., J. Halpern, and K. Levy. 2019. Cameras on beds: The ethics of surveillance in nursing home rooms. AJOB Empirical Bioethics 10(1):55–62.
Blain, H., Y. Rolland, J. M. G. A. Schols, A. Cherubini, S. Miot, D. O’Neill, F. C. Martin, O. Guérin, G. Gavazzi, J. Bousquet, M. Petrovic, A. L. Gordon, and A. Benetos. 2020. August 2020 interim EuGMS guidance to prepare European long-term care facilities for COVID-19. European Geriatric Medicine 11(6):899–913.
Bonifas, R. P. 2015. Resident-to-resident aggression in nursing homes: Social worker involvement and collaboration with nursing colleagues. Health & Social Work 40(3):e101–e109.
Braaten, K. L., and W. Malmedal. 2017. Preventing physical abuse of nursing home residents—as seen from the nursing staff’s perspective. Nursing Open 4(4):274–281.
Branch, J., D. Hiner, and V. Jackson. 2021. The impact of communication on medication errors. https://psnet.ahrq.gov/web-mm/impact-communication-medication-errors (accessed February 7, 2022).
Brauner, D., R. M. Werner, T. P. Shippee, J. Cursio, H. Sharma, and R. T. Konetzka. 2018. Does Nursing Home Compare reflect patient safety in nursing homes? Health Affairs (Millwood) 37(11):1770–1778.
Brawley, E. C. 2005. Design innovations for aging and Alzheimer’s: Creating caring environments. Hoboken, NJ: John Wiley & Sons.
Brophy, J., M. Keith, and M. Hurley. 2019. Breaking point: Violence against long-term care staff. New Solutions: A Journal of Environmental and Occupational Health Policy 29(1):10–35.
Brown, K. A., A. Jones, N. Daneman, A. K. Chan, K. L. Schwartz, G. E. Garber, A. P. Costa, and N. M. Stall. 2021. Association between nursing home crowding and COVID-19 infection and mortality in Ontario, Canada. JAMA Internal Medicine 181(2):229–236.
Brown, L. M., M. L. Bruce, K. Hyer, W. L. Mills, E. Vongxaiburana, and L. Polivka-West. 2009. A pilot study evaluating the feasibility of psychological first aid for nursing home residents. Clinical Gerontologist 32(3):293–308.
Brown, L. M., D. M. Dosa, K. Thomas, K. Hyer, Z. Feng, and V. Mor. 2012. The effects of evacuation on nursing home residents with dementia. American Journal of Alzheimer’s Disease and Other Dementias 27(6):406–412.
Cacchione, P. Z., L. M. Willoughby, J. C. Langan, and K. Culp. 2011. Disaster strikes! Long-term care resident outcomes following a natural disaster. Journal of Gerontological Nursing 37(9):16–27.
Calkins, M., and C. Cassella. 2007. Exploring the cost and value of private versus shared bedrooms in nursing homes. The Gerontologist 47(2):169–183.
Cameron, E. J., S. K. Bowles, E. G. Marshall, and M. K. Andrew. 2018b. Falls and long-term care: A report from the care by design observational cohort study. BMC Family Practice 19(1):73.
Cameron, I. D., S. M. Dyer, C. E. Panagoda, G. R. Murray, K. D. Hill, R. G. Cumming, and N. Kerse. 2018a. Interventions for preventing falls in older people in care facilities and hospitals. Cochrane Database of Systematic Reviews 9(9):CD005465.
CANHR (California Advocates for Nursing Home Reform). 2009. Omnicare settles drug kickback cases for $98m (November 3, 2009). http://www.canhr.org/newsroom/canhrnewsarchive/2009/DOJ110309.html (accessed January 18, 2022).
Casey, B., G. Peters, and R. Wyden. 2020. COVID-19 in nursing homes: How the Trump Administration failed residents and workers. https://www.aging.senate.gov/imo/media/doc/COVID-19%20in%20Nursing%20Homes%20Final%20Report.pdf (accessed September 14, 2021).
CDC (Centers for Disease Control and Prevention). 2020. Core elements of antibiotic stewardship for nursing homes. https://www.cdc.gov/longtermcare/prevention/antibiotic-stewardship.html (accessed April 29, 2021).
CDC. 2021. Preventing elder abuse. https://www.cdc.gov/violenceprevention/elderabuse/fastfact.html (accessed November 3, 2021).
CDC TRAIN. 2021. Nursing home infection preventionist training course. https://www.train.org/cdctrain/training_plan/3814 (accessed April 29, 2021).
Chang, H. J., C. Lynm, and R. M. Glass. 2010. Falls and older adults. JAMA 303(3):288.
Chapman, S., and C. Harrington. 2020. Policies matter! Factors contributing to nursing home outbreaks during the COVID-19 pandemic. Policy, Politics, and Nursing Practice 21(4):191–192.
Chaudhury, H., A. Mahmood, and M. Valente. 2004. The use of single patient rooms versus multiple occupancy rooms in acute care environments. https://www.healthdesign.org/sites/default/files/use_of_single_patient_rooms_v_multiple_occ._rooms-acute_care.pdf (accessed January 18, 2022).
Chen, M. K., J. A. Chevalier, and E. F. Long. 2021. Nursing home staff networks and COVID-19. Proceedings of the National Academy of Sciences of the United States of America 118(1):e2015455118.
Clemson, L., M. A. Fiatarone Singh, A. Bundy, R. G. Cumming, K. Manollaras, P. O’Loughlin, and D. Black. 2012. Integration of balance and strength training into daily life activity to reduce rate of falls in older people (the LiFE study): Randomised parallel trial. BMJ 345:e4547.
CMA (Center for Medicare Advocacy). 2019. Nursing Home Compare’s abuse icon is now live. https://medicareadvocacy.org/nursing-home-compares-abuse-icon-is-now-live (accessed November 3, 2021).
CMS (Centers for Medicare & Medicaid Services). 2019a. Specialized infection prevention and control training for nursing home staff in the long-term care setting is now available. https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/SurveyCertificationGenInfo/Downloads/QSO19-10-NH.pdf (accessed February 1, 2022).
CMS. 2019b. Medicare coverage of skilled nursing facility care. https://www.medicare.gov/Pubs/pdf/10153-Medicare-Skilled-Nursing-Facility-Care.pdf (accessed April 29, 2021).
CMS. 2021. Toolkit on state actions to mitigate COVID-19 prevalence in nursing homes. https://www.cms.gov/files/document/covid-toolkit-states-mitigate-covid-19-nursing-homes.pdf (accessed November 8, 2021).
CMS and CDC (Centers for Medicare & Medicaid Services and Centers for Disease Control and Prevention). 2020. COVID-19 long-term care facility guidance. https://www.cms.gov/files/document/4220-covid-19-long-term-care-facility-guidance.pdf (accessed August 25, 2021).
CNBC. 2020. WHO: Coronavirus patients who don’t show symptoms aren’t driving the spread of the virus. https://www.cnbc.com/video/2020/06/08/who-coronavirus-patients-who-dont-show-symptoms-arent-spreading-new-infections.html (accessed April 27, 2021).
Cohen, B., C. C. Cohen, B. Løyland, and E. L. Larson. 2017. Transmission of health care-associated infections from roommates and prior room occupants: A systematic review. Clinical Epidemiology 9:297–310.
Cohen, J., and Y. v. d. M. Rodgers. 2020. Contributing factors to personal protective equipment shortages during the COVID-19 pandemic. Preventive Medicine 141:106263–106263.
Connell, B. R., J. A. Sanford, and D. Lewis. 2007. Therapeutic effects of an outdoor activity program on nursing home residents with dementia. Journal of Housing for the Elderly 21(3–4):194–209.
Cutler, L. J., and R. A. Kane. 2006. As great as all outdoors. Journal of Housing for the Elderly 19(3–4):29–48.
D’Agata, E., M. B. Loeb, and S. L. Mitchell. 2013. Challenges in assessing nursing home residents with advanced dementia for suspected urinary tract infections. Journal of the American Geriatrics Society 61(1):62–66.
de Boer, B., H. C. Beerens, M. A. Katterbach, M. Viduka, B. M. Willemse, and H. Verbeek. 2018. The physical environment of nursing homes for people with dementia: Traditional nursing homes, small-scale living facilities, and green care farms. Healthcare 6(4):137.
Deandrea, S., F. Bravi, F. Turati, E. Lucenteforte, C. La Vecchia, and E. Negri. 2013. Risk factors for falls in older people in nursing homes and hospitals. A systematic review and meta-analysis. Archives of Gerontology and Geriatrics 56(3):407–415.
Demiris, G., D. P. Oliver, G. Dickey, M. Skubic, and M. Rantz. 2008. Findings from a participatory evaluation of a smart home application for older adults. Technology and Health Care 16(2):111–118.
Demiris, G., D. P. Oliver, J. Giger, M. Skubic, and M. Rantz. 2009. Older adults’ privacy considerations for vision based recognition methods of eldercare applications. Technology and Health Care 17(1):41–48.
Denny-Brown, N., D. Stone, B. Hays, and D. Gallaghe. 2020. COVID-19 intesifies nursing home workforce challenges. Washington DC: Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services.
Desai, R., C. E. Williams, S. B. Greene, S. Pierson, and R. A. Hansen. 2011. Medication errors during patient transitions into nursing homes: Characteristics and association with patient harm. American Journal of Geriatric Pharmacotherapy 9(6):413–422.
Dichter, M. N., A. Berg, J. Hylla, D. Eggers, D. Wilfling, R. Möhler, B. Haastert, G. Meyer, M. Halek, and S. Köpke. 2021. Evaluation of a multi-component, non-pharmacological intervention to prevent and reduce sleep disturbances in people with dementia living in nursing homes (MoNoPol-sleep): Study protocol for a cluster-randomized exploratory trial. BMC Geriatrics 21(1):40.
DOJ (Department of Justice, Office of Public Affairs). 2015. Nation’s second-largest nursing home pharmacy to pay $9.25 million to settle kickback allegations. https://www.justice.gov/opa/pr/nations-second-largest-nursing-home-pharmacy-pay-925-million-settle-kickback-allegations (accessed January 18, 2022).
Donelli, D., M. Antonelli, C. Bellinazzi, G. F. Gensini, and F. Firenzuoli. 2019. Effects of lavender on anxiety: A systematic review and meta-analysis. Phytomedicine 65: 153099.
Dong, X., R. Chen, and M. A. Simon. 2014. Elder abuse and dementia: A review of the research and health policy. Health Affairs 33(4):642–649.
Dwyer, L. L., L. D. Harris-Kojetin, R. H. Valverde, J. M. Frazier, A. E. Simon, N. D. Stone, and N. D. Thompson. 2013. Infections in long-term care populations in the United States. Journal of the American Geriatrics Society 61(3):341–349.
Edelman, L. S., J. Drost, R. P. Moone, K. Owens, G. L. Towsley, G. Tucker-Roghi, and J. E. Morley. 2021. Editorial: Applying the age-friendly health system framework to long term care settings. Journal of Nutrition, Health & Aging 25(2):141–145.
Edvardsson, D., D. Fetherstonhaugh, and R. Nay. 2010. Promoting a continuation of self and normality: Person-centred care as described by people with dementia, their family members and aged care staff. Journal of Clinical Nursing 19(17–18):2611–2618.
Eijkelenboom, A., H. Verbeek, E. Felix, and J. van Hoof. 2017. Architectural factors influencing the sense of home in nursing homes: An operationalization for practice. Frontiers of Architectural Research 6(2):111–122.
Ellis, B., and M. Hicken. 2017. Sick, dying and raped in America’s nursing homes. https://www.cnn.com/interactive/2017/02/health/nursing-home-sex-abuse-investigation/ (accessed February 4, 2022).
Fedschun, T. 2019. Nurse arrested in rape of woman in vegetative state who gave birth at care facility. https://www.foxnews.com/us/nurse-arrested-in-rape-of-woman-in-vegetative-state-who-gave-birth-at-care-facility (accessed February 4, 2022).
FEMA (Federal Emergency Management Agency). 2016a. Emergency support function #8—Public health and medical services annex. https://www.fema.gov/sites/default/files/2020-07/fema_ESF_8_Public-Health-Medical.pdf (accessed August 12, 2021).
FEMA. 2016b. Emergency support function #15—External affairs annex. https://www.fema.gov/sites/default/files/2020-07/fema_ESF_15_External-Affairs.pdf (accessed September 24, 2021).
FEMA. 2020. National Response Framework. https://www.fema.gov/emergency-managers/national-preparedness/frameworks/response (accessed August 12, 2021).
FEMA. 2021. About us. https://www.fema.gov/about (accessed August 12, 2021).
Figueiro, M. G., B. A. Plitnick, A. Lok, G. E. Jones, P. Higgins, T. R. Hornick, and M. S. Rea. 2014. Tailored lighting intervention improves measures of sleep, depression, and agitation in persons with Alzheimer’s disease and related dementia living in long-term care facilities. Clinical Interventions in Aging 9:1527–1537.
Figueroa, J. F., R. K. Wadhera, I. Papanicolas, K. Riley, J. Zheng, E. J. Orav, and A. K. Jha. 2020. Association of nursing home ratings on health inspections, quality of care, and nurse staffing with COVID-19 cases. JAMA 324(11):1103–1105.
Fischer, B. L., C. E. Gleason, R. E. Gangnon, J. Janczewski, T. Shea, and J. E. Mahoney. 2014. Declining cognition and falls: Role of risky performance of everyday mobility activities. Physical Therapy 94(3):355–362.
Forbes, D., C. M. Blake, E. J. Thiessen, S. Peacock, and P. Hawranik. 2014. Light therapy for improving cognition, activities of daily living, sleep, challenging behaviour, and psychiatric disturbances in dementia. Cochrane Database Systematic Review 2014(2):CD003946.
Galambos, C., M. Skubic, S. Wang, and M. Rantz. 2013. Management of dementia and depression utilizing in-home passive sensor data. Gerontechnology 11(3):457–468.
Galambos, C., M. Rantz, A. Craver, M. Bongiorno, M. Pelts, A. J. Holik, and J. S. Jun. 2019. Living with intelligent sensors: Older adult and family member perceptions. Computers, Informatics, Nursing 37(12):615–627.
GAO (U.S. Government Accountability Office). 2007. Federal actions needed to improve targeting and evaluation of assistance by quality improvement organizations. Washington DC: U.S. Government Accountability Office.
GAO. 2019a. Nursing homes: Improved oversight needed to better protect residents from abuse. Washington, DC: U.S. Government Accountability Office.
GAO. 2019b. Elder abuse: Federal requirements for oversight in nursing homes and assisted living facilities differ. Washington, DC: U.S. Government Accountability Office.
GAO. 2019c. Nursing homes: Better oversight needed to protect residents from abuse, a statement for the record by John E. Dicken, director, health care. Washington, DC: U.S. Government Accountability Office.
GAO. 2020. Infection control deficiencies were widespread and persistent in nursing homes prior to COVID-19 pandemic. Washington, DC: U.S. Government Accountability Office.
Gates, D., E. Fitzwater, and P. Succop. 2003. Relationships of stressors, strain, and anger to caregiver assaults. Issues in Mental Health Nursing 24(8):775–793.
Geng, F., D. G. Stevenson, and D. C. Grabowski. 2019. Daily nursing home staffing levels highly variable, often below CMS expectations. Health Affairs 38(7):1095–1100.
Gillespie, S. M., L. J. Gleason, J. Karuza, and M. N. Shah. 2010. Health care providers’ opinions on communication between nursing homes and emergency departments. Journal of the American Medical Directors Association 11(3):204–210.
Giri, S., L. M. Chenn, and R. Romero-Ortuno. 2021. Nursing homes during the COVID-19 pandemic: A scoping review of challenges and responses. European Geriatric Medicine 12(6):1127–1136.
Goldstein, M., and R. Gebeloff. 2019. Dozens of nursing homes with HUD-backed mortgages have ‘serious deficiencies’. https://www.nytimes.com/2019/06/24/business/nursing-homeshud.html (accessed February 7, 2022).
Gozalo, P., S. Prakash, D. M. Qato, P. D. Sloane, and V. Mor. 2014. Effect of the Bathing Without a Battle training intervention on bathing-associated physical and verbal outcomes in nursing home residents with dementia: A randomized crossover diffusion study. Journal of the American Geriatrics Society 62(5):797–804.
Green House Project. 2012. Pilot study finds meaningful savings in the Green House® model for eldercare. https://thegreenhouseproject.org/wp-content/uploads/Cost_Savings_Summary_2012.pdf (accessed August 26, 2021).
Gulka, H. J., V. Patel, T. Arora, C. McArthur, and A. Iaboni. 2020. Efficacy and generalizability of falls prevention interventions in nursing homes: A systematic review and meta-analysis. Journal of the American Medical Directors Association 21(8):1024–1035.e1024.
Hado, E., and L. Friss Feinberg. 2020. Amid the COVID-19 pandemic, meaningful communication between family caregivers and residents of long-term care facilities is imperative. Journal of Aging & Social Policy 32(4–5):410–415.
Harnett, P. J., S. Kennelly, and P. Williams. 2020. A 10-step framework to implement integrated care for older persons. Ageing International 45(3):288–304.
Harrington, C., J. M. Wiener, L. Ross, and M. Musumeci. 2017. Key issues in long-term services and supports quality. https://www.kff.org/medicaid/issue-brief/key-issues-in-long-term-services-and-supports-quality (accessed August 25, 2021).
Harrington, C., L. Ross, S. Chapman, E. Halifax, B. Spurlock, and D. Bakerjian. 2020. Nurse staffing and coronavirus infections in California nursing homes. Policy, Politics, and Nursing Practice 21(3):174–186.
Hickman, S. E., A. L. Barrick, C. S. Williams, S. Zimmerman, B. R. Connell, J. S. Preisser, C. M. Mitchell, and P. D. Sloane. 2007. The effect of ambient bright light therapy on depressive symptoms in persons with dementia. Journal of the American Geriatrics Society 55(11):1817–1824.
Hodgson, N. A., L. N. Gitlin, L. Winter, and K. Czekanski. 2011. Undiagnosed illness and neuropsychiatric behaviors in community residing older adults with dementia. Alzheimer Disease and Associated Disorders 25(2):109–115.
Hoel, R. W., R. M. Giddings Connolly, and P. Y. Takahashi. 2021. Polypharmacy management in older patients. Mayo Clinic Proceedings 96(1):242–256.
HRW (Human Rights Watch). 2018. “They want docile”: How nursing homes in the United States overmedicate people with dementia. New York: Human Rights Watch.
HRW. 2021. U.S.: Concerns of neglect in nursing homes—Pandemic exposes need for improvements in staffing, oversight, accountability. https://www.hrw.org/news/2021/03/25/us-concerns-neglect-nursing-homes# (accessed September 8, 2021).
Hughes, R. G. 2008. Patient safety and quality: An evidence-based handbook for nurses. Rockville, MD: Agency for Healthcare Research and Quality.
Hyer, K., L. M. Brown, L. Polivka-West, and A. Berman. 2010. Helping nursing homes prepare for disasters. Health Affairs 29(10):1961–1965.
IOM (Institute of Medicine). 1986. Improving the quality of care in nursing homes. Washington, DC: National Academy Press.
IOM. 2001. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
IOM. 2012. Crisis standards of care: A systems framework for catastrophic disaster response: Volume 1: Introduction and CSC framework. Washington, DC: The National Academies Press.
IOM and NRC (Institute of Medicine and National Research Council). 2014. Elder abuse and its prevention: Workshop summary. Washington, DC: The National Academies Press.
Isaksson, U., U. H. Graneheim, and S. Åström. 2009. Female caregivers’ experiences of exposure to violence in nursing homes. Journal of Psychiatric and Mental Health Nursing 16(1):46–53.
Iversen, M. H., A. Kilvik, and W. Malmedal. 2015. Sexual abuse of older residents in nursing homes: A focus group interview of nursing home staff. Nursing Research and Practice 2015:716407.
Jaffe, S. 2021. After pandemic ravaged nursing homes, new state laws protect residents. https://khn.org/news/article/after-pandemic-ravaged-nursing-homes-new-state-laws-protect-residents (accessed August 25, 2021).
Joosse, L. L. 2011. Sound levels in nursing homes. Journal of Gerontological Nursing 37(8):30–35.
Jump, R. L. P., C. J. Crnich, L. Mody, S. F. Bradley, L. E. Nicolle, and T. T. Yoshikawa. 2018. Infectious diseases in older adults of long-term care facilities: Update on approach to diagnosis and management. Journal of the American Geriatrics Society 66(4):789–803.
Kane, R. A., T. Y. Lum, L. J. Cutler, H. B. Degenholtz, and T.-C. Yu. 2007. Resident outcomes in small-house nursing homes: A longitudinal evaluation of the initial Green House program. Journal of the American Geriatrics Society 55(6):832–839.
Kennedy, C., and J. Will. 2021. Interventions for preventing abuse in the elderly. International Journal of Nursing Practice 27(1):e12870.
King, B. J., A. L. Gilmore-Bykovskyi, R. A. Roiland, B. E. Polnaszek, B. J. Bowers, and A. J. H. Kind. 2013. The consequences of poor communication during transitions from hospital to skilled nursing facility: A qualitative study. Journal of the American Geriatrics Society 61(7):1095–1102.
Kristiansen, L., O. Hellzén, and K. Asplund. 2006. Swedish assistant nurses’ experiences of job satisfaction when caring for persons suffering from dementia and behavioural disturbances. An interview study. International Journal of Qualitative Studies on Health and Well-being 1(4):245–256.
Kua, C. H., V. S. L. Mak, and S. W. Huey Lee. 2019. Health outcomes of deprescribing interventions among older residents in nursing homes: A systematic review and meta-analysis. Journal of the American Medical Directors Association 20(3):362–372.e311.
Lachs, M. S., T. Rosen, J. A. Teresi, J. P. Eimicke, M. Ramirez, S. Silver, and K. Pillemer. 2013. Verbal and physical aggression directed at nursing home staff by residents. Journal of General Internal Medicine 28(5):660–667.
Lachs, M. S., J. A. Teresi, M. Ramirez, K. van Haitsma, S. Silver, J. P. Eimicke, G. Boratgis, G. Sukha, J. Kong, A. M. Besas, M. R. Luna, and K. A. Pillemer. 2016. The prevalence of resident-to-resident elder mistreatment in nursing homes. Annals of Internal Medicine 165(4):229–236.
Lachs, M., L. Mosqueda, T. Rosen, and K. Pillemer. 2021. Bringing advances in elder abuse research methodology and theory to evaluation of interventions. Journal of Applied Gerontology 40(11):1437–1446.
Lane, K. R., C. Galambos, L. J. Phillips, L. L. Popejoy, and M. Rantz. 2019. Aging in place: Transitional housing and supported housing models. In T. Fulmer and B. Chernof (eds.), Handbook of geriatric assessment. Burlington, MA: Jones & Bartlett Learning. Pp. 365–371.
Lane, S. J., and E. McGrady. 2016. Nursing home self-assessment of implementation of emergency preparedness standards. Prehospital and Disaster Medicine 31(4):422–431.
Lane, S. J., and E. McGrady. 2018. Measures of emergency preparedness contributing to nursing home resilience. Journal of Gerontological Social Work 61(7):751–774.
Laxton, C. E., D. A. Nace, and A. Nazir. 2020. Solving the COVID-19 crisis in post-acute and long-term care. Journal of the American Medical Directors Association 21(7):885–887.
Lee, S. W. H., V. S. L. Mak, and Y. W. Tang. 2019. Pharmacist services in nursing homes: A systematic review and meta-analysis. British Journal of Clinical Pharmacology 85(12):2668–2688.
Leipzig, R. M., R. G. Cumming, and M. E. Tinetti. 1999a. Drugs and falls in older people: A systematic review and meta-analysis: I. Psychotropic drugs. Journal of the American Geriatrics Society 47(1):30–39.
Leipzig, R. M., R. G. Cumming, and M. E. Tinetti. 1999b. Drugs and falls in older people: A systematic review and meta-analysis: II. Cardiac and analgesic drugs. Journal of the American Geriatrics Society 47(1):40–50.
Leland, N. E., S. J. Elliott, L. O’Malley, and S. L. Murphy. 2012. Occupational therapy in fall prevention: Current evidence and future directions. American Journal of Occupational Therapy 66(2):149–160.
Levy, K., L. Kilgour, and C. Berridge. 2019. Regulating privacy in public/private space: The case of nursing home monitoring laws. Elder Law Journal 26:323–363.
Lin, P. J., D. I. Kaufer, M. L. Maciejewski, R. Ganguly, J. E. Paul, and A. K. Biddle. 2010. An examination of Alzheimer’s disease case definitions using Medicare claims and survey data. Alzheimer’s & Dementia 6(4):334–341.
Lindbloom, E. J., J. Brandt, L. D. Hough, and S. E. Meadows. 2007. Elder mistreatment in the nursing home: A systematic review. Journal of the American Medical Directors Association 8(9):610–616.
Lum, T. Y., R. A. Kane, L. J. Cutler, and T.-C. Yu. 2008. Effects of Green House nursing homes on residents’ families. Health Care Financing Review 30(2):35–51.
Lynch, R. M., and R. Goring. 2020. Practical steps to improve air flow in long-term care resident rooms to reduce COVID-19 infection risk. Journal of the American Medical Directors Association 21(7):893–894.
Malmedal, W., M. H. Iversen, and A. Kilvik. 2015. Sexual abuse of older nursing home residents: A literature review. Nursing Research and Practice 2015:902515.
Martin, J. L., and S. Ancoli-Israel. 2008. Sleep disturbances in long-term care. Clinics in Geriatric Medicine 24(1):39–50.
McCrystal, T., M. Burghardt, and S. Ferranti. 2010. Buyer beware: OIG shines a spotlight on provider relationships with long term care pharmacies and scrutinizes contract pricing structures. https://www.ropesgray.com/-/media/Files/in-the-news/2010/07/impact-of-omnicare-settlement-for-pharmacy-providers-and-long-term-care-facilities.pdf (accessed January 18, 2022).
McGarry, B. E., D. C. Grabowski, and M. L. Barnett. 2020. Severe staffing and personal protective equipment shortages faced by nursing homes during the COVID-19 pandemic. Health Affairs 39(10):1812–1821.
McGarry, B. E., G. K. SteelFisher, D. C. Grabowski, and M. L. Barnett. 2021. COVID-19 test result turnaround time for residents and staff in US nursing homes. JAMA Internal Medicine 181(4):556–559.
MedPAC (Medicare Payment Advisory Commission). 2021. March 2021 report to the congress: Medicare payment policy. Washington, DC: Medicare Payment Advisory Commission.
Meuleners, L. B., M. L. Fraser, M. K. Bulsara, K. Chow, and J. Q. Ng. 2016. Risk factors for recurrent injurious falls that require hospitalization for older adults with dementia: A population based study. BMC Neurology 16(1):188.
Meyer, D. L., B. Dorbacker, J. O’Rourke, J. Dowling, J. Jacques, and M. Nicholas. 1992. Effects of a “quiet week” intervention on behavior in an Alzheimer boarding home. American Journal of Alzheimer’s Care and Related Disorders and Research 7(4):2–7.
Mishra, A. K., M. Skubic, M. Popescu, K. Lane, M. Rantz, L. A. Despins, C. Abbott, J. Keller, E. L. Robinson, and S. Miller. 2020. Tracking personalized functional health in older adults using geriatric assessments. BMC Medical Informatics and Decision Making 20(1):270.
Mitchell, S. L. 2021. Care of patients with advanced dementia. https://www.uptodate.com/contents/care-of-patients-with-advanced-dementia (accessed February 8, 2022).
MITRE (The MITRE Corporation). 2020. Coronavirus Commission for Safety and Quality in Nursing Homes: Commission final report. https://sites.mitre.org/nhCOVIDcomm/wp-content/uploads/sites/14/2020/09/FINAL-REPORT-of-NH-Commission-Public-Release-Case-20-2378.pdf (accessed August 20, 2021).
Mody, L., S. L. Krein, S. Saint, L. C. Min, A. Montoya, B. Lansing, S. E. McNamara, K. Symons, J. Fisch, E. Koo, R. A. Rye, A. Galecki, M. U. Kabeto, J. T. Fitzgerald, R. N. Olmsted, C. A. Kauffman, and S. F. Bradley. 2015. A targeted infection prevention intervention in nursing home residents with indwelling devices: A randomized clinical trial. JAMA Internal Medicine 175(5):714–723.
Mody, L., M. T. Greene, J. Meddings, S. L. Krein, S. E. McNamara, B. W. Trautner, D. Ratz, N. D. Stone, L. Min, S. J. Schweon, A. J. Rolle, R. N. Olmsted, D. R. Burwen, J. Battles, B. Edson, and S. Saint. 2017. A national implementation project to prevent catheter-associated urinary tract infection in nursing home residents. JAMA Internal Medicine 177(8):1154–1162.
Mody, L., K. J. Gontjes, M. Cassone, K. E. Gibson, B. J. Lansing, J. Mantey, M. Kabeto, A. Galecki, and L. Min. 2021. Effectiveness of a multicomponent intervention to reduce multidrug-resistant organisms in nursing homes: A cluster randomized clinical trial. JAMA Network Open 4(7):e2116555.
Montoya, A., and L. Mody. 2011. Common infections in nursing homes: A review of current issues and challenges. Aging Health 7(6):889–899.
Montoya, A., M. Cassone, and L. Mody. 2016. Infections in nursing homes: Epidemiology and prevention programs. Clinics in Geriatric Medicine 32(3):585–607.
Muir, S. W., K. Gopaul, and M. M. Montero Odasso. 2012. The role of cognitive impairment in fall risk among older adults: A systematic review and meta-analysis. Age and Ageing 41(3):299–308.
Munier-Marion, E., T. Bénet, C. Régis, B. Lina, F. Morfin, and P. Vanhems. 2016. Hospitalization in double-occupancy rooms and the risk of hospital-acquired influenza: A prospective cohort study. Clinical Microbiology and Infection 22(5):461.e467–461.e469.
Murray, T., and J. Friedman. 2020. Nursing home safety during COVID: PPE shortages, seven months into pandemic, 20 percent of facilities lacked enough supplies. https://uspirg.org/feature/usp/nursing-home-safety-during-covid-ppe-shortages (accessed November 29, 2021).
Musumeci, M., and P. Chidambaram. 2020. Key questions about nursing home regulation and oversight in the wake of COVID-19. https://www.kff.org/coronavirus-covid-19/issue-brief/key-questions-about-nursing-home-regulation-and-oversight-in-the-wake-of-covid-19 (accessed December 7, 2020).
Myhre, J., S. Saga, W. Malmedal, J. Ostaszkiewicz, and S. Nakrem. 2020. Elder abuse and neglect: An overlooked patient safety issue. A focus group study of nursing home leaders’ perceptions of elder abuse and neglect. BMC Health Services Research 20(1):199.
Nakrem, S., A. G. Vinsnes, G. E. Harkless, B. Paulsen, and A. Seim. 2013. Ambiguities: Residents’ experience of ‘nursing home as my home’. Internal Journal of Older People Nursing 8(3):216–225.
Narang, P., M. El-Refai, R. Parlapalli, L. Danilov, S. Manda, G. Kaur, and S. Lippmann. 2010. Antipsychotic drugs: Sudden cardiac death among elderly patients. Psychiatry (Edgmont) 7(10):25–29.
National Consumer Voice (The National Consumer Voice for Quality Long-Term Care). 2021. The devasting effect of lockdowns on residents of long-term care facilities during COVID-19. https://theconsumervoice.org/uploads/files/issues/Devasting_Effect_of_Lockdowns_on_Residents_of_LTC_Facilities.pdf (accessed September 8, 2021).
NCEA (National Center on Elder Abuse). 2021a. Research, statistics, and data. https://ncea.acl.gov/What-We-Do/Research/Statistics-and-Data.aspx (accessed May 20, 2021).
NCEA. 2021b. World Elder Abuse Awareness Day is June 15th. https://ncea.acl.gov/WEAAD.aspx (accessed November 3, 2021).
Nguyen Thi, P. L., S. Briançon, F. Empereur, and F. Guillemin. 2002. Factors determining inpatient satisfaction with care. Social Science and Medicine 54(4):493–504.
NIA (National Institute on Aging). 2021. The dangers of polypharmacy and the case for deprescribing in older adults. https://www.nia.nih.gov/news/dangers-polypharmacyand-case-deprescribing-older-adults#:~:text=Inappropriate%20polypharmacy%20%E2%80%94%20the%20use%20of,or%20causes%20a%20new%20one (accessed February 1, 2022).
Nursing Home Abuse Guide. 2021. Financial abuse. https://nursinghomeabuseguide.com/elder-abuse/financial (accessed November 8, 2021).
Nursing Home Abuse Justice. 2021. Mandated reporting laws for elder abuse. https://www.nursinghomeabuse.org/articles/elder-abuse-reporting-laws (accessed November 3, 2021).
Nygaard, A., L. Halvorsrud, E. K. Grov, and A. Bergland. 2020. What matters to you when the nursing is your home: A qualitative study on the views of residents with dementia living in nursing homes. BMC Geriatrics 20(1):227.
ODPHP (Office of Disease Prevention and Health Promotion, U.S. Department of Health and Human Services). 2021. Adverse drug events. https://health.gov/our-work/national-health-initiatives/health-care-quality/adverse-drug-events (accessed November 3, 2021).
Ogletree, A. M., R. Mangrum, Y. Harris, D. R. Gifford, R. Barry, L. Bergofsky, and D. Perfetto. 2020. Omissions of care in nursing home settings: A narrative review. Journal of the American Medical Directors Association 21(5):604-614.e606.
OIG (Office of the Inspector General). 2011. Medicare atypical antipsychotic drug claims for elderly nursing home residents. Washington, DC: Office of the Inspector General, U.S. Department of Health and Human Services.
OIG. 2012. Gaps continue to exist in nursing home emergency preparedness and response during disasters: 2007–2010. Washington, DC: Office of the Inspector General, U.S. Department of Health and Human Services.
OIG. 2014a. Adverse events in skilled nursing facilities: National incidence among Medicare beneficiaries. Washington DC: Office of the Inspector General, U.S. Department of Health and Human Services.
OIG. 2014b. Hospital emergency preparedness and response during Superstorm Sandy. Washington, DC: Office of the Inspector General, U.S. Department of Health and Human Services.
OIG. 2019. Incidents of potential abuse and neglect at skilled nursing facilities were not always reported and investigated. Washington DC: Office of the Inspector General, U.S. Department of Health and Human Services.
OIG. 2021. CMS could improve the data it uses to monitor antipsychotic drugs in nursing homes. Washington, DC: Office of the Inspector General, U.S. Department of Health and Human Services.
O’Mahony, D., D. O’Sullivan, S. Byrne, M. N. O’Connor, C. Ryan, and P. Gallagher. 2014. STOPP/START criteria for potentially inappropriate prescribing in older people: Version 2. Age and Ageing 44(2):213–218.
Ouslander, J. G., and D. C. Grabowski. 2020. COVID-19 in nursing homes: Calming the perfect storm. Journal of the American Geriatrics Society 68:2153–2162.
Passini, R., H. Pigot, C. Rainville, and M.-H. Tétreault. 2000. Wayfinding in a nursing home for advanced dementia of the Alzheimer’s type. Environment and Behavior 32(5): 684–710.
Pierce, J. R., S. K. Morley, T. A. West, P. Pentecost, L. A. Upton, and L. Banks. 2017. Improving long-term care facility disaster preparedness and response: A literature review. Disaster Medicine and Public Health Preparedness 11(1):140–149.
Pillemer, K., D. Burnes, C. Riffin, and M. S. Lachs. 2016. Elder abuse: Global situation, risk factors, and prevention strategies. The Gerontologist 56(Suppl 2):S194–S205.
Poon, E. G., C. A. Keohane, C. S. Yoon, M. Ditmore, A. Bane, O. Levtzion-Korach, T. Moniz, J. M. Rothschild, A. B. Kachalia, J. Hayes, W. W. Churchill, S. Lipsitz, A. D. Whittemore, D. W. Bates, and T. K. Gandhi. 2010. Effect of bar-code technology on the safety of medication administration. New England Journal of Medicine 362(18):1698–1707.
Popejoy, L. L., M. A. Khalilia, M. Popescu, C. Galambos, V. Lyons, M. Rantz, L. Hicks, and F. Stetzer. 2015. Quantifying care coordination using natural language processing and domain-specific ontology. Journal of the American Medical Informatics Association 22(e1):e93–e103.
Powell, T., D. Hanfling, and L. O. Gostin. 2012. Emergency preparedness and public health: The lessons of Hurricane Sandy. JAMA 308(24):2569–2570.
Pugh, T. 2020. Flu shot mandates for nursing home staff urged as COVID persists. https://news.bloomberglaw.com/health-law-and-business/flu-shot-mandates-for-nursing-home-staff-urged-as-covid-persists (accessed August 25, 2021).
Rabig, J., W. Thomas, R. A. Kane, L. J. Cutler, and S. McAlilly. 2006. Radical redesign of nursing homes: Applying the Green House concept in Tupelo, Mississippi. The Gerontologist 46(4):533–539.
Ramsey-Klawsnik, H. 2018. Part 1: Understanding and working with adult protective services (APS). https://ncea.acl.gov/NCEA/media/Publication/Understanding-and-Working-with-APS_May2018.pdf (accessed November 8, 2021).
Rantz, M. J., K. D. Marek, M. Aud, H. W. Tyrer, M. Skubic, G. Demiris, and A. Hussam. 2005. A technology and nursing collaboration to help older adults age in place. Nursing Outlook 53(1):40–45.
Rantz, M. J., R. T. Porter, D. Cheshier, D. Otto, C. H. Servey, 3rd, R. A. Johnson, M. Aud, M. Skubic, H. Tyrer, Z. He, G. Demiris, G. L. Alexander, and G. Taylor. 2008. Tigerplace, a state-academic-private project to revolutionize traditional long-term care. Journal of Housing for the Elderly 22(1–2):66–85.
Rantz, M. J., L. Phillips, M. Aud, L. Popejoy, K. D. Marek, L. L. Hicks, I. Zaniletti, and S. J. Miller. 2011. Evaluation of aging in place model with home care services and registered nurse care coordination in senior housing. Nursing Outlook 59(1):37–46.
Rantz, M., L. L. Popejoy, C. Galambos, L. J. Phillips, K. R. Lane, K. D. Marek, L. Hicks, K. Musterman, J. Back, S. J. Miller, and B. Ge. 2014a. The continued success of registered nurse care coordination in a state evaluation of aging in place in senior housing. Nursing Outlook 62(4):237–246.
Rantz, M., L. Popejoy, K. Musterman, and S. J. Miller. 2014b. Influencing public policy through care coordination research. In G. Lamb (ed.), Care coordination: The game changer. Silver Spring, MD: American Nurses Association. Pp. 203–220.
Rantz, M., K. Lane, L. J. Phillips, L. A. Despins, C. Galambos, G. L. Alexander, R. J. Koopman, L. Hicks, M. Skubic, and S. J. Miller. 2015. Enhanced registered nurse care coordination with sensor technology: Impact on length of stay and cost in aging in place housing. Nursing Outlook 63(6):650–655.
Rau, J. 2020. Coronavirus stress test: Many 5-star nursing homes have infection-control lapses. https://khn.org/news/coronavirus-preparedness-infection-control-lapses-at-top-rated-nursing-homes/ (accessed January 27, 2022).
Redmond, P., T. C. Grimes, R. McDonnell, F. Boland, C. Hughes, and T. Fahey. 2018. Impact of medication reconciliation for improving transitions of care. The Cochrane Database of Systematic Reviews 8(8):CD010791-CD010791.
Regnier, V. 2018. Housing design for an increasingly older population: Redefining assisted living for the mentally and physically frail. Hoboken, NJ: John Wiley & Sons.
Reid, J., K. Wilson, K. E. Anderson, and C. P. Maguire. 2015. Older inpatients’ room preference: Single versus shared accommodation. Age and Ageing 44(2):331–333.
Reiling, J., R. Hughes, and M. Murphy. 2008. The impact of facility design on patient safety. In R. Hughes (ed.), Patient safety and quality: An evidence-based handbook for nurses. Rockville, MD: Agency for Healthcare Research and Quality.
Riemersma-van der Lek, R. F., D. F. Swaab, J. Twisk, E. M. Hol, W. J. Hoogendijk, and E. J. Van Someren. 2008. Effect of bright light and melatonin on cognitive and noncognitive function in elderly residents of group care facilities: A randomized controlled trial. JAMA 299(22):2642–2655.
Roubein, R. 2021. Will the nursing home of the future be an actual home? Politico, April 30. https://www.politico.com/news/agenda/2021/04/30/nursing-home-future-483460 (accessed November 29, 2021).
Sabatino, C. P., and C. Harrington. 2021. Policy change to put the home back into nursing homes. BIFOCAL, Journal of the ABA Commission on Law and Aging 42(6):119–125.
Sandvoll, A. M., E. K. Grov, and M. Simonsen. 2020. Nursing home residents’ ADL status, institution-dwelling and association with outdoor activity: A cross-sectional study. PeerJ 8:e10202.
Schnelle, J. F., C. A. Alessi, N. R. Al-Samarrai, R. D. Fricker, Jr., and J. G. Ouslander. 1999. The nursing home at night: Effects of an intervention on noise, light, and sleep. Journal of the American Geriatrics Society 47(4):430–438.
Schwarz, B. 1997. Nursing home design: A misguided architectural model. Journal of Architectural and Planning Research 14(4):343–359.
Scott, A. M., J. Li, S. Oyewole-Eletu, H. Q. Nguyen, B. Gass, K. B. Hirschman, S. Mitchell, S. M. Hudson, and M. V. Williams. 2017. Understanding facilitators and barriers to care transitions: Insights from project achieve site visits. Joint Commission Journal on Quality and Patient Safety 43(9):433–447.
Shen, K. 2020. Relationship between nursing home COVID-19 outbreaks and staff neighborhood characteristics. medRxiv, December 6. https://doi.org/10.1101/2020.09.10.
Shen, Y., F. Sun, A. Zhang, and K. Wang. 2021. The effectiveness of psychosocial interventions for elder abuse in community settings: A systematic review and meta-analysis. Frontiers in Psychology 12:679541.
Siegel, J. D., E. Rhinehart, M. Jackson, and L. Chiarello. 2017. Management of multidrug-resistant organisms in healthcare settings, 2006. https://www.cdc.gov/infectioncontrol/pdf/guidelines/mdro-guidelines.pdf (accessed September 8, 2021).
Silow-Carroll, S., D. Peartree, S. Tucker, and A. Pham. 2021. Fundamental nursing home reform: Evidence on single-resident rooms to improve personal experience and public health. https://www.healthmanagement.com/wp-content/uploads/HMA.Single-Resident-Rooms-3.22.2021_final.pdf (accessed November 5, 2021).
Simmons, S., J. Schnelle, J. Slagle, N. A. Sathe, D. Stevenson, M. Carlo, and M. L. McPheeters. 2016. Resident safety practices in nursing home settings, Technical briefs, no. 24. Rockville, MD: Agency for Healthcare Research and Quality
Skubic, M., R. D. Guevara, and M. Rantz. 2015. Automated health alerts using in-home sensor data for embedded health assessment. IEEE Journal of Translational Engineering in Health and Medicine 3:1–11.
Sloane, P. D., V. J. Honn, S. A. R. Dwyer, J. Wieselquist, C. Cain, and S. Myers. 1995. Bathing the Alzheimer’s patient in long term care: Results and recommendations from three studies. American Journal of Alzheimer’s Disease 10(4):3–11.
Sloane, P. D., C. M. Mitchell, G. Weisman, S. Zimmerman, K. M. Foley, M. Lynn, M. Calkins, M. P. Lawton, J. Teresi, L. Grant, D. Lindeman, and R. Montgomery. 2002. The Therapeutic Environment Screening Survey for Nursing Homes (TESS-NH): An observational instrument for assessing the physical environment of institutional settings for persons with dementia. Journals of Gerontology, Series B: Psychological Sciences 57(2):S69–S78.
Sloane, P. D., C. S. Williams, C. M. Mitchell, J. S. Preisser, W. Wood, A. L. Barrick, S. E. Hickman, K. S. Gill, B. R. Connell, J. Edinger, and S. Zimmerman. 2007a. High-intensity environmental light in dementia: Effect on sleep and activity. Journal of the American Geriatrics Society 55(10):1524–1533.
Sloane, P. D., L. W. Cohen, C. S. Williams, J. Munn, J. S. Preisser, M. D. Sobsey, D. A. Wait, and S. Zimmerman. 2007b. Effect of specialized bathing systems on resident cleanliness and water quality in nursing homes: A randomized controlled trial. Journal of Water and Health 5(2):283–294.
Sloane, P. D., N. J. Brandt, A. Cherubini, T. S. Dharmarajan, D. Dosa, J. T. Hanlon, P. Katz, R. T. C. M. Koopmans, R. D. Laird, M. Petrovic, T. P. Semla, E. C. K. Tan, and S. Zimmerman. 2021. Medications in post-acute and long-term care: Challenges and controversies. Journal of the American Medical Directors Association 22(1):1–5.
Spanko, A. 2020. New CMS push to target nursing homes in hotspots “misleading,” “underresourced.” https://skillednursingnews.com/2020/07/new-cms-push-to-target-nursing-homes-in-hotspots-misleading-under-resourced (accessed August 25, 2021).
Spinewine, A., P. Evrard, and C. Hughes. 2021. Interventions to optimize medication use in nursing homes: A narrative review. European Geriatric Medicine 12(3):551–567.
Stall, N. M., A. Jones, K. A. Brown, P. A. Rochon, and A. P. Costa. 2020. For-profit long-term care homes and the risk of COVID-19 outbreaks and resident deaths. Canadian Medical Association Journal 192(33):E946–E955.
Stiller, A., F. Salm, P. Bischoff, and P. Gastmeier. 2016. Relationship between hospital ward design and healthcare-associated infection rates: A systematic review and meta-analysis. Antimicrobial Resistance & Infection Control 5(1):51.
Stone, E., M. Skubic, M. Rantz, C. Abbott, and S. Miller. 2015. Average in-home gait speed: Investigation of a new metric for mobility and fall risk assessment of elders. Gait Posture 41(1):57–62.
Stone, P. W., C. T. A. Herzig, M. Agarwal, M. Pogorzelska-Maziarz, and A. W. Dick. 2018. Nursing home infection control program characteristics, CMS citations, and implementation of antibiotic stewardship policies: A national study. Inquiry 55:46958018778636.
Storey, J. E. 2020. Risk factors for elder abuse and neglect: A review of the literature. Aggression and Violent Behavior 50:101339.
Strausbaugh, L. J., and C. L. Joseph. 2000. The burden of infection in long-term care. Infection Control and Hospital Epidemiology 21(10):674–679.
Strausbaugh, L. J., S. R. Sukumar, C. L. Joseph, and K. P. High. 2003. Infectious disease outbreaks in nursing homes: An unappreciated hazard for frail elderly persons. Clinical Infectious Diseases 36(7):870–876.
Su, B. Y., M. Enayati, K. C. Ho, M. Skubic, L. Despins, J. Keller, M. Popescu, G. Guidoboni, and M. Rantz. 2019. Monitoring the relative blood pressure using a hydraulic bed sensor system. IEEE Transactions on Biomedical Engineering 66(3):740–748.
Tay, E. L., S. W. H. Lee, G. H. Yong, and C. P. Wong. 2018. A systematic review and meta-analysis of the efficacy of custom game based virtual rehabilitation in improving physical functioning of patients with acquired brain injury. Technology and Disability 30(1–2):1–23.
Terrell, K. M., and D. K. Miller. 2006. Challenges in transitional care between nursing homes and emergency departments. Journal of the American Medical Directors Association 7(8):499–505.
Thomas, K., R. Gebeloff, and J. Silver-Greenberg. 2021. Phony diagnoses hide high rates of drugging at nursing homes. https://www.nytimes.com/2021/09/11/health/nursing-homes-schizophrenia-antipsychotics.html (accessed November 8, 2021).
Thompson, D.-C., M.-G. Barbu, C. Beiu, L. G. Popa, M. M. Mihai, M. Berteanu, and M. N. Popescu. 2020. The impact of COVID-19 pandemic on long-term care facilities worldwide: An overview on international issues. BioMed Research International 2020:8870249.
TROPOS (Leibniz Institute for Tropospheric Research). 2020. COVID-19: Indoor air in hospitals and nursing homes requires more attention: Recommendations on how to reduce SARS-CoV-2 aerosol dispersal. www.sciencedaily.com/releases/2020/12/201214104710.htm (accessed January 27, 2022).
True, S., J. Cubanski, R. Garfield, M. Rae, G. Claxton, P. Chidambaram, and K. Orgera. 2020. COVID-19 and workers at risk: Examining the long-term care workforce. https://www.kff.org/coronavirus-covid-19/issue-brief/covid-19-and-workers-at-risk-examining-the-long-term-care-workforce (accessed August 25, 2021).
Truitt, E., R. Thompson, D. Blazey-Martin, D. NiSai, and D. Salem. 2016. Effect of the implementation of barcode technology and an electronic medication administration record on adverse drug events. Hospital Pharmacy 51(6):474–483.
University of Nebraska–Lincoln. 2021. Ventilation in residential care environments. Washington, DC: Office of Energy Efficiency and Renewable Energy, U.S. Department of Energy.
U.S. Congress, Senate, Committee on Finance. 2019. Not forgotten: Protecting americans from abuse and neglect in nursing homes. 116th Cong., March 6 (statement of Maya Fischer: Daughter of Sonja Fischer, Nursing Home Rape Victim). https://www.finance.senate.gov/imo/media/doc/Fischer%20Testimony.pdf (accessed February 4, 2022).
U.S. Senate Committee on Finance. 2018. Sheltering in danger: How poor emergency planning and response put nursing home residents at risk during hurricanes Harvey and Irma. https://www.finance.senate.gov/imo/media/doc/Sheltering%20in%20Danger%20Report%20(2%20Nov%202018).pdf (accessed September 14, 2021).
van den Berg, M. E. L., M. Winsall, S. M. Dyer, F. Breen, M. Gresham, and M. Crotty. 2019. Understanding the barriers and enablers to using outdoor spaces in nursing homes: A systematic review. The Gerontologist 60(4):e254–e269.
van Hoof, J., H. Verbeek, B. M. Janssen, A. Eijkelenboom, S. L. Molony, E. Felix, K. A. Nieboer, E. L. Zwerts-Verhelst, J. J. Sijstermans, and E. J. Wouters. 2016a. A three perspective study of the sense of home of nursing home residents: The views of residents, care professionals, and relatives. BMC Geriatrics 16(1):169.
van Hoof, J., M. L. Janssen, C. M. C. Heesakkers, W. van Kersbergen, L. E. J. Severijns, L. A. G. Willems, H. R. Marston, B. M. Janssen, and M. E. Nieboer. 2016b. The importance of personal possessions for the development of a sense of home of nursing home residents. Journal of Housing for the Elderly 30(1):35–51.
van Zadelhoff, E., H. Verbeek, G. Widdershoven, E. van Rossum, and T. Abma. 2011. Good care in group home living for people with dementia. Experiences of residents, family and nursing staff. Journal of Clinical Nursing 20(17–18):2490–2500.
Verbeek, H., E. Van Rossum, S. M. Zwakhalen, G. I. Kempen, and J. P. Hamers. 2009. Small, homelike care environments for older people with dementia: A literature review. International Psychogeriatrics 21(2):252–264.
Verrue, C. L., M. Petrovic, E. Mehuys, J. P. Remon, and R. Vander Stichele. 2009. Pharmacists’ interventions for optimization of medication use in nursing homes: A systematic review. Drugs Aging 26(1):37–49.
Vlaeyen, E., J. Coussement, G. Leysens, E. Van der Elst, K. Delbaere, D. Cambier, K. Denhaerynck, S. Goemaere, A. Wertelaers, F. Dobbels, E. Dejaeger, and K. Milisen. 2015. Characteristics and effectiveness of fall prevention programs in nursing homes: A systematic review and meta-analysis of randomized controlled trials. Journal of the American Geriatrics Society 63(2):211–221.
Wang, L., I. Norman, T. Xiao, Y. Li, and M. Leamy. 2021. Psychological first aid training: A scoping review of its application, outcomes and implementation. International Journal of Environmental Research and Public Health 18(9).
Wang, R., L. Chen, L. Fan, D. Gao, Z. Liang, J. He, W. Gong, and L. Gao. 2015. Incidence and effects of polypharmacy on clinical outcome among patients aged 80+: A five-year follow-up study. PLoS One 10(11):e0142123.
Waters, R. 2021. The big idea behind a new model of small nursing homes. Health Affairs 40(3):378–383.
Wegerer, J. 2017. The connection between UTIs and dementia. https://www.alzheimers.net/2014-04-03-connection-between-utis-and-dementia (accessed February 8, 2022).
Welsh, T. J., A. McGrogan, and A. Mitchell. 2020. Deprescribing in the last years of life—It’s hard to STOPP. Age and Ageing 49(5):723–724.
Werner, R. M., A. K. Hoffman, and N. B. Coe. 2020. Long-term care policy after COVID-19—Solving the nursing home crisis. New England Journal of Medicine 383(10):903–905.
Wiener, J. M., M. P. Freiman, D. Brown, and RTI International. 2007. Nursing home care quality: Twenty years after the Omnibus Budget Reconciliation Act of 1987. Durham, North Carolina: RTI International.
Wood, K., N. Mehri, N. Hicks, and J. M. Vivoda. 2020. Family satisfaction: Differences between nursing homes and residential care facilities. Journal of Applied Gerontology 40(12):1733–1742.
Woodbridge, R., M. P. Sullivan, E. Harding, S. Crutch, K. J. Gilhooly, M. Gilhooly, A. McIntyre, and L. Wilson. 2018. Use of the physical environment to support everyday activities for people with dementia: A systematic review. Dementia 17(5):533–572.
Woolcott, J. C., K. J. Richardson, M. O. Wiens, B. Patel, J. Marin, K. M. Khan, and C. A. Marra. 2009. Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Archives of Internal Medicine 169(21):1952–1960.
Wrublowsky, R. 2018. Design guide for long-term care homes. https://www.fgiguidelines.org/wp-content/uploads/2018/03/MMP_DesignGuideLongTermCareHomes_2018.01.pdf (accessed September 8, 2021).
Wu, M. C., H. C. Sung, W. L. Lee, and G. D. Smith. 2015. The effects of light therapy on depression and sleep disruption in older adults in a long-term care facility. International Journal of Nursing Practice 21(5):653–659.
Yon, Y., M. Ramiro-Gonzalez, C. R. Mikton, M. Huber, and D. Sethi. 2019. The prevalence of elder abuse in institutional settings: A systematic review and meta-analysis. European Journal of Public Health 29(1):58–67.
Yurkofsky, M., and J. G. Ouslander. 2021. COVID-19: Management in nursing homes. https://www.uptodate.com/contents/covid-19-management-in-nursing-homes (accessed July 8, 2021).
Zhu, X., H. Lee, H. Sang, J. Muller, H. Yang, C. Lee, and M. Ory. 2022. Nursing home design and COVID-19: Implications for guidelines and regulation. Journal of the American Medical Directors Association 23(2):272–279.e271.
Zimmerman, S., B. J. Bowers, L. W. Cohen, D. C. Grabowski, S. D. Horn, P. Kemper, and the THRIVE Research Collaborative. 2016. New evidence on the Green House model of nursing home care: Synthesis of findings and implications for policy, practice, and research. Health Services Research 51(Suppl 1):475–496.
Zimmerman, S., C. Dumond-Stryker, M. Tandan, J. S. Preisser, C. J. Wretman, A. Howell, and S. Ryan. 2021. Nontraditional small house nursing homes have fewer COVID-19 cases and deaths. Journal of the American Medical Directors Association 22(3):489–493.






















































