2
Potential Long-Term Effects of COVID-19 on Health Equity
While the acute infections of the virus have clearly devastated millions around the world, the effects have not been evenly felt. Some populations have been hit harder than others, and many inequities have emerged in the available data. The importance of mental health and its intersection with the pandemic has also been increasingly appreciated. Additionally, hospitalization and death are not the only critical outcomes to COVID-19. Even following mild cases, many people find themselves suffering from symptoms for weeks or even months afterward, without answers or solutions (WHO, 2020). This chapter first highlights the inequalities and inequities illuminated by the pandemic in the United States. It discusses the relationship between coronavirus disease 2019 (COVID-19), mental health, and social determinants of health (SDOH), and concludes with some of the long-term implications of COVID-19, through the “long COVID” condition experienced by both adults and children.
PANDEMIC INEQUALITIES IN THE UNITED STATES
Presented by David Blumenthal, Commonwealth Fund
David Blumenthal, Commonwealth Fund, noted that equity has been front and center throughout the pandemic and shared evidence of specific instances of pandemic-related inequity and some potential solutions. For example, COVID-19 hospitalizations differ by race and ethnicity, with
rates for Indigenous, Black, and Hispanic1 persons three times higher than that of White or Asian persons in the United States (CDC, 2021; NCIRD, 2021). Similarly, the death rates were also at least twice as high for those three groups compared to White and Asian persons (CDC, 2021). People of color were also differently affected economically, Blumenthal commented, as 32 percent of Black older adults (over age 65) and 39 percent of Hispanic older adults in the United States reported using their savings or losing their source of income because of the pandemic, compared to just 14 percent of White older adults. The overall average of older adults (regardless of race or ethnicity) reporting these financial difficulties in countries belonging to the Organization for Economic Co-operation and Development (OECD) ranged from 4 percent in Switzerland to 19 percent in the United States (Williams et al., 2021). In the United States, older adults are the only population eligible for universal health coverage, which they access under the Medicaid program.
To posit some causes of disparities, Blumenthal shared additional examples of rates of uninsurance by race and rural versus urban divides. Because the United States is the only country in the developed world that does not have universal health coverage, he said, not having health insurance can influence health disparities, and that is not felt equally across race or ethnicity groups. On average for adults between 19 and 64, nine percent of White Americans are uninsured, compared to 14 percent of Black Americans, and nearly 26 percent of Hispanic Americans (U.S. Census Bureau, 2019). Across all states, in 2018 and 2020, rates of uninsurance were considerably higher for people at or below 100 percent of the federal poverty limit (see Figure 2-1). This was more pronounced in states that did not expand Medicaid through the Affordable Care Act (ACA), he added. The same differential rates of insurance are observable in relation to income.
There are also important considerations about where people live, specifically examining rural versus urban America, Blumenthal continued. Sixty million people or one in five Americans, live in rural areas. But these regions have seen hospitals closing at a much higher rate over the last several years, leaving area residents with fewer and fewer health care options. In 2020 alone, a record 20 rural hospitals closed, he said. These institutions are sometimes the only source of care within hours of driving, making access even more difficult, but they also act as a source of employment and vitality for the region (Ellison, 2021).
___________________
1 Throughout this proceedings, language describing racial and ethnic populations reflects the terms used by individual speakers.
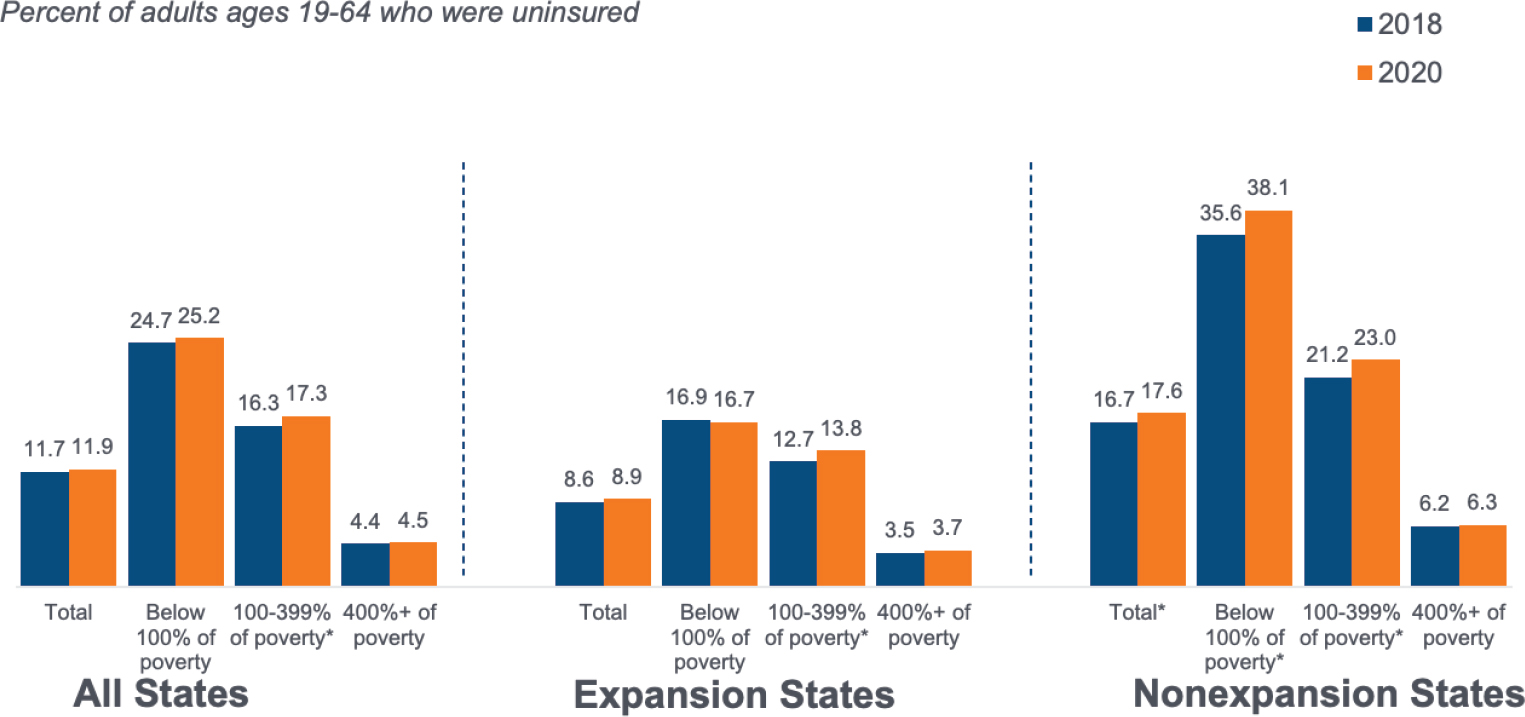
SOURCES: David Blumenthal on September 21, 2021; U.S. Census Bureau, 2021.
Forward-Looking Solutions
Blumenthal offered several potential solutions for the future—both inside and outside the health care system. First, thinking inside the system, he suggested providing meaningful health insurance coverage for people of color and who have low income. Additionally, strengthening the ACA process through more generous subsidies for the purchase of insurance, and expanding the Medicaid program in the remaining 12 states that have yet to do so could increase health insurance coverage. Echoing earlier comments from H. E. Hanan Al Kuwari, Blumenthal noted that many solutions to these issues lie outside the health care system, but this will require combat-ting the racism that underlies social and economic patterns undermining the health of people of color. New legislation is needed to invest in social infrastructure to remedy the social and economic drivers of health, he argued. The Biden administration has introduced legislation that would invest in a whole range of supports for social and economic issues related to inequality, including child care, home care for the elderly, and childhood education, but it continues to be debated by Congress (White House, 2021). Looking forward, Blumenthal concluded, another pandemic would almost certainly repeat the problems experienced over the past 2 years. He emphasized the importance of some of these reforms being considered in order to avoid repeating these same inequities in the future.
MEASURING MENTAL HEALTH AND SOCIAL DETERMINANTS
Presented by Mir M. Ali,
Office of the Assistant Secretary for Planning and Evaluation
Mir M. Ali, Office of the Assistant Secretary for Planning and Evaluation within the Department of Health and Human Services (HHS), shared a recent HHS report that examined the new onset of mental health conditions among individuals who had contracted COVID-19 (Ali, 2021). HHS also wanted to see what factors correlated with new onset of mental health conditions after COVID-19 diagnosis, particularly related to SDOH. There were concerns surrounding mental health since the early phases of the pandemic, Ali said, and patients with mental health conditions can be more susceptible to COVID-19 (Yao et al., 2020). There is also evidence of a bidirectional relationship between COVID-19 and mental illness, with an increased risk of a diagnosis of psychiatric sequelae after acute COVID-19 diagnosis (Taquet et al., 2021). Ali noted that the pandemic highlighted existing inequities, especially in the United States. While it has long been accepted that health is not confined within treatment centers, he continued, the pandemic demonstrated the increased prevalence of preexisting health
conditions in disadvantaged communities. Increasingly, evidence shows that the pandemic’s effects may be long lasting, including things such as food insecurity, housing instability, and slow job recovery (Peretz et al., 2020).
While these SDOH factors have not historically been documented in clinical health records, the most recent update of the International Classification of Diseases, 10th revision in 2015, included “Z codes” that correspond to various SDOH factors to assist providers in documenting them for each patient. Thus far, the use of Z codes has been quite low. Given this, Ali explained HHS was interested in analyzing these factors to answer questions about the new onset of mental health conditions, SDOH factors, and COVID-19 diagnosis. This analysis used U.S. open-source data claims through IQVIA between December 2018 and January 2021 to identify individuals with COVID-19 diagnoses and no mental health claims in the last 12 months. Mental health conditions include psychosis, major depression, mood disorder, and anxiety-related disorders. Ali reported that those with a COVID-19 diagnosis who did not develop a mental health condition were less likely to be hospitalized than those who developed a mental health condition (15 percent vs. 28 percent), and they were also less likely to have some of the comorbidities that are known to result in more serious illness with COVID-19, such as asthma, bronchitis, diabetes, heart disease, hypertension, and obesity. While HHS expected the Z code use to be low, he said, overall, less than one percent of patients had a Z code entered. However, those with mental health conditions had nearly three times the likelihood of Z codes being used within that group. Though conservative due to the paucity of entered Z codes, the researchers found that the odds ratios (ORs) were quite high for new onset of mental health conditions for those with Z codes entered. Factors such as education (OR = 8.26), employment (OR = 4.49), childhood upbringing (OR = 13.34), and housing (OR = 3.5) “were highly correlated with new onset of a mental health condition,” Ali concluded. HHS performed a robustness check of the timing of when the Z code was entered but found that the effects were still significant whether it was entered before the COVID-19 diagnosis, or after. The effects were especially magnified when it was entered after COVID-19 diagnosis, as social circumstances may have been exacerbated because of illness (Ali, 2021).
In conclusion, Ali said that SDOH were a “significant predictor of new onset of mental health conditions” regardless of when the Z codes were entered. There is growing consensus that addressing SDOH is crucial to improving mental health and health more broadly. Low use of Z codes by providers remains, and he posited that this could be attributable to limited awareness that they exist or a lack of incentives for use. A participant asked how to increase the use of Z codes by providers. Ali replied that certain providers tend to use them more than others, such as behavioral health providers. This highlights the opportunity of more provider training in this
area, which can include how Z code use can affect the treatment trajectory of patients. Medical coding is a big puzzle in the United States, he noted, and why certain providers use certain codes is a large function of their reimbursement from health insurance. Currently, there are no incentives for them to use Z codes, so creating such incentives would also be beneficial to increasing their usage.
DISEASE MECHANISMS OF LONG COVID-19
In addition to the clear effects of acute disease that COVID-19 has inflicted upon the millions of patients worldwide, as the months went on, more reports emerged of patients unable to recover. Their symptoms persisted for weeks or months at a time, without any clear reason for why. Similar reports have been found in both adults and children, as discussed in this section.
Long COVID-19 Presentation in Adults
Presented by Akiko Iwasaki, Yale University
Akiko Iwasaki from Yale University focused her remarks on long COVID in adults. These patients can experience a myriad of symptoms weeks or even months after infection, she said, including most commonly fatigue (78 percent), postexertional malaise (72 percent), and cognitive dysfunction (55 percent) (Davis et al., 2021). Of these patients, Iwasaki said 45 percent of cases require a reduction in their usual workload, and 22 percent are completely unable to return to work (Davis et al., 2021). A significant percentage of COVID-19 survivors develop long COVID; Iwasaki highlighted a study that found that 63.2, 71.9, and 45.9 percent exhibited one or more post-COVID-19 symptom at 30, 60, or 90 days after onset or hospitalization (Fernández-de-Las-Peñas et al., 2021). However, she noted that not everyone is affected equally. Compared to men of the same age, women under 50 were five times less likely to report feeling recovered from the acute illness, seven times more likely to become breathless, and more likely to have a greater disability (Sigfrid et al., 2021).
Iwasaki described two different types of long COVID: (1) Post Severe COVID-19 Syndrome includes a severe case of COVID-19 where, following hospital discharge, 70 percent of patients report long-term symptoms, including fibrosis, tissue damage, and even organ damage; and (2) Post COVID-19 Fatigue Syndrome follows a mild or asymptomatic case, where 10 to 30 percent experience long-term symptoms such as fatigue, brain fog, postexertional malaise, and dysautonomia, which can affect functions like heartbeat and breathing. COVID-19 can cause long-lasting symptoms
across multiple organs in the body, she explained, with more than 200 different symptoms being reported for those experiencing long COVID. She shared some hypotheses for long COVID, the first one being that it acts as a viral reservoir, which has been seen in multiple studies. A second hypothesis is that the virus triggers autoreactive lymphocytes and can lead to reactive autoimmunity. Other possibilities include tissue damage following dysbiosis (dysregulation of the microbiome), with latent virus reactivation caused by immunosuppression experienced by patients that then triggers inflammation. There is evidence for all of these hypotheses, she mentioned.
In terms of treatment, some have noticed improvement in their long COVID symptoms following vaccination (see Figure 2-2). Although, while 57 percent of patients in a United Kingdom study improved following vaccination (including multiple vaccine types), 19 percent got worse (LongCOVIDSOS, 2021). Researchers are continuing to study this interaction, and she said it has revealed very interesting and important biological findings so far. Vaccines may improve long COVID symptoms by eliciting robust antiviral antibodies to clear the viral reservoir. Vaccines may also trigger innate and adaptive immune responses to redirect the immune system away from sustaining autoreactive lymphocytes, thereby improving patient symptoms. Iwasaki emphasized that there is currently no effective treatment for long COVID.
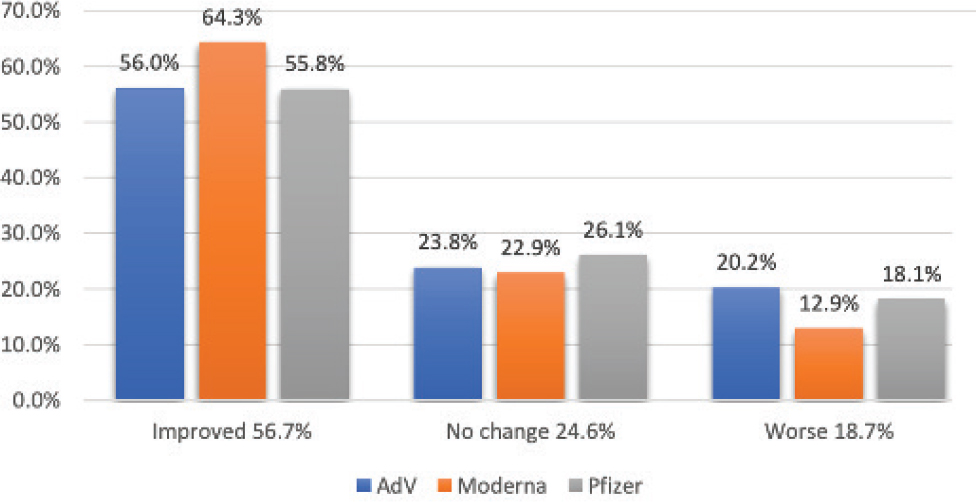
NOTE: AdV = adenovirus vaccines.
SOURCES: Akiko Iwasaki on September 21, 2021; LongCOVIDSOS, 2021.
Post-Acute COVID-19 Syndrome in Children
Presented by Danilo Buonsenso,
Fondazione Policlinico Universitario A. Gemelli
Danilo Buonsenso, Fondazione Policlinico Universitario A. Gemelli in Italy, presented his research on long COVID in children. He said the work began a year prior when researchers first described persistent symptoms in adults, weeks to months after their initial diagnosis. Naturally, pediatricians wanted to know whether this same condition was being seen in children. Through international collaboration, his team developed a survey to see whether and how children were affected and found a similar reporting of symptoms to adults. For example, a significant number of children had at least three symptoms affecting their daily routines, such as persistent cough, fatigue, muscle or joint pain, insomnia, and skin rashes (Buonsenso et al., 2021b).
Through another study in the United Kingdom, researchers found similar results in a cohort of children, with fatigue being one of the main symptoms. They also learned through that study, said Buonsenso, that symptoms were not consistent over time and would sometimes worsen and sometimes improve. Only 10 percent of children with COVID symptoms persisting longer than 4 weeks had returned to previous physical activity levels (Buonsenso et al., 2021a). Many other studies across several countries have been conducted since, Buonsenso commented, and they have found persistent symptoms after acute disease. To ensure the children’s reporting of symptoms was not connected to adults in the house who may also be suffering from long COVID, a larger follow-up study examined children and adults living in the same household with previous COVID-19 diagnosis. They found that children’s symptoms were not correlated to adult symptoms, indicating no psychological transfer of symptoms.
The majority of children who do get COVID-19 typically have a mild case and fully recover, he said. But some children will have acute post-infectious complications such as multisystem inflammatory syndrome or acute onset neurological diseases, and another subset of children will struggle to return to normal life. These children experience persistent headaches, extreme fatigue, and other symptoms (Buonsenso et al., 2021a,b). While there is now increased recognition of long COVID in children, there is still a narrative that says most of their symptoms are psychological, said Buonsenso. Whenever this is discussed, it often leads to dismissing their symptoms or blaming them on another cause.
For the next phase of the pandemic, Buonsenso called for a child-focused strategy. Long COVID needs to be recognized as an outcome of acute pediatric COVID-19 infection, he said. If this is done, then long
COVID can be more relevant, and it will be easier to generate necessary funds for additional clinics and research to care for these children. It will also help in the overarching assessment of risks and benefits of the vaccines, as the considerations go beyond just influencing the relationship with acquiring acute infection. But vaccines could also reduce transmission and the long-term sequelae that many children experience.
This strategy should also include preventive measures in close childhood environments, such as masks and proper ventilation, but he supported stopping the indiscriminate closure of childhood activities such as schools. In summary, he said there is increasing evidence of children with long COVID worldwide, and it is important to consider and count long COVID to inform funding and research policies, develop better partnerships with patients and parents, and share protocols worldwide. Ideally, this work can also help better understand other postviral conditions affecting many worldwide.
DISCUSSION
A participant highlighted the health inequities Indigenous populations and Asian Americans experienced in the United States throughout the pandemic. Blumenthal stated that, while there are problems with discrimination and bias against Asian populations in the United States, there is less evidence for a greater direct negative effect of the virus in this population. Conversely, Indigenous populations in the United States have been severely and disproportionately affected. He highlighted key factors, saying that they are often confined to reservations and typically in rural areas, much less well supplied. Kumanan Rasanathan, World Health Organization, also pointed out the lack of data specifically for Indigenous populations across many countries, but where available, data show important inequities.
Another participant asked about the problematic political discourse around health care in the United States, and how politicians can transcend their differences to address the inequities in a bipartisan fashion. Essentially, what is the most politically feasible way forward to balance coverage and costs? Blumenthal replied that there had been steady progress toward the expansion of coverage over the years, though it has been incremental, periodic expansion. The problem, he added, is actually fundamental to our political system, as the Electoral College grants disproportionate power to rural areas that tend to uphold conservative opinions. Much of what is needed to be addressed in health care will occur outside of the health system, he argued.
A participant asked Iwasaki about vascular disease prevalence that may result from COVID-19, as those infected by the virus, either through acute cases or long COVID often appear to incur damages to the vasculature,
resulting in damages to several organs. Iwasaki said this could occur in a few different ways. The virus may affect endothelial cells, which then become damaged because of infection. Another possibility is cytokines from the immune system can harm endothelial cells, causing damage or leakage. Even mild cases of COVID-19 can result in elevated cytokines, she mentioned. The blood–brain barrier may also be compromised.
As a bench scientist, she noted the very interdisciplinary approach that she and other colleagues have taken to try to build a relationship between politics and health. Her team is collaborating with data scientists and linguists, among others, to connect the technical science to broader social challenges and inform politics. She noted that the world is becoming more and more integrated, and platforms like Twitter are a good way to understand what is happening in other parts of the world and quickly share information.
Another participant asked whether the seemingly similar distribution of long COVID across populations that vary in vaccination or socioeconomic status could help bring people together to address the issue. Buonsenso was not convinced it could be that influential, as there is still disagreement and discussion about just how much the disease or the immune system plays a role in long COVID, or whether it is more psychosocial because of other disruptions through the pandemic. Iwasaki noted that she is hopeful it would bring people together, but historically diseases that affect women are often ignored or dismissed in the medical community, which has also been the case with long COVID. She predicted long COVID would definitely be seen in other countries, but many parts of the world will not have good data on incidence. There is even the potential of getting long COVID after vaccination. Those data are not easily accessible, she said but would be really helpful in informing the work and understanding how many people are suffering and what can be done about it.
Also related to vaccinations, a participant asked how vaccinations might affect long COVID and where the field might be in its understanding over the next year. Iwasaki explained that vaccine data are used as a window into the pathogenesis of long COVID, but the effect of vaccines on long COVID is variable, so it is difficult to tell whether vaccines alone will be a solution. A better approach is needed to at least understand who might benefit more from the interventions, she said. For example, vaccines might be removing the viral reservoir in people. If a sufficient biomarker for a viral reservoir can be identified, then those patients can be categorized and given antivirals or other therapies to remove the reservoir. Other patients suffering from autoimmunity might benefit more from immunosuppressants, but researchers need to understand the fundamental pathogenesis, she argued.










