2
Family-Focused Interventions in Health Care Settings
The workshop began with opening remarks from Leslie Walker-Harding, chair of the workshop planning committee and chair of pediatrics at the University of Washington. She explained that most adults with substance use disorders (SUDs) begin using substances in adolescence, marking this period of life crucial for interventions targeting prevention of SUD. While adolescents do not have the highest rates of overdose, she said, these rates increase significantly for people age 24–34. Walker-Harding commented that preventing overdoses needs to start in adolescence and that, generally, people use drugs for about 10 years before their likelihood of mortality starts to increase. She also noted the critical disparities in overdose death rates based on race and/or ethnicity—Latinx and Native American people have higher rates of overdose mortality than White, non-Hispanic Americans (Friedman et al., 2022). These disparities are often linked with differing rates of exposure to adverse experiences, which are often risk factors for substance use, Walker-Harding explained.
According to the 2019 Youth Risk Behavior Survey conducted in high schools, Walker-Harding noted one in seven high school students reported misusing prescription opioids. Mental health struggles can be a reason some youth use substances, she said, but there are many other risk factors to consider as well. She explained that while people often assume peer pressure results in other youth using drugs, research shows parents and caregivers also have high levels of influence.
More than 35 percent of children under 18 will try a substance at least once, said Walker-Harding. Although this number has decreased in recent years, it is still important to ask why adolescents are willing to take risks
related to substance use. She acknowledged that adolescence is the time in which youth are most developmentally likely to engage in risk-taking behavior, and noted that such behavior is an important part of their growth into adulthood. However, Walker-Harding said, caregivers should help their adolescents identify healthy risks.1 She presented evidence that when youth choose not to use substances, they are more likely to graduate and less likely have depression and anxiety.2
In discussing the importance of prevention efforts, Walker-Harding shared data showing the discrepancy in federal drug control spending that goes toward prevention programs compared with the investment in law enforcement and treatment programs for substance use disorder (see Figure 2-1). If funding is redirected further upstream, she noted, fewer people would be in need of rescue, and fewer people would suffer substance use-related morbidity and mortality as adults. Walker-Harding thus called for more funding to focus on evidence-based prevention efforts.
The remainder of this chapter looks at a program within a large health care system, and discusses motivations for and the importance of family-focused interventions. It considers the potential for increasing effectiveness of prevention efforts by expanding the focus from the individual patient to the patient’s family and close network. Finally, the chapter ends with potential policies that can be leveraged to support these interventions.
A SYSTEMS PERSPECTIVE
Breda Velasquez, a child and adolescent psychiatrist at Kaiser Permanente Medical Care, introduced work within Kaiser Permanente’s San Diego Medical Center explaining that primary prevention is a new area of emphasis for this system. To better understand how its prevention efforts could best be targeted, the medical center leadership conducted a survey of their pediatricians to identify common challenges in pediatric settings. They received a nearly uniform response around two key issues: anxiety disorders and substance use. Recognizing that resources for anxiety are more readily available than resources for substance use, their team decided to focus on primary prevention for substance use with the intention of reducing the number of adults in their mid-twenties and early thirties requiring crisis care and hospitalization.
___________________
1 Healthy risks benefit adolescents’ well-being, carry mild potential costs compared with unhealthy risks, and are generally socially acceptable (Duell and Steinberg, 2019). Examples include participating in a team sport, public speaking, or asking someone out on a date (NASEM, 2020).
2 For more details on these effective parenting programs see https://www.blueprintsprograms.org/program-search
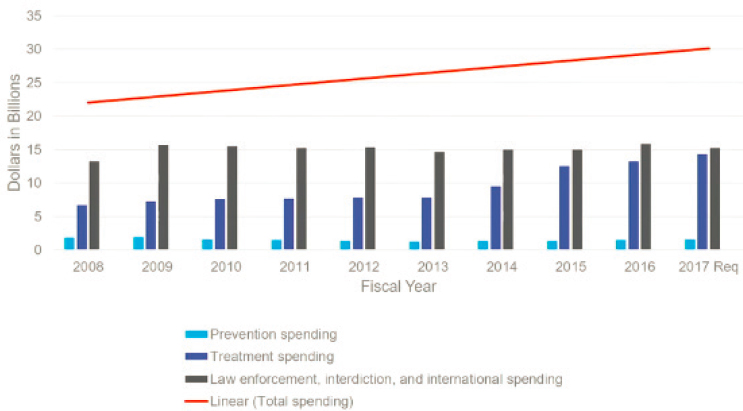
SOURCE: Walker-Harding’s presentation, May 5, 2022.
Since tackling this would require additional resources, the team developed a framework for approaching the work and securing buy-in from the executive leadership. Velasquez noted they first attempted to identify existing programs within the health system that could be expanded, but found no such programs. Instead, staff expressed that a substance use prevention program would be greatly appreciated.
Considering existing pediatric practices, Velasquez noted two questions asked as part of an 11-year-old well-child visit, one related to alcohol and drug use with the other asking if the child is around people who smoke. Recently, a third question was added to this line of questioning, asking whether the child has ever used drugs, alcohol, pills, cigarettes, or other substances. She heard from a few physicians that while some caregivers answer “yes” on behalf of their child to this last question, the physician often did not know what next steps to follow, highlighting the need for tools for pediatricians working directly with these patients.
Understanding the best age to target a new prevention program was also a challenge, noted Velasquez, Kaiser Permanente’s San Diego group thus contemplated whether 11 was too old or too young. In California, substance use issues become confidential at age 12, which can make it difficult to involve caregivers in critical conversations, she said. Therefore they decided to target their intervention at children aged nine or 10. However, Velasquez emphasized that a focus on substance use prevention should continue over time with pediatric patients. Furthermore, while some nine-year-olds may be very familiar with these topics, others may be less able to
grasp the messages. She suggested a focus on opening dialogue with this age group and creating a safe space where a child can ask questions without fear of getting in trouble.
Kaiser Permanente’s San Diego group next considered how to provide education to caregivers and families. While programs and events are available for parents and caregivers at schools, they are often led by law enforcement presenting extreme cases and lack actionable tools, Velasquez said. While families often view frontline providers, like pediatricians, as trusted messengers, she noted, time constraints limit patient visits and adolescents are less likely to come in regularly for well visits as they get older. Although the COVID-19 pandemic halted the development of this program, Velasquez noted the pandemic has worsened mental health for many youth, and the need for such interventions is likely greater now than before.
MAKING THE CASE FOR INTERVENTIONS
This section focuses on the motivations and justifications for family-focused interventions targeting prevention. Speakers discuss the impacts of interventions on children and families, the structural racism that affects successful outcomes, and the potential for culturally sensitive interventions for specific population groups.
Impact of Substance Use Disorder
Beginning with a real-world case example, Hoover Adger Jr., professor of pediatrics at Johns Hopkins University School of Medicine, described his experience with a panel of patients as a new faculty member at Johns Hopkins Hospital. That panel included a 10-year-old boy who had insulin-dependent diabetes. Every 2–3 months, he said, this boy would be admitted to the hospital because his blood sugar was too high and Adger’s team was struggling to understand how to keep the boy more stable. Adger tried multiple approaches, including diabetes education, but nothing was effective. Finally, he sat down for a detailed family history and learned that the boy was diagnosed at the age of two. He also learned the boy’s mother was the one responsible for administering his insulin. When impaired by her alcohol use disorder, she would sometimes administer too much or too little insulin in the syringe. Adger reported that after helping the mother get into treatment for her substance use disorder, the boy did not have any more diabetic-related hospitalizations over the next 10 years.
From this experience, Adger realized that centering the family in a patient’s care could have multiple benefits, including the recognition that treatment for parents and caregivers is often a form of prevention for their children. He shared data showing the number of children who have either
one or both parents with a substance use disorder, with about 7 million children having both parents affected (see Figure 2-2).
To underscore the point that many children live in these situations, Adger added that 9.7 million children were living in households in which one or more adults were using alcohol harmfully (Grant, 2000). One in every four children in the United States is exposed to alcohol use disorders in their family, he said, resulting in children being thrust into environments that pose extraordinary risk to their well-being and threaten their potential. Sadly, Adger noted, most of these at-risk adolescents go undetected. In a study his team conducted, they found that zero percent of cases in which children were exposed to substance use disorders at home were correctly identified.
Summarizing data from the literature, he shared two relevant conclusions. The first is that family variables and dynamics can affect a child’s outcomes. Second, two dimensions characterize parent-child interaction: the ability to provide nurturance, warmth, and support, and the ability to provide supervision and monitoring.
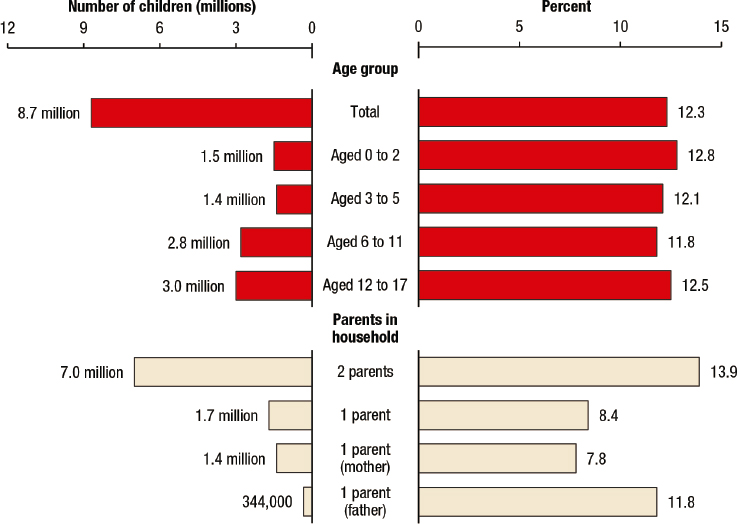
SOURCE: Adger’s presentation, May 5, 2022. Data from the National Surveys on Drug Use and Health, 2009 to 2014, Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration.
Adger introduced the family disease model of addiction (see Figure 2-3), saying that children living in these environments may have increased risk because of genetic, psychological, or environmental factors. They often learn early in life to avoid talking about family business and may lack trust in others or themselves.
Competencies and Roles of Providers
It is crucial to be aware of the medical, psychiatric, and behavioral symptoms of substance use disorder, said Adger, but it is also crucial to be aware of the benefit of timely and early intervention. He suggested core competencies for health care providers working with families affected by substance use, including being familiar with community resources, providing appropriate screening for substance use, and communicating appropriate concern while offering information and support (Adger et al., 1999).
The role of primary health providers can include multiple aspects of prevention, screening, and treatment. For example, Adger advocated for primary health providers to educate patients and families about the dangers of and risk factors associated with substance use, to screen for risky substance use, to provide interventions as well as referrals for assessment, and to help make connections to treatment services for cases that require more resources and expertise. However, while the evidence supports primary care
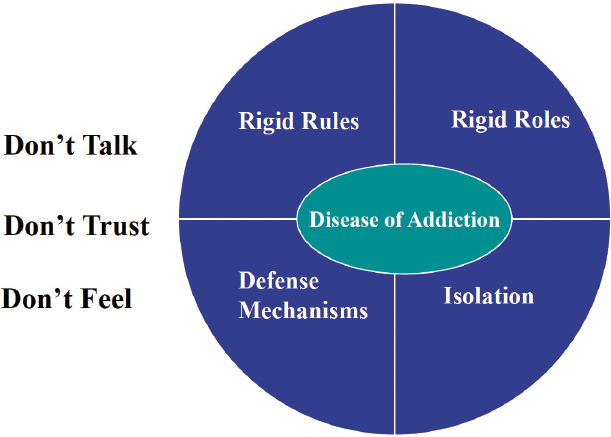
SOURCE: Adger’s presentation, May 5, 2022.
providers as ideal messengers for prevention and early intervention, he said, few providers have the skill set and knowledge to do so. He acknowledged the numerous barriers to prevention work, but suggested the barriers could be overcome through improved integration of evidence-based interventions. In summary, Adger said a little bit of caring goes a long way. Communicating with youth about making healthy choices can help them become children of promise instead of risk.
Acknowledging Historically Racist Systems and Their Role in Achieving Outcomes
Even though some may pretend otherwise, adolescents get a bad rap, said Kimá Joy Taylor, founder of Anka Consulting LLC. However, she said, the goal is for adolescents, their families, and their communities to thrive. While prevention, screening, and treatment programs associated with health concerns such as diabetes or sexual health are not perfect, Taylor said, at least they provide a way to talk about those concerns without causing more harm—something yet to be figured out for substance use. She commented that approaches to addressing substance use are historically laden with racism, judgment, and attacks on drug users. Without deconstructing this historical perspective, Taylor noted, it will be difficult to provide effective family-focused prevention interventions in health care settings. She called for a relearning of the health care, social service, and school systems. Without acknowledging the structurally racist and punitive history of approaches to substance use, she said, it will be difficult to achieve equitable outcomes.
Taylor identified several challenges to implementing family-focused interventions in culturally and linguistically effective ways, which can ultimately lead to more equitable access and outcomes. First, substance use is not recognized as a stand-alone concern and is often paired with mental health concerns. Instead, Taylor said, substance use, not just mental health or substance use disorder, needs to be addressed. The second challenge she highlighted is that interventionists often do not reach the people who need or want services. She advocated for including youth and families from all different backgrounds in the creation and evaluation of a new prevention-focused system. Another challenge she noted is lack of trust in the health care system, which becomes more prominent as children become adolescents, and she emphasized the importance of authentic partnerships with youth and their families.
Taylor highlighted opportunities for addressing these challenges to realize better outcomes for youth. For example, she noted that outcomes-based payments could define outcomes based on feedback from diverse youth and the community. Different children and different communities will have different needs, she noted. There is also an opportunity through collecting
data to ensure that efforts are effective, while also ensuring data collection is not used to stereotype or harm. When the data reveals that efforts are ineffective, providers should reevaluate, reconfigure, and find a way to intervene more effectively, she said.
Finally, Taylor emphasized the need for a focus on equity. Many assume it will be included, she said, but that has yet to be true. Instead, she advocated for equitable access and culturally and linguistically effective interventions to meet the needs of all youth.
Creating a Culturally Relevant Prevention Intervention
John Lowe, professor at the University of Texas at Austin School of Nursing, introduced himself as a Cherokee tribal member, and explained that most of his work is centered on community-based participatory research (CBPR), which is very important for Native American communities. He emphasized a common belief that substance use is worsened by the dispossession of culture, land, and identity of Native Americans over generations. The elders in his community felt a focus on youth was necessary to save both their people and their culture. As the three basic guiding principles of an effective intervention, Lowe said, the youth need to know who they are, where they are, and where they are going.
Lowe described the talking circle intervention, based on the Native-Reliance Framework which was built around traditional and cultural approaches. The intervention runs once per week for 10 weeks, beginning with a session asking the youth to consider the question “who are you?”
Lowe explained his community ensures the youth involved understand it is a confidential, safe space. Their approach has three layers, the first being the community center facility itself, where the intervention sessions are held. The second layer is the school, in which many of the youth feel a high level of support. Finally, the third layer is the tribe or community partnership level.
Lowe explained that they started this work with high school-age adolescents and approached it as prevention and early treatment. However, feedback from participants encouraged them to start the program with younger children and to increase the emphasis on prevention. They work within the school system to provide sessions to families and obtain consent for youth participation from parents. Sometimes, Lowe said, when parents build trust with intervention providers, they disclose their own concerns, and the program can connect them with appropriate, non-judgmental resources.
Lowe provided an example of a session discussion, in which he would ask the youth in the group what they would do if a bear came in the room—run or stay and fight? He uses this to teach fight or flight responses, how cortisol works in the body, and what happens when cortisol levels remain
elevated for long periods. They then shift to using the bear as a metaphor and talk with the youth about what their “bear” is—whether it’s parents coming home in a “bad way,” not having a place to sleep, missing a meal, or a situation at school that makes them anxious or stressed. Whatever the case, Lowe asks what their strength is, which is often steeped in ancestral knowledge and traditions. He discusses alternatives to substance use for youth to deal with their metaphorical bear showing up. Sometimes they rely on the community members or elders to help youth identify their traditions and integrate them into their routine. While the intervention is 10 weeks long, Lowe said that once that intensive period ends, some of the youth become peer leaders and give similar sessions in camp settings or other venues. This is often only a catalyst, he noted, and initiates conversations with families in a nonthreatening way.
In evaluating the program, Lowe shared that 12 months after program participation, interest in substance use often continues to decrease. When the intervention has cultural significance, he said, youth are better able to connect with and internalize it. Programs without cultural competency are far less effective. As a next step, the program has received funding from the Rita and Alex Hillman Foundation to scale it to a county school system with a high percentage of Native American youth.
Discussion Session with Panelists and Workshop Attendees
A participant asked about the definition of family in these efforts and pointed out that a nuclear family is not the main avenue of support for many youth. Vincent Guilamo-Ramos, planning committee member and dean of the Duke University School of Nursing, responded that, when thinking about family, important mechanisms include a notion of monitoring and supervision, as well as nurturance, connectedness, role modeling, and communication. This does not need to be a biological parent, Guilamo-Ramos continued, but the people in that child’s life who have primary responsibility for enacting those mechanisms.
Nataki MacMurray, prevention policy analyst at the Office of National Drug Control Policy, asked about the opportunity to scale additional substance use screening. Lowe responded that many screening efforts happen at the community level or in school systems but not as much within the health system. Since teachers are with the children every day, they are likely to know what is happening in their students’ lives and may be more apt to follow up. However, Lowe said, the degree to which this occurs depends on resource availability within schools.
MacMurray also highlighted the importance of messaging to change the conversation around substance use, as well as navigating the best ways to integrate that messaging into family-focused interventions. Taylor agreed,
and shared that her own children mock the current public service announcements about opioids and vaping. Instead, she argued, adults should simply have open conversations with youth. She said youth deserve messages that are effective and clear. Adger added that there is also evidence on effective messaging to educate adolescents on risks associated with specific behaviors. When risk perception increases, associated behaviors decrease, he explained. Involving parents or caregivers who have an active substance use issue is another challenge, and Lowe noted that his communities approach is to talk about the family dynamics and history in a nonthreatening way. Adger added that providers need to ensure they are not shaming or humiliating parents, but are helping them understand how their behavior affects their children’s behavior.
LEVERAGING SUPPORTIVE POLICIES
While there are compelling reasons for family-focused prevention efforts, questions often arise about the best ways to fund and support them. This section offers ways to support a broader approach, potential state level policies to support prevention, and ways to leverage or incorporate Medicaid to bolster efforts.
Need for a Broader Approach to Prevention
Linda Richter, vice president of prevention research and analysis at Partnership to End Addiction, shared some of her work on promoting a broader and earlier approach to prevention. She highlighted that many current prevention efforts focus on adolescence because it is a period of intense brain development and the developmental stage most vulnerable to taking risks, including experimenting with substance use. However, she said, the earlier someone initiates substance use, the higher the risk of substance use disorder (see Figure 2-4). Thus, early intervention is crucial and starting prevention efforts earlier in life may be beneficial.
Richter shared data that showed encouraging trends over the last few decades with decreasing numbers of young people in the United States using nicotine, alcohol, or other drugs (Levy et al., 2020). Providing context around this trend, she also highlighted the increasing trends in protective factors, such as parental monitoring, positive attitudes toward school, and strong youth disapproval of peer substance use. Furthermore, there have been shifts in approaches to addiction and substance use—moving from a strict moral model to a biopsychosocial model in which various risk and protective factors are taken into account. The good news is that rates of non-use are increasing, she said, and there are more nuanced views to addiction and prevention. However, youth who do still use tend to do
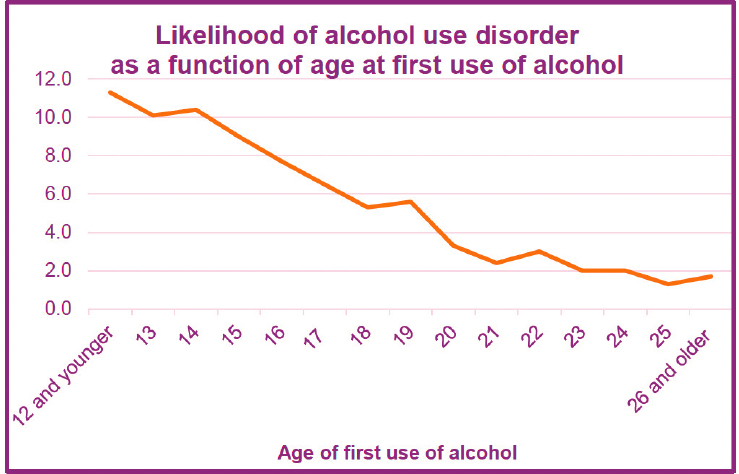
SOURCE: Richter’s presentation, May 6, 2022.
so excessively, and the current youth mental health crisis could lead to increased rates in the near future.
What Can Be Done?
Current approaches to substance use prevention have limitations, Richter noted. Even though mitigating risk factors and strengthening protective factors within the family and community are understood to be important, they are not always prioritized. Traditional approaches to prevention tend to focus on reducing risk instead of promoting health and resilience, and target the child to the exclusion of the influences on the child in the surrounding environment, Richter said. She argued that the focus is too narrow and puts too much burden on the parents and caregivers. There is often an over-focus on evidence-based programs for prevention with outcomes available in a short time, which misses evidence on long-term outcomes that are costlier and more difficult to measure. Additionally, she added, the ideal outcome of not using substances is a nonevent, meaning it is difficult to measure the effectiveness of a prevention program because you are measuring a null.
Richter suggested the substance use field could absorb lessons from other fields in child development. Substance use is often siloed, she said, but other fields are looking at the same risk and protective factors. While
the outcomes might be different, there is a lot to be learned from researchers and practitioners working to reduce child poverty or increase child literacy, for example.
Why the Early Years Matter
Richter reviewed the impacts of adverse childhood experiences (ACEs) and other factors that can affect brain development in children, including any type of abuse or neglect, family mental illness, or being exposed to violence towards a parent. These experiences lay the groundwork for future risk. When the ACE is prolonged, she said, it can produce a toxic stress response which interferes with normal brain development and effects can often be intergenerational. Although it is unusual to think this way, she noted, building a framework to address risk factors even as early as infancy and early childhood would be a valuable approach. For example, ensuring prenatal nutrition and supporting positive parenting practices in order to create a secure parent-child attachment can provide a strong basis for substance use prevention, she said. Addressing risk factors such as poverty can also influence outcomes. Research has demonstrated that cash payments to low-income families can result in faster brain activity within the baby’s first year of life, as well as improved brain development (Yoo et al., 2022).
Supporting a Broader Approach to Substance Use Prevention
Richter said that intervening earlier and more broadly can help to promote child health, prevent youth substance use and addiction, avoid future drug epidemics, and reduce the damaging consequences of addictive substances on future generations. To achieve these outcomes, she offered several approaches, outlined below:
- Broaden the focus: Current efforts are necessary but insufficient. There is a need to go beyond the individual target and include structural influences on risk and protection.
- Apply the “Swiss cheese” model: Prevention should be a layered approach, targeting each level of risk separately (i.e., sociocultural, community, school, family, and individual), creating comprehensive protection.
- Providers lay the groundwork: Providers can educate parents about different risk and protective factors, screen young patients for all types of risk—including adverse childhood experiences—and provide counseling and parenting support.
- Take advantage of the policy climate: The COVID-19 pandemic raised awareness of the need to focus on efforts to protect youth,
- Facilitate healthy child development: This requires federal-level efforts, including ensuring family income, food, and housing security; supporting quality child care and paid family leave; providing support to strengthen parenting skills and help accessing mental health and addiction treatment; and supporting programs that nurture childhood health, resilience, as well as self-regulation.
- Promote collaboration, and coordinate funding and management of youth protective services: This includes establishing a federal coordinating body focused on children’s health and well-being, including data reporting requirements in social determinants of health policies, and applying a significant portion of state opioid settlements to bolster prevention infrastructure in an equitable way.
- Support direct services to parents to strengthen parenting: Support could include improving insurance reimbursements for parental health care services that can help foster a safe home environment for children, strengthening enforcement of laws and regulations to prohibit discriminatory coverage of benefits for mental health and SUDs, and supporting parenting education and home visiting programs.
- Support direct services to children to promote health and reduce risk: This includes efforts to incentivize routine pediatric screening for a range of risk factors in children, expand and make permanent COVID-relief funding for school-based mental health services and family poverty reduction efforts, invest in social-emotional learning interventions, and invest in training for school psychologists and counselors in primary prevention.
- Ensure sustainable funding for a broader and earlier approach to prevention: This can be done through documenting short- and long-term effects of investments in family health and stability on youth risk, tracking changes in risk factor prevalence for ACEs and protective factors, and monitoring longer-term effects of prevention programs on youth substance use.
and government attention has turned to the importance of investing in early social determinants of health. Opioid settlements also provide an opportunity to dedicate state funds to early prevention.
State-Level Policies to Support Family-Focused Interventions
Vinu Ilakkuvan, founder and principal consultant at PoP Health, LLC,3 reviewed state policies to support the types of family-focused prevention
___________________
3 PoP Health is a public health consulting agency that aims to help communities and organizations prioritize prevention by more effectively addressing upstream social determinants of health. For more information, see https://www.pophealthllc.com/about-1
interventions from a population- and systems-level perspective. Many approaches in health, she said, are trying to fit a square peg into a round hole. The square peg represents single-person solutions and after-the-fact treatments, while the round hole represents population- and systems-level preventive solutions that could influence shifts in public health. Applying this lens to the topic of adolescent substance use, Ilakkuvan said there are three key focus areas. First, a population-level focus includes the role of schools and other key settings. Second, a systems-level focus highlights the need for more meaningful family engagement. Third, a prevention focus speaks to starting younger and sustaining supports through adolescence.
Schools, the first focus area, are often a key setting for health care delivery, Ilakkuvan commented. Between 70 and 80 percent of children receiving mental health supports receive them in school (Rones and Hoagwood, 2000), so the importance of this setting cannot be overstated, she said. Additionally, primary health care can also be delivered in jails, detention centers, and even at home.
Furthermore, it is imperative to enhance family engagement across all child-serving systems, she argued, as families are a key influence for adolescents. Echoing back to Adger’s earlier comments, Ilakkuvan said researchers and practitioners need to talk and deeply listen to families, and move away from blaming and shaming them, noting it should be easier for families to connect with information and strategies they can use to prevent adolescent substance use. She provided examples from her work in school mental health in Washington, DC, and Northern Virginia, where schools have designated family liaisons or community-based family peer support partners who have navigated the system for their own child and can now guide others to connect with families. Leaders in this field should also equip providers with the training they need to engage effectively through positive youth development and trauma-informed approaches, she said.
Ilakkuvan concluded by reiterating the need to start prevention work earlier in life, knowing that substance use is a behavior that can be passed down through generations. This also intersects with trauma, she noted, as a parent’s trauma contributes to their substance use, which then contributes to the child’s trauma, and so on. There is a great opportunity for investing in multigenerational services, she commented, and there should be greater investment in substance use prevention and treatment for those who are pregnant. Furthermore, she added, beginning with social and emotional learning for preschoolers and sustaining prevention work as children get older will be critical in facilitating better outcomes.
There are also state policies to help in promoting implementation of effective family-focused interventions, and Ilakkuvan highlighted five key areas for advancement through state policy: collaboration and community
ownership; data collection and sharing; sufficient, flexible, and coordinated financing; technical assistance; and social policies broadly.
First, there are numerous examples of collaboration across home, school, and community. Ilakkuvan gave the example of Communities that Care (CTC), a prevention-planning system and network for promoting positive youth development, which involves building community partnerships to target risk factors such as antisocial behavior and family conflict before they become problems. A randomized controlled trial of 24 communities that received the CTC intervention found sustained positive impacts on youth behaviors. For example, students in participating communities were more than 31 percent less likely to initiate alcohol or gateway drug use and had 14 percent lower odds of engaging in violent behavior at the end of high school, eight years after CTC was first implemented (Hawkins et al., 2014). States can invest directly in these types of approaches, she explained, and can be especially impactful when they invest in partnership development, implementation, and maintenance. Often funders prioritize programmatic elements but neglect the infrastructure needed to sustain the program, Ilakkuvan commented. States can play a role in community partnership by funding and requiring CBPR in their grant awards. There is also an opportunity to build accountability into state and local government work, she said. For example, Accountable Communities for Health has done this through shared community health assessments and improvement plans.
The second area, data collection and sharing, is important for establishing common measures on family-level risk and protective factors, and fostering analyses that can show whether there is equitable access to and outcomes from various programs, Ilakkuvan said. She explained that the data collected by the state can be made publicly available and accessible to communities who can then use it to inform their own assessments and evaluations of programs; leading to a more evidence-based and objective review of efforts across the state. State agencies can also provide incentives to share data and require grantees to conduct rigorous evaluations so that data and evidence are continually generated to inform program efforts, she added. She gave an example of work in Allegheny County, Pennsylvania. The Department of Human Services within the county operates a data warehouse, which is a central repository of cross-sector data that includes measures related to juvenile justice, early childhood substance use, mental health, and public schools. The warehouse allows data sharing among county departments and other local school districts in order to encourage effective policy making.
Another opportunity for state policy is through sufficient, flexible, coordinated financing, Ilakkuvan said. States can invest directly in substance use prevention strategies and fully leverage existing policies that enable use
of child welfare funds for things like mental health or parenting programs. Using Medicaid and insurance as an example, Ilakkuvan noted that some clinically licensed agencies bill Medicaid for the Strengthening Families Program as family group therapy. A large number of provider types can deliver many of these interventions, so thinking about how to expand insurance reimbursement to cover those beyond physicians is another financing opportunity. She highlighted another often under-utilized Medicaid benefit, the Early Periodic Screening, Diagnosis, and Treatment program, which allows Medicaid to pay for well-child visits and other things related to the child’s well-being. Other funding opportunities at the state level include non-traditional mechanisms, such as “pay for success” programs and other outcomes-based financing models to scale prevention investment. It is important to not approach this from a siloed perspective, she continued, so states can enable better coordination of funding through “blending and braiding.” Funders at all levels can play a role in coordinating multiple streams of funding toward a unified goal and desired outcome. For example, the Children’s Services Act in Virginia blends funding in ways that support upstream substance use prevention. This type of blending means that case managers have flexibility to tailor their services to the individual needs of those families they are working with, including things like emergency rent support or car repair, that can keep adolescents safely housed and in school, she explained.
A fourth area, technical assistance, has been identified as a need to avoid reinventing the wheel or trying to recreate effective programs. It can be challenging for schools to determine the right set of programs; a state-level center could provide aggregated information and support implementation in different contexts, alleviating much of the burden on schools, said Ilakkuvan. As an example, the Evidence-based Prevention and Intervention Support center in Pennsylvania acts as a statewide technical assistance center and supports prevention by connecting research, policy, and practice. It also facilitates dissemination and sharing of best practices, provides technical assistance and access to learning networks, and supports continuous improvement of locally developed positive youth programs.
Finally, states can adopt a range of social policies for advancing prevention of adolescent substance use, she said. Some of these are relatively direct, such as expanding Medicaid and strengthening insurance parity for mental health and substance use services, investing in the behavioral health workforce, and passing policies that make it harder for youth to access alcohol and drugs. Other policies are broader, and related to upstream causes like prevention of bullying, reform of school discipline policies, reduction of incarceration, and provision of economic assistance to low-income families. The health care sector can play a role in advocating for these policies to support the health of children and families, Ilakkuvan concluded.
Opportunities to Support Prevention through Medicaid
Kelsey Brykman, senior program officer for the Center for Health Care Strategies, supports Medicaid agencies in advancing payment and care delivery models to enable better and more equitable care. She noted that work on substance use prevention is well aligned with the current Medicaid policy priorities. Medicaid has been increasing its focus on reducing the longstanding health inequities that have become more apparent in recent years, and policymakers are becoming aware of the behavioral health crisis among adolescents.
Within Medicaid, there are several policy levers to consider, said Brykman. She focused her remarks on what is covered within Medicaid and how certain interventions can be financed. To provide some background, she explained that state Medicaid agencies set health priorities and determine what services are covered at a basic level. Some Medicaid agencies contract with providers directly, but many states run Medicaid through a managed care program. She acknowledged that Medicaid billing is very complicated, which results in challenges when thinking about how to pay for and scale new evidence-based interventions. To understand how policymakers at this level think, Brykman highlighted two components of Medicaid: state plan elements, which describe how each state administers its Medicaid program, and waivers, which allow flexibility beyond existing federal regulations. While developing waivers can be time intensive, they can be an important policy lever for innovative models. The 1115 waiver, for example, gives broad authority to test policy innovations, she explained.
Brykman highlighted a couple examples of innovative care models and services related to SUD prevention that Medicaid agencies are supporting through state plan amendments. Some states use Medicaid to cover services provided by staff with lived experience, including community health workers supporting team-based care or youth peer support services. Home-visiting programs are an example of how Medicaid can cover part of an intervention, such as the care management component of a home visit, without covering the entire intervention. This also highlights the importance of blending and braiding funding opportunities within the state. Brykman described North Carolina’s Health Opportunities Pilots as an example of how states are addressing health-related social needs through 1115 waivers.
When considering coordination with Medicaid managed care organizations (MCOs), Brykman said, it is important to think about how to monitor and incentivize plans. For example, she explained that states may set and monitor network adequacy standards for primary and behavioral health, or tie a portion of managed care payment to specific quality measures related to prevention. Additionally, states can require plans to participate in quality
improvement initiatives, she said. As just one example, Brykman explained how Oregon ties a portion of payment to its care coordination organizations (networks of health care providers, similar to MCOs in other states) to meeting performance targets, including metrics related to screenings and brief interventions for substance use, as well as supporting social-emotional health of young children. She added that Oregon also requires care coordination organizations to participate in a performance improvement project aimed at improving access to mental health services.
Many states and other payers are moving towards value-based payments that link financial incentives to providers’ performance on a defined set of quality measures. Brykman explained that such models could potentially support SUD prevention efforts by: (1) offering financial incentives for the adoption of evidence-based interventions and (2) providing more upfront payment in order to allow providers more flexibility to deliver innovative care models that may not be supported by fee-for-service payment. As there is limited opportunity for short-term cost savings for the pediatric population, value-based payment models for this population should focus more on supporting quality improvement, Brykman said. It is important to consider how to define value broadly, beyond just cost of care, to advance interventions aimed at SUD prevention.
Brykman gave one example of state efforts to improve primary care through more flexible, value-based payment in Washington State, which is designing a multi-payer Primary Care Transformation Model aimed at increased investment in and incentives for integrated, whole-person, and team-based care. Another example is the Center for Medicare & Medicaid Innovation’s Integrated Care for Kids model, through which a state-specific delivery system and payment models will be piloted to improve early identification and treatment of health needs in a more integrated way, she explained.
A particular challenge Brykman noted with state care delivery reform efforts (such as those implemented through 1115 waivers) and value-based payment models is their tendency to work on a short time frame, which is difficult when working with prevention efforts, as results can take much longer to realize. Current time frames are often limited to a one- or five-year period, so Brykman advocated for extending these time frames or developing other ways to reward stakeholders for interventions with longer-term benefits in order to support more prevention approaches and allow for gathering evidence on their effectiveness. Due to pressures to reduce costs, many care delivery reforms are focused on adults with complex needs, she said, but there are opportunities for states to develop programs with the unique needs of children and adolescents in mind. Finally, Brykman again highlighted the opportunities for braiding and blending funding across different government sectors to support interventions aimed at prevention.
Discussion Session with Panelists and Workshop Attendees
One of the first comments from participants was related to the emphasis on ACEs as predictive factors in pediatrics, and highlighted the known protective factors that should also be articulated to families. Ilakkuvan noted that these protective factors also bring a meaningful additive value to understanding how interventions can be better developed. Richter added that even for children with many ACEs in their young lives, having just one protective factor or positive experience can change their trajectory.
The discussion also centered on funding and accountability to encourage a more comprehensive approach to addressing multiple risk factors simultaneously. Brykman emphasized the importance of cross-sector collaboration or having multiple agencies at the state level aligning themselves on outcomes that matter, so that there is a common metric or goal. Disseminating the evidence and building a case among policymakers to emphasize or monitor child health can help bring accountability to the state level, she said.
Furthermore, Brykman and Walker-Harding both commented that the conversation needs to move beyond screening only, and focus further upstream on more preventive efforts, as well getting prevention interventions covered universally by insurance. Ilakkuvan suggested that several interventions have strong evidence in preventing adverse outcomes, which the federal government could fund, including prenatal care, early childhood, and parenting supports. Right now, the health paradigm in society is focused on the individual, Ilakkuvan continued, but until that shifts to thinking about the population more broadly, it will be difficult to build public support for these efforts.
Several funding mechanisms are currently available because of opioid settlements and COVID-19 funding, as well as momentum for greater support for mental health and substance use prevention. Many speakers argued that much of this funding should be used to build infrastructure and implementation support for interventions that will be sustainable over the long term. Ilakkuvan suggested having backbone organizations working on collaboration, along with financial intermediaries, so that the coordination of financing is seamless. People get very excited about individual programs, she said, but excitement is also needed around establishing long-term infrastructure that can be customized to the needs of different communities.
This page intentionally left blank.




















