2
The Decision-Making Process of Leaders
Session objective: To understand the decision-making process of choices made by educational leaders during the COVID-19 pandemic related to the role of students in the health system.
Erin Patel, acting chief of health professions education for the Office of Academic Affiliations at the Veterans Health Administration, led off the first of the six workshop sessions by welcoming the three panelists, the forum members, and the other participants joining the virtual workshop. She then passed the microphone to her comoderator, Robert Cain, president and chief executive officer of the American Association of Colleges of Osteopathic Medicine, to “describe some of the thinking that went into the design of today’s session.” Cain explained what led to his presentation of a first draft of a decision tree. As part of this decision tree, he said, speakers have been asked to share their recent experiences in how decisions were made to remove learners from in-person, experiential learning at the start of the pandemic. First, Alison Whelan described the process the Association of American Medical Colleges (AAMC) went through. Next, Julie Kornfeld from Columbia University outlined the thought process and steps they went through with the public health program. Finally, Kecia Kelly from Legacy Health explained how the decision was made in Portland, Oregon, to pull nursing students from clinical rotations.
ASSOCIATION OF AMERICAN MEDICAL COLLEGES
Alison Whelan, Chief Medical Education Officer
The Physician Charter on Professionalism of 2002 emphasized the primacy of patient welfare, patient autonomy, and social justice, said Alison Whelan. These, along with the AAMC mission statement, were the guiding principles of the AAMC response to the COVID-19 pandemic. When thinking about the role of learners in the clinical setting, she added, there are three main priorities: patient care and safety, public and population safety, and student learning and safety. Medical trainees have always been expected to assume some personal risk as clinical care givers, Whelan noted, and there is always an effort to balance those risks based on the skill level of the learner and the responsibility learners had to their team, as well as minimizing the risk to patients. For example, influenza infection has always been a routine risk taken by learners; it is considered a low risk if personal protective equipment (PPE) is available. When COVID-19 struck, the challenge was to figure out what differentiated COVID-19 risks from those associated with influenza or other transmissible diseases.
In March 2020, it was known that COVID-19 had high transmissibility, an asymptomatic contagious phase, and high morbidity with relatively high mortality. Some parts of the country exhibited elevated levels of community spread, while other parts had relatively few or no cases. Importantly, Whelan emphasized, there was insufficient PPE and testing was not available. Prior to the pandemic, learners were generally thought of in terms
of how they affected patient care and safety. However, COVID-19 placed new emphasis on the potential for learners to affect public and population safety—that is, to either spread disease or to help “flatten the curve.” This consideration (Figure 2-1) drove AAMC’s decision-making process in the early phase of the pandemic, said Whelan.
As no one at AAMC had been through a pandemic before, it was a time of uncertainty and required a thoughtful decision-making process that involved three components where AAMC
- identified data gaps, ethical conflicts, and its role as a decision maker;
- used its mission, values, and data; and
- created a rapid-cycle core team, as well as trust reviewers across the continuum.
AAMC’s mission is to “lead and serve academic medicine,” said Whelan, and it was challenging to determine the appropriate role of leading versus serving. During noncrisis times, AAMC takes on several roles. These include creating guidelines and recommendations for members, collecting and disseminating resources, convening members and constituents, and providing public statements. Such roles were critically important during COVID-19 as well, Whelan commented. For example, AAMC collected data on what schools were doing if students were not working in clinical settings, and disseminated resources on alternative educational approaches.
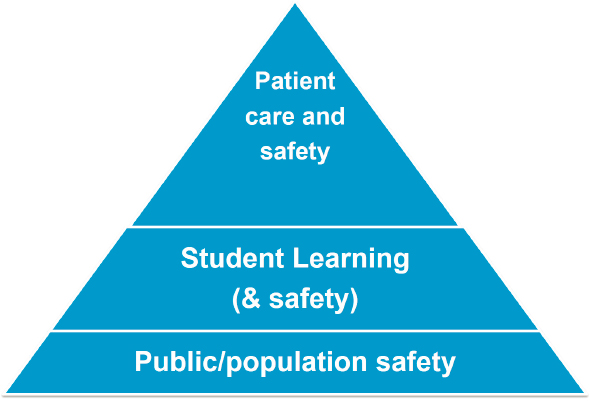
SOURCE: Whelan presentation, September 30, 2021.
AAMC released a three-page guideline in March 2020 about student involvement in patient contact.1 The guideline stated that AAMC “strongly suggest[s] that medical students not be involved in any direct patient care activities” in areas where there is significant spread of COVID-19, limited supply of PPE, or limited availability of testing. Whelan emphasized this was guidance rather than a recommendation, and that every school needed to do what worked best with its mission, the local pandemic situation, and the needs of local stakeholders. Furthermore, she said, the driving motivation behind the guidance was an urgency to “bend the curve” for public health, conserve PPE, and maintain public and health care worker safety, given limited testing capacity.
In August 2020, AAMC added an addendum to the guidance,2 which introduced the idea that while individual medical students are not “essential workers,” medical students as a group are “the essential, emerging physician workforce.” As such, “Clinical education of medical students, including direct patient contact … must continue, with appropriate attention to safety.” This addendum, said Whelan, was motivated by the fact that there was some resistance among hospitals and clinics to bringing students back to clinical settings or to providing them with PPE. The addendum pointed out today’s students are tomorrow’s workforce for these hospitals and clinics. To this point, Whelan noted how early graduation was encouraged among fourth-year students with demonstrated skills and competencies for entering the workforce but also underscored the point that a learners’ contributions to health care teams depended heavily on how far along they were in training.
The work of AAMC has continued to evolve over the course of the pandemic, said Whelan, with a constant reevaluation of AAMC’s roles. The “part that doesn’t show up” in these official documents, she added, are the informal conversations between stakeholders. Whelan emphasized that she would call people “at 5 in the morning and at 11 o’clock at night” to discuss what was happening at medical schools across the country and what AAMC should be doing to lead and serve. What worked best, she said, was for AAMC to return again and again to its mission, its values, and the current data in order to decide how to both lead and serve its members and students.
___________________
1 See https://lcme.org/wp-content/uploads/filebase/March-23-2020-Interim-Guidance-on-Medical-StudentsE28099-Voluntary-Participation-in-Direct-Patient-Contact-Activities.pdf (accessed July 6, 2022).
2 See https://www.aamc.org/system/files/2020-08/meded-August-14-Guidance-on-Medical-Students-on-Clinical-Rotations.pdf (accessed July 6, 2022).
PUBLIC HEALTH: COLUMBIA UNIVERSITY
Julie Kornfeld, Vice Provost for Academic Programs
Julie Kornfeld spoke about how Columbia University made decisions regarding its learners in its public health program. There were a number of considerations taken into account in the decision-making process. Public health students are critical members of interprofessional health teams, and public health schools often share a campus, and even classrooms, with other health professions schools, said Kornfeld. Public health students are engaged in both didactic and experiential learning, and although they do not participate in clinical care, part of their training is being in the field embedded in community-based organizations.
New York City was one of the early epicenters of the epidemic, and Kornfeld remarked that public health students have a powerful call to service that leads them to “run towards an emergency.” There were also a number of key players involved in the process, including leaders across the university and the health professions campus, the Council on Education for Public Health (CEPH), state regulatory agencies, and legal and risk management offices. Kornfeld underscored that perspectives, guidance, and requirements of each of these stakeholders were considered to determine what was safe and feasible for students.
One aspect of Columbia’s Master of Public Health program that presented a challenge during the pandemic was the requirement for experiential learning. All students are required to be embedded in a domestic or international organization, and CEPH has very specific guidelines about what constitutes a field experience (e.g., the student must work with a community preceptor). When the pandemic began in spring of 2020, most students had finalized their plans for a summer experience. Fortunately, said Kornfeld, CEPH provided “maximum flexibility” and allowed schools to use creative solutions to ensure completion of the requirement. Nearly all students in both the summer of 2020 and 2021 completed their experiences remotely, with few exceptions.
There were both challenges and opportunities in shifting to a remote approach, said Kornfeld. Some practice sites were not able to accommodate students remotely, while others were eager for assistance and had increased needs during the pandemic. A need was identified to review and consider students on a case-by-case basis, which was “incredibly resource intensive.” If the original placement and activity were no longer possible, a new placement or activity had to be identified to ensure the student achieved the necessary competencies and learning objectives. For example, a placement involving going door-to-door to conduct a community survey would not be feasible in the early days of COVID-19, so a replacement activity had to
be identified. To ensure all students still had an appropriate learning experience, faculty turned to contacts in the community or served as preceptors themselves. In addition, students used existing relationships and, when appropriate, were given permission to fulfill their experiential requirements through their current place of employment.
Shifting students’ experiential opportunities from in person to remote was a “tremendous amount of work,” but led to a number of important lessons learned, Kornfeld noted. First, meaningful experiences are possible in a remote format; Kornfeld added that if “somebody told us this 3 years ago … we may not have believed them.” Second, the pandemic forced schools, students, and organizations to be flexible, which led to innovation; organizations were able to use students in new ways to advance their work. Third, there is an important opportunity to develop criteria for remote experiences based on what happened during the pandemic. Fourth, decision making should be informed by the pandemic, and the resulting innovations and flexibility could improve health professions education in both crisis and noncrisis times. Fifth and lastly, flexibility in regulation was critical during the pandemic, and it may be necessary to advocate for this flexibility to be extended to allow students to take advantage of meaningful remote opportunities in the future.
Kornfeld closed with an example of a student who was supposed to be embedded in a global organization in Chile and was “devastated” by the fact that these plans were derailed by the pandemic. However, when Kornfeld spoke to him several months later, he was energized about his experience working with the organization remotely on a data surveillance project. The organization was “incredibly short staffed” during the early days of the pandemic, and the student was able to step in and advance their work in a way that benefited both the student and the organization. While he missed out on some of the experiences he would have had face to face, it was nonetheless a successful experience and important public health work was achieved.
NURSING: LEGACY HEALTH
Kecia Kelly, Senior Vice President and Chief Nursing Officer
Legacy Health is a small, not-for-profit health care organization in the Pacific Northwest with about 14,000 employees, including 5,000 nurses. In July 2020, Legacy was still recovering from a staffing crisis, with over 1,500 open positions. Part of its workforce planning strategy, Kecia Kelly noted, was a residency program for new graduate nurses. The accredited residency program helped new nurses transition into practice by building confidence through hands-on experiences under the guidance of nurse preceptors and mentors.
In August 2020, 72 nurse residents joined the organization. As most of the residents had graduated nursing school during the pandemic, many of their final days of training were conducted virtually rather than in person. “This was a different landscape of new nurses,” said Kelly. In addition, Oregon was experiencing a new surge of COVID-19 cases and hospitalizations. Legacy made the “difficult decision” to pull nursing students out of clinical rotations so the organization could focus on making sure the new residents and current employees could be successful.
Kelly described the higher than usual patient loads for understaffed nurses, the need to protect and educate nurse residents, and the risk of burnout, before reflecting on how this experience led Legacy to develop a new approach for bringing nursing students back into the clinical setting. There were some core competencies, said Kelly, that new residents had missed out on developing, which meant residents had a “very steep” learning curve. These competencies included many simple tasks such as checking vital signs and turning patients. Working with their academic partners, Legacy developed a program focused on teaching students the basic fundamentals of nursing in targeted sites. This pilot program was a win-win situation that not only gave nursing students an opportunity to develop clinical skills but also used students’ work to help deliver safe care to patients.
KEY QUESTIONS FROM BREAKOUT GROUPS
Following the three presentations, participants joined one of six breakout groups. These small group conversations aimed to encourage dialogue across professions and sectors in working toward developing a question or comment posed to the speakers for their reflections. One group consisted of students and trainees, and the other five groups included health professionals and educators. Because of insufficient time, the panelists responded to specific questions presented by individuals from each of the breakout groups (see Appendix B for a list of the other questions asked).
Pam Jeffries, Vanderbilt School of Nursing, asked how health care organizations can better accommodate new workers who have gaps in their skills and competencies. Jeffries, who is a dean of nursing, suggested some ideas, such as longer orientations, skills assessments, and teaching skills on the job. Kelly responded saying, when the nurse residents at Legacy started in August, they were “literally terrified” to touch patients or even go into their rooms. To help them transition into the workforce, nurse trainees were divided into small cohorts. Each cohort received a coach who facilitated their learning and a preceptor who they shadowed. New nurses were intentionally placed with preceptors, who have been practicing for 1 to 3 years, she said, rather than a nurse with more experience, to avoid the potential
for intimidation. In addition, new nurses were provided with a mentor so they could “vent and unload and share their fears and concerns.” Nurses entering the workforce are “fragile,” Kelly said, and there is a risk of them leaving the profession altogether, so “we handle them with kid gloves” in the hopes of making their transition smoother and more successful.
Another question was asked by Mark Merrick, Commission on Accreditation of Athletic Training Education. He asked if this crisis created a case for competency-based education that gives more flexibility in determining learner competence, rather than the more structured and rigid current models? Kornfeld answered by raising the issue of a need to pivot to competency-based education for greater flexibility, particularly during a crisis. She noted that students enter health professions education with different backgrounds and different life experiences, and they have different experiences in school as well. Competency-based education allows us to better assess where learners are, to meet their needs, and to prepare them to enter the workforce. It gives schools the ability to be flexible in how competencies are developed, and it allows for innovation when circumstances require, such as during times of crisis.
Building upon the remarks of Kornfeld, Whelan provided the perspective of a practicing health professional who was redeployed during the pandemic and for whom competency-based education was critical to be able to work effectively in a new area. Whelan then addressed a question about technology. The quick answer is “We’ve learned a lot, and we need to just take those lessons forward and use technology when appropriate and in person as indicated.”
Regarding the student voice, Whelan commented on the numerous exchanges she had with students and leaders across professions and from different institutions, not only about their experiences during the pandemic but also with regards to the recent civil unrest related to racism. Schools that truly included students in decision making and included students at the table, said Whelan, “were most successful in meeting the students where they were.” Whelan closed by introducing a parallel concept to the social determinants of health, which is the social determinants of education (SDE). SDE reflects barriers to entry into, and progression through, the health professions, which the pandemic highlighted and which “we really need to pay attention to if we want to achieve truly equitable health professions education.”








