Infectious Diseases:
Characterizing Pathogens and Preventing Spread
Since 1970, the world has confronted a variety of new and re-emerging infectious diseases—with mixed success. Vaccines have proven to be the most powerful method of preventing such diseases, but accessibility and delivery are uneven, particularly in less wealthy countries, and vaccines for many diseases remain elusive.
1976
Identification of the Ebola Virus
Ebola virus, which causes one of the world’s deadliest viral diseases, was first discovered in 1976 when an outbreak of fatal hemorrhagic fever struck Zaire, now the Democratic Republic of the Congo. Soon afterwards a second outbreak of a different viral strain occurred 500 miles away. Scientists believe the virus made the jump to humans from animals, though they have yet to determine its precise origin. Since its discovery, the majority of Ebola outbreaks have occurred in Africa, though the Ebola epidemic in West Africa showed the potential for social and economic disruptions worldwide.
1980
World Declared Free from Smallpox
The eradication of smallpox is considered the greatest achievement of international public health. Smallpox had stalked the world for millennia, killing an average of 3 of every 10 people infected. An effective vaccine for preventing smallpox became available at the end of the 18th century, but not until 1980, after repeated efforts to eliminate the virus, did the World Health Organization officially declare the world free of the disease.

1989
Widespread Measles Vaccination
Widespread use of the measles vaccine, which first became available in the United States in 1963, drastically reduced the incidence of infection. However, after a 1989 measles outbreak among vaccinated school-aged children, a second dose of the vaccine was recommended for all children, which further reduced measles rates. Though measles was declared eliminated from the United States in 2000, it continues to cause about 100,000 deaths worldwide each year. Also, travelers continue to bring the disease into the United States, where it can spread and cause outbreaks among people who have not received the measles vaccine.


1993
The Largest Waterborne Outbreak in American History
Cryptosporidium, a parasitic disease that causes dehydration, fever, stomach cramps, and diarrhea, contaminated one of Milwaukee’s two water treatment plants in 1993. Roughly 403,000 people contracted the disease and 69 people died, making it the largest waterborne outbreak in American history. Cryptosporidiosis, which has no vaccine and few treatments, remains a concern in the United States, with a 13 percent increase in cases between 2009 and 2017, which amounted to a total of 7,465 cases across that time.
1995
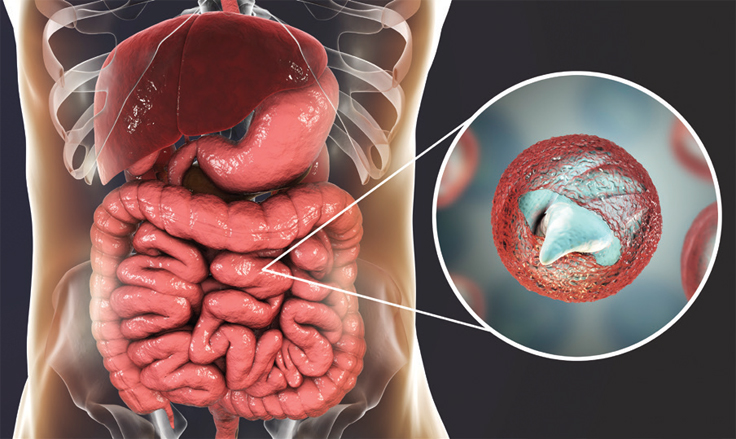
Progress Toward Eliminating River Blindness
Occurring mostly in Africa and spread through bites of an infectious blackfly, onchocerciasis, commonly known as river blindness, is a parasitic, tropical disease that can cause severe itching, bumps under the skin, and loss of sight. In 1995, the African Programme for Onchocerciasis Control (APOC) was launched. A combination of health education, mass drug administration, and blackfly vector control have been successful in the Americas, with Colombia becoming the first country to eliminate river blindness in 2013. Ecuador, Mexico, and Guatemala received official verification of elimination in 2014, 2015, and 2016, respectively.
2003
Spread of Severe Acute Respiratory Syndrome
Severe acute respiratory syndrome (SARS) is a viral respiratory disease discovered in the Guangdong province of China in early 2003. Within a matter of weeks, SARS spread to 37 countries, creating alarm that global travel could cause the disease to rival the 1918 influenza pandemic that killed at least 50 million people. These predictions were not realized, in part due to relatively swift containment, but it had severe economic impacts as countries braced for possible widespread transmission.
2004
Eliminating Rubella in the United States
Rubella is a contagious virus that in pregnant women poses particular risks to unborn babies. Before the initiation of the rubella vaccination program in 1969, rubella was common in the United States. The last major U.S. outbreak in 1964–1965 resulted in 11,000 miscarriages, 2,100 newborn deaths, and 20,000 babies born with congenital rubella syndrome. Through widespread administration of a triple vaccine against measles, mumps, and rubella, the United States eliminated rubella in 2004.
2008
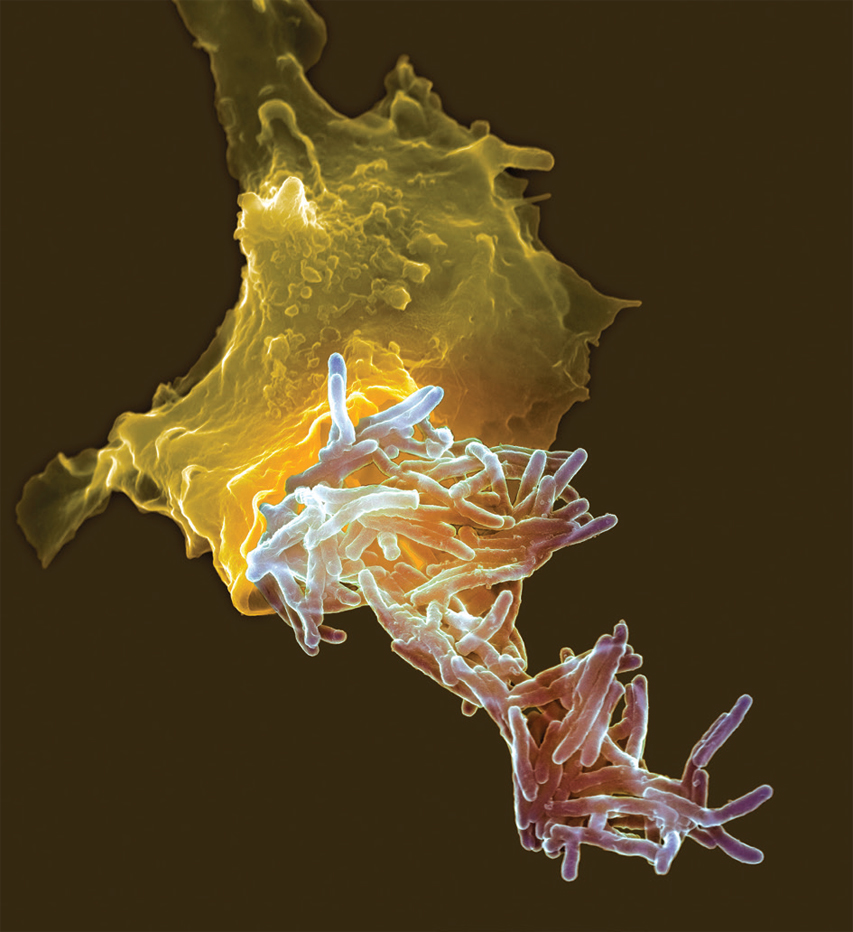
A Global Push to Eradicate Tuberculosis
Tuberculosis (TB) is a contagious, infectious disease caused by a bacterium that currently infects nearly one-quarter of the world’s population. The airborne disease can be particularly harmful among people with compromised immune systems and remains the leading cause of human death from a curable infection. Multidrug-resistant TB is a rising threat to existing treatments. In 2008, the World Health Organization established a goal of eradicating TB by 2050, but doing so will require combined improvements in drug treatment, diagnostic instruments, and prevention strategies.

2014
Whooping Cough Vaccination for Pregnant Women
Every few years, epidemics of pertussis recur in the United States. Also known as whooping cough, pertussis is highly contagious, with severe cases primarily occurring in infants. Following a spike of cases in 2014, the Advisory Committee on Immunization Practices recommended that pregnant women receive the whooping cough vaccine during their third trimester to optimize protection at birth.
2014
Stemming a Major Ebola Outbreak
On March 23, 2014, the World Health Organization reported cases of Ebola in the forested rural region of southeastern Guinea, marking the beginning of the largest outbreak of the disease in history. Poor public health infrastructure, from disease surveillance to response, enabled the virus to spread to other countries. The outbreak finally ended 2 years later, largely through engaging with trusted community leaders and careful implementation of health policies at the national and global levels. Then, in August 2018, the Democratic Republic of the Congo declared an Ebola virus outbreak that evolved into the second largest in history, and took nearly 2 years to eradicate, despite significant local and international support.
2019 Dealing with a Modern Pandemic
Coronavirus disease 2019 (COVID-19) is a respiratory, primarily airborne illness that originated in Wuhan, China, at the end of 2019 and then spread rapidly and widely around the world. By the end of 2021, the novel coronavirus had caused more than 5 million deaths worldwide. Uncertainty about the virus and a lack of global coordination resulted in regional responses to the pandemic, with rates of infection and death reflecting a range of approaches taken. In addition, scientific and medical personnel had to learn how to treat COVID-19 in real time, causing extreme stress to health care professionals and others on the front lines. COVID-19 impacted not only people’s health and well-being but also caused drastic societal and financial disruptions. It forced the shutdown of schools, businesses, and travel; demanded once-in-a-century public health measures; and changed expectations of what individuals do to protect fellow human beings, especially more vulnerable groups. The world will continue to have to reflect, adapt to, and prepare for a new normal after this pandemic and its ongoing, deep, and widespread consequences.


The COVID-19 pandemic highlighted the severe toll that infectious diseases continue to take on human health and welfare. Future outbreaks are inevitable as microbes evolve and new diseases emerge. The challenge will be for the scientific community to help the world better prepare for and respond to the next outbreak. Furthermore, outbreaks of these types and levels of severity—including H1N1, Middle Eastern respiratory syndrome, Ebola, and Zika—have become increasingly frequent over the last two decades. This concerning trend, especially in light of the COVID-19 crisis, demands urgent global attention to better support the health of all.




