2
Workshop 1 Keynote: Community Health Workers
INTRODUCTION TO WORKSHOP
Lauren Hughes, associate professor of family medicine and state policy director of the Farley Health Policy Center at the University of Colorado, explained that the first workshop will explore the Agency for Healthcare Research and Quality’s (AHRQ’s) proposed priorities and strategies to make them clearer and more likely to lead to high-impact funding and projects, while also being consistent with the congressional mandate to invest funds from the Patient-Centered Outcomes Research Trust Fund (PCORTF). The
day’s sessions began with a keynote address on the important role community health workers can play in equitable implementation of patient-centered outcomes research (PCOR). The sessions then discussed innovative models of care delivery, approaches to guiding decision-making regarding PCORTF investments, how to train PCOR investigators, and the use of digital tools to expand implementation of PCOR findings.
SPONSOR REMARKS FROM AHRQ
Following Hughes’s introductory remarks, Karin Rhodes, AHRQ’s chief implementation officer, provided additional background on PCORTF and AHRQ’s role. Rhodes provided some definitions before discussing PCORTF’s mandate. PCOR, she explained, provides decision makers with objective scientific evidence on comparative effectiveness of different treatments, services, and other interventions used in health care, while PCORTF, which receives most of its funds from a tax on private insurance plans, provides funding to support dissemination, training, and data infrastructure for PCOR. She explained that Congress mandated that 80 percent of trust fund spending would go to the Patient-Centered Outcomes Research Institute (PCORI) to conduct comparative effectiveness research. AHRQ receives 16 percent of trust fund spending to disseminate this evidence into practice as well as train health services researchers, and the Assistant Secretary for Planning and Evaluation (ASPE) at the U.S. Department of Health and Human Services receives the remaining 4 percent to develop the data infrastructure for PCOR.
She explained that Congress reauthorized PCORTF in 2020, and PCORI, AHRQ, and ASPE are all now engaged in strategic planning for the next 10 years. Rhodes noted that unlike most congressionally authorized funds, which have to be spent in the year Congress authorizes them, PCORTF can rollover unused funds, which provides a chance to conduct longer-range strategic planning. AHRQ began this process by pulling together an interdisciplinary group at the staff level from across AHRQ’s centers, offices, and divisions. The planning process will create the strategic framework with appropriate stakeholder engagement, invest in the necessary infrastructure to accomplish AHRQ’s goals for PCORTF, and then develop an evaluation of its efforts.
Rhodes explained that AHRQ’s mission is to “synthesize and support the dissemination of evidence into practice and train the next generation of patient-centered outcomes researchers,” with an overarching vision of delivering equitable, whole-person care across the life span (AHRQ, 2022). AHRQ developed a strategic framework with five high-level priorities and desired outcomes for trust fund investments through fiscal year 2029 to fulfill this mission (see Appendix D). The five priority areas of the framework are
- health equity;
- prevention and improved care of people with chronic conditions;
- patient, family, and provider experience of care that enhances trust in the health care system;
- high-quality, safe care that is aligned with national health priorities; and
- primary care transformation.
AHRQ published a notice in the Federal Register seeking public input that closed a week before this workshop, said Rhodes. AHRQ has also established a subcommittee of the AHRQ National Advisory Committee to address issues pertaining to the strategic framework. In addition, AHRQ is coordinating closely with PCORI and ASPE to tell one narrative of how the three entities spend PCORTF dollars to enhance health care and health care quality. This framework, she noted, will evolve, as will the projects it funds and the national priorities driving those projects.
COMMUNITY HEALTH WORKERS: A LINK BETWEEN PROVIDER AND PATIENT
Shreya Kangovi, founding executive director of the Penn Center for Community Health Workers and associate professor at the University of Pennsylvania Perelman School of Medicine, began by explaining that community health workers1 (CHWs) embody the concepts of person-centered, equitable, whole-person care across the life span. The nation’s 86,000 community-based organizations employ the majority of the nation’s CHWs though public health departments and, more recently, value-based health care organizations.2 Kangovi noted CHWs are not siloed in one part of the care continuum or one specific patient population. They are frontline public health workers with a uniquely broad and deep understanding of the community they serve. This understanding allows them to fulfill roles across and beyond the care continuum, such as:
- providing social and emotional support,
- care navigation and care coordination,
___________________
1 A community health worker is a frontline public health worker who uses their trust and/or membership in a community to link community members to social and health-related services. They may also engage in advocacy, health education, or health communication (APHA, 2022).
2 Value-based health care is a health care delivery model in which providers, including hospitals and physicians, are paid based on patient health outcomes (NEJM Catalyst, 2017).
- cultural mediation,
- life coaching,
- advocacy, and
- outreach.
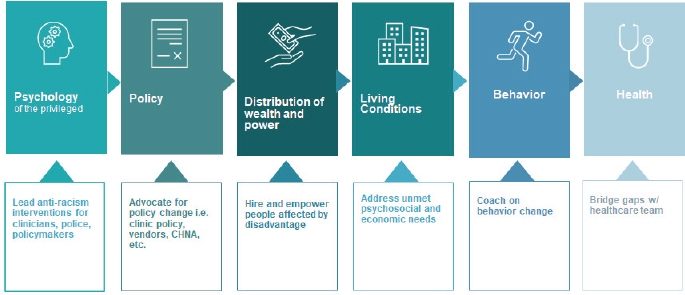
Kangovi noted that CHWs can address all levels of health inequity. Many people consider health inequity an imbalance of diseases that affect “vulnerable populations,” but she pushes back on that notion. She defines health inequity as a psychological condition that starts with people who have privilege, which creates psychological distortions such as savior complex, group narcissism, and implicit bias that influence policy decisions. These decisions often shape the distribution of wealth and power within institutions and across society, she continued. In turn, these societal factors affect living conditions and health-affecting behaviors, such as smoking or a lack of physical activity, and produce disparities across a range of different health conditions and outcomes (Figure 2-1). She noted that adopting this framework for the root causes of health inequities changes the dynamics of who health inequity affects. Health inequity is “a condition that starts in one group of people but whose symptoms are manifest in a different group of people,” said Kangovi.
Kangovi explained that CHWs can bridge the gap between individuals and their health care team, and they can also coach individuals on behavior change, such as quitting smoking or getting more exercise. Additionally, beyond directly addressing health concerns, CHWs have lived experience regarding health inequity. This allows them to change the distribution of wealth and power in institutions because they have the power and autonomy to help shape health care interventions and decisions. Kangovi suggested that
SOURCE: Presented by Shreya Kangovi on June 9, 2022, at Accelerating the Use of Findings from Patient-Centered Outcomes Research in Clinical Practice to Improve Health and Health Care: A Workshop Series.
CHWs are also some of the best policy advocates she has met, in large part because of their lived experience. She offered an example of her own institution, where executives now have CHWs mentoring them to help foster awareness of their own privilege and to make equitable decisions.
Brea Burke, a Virginia certified CHW with Healing Hands Health Center and founder of CHWUnited, explained that serving the community is something that has been part of her life since she was a young girl. She would often join her father, a pastor, when he visited people in the hospital or at their home. Burke noted that CHWs take on many different roles depending on the needs of their patients: “We become what the patient needs most: a friend, a confidant, a gym partner, a walking buddy, an advocate at appointments, a shoulder to cry on,” she said. She described CHWs as the link that helps health care providers see and understand the whole picture of their patients’ lives, not just the part they see in their offices.
Burke told the story of one of her clients, a woman whose clinical providers thought might need some extra support, for which they referred her to Burke. When she first met her new client at the client’s home, she discovered that the only furniture the woman had was two wooden kitchen chairs and a small wooden table. The woman had disposed of the rest of her furniture due to a previous bed bug infestation in her apartment building and could not afford new furniture. Burke learned during that first conversation that the woman had experienced a cocaine addiction following the loss of her husband, in addition to experiencing an ongoing alcohol use disorder and mental health disorders. Burke helped the woman identify priorities and set goals that would improve her health and happiness. Burke then provided support for the woman to attain those goals, such as connecting her with a community organization to acquire furniture, walking with her to the nearest grocery store, and connecting her to mental health services.
IMPaCT: A Case Study of Translating PCOR to Improve Health
Kangovi explained that she and her colleagues began developing the Individualized Management for Patient-Centered Targets (IMPaCT) program 12 years ago, when she partnered with a CHW from southwest Philadelphia to learn about the health-related concerns of the residents of south and southwest Philadelphia. Specifically, they asked what community members identified as barriers to maintaining good health and what the health care system could be doing differently to address those barriers. They interviewed 1,500 people in a variety of locations, including on their front porches, at their bedsides, and in shelters for people experiencing homelessness. Kangovi noted that the people interviewed lived in chronically under-resourced neighborhoods.
She described three common themes that were observed in the interviews. The first theme was the importance of the social determinants of health, as those real life issues drove their lives. The second theme was that the people interviewed wanted help managing those real life issues from someone to whom they could relate, particularly someone who had similar lived experiences. The third theme was that they wanted to retain power. The people that were interviewed wanted support and resources so they could manage their health. She noted that these themes connected with the work typically done by community health workers.
Kangovi noted that when she began researching the barriers to successful CHW programs, she expected the primary barriers would be lack of funding and political will. However, she learned that the main impediments were implementation factors, staff turnover, lack of infrastructure, not truly understanding what CHWs should be doing, and a lack of understanding of how to incorporate this unique workforce into the health care system without destroying or over medicalizing3 them.
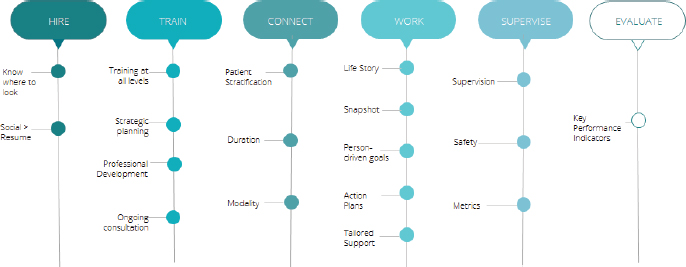
Kangovi and colleagues developed the IMPaCT program, which was informed by their interviews and her research of the community health worker field. The program includes a stepwise process to recruit, train, and deploy CHWs (Figure 2-2). The program recruits CHWs through community health organizations and emphasizes finding people that have the needed interpersonal skills more than those with formal training. The IMPaCT model includes providing CHWs with a formalized framework to consider who they should be supporting, as well as when to make the connection at a time and place that is useful and comfortable for the patient. The IMPaCT team developed “playbooks” that teach the CHWs how to get to know their clients’ life stories and turn that information into person-driven goals that translate into meaningful action. Kangovi and her collaborators also developed best practices for supervisors and developed key performance indicators for program evaluation.
Kangovi said that she and her IMPaCT colleagues have evaluated their CHW program through multiple disease-agnostic, person-centered clinical trials. Inclusion criteria for these studies required the client to
- be a Medicaid or dually eligible beneficiary;
- live in an under-resourced zip code; and
- have had either one hospitalization or two or more chronic conditions, including smoking or obesity.
___________________
3 Medicalization refers to the degree to which society considers something to be “medical” in nature, such as by considering a profession to be part of the broader health care system, or a certain condition being considered a disease (Maturo, 2012).
SOURCE: Presented by Shreya Kangovi on June 9, 2022, at Accelerating the Use of Findings from Patient-Centered Outcomes Research in Clinical Practice to Improve Health and Health Care: A Workshop Series.
These studies found that the IMPaCT program approach to CHWs produced net savings on health care spending of $2,500 per person per year (Kangovi et al., 2020; Morgan et al., 2016). They also found that patients supported by CHWs had fewer days of hospitalization when compared to matched control patients who did not have support from a CHW (Vasan et al., 2020). Those clients also had higher scores on health care services surveys regarding primary care access and quality, and also had improved chronic disease management and mental health (Kangovi, 2018).
Kangovi noted that the IMPaCT team has also translated and disseminated some of its work to inform public policy. For example, President Biden included Medicare coverage for CHWs in the fiscal year (FY) 2023 budget proposal. In January 2022, a bipartisan group of senators introduced the Building a Sustainable Workforce for Healthy Communities Act.4 This bill would reauthorize and revise a Centers for Disease Control and Prevention (CDC) program that supports the use of CHWs to improve health outcomes in medically underserved communities. In April 2022, the Health Resources and Services Administration (HRSA) announced it would provide $226.5 million to launch a multiyear CHW training program.5
___________________
4Building a Sustainable Workforce for Healthy Communities Act, S.3479, 117th Cong, 2nd sess. (January 11, 2022).
5 Additional information is available at https://www.hhs.gov/about/news/2022/04/15/hhs-announces-226-million-launch-community-health-worker-training-program.html (accessed September 15, 2022).
DISCUSSION
Hughes opened the discussion by asking Kangovi to list what she considers the top barriers to implementing CHWs more broadly in U.S. health care systems. Kangovi replied that the barriers have changed over the years. When she first started IMPaCT, the primary barrier was a lack of evidence to inform how to best disseminate and implement these programs. However, there have now been dozens of randomized, controlled trials conducted across the country and internationally that consistently point to a set of best practices for implementation. These best practices have been outlined in reports from the National Committee for Quality Assurance and the World Health Organization, among others (Lau et al, 2021; WHO, 2018b). She emphasized that it is important to understand that training is not the only necessity to produce good outcomes.
Kangovi highlighted two funding related challenges for CHW programs that should be addressed at the policy level. First, she said, there is a need for sustainable and adequate funding for CHW programs, as opposed to the current patchwork of grants and demonstration projects. She called for Medicaid and Medicare to cover the full range of evidence-based support provided by CHWs. Second, she said, funding for CHW programs should be tied to implementing best practices, and regulation is needed to protect the professional identity of this workforce and ensure the quality of the services they provide. Burke echoed these concerns, noting that her position is currently funded by a grant.








