2
Defining Whole Health
In 1948 the World Health Organization (WHO) defined health as “a state of complete physical, mental and social well-being and not merely the absence of disease and infirmity” (WHO, 2020, p. 1). Some criticized this definition as being excessively broad, vague, and unmeasurable, and in subsequent years health care focused more on a biomedical reductionist model than on achieving that more holistic vision of health. In 1984 the WHO revisited and updated the definition of health, shifting it from a desirable state of being to a dynamic set of resources for living well—“the extent to which an individual or group is able to realize aspirations and satisfy needs to change or cope with the environment . . . health is a resource for everyday life, not the objective”—that emphasized the social and personal resources as well as physical capabilities that are a part of health (WHO, 1984, p. 34).
More recently, the term whole health has emerged. The concept of whole health is not novel, and it has been evolving for decades under a range of different names such as salutogenesis, patient-centered care, people-centered care, integrated care, and population health (Anastas et al., 2018; Bhattacharya et al., 2020; Nash et al., 2016; National Committee for Quality Assurance, 2018; Stewart, 2014; Thomas et al., 2018). Two recent reviews considered the history and evolution of the term whole health and identified several common themes (Jonas and Rosenbaum, 2021; Thomas et al., 2018). These common themes suggest that whole health systems require a multidimensional, integrated approach that recognizes the importance of the therapeutic relationship, acknowledges the clinician’s humanity, recognizes the patient’s individual personhood, and employs a range of treatment modalities using a holistic biopsychosocial approach
that involves additional health care practitioners. Frameworks such as the Chronic Care Model, Patient-Centered Medical Home, accountable care organizations, Accountable Health Community, and Optimal Healing Environment Health have also described community systems that deliver and support whole health components (Alley et al., 2016; Jonas and Chez, 2004; Kuzel, 2009; Martin et al., 2004; McClellan et al., 2010; Primary Care Collaborative, 2022; Tipirneni et al., 2015; Wagner et al., 1996, 2001; Wiley and Matthews, 2017).
Driven by the unique needs of veterans returning from combat and suffering from long-term symptomatic mind–body consequences and functional injuries, the Department of Veterans Affairs (VA) and Samueli Institute have been leaders in advancing the whole health concept. In 2003 the Samueli Institute developed the Optimal Healing Environment framework to include the psychological, spiritual, physical, and behavioral components of health care (Jonas and Chez, 2004). It addressed people in relationships, their health-creating behaviors, and the surrounding physical environment as a pathway to well-being (Sakallaris et al., 2015). Several health care systems that adopted this approach realized improved patient experiences and demonstrated business case benefits. From this emerged the Total Force Fitness model that went beyond a medical environment to include physical, psychological, spiritual, social, and even economic aspects of human flourishing, integrated into a single framework for active-duty service members (Jonas and Rosenbaum, 2021). The VA implemented multiple offshoots of the program, including the Performance Triad, Operation LiveWell, and Holistic Health and Fitness Program (Jonas and Rosenbaum, 2021).
Today, the VA presents patients with the following definition to describe its Whole Health System (WHS):
Whole Health is VA’s cutting-edge approach to care that supports your health and well-being. Whole Health centers around what matters to you, not what is the matter with you. This means your health team will get to know you as a person, before working with you to develop a personalized health plan based on your values, needs, and goals. (VA, 2022a)
Another definition the VA has used that is geared more toward clinicians describes whole health as “an approach to care that empowers and equips a person to take charge of their health and well-being and live their life to the fullest” (Kligler, 2022, p. 1).
The VA’s definition of whole health purposefully shifts the focus from a “disease” care system to a “health” care system by emphasizing the idea that people need to be enabled, empowered, and equipped to take charge of their health and well-being and to live life to the fullest (VA, 2021). As Figure 2-1 shows, the VA’s WHS model is supported by three pillars:

SOURCE: VA, 2022b.
- The pathway—engaging veterans with fellow veterans (who are themselves trained peer facilitators) to discover their mission, aspiration, and purpose through personal health plans.
- Well-being programs—encouraging self-empowerment, self-healing, self-care, and improvements in the social and structural determinants of health.
- Whole health clinical care—a cultural transformation in care delivery to include prevention and treatment and conventional and complementary approaches. Together these elements aim to create a “circle of health.” (See Figure 4-1 in Chapter 4 for a more detailed discussion of the circle of health.)
The circle includes four elements: the person, self-care, professional care, and the community. The person is at the center and where whole health starts. As each person is unique, what matters to the individual
person is what ultimately determines what whole health means. Each person has the power to affect their well-being through self-care, and whole health offers the skills and support needed to make the changes a person wants. A health team delivers professional care, including prevention and treatment of disease and illness. The community encircles the person virtually and in the real world as these are the people and groups that a person connects with, including the professional and personal elements of health and self-care.
To operationalize its approach to whole health, the VA made systemic and cultural shifts in its approach to care. Chapters 4 and 5 of this report detail how the VA operationalized these changes and the evidence on the impact it had on health outcomes and the care delivery experience for veterans and clinicians.
A UNIVERSAL DEFINITION OF WHOLE HEALTH
The statement of task for this study directed the committee to consider the following (see Chapter 1 for the complete statement of task): (1) Where is whole health currently being implemented, (2) what does whole health accomplish, (3) how can effective whole health strategies spread, and (4) what other factors affect the performance of whole health? To address this statement of task, the committee created a universal definition of whole health and the whole health approach. The committee needed this definition to identify and examine whole health implementations outside of the VA. To create the definition, the committee reviewed the existing definitions, foundational elements, best practices, and lessons learned from identified whole health and whole health–like approaches operating by different names. This included ideas about what it means for a person or community to achieve or have whole health as well as what is needed from health care systems to bring out, deliver, and support whole health.
From these fact-finding activities, the committee developed the following definition for whole health:
Whole health is physical, behavioral, spiritual, and socioeconomic wellbeing as defined by individuals, families, and communities. To achieve this, whole health care is an interprofessional, team-based approach anchored in trusted longitudinal relationships to promote resilience, prevent disease, and restore health. It aligns with a person’s life mission, aspiration, and purpose.
While the committee’s definition is different from the VA’s definition—it is more inclusive of other systems’ approaches to whole health—it is highly aligned with and derived from the VA’s work. It is an aspirational definition,
as the committee found no systems that have fully implemented this definition of a whole health approach for the entire community to whom they are accountable (see Chapters 4 and 5). Nevertheless, this aspirational definition is essential to set goals for what the VA and other health systems need to do to help people, families, and communities achieve whole health.
The state of whole health envisioned by the committee is fundamentally different from how health care currently views health and well-being in three ways. First, whole health is not just about the conventional “medical” well-being that health care currently addresses, nor is it merely the absence, prevention, or control of disease. Instead, it is about a whole state of well-being that spans physical, behavioral, spiritual, and socioeconomic well-being. Whole health is the extent to which an individual or group can realize goals and satisfy needs to change or cope with the environment (IOM, 2009).
Second, the philosophy of person-, family-, and community-centered-ness is essential to define what the “whole state of well-being” means. Individual people, families, and communities get to say what physical, behavioral, spiritual, and socioeconomic well-being means to them. To understand the needs and desires of those they serve, whole health providers and systems need to build trustworthy relationships. Third, an ideal state of whole health is not just about being healthy, but is about being supported to enable a person, family, and community to achieve what they want from life. It is a resource for everyday life and not an objective.
The systems that deliver whole health are also fundamentally different from the current systems that deliver health care. Whole health systems are cross-sectoral, spanning health care, mental health, health behavior promotion, public health, community care, social services, the built environment, education, religion, and the financial and economic sectors. This means whole health systems cannot just be located in hospitals and clinician offices but need to span community settings that include where people live, work, and play.
In addition, whole health systems are not merely the sum of their parts. There is seamless coordination and provision of services across sectors and interprofessional1 care teams with a shared goal of helping people and communities achieve whole health. Moreover, whole health systems start by identifying how people, families, and communities define what health and well-being means for them and what they need to achieve it. This can be done through a range of approaches such as creating care plans or doing
___________________
1 An interprofessional care team includes a variety of clinical and nonclinical team members that collectively meet the whole health needs of a population or community. An interprofessional team will look different depending on available resources and local needs and should ideally reflect the diversity of its community.
needs assessments, but at its core, the delivery of whole health starts by listening to what people say they want and need.
FOUNDATIONAL ELEMENTS OF WHOLE HEALTH
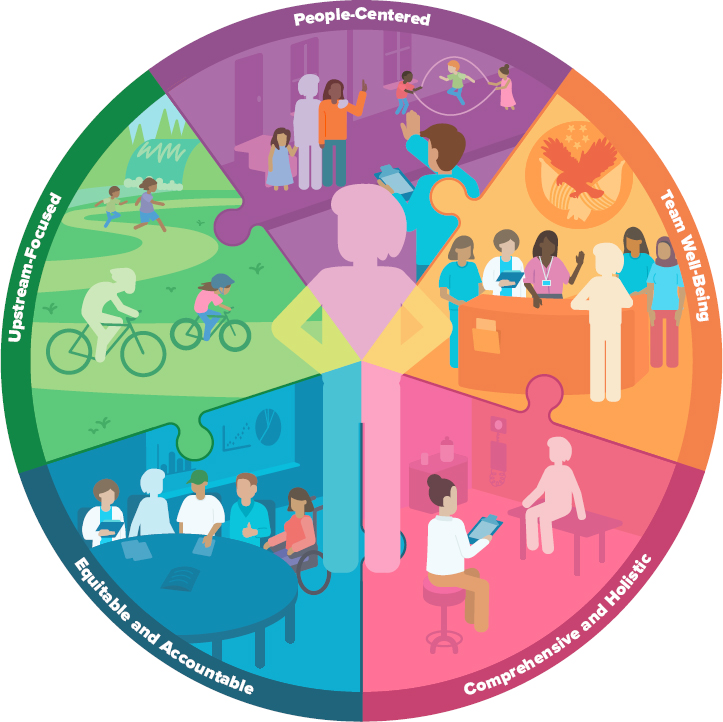
From the review of whole health definitions and various program descriptions, the committee identified five interdependent and foundational elements of whole health systems: (1) people-centered, (2) comprehensive and holistic, (3) upstream-focused, (4) accountable and equitable, and grounded in (5) team well-being (Table 2-1 and Figure 2-2).
People-Centered
Whole health requires a partnership with people to ensure that the health system respects, informs, engages, supports, and treats people, their families, and their communities with dignity and compassion (Epperly et al., 2015; Stewart, 2014). Whole health delivery occurs within the context of social and cultural environments and starts by understanding peoples’ needs and goals and then directing tailored, effective care around those needs and goals (Cloninger et al., 2014). Thus, whole health is more than the absence
TABLE 2-1 Foundational Elements of Whole Health
| People-centered | Achieving a sense of purpose through longitudinal, relationship-based care People/families/communities direct goals of care Care delivered in social and cultural context of people/family/community |
| Comprehensive and holistic | Address all domains that affect health—acute care, chronic care, prevention, dental, vision, hearing, promoting healthy behaviors, addressing mental health, integrative medicine, social care, and spiritual care Attend to the entirety of a person/family/community’s state of being Components and team members are integrated and coordinated |
| Upstream-focused | Multisectoral, integrated, and coordinated approach to identifying and addressing root causes of poor health Address the structures and conditions of daily life to make them more conducive to whole health |
| Equitable and accountable | Whole health systems need to be accountable for the health and wellbeing of the people, families, and communities they serve Care needs to be accessible to and high quality for all |
| Team well-being | The health of the care delivery team is supported |
of disease, and it is also more than a state of wellness. Achieving person-centered whole health is a process grounded in longitudinal relationships with team members and organizations that build shared understanding and trust over time. This includes relationships among individual clinicians, care teams, and health systems and the people, families, and communities for whom they are accountable. It is in the context of these relationships that the whole health system supports people to articulate and achieve their missions, aspirations, and purposes and to continually learn from their work, such that aspirations and goals are redefined over time. Examples of processes to achieve purpose can include tasks such as goal setting, care planning, and group-level assessments (Bolton et al., 2019; Fix et al., 2017; Kilbourne et al., 2014; Seidel et al., 2021; Vaughn and Lohmueller, 2014).
Comprehensive and Holistic
Critical to whole health is attention to the entirety of the person’s state of being, and the design of whole health systems needs to address this entirety. It recognizes that “the whole” is more than the sum of its parts for the people, communities, and the health systems that care for them. This diverges from how medicine often uses the term “holistic care” today as a code for therapeutics outside of conventional medicine. Therapeutics outside of conventional medicine is a component of whole health care, but merely adding it to conventional care does not make whole health care. Fundamentally, designing and developing whole health delivery systems cannot be done simply by creating and adding in each individual component of whole health to current systems. It requires the components and the care team members delivering the components to be collaboratively interwoven, coordinated, and comprehensive in their approach to addressing the goals and needs of the people, families, and communities they serve. This includes conventional medical care—acute, chronic, preventive, reproductive, and mental health care, dental, hearing, and vision care—plus the components of complementary and integrative health, spiritual care, and upstream factors such as health behaviors, education, and social needs.
Upstream-Focused
It is well known that socioecological factors and life-course events are the key drivers of health (McGinnis and Foege, 1993; Mokdad, 2004; IOM/NRC, 2013). Four unhealthy behaviors—tobacco use, unhealthy diet, physical inactivity, and risky alcohol use—account for nearly 40 percent of preventable deaths in the United States (Mokdad, 2004). The growing pandemic of unhealthy drug use, including opioids, further undermines health and well-being. Empowering people with the tools, resources, and the environment to more easily adopt healthy behaviors is an essential component of whole health care. Whole health systems also need to address the social and structural determinants of health—poverty, housing, food, finances, education, environment, equity, and racism—which represent both the cause of poor health (social determinants) and the cause of the causes of poor health (structural determinants) (Braveman and Gottlieb, 2014). Because factors and events vary from person to person and community to community, whole health systems need to seek to understand and address the specific root causes affecting the people, families, and communities they serve. A major challenge is that these socioecological and life-course events and structural determinants of health are often the most difficult things to change. They are engrained in our lives through our daily activities, the communities we live in, the places that we work, and family events reaching
back generations. Root causes of poor health cannot be dealt with solely by health care but need to be addressed everywhere. In addition, a range of expertise is needed that extends beyond health care. Whole health systems require multisector collaborations, and whole health care teams should include interprofessional members.
Equitable and Accountable
Whole health systems should focus on providing high-quality, safe, and evidence-based care. This means providing the right care at the right time to the right people (Campbell, 2016). Because health inequities are such a key driver of poor health (AHRQ, 2019; Nelson et al., 2020), ensuring whole health means ensuring health equity. While whole health systems cannot solve all of society’s ills, they need to address the root causes of inequity, including intrapersonal, interpersonal, institutional, and systemic mechanisms as well as the unequal distribution of power and resources (Weinstein et al., 2017). A key step in this process is accepting accountability for people, families, and communities. This allows whole health systems to be proactive in their care, using population health approaches that reach out to people and communities and do not wait for people to access care when they think they need it. It also means that some systems should be accountable for every person, family, and community—everyone needs a home and a system that will make sure that they do not fall through the cracks. Empanelment, the process of individuals within a given population declaring a source of primary care (or being assigned to one) is one method of helping ensure accountability within a system or geographic area (see Chapter 3 for more detail).
Whole health care should also create accessibility. People, families, and communities who need care should be able to access care through many avenues with a “no wrong door” type approach. Because achieving whole health needs to occur where people live, work, learn, and play—and not just in health care settings—the supports, resources, and surrounding environment should all provide access to and support for achieving whole health.
Team Well-Being
Interprofessional teams deliver whole health. The team is organized around the person, family, or community and includes, based on needs, conventional health care clinicians, integrative medicine providers, and professionals from non–health care sectors, such as social services and education, spiritual, and financial areas. Team members also include community and peer providers. Clinician stress and burnout are common in health care and can hamper the ability to provide high-quality care (Schwenk,
2018). In addition to assembling the right team for the right care, members of the care team and the team itself need to be healthy. Clinician stress and burnout hurt not only clinicians but also patients, communities, health care organizations, and learners. Ensuring and enhancing the health of those who care for and support communities creates an engaged and effective workforce, high-functioning care teams, and healing person–clinician relationships. While many health systems have implemented employee well-being programs, they tend to focus on individual-level interventions, such as providing benefits to employees to improve health and well-being (e.g., complementary integrative health such as yoga, acupuncture, and meditation). While some of these efforts are valuable, these approaches are less effective at preventing burnout and improving well-being than more systemic approaches that improve workflow efficiency, reduce administrative burden, improve technology usability, and reduce unreasonable work demands (NASEM, 2019b) (see Chapter 3 for more detail). Whole health care team members need to have the necessary systems to effectively and efficiently deliver whole health care, a supportive and positive work environment, and to experience whole health themselves.
Overlap of Whole Health with Other Care Delivery Models
The whole health approach overlaps with other concepts and care delivery models. To accomplish its statement of task, the committee reviewed and included major reports summarizing critical thinking about these concepts and models. In this section the committee identifies and describes these concepts and models, highlights how they are related to the concept and delivery of whole health, and discusses how they informed the committee’s work.
Primary Care
The committee’s definition of whole health aligns well with high-quality primary care. In 2021 the National Academies of Sciences, Engineering, and Medicine (National Academies) published the report Implementing High-Quality Primary Care: Rebuilding the Foundation of Health Care (NASEM, 2021). The report defined high-quality primary care as
the provision of whole-person, integrated, accessible and equitable health care by interprofessional teams who are accountable for addressing the majority of an individual’s health and wellness needs across settings and through sustained relationships with patients, families, and communities. (p. 4)
Primary health care is a similar but broader concept than primary care. Primary health care includes primary care but also focuses on population health and health system strengthening and public health approaches (WHO, 2022). Whole health is built upon both concepts.
High-quality primary care is the foundation of health care in any high-functioning health system and is rooted in a generalist approach. Primary care clinicians start with a focus on the whole person, which considers a person’s family and community context. Primary care clinicians build relationships with a person, understanding their preferences and priorities and working with the person to address concerns while keeping the whole in view (NASEM, 2021). In addition to the relationship between a person and his or her primary care clinician, there are a growing number of primary care practices in which clinicians work as part of an interprofessional team that may include behavioral health specialists, community health workers, health coaches, pharmacists, and others. These professionals work together to care for people in a manner that integrates physical, behavioral, and social and economic well-being. When a person requires specialist care, primary care clinicians and teams coordinate and connect the person to care. Primary care is a force for bringing the more fragmented parts of a person’s health care together, which is also an essential element of whole health care.
Primary care in its ideal form—which is not what primary care is for most people in the United States today—is the foundation of effective whole health systems. Primary care clinicians are core members of the whole health interprofessional team, and primary care clinicians often have a trusted longitudinal relationship with patients. It is in the context of this relationship that primary care clinicians personalize and align a person’s care with life mission, aspiration, and purpose. Primary care clinicians are also a conduit between the person and other professionals who help promote wellness in the fullest sense, and the primary care clinician and team add value by ensuring the parts of a person’s health care are connected, not fragmented, and continue to align well with the view of the person as a whole. Whole health is an outcome of a high-quality comprehensive primary care system.
Given that a wide variety of environments and experiences influence an individual’s well-being, the journey to achieving and maintaining whole health needs to involve professionals outside of primary care. The comprehensive and coordinated approach to the individual’s well-being should be embedded in care provided by all medical and behavioral specialists as well as every professional on the health care team and the community.
The National Academies’ recommendations for implementing high-quality primary care are also applicable to implementing whole health (NASEM, 2021). The five overarching objectives of the Implementing High-Quality Primary Care implementation plan include
- Paying for primary care teams to care for people, not doctors to deliver services.
- Ensuring that high-quality primary care is available to every individual and family in every community.
- Training primary care teams where people live and work.
- Designing information technology that serves the patient, family, and interprofessional care team.
- Ensuring that high-quality primary care is implemented in the United States.
For each of these recommendations, the words “whole health” could replace “primary care,” and this list would then identify the requirements for implementing whole health in the United States. While this committee’s statement of task differed from that of the committee that authored Implementing High-Quality Primary Care, this committee recognizes that widespread implementation of those recommendations would align with and help facilitate the systematic scaling and spreading of a whole health system of care. However, the subsequent chapters and recommendations of this report will focus on the issues unique to whole health.
Health Centers
Health centers (also commonly known as community health centers) include federally qualified health centers (FQHCs), tribal health centers, urban Indian health centers, health care for people who are homeless, health centers for residents of public housing, school-based health clinics, and migrant health centers (NASEM, 2021). A defining feature of health centers is that they provide locally tailored, comprehensive primary care and preventive health (including dental, cancer screening, family planning, and immunizations) to underserved populations, regardless of insurance status (HRSA, 2021). Many health centers are certified patient-centered medical homes and also offer more holistic and comprehensive services, such as gynecologic, behavioral health, vision and eye care, and diagnostic and radiologic services. They may also provide various services that focus on upstream factors including case management, referrals to specialty care and social services (many of which address root causes of poor health), and transportation and translation services (National Association of Community Health Centers, 2022).
Health centers have several features that align closely with the equitable and accountable foundational element of whole health. They are financially accessible. They will provide services to individuals regardless of their insurance status or ability to pay (Schwartz, 2014). Overall, health centers are widely accessible geographically and are a regular source of care for
people in underserved communities. As of 2021, they served 1 in 11 people in the United States (29 million people total), including 1 in 8 children and 1 in 7 racial and ethnic minorities. They served 376,000 veterans, 1.3 million people experiencing homelessness, over 5 million people living in public housing, 658,000 in school-based health centers, nearly 1 million agricultural workers, and almost 7 million best served in a language other than English (National Association of Community Health Centers, 2022).
Over 90 percent of people who use health centers are near or in poverty. The proportion of people they serve who are on Medicaid is much higher than in the general population (48 percent compared to 15 percent), as is the proportion of people they serve who are uninsured (23 percent compared to 9 percent). Nationally, 63 percent of people who seek care at health centers are members of a racial or ethnic minority, compared with 42 percent of the general population. Health centers are 35 percent more likely to have patients with chronic conditions than private practices (National Association of Community Health Centers, 2022).
FQHCs receive Health Resources and Services Administration Health Center Program federal grant funding to improve the health of underserved populations in the United States. (HRSA, 2022). Nearly 1,400 FQHCs operate in the United States today, a number that has held steady since 2015, at about 14,000 delivery sites. Despite the lack of growth, FQHCs have expanded the number of services they offer and outperform the national averages for many health outcomes despite serving a higher-risk population. For example, 58 percent of people whom health centers serve have their hypertension under control versus only 26 percent in the nation overall, while 64 percent of people whom health centers serve have their diabetes under control versus 19 percent in the nation overall. People who go to health centers are also less likely to have delays in medical care or dental care than those who seek care elsewhere (National Association of Community Health Centers, 2022). People who receive care at health centers also had 24 percent lower spending than those who received care from other medical facilities across all services provided (HRSA, 2022).
A key feature of health centers is that they are accountable to the communities they serve. They must have at least 51 percent of their governing boards of directors composed of people in the community who seek care at the health center (NASEM, 2021). Governing boards must also reflect the demographic characteristics of the overall populations that the health centers serve, although there is some evidence that this is not always the case (Wright, 2013, 2015). The purpose of this requirement is to ensure that the people served, who are often from underserved communities that are rarely included in organizational decision making, can have a voice in health center decisions regarding daily operations and how the health center delivers services.
Health centers are also required to annually assess the geographic catchment area of the people whom they serve (HRSA, 2018). They also need to complete a community needs assessment every 3 years, including a review of barriers to care, unmet health needs, health indexes for the population served, poverty level, and other demographic factors that affect the demand for services (such as percentage of population over the age of 65) and then adjust their services to better address the assessed needs. They are also required to make and maintain a reasonable effort to build partnerships with clinicians and services, including other hospitals and specialists, within their catchment areas to help facilitate coordination of services that the health center does not offer. Health centers often complete their needs assessments in coordination with nonprofit hospitals (which also should complete their own needs assessments to maintain their nonprofit status) and public health departments with the goal of coordinating their collective response to identified needs (NASEM, 2021).
Overall, the health center model shares many features of whole health and could be a logical platform to expand whole health throughout the U.S. health system. Some health centers, including Southcentral Foundation’s Nuka System of Care and Mary’s Center in Washington, D.C. (both of which are described in detail in Chapter 4), already align closely with the whole health approach.
Social and Structural Determinants of Health
Social and structural determinants of health (commonly referred to as “social determinants” or “social needs”) are the true reasons for health inequities and a whole health approach is key to addressing them at the population and community levels. They include things like poverty and economic systems in communities, structural racism and oppression, gender bias, and other social and economic factors—physical, social, cultural, community, economic, legal, and structural factors—that affect health, such as access to healthy food and having a place to live (Benjamin, 2011; Lushniak et al., 2015). Everyone has social and economic factors that shape their health. Social determinants of health are “social risks” when they negatively affect a person’s health. For example, not having access to reliable transportation might limit a person’s ability to attend a medical visit (Grembowski et al., 2014; Loeb et al., 2015; Safford et al., 2007). The structural determinants of health are the structures and systems that cause social and health needs; they span a wide range of socioeconomic systems, physical environment, education, social support networks, employment, and even health care equity (Braveman and Gottlieb, 2014).
Public health leaders, including the National Academies, have recognized the potential negative effects of social risk on health and have
recommended that health care organizations, including clinicians and teams in these organizations, systematically collect and document information about patients’ social risks (NASEM, 2019a; Wyatt et al., 2016). The 2019 National Academies report Integrating Social Care into the Delivery of Health Care: Moving Upstream to Improve the Nation’s Health provides a comprehensive list of the social and structural determinants that affect peoples’ health and summarizes the compelling and growing body of evidence that shows that these factors affect health directly (NASEM, 2019a). That report also recommended screening for these factors and identified five health system activities that strengthen social care integration:
- Awareness activities focus on individuals and identify the social risks and assets of individuals and communities.
- Adjustment activities focus on individuals and alter clinical care to accommodate identified social barriers.
- Assistance activities focus on the community and reduce social risk by providing assistance in connecting people with relevant social services.
- Alignment activities focus on community health systems, which undertake them to understand existing social care assets in the community, use them efficiently, and invest in and deploy them to improve health outcomes.
- Advocacy activities focus on both individuals and the community to promote policies that facilitate or strengthen efforts to improve social needs.
Achieving whole health depends in part on engaging in these five activities. In some cases, social risks will shape the extent to which patients are able to engage in whole health care. In other cases, social risks may be the root cause of poor health. In all cases systems that aim to deliver care that is holistic, optimally aligned with patients’ preferences, and focused on the whole person will, at a minimum, need to collect information about patients’ social and structural determinants of health and equip the interprofessional care team to help mitigate social risks and are necessarily relevant to whole health care at both a person and system level.
Addressing the social and structural determinants of health is not something that health care can or should do alone. Social services, community programs, educational systems, environmental planners, judicial systems, and employers are essential and, in many cases, primarily charged with addressing social and structural determinants of health.
Integrated Behavioral Health
The committee uses the term “integrated behavioral health” to describe when medical and behavioral health care is delivered together. The committee considered behavioral health to include both mental health and healthy behaviors, and adopted the following definition of the term:
[Integrated behavioral health] results from a practice team of primary care and behavioral health clinicians, working together with patients and families, using a systematic and cost-effective approach to provide patient-centered care for a defined population. This care may address mental health and substance abuse conditions, health behaviors (including their contribution to chronic medical illnesses), life stressors and crises, stress-related physical symptoms, and ineffective patterns of health care utilization. (Peek and the National Integration Academy Council, 2013, p. 2)
There is a growing body of research that suggests that patient experience becomes better, health outcomes improve, and costs are contained when conventional medical and behavioral health needs are addressed together (Katon and Guico-Pabia, 2011; Reiss-Brennan et al., 2016; Unützer et al., 2013).
As with addressing social needs, integrated behavioral health is a critical part of the whole health care approach (Hodgkinson et al., 2017; Miller et al., 2014; Reiss-Brennan et al., 2016). Whole health is intended to attend to and care for the whole person, and integrated behavioral health reflects that by recognizing that health and well-being include wellness for the mind and the body as well as a daily pattern of healthy behaviors. Whole health care aims to deliver care that is integrated and coordinated, not siloed. The integrated behavioral health movement has found that care is best “integrated” when delivered from a single location by co-located interprofessional team members who create a seamless experience for patients (Asarnow et al., 2015; Bokhour et al., 2020; Reiss-Brennan et al., 2016). This concept will be important for whole health systems to consider, but it may be evolving with telehealth advancements that can create seamless experiences without co-location.
Community Health
The committee identified several key concepts concerning whole health and whole health systems when reviewing critical thinking on community health (Peek et al., 2021; Sturmberg et al., 2019; Sweeney et al., 2012; Weinstein et al., 2017). When examining the field of community health, the committee broadly considered the domains of community health, population health, and public health. Communities can be defined by physical
location, shared interests, common characteristics, or other unifying factors. Veterans are a clear example of a community joined by a shared experience.
As part of the definition process, the committee decided that whole health systems are responsible for the collective health of the communities they serve, not just for individual people. When applying the whole health definition to communities, it would have the same characteristics and essential elements as applied to individual people. For example, “community whole health” is not just the absence of disease in a community but ensuring that the community thrives.
In a 1983 report, Community-Oriented Primary Care: New Directions for Health Services Delivery (IOM, 1983), the Institute of Medicine described how community context is critical when dealing with the complexities of delivering high-quality primary care. It described community-oriented primary care as
an approach to medical practice that undertakes responsibility for the health of a defined population, by combining epidemiological study and social intervention with the clinical care of individuals, so that the primary care practice itself becomes a community medicine program. Both the individual and the community or population are the focus of the diagnosis, treatment, and ongoing surveillance. (p. 70)
This description highlights the need for a population health approach to care, which is also needed to provide whole health care. Community-oriented care starts with assuming responsibility for the health of a community and proceeds to consider population-level interventions for care. This requires identifying those who need care and proactively reaching out to ensure that they get care rather than waiting to react to community members seeking care. This process ensures that people do not fall through the cracks. It is also concerned with preventing people from getting sick so that they do not need care in the first place. Proactive population health is an essential tool for health equity.
Despite the biomedical-centric language in the description above which is reflective of the time, community-oriented care also addresses the social and cultural context of individuals and families. The Implementing High-Quality Primary Care report describes this feature of community-oriented health in detail (NASEM, 2021). Including the social and cultural context in care can improve outcomes across different populations and conditions (Black et al., 2017; Derose et al., 2019; Epstein et al., 2002; Izquierdo et al., 2018; Jones et al., 2018). However, incorporating community-oriented approaches into traditional biomedical fee-for-service models does come with challenges. For example, a 2018 study found that primary care clinicians had trouble incorporating or even seeing how it could be possible to
incorporate evidence-based community, proactive, population-based programs for disease management and prevention because of health system and financial pressures to focus on diagnosis and treatment (Leppin et al., 2018).
The community is also a tool and source for the delivery of care. Being a member of a community can create a sense of belonging and purpose. It is a source of support and a resource to achieve one’s aspirations, purposes, and mission, and connection to community can be a pathway to achieving whole health (Kitchen et al., 2012). The community can be a source for understanding and changing factors that influence health, such as the social and structural determinants of health or environmental factors (Woolf et al., 2016). In addition, many community health interventions require policy, environment, community organizational, and social/interpersonal actions that only community partners can achieve (Ackermann, 2013). Achieving whole health for people and communities requires understanding the community in which people live and partnership with public health and community organizations (Krist et al., 2013).
Learning Health Systems
In 2007 the Institute of Medicine held its first in a series of workshops on the learning health system that focused on issues related to improving the evidence being created and used to inform decision making in health care (IOM, 2007). The Institute of Medicine defined a learning health system as a system “in which knowledge generation is so embedded into the core of the practice of medicine that it is a natural outgrowth and product of the health care delivery process and leads to continual improvement in care” (IOM, 2007, p. 6). Learning health systems should emphasize continuous learning and have learning and knowledge translation inform patient care (Grumbach et al., 2014). Moreover, synergies should exist among the research, clinical, and educational missions of the learning health system.
Learning health systems need data they can access rapidly in order to make iterative changes. Multiple sources, such as a system’s electronic health record or claims data sourced from an insurer or accountable care organization, can provide the necessary data (Etheredge, 2007). In addition, a learning health system requires methods for analyzing big data combined with system sciences, such as translational and implementation sciences, to understand the impacts of changes on person and system outcomes (Maddox et al., 2017; Mandl et al., 2014; Mullins et al., 2018). This learning health systems approach can guide the evidence for enabling a health system’s transformation to delivering whole health.
FINDINGS AND CONCLUSIONS
To support the committee in identifying and studying whole health systems within the VA and more broadly in the United States and internationally, this chapter provides an updated universal definition of whole health, identifies the essential elements of whole health systems, and highlights lessons from other domains of critical thinking that can inform whole health system design. This information provides the framework for the findings presented in the subsequent chapters of this report. More importantly, this chapter provides a concrete description of the aspirational goals for systems interested in providing whole health, and the subsequent chapters provide a detailed roadmap with examples including successes and failures, challenges, and lessons learned from the whole health field.
The universal definition defines what whole health is—“physical, behavioral, spiritual, and socioeconomic well-being as defined by individuals, families, and communities.” The definition also defines what a whole health approach is—“an interprofessional, team-based approach anchored in trusted longitudinal relationships to promote resilience, prevent disease, and restore health. It aligns with a person’s life mission, aspiration, and purpose.” The five foundational elements of whole health are broadly identified as (1) people-centered, (2) comprehensive and holistic, (3) upstream-focused, (4) equitable and accountable, and grounded in (5) team well-being.
An important feature of whole health care is that it is tailored to the needs of the person, family, and community, which means that there will be considerable variation in how effective whole health systems look and function. For example, systems that care for communities with higher social needs will look different from those that care for communities with higher mental health needs. Another key feature is that whole health is grounded in equity. Inequity is a primary cause for poor health, and it is not possible for communities to achieve whole health without addressing inequity.
The VA has been a leader in creating a culture of whole health and is redesigning its system to deliver whole health care. It has successfully focused its design to address several pressing needs of veterans, specifically chronic pain, post-traumatic stress disorder, mental trauma, and disability. Expanding the whole health focus to address the full range of veteran needs across different communities and supporting veterans in different phases of their life will be necessary for all veterans to receive the benefits of whole health care. This will require the VA to expand is definition and support for whole health.
Many veterans receive care outside of the VA. Therefore, for all veterans to receive whole health benefits, they must be able to access whole health care in all settings, not just VA settings. Fortunately, the concept of
whole health is gaining widespread acceptance as the aspirational goal of health care. Accordingly, many health systems beyond the VA have adopted a mission to promote whole health and are developing their approaches to whole health care delivery.
However, this field is very much in its infancy. Improving the understanding of what whole health means and the best way to help people, families, and communities achieve it is an enduring adaptive process. It is worth pursuing and should be a common health care goal. The committee’s definition and the five foundational elements can help to inform the next phases of this national journey.
REFERENCES
Ackermann, R. T. 2013. Bridging the why and the how of clinical–community integration. American Journal of Preventive Medicine 45(4):526–529.
AHRQ (Agency for Healthcare Research and Quality). 2019. 2018 National Healthcare Quality and Disparities Report. AHRQ Publ. No. 19-0070-EF. Rockville MD: Agency for Healthcare Research and Quality.
Alley, D. E., C. N. Asomugha, P. H. Conway, and D. M. Sanghavi. 2016. Accountable health communities—Addressing social needs through Medicare and Medicaid. New England Journal of Medicine 374(1):8–11.
Anastas, T., E. N. Waddell, S. Howk, M. Remiker, G. Horton-Dunbar, and L. J. Fagnan. 2018. Building behavioral health homes: Clinician and staff perspectives on creating integrated care teams. Journal of Behavioral Health Services & Research 46(3):475–486.
Asarnow, J. R., M. Rozenman, J. Wiblin, and L. Zeltzer. 2015. Integrated medical–behavioral care compared with usual primary care for child and adolescent behavioral health: A meta-analysis. JAMA Pediatrics 169(10):929–937.
Benjamin, R. M. 2011. The national prevention strategy: Shifting the nation’s health-care system. Public Health Reports 126(6):774–776.
Bhattacharya, S., K. B. Pradhan, M. A. Bashar, S. Tripathi, A. Thiyagarajan, A. Srivastava, and A. Singh. 2020. Salutogenesis: A bona fide guide towards health preservation. Journal of Family Medicine and Primary Care 9(1):16–19.
Black, R. E., C. E. Taylor, S. Arole, A. Bang, Z. A. Bhutta, A. M. R. Chowdhury, B. R. Kirk-wood, N. Kureshy, C. F. Lanata, J. F. Phillips, M. Taylor, C. G. Victora, Z. Zhu, and H. B. Perry. 2017. Comprehensive review of the evidence regarding the effectiveness of community-based primary health care in improving maternal, neonatal and child health: 8. Summary and recommendations of the expert panel. Journal of Global Health 7(1):010908.
Bokhour, B. G., J. Hyde, S. Zeliadt, and D. Mohr. 2020. Whole health system of care evaluation—A progress report on outcomes of the WHS pilot at 18 flagship sites. Bedford, MA: VA Center for Evaluating Patient-Centered Care in VA.
Bolton, R. E., B. G. Bokhour, T. P. Hogan, T. M. Luger, M. Ruben, and G. M. Fix. 2019. Integrating personalized care planning into primary care: A multiple-case study of early adopting patient-centered medical homes. Journal of General Internal Medicine 35(2):428–436.
Braveman, P., and L. Gottlieb. 2014. The social determinants of health: It’s time to consider the causes of the causes. Public Health Reports 129(Suppl 2):19-31.
Campbell, R. 2016. The five rights of clinical decision support: CDS tools helpful for meeting meaningful use. Journal of AHIMA 84(10):42–47.
Cloninger, C. R., L. Salvador-Carulla, L. J. Kirmayer, M. A. Schwartz, J. Appleyard, N. Goodwin, J. Groves, M. H. M. Hermans, J. E. Mezzich, C. W. van Staden, and S. Rawaf. 2014. A time for action on health inequities: Foundations of the 2014 Geneva Declaration on Person- and People-Centered Integrated Health Care for All. International Journal of Person Centered Medicine 4(2):69–89.
Derose, K. P., M. V. Williams, C. A. Branch, K. R. Flórez, J. Hawes-Dawson, M. A. Mata, C. W. Oden, and E. C. Wong. 2019. A community-partnered approach to developing church-based interventions to reduce health disparities among African Americans and Latinos. Journal of Racial and Ethnic Health Disparities 6(2):254–264.
Epperly, T., R. Roberts, S. Rawaf, C. V. Weel, R. Phillips, J. E. Mezzich, R. Wilson, Y. P. T. Ghebrehiwet, and J. Appleyard. 2015. Person-centered primary health care: Now more than ever. International Journal of Person Centered Medicine 5(2):53–59.
Epstein, L., J. Gofin, R. Gofin, and Y. Neumark. 2002. The Jerusalem experience: Three decades of service, research, and training in community-oriented primary care. American Journal of Public Health 92(11):1717–1721.
Etheredge, L. M. 2007. A rapid-learning health system. Health Affairs (Millwood) 26(2): w107–w118.
Fix, G. M., R. E. Bolton, and B. G. Bokhour. 2017. Challenges in implementing personalized care planning. JAMA 318(17):1713–1714.
Grembowski, D., J. Schaefer, K. E. Johnson, H. Fischer, S. L. Moore, M. Tai-Seale, R. Ricciardi, J. R. Fraser, D. Miller, L. LeRoy, and AHRQ MCC Research Network. 2014. A conceptual model of the role of complexity in the care of patients with multiple chronic conditions. Medical Care 52(Suppl 2):S7–S14.
Grumbach, K., C. R. Lucey, and S. C. Johnston. 2014. Transforming from centers of learning to learning health systems: The challenge for academic health centers. JAMA 311(11):1109–1110.
Hodgkinson, S., L. Godoy, L. S. Beers, and A. Lewin. 2017. Improving mental health access for low-income children and families in the primary care setting. Pediatrics 139(1):e20151175.
HRSA (Health Resources and Services Administration). 2018. Health center program compliance manual. Washington, DC: Health Resources and Services Administration.
HRSA. 2021. What is a health center? https://bphc.hrsa.gov/about-health-centers/what-health-center (accessed November 1, 2022).
HRSA. 2022. Health center program program: Impact and growth. https://bphc.hrsa.gov/about-health-centers/health-center-program-impact-growth (accessed July 11, 2022).
IOM (Institute of Medicine). 1983. Community oriented primary care: New directions for health services delivery. Washington, DC: National Academy Press.
IOM. 2007. The learning healthcare system: Workshop summary. Washington, DC: The National Academies Press.
IOM. 2009. State of the USA health indicators: Letter report. Washington, DC: The National Academies Press.
IOM/NRC (National Research Council). 2013. U.S. health in international perspective: Shorter lives, Poorer health. Washington, DC: The National Academies Press.
Izquierdo, A., M. Ong, E. Pulido, K. B. Wells, M. Berkman, B. Linski, V. Sauer, and J. Miranda. 2018. Community partners in care: 6- and 12-month outcomes of community engagement versus technical assistance to implement depression collaborative care among depressed older adults. Ethnicity & Disease 28(Suppl 2):339–348.
Jonas, W. B., and R. A. Chez. 2004. Toward optimal healing environments in health care. Journal of Alternative and Complementary Medicine 10(Suppl 1):S1–S6.
Jonas, W. B., and E. Rosenbaum. 2021. The case for whole-person integrative care. Medicina 57(7):677.
Jones, K. A., S. Do, L. Porras-Javier, S. Contreras, P. J. Chung, and T. R. Coker. 2018. Feasibility and acceptability in a community-partnered implementation of centering parenting for group well-child care. Academic Pediatrics 18(6):642–649.
Katon, W., and C. J. Guico-Pabia. 2011. Improving quality of depression care using organized systems of care: A review of the literature. Primary Care Companion for CNS Disorders 13(1):e1–e8.
Kilbourne, A. M., M. Bramlet, M. M. Barbaresso, K. M. Nord, D. E. Goodrich, Z. Lai, E. P. Post, D. Almirall, L. Verchinina, S. A. Duffy, and M. S. Bauer. 2014. SMI life goals: Description of a randomized trial of a collaborative care model to improve outcomes for persons with serious mental illness. Contemporary Clinical Trials 39(1):74–85.
Kitchen, P., A. Williams, and J. Chowhan. 2012. Sense of community belonging and health in Canada: A regional analysis. Social Indicators Research 107:103–126.
Kligler, B. 2022. Whole health in the Veterans Health Administration. Global Advances in Health and Medicine 11:1–4.
Krist, A. H., D. Shenson, S. H. Woolf, C. Bradley, W. R. Liaw, S. F. Rothemich, A. Slonim, W. Benson, and L. A. Anderson. 2013. Clinical and community delivery systems for preventive care. American Journal of Preventive Medicine 45(4):508–516.
Kuzel, A. J. 2009. Ten steps to a patient-centered medical home. Family Practice Management 16(6):18–24.
Leppin, A. L., K. Schaepe, J. Egginton, S. Dick, M. Branda, L. Christiansen, N. M. Burow, C. Gaw, and V. M. Montori. 2018. Integrating community-based health promotion programs and primary care: A mixed methods analysis of feasibility. BMC Health Services Research 18(1):72.
Loeb, D. F., I. A. Binswanger, C. Candrian, and E. A. Bayliss. 2015. Primary care physician insights into a typology of the complex patient in primary care. Annals of Family Medicine 13(5):451–455.
Lushniak, B. D., D. E. Alley, B. Ulin, and C. Graffunder. 2015. The national prevention strategy: Leveraging multiple sectors to improve population health. American Journal of Public Health 105(2):229–231.
Maddox, T. M., N. M. Albert, W. B. Borden, L. H. Curtis, T. B. Ferguson, Jr., D. P. Kao, G. M. Marcus, E. D. Peterson, R. Redberg, J. S. Rumsfeld, N. D. Shah, and J. E. Tcheng. 2017. The learning healthcare system and cardiovascular care: A scientific statement from the American Heart Association. Circulation 135(14):e826–e857.
Mandl, K. D., I. S. Kohane, D. McFadden, G. M. Weber, M. Natter, J. Mandel, S. Schneeweiss, S. Weiler, J. G. Klann, J. Bickel, W. G. Adams, Y. Ge, X. Zhou, J. Perkins, K. Marsolo, E. Bernstam, J. Showalter, A. Quarshie, E. Ofili, G. Hripcsak, and S. N. Murphy. 2014. Scalable collaborative infrastructure for a learning healthcare system (SCILHS): Architecture. Journal of the American Medical Informatics Association 21(4):615–620.
Martin, J. C., R. F. Avant, M. A. Bowman, J. R. Bucholtz, J. C. Dickinson, K. L. Evans, L. A. Green, D. E. Henley, W. A. Jones, S. C. Matheny, J. E. Nevin, S. L. Panther, J. C. Puffer, R. G. Roberts, D. V. Rodgers, R. A. Sherwood, K. C. Stange, and C. W. Weber. 2004. The Future of Family Medicine: A collaborative project of the family medicine community. Annals of Family Medicine 2(Suppl 1):S3–S32.
McClellan, M., A. N. McKethan, J. L. Lewis, J. Roski, and E. S. Fisher. 2010. A national strategy to put accountable care into practice. Health Affairs (Millwood) 29(5):982–990.
McGinnis, J. M., and W. H. Foege. 1993. Actual causes of death in the United States. JAMA 270(18):2207–2212.
Miller, B. F., S. Petterson, B. T. Burke, R. L. Phillips, Jr., and L. A. Green. 2014. Proximity of providers: Colocating behavioral health and primary care and the prospects for an integrated workforce. American Psychologist 69(4):443–451.
Mokdad, A. H. 2004. Actual causes of death in the United States, 2000. JAMA 291(10):1238–1245.
Mullins, C. D., L. T. Wingate, H. A. Edwards, T. Tofade, and A. Wutoh. 2018. Transitioning from learning healthcare systems to learning health care communities. Journal of Comparative Effectiveness Research 7(6):603–614.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2019a. Integrating social care into the delivery of health care: Moving upstream to improve the nation’s health. Washington, DC: The National Academies Press.
NASEM. 2019b. Taking action against clinician burnout: A systems approach to professional well-being. Washington, DC: National Academies Press.
NASEM. 2021. Implementing high-quality primary care: Rebuilding the foundation of health care. Washington, DC: The National Academies Press.
Nash, D. B., R. J. Fabius, A. Skoufalos, and J. L. Clarke. 2016. Population health: Creating a culture of wellness. Burlingon, MA: Jones and Bartlett Learning.
National Association of Community Health Centers. 2022. Community health center chartbook. Bethesda, MD: National Association of Community Health Centers.
National Committee for Quality Assurance. 2018. Goals to care: How to keep the person in “person-centered”. National Committee for Quality Assurance. https://www.ncqa.org/news/person-centered-care-planning-identifying-goals-and-developing-care-plans/ (accessed October 20, 2022).
Nelson, H. D., A. Cantor, J. Wagner, R. Jungbauer, A. Quinones, L. Stillman, and K. Kondo. 2020. Achieving health equity in preventive services: A systematic review for a National Institutes of Health pathways to prevention workshop. Annals of Internal Medicine 172(4):258–271.
Peek, C. J., and the National Integration Academy Council. 2013. Lexicon for behavioral health and primary care integration: Concepts and definitions developed by expert consensus. Rockville, MD: Agency for Healthcare Research and Quality.
Peek, C. J., J. M. Westfall, K. C. Stange, W. Liaw, B. Ewigman, J. E. DeVoe, L. A. Green, M. E. Polverento, N. Bora, F. V. deGruy, P. G. Harper, and N. J. Baker. 2021. Shared language for shared work in population health. Annals of Family Medicine 19(5):450–456.
Primary Care Collaborative. 2022. Joint principles of the patient-centered medical home. https://www.pcpcc.org/ (accessed February 1, 2022).
Reiss-Brennan, B., K. D. Brunisholz, C. Dredge, P. Briot, K. Grazier, A. Wilcox, L. Savitz, and B. James. 2016. Association of integrated team-based care with health care quality, utilization, and cost. JAMA 316(8):826–834.
Safford, M. M., J. J. Allison, and C. I. Kiefe. 2007. Patient complexity: More than comorbidity. The vector model of complexity. Journal of General Internal Medicine 22(Suppl 3):382–390.
Sakallaris, B. R., L. MacAllister, M. Voss, K. Smith, and W. B. Jonas. 2015. Optimal healing environments. Global Advances in Health and Medicine 4(3):40–45.
Schwartz, R. 2014. Re: OIG-403-p3, medicare and state health care programs: Fraud and abuse; revisions to safe harbors under the anti-kickback statute, and civil monetary penalty rules regarding beneficiary inducements and gainsharing. Bethesda, MD: National Association of Community Health Centers.
Schwenk, T. L. 2018. Physician well-being and the regenerative power of caring. JAMA 319(15):1543–1544.
Seidel, I., B. Garcia, R. Cendreda, N. Purcell, and K. H. Seal. 2021. Virtual whole health passport group: Empowering veterans with smart goals and community during COVID-19. Global Advances in Health and Medicine 10:27.
Stewart, M. 2014. Patient-centered medicine: Transforming the clinical method, 3rd ed. London: Radcliffe Publishing.
Sturmberg, J. P., M. Picard, D. C. Aron, J. M. Bennett, J. Bircher, M. J. deHaven, S. M. W. Gijzel, H. H. Heng, J. A. Marcum, C. M. Martin, A. Miles, C. L. Peterson, N. Rohleder, C. Walker, M. G. M. Olde Rikkert, and R. J. F. Melis. 2019. Health and disease—Emergent states resulting from adaptive social and biological network interactions. Frontiers in Medicine 6:59.
Sweeney, S. A., A. Bazemore, R. L. Phillips, Jr., R. S. Etz, and K. C. Stange. 2012. A reemerging political space for linking person and community through primary health care. American Journal of Public Health 102(Suppl 3):S336–S341.
Thomas, H., G. Mitchell, J. Rich, and M. Best. 2018. Definition of whole person care in general practice in the English language literature: A systematic review. BMJ Open 8(12):e023758.
Tick, H., and A. Nielsen. 2019. Academic consortium for integrative medicine and health commentary to Health and Human Services (HHS) on inter-agency task force pain management best practices draft report. Global Advances in Health and Medicine 8:216495611985765.
Tipirneni, R., K. D. Vickery, and E. P. Ehlinger. 2015. Accountable communities for health: Moving from providing accountable care to creating health. Annals of Family Medicine 13(4):367–369.
Unützer, J., M. Schoenbaum, and B. Druss. 2013. The collaborative care model: An approach for integrating physical and mental health care in Medicaid health homes. Center for Health Care Strategies. https://www.chcs.org/resource/the-collaborative-care-model-anapproach-for-integrating-physical-and-mental-health-care-in-medicaid-health-homes/ (accessed October 17, 2022).
VA (Department of Veterans Affairs). 2021. Whole Health System implementation guide. Washington, DC: U.S. Department of Veterans Affairs.
VA. 2022a. Whole health. https://www.va.gov/wholehealth/ (accessed January 5, 2022).
VA. 2022b. Implementing a Whole Health System: patient and team perspectives. https://www.va.gov/WHOLEHEALTHLIBRARY/overviews/implementing-a-whole-health-system.asp (accessed December 12, 2022).
Vaughn, L. M., and M. Lohmueller. 2014. Calling all stakeholders: Group-level assessment (GLA)-a qualitative and participatory method for large groups. Evaluation Review 38(4):336-355.
Wagner, E. H., B. T. Austin, and M. Von Korff. 1996. Organizing care for patients with chronic illness. Milbank Quarterly 74(4):511–544.
Wagner, E. H., B. T. Austin, C. Davis, M. Hindmarsh, J. Schaefer, and A. Bonomi. 2001. Improving chronic illness care: Translating evidence into action. Health Affairs (Millwood) 20(6):64–78.
Weinstein, J. N., A. Geller, Y. Negussie, A. Baciu, and National Academies of Sciences, Engineering, and Medicine Committee on Community-Based Solutions to Promote Health Equity in the United States. 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press.
WHO (World Health Organization). 1984. Health promotion: A discussion document on the concept and principles: Summary report of the Working Group on Concept and Principles of Health Promotion, Copenhagen, 9–13 July 1984. Regional Office for Europe. Geneva: World Health Organization.
WHO. 2020. Basic documents. 49th ed. Geneva: World Health Organization.
WHO. 2022. Primary health care. https://www.who.int/health-topics/primary-healthcare#tab=tab_1 (accessed November 30, 2022).
Wiley, L. F., and G. W. Matthews. 2017. Health care system transformation and integration: A call to action for public health. Journal of Law, Medicine and Ethics 45(1 Suppl):94–97.
Woolf, S. H., E. Zimmerman, A. Haley, and A. H. Krist. 2016. Authentic engagement of patients and communities can transform research, practice, and policy. Health Affairs 35(4):590–594.
Wright, B. 2013. Who governs federally qualified health centers? Journal of Health Politics, Policy, and Law 38(1):27–55.
Wright, B. 2015. Do patients have a voice? The social stratification of health center governing boards. Health Expectations 18(3):430–437.
Wyatt, R., Laderman, M., Botwinick, L, Mate, K., Whittington, J. 2016. Achieving health equity: A guide for health care organizations. IHI white paper. Cambridge, MA: Institute for Healthcare Improvement.
This page intentionally left blank.


























