1
Introduction
The development of genome editing technologies that have the potential to precisely and efficiently make modifications to DNA inside cells has resulted in renewed attention to the implications of such advances for clinical use in humans. These technologies can be used in different ways; this report focuses on one type of use—making changes to human DNA that could be inherited by future generations. This possibility occurs when genome editing results in the alteration of the DNA in gametes (eggs or sperm) or any cells that give rise to gametes, including the single cell zygote resulting from fertilization of an egg by a sperm cell, or cells of an early embryo. When used clinically, changes to the DNA in such cells can be passed on to the next generation—a process referred to in the report as heritable human genome editing (HHGE) (see Box 1-1).
Germline genome editing is already in use in plant and non-human animal species, primarily in a research context. But the use in humans of heritable genome editing raises many critical and potentially contentious issues. The challenge of assessing safety and efficacy is particularly great, since the effects may not be immediately apparent and could affect future generations. Moreover, individuals’ ability to access HHGE, as with other medical technologies, would likely be uneven, raising issues of equity and social justice. Decisions about whether or not to make heritable changes in human DNA sequences and, if so, the nature of genetic changes that should or should not be permitted, requires extensive input from across a country. If extensive societal discussions were to result in approval to consider certain clinical applications of HHGE, it would be essential to have an effective
translational framework for evaluating the safety and efficacy of the genome editing, assessing the balance of benefits and harms for any given treatment, and overseeing and governing its responsible development and use.
INTERNATIONAL DISCUSSIONS OF HERITABLE HUMAN GENOME EDITING
There is a long history of discussions on ethical and social implications of making heritable changes to the human genome (Evans, 2002; Fletcher, 1971; Frankel and Chapman, 2000; President’s Commission, 1982; Stock and Campbell, 2000), and recent developments in genome editing methods have resulted in renewed urgency in these discussions, which are no longer of purely theoretical interest. Following the demonstration that CRISPR-Cas systems1 can be used to readily edit the genomes of living human cells,
___________________
1 CRISPR stands for clustered regularly interspaced short palindromic repeats, and Cas stands for CRISPR-associated protein. See the glossary at the end of the report for the definition of these and other terms used throughout.
multiple members of the scientific community developing the technology, professional scientific societies, academies of sciences and medicine, bioethics scholars and organizations, and many others convened discussions and published statements and reports addressing the implications of genome editing in humans. For example, the International Bioethics Committee of the United Nations Educational, Scientific, and Cultural Organization issued updated guidance to reflect genome editing advances (UNESCO, 2015). The U.S. National Academy of Sciences and National Academy of Medicine, the U.K.’s Royal Society, and the Chinese Academy of Sciences convened an International Summit on Human Gene Editing that drew more than 3,500 in-person and online participants (NASEM, 2015). More than 60 reports have been published from more than 50 countries dealing wholly or in part with HHGE (e.g., ANM, 2016; Bosley et al., 2015; Brokowski, 2018; CEST, 2019; EGE, 2016; FEAM, 2017; Hinxton Group, 2015; ISSCR, 2015; KNAW, 2016; Lanphier et al., 2015; Leopoldina, 2015; NASEM, 2017). Many groups reiterated that any use of HHGE remained premature and should not be undertaken, with some calling for an explicit moratorium or international prohibition on such use, and others emphasized that HHGE should not be attempted unless or until safety and efficacy were better understood and extensive public engagement and social decision making had taken place. Reports similarly noted the need for appropriate national and transnational oversight and governance structures to be developed prior to any clinical use of HHGE (ISSCR, 2016; NCB, 2016).
In 2017, the U.S. National Academies of Sciences, Engineering, and Medicine released a report authored by an international committee that examined both somatic cell and germline genome editing, possible clinical applications of these technologies, potential risks and benefits, and the regulation of human genome editing (NASEM, 2017). As with prior studies, the report emphasized that any clinical use of HHGE would be premature and that extensive public participation should precede any consideration to authorize clinical trials. However, the report went on to say that HHGE might be permissible sometime in the future, after much more research had been done on balancing risks and benefits, and identified 10 criteria for potential future clinical evaluation of the process as part of a robust regulatory framework. Likewise, in a 2018 extension of its earlier report, the Nuffield Council on Bioethics stated that it could “envision circumstances in which heritable genome editing interventions should be permitted” (NCB, 2018, p. 154). However, such uses would need to safeguard the welfare of people affected by such interventions and not produce or exacerbate social divisions or the marginalization of disadvantaged groups within a country.
CLINICAL USE OF HERITABLE HUMAN GENOME EDITING REPORTED
In 2018, on the eve of the Second International Summit on Human Genome Editing in Hong Kong, a scientist working in Shenzhen, China, announced that he had used genome editing tools to make alterations in early human embryos that were subsequently transferred to the intended mother, resulting in the birth of twin girls (NASEM, 2019b). At the summit, the researcher revealed that a second pregnancy had been established using a similarly-edited embryo. In his presentation at the summit, he described how his research team had “conducted experiments on embryos from mice and monkeys, human embryonic stem cells, and cultured human embryos” to introduce a deletion into the CCR5 gene, which “plays a role in the infection of cells by human immunodeficiency virus” (NASEM, 2019b, p. 2). Concluding that the procedure was safe, the researcher and his associates used CRISPR-Cas9 in fertilized human eggs in an attempt to edit CCR5 and protect the resulting children against infection by this virus. The data presented in Hong Kong revealed that the CCR5 target was fully modified in only one of the embryos, and the scientists’ claims have not been independently and publicly verified (Cohen, 2019a; Cyranoski, 2019). Following an investigation by Chinese authorities, it was announced at the end of 2019 that the researcher and his collaborators had been found guilty of having “forged ethical review documents and misled doctors into unknowingly implanting gene-edited embryos into two women” and had received fines and prison sentences (Normile, 2019).
The response to the news of this clinical use of HHGE was immediate and forceful. Despite what many had viewed as general agreement within scientific and clinical communities that it would be premature and irresponsible to undertake HHGE at this time, it had apparently taken place. In its concluding statement, the summit organizing committee described the reported clinical use of HHGE as “deeply disturbing” and criticized the violation of ethical standards and lack of transparency in the development, review, and conduct of the clinical procedures. It went on to state that clinical trials of HHGE could become acceptable in the future if (1) the risks could be evaluated and satisfactorily addressed, and (2) criteria on societal acceptability were met. It suggested that “it is time to define a rigorous, responsible translational pathway toward such trials” (NASEM, 2019b, p. 7).
More than 100 Chinese scientists signed an online declaration calling the work “crazy” (Cohen, 2019b). Scientists declared that such an experiment on human beings is not morally or ethically defensible. There were renewed calls for a global moratorium on clinical use of HHGE for a defined period of time, to allow time to develop international guidelines
(ASGCT, 2019; Lander, et al., 2019). The German Ethics Council echoed the call for an international moratorium and recommended that an international oversight agency be established to develop standards by which such interventions could be administered, should they be determined to be safe, efficacious, and permissible (GEC, 2019). While supporting the need to address HHGE, others argued against declaring a moratorium because of concerns that it would be open-ended in duration, could impede scientific research, and could be less effective than developing stringent oversight systems (Adashi and Cohen, 2019).
FORMATION OF THE INTERNATIONAL COMMISSION AND WORLD HEALTH ORGANIZATION EXPERT COMMITTEE
Two international committees were convened following these calls to further develop an understanding of what would be involved in a responsible translational pathway toward HHGE and to make progress on effective coordination and governance of human genome editing.
The International Commission on the Clinical Use of Human Germline Genome Editing (the Commission authoring the present report) was convened by the U.S. National Academy of Medicine, the U.S. National Academy of Sciences, and the U.K.’s Royal Society. The Commission has been tasked with developing a framework for scientists, clinicians, and regulatory authorities to consider when assessing potential clinical applications of HHGE. This framework could be used in the development of a potential pathway from research to clinical use, should a country conclude that HHGE applications are acceptable. The Commission’s goal is to prepare the way for international agreement on specific criteria and standards that would have to be met before HHGE could be deemed permissible, if permissible at all.
The World Health Organization (WHO) also established a global multidisciplinary expert committee to examine the scientific, ethical, social, and legal challenges associated with human genome editing—both somatic and heritable (WHO, 2019b). The Expert Advisory Committee on Human Genome Editing will advise the director general of the WHO on appropriate oversight and governance mechanisms, both at the national and global levels.
While the deliberations of the Academies’ International Commission and the WHO’s Expert Advisory Committee are likely to overlap to some extent with respect to HHGE, the WHO Committee’s focus is on governance mechanisms, while the Academies’ Commission is more concerned with the scientific and technological questions that would need to be addressed as part of such governance. The WHO Committee will also consider the broader social and ethical questions raised by the possible use of
HHGE, whereas this Commission’s mandate is limited to issues inextricably linked to research and clinical practice.
This report has been released while the WHO Committee is still developing its recommendations and is intended to inform that committee’s deliberations. It should also be relevant to national and international policy makers as they consider laws and regulatory frameworks for HHGE. Inevitably, it provides a current snapshot of the relevant technologies and addresses only some of the issues that policy makers will need to take into account.
MITOCHONDRIAL REPLACEMENT TECHNIQUES: MODIFYING THE EMBRYO
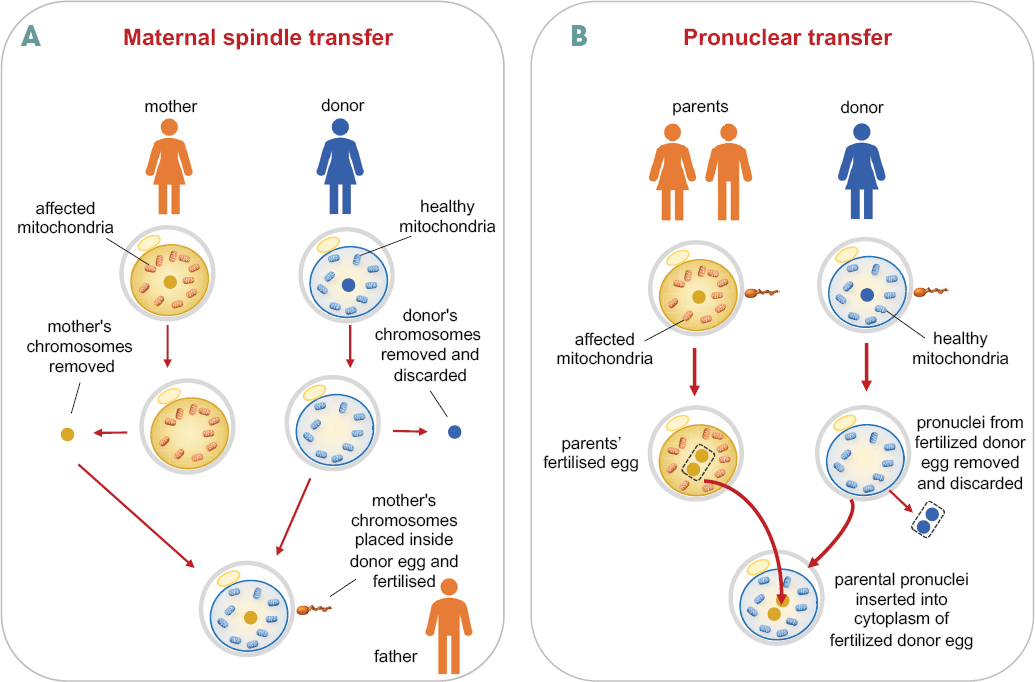
In developing its recommendations, the Commission sought to learn from prior experience with related technologies. Mitochondrial replacement techniques (MRT) constitute the only technology currently approved anywhere in the world that results in genetic changes that can be inherited. The approval of MRT for clinical use in the United Kingdom was driven by patient need and was introduced only after extensive preclinical research and consideration by a regulatory body already established for the oversight of assisted reproductive technologies (ARTs).2 The principle of MRT is illustrated in Figure 1-1.
In addition to the DNA contained in chromosomes in the cell nucleus (the nuclear genome), eukaryotic cells also contain hundreds or thousands of DNA molecules in organelles called mitochondria; these DNA molecules constitute the mitochondrial genome. People inherit their mitochondrial DNA (mtDNA) only from their biological mother, since sperm mitochondria are eliminated during embryo development. Disease-causing mtDNA mutations can occur in all or a fraction of the mitochondria in a person’s cells.3 These mutations can cause a wide variety of human diseases for which little or no treatment is currently available. One in every 5,000 to 10,000 people develops a symptomatic mtDNA disease.
In one method of MRT, referred to as maternal spindle transfer, eggs are harvested from the intended mother who has pathogenic mtDNA, and the chromosomes of the nuclear genome of each egg are removed and transferred to the donated eggs of a woman with healthy mtDNA from which the chromosomes of the nuclear genome have been removed. After fertil-
___________________
2 Additional information is available at https://www.hfea.gov.uk/treatments/embryo-testing-and-treatments-for-disease/mitochondrial-donation-treatment/.
3 A change in DNA sequence that produces a change in phenotype is referred to in this report as a “mutation” or a “pathogenic variant.” Other changes in DNA sequence that are typically common in the population and have little or no effect on disease risk are referred to as “variants.”
ization, the resulting embryos are transferred to the intended mother. An alternative method of MRT, called pronuclear transfer, involves transferring chromosomes of the nuclear genome between zygotes rather than between unfertilized eggs. With both methods, a child born using MRT has nuclear DNA from the child’s mother and father and mtDNA from the egg donor.
With MRT, no DNA sequences are directly altered; rather, entire chromosomes are transferred from one egg to another. By contrast, HHGE makes it possible to alter the DNA sequence of any of the 6 billion base pairs comprising the complete set of the mother’s and father’s chromosomes.
MRT was first legally approved for clinical use in the United Kingdom and is carried out under the regulatory framework of the U.K. Human Fertilisation and Embryology Authority (HFEA), which grants approval for treatment on a case-by-case basis. MRT is only permitted for the prevention of serious mtDNA disease, with the additional caveats that licenses can only be granted to named clinics after demonstration of their competence, and any use is restricted to prospective parents with no suitable alternative for having an unaffected, genetically-related child. The steps involved in developing a translational pathway for MRT in the United Kingdom are summarized in Box 1-2. Despite the important differences between MRT and HHGE, this pathway can provide insights to inform similar debates about HHGE.
A TRANSLATIONAL PATHWAY FOR HERITABLE HUMAN GENOME EDITING
By a “translational pathway” for HHGE, the Commission means the steps that would be needed to enable a proposed clinical use to proceed from preclinical research to application in humans. Elements that formed the pathway leading to clinical use of MRT in the United Kingdom have informed the Commission’s development of a clinical pathway toward HHGE, presented in this report. The core elements of this pathway are shown in Figure 1-2 and described below.
Societal Considerations
As demonstrated by the example of MRT, progress through a clinical translational pathway for controversial technologies such as HHGE requires widespread public discussion about whether a technology is broadly acceptable and, if so, for what purposes, with which checks and balances, and with what oversight. These considerations are shown in the orange boxes in Figure 1-2.
The upper box on the left side of the figure represents critical deliberations that would be required prior to any society determining that it would permit the clinical use of HHGE. Such discussions will need to include broad public engagement on the potential uses and implications of HHGE, as well as development of those legislative, regulatory, and institutional foundations that would need to be in place prior to any clinical use.
The lower box reflects the fact that, even were an initial clinical use and evaluation of HHGE to be permitted and undertaken, societal deliberations would need to continue. The outcomes of any initial human use of HHGE would need to be considered, lessons taken into account, and further extensive scientific, clinical, stakeholder, and public input incorporated to decide whether to consider any further clinical uses.
These discussions are as important as the clinical pathway components (on the right side of the figure) but are beyond this Commission’s Statement of Task (see Box 1-3). Questions that deserve significant attention include how to effectively engage multiple sectors of the public, including genetic disease and disability communities, and how to incorporate the diverse input received into a country’s decision-making processes. Through presentations to the Commission and responses to the Commission’s call for evidence, respondents from civil society, including genetic disease and disability communities, shared elements they felt are important to consider. Though addressing these elements was not in the Commission’s charge, two themes may inform future HHGE deliberations:
- The need for discourse within civil society about human genome editing. It will be important not to limit the focus of public engagement and civil society discussions to only scientific and clinical dimensions. Discussions must also occur concerning the implications of HHGE for inequity and social justice, the value placed on genetic relatedness of a child and on parental reproductive preferences, societal attitudes toward disease and disease prevention, privacy considerations, religious scholarship, and ethics.
- The importance of engaging directly with people who have conditions that might be considered for HHGE. People who are living with genetic disease or disability must be able to meaningfully participate in societal discussions of genome editing and take part in policy development processes. It is important that not all engagement be led by scientific and clinical communities but also by those whom the technology would most affect.
Decision by a Country to Permit Consideration of Heritable Human Genome Editing for a Proposed Clinical Use
A country’s lawmakers need to assess information on the safety and potential therapeutic efficacy of a technology and give consideration to public opinion to decide whether a new medical technology should be made available within its jurisdiction and, if so, for what uses it should be permitted. These considerations are shown in the green box in Figure 1-2. The outcomes of extensive societal deliberations and sufficient progress in preclinical development of the techniques for HHGE would together feed into a country’s decision on whether or not HHGE could be considered for clinical use. If a country’s legislative body does not permit the consideration of HHGE for the proposed purpose, the pathway toward clinical use cannot proceed beyond basic laboratory research and preclinical development. HHGE currently remains illegal or otherwise not approved in many countries. It is not specifically regulated in other countries, which would need to consider establishing relevant national regulations.
Clinical Pathway for a Specific Proposed Use of Heritable Human Genome Editing
The focus of this Commission’s task is the track shown on the right side of Figure 1-2 in the blue boxes. Any pathway for the use of HHGE starts with a specific proposed use. It consists of four primary elements. The blue box at the top of the figure represents the development of preclinical evidence that demonstrates the feasibility of HHGE for the proposed use.
Such evidence would be obtained from laboratory studies in cultured cells, genome editing in other types of non-germline human tissues, studies in animal models, and research in human embryos that are not used to create a pregnancy. Research into heritable genome editing is currently at this stage of the pathway.
Two critical decision points occur in the middle of the pathway. First, as described above, a country must permit the consideration of HHGE for clinical use (green box). Were a country to permit the relevant national regulatory authority to consider a request to use HHGE for a proposed purpose, a second critical decision point is reached (second blue box). Once the preclinical evidence base has been established and a particular methodology is deemed to meet safety and efficacy thresholds, an application may be made to the appropriate regulatory body requesting the opportunity to use the technology in humans. Any clinical team seeking to proceed with an initial use of HHGE would need to receive scientific and ethics approvals from institutional and/or national advisory bodies or regulatory authorities prior to undertaking any clinical use.
Finally, should such approvals be granted, clinical use of HHGE for the proposed purpose could be undertaken (lower blue box). This is the stage at which a human pregnancy would be attempted by uterine transfer of an embryo whose genome had undergone editing. Further evidence on the safety and efficacy of the technology would be obtained, including through monitoring during the pregnancy and by follow-up of individuals born with edited genomes. Information on the outcomes would be integrated into the overall evidence base, and further deliberations would be needed to decide whether to undertake future clinical uses.
STUDY FOCUS AND APPROACH
The Commission’s full Statement of Task is provided in Box 1-3. The Commission is international in its mandate and composition, with membership spanning 10 nations and 4 continents and including experts in science, medicine, genetics, psychology, ethics, regulation, and law. The Commission’s deliberations included, among other activities, a public meeting held in August 2019, a request for public input to targeted questions gathered in September 2019, public webinars on genome editing technology held in October 2019, and a public workshop held in November 2019. At a third meeting in January 2020, Commission members developed the findings, conclusions, and recommendations presented in this report. See Appendix A for further information on how the Commission conducted its work and Appendix B for brief biographies of Commission members.
This report cannot serve as a checklist that encompasses the details of every experiment, method, or process that would need to be carried out
for genome editing to go from laboratory research to clinical use in human embryos. The science of genome editing is advancing so rapidly that new methods and data are reported weekly. The regulatory environments for both genome editing and ARTs vary widely across the globe, and whether HHGE would ever be permitted or how it would be overseen by a country remains to be determined. It is premature to establish specific “protocols” for many of the tasks identified in Box 1-3. Instead, the report describes the key elements that would need to form the foundation for a potential translational pathway for HHGE, lays out scientific and clinical issues that will need to be considered to undertake HHGE responsibly, and identifies preclinical and clinical requirements that would need to be met to establish safety and efficacy.
ORGANIZATION OF THE REPORT
This chapter introduces what the Commission means by a translational pathway toward possible future clinical uses of HHGE, should a country ever permit such use. The subsequent chapters of the report explore components of the pathway in greater detail. The report discusses the current state of the science and whether sufficiently safe and effective editing methodologies currently exist, along with circumstances associated with various types of proposed uses of HHGE. The report also specifies what preclinical evidence and clinical protocols would be required, and what associated oversight frameworks would be needed for any potential clinical use of HHGE.
Chapter 2 provides an overview of areas of science and technology involved in heritable genome editing. Sections address what is known about the genetics of human diseases, reproductive technologies (including in vitro fertilization and preimplantation genetic testing), and genome editing technologies and methodologies for characterizing their effects, and what is known about the possibilities of human genome editing in both embryos and gametes. It concludes by identifying key knowledge gaps that would need to be filled prior to considering any clinical use.
Chapter 3 classifies potential categories of uses for HHGE, each having distinct characteristics. It discusses scientific and clinical issues that would need to be considered in any assessment of the potential use of HHGE in these categories. Based on the current state of understanding, it concludes by identifying categories of potential uses for which the Commission felt it was possible to describe a responsible clinical translational pathway toward an initial human use of HHGE, should a country conclude that such applications are acceptable.
Chapter 4 describes the preclinical and clinical requirements that would need to be met as part of the potential translational pathway for the initial clinical use of HHGE described in this report.
Finally, Chapter 5 sets out recommendations on requirements for oversight frameworks in any country that is considering enabling the clinical use of HHGE. It also emphasizes the need for international coordination and makes recommendations for core components of such efforts. The establishment of oversight mechanisms and infrastructure to govern the use of HHGE is critical to any responsible translational pathway and for preventing misuse of the technology.