March 2019 was a good month for psychiatry, said Charles (Chuck) Zorumski, the Samuel B. Guze Professor, head of the Department of Psychiatry, and professor of neuroscience at the Washington University School of Medicine. The second drug that received FDA approval that month, after intranasal esketamine for treatment-resistant depression, was brexanolone (Zulresso™) for women with PPD. Brexanolone, a modulator of GABA, represents the first neuroactive steroid to be approved for a psychiatric indication, said Zorumski.
CLINICAL AND PATIENT EXPERIENCES WITH BREXANOLONE
Brexanolone is a novel formulation of the endogenous neuroactive steroid allopregnanolone, and has been approved by FDA as a breakthrough therapy for the treatment of PPD. Between 10 to 20 percent of women worldwide experience PPD after childbirth (Gerbasi et al., 2021). The condition is commonly characterized by depression, unstable mood, sadness, fear, and difficulty forming an emotional attachment with the baby (Vliegen et al., 2014). PPD is a major cause of maternal mortality and morbidity (Azhar and Din, 2021). Untreated, the condition can persist for months or longer. Without intervention, there may be lasting negative effects not only on mothers, but on their children as well, explained Samantha Meltzer-Brody. SSRI antidepressants have been considered the gold standard for treating PPD, but they are slow acting and ineffective for many women, she continued. Although the underlying cause of PPD is not fully understood, it is likely multifactorial—involving inflammatory signaling, fluctuations in perinatal hormones, dysregulation of stress pathways, and GABA signaling dysfunction, she continued.
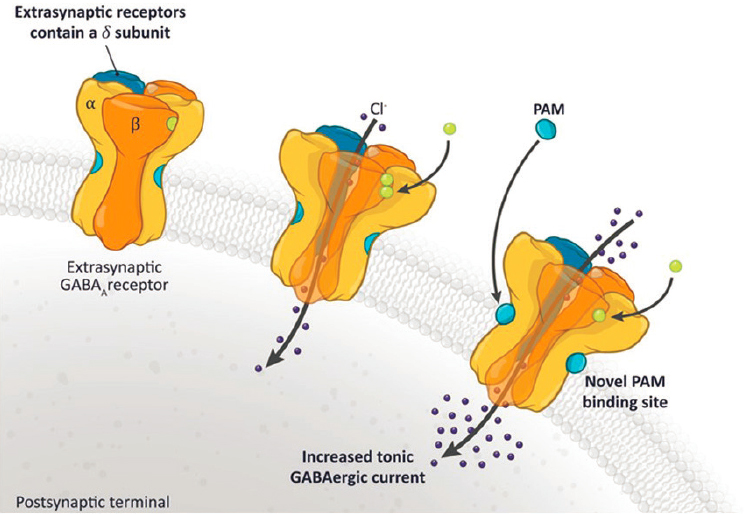
Brexanolone was already known to be a positive allosteric modulator1 (PAM) of GABAA receptors, said Meltzer-Brody (see Figure 4-1). There had been a long-standing theory that PPD was associated with GABAergic hypo-function, providing an underlying theory that made a strong case for why it was important to investigate the impact of brexanolone in PPD patients. In the initial open-label study of brexanolone (then called SAGE-547), in which both health care providers and patients were aware that the drug was being administered, Meltzer-Brody recalled the excitement of seeing the first patient exhibit a rapid and dramatic improvement in their PPD symptoms. Promising results with three more patients prompted SAGE to move forward with two double-blind Phase 3 studies, she said. These studies showed that a 60-hour intravenous infusion of the drug produced a
___________________
1 Positive allosteric modulators are drugs that bind to a secondary binding site on a receptor, causing a conformational change to the primary binding site, leading to enhanced binding affinity for ligands at the primary binding site (Abdel-Magid, 2015).
SOURCES: Presented by Jamie Maguire and Samantha Meltzer-Brody, March 8, 2021. © Sage Therapeutics, Inc., All Rights Reserved.
dramatic antidepressant effect at the 24-hour mark that was sustained for several weeks (Meltzer-Brody et al., 2018). Now using brexanolone clinically, Meltzer-Brody said, “it remains a very dramatic experience to watch people with this acute affective state change within a day. Women who were severely depressed suddenly have affective brightening and relief of horrible symptoms of depression and comorbid anxiety.”
An oral formulation called zuranolone is also in clinical development for both PPD and major depressive disorder, said Meltzer-Brody. This once-daily tablet does not work as fast as brexanolone, but still produces dramatic results, she said, with an onset of action observed after around 2 days and the full effect seen after about 1 week.
Meltzer-Brody and others are optimistic that brexanolone may provide relief for patients experiencing symptoms from other psychiatric illnesses as well. Moreover, she called brexanolone a “great example of using underlying hypotheses of pathophysiology to develop novel treatments.” Although
brexanolone has not been studied for mood disorders outside of PPD yet, she suggested that it provides an important opportunity to probe circuits and get a better understanding of what is happening. “I think there’s a tremendous amount we have yet to learn about this really dramatically powerful drug,” she said. “It’s untapped right now.”
BREXANOLONE’S MECHANISM OF ACTION
Brexanolone is a novel formulation of the endogenous neuroactive steroid allopregnanolone, and is the first neuroactive steroid to be approved for a psychiatric indication, said Zorumski. Neurosteroids describe a class of steroids that are synthesized in the brain and nervous system from cholesterol or steroid precursors and act on the brain, he said. Neuroactive steroids like brexanolone are potent, highly effective, and broad-spectrum PAMs of GABAA receptors, and can modulate both phasic inhibition and tonic inhibition, said Zorumski. Working at low concentrations in the nanomolar range to modulate GABAA receptor function, these agents are among the most effective PAMs that exist for GABAA receptors. He added that these agents also engage intracellular molecular targets that may be important considerations for understanding the mechanism of action, including effects on inflammation and receptor trafficking.
Working with Istvan Mody at the University of California, Los Angeles, in 2008, Jamie Maguire, the Kenneth and JoAnn G. Wellner Professor of Neuroscience at the Tufts University School of Medicine, discovered that mice lacking neurosteroid-sensitive GABA receptors exhibit abnormal maternal behaviors as well as behavioral deficits in the postpartum period, with pups suffering increased mortality due to cannibalism or neglect (Maguire and Mody, 2008). Maguire’s research further showed that a selective agonist of the delta subunit of GABAA receptors improved maternal behaviors and increased pup survival.
Therefore, Maguire proposed that high levels of neurosteroids during pregnancy are associated with a homeostatic downregulation of GABAA receptors to maintain an ideal level of inhibition during the pregnancy. When these neurosteroids begin to dramatically decrease at the time of delivery, the GABAA receptors need to be recovered to maintain an ideal level of inhibition in the postpartum period, she said. Deficits in the ability to recover these receptors at the time of delivery may increase the mother’s vulnerability to PPD, she explained. She also proposed that potentiating GABAA receptors may be therapeutic for the treatment of PPD. More recently, Maguire and colleagues showed that treatment of the GABA receptor knock-out mice with a compound from SAGE Therapeutics called SAGE-516 improved postpartum behavior and decreased pup mortality. Taken together, Maguire said, these preclinical studies laid the foundation
for the idea that GABA PAMs would be beneficial for the treatment of PPD in humans.
Harder to explain, said Maguire, is how the action of PAMs on GABA receptors results in the persistent antidepressant effect of brexanolone seen in women with PPD. University of North Carolina School of Medicine Scientist David Rubinow proposed that allopregnanolone may mediate effective switching between neural network states, Maguire continued. Inspired by this idea, Maguire and colleagues proposed that these neurosteroids may help potentiate a high level of tonic inhibition that synchronizes the neural network and mediates a transition to a more stable and a healthier network state (Pavlov et al., 2014).
Shifting their focus to the basal lateral amygdala, an area of the brain involved in emotional processing, Maguire’s team demonstrated a critical role for parvalbumin (PV) interneurons2 in mediating shifts between behavioral states related to fear; they showed that these interneurons express a high level of neurosteroid-sensitive GABA receptors (Antonoudiou et al., 2021). Further studies of the action of neurosteroids on PV interneurons confirmed that allopregnanolone and its synthetic analogs, such as SAGE-516, modulate behavioral states and neural network activity in the basal lateral amygdala via the delta subunit of the GABAA receptor on PV interneurons, said Maguire. In animals exposed to chronic stress, SAGE-516 had a profound effect on reversing anhedonia and other behaviors indicative of learned helplessness, she said. Her lab is now trying to harness the capability of endogenous neurosteroid synthesis to ensure the production and delivery of allopregnanolone at the intended site of action as a possible strategy to prevent some of the adverse side effects associated with exogenous neuroactive steroid treatment. Maguire added that there are likely multiple ways to disrupt this network, which may underlie the heterogeneity of symptoms observed in major depression or PPD.
CONVERGENCE OF MECHANISMS: KETAMINE AND BREXANOLONE
Different agents, including ketamine and brexanolone, may mediate their antidepressant effects by converging on the same molecular targets, Lisa Monteggia, the Barlow Family Director of the Vanderbilt Brain Institute and professor of pharmacology, psychiatry, and psychology at Vanderbilt University. One indicator of convergence, she said, is that both drugs can trigger antidepressant effects for up to 1 week. Because this time course supersedes the time it takes the drugs to clear the central nervous system
___________________
2 PV interneurons are a subset of GABAergic interneurons that help regulate excitation and inhibition in brain circuits to drive behaviors (Ferguson and Gao, 2018).
and is not due to persistent blocking of NMDA or neurosteroid receptors, Monteggia suggested that some type of plasticity is engaged. Similar molecular mechanisms may also underlie the downstream effects of blocking NMDA and GABAA receptors, said Monteggia. To understand this possible convergence, she suggested mapping out the neurocircuitry of antidepressant effects at a molecular level, adding that this could also help to identify new targets for pharmacological intervention. For example, if brexanolone and ketamine trigger antidepressant effects by engaging different receptors, but with convergence occurring downstream either molecularly or synaptically, a more nuanced but systematic approach may be needed to probe these pathways further, she said.
Maguire said she has also been intrigued by the potential convergence between the mechanisms of ketamine and GABA PAMs and how changes in neural network states relate to the therapeutic effects of these compounds and their impact on behavior. She noted that modulation of both NMDA and GABA receptors may influence neural network function and could have similar effects on plasticity, adding that just as there are numerous ways to disrupt the neural network, there may also be multiple ways to restore a healthy neural network state. Indeed, György Buzsáki, the Biggs Professor of Neuroscience at New York University, said nearly every psychiatric condition can be characterized by a change in the constellation of neural network effects, and virtually every drug used in psychiatry affects the balance of inhibition and excitation. He added that tonic suppression of spiking may not equally affect neurodynamics in every brain state and that finding brain region-specific effects could be very useful for therapy.
John Murray, assistant professor of psychiatry, neuroscience, and physics at Yale, added that by looking at cell-specific gene expression using single-neuron RNA seq data, it may be possible to identify the pathways involved at the cellular and microcircuit levels, which could help illuminate the paradoxical effects of central nervous system drugs on inhibitory neurons in certain brain structures.
Walter Koroshetz, director of the National Institute of Neurological Disorders and Stroke, noted that ECT produces a sustained reduction in depressive symptoms similar to what is seen with brexanolone and ketamine, suggesting there are circuit changes that respond to the types of short-term neural circuit manipulations that ECT causes. Maguire agreed that this represents another point of convergence. If ECT is resetting the network in a similar way to ketamine and GABA PAMS, investigating these commonalities might lead researchers in the direction of more targeted treatments, she said.






