 |
Proceedings of a Workshop—in Brief |
Brain-Machine and Related Neural Interface Technologies: Scientific, Technical, Ethical, and Regulatory Issues
Proceedings of a Workshop—in Brief
INTRODUCTION
On September 22 and 23, 2022, an ad hoc planning committee under the auspices of the National Academies of Sciences, Engineering, and Medicine’s Committee on Science, Technology, and Law (CSTL) hosted a virtual workshop, Brain-Machine and Related Neural Interface Technologies: Scientific, Technical, Ethical, and Regulatory Issues. Brain-machine and related neural interface technologies (BMIs)1 refer to a range of devices2 that “read” the brain or other neural tissue by capturing electrical signals and decoding their meaning and those that “write” to the brain or other neural tissue by providing electrical stimulation to affect their function. In addition to exploring what these technologies offer now, what is not possible with these technologies, and what may be possible with these technologies in the future, the workshop considered the implications of these technologies for user autonomy, data privacy, and equity and access, while touching briefly on potential gaps in U.S. regulatory oversight.3 A key goal of the workshop was to understand the scientific, ethical, legal, and social questions that the technologies raise for researchers, funding agencies, regulators, patients, and the public.
CSTL Co-chair David S. Tatel (U.S. Court of Appeals for the District of Columbia Circuit) welcomed workshop participants and noted that that BMIs raise important issues that are increasingly urgent as our understanding of the brain advances, as new technologies are developed, and particularly as devices move from research settings into clinical and consumer contexts. He emphasized that, when considering emerging technologies like BMIs, it is important to remain cognizant of ethical, legal, and societal issues that they raise.
In introducing the workshop, planning committee co-chair Nita Farahany (Duke University School of Law) emphasized that a shared understanding of the facts surrounding BMIs is necessary to evaluate the ethical, legal, and societal implications of these technologies. Importantly, the facts relate not only scientific and technical aspects, but to the lived experience of users of
__________________
1 For these proceedings, BMI is used as shorthand for brain-machine and related neural interface technologies unless otherwise noted.
2 BMI devices can be implanted in the body or placed externally. The latter category of devices is often referred to as “wearable” devices. All BMI devices rely, in some capacity, on computers to perform their functions and are sometimes referred to as brain-computer interfaces (BCIs).
3 International frameworks for the oversight of these technologies, while important, did not form a significant part of workshop discussions.
BMIs, the regulatory environment, and public perceptions about BMIs as shaped by the media. It will be essential, she emphasized, to understand what is and is not possible with these devices now and into the future.
Planning committee co-chair John Donoghue (Brown University) spoke about the promise of BMI technologies, including devices that are implanted in the body and those that are wearable. He said that BMIs raise a number of challenges and opportunities as they move from research settings to the clinic, are made available via a complex healthcare system, and ultimately reach the users who need them. Donoghue emphasized that a diverse set of perspectives is needed to explore the numerous issues that BMIs raise, including those of scientists and engineers, clinicians, industry representatives, users of the technologies, government regulators, and legal scholars. In planning the workshop, he said, the members of the planning committee took great care to ensure that these diverse perspectives were represented.
THE STATE AND LIMITATIONS OF THE TECHNOLOGY
Donoghue moderated the workshop’s first session. The purpose of the session, he said, was to identify and consider the range of BMI technologies available today and into the near future that will enable us to read the brain by capturing a record of its activity and to write to the brain by stimulating changes in function.
Cindy Chestek (University of Michigan) spoke about the potential (and limitations) of devices implanted to restore function in patients with spinal cord injuries. She said that implanted electrodes have been able to restore function by, for example, allowing affected individuals to use a fork. She noted, however, that these devices are far from able to confer full, able-bodied control. There are likely to be advances in the near future that will allow stimulation or recording of a larger number of neurons, and while this will increase the capabilities of these devices, advances will be incremental. The stimulation or recording capabilities provided by an implanted device will continue to be slight compared to signals naturally present in the brain because the number of neurons a BMI can effectively reach is very small. Chestek listed as key limitations the challenges of maintaining electronics implanted in the body; issues related to powering implanted devices; and challenges in attaining the high data bandwidth necessary to comprehensively read the brain’s electrical signals. She suggested that, in the future, BMIs will not make people smarter: in 1,000 years, she predicted, people will still be using their natural eyes, but devices will be available to help the blind see.
Tim Denison (Oxford University) provided an industry perspective on BMIs, highlighting the tremendous economic burden from neurological diseases by presenting a figure that illustrates the cost of disorders of the brain in Europe in 2010 (see Figure 1). He said that implanted devices to treat Parkinson’s Disease have been available for decades and that recent work has focused on decreasing the side effects they cause. Advances include: (1) the development of directional electrical leads to decrease off-target stimulation (which can produce side effects); (2) stimulation that adapts in response to brain signals (i.e., closed loop systems); and (3) miniaturized systems. External systems have also been developed that employ transcranial magnetic stimulation (TMS)4 and other forms of stimulation to successfully treat depression and other disorders. Denison reported that Dr. Linda Carpenter (Carney Institute for Brain Science, Brown University) estimates that, in the United States, 20 million TMS treatments for depression have been provided between 2008 and 2022. He emphasized that BMIs must not only show clinical necessity, scientific validity, and technological maturity, but contend with challenges related to economic viability, the burden placed on clinicians and patients, and regulatory constraints in the United States and abroad. Denison said that ethical considerations relating to the necessity of providing long-term support for patients even if device manufacturers no longer make or service devices, data security, and issues of equity and access deserve important consideration by the community of individuals developing these technologies.
__________________
4 Transcranial magnetic stimulation is a form of brain stimulation in which a changing magnetic field is used to induce an electric current at a specific area of the brain to stimulate neurons at that site.
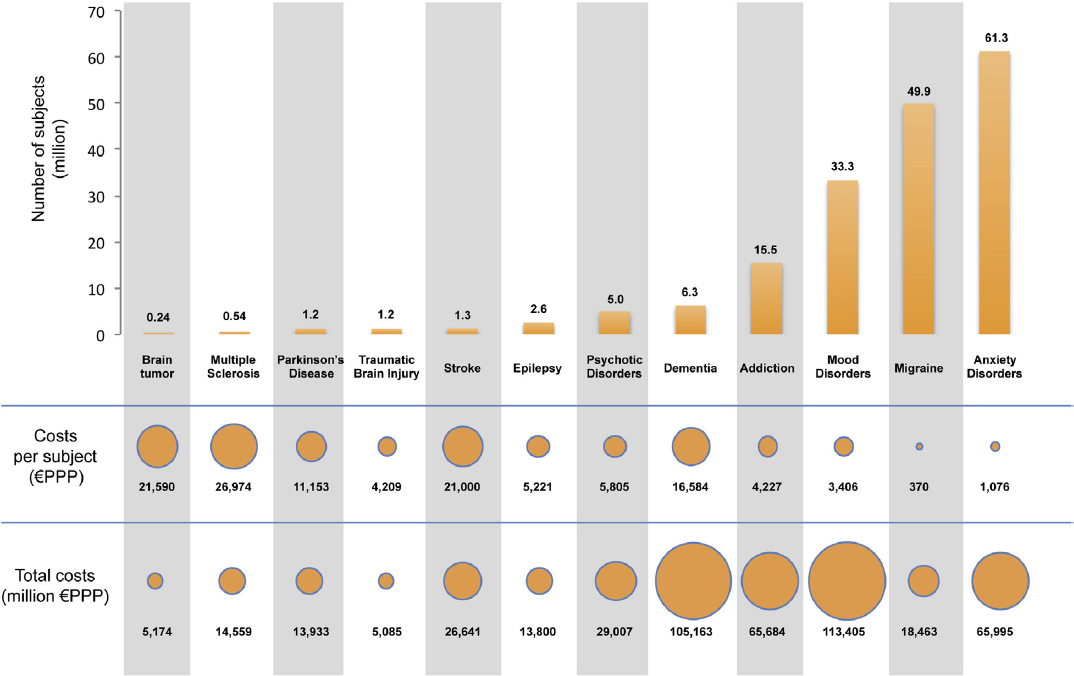
SOURCE: Reprinted from Monica DiLuca and Jes Olesen, “The Cost of Brain Diseases: A Burden or a Challenge?” Neuron, Vol. 82, p. 4, Copyright 2014, with permission from Elsevier.
Ana Maiques (Neuroelectrics) discussed a product that her company developed for the treatment of epilepsy and sleep disorders. This device, a wearable cap with integrated electrodes, collects wireless electroencephalogram (EEG) readings of brain activity and can stimulate the brain using targeted current to lower seizure occurrence. In a pilot clinical trial, epilepsy patients experienced a 47 percent decrease in seizure activity when using the cap. This “sense and stimulate” system could also be used to treat depression, and Maiques’ company hopes to start a clinical trial for that application soon. Maiques said that home use of the cap would be preferable for certain indications, but that at-home use without direct oversight by researchers or clinicians raises concerns about appropriate means of commercialization, data security, and guarding against misuse. She noted that her device was granted “breakthrough” designation by the U.S. Food and Drug Administration (FDA) for treatment of epilepsy, but that the Centers for Medicare and Medicaid Services (CMS) no longer covers devices with this designation. This, she said, is a significant issue that will limit the use of neuroelectric devices. She said that neurotechnology raises ethical issues related to patient autonomy, equity and access, responsibility for unintended effects, data privacy, and the possibility of device “hacking.”
Krishnan Thyagarajan (Palo Alto Research Center) discussed advances in BMIs as part of a temporal continuum, noting that major advances in human efficiency and productivity inevitably have unintended ramifications that must be managed. In comparing different types of BMIs, he identified challenges related to spatial resolution (how well a device discriminates signals that are spatially close to each other), temporal resolution (how well a device discriminates signals that are temporally close to each other), bandwidth (how much information can be retrieved from the device), latency (how well the device provides stimulation on an appropriate timescale for the brain), and corporeal tolerance for such devices. Often, he said, there are trade-offs: wearable devices may be better tolerated by the body, but because they are external to the body, they have low spatial and temporal resolution as compared
to implanted devices. Thyagarajan urged caution, particularly for companies, when developing devices: “It’s important to build trust, especially when a for-profit company ends up making a device that can tap into the brain. Trust takes time to build, which is slightly antagonistic to the rapidity with which often we desire to reach the market.” “We shouldn’t,” he said, “necessarily be accelerating things at the risk of jeopardizing future opportunities.”
Sebastián Alvarado (City University of New York) drew on his experience both as a professor of biology and a consultant for science fiction movies to identify key questions raised by BMIs, particularly those used to enhance or augment the brain. He posited four questions: (1) Who owns the data generated by these technologies and how will they use it?; (2) How will these devices affect our humanity, particularly in light of the fact that enhanced or augmented humans may be seen as less human?; (3) Will advances in BMI technology hurt society more than they help, especially given the potential for these technologies to be abused, misused, or used to increase disparities?; and (4) How can we ensure the security of these devices and the data they collect? Alvarado warned that we are likely to see many neurotechnology failures, stating that “there are those in industry that think the brain is a tissue that can be hacked like an electric car.” He suggested that, as the brain is biologically complex with multiple cell types and molecular processes, it cannot be reduced to a simple set of electrical impulses. He urged caution, saying that there are many “known unknowns” about the biology of the brain. BMIs, he said, will not be able to interpret or modulate many brain signals, but they will interact with them in unpredictable ways.
DISCUSSION
Donoghue led a wide-ranging discussion with panelists and planning committee members. One thread explored the limitations of the models of the human brain that are used to design BMIs and predict how stimulation will affect the brain. Maiques referenced the Neurotwin project at Neuroelectrics, which aims to produce individualized models of each patient’s brain to predict responses to stimulation but said that the models are not yet good enough to provide a meaningful simulation. Alvarado described previous, unsuccessful efforts to model the whole brain and mentioned that brains include biochemical functions that may not be captured in electrophysiology-based mapping. Chestek suggested that we might eventually understand the physics of electrical interactions with the brain to a degree where useful brain models could be developed.
A separate discussion thread considered BMIs’ capacity to affect a user’s sense of autonomy. Denison mentioned the NeuroVista trial where patients reported very different feelings about their implanted devices following long-term recording of brain activity, with one participant considering it a part of themselves and another thinking of it as a foreign body.5 Maiques noted that there are no requirements6 from FDA or elsewhere to collect this type of subjective information from patients (even though it may be important to patient autonomy and feelings of self). No one, she said, tracks situations where a patient’s loved one might say, “You’re acting weird, turn off the machine!” Planning committee member Gina Poe (University of California, Los Angeles) asked if a patient would be responsible if they committed a crime while using a BMI. Farahany said that there are analogous legal cases where defendants claimed that a brain condition impacted their behavior but said that such defenses are typically discounted by the courts.
Chestek and Maiques noted that approvals of implanted devices require extensive engagement with FDA. Wearable devices (like the Neuroelectrics platform) usually require less, though still rigorous,
__________________
5 See Christine Kennedy, “Do Brain Implants Change Your Identity?,” New Yorker, April 19,2021, available at: https://www.newyorker.com/magazine/2021/04/26/do-brain-implants-change-your-identity. See also the original trial results in Mark J. Cook et al., “Prediction of seizure likelihood with a long-term, implanted seizure advisory system in patients with drug-resistant epilepsy: a first-in-man study,” The Lancet Neurology. Vol. 12, Issue 6, p. 563–571, June 1, 2013, available at https://www.thelancet.com/journals/laneur/article/PIIS1474-4422(13)70075-9/fulltext.
6 FDA regulation of implanted BMIs focuses on whether they are safe for the patient and effective for a particular use. FDA regulates wearable BMIs if the developers claim that their device has a medical benefit. For wearable devices without a medical claim, there is no pre-market authority that requires tests for safety or effectiveness. However, if a device is found to be unsafe, consumer protection laws enforced by the Federal Trade Commission or the Consumer Products Safety Commission can be invoked to remove the product from the market or otherwise address the harm.
interaction. Denison observed that there are many potential opportunities for early intervention in disease progression in young patients but stated that BMI use by children should be given special consideration, including with regard to practical issues such as electrode cap design to ensure proper fit for children and longer-term support to maintain device function.
Discussants identified several practical issues that bear on how widely used wearable BMIs become, including that scalp electrodes require gel to transmit current and the difficulty in attaching electrodes over kinky hair, which may raise questions related to equity and access.
READING AND WRITING THE BRAIN FOR MOVEMENT
Session moderator Veljko Dubljević (North Carolina State University) introduced the workshop’s second panel by considering how BMIs designed to assist with movement have been depicted in science fiction, including as exoskeletons designed to enhance capabilities, in military applications, and as robots merged with humans. He emphasized the importance of separating science fact from science fiction.
The session’s first panelist, Vivian Mushahwar (University of Alberta), described work on the stimulation of spinal cord neurons to restore walking ability after spinal cord injury. Mushahwar’s lab used functional mapping to identify the parts of the spinal cord responsible for walking behavior in multiple species and individual animals. By implanting electrodes in cats that penetrate the spinal cord and provide micro-stimulation, researchers were able to restore walking function that is predictable, coordinated, weight-bearing, propulsive, and fatigue-resistant. Mushahwar’s lab is working on adapting these implantables for use in larger animals, such as pigs, and on reducing barriers to their use in humans.
Douglas Weber (Carnegie Mellon University) discussed advances in the stimulation of the spinal cord for neuromotor rehabilitation in stroke patients. While strokes occur in the brain, spinal cord stimulation can be used to restore motor function lost due to stroke. Weber described a pilot, three-patient clinical trial where implants were inserted for a short term (30 days) to provide epidural stimulation (i.e., stimulation of the surface of the spinal cord) in the neck region of the spine. In one patient, stimulation of the spinal cord improved function that was measurable via multiple tests of strength and dexterity in the affected arm. Weber said that this type of stimulation, when combined with activity-based rehabilitation, could help restore strength, dexterity, or coordination for stroke patients. As ethical priorities, he emphasized safety and equity and access to the benefits of the technology.
Jennifer L. Collinger (University of Pittsburgh) spoke about implanted BMIs that record signals from the brain’s motor cortex7 and decode the information to allow human research subjects to control a robotic hand or a computer cursor. A sensor on the robotic hand has been able to provide tactile feedback to the brain via stimulation of the sensory cortex.8 Collinger said that researchers can reliably record neural activity over multiple years to enable user control for functional tasks, including reaching and grasping with a robotic arm. Devices with sensors that drive brain stimulation have been used to provide meaningful tactile sensations that increase a user’s performance on tasks such as grasping. Although these tasks are usually conducted in labs with oversight from researchers, devices used to control computer cursors are being used in homes. Collinger listed as practical challenges the need for device longevity with less calibration and the need to improve hardware for bandwidth, portability, and reliability.
Geoffrey Ling (On Demand Pharmaceuticals, formerly of the Defense Advanced Research Projects Agency) enthusiastically called for a “moonshot” to radically advance the science of BMIs. He said that the original moonshot, the Apollo program that sent astronauts to the moon within a decade, “had a budget of 4.4 percent of the federal budget… an astronomical sum.” Ling said that we need to think big and ask questions such as “How do we get a moonshot for BMIs? How can we create something that would capture the imagination
__________________
7 The motor cortex is a region on the surface of the brain that plans and coordinates movement in the body.
8 The sensory cortex is a region on the surface of the brain that receives and interprets information related to sensory information, including from visual, auditory, tactile, olfactory, and gustatory inputs.
of the non-scientific population so that they would be willing to commit a high level of resources toward this?” He suggested that we consider the value proposition of BMIs, particularly vis-à-vis commercial and consumer products that might be used by a wide range of people. Beneficence and addressing conditions such as stroke and spinal cord injuries may not, he said, be enough to convince the public that BMIs are worth a substantial investment.
Justin Lowery (BrainGate Clinical Trial Participant) drew on his experience as a user of an implanted device that decodes signals from his brain to allow interaction with a computer. Lowery told the story of a rafting accident in 2008 in which he suffered a spinal cord injury that left him paralyzed and described how he and his family made the decision to participate in a BrainGate clinical trial.9 Lowery’s implanted device allows him to control a variety of programs on a computer including programs that allow him to type to communicate, create visual art, and write music. He seconded the idea of a BMI “moonshot” to expand opportunities for commercialization, to improve the capabilities of devices that enable people living with disabilities, and to bring them to more people.
Cristin Welle (University of Colorado School of Medicine) spoke of her previous experience as part of an FDA research team that worked on BMIs but focused on current work on the use of electrical stimulation of the vagus nerve10 to drive enhanced motor learning. Using implanted devices in mice, Welle’s lab has demonstrated that providing electrical stimulation to the vagus nerve in mice who successfully conduct a reaching movement reinforces the behavior, ultimately enabling the mouse to more quickly learn the movement. She also noted that, in humans, vagus stimulation during the conduct of motor rehabilitation tasks post-stroke triggers improved outcomes. Welle presented data from her lab that showed that vagus nerve stimulation in mice can help with recovery from injuries that demyelinate neurons.11 This suggests implications for the treatment of patients with diseases such as multiple sclerosis, which is characterized by a decrease in myelination.
DISCUSSION
Dubljević opened discussion with a question about the possibility of using BMIs to enhance function rather than to restore lost function. Collinger suggested that we are decades away from the ability to meaningfully enhance motor function. Mushahwar said that wearable devices (e.g., clothes as an exoskeleton that provides structural support or electrical stimulation when needed) may have some promise in the future. Welle said that there is a lot of interest in wearable devices to improve “wellness” (which can encapsulate enhancement). Ling suggested that wearable devices designed for non-medical uses or enhancement might be the key to capturing the public’s imagination and generate support for a BMI moonshot.
Poe asked a question about regulatory oversight of BMIs: What is stopping people from developing their own implanted devices? Welle said that wearable or other external devices marketed for wellness or for enhancement (and not medical purposes) are not subject to FDA approval and will “fly under the radar” unless a serious safety issue arises. She added that there is a “gray area” concerning how FDA’s authorities might apply to implantable devices absent any medical claims. Weber suggested that issues are likely to arise in this space in the near future, noting that it is currently possible to buy unregulated transcranial stimulation (TCS) devices or EEG readers that connect to smartphones and that biohackers have already implanted other types of technologies without FDA oversight (e.g., radio-frequency identification [RFID] chips implanted in their hands).
Donoghue and workshop planning committee member Helen Mayberg (Icahn School of Medicine at Mount Sinai) cautioned that terms like “non-invasive” are often used to imply that a wearable device is “safe” or “reversible,” but said that it is important to emphasize
__________________
9 BrainGate is a research effort that develops implantable BMIs to restore the communication, mobility, and independence of people with neurologic disease, injury, or limb loss.
10 The vagus nerve is the main nerve of the parasympathetic nervous system, which controls involuntary body functions such as digestion, heart rate, and immune system. It is the longest cranial nerve, passing from the brain through the neck to the abdomen.
11 “Myelination is the process by which brain oligodendrocytes produce layers of myelin that wrap around the neuronal axons and act as a layer of insulation for the transmission of electric action potentials down the neuronal axon.” See https://www.sciencedirect.com/topics/medicine-and-dentistry/myelination#:~:text=Myelination%20is%20the%20process%20by,potentials%20down%20the%20neuronal%20axon.
that even wearable and other external devices that stimulate the brain can carry risks—and that long-term risks might be hard to determine.
In response to a question about the longevity of BMIs, Weber said that some implanted devices are currently approved for long-term use and that these could be designed to be updated wirelessly. Currently, implanted deep brain stimulation (DBS)12 systems require a minor surgery every 3–5 years to replace batteries. Mushahwar noted that it is unclear whether spinal cord implants can be safely removed and replaced, but she believes that a 10–15-year timeframe (the amount of time that an artificial hip is expected to last) might be a “meaningful benchmark” of longevity. Collinger said that the field is new, so we don’t yet know what the limits might be for how long these devices can last and what factors might be most important.
Audience questions emphasized the need to communicate the risks of BMIs and the need to develop appropriate measures of benefits. Mushahwar highlighted the importance of transparency about the process, potential risks, and potential benefits in the consent process as overseen by Institutional Review Boards (IRBs) and by FDA. Lowery said that, as part of the consent process for his device, the research team carefully described the associated risks, but to him, the risks of brain surgery were apparent: “If somebody’s digging into your skull, then there’s the potential for something [bad] happening.” With regard to measuring benefits, Collinger said that it is hard to establish standards for demonstrating meaningful improvements in function or independence. Lowery suggested that patient statements about how a device has improved their life is a measure of benefit.
READING AND WRITING THE BRAIN FOR MOOD AND AFFECT
Session moderator Marcello Ienca (Swiss Federal Institute of Technology in Lausanne [EPFL]) said that mood disorders are estimated to affect hundreds of millions of people around the world annually and that new treatments are needed. He identified ethical and societal issues that devices designed to treat mood disorders may raise, including equitable access to their benefits, manufacturer obligations (e.g., to ensure the capacity for long-term maintenance of devices), ensuring the privacy of highly sensitive data collected from the brain, and issues related to changing neuronal activity or writing to the brain.
Andrew Krystal (University of California, San Francisco) presented his lab’s patient-specific approach to treating depression with implanted, closed-loop devices. These devices read signals from the brain and provide stimulation based on an interpretation of those signals. In three patients, 10 electrodes were implanted in different places in the brain to map where stimulation might be most effective at improving mood for each patient. Based upon changes in brain activity, a device was then implanted to stimulate the brain when it detects a specific pattern of activity that might indicate a “state of depression.” Krystal said that the mapping process was long and challenging due, for example, to the difficulty of identifying biomarkers that provide indices of when stimulation is needed and the need for patients to constantly report their mood during mapping.
Talma Hendler (Tel Aviv University) spoke about wearable, closed-loop self-neuromodulation for improved mental health. She said that neurofeedback can be used to teach the brain to change. By conducting EEG and functional magnetic resonance imaging (fMRI)13 at the same time, Hendler’s group has been able to develop a “smarter” EEG model that can detect patterns of activity in different regions of the brain specific to different conditions. Hendler described experiments in which soldiers used EEG caps to treat mood disorders. In the experiments, each soldier was provided feedback about the level of activity in their amygdala, a region of the brain that processes fear and emotions. Through a neuromodulation feedback process, the research subjects were able to learn to decrease amygdala activity. Although these experiments were conducted with healthy subjects, this outcome has implications for the treatment of post-traumatic stress disorder, which is often characterized by hyperactivity in the amygdala.
__________________
Daniel Chao (Neurotechnology Entrepreneur) described several different approaches to treating mood disorders with BMIs. He said that DBS has been used for decades and has been determined by FDA to be safe and effective, particularly for treating movement disorders such as Parkinson’s Disease. He noted, however, that improvements in equipment, including in electrical stimulators, have been incremental. TMS has also been approved by FDA and has many applications, including as treatment for migraines, smoking cessation, and anxiety. Chao noted that TMS takes time to be effective and that treatment must take place at a clinical site. Transcranial direct current stimulation (tDCS) and transcranial alternating current stimulation (tACS)14 are being developed for use in wearable devices, but these methods are limited to stimulating structures close to the brain’s surface. Chao suggested that “there’s an opportunity [with tDCS], because the equipment is so simple […, that trials could] be potentially run at home.” He asked whether FDA could provide guidance on how such home trials should be conducted.
Brandy Ellis (Neuromodulation Patient Advocate) provided her perspective as a patient with a brain implant for treatment-resistant depression. She described her experience with debilitating depression that did not respond to traditional treatments (e.g., psychotherapy, medication, and electroconvulsive therapy). She said that most clinical trials on treatments for depression are first-line treatments (i.e., those that treat depression when it first arises) and that there are few options for those with treatment-resistant disease. In 2011, she joined a clinical trial for treatment-resistant depression at Emory University School of Medicine and had a device implanted to deliver DBS. Following her surgery, Ellis saw improvement after 6 months, was in remission after two years, and is now a fully engaged member of society. She emphasized that the implant does not make her happy all the time but gives her what she called an “appropriate” mood: “This device didn’t change me, it just restored me to me.” Ellis said that her life will be at risk if she loses access to the device, noting that, at one point, the battery for the device became fully discharged and she began to get sick. Ellis expressed concerns about what would happen if the manufacturer of her device went out of business or is no longer able to maintain the implant.15 She highlighted the need for a robust consent process for trials; strong protections for privacy and anonymity (a challenge in research cohorts because there are very few patients with devices); and devices that are secured against hacking.
Vivek Pinto (U.S. Food and Drug Administration) described the organizational structure of FDA and said that oversight of BMIs is conducted by the Office of Neurological and Physical Medicine Devices within the Center for Devices and Radiological Health. He noted that FDA takes a risk-based approach to regulation: as potential risk increases, so does the level of regulatory oversight. Pinto described key elements for submissions for FDA device approval, noting the importance in the regulatory process of a sponsor who works with a lead FDA reviewer who can, in turn, loop in expertise within the agency. FDA can also call on expertise from other government agencies or establish an external advisory panel when needed. Pinto emphasized that device sponsors should contact FDA as early as possible in the development of a new technology to best understand the regulatory process and establish lines of communication. In evaluating devices, he said, FDA looks at the “totality of evidence” that is provided by the sponsor and weighs probable benefits against probable risks. He said that FDA is considering how to best incorporate patient preferences into its decision making, but that it is been difficult to assess how much risk patients are willing to accept.
DISCUSSION
Ienca opened discussion with a question from Poe about the possibility of using a BMI to control or to sap motivation from adversaries during war or conflict. Dubljević noted that a wearable device that uses, for example, tDCS could be hacked to potentially harmful effect. Krystal said that Ellis’s experience and the
__________________
14 Transcranial direct current stimulation is a technique that uses direct, constant electrical currents from a wearable device to stimulate the outside of the brain. Transcranial alternating current stimulation is similar, but instead uses currents that alternate at some frequency.
15 In the discussion session for this panel, Ellis said that, initially, she had a surgery about once a year to replace the battery in her device, but that she now has a rechargeable battery that requires recharging for about 90 minutes every 3 days. She noted that, while this is inconvenient and bothers some patients, for her, the recharging process is preferable to having surgery every year.
experience of patients in his study suggest that implanted devices designed to treat depression do not control people but can restore them to an appropriate mood.
A question about stigma associated with depression and mood disorders stimulated robust discussion. Ellis said that stigma is a serious issue, and she speaks publicly because she knows others can’t. Krystal observed that several patients who were successfully treated for depression said their experience that brain stimulation could lead to immediate improvement in their symptoms led them to conclude that their illness was not their “fault.” Thyagarajan said that heart pacemakers carry virtually no stigma and wondered how anonymization of device users might influence stigma. Mayberg said that a key challenge in keeping device users anonymous is the necessity for medical professionals to know if a patient has a device to prevent against inadvertent harm.16 Chao said that wearable devices could conceivably become more widely used than implanted devices and allow patients to get treatment at home rather than going to a clinic. This, in turn, could increase the use and acceptance of BMIs.
Mayberg raised the issue of personalization of BMIs, observing that it may not be necessary to determine ideal placement of implanted devices or stimulation patterns for each patient. Patients, she said, can learn to use a device effectively even if it is not specifically optimized to the individual. Hendler agreed, noting that individuals may have different symptoms and patterns of brain activity and that the human brain has an enormous capacity for change. Krystal said that mapping the regions of the brain where stimulation is most effective for patients with different symptoms should improve the effectiveness of these devices for all—as this mapping will provide general information regarding placement of stimulators.
READING AND WRITING THE BRAIN FOR THOUGHT, COMMUNICATION, AND MEMORY
Before introducing the panelists of the workshop’s final session, session moderator Farahany drew attention to the idea of “reading” the brain. She suggested that reading the brain for thought, communication, and memory might be “the most over-hyped but also the most incredibly promising area of BMI technology in the near-term.”
Michael Kahana (University of Pennsylvania), the session’s first panelist, spoke about using closed-loop BMIs to improve memory. Using intracranial recordings from electrodes on the surface of the brain, his research team has been able to identify brain states that predict successful recall during a word-based memory task. He reported that stimulation of the brain’s lateral temporal cortex17 increased successful recall when patients were experiencing a memory lapse. Kahana said that it is imperative to develop and advance BMI technologies to reduce the burden of disease. He said that technologies are getting better at interpreting electrical signals from the brain to decode the contents of the memory. When monitoring the performance of word-based tasks, researchers were often able to predict, for example, the category of word that a subject later recalled based on the brain’s pattern of activity. Kahana suggested that BMIs could potentially bias memory in this type of task toward certain categories of words.
Rajesh P. N. Rao (University of Washington, Seattle) discussed the possibilities of incorporating artificial intelligence (AI) into BMI technologies. He discussed AI as a “brain co-processor” that could take input from the brain and other sources (e.g., sensors, cameras, or even the internet) and send information or stimulation back into a brain or to an actuator to control, for example, a robotic arm. Rao described work where an individual wearing an EEG cap imagined moving their hand, and the signal recorded by the EEG was transmitted via TMS into the brain of a second individual whose brain decoded the information and moved their hand. This type of brain co-processing can be extended to multiple individuals who can provide inputs (e.g., by generating brain signals that are recorded by an EEG) or integrate signals received (e.g., through TMS) and decide how to respond. Rao said that the use of AI in such systems could lead to
__________________
16 For example, emergency room personnel may want to conduct magnetic resonance imaging (MRI) but performing an MRI on a patient with an implanted device would harm the patient.
17 The lateral temporal cortex is a region on the surface of the brain that is important for encoding memory and for language comprehension.
co-adaptation of the brain with the AI, noting that such integrations could raise questions related to liability and personal responsibility.
Leigh Hochberg (Massachusetts General Hospital, Brown University, and VA Providence Healthcare System) spoke about the use of BMIs to restore the ability to communicate. Developments in this space have the potential to assist a wide range of patients, he said. Hochberg described current and near-future capabilities, including enabling text-based, “point- and-click” interaction (he noted that up to 150 correct characters per minute will be possible), decoding intended handwriting (currently >90 correct characters per minute), understanding intended speech (today the vocabulary is about 50 words, but a full vocabulary may soon be possible), and restoring the ability to create art and music. Hochberg believes that it will not be possible for BMIs to decode “unconstrained thought”18 in the foreseeable future but noted that data currently collected includes very private information (e.g., communications intended for close family members) and, as such, raises important privacy concerns. He suggested that collected data should belong to the user alone and emphasized that, particularly for small-n trials, collected data may not be fully de-identifiable. Hochberg raised several additional ethical issues, including the question of who decides when a communication device is turned on, considerations related to the appropriate oversight of human subjects research, culpability when a device malfunctions, and issues related to access, societal expectations and culture, and personhood.
Andreas Forsland (Cognixion) described Cognixion ONE, a “brain computer interface with [an] augmented reality, wearable speech generating device” designed to assist individuals with an impediment to verbal communication. The device presents information holographically in the user’s visual field and collects input from the brain using an EEG system. The user learns to use the EEG system to interact with menus and keyboards that allow them to select communication outputs. The company is currently working to improve their platform by: integrating a wider range of software; partnering with Amazon and their Alexa device to provide easier access to information; making the device more comfortable; reducing its susceptibility to background visual noise; improving its ability to better understand utterances; and making accommodation for a wider range of physical movements during use. Forsland emphasized the importance of incorporating multimodal inputs to better meet users’ needs (e.g., by using eye trackers or haptic interactions that depend on touch or movement to better understand their intentions).
Paul Larkin (ALS Association) provided perspective from the ALS Association, which advocates on behalf of patients with Amyotrophic Lateral Sclerosis (ALS), a fatal neurodegenerative disease that progressively destroys speech and motor function. He presented data from the ALS Focus Survey Program, which collects information from ALS patients and caregivers, to illustrate that communication difficulties are common and impactful for those with ALS. Larkin spoke about the limitations of BMIs, emphasizing the need for conversational speed, safety, and practicality (such devices need, for example, to be wireless, comfortable, and easy to use). Larkin also mentioned that users want devices to be customizable (e.g., to have the ability to mimic their own voices), compatible with devices like phones, and easy for caregivers to use. Larkin expressed concerns about access to the technology, how devices will be paid for, and fears that technologies will become obsolete or unsupported in the future.
In his remarks, the session’s final speaker, Carlos Peña (The Jacobs Institute), drew upon his experience at the non-profit Jacobs Institute and his previous role as Director of the Office of Neurological and Physical Medicine Devices at the Center for Devices and Radiological Health at FDA to provide a multi-stakeholder perspective. He emphasized that there are many stakeholders in the BMI ecosystem that are united in their focus on the user or patient, including individuals from academia, industry, government, innovation centers, and non-governmental organizations. FDA regulatory oversight of these technologies is based on the technology, the data (particularly from
__________________
18 The phrase “unconstrained thought” is not well defined, and the concept is discussed in more detail during the Discussion session.
clinical investigations that are focused on validated end points), safety, and efficacy claims made by the product’s developer. Peña acknowledged that there were perceived areas where there is uncertainty about regulatory oversight,19 adding, “There needs to be more discussion about what frameworks do exist at FDA, CPSC [Consumer Products Safety Commission], FTC [Federal Trade Commission], or OSTP” (the White House Office of Science and Technology Policy, which facilitates coordination among federal agencies). While these frameworks are “not perfect,” he said, “they have some pretty good tools that can be brought to bear fast upon areas where there is some uncertainty.”
DISCUSSION
Farahany asked Hochberg whether BMIs can read “unconstrained thought” and noted that this term, used by Hochberg in his presentation, is not well defined. Hochberg said that they cannot and does not expect this to be possible in the foreseeable future. Kahana noted that his lab was able to predict reasonably well the category of a word that a person was about to recall when performing a memory task. Hochberg pointed out that this was only possible in a very constrained situation and therefore it does not count as reading unconstrained thought. Kahana suggested that, if a thought looms large in someone’s mind, BMIs will be able to decode it. Rao said that having access to continuous brain recordings could greatly increase the capacity of computers to read thoughts. Forsland said that clinicians and researchers are often surprised at what users can do when given enabling devices. We are, he suggested, likely to see more surprises as these devices become more widely and more intensively used.
Larkin pointed out that the ALS community urgently needs communications solutions now but agreed that powerful devices that can read “unconstrained thoughts” could become a legitimate concern in the long term. Peña agreed, suggesting that the technologies that raise such concerns do not exist yet and suggested that there will be time during the device development process to address issues related to devices reading thoughts.
Farahany asked whether there might be a difference between decoding “intended” communications and decoding “unintended” ideas or imaginings, which she believed would likely be more private. Forsland suggested that devices could build in safeguards and filters to ensure that unintended thoughts are not decoded or shared. Hochberg agreed, adding that intended actions are encoded differently in the brain than imagined actions. Peña said that researchers could work with FDA to develop ways to narrow the number of channels BMIs decode to limit them to the achievement of intended outcomes while avoiding unnecessary access to a user’s thoughts.
Farahany raised the issue of data storage and ownership, pointing out that data collected now could be mined later to gain access to earlier thoughts or ideas. Rao said that it may not matter whether data has been retained if it has already been used to train an AI system to learn its patterns. Forsland argued that users should be the owners of the collected data and could choose for it to be limited or ephemeral. Farahany observed that this is not a widespread approach. She suggested that a framework to protect the use of neuronal data in certain, sensitive circumstances could be developed in a manner similar to the way that GINA (the Genetic Information Non-discrimination Act) protects against the misuse of genetic information.
Larkin and Hochberg emphasized that the need for BMIs is enormous, and Larkin said that, from a patient perspective, concerns about the technologies should not be an impediment to their short-term development.
CONCLUDING THOUGHTS AND KEY TAKEAWAYS
During the workshop’s final session, members of the planning committee provided final thoughts and highlighted workshop themes.20
Kate Rosenbluth (Cala Health) said that she was struck by the ability of BMIs to provide personalized or individually calibrated therapies, therapies which are often not available with traditional pharmaceuticals. The promise of personalization for treating disorders, particularly with wearable devices, she said, has
__________________
19 As noted in Footnote 6, products for which the developer does not make medical claims may not be subject to FDA oversight, but instead may be regulated under authorities held by the Federal Trade Commission or the Consumer Products Safety Commission.
20 Planning Committee Members Edward F. Chang (University of California, San Francisco), Gina Poe, and Gaurav Sharma (Human Performance Wing, Air Force Research Laboratory) were unable to participate in this session.
implications for access, cost, and for meeting translational and evidence-based requirements for therapeutics.
Abidemi Bolu Ajiboye (Case Western Reserve University) highlighted responsibility to end-users and patients, pointing out that, while funding for academic clinical trials is time-limited, trial participants often keep their implanted devices when the trial concludes. He said that there is no definitive model for researchers and others to follow to meet obligations to those users. Donoghue added that funding agencies have some responsibility here, and that responsibility extends not just to maintaining a device, but to addressing complications that arise from the removal of the device.
Ienca emphasized that there is a lack of qualitative measures to capture the subjective experience of users of these devices.
Mayberg said that, while there are many issues to be concerned about with these technologies, the near-term focus should be on patients and on addressing pragmatic issues related to the better treatment of disease.
Farahany emphasized the importance of maintaining data privacy. She noted that, for big technology companies, data acquisition is a major business goal. She raised the issue of access and equity, suggesting that wearable devices might allow for more universal access to these technologies. “The ability to understand the human condition through decoding is so powerful and valuable that we have an imperative to move ahead,” she said, “but we have tall and large issues to address as a society to be able to embrace the technology.”
Donoghue appreciated that the workshop highlighted a shared commitment to strong ethical principles in the development of new technologies. He ended the workshop by reflecting on how far BMIs have come in recent decades: “It’s almost 20 years since we implanted one of the first people that ever had a brain-computer interface. It went very slowly at first but now things are really going in many different directions with a lot of benefit.”
DISCLAIMER This Proceedings of a Workshop—in Brief has been prepared by Sarah Carter, Steven Kendall, and Anne-Marie Mazza as a factual summary of what occurred at the meeting. The committee’s role was limited to planning the event. The statements made are those of the individual workshop participants and do not necessarily represent the views of all participants, the project sponsors, the planning committee, the Committee on Science, Technology, and Law, or the National Academies.
REVIEWERS To ensure that it meets institutional standards for quality and objectivity, this Proceedings of a Workshop—in Brief was reviewed by Christine Grady, U.S. National Institutes of Health; Story Landis, U.S. National Institutes of Health (ret.); Helen Mayberg, Icahn School of Medicine at Mount Sinai; Jonathan Moreno, University of Pennsylvania; and Treye Thomas, U.S. Consumer Product Safety Commission. Marilyn Baker, National Academies of Sciences, Engineering, and Medicine, served as the review coordinator.
COMMITTEE ON BRAIN-MACHINE AND RELATED NEURAL INTERFACE TECHNOLOGIES: SCIENTIFIC, TECHNICAL, ETHICAL, AND REGULATORY ISSUES, PROCEEDINGS OF A WORKSHOP—IN BRIEF John P. Donoghue (Co-chair) (Brown University); Nita Farahany (Co-chair) (Duke University School of Law); Abidemi Bolu Ajiboye (Case Western Reserve University); Edward F. Chang (University of California, San Francisco); Marcello Ienca (Swiss Federal Institute of Technology in Lausanne [EPFL]); Helen S. Mayberg (Icahn School of Medicine at Mount Sinai); Gina Poe (University of California, San Francisco); Kate Rosenbluth (Cala Health); Gaurav Sharma (711th Human Performance Wing, Air Force Research Laboratory)
STAFF Steven Kendall, Program Officer; Anne-Marie Mazza, Senior Director; Dominic LoBuglio, Senior Program Assistant
SPONSORS This project has been funded in whole or in part with Federal funds from the BRAIN Initiative® of the National Institutes of Health, the National Institute of Mental Health, and the National Institute of Neurological Disorders and Stroke, Department of Health and Human Services, under Contract No. HHSN263201800029I. For additional information about the Committee on Brain-Machine and Related Neural Interface Technologies: Scientific, Technical, Ethical, and Regulatory Issues, visit https://www.nationalacademies.org/our-work/brain-machine-interface-technologies-scientific-technical-ethical-and-regulatory-issues-a-workshop.
For additional information about the Committee on Science, Technology, and Law (CSTL), visit https://www.nationalacademies.org/cstl/committee-on-science-technology-and-law.
Suggested citation: National Academies of Sciences, Engineering, and Medicine. 2023. Brain-Machine and Related Neural Interface Technologies: Scientific, Technical, Ethical, and Regulatory Issues, Proceedings of a Workshop—in Brief. Washington, DC: The National Academies Press. https://doi.org/10.17226/26835.
|
Policy and Global Affairs Copyright 2023 by the National Academy of Sciences. All rights reserved. |
 |













