6
Participant Discussion: Future Directions for the Food and Nutrition Board
The third session, moderated by Bernadette Marriott, Professor Emerita at the Medical University of South Carolina, was a panel discussion. For the first topic, A. Catharine Ross and Cheryl A. M. Anderson provided their views on nutrients in life from the perspective of then, now, and future considerations. The second panel, presented by Barbara Kowalcyk and Stephen Taylor, provided their perspectives on food safety, foodborne contaminants, and how these topics may be managed in the future. The last panel, presented by Benjamin Caballero and Jamy Ard, addressed applications of the Dietary Reference Intakes (DRIs) toward optimizing diet and health outcomes, and the issue of obesity from a global perspective.
NUTRIENTS IN LIFE: WHERE ARE WE AFTER 100 YEARS AND WHERE ARE WE HEADED?
Ross, Professor and Occupant of the Dorothy Foehr Huck Chair of Nutrition, and Head of the Department of Nutritional Sciences at The Pennsylvania State University, began with a brief timeline of vitamin A research that was conducted prior to formation of the Food and Nutrition Board (FNB). She described the work of E. V. McCollum, who was one of the longest serving members of the board. Long before the chemical identities of many nutrients were known, there was a lot known about their functions, she said. In the case of vitamin A, that included its role in vision, reproduction, and immunity. Next came the era of chemical elucidation with pioneers such as Paul Karrer, who received a Nobel Prize for his work in this area. That was followed by work in food security and rationing,
which included vitamin A. Ross referred to a timeline on DRI development (see Figure 6-1). The Recommended Dietary Allowances (RDAs), she noted, were based on the concept of a healthy population. Two influential reports in the late 1980s, the Surgeon General’s Report (HHS, 1988) and Diet and Health (NRC, 1989), and in the 1990s, the IOM report How Should the Recommended Dietary Allowances be Revised? (IOM, 1994a) brought in the concept of chronic disease.
Returning to vitamin A, Ross mentioned that the last DRI report on vitamin A was published in 2001. “At that time, what did we know?” she asked. Among the types of evidence available were dark adaptation studies, conducted from the 1940s to the 1970s with a total of 13 individuals. We could not establish Estimated Average Requirements (EARs) and RDAs separately for men and women because there were only two women in the study, she said. Likewise, she added, there was no data available to establish an EAR for children and adolescents, thus the DRIs for children were extrapolated from adults based on metabolic weight. The same was true for the report on carotenoids. Since that time, noted Ross, we have many new studies that have given us a clearer understanding of nutrient absorption, turnover, and disposal; of how intake or requirement might be related to health status; and the impact of inflammation on micronutrient assessment. She included an example from the field of personalized nutrition in which a single nucleotide polymorphism in the gene that converts beta carotene into vitamin A differs not only in individuals, affecting their metabolism, but also among populations of varying ancestry.
In terms of the future, Ross said that her recommendation for the DRI process would be to step back and take a critical look at the model. The model assumed a distribution of data, and when data were not adequate,
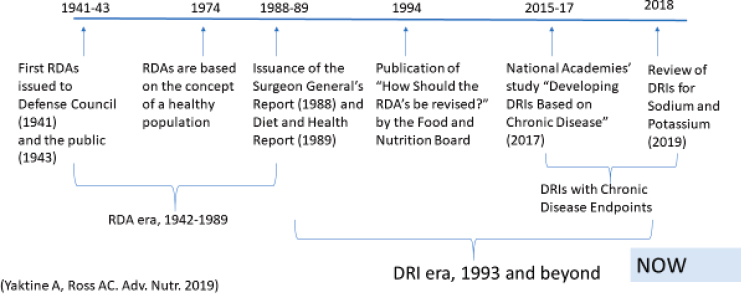
SOURCES: Presented by A. Catharine Ross on February 28, 2020. Reprinted with permission from Yaktine and Ross, 2018.
we had to fall back on solutions that were totally model driven, she said. There needs to be a consistent plan for updating, and that might not need to be an entirely new report, but some way of scanning the literature to know that the DRIs are up to date. In conclusion, Ross suggested that the FNB continue to advise the nation in a proactive, forward-facing way, providing advice for healthy living and a longer lifespan. She added her wish for the FNB to revisit the Diet and Health report because it addressed nutrition issues in a very comprehensive way.
Anderson, Professor and Interim Chair of the Department of Family Medicine and Public Health in the School of Medicine at the University of California, San Diego, continued the discussion of nutrients and life with remarks on current challenges and future considerations. She began with her thoughts on the early phase of the relationship to nutrients and life. She noted that there was a strong focus on nutrient inadequacy and concerns about infectious disease, because those were the primary killers of humans. There was also a food system without much fortification, she added.
While discovery is still important, said Anderson, what we will be facing in the coming decade is how to balance personalized nutrition, understanding genetic information better, and the public health approach. “Saving lives one at a time. Saving lives millions at a time,” she said. Also, thinking about moving from that limited knowledge base into a more robust evidence base, she added. Anderson reminded the audience that not everything can be studied in a clinical trial context. There is a need to better understand how to use epidemiologic data to better inform what we are trying to do, moving beyond age and sex specifications, and really thinking about the diversity in our populations, she noted. Anderson gave as an example the understudied area of transgender individuals and how the process of transition might impact nutritional needs. Adding to comments made earlier by Ross and Janet King, Anderson noted there is a need to think about the DRI framework and where it needs to evolve. For example, the birth to 24 movement and thinking about greater diversity in the DRIs will be very useful, she said.
Every Dietary Guideline Advisory Committee now thinks about nutrients of concern for overconsumption. “We now have to get to a place where we can have healthy dietary recommendations be the default choice for individuals where access is available to everyone regardless of where you live, work, play, or learn,” she said. Anderson reminded the audience that we do not eat nutrients, we eat foods, but not in isolation; we eat them in patterns. With regard to the food system, Anderson noted that it has never been a simple system, adding that if we are going to advance in that area, then we need to partner with the food industry. She acknowledged the potential for conflicts of interest with the food industry and noted that it is an
important area for the FNB. Anderson concluded with a slide summarizing current challenges and considerations for the future (see Figure 6-2).
MANAGEMENT OF FOOD SAFETY: HOW DO WE PROCEED TODAY FOR THE FUTURE?
Kowalcyk, Director of the Center for Foodborne Illness Research and Prevention, Department of Food Science and Technology at The Ohio State University, offered her perspectives on food safety and how to proceed today for the future. She began by noting that food safety is a global issue and a global public good. “It is critical to food security and nutrition—you cannot have food security or nutritious food if it is actually making you sick,” she said. Kowalcyk then spoke about food safety as an economic issue. She referred to estimates of medical costs and lost productivity, which place a significant burden on the economy, adding that there is a loss of consumer confidence as well when food is unsafe. In low- and middle-income countries food safety can be a barrier to market access both internationally and domestically. In these countries, she noted, many small holder farmers
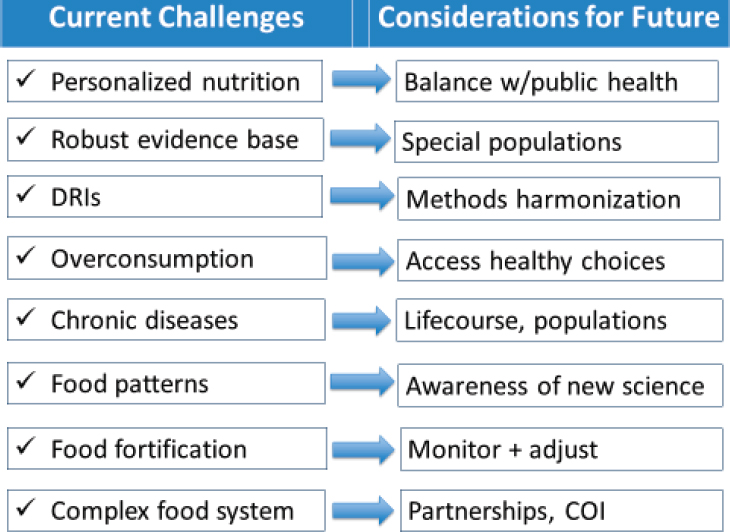
NOTE: COI = conflict of interest; DRI = Dietary Reference Intake.
SOURCE: Presented by Cheryl A. M. Anderson on February 28, 2020.
can only operate within the informal markets, and food safety can lead to food loss and waste—an important consideration when thinking about a growing global population.
Kowalcyk reported that the World Health Organization (WHO) estimates that 600 million people (about 1 in 10) get a foodborne illness each year globally, resulting in 421,000 deaths, one-third of which are children, and 33 million healthy life years lost. She added that these statistics are on par with the incidence of malaria and tuberculosis worldwide: “It is a significant public health issue that has not gotten the attention that it needs.” Kowalcyk went on to discuss long-term health outcomes associated with foodborne illness. These include reactive arthritis, irritable bowel syndrome, Crohn’s disease, and ulcerative colitis. She also noted there are several neurologic disorders associated with Listeria moncytogenes and Toxoplasma gondii, and renal sequelae such as hemolytic uremic syndrome caused by Shigella and shigella-producing E. coli. Kowalcyk added that emerging data on outcomes suggests a relationship between Toxoplasma gondii and schizophrenia and depression. To illustrate the complexity of the food supply, Kowalcyk showed an infographic called The Well-Traveled Salad (see Figure 6-3).
The U.S. food supply is global and a single meal can contain ingredients from around the world, and this shows the complexity of the food supply chain and how difficult it is to manage the risks, she said. The best way to approach food safety is using a risk-based approach. “You have to think about animal contact, food pathways, the environment, and how that affects human exposure to these pathogens and potentially results in disease,” noted Kowalcyk, adding that we have to take into consideration the willingness of society to change, the choices available to us, and the costs (see Figure 6-4). The risk-based food safety system is about continuous process improvement, remarked Kowalcyk. She then posed the question: If we only have enough resources for either research dollars or intervention for one pathogen, which one do we pick? It is about understanding and ranking the risks.
With regard to the future of food safety, Kowalcyk pointed to analytics and tools, noting the important role of observational data to inform decision making. If we could leverage both public and private data sources, she said, that would have a huge impact on public health. In closing, Kowalcyk stressed the need to look at food safety as a global issue, noting that our food safety system is only as good as the weakest link, which means we need to work globally to improve the system. She would like to see an integrated, holistic, systems-based approach that is proactive, preventive, and anticipatory, not reactive like the current system. “It considers not just human health, but animal, environmental, and plant health as well, and ultimately delivers safe, sufficient, and nutritious food for all.”

SOURCE: Presented by Barbara Kowalcyk on February 28, 2020.
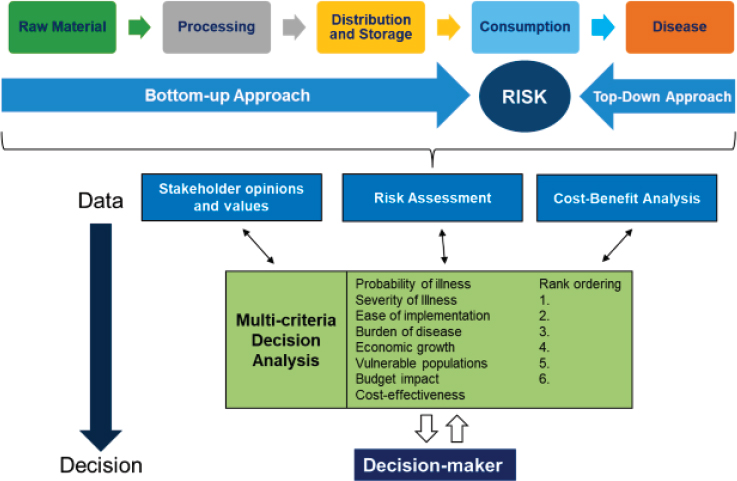
SOURCES: Presented by Barbara Kowalcyk on February 28, 2020. Reprinted from Devleesschauwer B, Scharff R, Kowalcyk B, Havelaar A. Burden and risk assessment of foodborne disease. In T. Roberts (ed.), Food Safety Economics Incentives for a Safer Food Supply (pp. 83–106). Springer International Publishing 2018. Reprinted with permission from Devleesschauwer et al., 2018.
Taylor, Founding Director of the Food Allergy Research and Resource Program and Professor Emeritus with the Department of Food Science and Technology at the University of Nebraska–Lincoln, began by noting an observation from the father of toxicology, Paracelsus, that “only the dose makes the poison.” All chemicals are toxic, Taylor said; it is just a question of dose, adding that nutrients can be toxic too. Taylor then spoke about naturally-occurring contaminants, noting that phycotoxins are likely of greatest concern, although now we are thinking about algae as sources of novel foods. Human-made contaminants, such as those that may be released when industrial accidents occur, generally do not cause many problems, he said, while human-made adulterants have become an issue in recent years. Taylor added that although we worry about food additives, they are not very toxic. Allergens are safe for most of us, unless you have an allergy or intolerance.
Among the reports that he relies on most, Taylor said, are Toxicants Occurring Naturally in Foods (NRC, 1973), which contains information not even available on the Internet; and Seafood Safety (IOM, 1991), which showed that nutritious and healthful food can also be hazardous. Taylor also mentioned the report Finding a Path to Safety in Food Allergy
(NASEM, 2017), a topic he characterized as one that is huge and probably needs to be subdivided into individual studies to have greater impact. Taylor noted that the future of food safety includes novel food sources as well as foods from around the world, and it falls on the U.S. Food and Drug Administration (FDA) to ensure they are safe. Bioactives are another group of substances that may be toxic at doses that people consume. He referred back to the report on toxins occurring naturally in foods, noting that the report includes chapters on some foods that are now nutraceuticals. “Consumers believe that if it is natural, it is safe,” he added. As we have more individualized health and nutrition, what is good for one might not be so for another. Nutrients can include nutraceuticals, dietary supplements, and bioactives, he said, but they all have toxicities and assessing the safety of these materials is a big task.
Among regulatory issues that Taylor noted is that when the Federal Food, Drug, and Cosmetic Act was passed, it was determined that if a chemical came from a natural source, it was safe. In addition, the Delaney clause states that if a chemical is found to cause cancer, it cannot be in foods. We have many food ingredients that have been banned because of their ability to induce cancer in laboratory animals that may not be unsafe in humans at lower doses, he said. Taylor closed by stating that the FNB could do more on chemical food safety in the next 80 years and the U.S. population would benefit.
GLOBAL UNDERSTANDING AND APPROACHES FOR OPTIMAL DIET AND HEALTH
Caballero, Professor Emeritus in the Department of International Health at the Johns Hopkins Bloomberg School of Public Health, focused his remarks on the rationale and basis for the DRIs, and whether there is a global role for those values at the international level. Caballero spoke from his experience on the macronutrient panel for the first DRIs. He began by referencing the previous talk by Janet King about global harmonization of the DRI approach, noting that with regard to the marketplace, the DRIs are a global endeavor. Foods need to be transported, controlled, and approved across borders, and it is essential to have a minimal consensus in order to ensure quality in the food chain, he said. Furthermore, we know that the DRIs are adopted by other countries—many have simply picked up the numbers they want and use them. Furthermore, in his visits to educational institutions in other countries, Caballero has seen students and teachers of nutrition using the DRIs as textbooks. Thus, the DRIs have an international presence, formally and informally. The question is, he said, is this international presence supported by science? He thinks not. One reason is that the databases, for macronutrients in particular, are not representative
of the diverse populations and variety of dietary patterns around the world. In fact, the vast majority of data on which the DRIs are based are from Western, white populations. “The reality is that our aspiration and our responsibility as a powerful country that generates a lot of information that the rest of the world uses requires that we consider this if we want the DRIs to play a global role,” remarked Caballero.
Caballero then addressed the importance of considering new knowledge that will be acquired from data on different populations. In the past, the focus has been on measures of centrality, and not enough attention has been paid to measures of dispersion, which explains why determining nutrient requirements goes beyond just body size, he noted. Responses to the environment and genetic or epigenetic responses to diet composition among individuals will cause differences in absorption, metabolism, and utilization of nutrients. Caballero added that in the future, we will need a better understanding of the characteristics that determine nutrient requirements for individuals; perhaps criteria that are based on function or individual characteristics. Personalized medicine or nutrition will only be possible if we can identify indicators that are not simply an expression of measurement error or variability, but of specific physiologic function that can be used to predict requirements for different nutrients.
Caballero next addressed requirements for protein and nutrients associated with high quality proteins. Protein quality measures used to be based on the type of amino acids in eggs and milk but is now determined by an amino acid score, which is a problem because millions of people do not have access to high-quality animal proteins. Therefore, to base a recommended intake on a protein that is not attainable for millions of people globally does not make a lot of sense. Caballero added that using digestibility to adjust for protein quality can correct for a low amino acid score, but that requires consuming more in order to achieve the level of high-quality protein needed. “It would be more useful for nutritionists around the world if we are talking about protein that is available to people,” he remarked. This is related to sustainability, and high-quality animal protein is not sustainable. It is not possible to provide that kind of protein to all humans, and attempts to do that will create serious damage to the environment, he added. Caballero cited an article, the EAT-Lancet diet (Hirvonen et al., 2019), which recommends 14 grams of animal protein per day, noting that he did not know if it was possible to meet the adult protein requirement of 62 grams of high-quality protein starting with just 14 grams of animal protein. Caballero clarified that addressing sustainability of diets was not a traditional mandate of the DRI panels, but this would likely have to change in the future, he said.
In closing, Caballero recalled that, in the past, organizations like WHO and foundations like the Nestlé Foundation were an important part of
research on nutrient requirements. “We need to make the case that without an extraordinary amount of funding these activities cannot be carried on.… We need to motivate the younger generations to carry on the efforts that are going to be needed in the years to come,” remarked Caballero.
Ard, Professor in the Department of Epidemiology and Prevention and the Department of Medicine at Wake Forest Baptist Health, gave the final presentation for the session from the perspective of using obesity as a framework to consider the future of nutrition and chronic disease. He began by asking whether there was a realistic path toward mitigating the prevalence of obesity worldwide. Ard noted that for most of human existence, scarcity was the problem, and those who were heavier were considered to be well-off, because it was an indicator of access to food. The problem is that currently the inverse is true, especially in high-income countries where there is a high prevalence of obesity. Now, he added, as higher socioeconomic status countries see an increase in the prevalence of obesity, the burden of chronic disease is borne disproportionately by lower income groups (see Figure 6-5).
Another scenario that starts to play out, noted Ard, is that healthfulness becomes a brand and a status that you can buy if you are wealthy. Costly exercise options are being presented as a way to get healthy. We have started to link the idea of health to expenditure of money. Ard then described a study to illustrate the point. In the study, consumers were asked to choose the healthier option of two similar chicken wraps. In the first condition, one wrap was more expensive and in the second condition, the other wrap was more expensive.
In both conditions, the test subjects chose the more costly wrap. “This intuition that we have, if it costs more then it must be healthier, is something that is being exploited in marketing, but it is also being internalized in consumer behavior,” he said, adding that “it starts to change how we think about ability to access health.”
Ard described a similar occurrence in emerging economies, especially where individuals move from a lower socioeconomic class to a middle-income class. “Individuals who previously would have been more likely to have issues of undernourishment are now finding that their problems are related to excess calories,” he said. Ard shared a quote from a Washington Post article: “Once underfed, Brazil’s poor have a new problem: obesity.” He explained that when you compound access to what are seen as luxury items together with food insecurity, it leads to and is associated with chronic disease (see Figure 6-6).
Ard noted that this kind of transformation of disparities that goes from undernutrition to excess is something we are experiencing not only in the United States, but globally. He told the audience that we have to solve for how we provide for equitable access to a high-quality diet in this setting
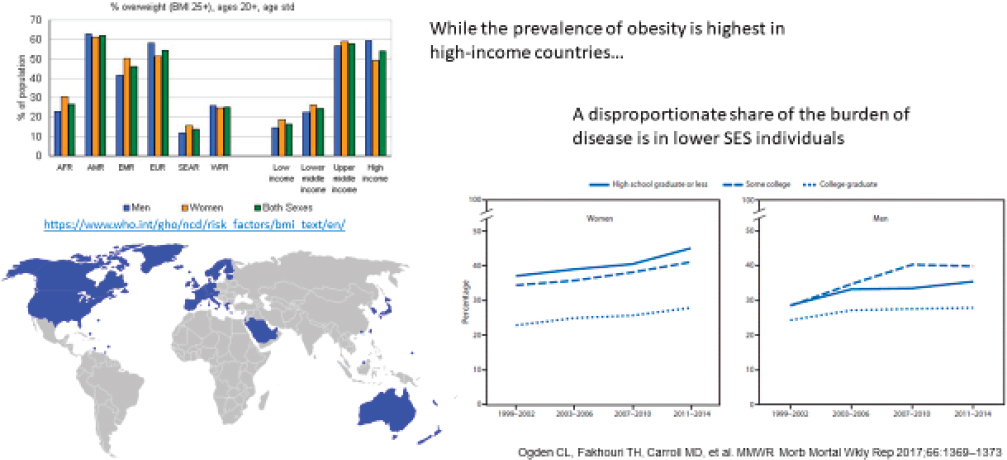
SOURCES: Presented by Jamy Ard on February 28, 2020. From Ogden et al., 2017; WHO, 2012.

SOURCES: Presented by Jamy Ard on February 28, 2020. From Coleman-Jensen et al., 2018.
of abundance. “If we do not do this,” he added, “the consequences are dire because things like diabetes will continue to increase.” An idea that Ard proposed is to repurpose our goal of alleviating hunger, for example, through the Supplemental Nutrition Assistance Program. His idea, he explained, is to change the central goal by providing key foods for the basis of a nutritious diet to promote health. The Special Supplemental Program for Women, Infants, and Children, he noted, provides the basics of a healthy diet. Why would we not think about giving people enough food so that they know they have something to eat, and if they consume it, will have a better chance of being healthy?, he asked. That would allow them to put their resources into other areas that could permit them to be more upwardly mobile and not priced out of healthy food options or exercise.
Ard suggested using incentives to motivate behavior change. Providing incentives to participants to both increase fruit and vegetable intake and decrease sugar-sweetened beverage intake would prevent cardiovascular disease, he said. “It would seem to me that we should be able to figure out how to feed a population and change what we do in terms of resources, so that we end up promoting health and wellness and making it accessible and equitable,” remarked Ard.
DISCUSSION
Marriott moderated the discussion session. She opened with a question to the entire panel. She asked each speaker to identify the most important thing the FNB could do, given unlimited funds, and to identify which issues would be the highest priority. Ard responded that his highest priority would be to revisit the ideas around chronic disease risk reduction and nutrition, especially as it relates to energy balance. Ard went on to suggest going beyond prevention to control of chronic disease because of its widespread prevalence. Kowalcyk identified her priority as taking a more integrated approach to nutrition, food security, and food safety; and taking a more active leadership role in the prevention of foodborne disease. Caballero suggested separating domestic from international health. He explained that obesity makes lower income people more vulnerable, and the kind of comorbidities they experience are types that require continuous care. “Obesity and the health care system are the two big challenges,” he said, adding that we need to consider the lack of access to healthy diets. Taylor remarked that FNB could be very helpful in the interface between food safety and nutrition because the definition of nutrition keeps expanding. He noted novel foods and bioactive substances as examples. “I think the FNB could help the FDA and other organizations in how we should assess the comparative benefits and risks, hazard assessment of new products,” he added.
Anderson suggested a continued but transdisciplinary focus on the food system—thinking about building, re-building, reimagining the food system and the built environment so that it sustains health. Anderson went on to suggest completely rebuilding the food system, using one small town to implement changes and a different town as a control. Ross recommended that the FNB step back and ask how its reports have been impactful and how can the FNB be a more public-facing information entity. She added that she thought the output could be magnified so that the FNB would become more of a household word. Schneeman said that a thread that ran through many of the comments is the question: How does the science impact behavior change? Schneeman went on to say that her interest was in thinking about the future. “How do we need to think about that challenge of making sure that science is used in a way that actually leads to behavior change?” she asked. Anderson added that the socio-ecological model provides a framework to consider whether there can be an impact at the individual level, adding that a systems approach will be key to getting to sustainable solutions.
Shiriki Kumanyika, Chair of the FNB, commented on nutrition transition effects in lower income, rural, and urban populations. “I wonder what we can do about the fact that we know we have several different Americas related to income; and have you thought about how we could face that?” she asked. Caballero responded that he saw that as the core of the problem. One approach, he added, would be to identify the most at-risk population based on the standards of the society and decide whether the target is the population or the society. The reason, he explained, is that characteristics that increase risk in a vulnerable population are important factors in determining how to change them. John Erdman from the University of Illinois asked Ross to expand on her suggestion to revisit the Diet and Health report (NRC, 1989). He asked if it might be more or less valuable to look at the report again. Ross answered that the report was impactful, and that she was thinking more about chronic disease and its associated behaviors, adding that something more comprehensive was needed.
Nancy Chapman from Chapman and Associates asked the panel about raising the visibility of how important nutrition is to the survival of those incarcerated in refugee camps. Caballero responded that disrespecting human rights carried health consequences because basic needs like food and health care are ignored. He added that it does not have much to do with requirements or guidelines; it is a political problem, in his opinion. Anderson added that there are two other dimensions to the issue. One, she said, is the gap in knowledge about what social migration means for health outcomes, and the other is that sometimes refugees experience a nutrition transition in coming from an environment in which their behaviors are protective of health into one where overconsumption begins to happen.
Audience member Connie Weaver remarked that Anderson had raised an issue for the FNB to think more carefully about—that is, personalized nutrition for one versus public health recommendations for millions. “Have we had any breakthroughs that would lead to much more than the occasional Single Nucleotide Polymorphism that has a different requirement with all the new technology? Where are we headed in that?” she asked. Ard responded that he thought the commercial space has leveraged interest in genetics, with commercialization of personalized diets. The added benefit is small, he said, whereas, from a public health perspective, if we do what we already know is effective, then we will see large effect sizes across the population. Anderson added that, on a population level, some interventions have relatively small effects, but they are big in terms of what happens to mortality and other chronic disease effects. She concluded the discussion by remarking, “If we are doing the right things that we know through our studies’ work, we really do stand a chance to shift that population distribution in the right direction.”
This page intentionally left blank.
















