3
Barriers to and Opportunities for Program Implementation and Widespread Scale-Up
While theory and research demonstrate the positive outcomes of implementing family-focused prevention interventions for adolescent substance use, putting those interventions into practice can prove to be difficult. Different settings have seen varying levels of success, and lessons can be learned for future implementation, especially since the start of the COVID-19 pandemic. This chapter discusses the various barriers to and opportunities for both program implementation and widespread scale-up of interventions.
BARRIERS TO AND OPPORTUNITIES FOR PROGRAM IMPLEMENTATION
This section offers an overview of implementing programs in various settings and reviews the existing structural barriers that need to be addressed in order to successfully execute these programs.
Translating In-Person Interventions to Virtual Platforms
Yannine Estrada, research assistant professor at the University of Miami School of Nursing and Health Studies, reviewed the implementation of eHealth Familias Unidas in pediatric primary care settings. This program is an online adaptation of the Familias Unidas intervention, which is a culturally informed program focused on preventing drug use and sexual risk behaviors among Latinx youth. Estrada explained that the original intervention is delivered through eight family-centered parent group ses-
sions and four targeted family sessions. During the parent group sessions, parents discuss methods of prevention and how to communicate with their children. The information gathered in these group sessions is discussed in the family sessions. The program is highly participatory, said Estrada, and parents often find solutions to their problems among themselves. However, even though the program has been successful, like many evidence-based programs, it has not been widely disseminated.
In an effort to increase dissemination of the intervention, Estrada said, the Familias Unidas team created an online version of the intervention, eHealth Familias Unidas, using four different elements. The first element includes a parent group session via video, in which parents watch other parents have discussions about how to talk to their adolescents about difficult topics such as substance use and sexual behavior. Second, Estrada continued, the research team created a telenovela series with eight episodes that directly map on to the content of the parent video sessions. Third, the research team paired the video sessions with interactive exercises asking parents key questions. Estrada explained that the last component uses video-conferencing software to deliver virtual family sessions, which are the same as the family sessions conducted as part of the in-person intervention.
Estrada said feedback from clinic personnel, facilitators, and parents showed them how important it was to understand the relevance and effectiveness of the intervention. Feedback from clinic personnel highlighted the importance of minimizing clinic disruptions, providing an administrative assistant to sort through logistics, and having technical and clinical support. While the evaluation studies are still ongoing, Estrada shared preliminary results that show direct effects on past-90-day drug use from baseline to 24 months post baseline. There have also been positive parenting and parental involvement findings from baseline to post-intervention. Furthermore, Estrada reported, 63 percent of parents completed all of the sessions, while only about 16 percent did not participate in any of them.
The research team is working to apply their findings to an ongoing trial. Early on, they noticed that many families see primary care as a less stigmatizing setting to receive services, Estrada explained, and many families see doctors as trusted sources of information. The research team listens to the clinic personnel and integrates the feedback to make the program more likely to be sustained over time. In conclusion, Estrada said they are just beginning a Type 1 effectiveness implementation hybrid trial. This allows them to test the intervention randomizing time to look at sustainment as a primary outcome, which will help them understand whether the clinic is able to continue offering the program after the research team leaves.
Using Screening and Family-Based Intervention in Pediatric Primary Care
Daniel S. Shaw, director of the Center for Parents and Children and the Pitt Parents and Children Laboratory at the University of Pittsburgh, began by highlighting some of the known barriers to implementing prevention-based interventions. One of the biggest challenges for prevention science is simply how to scale up evidence-based programs, he noted. There is limited uptake of evidence-based science in real-world community settings. Furthermore, Shaw added, disparities are particularly pronounced for families living in poverty and for racial and ethnic minorities because of institutional and structural racism. He commented that in the primary care setting specifically, other barriers arise, including insufficient time in pediatric visits for physicians to implement evidence-based parenting programs and lack of resources or training to manage screenings. However, Shaw noted, primary care settings also have several benefits, including trust and familiarity from families, sustainable infrastructure, and broad access.
As one example of embedding evidence-based interventions into an existing primary care setting, Shaw explained a screening and intervention program, the former using the Ridenour Youth Risk Index, which includes 23 items that were the best predictors of substance use one year later in a longitudinal study. The screening survey takes about seven minutes to complete—both the child and the parent fill one out—and it can be done in the waiting room or exam room while waiting for the physician. Shaw said the second component of the program is the Family Check Up (FCU). The FCU begins with an initial interview including questions about parent aspirations for their children, then an assessment of the child and family, and then parent feedback, ending in goal setting and, in most cases, brief evidence-based parent management training sessions. As Shaw elaborated, the initial interview helps the provider to get to know the parents and their goals for their child. Using data from the assessment and the initial interview, parents are then engaged in a feedback process designed to motivate and activate parents to improve their parenting, their well-being, and their child’s behavior. Following the feedback, parents can work with the parent consultant, do the work themselves, or be referred to obtain other appropriate community resources (e.g., housing, employment, medication for mental health issues). Shaw shared data from multiple studies demonstrating that when parents and caregivers are provided with concrete tools to prevent or address substance use among their children, they will put those tools to use.
Shaw discussed initial results from a current study on the effectiveness of this screening and intervention program. More than 93 percent of families completed the intervention, making it through three or more sessions to the feedback and treatment stages. Participating children were 10–13 years old and were followed for one to two years with more than 85 percent
retention. Participation in the intervention reduced risk of initiating use of a new substance by 37 percent and reduced risk of drinking by 26 percent. Additionally, the results showed decreased rates of reported anxiety.
In early childhood prevention efforts, Shaw described another sample of more than 700 families enrolled in the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) who were randomly assigned to the FCU. This study (Galán et al., in press) demonstrated how intervening for children as young as two can lead to decreased substance use in adolescence by reducing lifetime risk factors and increasing lifetime protective factors.
Shaw also commented on genetic risk factors related to substance abuse. While there is a genetic component, his team conducted a study in which genetic risk that led to substance use in adolescence in the control group was attenuated in the intervention group for families randomly assigned to the FCU (Elam et al., 2022). The genetic risk can be thought of as malleable, he concluded.
Finally, Shaw shared results from the same WIC-based study looking at intergenerational trauma, considering children of mothers who experienced emotional, physical, and sexual trauma in their lives. For the control group, children of mothers (and mothers themselves) with trauma had higher rates of marijuana use than children of mothers who did not experience trauma (see Figure 3-1). In the group that participated in the FCU, children of mothers (and mothers themselves) who experienced these three types of maltreatment actually had lower rates of marijuana use than their peers.
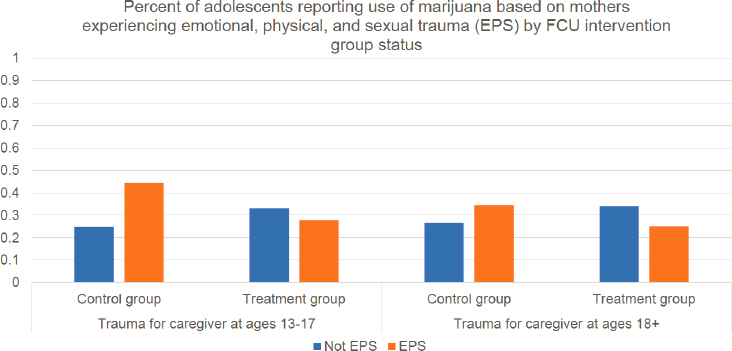
SOURCE: Shaw’s presentation, May 5, 2022.
Preventing substance use for youth at risk is both possible and feasible, said Shaw. This was demonstrated by the reduced risk of youth substance use through the FCU. Shaw also highlighted the potential for reimbursement for such interventions, noting that a licensed clinical psychologist at Children’s Hospital of Pittsburgh uses a current procedural terminology code to bill for the FCU and receives reimbursement from Medicaid and other insurance providers.
Identifying Structural Barriers to and Facilitators of Family-Focused Interventions
Brenda Miller, senior scientist at the Pacific Institute for Research and Evaluation, presented some of the structural barriers to implementing family-focused interventions. She highlighted four components to consider in these discussions: the culture of prevention; differing infrastructures for delivering best practices; internal organizational barriers and facilitators; as well as laws and policies at the local, state, and federal levels.
Culture of Prevention
The culture of prevention is the values, beliefs, and knowledge about prevention and its role within health promotion, Miller explained. This differs across families and communities, but the following key concepts characterize a culture of prevention that is supportive of action. These concepts include:
- Public acceptance of values and ideals;
- Policies and legal frameworks that support prevention;
- Equitable allocation of resources;
- Incorporation of scientific findings and clinical knowledge in communication; and
- Coordination of services across multiple sectors of non-governmental organizations and government agencies.
Miller also commented on beliefs that become barriers to adopting this prevention culture, such as the concern that focusing on prevention will redirect resources away from treatment. Additionally, families may push back, saying that prevention interventions are not relevant to them because their children do not use substances. The recent emerging distrust of scientific and clinical expertise can make it difficult to engage in constructive conversations with some parents and caregivers. Thus, a paradigm shift is needed, she said.
First, Miller listed, instead of planning a system response focused only on treatment, a plan should be balanced on both prevention and treatment
(Petras et al., 2021). Secondly, she continued, there needs to be more effective communication and engagement with families. Moving forward, the first action should be centered on communicating to different audiences, she said. This can include articulating the economic benefits of prevention, as well as the investment in life potential. Human beings are resources more important than money, she continued. There is also an opportunity to develop more equitable models and to include families in prevention programs.
Differing Infrastructures
Miller called attention to the infrastructure needed to support the implementation of prevention strategies. Schools and health care settings provide great opportunities because of their easy access to the targeted age group, she said. They also represent existing infrastructures that have already established relationships with families. However, Miller noted, there are also barriers in these settings, such as the workforce not having the bandwidth to do more work and lack of engagement in school systems for some families. Furthermore, she added, schools may have difficulty reaching parents and caregivers, which can impede prevention efforts.
In the face of these challenges, Miller proposed more online delivery, noting the mounting evidence of its success, especially for primary prevention. Benefits include interactive content, low-cost delivery, and the ability for families to engage in self-directed delivery from their homes (Byrnes et al., 2019). Online delivery of prevention interventions can also be more easily updated with new information and current issues, she added. However, this avenue is not without challenges, as it requires funding to maintain the virtual components, requires families to have access to stable internet and technology, and requires funding for maintaining the websites that deliver interventions (Wang-Schweig et al., 2019). Miller suggested there are also opportunities to increase uptake of interventions through other community organizations, including faith-based organizations, community coalitions, and neighborhood hubs like barbershops or salons.
Internal Organizational Barriers and Facilitators
Even when an organization is well established and has a willing workforce, it may not be ready to implement a prevention intervention, said Miller. Additional organizational characteristics are needed to facilitate implementation, including organizational readiness (Shea et al., 2014), leadership for developing an implementation plan and supporting employee efforts (Aarons et al., 2015), and a climate of acceptance around how interventions are implemented (Ehrhart et al., 2014). Structural barriers
within organizations can also affect the implementation of family-based interventions, Miller added, including a lack of resources, a need for training on prevention approaches and outcome measurement, and disparity in access. Many communities do not have sufficient resources to provide effective prevention of adolescent substance use, she said. To better prepare for implementation, Miller noted, organizations should work with implementation science experts, invest in training in both the program and family engagement techniques, and engage in collaborative work and knowledge sharing with other community organizations and resources.
Laws and Policies
Lastly, Miller reviewed the barriers to and facilitators for laws and policies that support prevention interventions. For example, she said, evidence suggests that policies implementing higher alcohol taxes decrease adult alcohol consumption, which indirectly decreases youth drinking as well (Xuan et al., 2013).
However, Miller explained, there may also be unintended consequences of certain policies, as has been seen with social host laws, designed to discourage adults from hosting private parties with alcohol for teens. This can lead to teens having parties in less safe environments, such as local parks and open spaces. Miller commented that, instead of addressing the root problem, these laws just move the problem to a different setting. Finally, she added, passing a law does not necessarily mean it will be enforced. Studies have revealed that targeting adults who provide youth with alcohol or drugs requires resources, training, and buy-in from law enforcement (Jones-Webb et al., 2015).
Miller highlighted Mothers Against Drunk Driving as a successful example of efforts to change drinking and driving laws, which resulted in more legal enforcement, more serious legal and financial consequences, and more treatment approaches for drinking drivers with alcohol diagnoses. This effort, she said, represents a bottom-up or public demand for change rather than a top-down approach to create effective policies for addressing problems in communities.
Discussion Session with Panelists and Workshop Attendees
Initial questions from workshop attendees focused on how to shift the conversation from the opioid crisis to maintain a focus on prevention, as well as how to address prevention from a multiple substance standpoint. Miller expressed that part of the problem with shifting the conversation is that the health care system is fragmented, and so prevention and treatment often are not considered together when addressing substance use. Shaw
added that there is a need for systems of care at each developmental phase based on known challenges and available data. He noted community coalitions can also help sustain momentum and advance efforts when government support may wane. Regarding the use of multiple substances, Estrada noted that there are common underlying risk behaviors among youth, and that addressing those and examining the common protective factors could be an opportunity to move away from the single drug approach to prevention.
Another participant wanted to better understand why some families engage with interventions and some do not. Estrada replied that when looking at predictors of engagement for their intervention, they found that families with youth at higher risk are more likely to engage, as are parents with low social support. Regarding the FCU, Shaw answered that in many of their settings, the families are already at a health care appointment and so were waiting anyway. It was easy to convince them to engage in a 30-minute session. He added that they are seeing strong engagement rates with their online and remote versions as well.
Related to the importance of infrastructure, a workshop attendee asked if there is available information on where specific interventions are being implemented. Miller commented a central repository that inventories all of the evidence-based interventions could be useful to communities, but she did not know if one exists.
BARRIERS TO AND OPPORTUNITIES FOR WIDESPREAD SCALE-UP
While many programs have been successfully implemented in individual sites or systems, broadening their impact comes with its own challenges. This section highlights family-focused prevention in integrated care systems, challenges to more universal programs, and general barriers to widespread scale-up of these types of programs.
Parent-Focused Prevention in Integrated Care Systems
Jordan Braciszewski, associate research scientist and clinical psychologist at Henry Ford Health, presented his work on introducing a parent-focused prevention program into three integrated health care systems across the country, including Kaiser Permanente Northern California, Kaiser Permanente Colorado, and Henry Ford Health. He said Henry Ford Health, one of the largest integrated health systems in Michigan, is unique because they have embedded health researchers in most areas of care, enabling teams to be nimbler during implementation and delivery of programs since they are already working together.
Braciszewski explained their prevention program, Guiding Good Choices for Health (GGC) was initially an in-person intervention focused on parents, but as the COVID-19 pandemic began, they pivoted to offering it virtually. There are now six virtual sessions attended by parents, and the children attend one of the sessions in the middle. They focus particularly on specific parenting skills and strategies for promoting bonding. Braciszewski shared results from randomized controlled trials that demonstrate GGC as an effective program in reducing use of alcohol, cannabis, and cigarettes, as well as reducing depressive symptoms and antisocial behaviors over time.
The two Kaiser systems and Henry Ford Health are conducting a cluster randomized trial of GGC, said Braciszewski. The focus of the trial protocol is on implementation outcomes, but they are also hoping to measure effectiveness of the intervention (Scheuer, et al., 2022). Braciszewski said they have been able to reach more diverse families, in terms of race and ethnicity and Medicaid status, and have received positive feedback from parents and providers throughout implementation.
While integrating a program like this into primary care can be difficult given the time limitations of appointments, Braciszewski explained that they have a programmer who, working through the electronic health record, is able to send a note to doctors with the names of patients they will see the following week who fit the age range for recommendation to the program. Because this has minimized the workflow required, he said, the uptake has been positive. Across the three systems, parents also report high satisfaction scores. He shared results from key stakeholder interviews, highlighting the positive feedback about being able to offer the program both in-person and virtually depending on the specific needs of the family.
Critical Challenges to Universal Substance Use Prevention Implementation
Justin D. Smith, associate professor at the Spencer Fox Eccles School of Medicine at the University of Utah, discussed some of the needs of community health centers and federally qualified health centers (FQHCs) that differ from those of better-resourced settings, such as Kaiser Permanente and Henry Ford Health. He explained that, while evidence-based interventions for prevention of substance abuse are available, they are not widely implemented—especially in primary care. However, Smith said, more than 95 percent of children in the United States have a regular health care provider, and nearly 93 percent have had a well-child visit in the last year. The setup of repeated well-child visits over time also offers multiple opportunities for delivery of preventive interventions and follow-up, he said. Smith shared a 2020 systematic review his team conducted that found only 40 individual programs met their criteria of having at least part of an intervention delivered through primary care with parenting as the target and child
health outcomes reported (Smith et al., 2020). None of the 40 programs reported substance use outcomes. Thus, Smith concluded, there is a need for research on implementation strategies for supporting the adoption and sustained delivery of parenting programs in primary care.
From both the scientific literature and his own experience, Smith noted four key implementation challenges: staff and workforce; time and space within primary care; funding issues; and framing of parenting-based prevention services. He reiterated earlier comments on issues of uneven supply and demand within the workforce, noting that most systems, especially those that are under-resourced, have very few behavioral health staff. Competing priorities can also make it difficult for patients seeking preventive services to access the staff they need, he added, especially when the staff are in short supply, because of the need to address more emergent mental health concerns (e.g., serious mental illness, suicidality). Even specialized behavioral health staff often lack adequate training in clinical psychology and may not be trained in specific skills for working with adolescents, Smith said, including the types of preventive and parenting skills that are the focus of this workshop. To address this in part, his team trains pediatric clinicians, nurses, and medical assistants.
Time and space are often in short supply with many of their partnering clinics, so Smith offers a different type of service delivery model. He described a recent trial comparing integrated/collocated care delivery models, both of which took place within FQHCs, with a referral-based model that refers families to a team providing a parenting intervention outside of the primary care system (Smith, Berkel et al., 2021). Within six months, they found the integrated/collocated care model would not be effective and was not sustainable. He said few families were referred, and those who were barely received services. While they had trained seven providers in these FQHCs, they just did not have the time to deliver the parenting program. Instead, Smith’s research team shifted to a full referral-based model for all FQHCs and other primary care practices and organizations. The referral-based model addressed the issue of lack of space to provide services (Berkel et al., 2021). In a second study with the same referral-based delivery strategy, Smith said, implementation moved from primarily home visiting to a fully telehealth model due to the COVID-19 pandemic, which also addresses the space limitations of the built primary care setting.
Economics drives much of the decision-making in implementation science and health care, Smith commented, and he called for a value proposition for preventing substance use. There are multiple perspectives to consider, such as cost-benefit analysis, cost effectiveness, or opportunity cost. Rather than looking at risk assessment and forecasting cost for the next year, which is not appropriate for a prevention program, Smith called for looking over several years to look at future costs and how those could
be saved (see Figure 3-2). Current alternative payment models may not provide adequate incentives for the transformation necessary to address those determinants of health care cost that lie outside current clinic workflows, he noted.
While there is often tension when moving interventions into real-world systems, Smith emphasized the importance of knowing that adaptation is expected and necessary, and implementing teams need to prepare for it such that adaptations are fidelity-consistent to the program (Smith et al., 2018). While this typically means the intervention shifts to fit the system, he said, there are also opportunities for the system to accommodate the intervention as well. He shared the idea of designing interventions from the outset to align with the end user’s needs, resources, capacities, and desires, which is called designing for dissemination and sustainability (Kwan et al., 2022). Finally, he concluded by emphasizing the importance of equitable implementation and taking into account such factors as the history of racial discrimination and inequitable access to health care (Smith, Davis et al., 2021).
Barriers and Opportunities in Health Care Settings
The family environment is a critical context for child health and development, said Pamela A. Matson, assistant professor of pediatrics at Johns Hopkins University School of Medicine. A core tenet of her work is understanding that promoting health for the parent also promotes health for the child and the entire family unit. She presented data from the Substance Abuse and Mental Health Services Administration (SAMHSA) showing that from 2009–2014 as many as 8.7 million youth were at home with at least one parent with an alcohol or illicit drug disorder. Household substance
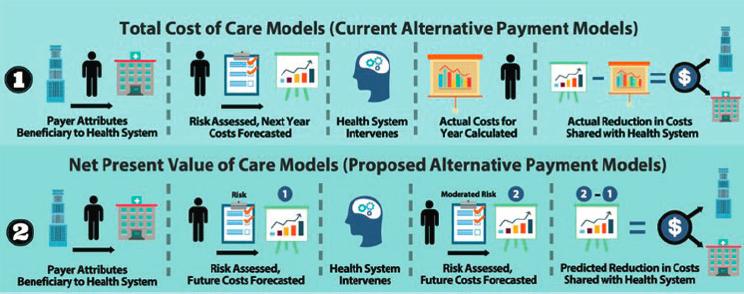
SOURCE: Smith’s presentation, May 5, 2022 (reproduced from Counts et al., 2019).
use disorder is considered an adverse childhood experience (Merrick et al., 2018). It also poses a more direct risk for young children, Matson said, with research showing that young children of parents with alcohol use disorders have higher health care utilization rates and increased risk of a variety of medical conditions (Ray et al., 2007).
As other speakers mentioned, Matson commented on the multiple barriers to screening during pediatric visits, including provider concerns about parent acceptability of screening. Matson and her team conducted a study in Baltimore to evaluate whether parents thought it was appropriate for a pediatrician to ask these questions. Overwhelmingly, parents responded that it was appropriate, and they thought pediatricians should ask such questions (Matson et al., 2022). Matson explained the results did not differ between parents who reported that they did have concerning substance use in the home and those who did not.
To implement screening on a widespread scale, Matson called for a multilevel approach. First, she said, pediatric providers have a responsibility to screen their patients and be aware of household substance use. However, pediatric providers are not expected to diagnose, manage, or treat substance use disorders in parents or caretakers. Pediatric residency training should focus on increasing comfort with and use of screening tools for household substance use, she said. Matson also suggested developing competencies in universal prevention programs, specifically increasing adoption of the evidence-based Screening, Brief Intervention, and Referral to Treatment.
Echoing previous speakers, Matson noted that time constraints are a critical issue for many providers. She suggested this can be partially addressed by optimizing screening into the workflow of primary care settings and incorporating standardized screening instruments into the medical records system, thus making it accessible and easier for providers to use. She also reiterated that a paradigm shift is needed to move pediatrics upstream, from a model of pathology and disease to a model focused on leveraging a range of prevention activities in primary care settings (see Box 3-1).
Finally, keeping in mind the multilevel approach, Matson advocated for policies and programs to support workforce development and sustainability. For example, she suggested a program similar to the National Institutes of Health loan forgiveness program for people who commit to pediatric and health disparities research. She suggested SAMHSA could establish a similar program for social workers or other professionals to incentivize greater participation in primary prevention programs. Noting that recommendations from the U.S. Preventive Services Task Force (USPSTF) would go a long way in supporting widespread scale-up of these types of efforts, Matson said more research is needed to make that feasible.
Discussion Session with Panelists and Workshop Attendees
The discussion began with a conversation around funding for implementation of intervention programs. Smith explained the two large grants they received were for implementation and coordination with primary care, but the grant pays for training and some services that are not reimbursable. Staff employed by Arizona State University provide the services through their coordinated referral-based approach, so they do not bill for services. He acknowledged this would vary by system. Braciszewski added that his experience was very similar in that their grant supports most of the services they are providing. However, they are hoping that having a health insurance plan owned by the health system will eventually lead to the ability to bill for these services.
Moving to the challenges in building an evidence base, one participant noted that the tension he experiences as a funder is that, while the USPSTF wants replication studies, funders are unlikely to want to fund a replica-
tion study. He asked about other study designs or intervention trials that could generate the evidence needed without being duplicates of existing programs. Smith acknowledged this challenge, saying there is some push-back because some family-focused interventions have not been tested in the pediatric primary care system, even though they have been successful in homes, schools, and online. He suggested the cumulative trial proposed by Hendricks Brown as a potential novel research design, in which as soon as there is evidence beyond reasonable doubt, you shift into replication within the same grant period. However, Smith said, they have pitched it a few times, but reviewers are hesitant and funders require more insight on what the second phase might look like.
Adding to earlier comments about supporting the workforce, Vincent Guilamo-Ramos, Duke University School of Nursing, highlighted the fact that most health promotion and wellness is delivered by the more than four million nurses in the United States. Comparatively, there are roughly 35,000 pediatricians in the country. He called for broadening the focus to leverage the entire health care team. Braciszewski agreed, and said to implement the GGC program widely they need to enlist nurses, medical assistants, and other support staff.














