6
NIH Current Approach to Strategic Planning for the Bethesda Campus Buildings and Facilities
This chapter describes the current National Institutes of Health (NIH) approach for strategic planning and capital project management, including the rationale and composition of capital projects on the Bethesda Campus, and a review of the completeness, accuracy, and relevance of cost estimates for proposed capital projects.
CONTEXT
Investment and NIH-Wide Strategic Plan for Fiscal Years 2016-2020—Turning Discovery into Health
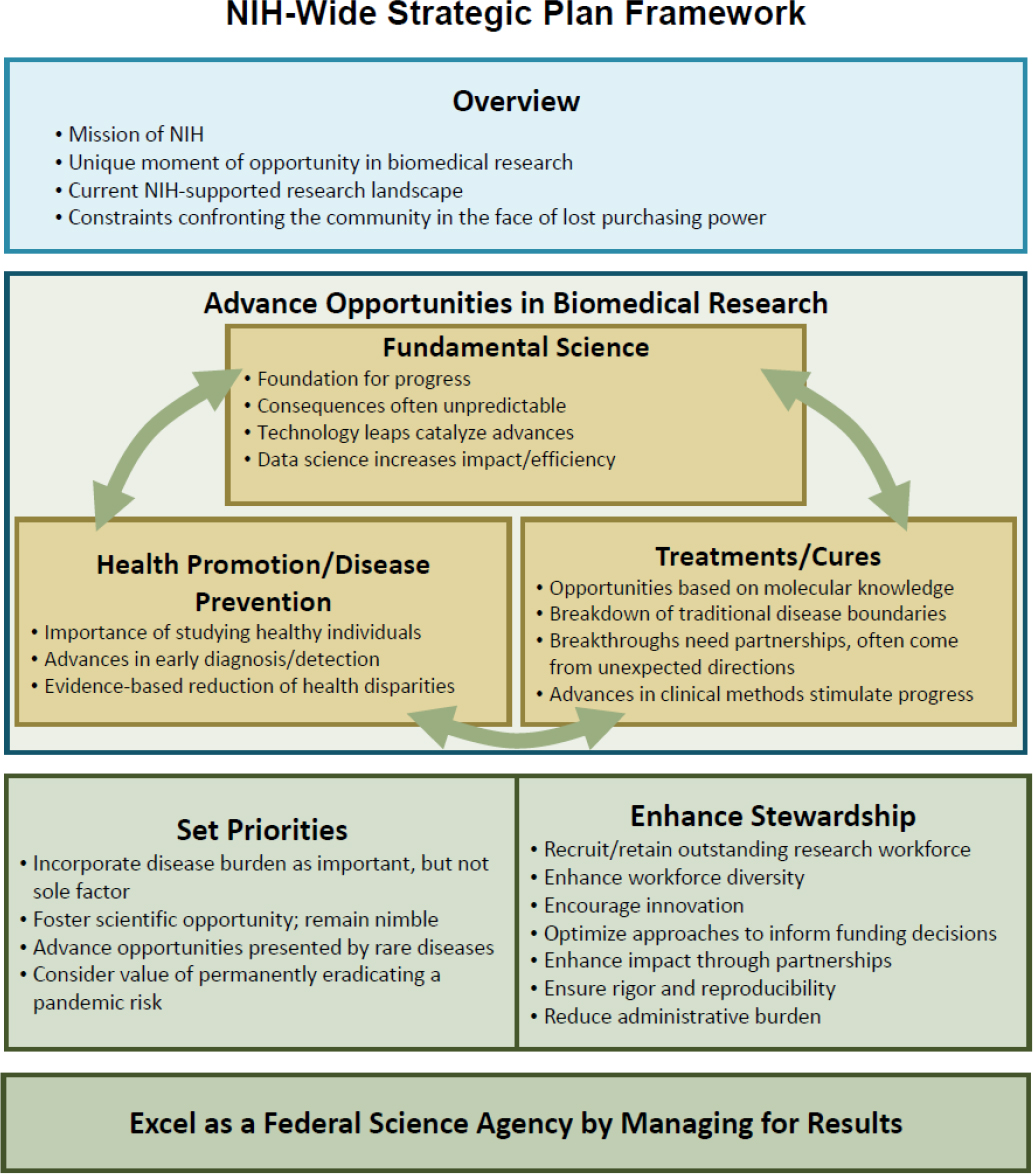
In 2015, NIH developed a comprehensive Strategic Plan designed to synchronize research program priorities and support forward-thinking decisions across the 27 institutes and centers (ICs) in response to the Congressional Consolidated and Further Continuing Appropriation Act of 2015 (P.L. 113-235, December 16, 2014).1 The plan was not to replace individual IC plans but to develop a framework (Figure 6.1) to ensure that scientific discoveries advance health and that NIH upholds its scientific stewardship responsibilities. The 2016-2020 research Strategic Plan has the opportunity to serve as the primary catalyst in the development of Bethesda Campus capital facilities planning.
NIH Mission and Research Goals
The NIH intramural research program facilitates high-impact science in a variety of ways, particularly the following:
___________________
1 NIH, NIH-Wide Strategic Plan Fiscal Years 2016-2020; hereafter “NIH-Wide Strategic Plan.”
- It encourages unique approaches to difficult research challenges, with frequent collaborations outside NIH institutions and scientists.
- It houses the NIH Clinical Center (CC), the world’s largest hospital dedicated solely to clinical research. The work of the CC links patient care with basic research discoveries and programs for the study of undiagnosed diseases and rare diseases and conditions.
The NIH-Wide Strategic Plan states that the mission of the organization is to “seek fundamental knowledge about the nature and behavior of living systems and to apply that knowledge to enhance health, lengthen life and reduce illness and disability.” In order to achieve this mission, the plan identifies four goals:
- To foster fundamental creative discoveries, innovative research strategies, and their applications as a basis for ultimately protecting and improving health;
- To develop, maintain, and renew scientific, human, and physical resources that will ensure the nation’s capability to prevent disease;
- To expand the knowledge base in medical science and associated sciences in order to enhance the nation’s economic well-being and ensure a continued high return on the public investment in research; and
- To exemplify and promote the highest level of scientific integrity, public accountability, and social responsibility in the conduct of science.
The Intramural Research Program (IRP) that supports the currently adopted NIH-Wide Strategic Plan goals includes the following:
- To prevent dire impacts on individual and community health,
- To retain a world-glass biomedical workforce, and
- To remain competitive in the global biomedical research environment.
NIH-Wide (Research) Strategic Plan
The four interdependent objectives outlined in the NIH-Wide Strategic Plan to achieve its mission and fulfill its stewardship obligation (see Figure 6.1) are as follows:
- Advance opportunities in biomedical research,
- Foster innovation by setting NIH priorities,
- Enhance scientific stewardship, and
- Excel as a federal science agency by managing for results. (NIH 2015b, p. 9)
While the NIH-Wide Strategic Plan calls out the need “to develop, maintain, and renew scientific human and physical resources that will ensure the nation’s capability to prevent disease,” that document does not identify any specific building or infrastructure facilities, space utilization policies, or capital investment strategies that will strategically support the growth and desire to be in more “nimble,” except through the annual Department of Health and Human Services (HHS) budget. It is unclear why the plan does not address the built environment, although it was suggested that because this is an enterprise-wide Strategic Plan, institutional facilities and capital needs were considered too minor of an issue to be called out. However, with respect to ensuring that NIH continues to prioritize the importance of capital facilities planning and reinvestment in existing capital assets, it was not evident to the committee that NIH leadership is aware that other major biomedical research institutions in the United States and internationally explicitly include specific capital investment requirements in their institutional strategic plans.
In addition, this committee did not see any evidence that NIH has developed strategic implementation plans or related capital asset plans that correspond to the NIH-Wide Strategic Plan. Most of NIH’s competitor research organizations develop and integrate short-term (0-3 years), mid-term (3-9 years), and long-term (10+ years) capital facility plans linked to strategic research plans within their implementation documents. Such strategic implementation plans usually include needed facility and infrastructure assets, including details in terms of size and capacity, cost, timeline, and location, and how the facilities align with
the research agenda. These proposed asset investments need to be analyzed and assessed on an ongoing basis, because rapid changes in science, fluctuations in funding and construction costs, changes in building conditions, and shifts in timelines all require that facility planning be tightly linked to short- and long-term research objectives. Developing proactive management practices that link strategic and facilities planning over time would help ensure that investments in facilities support the organizations’ mission and goals and that NIH can fulfill its scientific stewardship objectives.
As noted in the April 2016 Clinical Center Working Group Report to the Advisory Committee to the Director (NIH ACD, 2016), there was “inadequate attention to capacity and prioritization: There is little scientific prioritization across ICs, and this becomes particularly problematic in the case of shared resources” (p. 14). That report further noted that there was “no independent entity to verify that engineering controls for high-risk facilities meet appropriate regulations or standards prior to or after construction” (p. 17). The findings of the report are evidence that the types of risks assumed by leading-edge clinical research and hospital operations generally differ from those associated with biomedical research.
Long-Term NIH Intramural Research Program
Intramural Research Program Strategic Plan
As outlined in the Long-Term Intramural Research Program report by the working group of the NIH Director’s Advisory Committee (NIH ACD, 2014), the IRP’s long-term strategic goals are to train the next generation of scientists and to support large research efforts beyond what is reasonably achievable in the extramural community. Specifically, the NIH Director requested that the working group “identify areas of opportunity and uniqueness that should be enhanced within the IRP, as well as approaches to ensure the sustainability of the IRP going forward” (p. 1).
The working group developed recommendations in the areas of research, training, infrastructure and facilities, workforce, and administration. In the category of infrastructure and facilities, the working group recommendations were to (1) develop more robust programs with the extramural research community; (2) increase accessibility of all “core” resources such as the Clinical Center (including unique equipment); (3) develop data and computing capabilities; and (4) evaluate the feasibility of a centralized bio-bank (NIH ACD, 2014, p. 6).
The working group acknowledged that these objectives may require long-term investments, as well as the flexibility to change direction in response to new scientific discoveries or public health needs. The report also stated that the IRP has an important role in supporting the full integration of the NIH biomedical research effort. This integration will require changes in the IRP structure and culture to support team science and local, national, and international collaborations, and will require world-class state-of-the-art research facilities. The working group emphasized that facility and research infrastructure need to be integrated and optimized, especially given the cost of technologically advanced core facilities, research animal facilities, and a high-throughput computational IT infrastructure. In addition, the working group affirmed the commitment to maintain a state-of-the-art clinical research facility such as the Clinical Center.
Given the global competition to recruit, train, and retain an increasingly diverse scientific workforce, the report and several other NIH planning documents conclude that the IRP needs to build and support a biomedical research ecosystem that is second to none. Therefore, implementation of strategies to ensure that the organizational structure, culture, and capital planning efforts promote a physical work environment that continues to advance team science is needed. The proximity of the ICs within the Bethesda Campus and region and proposed close collaboration with the extramural national and international community together present a unique opportunity to ensure the nation’s continued global leadership in biomedical research.
MANAGING INVESTMENT
Comprehensive Master Plan—NIH Bethesda Campus
Four Priorities
In 2013, NIH developed an update to its 20-year Master Plan for the Bethesda Campus to serve as a tool for advancing NIH’s long-term scientific mission. The document was titled 2013 Comprehensive Master Plan—NIH Bethesda Campus (NIH ORF, 2013). During its discussions with NIH and its tours of the campus facilities and infrastructure, the committee observed that some aspects of the plan had been implemented, some revised, and still others not yet acted upon. The Master Plan identifies four priorities or strategies for implementation endorsed by the Facilities Working Group, which can be paraphrased as follows:2
- Advancement of NIH’s strategic research initiatives,
- Replacement of aging physical plant,
- Resolutions to regional traffic congestion, and
- Reduction of NIH’s leased facilities.
The 2013 Master Plan includes Master Plan Goals and Objectives. Goal I—“Foster innovative research to improve the nation’s health”—identifies six specific objectives associated with the long-term physical development on the historic Bethesda Campus:
- Establish a comprehensive and coordinated approach to physical development of NIH that is based on cost-effective, incremental options for growth while ensuring orderly development of the campus.
- Stimulate interaction and communications among scientists and staff to enhance quality of research and opportunities for interdisciplinary collaboration through adjacency of uses and creation of formal and informal meeting and gathering spaces on campus.
- Create a flexible development plan that will allow for changing program needs in the future.
- Organize campus into research clusters, which will aide in applying high-throughput technologies to understand fundamental biology, to uncover the causes of specific diseases; translating basic science discoveries into new and better treatments; and reinvigorating and empowering the biomedical research community.
- New research buildings proposed in the master plan will be multi-institute and flexible to facilitate the creation of centers of science such as the Porter Neuroscience Center and new Immunology Center to further scientific collaboration.
- Consider potential impacts of changes in technology and advances in research processes. (NIH ORF, 2013, p. 1-31)
However, the application of the six objectives will likely continue to challenge NIH’s current capital cost planning process due to the apparent broad and disorganized nature of planning requests received by the Office of Research Facilities (ORF), and in the future will likely require a more innovative and rigorous approach.
___________________
2 The four strategies as the appear in the plan are as follows: Optimize use of NIH sites to support science enterprise; provide safe, modern research space; sustain/improve existing facilities by modernizing assets; and plan to reduce lease space costs by utilizing government owned facilities (NIH ORF, 2013, p. 6-67).
Advancement of NIH’s Strategic Research Initiatives
As stated in the Master Plan, “NIH’s mission is to seek fundamental knowledge about the nature and behavior of living systems and the application of that knowledge to enhance health, lengthen life, and reduce the burdens of illness and disability.” The Master Plan’s vision is to promote scientific collaboration by organizing the campus into research clusters which will facilitate
- Applying high-throughput technologies to better understand fundamental biology and uncover the causes of specific diseases;
- Translating basic science discoveries into new and better treatments; and
- Reinvigorating and empowering the biomedical research community. (NIH ORF, 2013, p. i)
Although NIH does not anticipate significant growth in its science programs in the next 20 years, it does project changes in biomedical research that will require greater scientific collaboration across disciplines. This will require that research facilities be multi-institutional and flexible. It is anticipated that the creation of additional centers of science, such as the Porter Neuroscience Center and the new Immunology Center, will need to be constructed to enhance scientific collaboration. It is also projected that there will be more need for computational and systems biology facilities. These projected changes in science should drive the design and location of NIH’s new and renovated biomedical research facilities.
Replacement of Aging Physical Plant and Reduction of NIH’s Leased Facilities
Since NIH ICs do not expect to expand scientific programs, personnel, or space in the next 10 years, the Master Plan addresses two additional priorities: replacing its aging physical campus and reducing operating costs by reducing the number of leased facilities.
In addition to developing a campus Master Plan that addresses future scientific goals, the Master Plan also highlights the needs of an aging physical plant where existing facilities over the next 20 years may no longer be able to support the organization’s scientific mission. NIH uses several independent assessments to evaluate the physical conditions of the campus’s facilities, including the following:
- The Federal Real Property Council’s Performance Measures to evaluate its existing facilities with respect to mission, utilization, operating cost, condition, and disposal/remediation;
- The NIH Buildings and Facilities Model to aid in evaluating program impact, functional obsolescence, and facility impact; and
- Sustainability goals and sound stewardship practices, such as adapting and reusing historic buildings.
Based on these assessments, NIH estimates that 11 percent of gross square feet (GSF) of its research square footage marginally accommodates existing research needs and 5 percent is obsolete. These older research buildings’ structural systems and configurations cannot be readily updated to accommodate current research space as currently configured and mechanical systems requirements.
The Master Plan also addresses the federal requirement that all agencies strive to reduce the number of leased facilities to reduce operating costs. Therefore, the plan includes strategies to renovate outdated research facilities and build new administrative space to accommodate employees residing in leased space on campus.
Resolutions to Regional Traffic Congestion
The Master Plan also gives high priority to addressing the region’s traffic congestion. While NIH’s employee growth has contributed to the traffic congestion, the Bethesda Central Business District (CBD)
and the Friendship Heights CBD have grown still faster. The Master Plan includes the Transportation Management Plan, which outlines short- and long-term strategies to mitigate traffic congestion.
Implementation of Four Priorities
To address the above-mentioned priorities, contingent on future budgets, opportunities, and policy, the Master Plan outlines the following solutions.
Research
- Organize the campus into five research clusters to facilitate and nurture collaboration and create opportunities for development of multi-institutional centers and address other trends such as computational biology.
- Accommodate leased laboratories and the lack of modern research facilities by constructing 1.6 million GSF of research space. Five of the new buildings are planned to house intramural research.
- Stabilize 500,000 GSF of space in the old Clinical Center complex to prepare it for adaptive reuse, in addition to the 2,900,000 GSF already scheduled to be renovated.
- Replace housing and care facilities for animals with state-of-the-art facilities that satisfy modern design, accreditation, and program requirements.
Administration
- Bring all administrative functions back to the Bethesda Campus and reduce operating costs and enhance scientific collaboration.
- Construct 775,000 GSF of administrative and support space and three new parking garages.
Utilities
- Continue the upgrade and modernization program for utilities and infrastructure, particularly the central heating and refrigeration plant, campus steam, chilled water, and electric power distribution systems.
- Consolidate utility support and service functions in proximity to Building 11 and to the far south end of the campus.
Campus Environment
- Cluster administrative and biomedical research education functions in close proximity to the Medical Center Metro Station.
- Construct expanded childcare facilities and other amenities, including small-scale retail and food services.
- Enhance the natural buffer zone around the periphery of the campus by removing surface parking and increasing landscape plantings.
- Reduce pedestrian conflicts by constructing elevated pedestrian walkways and tunnels, and build parking garages within a 5-minute walking distance to employees’ workplaces.
- Enhance the Bethesda Campus environment by creating a series of development guidelines.
- Continue to develop a Transportation Management Plan that outlines short- and long-term strategies to mitigate the projected campus workforce increase of 3,000 employees and contractors.
NIH 2013 Comprehensive Master Plan—Bethesda Campus and Integration with the NIH-Wide Strategic Plan for Fiscal Years 2016-2020
As NIH implements its Master Plan, a few items should be considered to ensure that the plan remains relevant and adds long-term planning value to the institution. Establishing integrated proactive management practices that link the institution’s Strategic Plan and facilities planning efforts could facilitate timely updates and success of the plan.
Changes in Research Strategic Goals
The 2013 Master Plan incorporates the goals and objectives of NIH-Wide Strategic Plan. As the Master Plan is implemented, it will be important to ensure that it continues to reflect and adapt to changes in NIH’s strategic goals. As stated in Chapter 2, science is changing at a rapid and unpredictable pace. These ongoing changes will affect NIH’s existing programs, organizational structures, budgets, workforce, and myriad other elements, resulting in the need to periodically reassess the strategic initiatives and reconsider their effects on the plan. Because many of these changes may result from unforeseen national and global factors, the committee believes that input from both internal and external experts would be beneficial.
Space Utilization
Continuing to optimize space utilization of existing and new facilities is critical to long-term planning. As technology changes, existing standards for laboratory, research support facilities (e.g., animal facilities), and administrative space will change. The existing process that allocates space to separate ICs will make it increasingly difficult to assess whether space is optimally used and to develop long-term space need projections. While NIH is projecting no increase in its research programs for the next 20 years, annual reassessment of space utilization is necessary to optimize the daily use of facilities, identify swing space, and project long-term facilities’ needs.
In addition to developing long-term plans for animals and data facilities, a plan for the Clinical Center might be beneficial. Over the next 5 to 10 years, the nature of the patient care and research activities may change significantly, and the Clinical Center’s capabilities will need to adapt, especially if the type of patient volumes change (such as the trend toward increased outpatient care), and if external collaborations increase.
Given the space utilization and planning challenges to the current Bethesda Campus, NIH might consider multiple different approaches to accommodate increases in on-campus space needs. For example, given the scale of leased space across Montgomery County and in adjacent areas currently and over the next 5 to 10 years, NIH might consider increasing the building density on the Bethesda Campus, collaborating with nearby organizations (e.g., the Walter Reed National Medical Military Center), or accessing nearby land to enable an extension of the NIH Bethesda Campus operations, ensuring easily accessible and reliable transportation between the new area and the historical site.
Increasing Partnerships
Partnering with other public and private organizations has been identified in the NIH-Wide Research Strategic Plan as a high priority. It was noted that increased partnerships would not only enable NIH to make maximum use of finite resources but they would also advance science and help fulfill NIH’s mission. Strategies were identified in the Strategic Plan to continue to advance transdisciplinary knowledge and foster new collaborations through partnerships. Therefore, it is important that the Master Plan have the flexibility to address items such as increases in clinical facilities, access to high-end instrumentation/core
facilities, temporary utilization of laboratory facilities by external researchers, and current constraints imposed by existing security measures.
Surrounding Community
As outlined in the Master Plan, changes in the surrounding community will continue to affect the Bethesda Campus. The community’s strategic goals, corresponding NIH Master Plans, and population growth projections for the region will impact the campus. As articulated in the plan, the positive economic growth of the surrounding business communities has resulted in housing and traffic congestion. It is essential that NIH continue to build relationships and partnerships with the community to address these issues and to monitor changes over time. These relationships are beneficial in resolving community concerns, including the impacts of increased capacity, construction, noise and pollution.
Along these lines, there also has been very strict security instituted around the Bethesda Campus in response to the September 11, 2001, terrorist attacks. Unfortunately, the security measures generally exclude public access to the National Library of Medicine and the Natcher Conference Center, even though these entities are uniquely public-facing. Planning could examine new alternatives to ensure easy public access to resources on the Bethesda Campus to enhance relationships with the community.
Funding
The Master Plan and the NIH-Wide Research Strategic plan report that the lack of funding for strategic and facilities initiatives has hampered and will continue to hamper short- and long-term facilities planning and implementation on the Bethesda Campus. Therefore, it is essential that the Master Plan and NIH’s capital plans—the Buildings and Facilities (B&F)/Nonrecurring Expense Fund (NEF)-Funded 5-Year Plan) be flexible and capable of adjusting to capital funding and priority shifts. (The funding appropriated for NIH does not ring-fence or otherwise separate capital budget dollars from operating budget dollars.) In addition to submitting requests to Congress for capital and renovation dollars, NIH could, the committee believes, continue to explore alternative sources of funding such as private development funds,3 public-private partnerships,4 and joint federal projects to increase funds needed to address critical master planning issues.
A key challenge for the future built environments of all biomedical research enterprises is how to best integrate strategic programmatic objectives in the context of perpetual limited capital resources, the need for efficient space utilization, and the severe challenge of accelerating deferred maintenance of building systems and site infrastructure. These facility and infrastructure assets are key to effectively supporting the research enterprise as it grows and changes, and as it continually adapts to changes in local and regional physical planning constraints in concert with the key regulatory and compliance requirements.
Leading academic and other research organizations increasingly integrate planning for operating and capital resources, since those organizations must now conduct appropriate financial due diligence, establish long-term planning horizons, and engage in much more rigorous cost/benefit analytics related to a total cost of stewardship perspective. These organizations leverage the value of every dollar through emphasizing highly functional and productive research and instructional environments, energy efficiency, staff and faculty operating efficiencies, institutional carbon reduction, and other sustainability and disaster resilience objectives. The values of these elements are explicitly estimated and verified at each stage of the planning, design, renewal, and replacement processes for every facility and infrastructure asset.
___________________
3 See, for example, The Children’s Inn at NIH, “Corporate and Foundation Partners,” https://childrensinn.org/get-innvolved/corporatepartnerships/, accessed July 23, 2019.
4 See, for example, NIH, “Accelerating Medicines Partnership,” https://www.nih.gov/research-training/accelerating-medicines-partnership-amp, accessed July 23, 2019.
A longer, 10-year capital plan for NIH—currently there is the B&F/NEF-Funded 5-Year Plan discussed in Chapter 4—would have the opportunity to represent the long-term aspirations of the organization, including researchers, staff, and stakeholders. A successful long-range capital plan typically incorporates a flexible (not site specific) land use regulatory framework affecting a research campus, integrated with the institutional strategic scientific plan developed by the senior leaders of the research enterprise. To remain nimble in the scientific research environment, the built environment must remain equally nimble and flexible so that it can appropriately respond to future opportunities.
Capital Repair and Improvement—Current Reinvestment Approaches
The current NIH capital federal appropriation strategy, as an Operating Division of HHS, is to increase capital reinvestment resources to “repair,” or for “repair-by-replacement” (HHS, 2006, pp. 1-17), or for “improvements (Renovations/Alterations)” (pp. 1-11), or for a hybrid plan that may regularly combine some of each on an ongoing basis. As stated previously, the normal life expectancy for major building systems such as mechanical, electrical, and roofing is approximately 30 years. Due to the limits and inconsistency of federal funding availability, the replacement of many of these systems on the Bethesda Campus has been deferred—creating a significant and growing backlog of capital assets reinvestment or a decision to replace or remove the capital asset. These reinvestments are defined in the HHS Facilities Program Manual Volume I and are identified as “repair and improvement” capital funding requests, as opposed to “maintenance and improvements” requests. Line item projects (construction, improvements, or repairs) are also requested, which may, if funded, contribute to the reduction of the Bethesda Campus deferred maintenance backlog.
At this time, the ORF manages multiple federal funding sources annually for these types of capital reinvestments to sustain the Bethesda Campus research enterprise. (See the discussion in Chapter 4, in section “Funding for Capital Projects.”) Based on information received from ORF staff during open session presentations to the committee on September 25, 2018,5 with additional details provided to the committee subsequent to the presentation, it appears that the ORF identifies and prioritizes specific repair and improvement projects annually, and perhaps as often as quarterly, based on regular meetings among ORF maintenance and operations subject matter experts and other technical staff.
The current tactical management approaches to reduce the deferred maintenance backlog include (1) increasing capital funding requests with a focus on supporting the current annual building system replacement prioritization plan; (2) continuing comparative financial and related cost-benefit or “highest and best use of limited capital resource” evaluations of renewal versus replacement of buildings (for example, continue to “improve” portions of individual buildings by focusing on a 5-year-plus planning approach, versus deferring improvements in multiple buildings based on probability of building replacement in future years); or (3) continuing reinvestment in the campus site infrastructure by use of energy and other utility cost savings or cost avoidance strategies. In Chapter 4, the committee nonetheless recommends first funding long-term infrastructure projects from among the list of such already identified by NIH and totaling approximately $700 million (see Recommendation 4.1).
Current Capital Cost Planning at NIH-BC
Cost estimating and planning for high-performance biomedical research facilities and infrastructure is increasingly being scrutinized at leading research organizations. Due to the high capital costs associated with developing major new research buildings, efforts to avoid or defer significant new capital and
___________________
5 Jim Lewis and Dan Cushing, NIH Office of Research Facilities, Question and Answer session with the committee, September 25, 2018.
operating costs to operate and maintain the new facilities are active; these efforts are described in an Education Advisory Board study as “breaking the cost-to-grow curve.”6
Leading research organizations are also exploring different strategies to better manage capital and operating cost expenditures for new facility and infrastructure assets. The August 2017 consensus study report of the National Academies of Sciences, Engineering, and Medicine, Strengthening the Disaster Resilience of the Academic Biomedical Research Enterprise: Protecting the Nation’s Investment (NASEM, 2017, p. 311), noted
Two recurring capital cost reduction strategies in the academic research enterprise have been increased research space utilization or the redesign of existing research space to improve productivity outcomes. There is also renewed focus on the adaptive reuse of existing research or nontraditional research facilities, particularly for those research programs with a demand for more computational space and less wet laboratory space, programs desiring more open office space, or programs shifting from the bench to share core research facilities.
As noted earlier, the document, 2013 Comprehensive Master Plan—NIH Bethesda Campus (NIH ORF, 2013), specifies in Goal I the need to “Foster innovative research to improve the nation’s health.” The last two objectives in that goal (i.e., multi-institute, flexible new research buildings and adaptability to changing research processes) suggest that the needed facilities and infrastructure will require more in-depth planning and costing due diligence to enable nimble shifts in facility and space configurations. Among other factors, these new facilities will require consideration of structural flexibility, as well as the adaptability of information technology services and thermal management infrastructure. The requirements for these high-performance laboratories and work environments are often state-of-the-art, and therefore have limited cost data benchmarks in the industry. In contrast, standard or traditional building designs can use widely available cost data and benchmarks using common parameters (such as cost per square foot or linear foot) that can be applied during the earliest design development. A major challenge for cost planning for the NIH state-of-the-art facilities is the lack of available cost benchmarks during the earliest design phases and under limited investigation of the specific conditions of the proposed capital project.
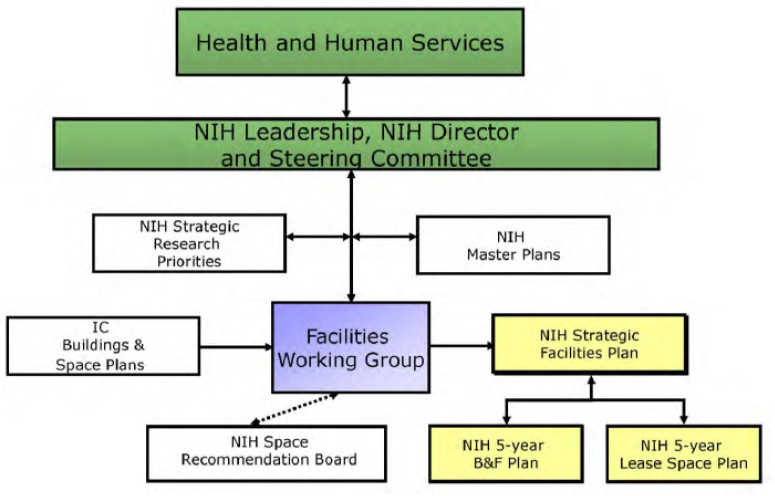
Current NIH IRP project-specific capital cost models appear to be prepared in response to requests received from a wide range of sources within the Bethesda Campus and from NIH facilities located off-campus. Figure 6.2, “Facilities Decision-Making Process,” excerpted from the 2013 Comprehensive Master Plan—Bethesda Campus, characterizes the multiple and complex planning pathways in place for the NIH Intramural Research enterprise (NIH ORF, 2013, p. 6-66). The diagram raises questions about the ongoing decision-making procedures, particularly to establish and enforce priorities and adjudicate disputes.
In general, the ORF responds to the cost model requests from the Facilities Working Group (FWG), the Space Recommendation Board, and individual ICs. The early project cost planning processes appear to be funded by (1) an individual IC or IC program; (2) ongoing HHS authorizations for B&F; (3) the HHS NEF; or (4) the ORF annual operating budget. The Office of Research Facilities’ Division of Facilities Planning, among many other responsibilities, also develops the NIH Lease Space Plan, the NIH Strategic Facilities Plan, and the Building and Facilities (B&F) budget plan. The FWG is described further in Chapter 5, in the section “Process by Which Projects Are Planned and Evaluated.”
The ORF appears to provide cost projections for all projects included in the regularly evolving NIH Condition Index, Sustainment, and Improvement Funding Needs Plan, and approved NEF-funded7 campus-wide transportation, utility, and information technology infrastructure improvement projects, which appear to be a significant portion of capital cost projection activity. These cost estimates are needed throughout the year, and particularly when the B&F funds are allotted quarterly.
___________________
6 Education Advisory Board, “Maximizing Space Utilization,” https://www.eab.com/research-andinsights/academic-affairs-forum/studies/2010/maximizing-space-utilization/the-space-utilization-imperative/breaking-the-cost-to-grow-curve, accessed February 6, 2019.
7 This source of monies is described further in Chapter 4, in the section “Funding for Capital Projects.”
Uncertainties and risks in capital planning for state-of-the-art research facilities include the higher cost than typical buildings, the lack of easily available standardized cost benchmarks, and complex capital cost planning requests. For these reasons, the ORF should consider establishing a clear and consistent annual schedule for review of capital project priorities and estimated costs.
NIH Bethesda Campus Project Capital Cost Factors
Underlying the NIH capital project cost assumptions are the critical issues related to complying with the requirements of the National Capital Planning Commission, the National Historic Preservation Act, Executive Orders, HHS plans, Principles for Federal Leadership in High-Performance and Sustainable Building, Fire and Life Safety, and the other national model building codes and standards (including seismic performance improvements and special provision for seismic loads in the research environment) and significant interagency federal security protection design requirements. Other core assumptions used by NIH for each capital project cost model include (1) appropriate construction cost escalation factors to midpoint of the projected construction schedule; (2) a traditional design-bid-build construction procurement strategy (not potential alternative project delivery systems, including design-build, construction manager at risk, or cost-plus type construction delivery agreements); and (3) owner contingency factors, which are variable based on each level of the project planning phase completion.
It is also important to note the geographic factors in the Washington, D.C., metropolitan area, which may impact design and construction delivery costs due to marketplace conditions regarding the volume and timing of regional construction activity and impacts of specific labor availability and cost. Of special note, NIH-owned facilities are required to follow the latest requirements of the NIH Design Requirements Manual (DRM)8 for new or renovated biomedical research and animal care facilities. The NIH DRM includes prescriptive requirements that intend to enhance the safety, energy efficiency, and indoor air
___________________
8 NIH, 2016, Design Requirements Manual: Biomedical and Animal Research Facilities Design Policies and Guidelines, https://www.orf.od.nih.gov/TechnicalResources/Pages/DesignRequirementsManual2016.aspx.
quality, as well as support cost-effective maintenance and improved building systems life cycles, while maintaining operations of biosafety level 1-4 facilities, animal care facilities, and tanks during normal conditions.
The 2016 edition of the NIH DRM also contains specific provisions for improving the resilience of the built environment during disasters—including utility service disruptions—by requiring a project-by-project risk assessment that considers the consequences of systems failures and development of appropriate and affordable mitigation actions. The provisions include a wide variety of requirements related to facility location, arrangement of space, location of critical equipment and utilities, and fail-safe control systems with the goal of mitigating the potential loss of critical building systems services loss in the clinical, laboratory, or animal care facilities.
According to material provided to this committee, NIH appears to have higher cost adjustment factors than many of its peer institutions due to a range of factors, including the location construction cost factors in the Washington, D.C., metropolitan region, and NIH and federal compliance requirements noted above. The committee believes that this makes a compelling case that NIH will have construction costs higher than those of other organizations not so constrained.
Capital Project Cost Projections—When Are Projections Provided?
The HHS Facility Project Approval Agreement (FPAA) documents a specific capital project with a concise summary of information, including projected cost. This agreement, if funded in the annual HHS capital budget submission, serves as the basis for a future commitment by NIH to meet the requirements noted: scope, schedule, capital cost project, and narrative justification.
The deliverable for the “Pre-Project Planning Phase” by the NIH ORF’s Division of Facilities Planning provides the data and information for inclusion in the NIH final FPAA Form 300 submission. The Facilities Working Group determines the annual recommendations for funding. FWG’s recommendations are forwarded to the IC directors, who review the FWG’s capital projects recommendations at an annual budget review meeting. It appears that the FWG, in concert with ORP, directs the level of cost model development completed or to be completed by the ORP Division of Facilities Planning based on three categories:
- Projects having sufficient information with a “program of requirement’s” (POR) and cost estimates to be considered for funding in an annual B&F Plan.
- Projects that are being studied in a current fiscal year that could be proposed for design in the next annual B&F Plan. Priority dictates the order in which the POR and cost estimates are completed.
- Projects that need further study before they are ready to be designed. Priority dictates the order in which studies are accomplished. (NIH ORF, 2013, p. 6-68)
The FPAA Form 300 is not a detailed cost estimate and represents only a concise one-page summary of more detailed cost projections including direct construction costs, construction cost escalation, construction contingencies, and indirect costs (including design consultant services, land acquisition costs, permitting and associated regulatory costs and fees, furnishings-furniture-equipment, project management costs, and project contingencies).
Table 6.1, provided by ORF staff, is intended to identify prioritization scoring as well as status of current preplanning actions. The table identifies three proposed capital project categories9 for NIH’s “Projects Proposed in Building and Space Plan Process in Spring 2017”: Section A: Complete POR, EIS, and IGE; Section B: Incomplete POR, EIS, and IGE; and Section C: Minimal Definition. Neither project capital cost projections nor potential fund sources were included in this Scoring Table as a decision making component when this blended prioritization and planning status table was created in spring 2017 by the ORF.
___________________
9 These categories, as well as the scoring and ranking system that populations them with projects, is described in detail in Chapter 5, in the section “Process by Which Projects Are Planned and Executed.”
TABLE 6.1 Projects Proposed in Building and Space Plan Process in Spring 2017
| Campus | B&F Line Item Projects | B&F Section | Proposing IC |
|---|---|---|---|
| Section A: Complete POR, EIS, and IGE | |||
| BC | Addition to the CRC to house Surgery/IR and RADIS/DLM—construction | A | CC |
| BC | Center for Disease Research (including vivarium to replace Building 14/28) | A | ORF |
| BC | Electrical power reliability for the Clinical Center | A | ORF |
| BC | Renovate building 6A as office, once empty | A | ORF |
| FC | Integrated Research Facility—construct a 271,000 GSF consolidated vivarium facility for relocation of animals and employees from 32 buildings to house the NCI research colonies and animal research support services at Frederick; also construct new utility plant at the south portion of the campus | A | NCI |
| RML | ORF/ORS/NIAID support building | A | ORF/ORS/NIAID |
| RTP | Site utility loop—construct | A | ORF |
| BC | Replace Clinical Center patient and visitors parking | A | ORF |
| RTP | Computational Science Building | A | NIEHS |
| RML | Comparative Medicine Center | A | NIAID |
| BC | Addition to Vaccine Research Center (Building 40) | B | NIAID |
| Section B: Incomplete POR, EIS, and IGE | |||
| BC | Building 10 West Distal Wing (H&J) renovation | B | ORF |
| BC | Building 10 East Distal Wing (A, B, C, & D) renovation | B | ORF |
| BC | Building 10 ACRF renovation | B | ORF |
| BC | Additional cell processing | B | ORF |
| BC | Convert G Wing to clinical offices | B | ORF |
| BC | Building 31 replacement, waste management facility, grounds maintenance, police station, parking structure, and associated infrastructure projects | B | ORF |
| BC | Renovate Building 1 | B | ORF |
| BC | New South Laboratory, adaptive reuse of Buildings 4, 5, 8, 30, and 41; Frederick, new parking structure, and associated infrastructure projects | B | ORF |
| BC | New Central Laboratory and associated infrastructure projects | B | ORF |
| RML | BSL-2 and 3 Research building (combination or previously requested research space) | C | NIAID |
| BC | New/expanded NIH Data Center for expanded scientific computing | B | CIT |
| Section C: Minimal Definition | |||
| BC | Renovate Building 29A as lab and animal facility | C | ORF |
| FC | Construct a 268,000 GSF laboratory facility to house the current and developing research/clinical programs to replace aging and outdated laboratories in Frederick | C | NCI |
| BC | Renovate Building 29 as computational/dry lab | C | ORF |
| BC | Continuing requirement for an additional MRI bay in the Clinical Center | C | NINDS |
| BC | In future Building 45 addition, provide future NCBI space requirements for staff growth and expand collections space to accommodate growth of collection material, driven by the increase in genomics research and high-throughput technologies | C | NLM |
| FC | Construct a 288,400 GSF four-story parking garage on the north portion of the | C | NCI |
| Frederick Campus to support the current and developing research/clinical programs | |||
| BC | New construction/addition to facilitate round-robin renovations in Building 10 | C | ORF |
| BC | Central quadrangle | C | ORF |
NOTE: Acronyms are defined in Appendix K.
Capital Project Cost Projections—Accuracy and Relevance
The capital cost for a project, above and beyond the value of the project to advancing the scientific mission, is a critical determinate in a research institution’s decision to pursue funding.
Cost planning is a rigorous discipline and requires large volumes of current data and senior-level professional expertise to achieve a high level of accuracy. Regardless of the phase of the design and construction process—from early conceptual predesign to a design that is poised to be competitively bid—cost matters to all parties. Effective capital cost planning represents a reflection of an institution’s credibility and viability. The example of cost planning for capital projects by the Bureau of Reclamation is discussed in Box 6.1.
To respond to the committee’s charge to evaluate at a high level the completeness, accuracy, and relevance of cost estimates at the Bethesda Campus, the ORF provided the committee with approximately 70 conceptual capital budget documents (as defined in the May 19, 2006, HHS Facilities Program Manual Volume I (HHS, 2006) as “preproject planning”-level materials) associated with proposed NIH capital projects. However, these documents are not considered detailed cost estimates because they contain limited details on the scope of the proposed capital construction, limited references to sources of the direct construction costs (professional cost planners, architects, RSMeans, or the Department of Defense Cost Estimating Guide, or other), or detailed construction costs based on recognized Uniformat or CSI cost model formats.
The committee concluded that the preproject capital planning documents, in general, appear to be prepared by ORF staff consistent with the following: (1) current HHS Facilities Program Manual Volumes I and II for “Costing Repair Needs” or “Opinions of Cost” (HHS, 2006, pp. 2-30 and 2-36); (2) Department of Energy GP Checklists; (3) additional HHS Facilities Program Manual required documents, including Project Definition Rating Indices; (4) Project Delivery and Contract Strategy evalulations; (5) NIH Nonrecurring Expense Fund Project Budget Justification narratives; (6) Appropriation/Obligation Budget summaries; and (7) an NIH ORF “Capital Cost Template” based on a basic Microsoft Excel spreadsheet.
The sample of NIH preproject planning capital cost, scope, and schedule planning documents provided to the committee indicate the use of consistent general capital cost categories defined by the HHS Facilities Program Manuals and included, if required, at a summary level in the HHS Form 300—Facility Project Approval Agreements (FPAA). Use of the HHS Form 300—FPAA is mandatory for Deputy Assistant Secretary for Facilities Management and Policy [DAS/OFMP] or HHS board-approved projects. The NIH Director has received the delegated authority and is responsible for the approval of construction and improvement projects under $1,000,000, and all repair projects under $3,000,000 (HHS, 2006, p. 2-1).
These summaries serve as the critical NIH capital budget request submission document reviewed during the annual HHS Capital Facilities Review Process: “The FPAA will serve as the project justification, and as such shall be submitted as part of the HHS budget formulation process” (HHS, 2006, p. 2-2). Individual FPAA project “Deviation” and “Revision” submissions are also regularly provided by NIH as part of the HHS Capital Facilities Review Process by use of the form “Changes to Facility Approval Agreement” (HHS, 2006, p. 2-10).
An objective comparative review of the cost planning-related documents provided to the committee indicates compliance with the broad categories of total project cost requested by the FPAA. However, the FPAA capital cost information appears to be informed, as noted earlier, from multiple, different, and potentially inconsistent data sources as noted in an ORF “Capital Cost Template.” This total capital project cost template is typically developed by the ORF project officer, often with the support of consulting professional engineers, architects, and construction and equipment cost planners.
Inconsistent metrics appear to exist within key NIH Capital Cost Template cost model line items. These inconsistencies do not appear to be based on typical variables, including geographic factors (e.g., seasonal or clinical or research operation schedule requirements or labor conditions impacts), construction cost scale of a project, project duration due to construction or regulatory entitlement processes, capital cost escalation factors, project complexity, construction phasing, acquisition of major equipment components, or other variables among individual capital projects.
Key inconsistent metrics within the NIH Capital Cost Template include the application of discrete and benchmarked annual escalation and geographic variability factors, the project design and construction contingency factors, “building commissioning” (Cx) and information technology systems and support (i.e., communications and information technology) factors, major fixed and movable equipment market-rate cost projections, and construction quality control and management factors, among others. These inconsistencies, particularly with the application of large project contingencies, are often a consequence of insufficent clarity of project scope and schedule during the preplanning process.
The NIH ORF Capital Cost Template for the Bethesda, Rocky Mountain Laboratory, and other IRP sites serves currently as the critical baseline financial planning document utilized by NIH staff who are most directly responsible for leadership and management of the preplanning phase capital cost model. The degree to which these total project cost models are accurate and comprehensive at the preplanning stage of a project may ultimately represent NIH’s leadership commitment to the scientists, staff, patients, and the nation by providing the most informed, credible, and defensible financial projection of each project’s capital need to sustain NIH’s missions. Clear decision making at these early planning stages has been demonstrated to be extremely important in mitigating finanical (e.g., budget, scope, and schedule) risks for individual capital projects while concurrently enhancing insitutional capital financial management credibility. Best practice evidence in capital project management typically identifies the critical role played by a rigorous, integrated, and comprehensive design preplanning process—successfully represented in the POR deliverable—as fundamental to successful investment of capital that will create the functional and inspirational built environment to enhance innovation and collboration within the research enterprise. The successful integration of scientific program leadership with the built-environment technical subject matter experts often begins at this first and earliest stage of the capital project planning process. The committee’s findings regarding the planning process and the completeness, accuracy, and relevance of the cost estimates appears at the end of the chapter.
Context for the Critical Importance of Accurate, Comprehensive, and Integrated Capital and Operating Cost Planning
Following recovery from the Great Recession of 2008, the trustees of many public and private academic biomedical research institutions adopted financial sustainability action plans, created detailed capital investment master plans, and integrated the two into one comprehensive financial plan (Motley, 2012). The integration of these traditionally separate budget-planning processes was recognition that institutional financial health is the critical prerequisite to sustaining excellence, innovation, and discovery within the research enterprise. Integrating the facilities and space needs of multiple schools, departments, or, for NIH, institutes and centers, into one comprehensive financial annual planning and forecasting process offers the opportunity to create more transparent and rigorous criteria for financial (operating and capital) resource allocation prioritization. The committee believes that the development and application of consistent and credible capital cost data is critical to sustaining the NIH intramural research program’s short-, mid-, and long-range capital plans.
To create a credible and useful capital financial planning framework for specific potential capital projects, capital planning experts typically seek as much accurate and complete information as possible regarding the research program’s activities from the specific research program leaders (termed by the ORF as the program of requirements, or POR), benchmarking equivalent programs at different research institutions, and informal or formal peer reviews through site visits and other investigations. The translation
of a research program’s activities at a preliminary and early stage of development into a built environment that does not yet exist is extremely challenging, but critically important to the capital plan’s institutional prioritization processes. Not all “proposed” scientific initiatives/projects and their potential space and infrastructure needs can be subject to lengthy and costly (in terms of both scientific staff time and dollars) assessment; at the same time, there must be sufficient information to allow the institution to credibly identify and evaluate the capital requirements.
Capital planning and decisions regarding capital resource allocation require sound projections of the space, equipment, and infrastructure needs required and the financial costs. Without in-depth understanding of program operational requirements, there is a high probability of inaccurate capital cost projections and the resulting significant negative impacts (e.g., reduction in project scope, delays in project completion, lost revenue, and other opportunity costs, including staff recruitment and retention impacts), which may be revealed only at later stages of an approved project’s development. Owing to the critical need to understand the science as much as the technical facilities requirements in creating conceptual capital budgets, many institutions are increasingly identifying scientists and program staff, not the more typical model of architects and engineers, to lead their capital planning activities. For example, Dr. S. Lui, former U.S. Department of Agriculture (USDA) Agricultural Research Service (ARS) principal investigator, currently directs the USDA’s principal intramural scientific research agency’s capital planning activities with support from his technical staff who possess expertise in facilities management and operations (see Box 6.3).
Under the increasing accountabilities contained in the results-oriented financial plans of the nation’s academic and governmental research enterprises, accurate capital cost projections and identification of all targeted capital fund source(s) opportunities and commitments become “mission critical” processes that, if demonstrated as credible through professional peers and peer agency reviews, can only deepen NIH’s national and global support and viability. The indispensable links among capital cost, operations of the research enterprise’s programs, and time (when the physical solution will be available) should be recognized in a comprehensive capital plan.
As noted in earlier chapters of this report, and as a critical first step, the ORF has successfully identified and categorized the critical assets and vulnerabilities in the Bethesda Campus built environment10,11—shared with the committee as the CISIP12 mentioned earlier in this chapter. At the same time, the Government Finance Officers Association identified the most challenging components of any institutional or corporate capital planning process: identifying priorities for investment and funding sources that will implement the plan (Kavanagh, 2007). Without targeted or realistic capital resources identified or committed, an institutional capital plan that includes all “great ideas” becomes more of a “wish list” that may not be credible to the research enterprise or its funders.
In summary, the rigor of capital cost planning focuses the attention from the level of the individual principal investigator managing and accountable for running his or her laboratory and clinic to the NIH Director on the NIH shared scientific mission; identifies realistic vulnerabilities and opportunities in the built environment to support the science; recognizes the financial constraints and capabilities facing the NIH center or program; and from the national perspective, enhances the financial viability and stability of the IRP by confronting the likely challenge of never having sufficient capital to meet all of its needs.13
___________________
10 D. Wheeland, “Sustainment and Improvement Strategy,” presentation to the HHS Capital Investment Review Board, July 2016.
11 D. Wheeland, “Modernization of NIH Facilities and Infrastructure,” presentation to the HHS Secretary’s Budget Council Meeting, September 23, 2016.
12 NIH Office of Research Facilities, “NIH Condition Index, Sustainment and Improvement Funding Needs Plan,” via e-mail, June 14, 2018.
13 Government Finance Officers Association, “Best Practices,” https://www.gfoa.org/best-practices, accessed August 30, 2018.
Capital and Cost Planning for the Research Enterprise
NIH, Stanford University (see Box 6.2), and the USDA ARS (see Box 6.3) utilize multiple and different levels of detail for capital project cost models at different stages of the capital planning process. As noted earlier, capital cost models developed for specific capital projects serve as the only realistic foundation for short-, mid-, and long-range institutional capital plan prioritization. The preliminary and later planning phase capital cost projections are key to successfully supporting the effectiveness of the NIH Capital Plan, whether as part of a request seeking authorizing legislation at the federal level of the Operating Divisions with HHS, or by an individual project manager within the ORF, who is managing the project to ensure that the project’s scope, schedule, and total cost identified earlier is balanced with the authorized appropriation. By supporting the capital plan, the NIH mission is served. Simply accelerating a response to the needs for new or improved space and facilities by the staff of the ORF, which may be out of balance with the available capital resources and the constantly evolving strategic scientific priorities, will only accelerate the degradation and limit the IRP’s strategic scientific missions.
TABLE 6.2.1 Stanford University 2017/18-2019/20 Capital Plan (in millions of dollars)
| Fiscal Year Project Schedule | Estimated Project Cost | Capital Budget 2017/2018 | Current Funds | In Hand or Pledged | To Be Raised | Service Center/Auxiliary Debt | Academic Debt | Other | Resources to be Identifieda | Debt Service | Operations & Maintenance | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Escondido Village Graduate Residences | ||||||||||||
| —Residence Building | 2016-2021 | 1,009.2 | 159.7 | 209.2 | 150.0 | 50.0 | 600.0 | 31.2 | 9.7 | |||
| —Underground Parking Garages | 2016-2021 | 82.5 | 11.5 | 82.5 | 2.4 | |||||||
| Stanford Redwood City Phase 1 | 2015-2019 | 568.8 | 329.4 | 25.0 | 543.8 | 32.1 | 21.2 | |||||
| Neuro/ChEM-H Research Complex | 2015-2019 | 257.0 | 119.2 | 109.5 | 102.0 | 23.0 | 22.5 | 1.3 | 6.6 | |||
| Center for Academic Medicine 1 (CAM 1) | ||||||||||||
| —Building | 2017-2020 | 166.0 | 77.4 | 31.3 | 134.7 | 1.8 | 2.2 | |||||
| —Underground Parking (854 spaces) | 2017-2020 | 56.9 | 26.5 | 51.9 | 5.0 | 0.3 | 1.8 | |||||
| BioMedical Innovations Building 1 and Tunnel (BMI 1) | 2017-2019 | 210.0 | 104.0 | 20.0 | 102.5 | 47.5 | 40.0 | 2.4 | 2.4 | |||
| University Terrace Faculty Homes | 2013-2018 | 176.5 | 45.0 | 162.0 | 14.5 | |||||||
| Anne T. and Robert M. Bass Biology Research Building | ||||||||||||
| —Bass Biology Building | 2014-2018 | 125.6 | 56.5 | 58.1 | 49.9 | 6.9 | 10.7 | 0.6 | 4.2 | |||
| —Connective Elements | 2014-2018 | 4.7 | 2.1 | 0.2 | 4.5 | |||||||
| —Central Loading Dock and Stauffer III Demolition | 2015-2018 | 21.9 | 0.3 | 1.9 | 20.0 | 1.2 | (0.2) | |||||
| Frost Amphitheater Improvements | 2015-2018 | 33.5 | 19.9 | 33.5 | 0.6 | |||||||
| Public Safety Building | 2017-2019 | 31.5 | 12.4 | 31.5 | 0.8 | |||||||
| Encina Complex Upgrades | 2016-2019 | 25.8 | 6.6 | 14.5 | 11.3 | |||||||
| Athletic Academic Advising and Rowing Building | 2017-2018 | 25.0 | 16.7 | 4.2 | 18.1 | 2.7 | 0.4 | |||||
| Denning House | 2016-2019 | 23.1 | 15.0 | 23.1 | 0.5 | |||||||
| Durand Renovation—Phase 4 | 2017-2018 | 17.4 | 10.3 | 17.4 | ||||||||
| Environmental Health and Safety Facility Expansion | 2017-2019 | 16.5 | 12.6 | 2.0 | 14.5 | 0.9 | 0.3 | |||||
| Children’s Center of Stanford Community | 2017-2019 | 11.5 | 7.2 | 11.5 | 0.3 | |||||||
| Schwab Residential Center Renovations | 2017-2018 | 11.3 | 3.8 | 11.3 | ||||||||
| District Work Centers | 2017-2019 | 8.5 | 5.0 | 8.5 | 0.5 | 0.2 | ||||||
| Stanford Oak Garden Children’s Center | 2017-2020 | 7.5 | 4.8 | 7.5 | 0.2 | |||||||
| Subtotal—Projects in Design and Construction | 2,890.7 | 1,045.9 | 656.2 | 496.9 | 30.1 | 762.0 | 696.3 | 149.2 | — | 72.3 | 53.6 |
a Anticipated funding for this category is through a combination of school, department, and university reserves, and other sources.
FINDINGS AND RECOMMENDATIONS
Finding: The NIH-Wide Strategic Plan 2016-2020 sets forward the overall objectives of NIH research activities. However, as noted in the April 2016 Clinical Center Working Group Report to the Advisory
Committee to the Director, there was “inadequate attention to capacity and prioritization: There is little scientific prioritization across ICs, and this becomes particularly problematic in the case of shared resources.” The risks inherent in leading-edge clinical research and hospital operations generally differ from those associated with biomedical research. The NIH-Wide Strategic Plan also does not consider the current, mid-term, or long-term implications of the proposed research with respect to its capital facility assets, including all buildings and infrastructure.
Finding: The NIH 2013 Bethesda Campus Master Plan explicitly references the NIH-Wide Strategic Plan (albeit from an earlier year), and prioritizes renewing aging physical facilities and reducing leased space. This Master Plan, however, has not been updated (as far as it has been presented to the committee) to reflect (1) changes in research strategic goals; (2) changes in research processes, personnel, and methods that affect space use and utilization; (3) progress to date on improved, renovated, or new capital facility assets (including buildings and infrastructure); and (4) changes in partnering opportunities and challenges.
Finding: The NIH currently has a detailed process for capital investment planning, as evidenced in the NIH Design Requirements Manual for new or renovated biomedical research and animal care facilities. While the HHS Form 300—FPAA requires evidence of projected institutional operating budget impacts associated with the proposed capital investment requested, the data appear to be incomplete in so far as they are limited to traditional maintenance and utility operating budget impacts.
Finding: Current Bethesda Campus cost planning utilizes a diverse and inconsistent range of capital cost model data and templates, with apparently regular modification of an informal cost model “template” by individual project officers or others.
Finding: The Bethesda Campus project and cost planning data do not appear to be evaluated by a peer expert panel. As noted by the April 2016 Clinical Center Working Group Report to the Advisory Committee to the Director, NIH, there was “no independent entity to verify that engineering controls for high-risk facilities meet appropriate regulations or standards prior to or after construction.” The committee was unable to identify evidence that formal or informal third-party peer review of NIH ORF preplanning PORs or total project capital cost models have been adopted.
Finding: Current capital investment planning does include a consideration of current maintenance backlog items, which appear to be input when maintenance staff familiar with Bethesda Campus buildings recognize critical needs. In addition, NIH employs an external contractor on a regular cycle to assess facility conditions and flag systems at the end of their useful life; key buildings undergo a comprehensive conditions audit on a regular and consistent schedule. However, these maintenance backlogs and condition assessments are not prioritized to maintain critical NIH mission activities.
Finding: Currently, NIH-peer state-of-the-art medical research organizations establish management processes and procedures that integrate the organization’s Strategic Plan with a Master Plan for facilities, infrastructure, and space needs across multiple schools, departments, divisions, or laboratories into one comprehensive financial annual planning and forecasting process. This integrated Strategic and Master Plan offers the opportunity to create a transparent and rigorous criteria for prioritization of financial operating and capital resource allocation.
Finding: Both the NIH-Wide Strategic (Research) Plan and the campus Master Plan, discussed above, emphasize the importance of enhancing interactions and collaboration among IRP research personnel and partners through shared space and facilities and the need for flexible and adaptable facilities to accommodate these collaborations and rapidly changing research program needs.
Recommendation 6.1: NIH should integrate its research strategic plan with its capital facility asset management plans, with explicit prioritization aimed at relating the long-term research strategy to the long-term campus Master Plan. This integration should include a rigorous and detailed 10-year plan for reduction of its Backlog of Maintenance and Repair that is embedded within the institution’s major capital improvement plan (currently the Buildings and Facilities/Nonrecurring Expenses Fund-funded 5-year plan). These plans should undergo annual review, redevelopment as needed based on review, and adoption at the highest levels of NIH.
Recommendation 6.2: NIH should establish a formal external interdisciplinary peer review panel to provide ongoing review of NIH capital assets, the annual project plan, the 5-year plan, the master plan, and the integrated research strategic plan and master plan, including enhancing interactions and collaboration among Intramural Research Program research personnel and partners.
Recommendation 6.3: NIH should establish processes and a system that ensure third-party, expert peer review of all adopted Office of Research Facilities preplanning programs of requirements and total project capital cost models.
























