Summary
If the measure of the performance of a country’s health system is the ability to ensure that everyone has a fair and just opportunity to be as healthy as possible, then the United States is failing. Life expectancy at birth in the United States has consistently trailed most other countries in the Organisation for Economic Co-operation and Development, and the gap is widening. Life expectancy at birth differs by as much as 18 years, depending on race and ethnicity. Compared to other high-income countries, the United States spends far more on health care and achieves worse outcomes, and trust in health systems continues to erode. The country’s current medical care infrastructure, and its focus on disease treatment and the dominant fee-for-service payment model, is not equipped to promote well-being and prevent the onset of disease. New goals and a systematic reorientation of resources and activities are necessary.
The 2001 Institute of Medicine report Crossing the Quality Chasm: A New Health System for the 21st Century identified patient-centered care as one of six pillars of quality care. Emphasizing patient-centered care shifts the traditional disease-focused model to one more focused on patient values and priorities. The World Health Organization further expanded the concept to people-centered care, which includes the life course of an individual plus care of the family and community. Going one step further, a whole health approach to care emphasizes that people-centered care should promote well-being as defined by the individuals, families, and communities themselves over the life course. Whole health care is intended to shift the focus from a reactive disease-oriented medical care system to one that promotes disease prevention, health, and well-being. It changes the
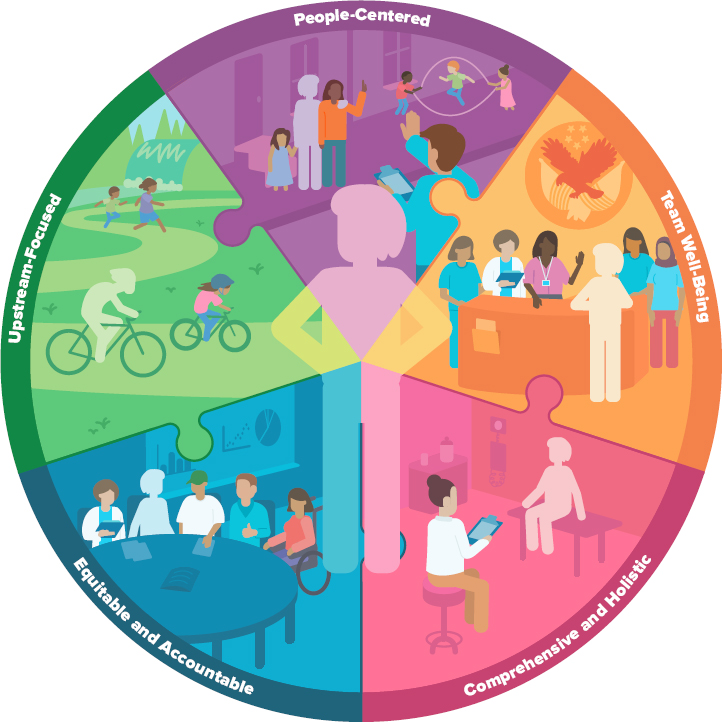
conversation with people from identifying what is the matter with them to identifying what matters to them, and it puts the person, not their symptoms, at the center of care (Figure S-1).
While the concept of whole health is not new, there has been a recent surge of health systems implementing whole health care. The Department of Veterans Affairs (VA) has been a leader in this movement, initially implementing its Whole Health System (WHS) in 18 sites and focusing on people with chronic pain, mental health needs, and disabilities. VA has since extended this program across all VA medical centers and expanded the scope of services and conditions it addresses. It plans to expand WHS to the entire VA system by 2027. VA’s people-centered, integrative, and transformative approach is designed to create and support health and wellbeing by incorporating individuals’ goals and priorities into care decisions.
It uses peer-led support, personalized health planning, coaching, and wellbeing courses, and it integrates evidence-based conventional medical care with complementary and integrative health, while also addressing the social determinants of health. The committee concluded that initial studies published by VA on the WHS are promising, demonstrating positive outcomes for pain management and opioid use and high patient satisfaction. This transformational approach to care could become a model for care across the country.
The unique financing and organization of VA makes it a logical setting in which to field and test whole health care. VA serves as both an insurer and care provider; provides health and social care services through the Veterans Health Administration and the Veterans Benefits Administration; and has data, resources, and a policy mandate to innovate and study whole health care. Most importantly, many veterans have service-related conditions that require new and innovative ways to address and deserve the support and care from VA to achieve their life goals.
Many health systems in the United States and abroad have also implemented some form of whole health care. While each of these exemplars has its own unique approach to whole health care, they are all built on a foundation of high-quality, well-supported primary care and are cross-sectoral, spanning conventional medical care, mental health, health behavior promotion, complementary and integrative health, public health, and social services. They have also demonstrated the positive benefits of a whole health approach, including improved patient experience and patient-reported outcomes; increased access to care; reduced emergency room use and hospitalizations; improved clinical quality metrics; improved outcomes for chronic pain, mental health, traumatic brain injury, and healthy aging; reduced maternal and infant mortality; improved health equity; the promotion of team well-being; and some reductions in health care expenditures. These early implementers can help translate the lessons of whole health care to the VA and the broader health care community.
STUDY CONTEXT AND CHARGE
In January 2019 a report from the Creating Options for Veterans’ Expedited Recovery Commission, a federally established advisory committee, recommended that VA commission the National Academies of Sciences, Engineering, and Medicine (National Academies) to provide input on how to accelerate whole person care transformation by building on current efforts in mental health, primary care, and whole health care. Responding to that recommendation, VA commissioned the National Academies to provide guidance on how to fill gaps and create processes to accelerate this transformation for veterans both inside and outside the VA system.
As a result, the National Academies formed the Committee on Transforming Health Care to Create Whole Health: Strategies to Assess, Scale, and Spread the Whole Person Approach to Health. The committee’s statement of task charged it with examining the potential for improving health outcomes through a whole health care model; identifying best practices and lessons learned from the flagship and design sites of VA’s Whole Health Initiative, as well as from health systems in the United States and internationally; and considering ways to transform health care by scaling and disseminating whole health care to the entire U.S. population. The committee’s charge was to consider the foundational elements of an integrated whole health model, but not to identify specific interventions that should be included in whole health models of care or defining specific evidentiary standards for making those decisions.
WHAT ARE WHOLE HEALTH AND WHOLE HEALTH CARE?
Having whole health is fundamentally different from being healthy in a biomedical model. Whole health is a resource for everyday life to enable people and communities to achieve their life aspirations and cope with change. Achieving whole health starts with understanding what matters to people and then builds the environment, resources, and support to help people and communities achieve their life goals. The committee believes that all people and all communities have a right to whole health. It is a common good and should be the desired goal of any effective health care system. The committee’s first task was to define whole health, and it developed this definition:
Whole health is physical, behavioral, spiritual, and socioeconomic wellbeing as defined by individuals, families, and communities. To achieve this, whole health care is an interprofessional, team-based approach anchored in trusted longitudinal relationships to promote resilience, prevent disease, and restore health. It aligns with a person’s life mission, aspiration, and purpose.
The committee also identified five foundational elements of whole health that are necessary to have an effective whole health care system: (1) people-centered, (2) comprehensive and holistic, (3) upstream-focused, (4) accountable and equitable, and (5) grounded in team well-being (Figure S-1).
Being people-centered is based on the idea that people, families, and communities should direct the goals of care, and it fosters self-empowerment through longitudinal, relationship-based care. Decades of research demonstrate that people-centered care most strongly influences patients’
experience of care, less strongly influences patients’ reported outcomes, and least strongly affects clinical or physiologic outcome measures.
Being comprehensive and holistic means that whole health care systems address all the domains of care that affect health and consider the entire person, their family, and their community. Robust evidence demonstrates that each component of comprehensive care (acute and chronic care, mental health care, oral care, vision care, hearing care, complementary and integrative health, spiritual care, social care, health behaviors, and additional upstream factors) improves peoples’ well-being. Evidence also shows that providing all components of comprehensive care in one setting (e.g., high-quality primary care) further improves well-being.
Being upstream-focused requires a multisectoral, integrated, and coordinated approach to identifying and addressing the root causes of poor health. It addresses the conditions of daily life with the goal of making them more conducive to whole health. These root causes of poor health (health behaviors, social needs, environment), often referred to as the social determinants of health, have more impact and influence on health than conventional medical care. Addressing these needs through cross-sector collaborations can have a tremendous impact on health.
At their core, whole health systems must be equitable and accountable in providing care. The people not seeking care are often in greatest need of care. By being held responsible for people, families, and communities, whole health systems can transform care from being reactive to proactive and help meet needs before they develop into problems.
Delivering a whole health approach will not be easy and can only succeed if attention is paid to the team well-being of the entire interprofessional care team.1 Burnout among health and social care professionals is at an all-time high. Caring for others requires a stable, healthy, resilient, and innovative team that can support the cultural transformations needed for whole health care.
SCALE AND SPREAD OF WHOLE HEALTH APPROACHES
Moving toward whole health will require a radically different mindset and significant systems change in which all participants embrace the committee’s five foundational elements, develop the structures and processes needed to support whole health, and achieve new levels of integration across settings and services. As the committee’s framework to scale and
___________________
1 An interprofessional care team includes a variety of clinical and nonclinical team members that collectively meet the whole health needs of a population or community. An interprofessional team will look different depending on available resources, and local needs, and should ideally reflect the diversity of its community.
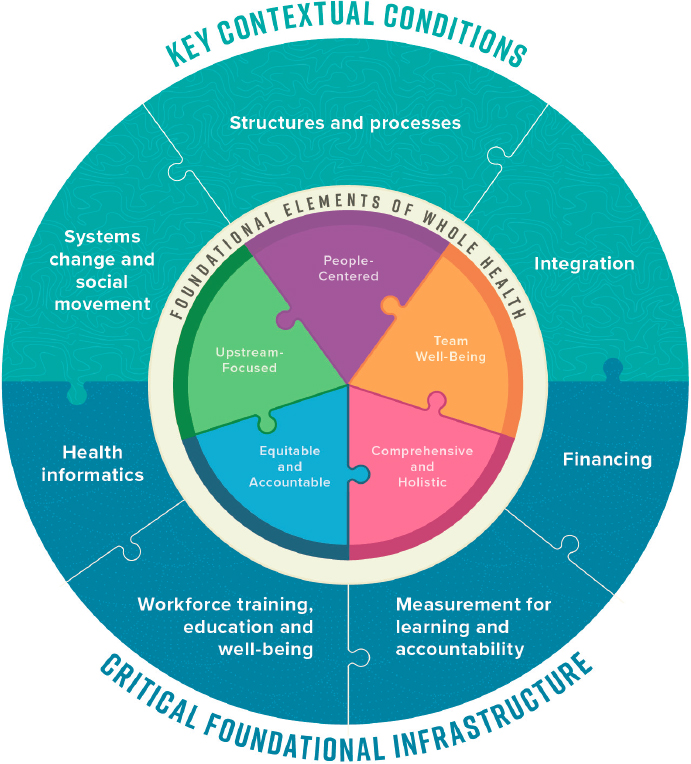
spread whole health (Figure S-2) indicates, developing and sustaining such systems will require both key contextual conditions (systems change and social movement, structures and processes for scale and spread, and integration of services) and alignment of critical foundational infrastructure (e.g., supportive health informatics; workforce training, education, and wellbeing programs; measurement systems for learning and accountability; and innovative health care financing). Or, to put it another way, without mutual reinforcement of systemic change, an embrace of whole health principles, development of structures and processes, integrated service delivery, and foundational infrastructure, the nation’s ability to scale and spread whole health will be limited.
Scaling and spreading a whole health approach requires integration across sectors, some of which, especially those that address upstream factors, typically operate outside of most health care systems today. Although this report is primarily focused on how VA health care and other U.S. health care systems can scale and spread whole health, similar reports could be written from the perspective of social services, community programs, public health, or education systems and how they can better integrate and scale and spread whole health themselves.
COMMITTEE GOALS AND RECOMMENDATIONS
This report and recommendations apply to both VA systems of care and, more broadly, to systems of care throughout the United States and internationally. To ensure that every veteran and every person has access to and can receive the support they need to attain whole health, the committee’s recommendations fall under six implementation goals. These goals describe a transformational journey in which health systems iterate goals as they learn to develop capacity for whole health care.
-
COMMIT to the shared purpose of helping people achieve whole health.
- Engagement, support, buy-in, and prioritization from the bottom up and top down are needed to enable the necessary cultural and structural transformations.
-
PREPARE for a whole health approach to care.
- Interprofessional teams, organizations, and systems need to understand where they are and what they need to change to deliver whole health care.
-
INTEGRATE across systems, services, and time to support whole health care throughout the lifespan.
- Achieving whole health will require support in all settings throughout peoples’ lifespan, and within and across the communities.
-
DELIVER all foundational elements of whole health care across the lifespan
- Each foundational element of whole health care is essential and interdependent, and successful whole health systems need to attend to all five elements.
-
EVALUATE to iteratively refine whole health care systems and create generalizable knowledge.
- The understanding of how to best deliver whole health care is evolving rapidly, so evaluating and adapting approaches and sharing learnings will be essential.
-
DESIGN public- and private-sector policies and payment to support whole health as a common good and whole health care as a way of achieving whole health.
- Scaling and spreading whole health care will not be possible without realigning infrastructure, policies, and payment.
GOAL ONE: COMMIT TO THE SHARED PURPOSE OF HELPING PEOPLE ACHIEVE WHOLE HEALTH
Recommendation 1.1: To scale and spread whole health, the Department of Veterans Affairs, the Department of Health and Human Services, other federal agencies addressing health and social services, state and local governments, health systems, social services, community programs, and external environment actors (payers, corporations, educators, and others) should make whole health a core value.
Making whole health a core value means committing to the goal of whole health and the cultural, structural, and process changes needed to achieve it. This commitment starts with leadership across public and private sectors, including health care, community programs, social services, and public health organization, payers, educators, and informatics-oriented organizations or vendors, making meaningful actions that include
- Securing prioritization and buy-in at all levels of leadership.
- Naming the care delivery approach as a “whole health approach.”
- Making a whole health approach part of the organization’s core mission statement.
- Creating a vision and roadmap for delivering whole health.
- Including the people, families, and communities that will be served in the design of the whole health care system.
- Financially investing in the development of whole health approaches.
- Identifying champions at the local level and supporting their efforts to lead needed transformations.
- Incorporating whole health approaches in day-to-day culture for patients and care team members.
GOAL TWO: PREPARE FOR A WHOLE HEALTH APPROACH TO CARE
Recommendation 2.1: National, regional, and facility VA leaders should ensure that all sites are ready to offer the Whole Health System of Care to all veterans by ensuring that each site understands and adopts the
whole health mission and vision and has the resources and services it needs to transform its care delivery approach.
While VA has made tremendous advances in developing, implementing, and spreading its Whole Health System (WHS), not all VA sites have fully implemented it. All veterans should have easy access to whole health care in their community, which requires more fully scaling and spreading the WHS to all VA facilities. Additionally, not all VA sites will have the resources and interprofessional team members to fully implement the WHS, so veterans should be able to access WHS services either on site or through virtual platforms as well as through non-VA health care and community-based systems by taking advantage of community programs through the Maintaining Internal Systems and Strengthening Integrated Outside Networks Act of 2008 (MISSION Act) (Recommendation 6.1).
Recommendation 2.2: Health care systems, community programs, social services, and public health organizations committed to helping people achieve whole health should ensure that all sites are ready to offer whole health care to the people, families, and communities they serve.
VA and other health systems have made significant advances in implementing whole health approaches, and others are just beginning their whole health journeys. Whether an organization is just starting to implement a whole health approach or is scaling and spreading an existing approach to new sites, multiple actions are needed to prepare for care transformation, including
- Assessing organizational and interprofessional team member readiness.
- Identifying potential facilitators, barriers, and strategies for overcoming barriers.
- Defining the elements of the current care system that will need to change to transition from conventional to whole health care.
- Determining what resources are available and what resources are needed and pursuing those that are lacking.
- Identifying sites to serve as early adopters and designating champions to lead the redesign, innovation, and implementation.
- Creating a sense of urgency.
- Organizing interprofessional teams around the whole health needs of the people, families, and communities served.
- Developing processes for interprofessional teams to collaborate, share information, and coordinate resources.
- Establishing ongoing dynamic mechanisms for meaningful input from the people, families, and communities who will be co-creating whole health care.
- Developing the clinical, social services, and community cross-sector partnerships needed to fully address all five foundational elements of whole health.
- Ensuring that the whole health needs of the interprofessional workforce are also met.
GOAL THREE: INTEGRATE ACROSS SYSTEMS, SERVICES, AND TIME TO SUPPORT WHOLE HEALTH CARE THROUGHOUT THE LIFESPAN
Recommendation 3.1: The Department of Veterans Affairs should integrate the delivery of whole health services between the Veterans Benefits Administration (VBA) and the Veterans Health Administration (VHA).
Many of the benefits that VBA offers to eligible veterans address the issues that are relevant to upstream factors foundational to whole health. However, VBA and VHA are separate administrations under the Department of Veterans Affairs, with separate leadership, budgets, and reporting structures. Currently, their efforts are siloed and do not fulfill the characteristic of being holistic with components and team members seamlessly integrated and coordinated. Integrating key VHA and VBA efforts and team members has the potential to maximize the effectiveness and efficiency of VA’s whole health efforts while also reducing health inequities among veterans.
Recommendation 3.2: Health care systems should create and strengthen the infrastructure needed to partner with community programs, social care, and public health systems.
This recommendation applies to both VA and non-VA systems committed to whole health. Even if VHA and VBA fully integrate their whole health services, a whole health approach will still require contributions from community programs, social services, and public health programs. Whole health systems will need infrastructure to support partnerships at the federal, state, and local levels and will need to include both the public and private sectors. To determine the specific partnerships necessary to build a whole health approach, health systems will need to identify the resource, service, and provider gaps in their current approaches to whole health care.
GOAL FOUR: DELIVER ALL FOUNDATIONAL ELEMENTS OF WHOLE HEALTH CARE ACROSS THE LIFESPAN
Recommendation 4.1: The Department of Veterans Affairs should fully incorporate all whole health foundational elements into its Whole Health System.
VA has made tremendous efforts in developing and implementing its WHS. Future efforts should more fully develop all five foundational elements of whole health care with particular attention paid to ensuring that the care offered is comprehensive and holistic, to addressing upstream factors and team well-being, and to being accountable to all veterans, with particular attention paid to equity for disabled, socially vulnerable, racial and ethnic minority, women veterans, and others who may have difficulty accessing services due to geography or other factors. Additionally, VA will need to extend its whole health approach to older veterans, women’s health, maternal health, family health, LGBTQ+ health, chronic disease management, and healthy aging.
Recommendation 4.2: Health care systems, community programs, social services, and public health organizations should model whole health approaches after the Department of Veterans Affairs and other early adopters.
Systems that are committed to helping people achieve whole health should begin by building on what others have successfully done, although local tailoring will be necessary to address the specific needs of the people served, available resources of the local care systems, the local environment, and opportunities for collaboration. Whole health care should be the default way that health care is practiced and should be available for all people in every community across the lifespan.
Recommendation 4.3: Building on its existing health center program, the Health Resources and Services Administration (HRSA) should lead the scale and spread of whole health care in the community.
HRSA is well positioned to serve as a federal leader in promoting whole health care adoption and implementation in non-VA settings. HRSA has established systems of accountability and addresses upstream factors as well as conventional health care. Particularly important has been HRSA’s ability to scale and spread initiatives across the nation, including in some of its most vulnerable communities, in collaboration with state and community partners. HRSA’s approach to promote uptake and delivery of whole health
care services can serve as a model for commercial and federal payers as well as state and local health departments.
GOAL FIVE: EVALUATE TO ITERATIVELY REFINE WHOLE HEALTH SYSTEMS AND CREATE GENERALIZABLE KNOWLEDGE
Recommendation 5.1: Systems fielding a whole health approach should systematically and continuously evaluate and participate in external evaluations of the implementation and adaptations of the approach and disseminate the lessons learned.
Scaling and spreading effective whole health approaches so that whole health is accessible to all will take fundamental changes to the structures, processes, and goals of how the nation thinks about and cares for people. It is essential for public and private systems fielding a whole health approach to evaluate how to implement whole health care and its outcomes. Evaluations should be prospective, longitudinal, and multilevel; should use a mix of methods and include information on how to achieve whole health; and should not be overly burdensome on clinicians or people receiving care. Findings should be openly and transparently shared so that others can learn and adapt approaches based on the results. These evaluations should focus on learning and should be distinct from the evaluations used to ensure accountability and the quality of whole health care.
Recommendation 5.2: Building on its overall mission to study the care of people and the allocation of Patient-Centered Outcomes Research Trust funding to disseminate evidence to practice, the Agency for Healthcare Research and Quality (AHRQ) should fund research to evaluate whole health care as well as research that disseminates evidence on whole health practices. Additional research support will be needed from other national and international organizations, foundations, and private payers.
To accomplish Recommendation 5.1, systems will need research support and funding. And, given its mission, AHRQ is a logical lead for this type of research. The National Institutes of Health’s dissemination and implementation portfolio and new Advanced Research Projects Agency for Health can also be applied to whole health care. Federal leadership from organizations such as the Office of the National Coordinator for Health Information Technology can create incentives for informatics vendors to develop and support the systems needed to deliver whole health care, integrate collection and measurement tools into the electronic care delivery
workflow, and make data more easily accessible to care systems and health services researchers.
GOAL SIX: DESIGN PUBLIC- AND PRIVATE-SECTOR POLICIES AND PAYMENT TO SUPPORT WHOLE HEALTH AS A COMMON GOOD
Recommendation 6.1a: The Department of Veterans Affairs, federal policy makers, and regional third-party administrators should determine how the MISSION Act applies to delivering whole health services.
Recommendation 6.1b: Regional third-party administrators of the MISSION Act should streamline the process for enrolling community providers in community care networks and define and enforce standards for health record transfer between community care systems and VA as a condition for reimbursement.
While well intentioned, the current implementation of the MISSION Act is fraught with problems and, as currently put into practice, has significant limitations in access to care through community (non-VA) clinicians. VA and federal policy makers need to clarify which whole health services the current MISSION Act legislation and policy covers and to hold regional third-party administrators accountable for establishing the clinical capacity needed to ensure timely, high-quality care. VHA and VBA programs should engage with non-VA health systems and social support programs to promote the routine identification of patients/participants with past military service and create coordinated care systems across VA and community settings to promote whole health.
For the MISSION Act to succeed, it will also have to ensure that there are sufficient networks of community providers and services in areas with unmet veteran needs. While building larger networks of community providers will be challenging, regional third-party administrators can make the process of becoming an eligible community care provider more efficient to attract more participants. They can also ensure that both VA and community systems have a complete picture of each veteran’s whole health status, needs, and preferences by facilitating reliable and consistent health record exchange between systems. Paying for care from community providers and adding whole health care should not undercut access to services at VA sites.
Recommendation 6.2: The Department of Veterans Affairs, in partnership with the Department of Health and Human Services (HHS), should create a national Center for Whole Health Innovation to design and advance the policies and payments for whole health care.
The magnitude of change needed to accomplish whole health care implementation is great, even among systems that are already on this path. New partnerships will need to be forged, policy and payment changes will be needed, and an unprecedented level of coordination will be needed at the local, state, and national levels. This is not a change that will be accomplished in the next few years, but rather will be a decades-long process. Moreover, no one organization currently has the authority or responsibility for envisioning and leading implementation of an effective whole health approach that spans health care, public health, community programs, education, and social services sectors. Given the magnitude of change needed, the current early stage of whole health implementation, and the need for a longer trajectory of iterative system design, research, and adaptation to implement and refine the whole health approach, the committee recommends creating and funding a national Center for Whole Health Innovation. The center would be charged with developing the needed policies, practices, and tools required to support scaling and spread of whole health both within VA and, more broadly, across health, community, and social systems nationally.
While the committee considered various entities to lead this effort, it concluded that, given the complexity and needs across sectors, only the federal government has the authority and resources to oversee the required changes. The committee is not aware of a single other public or private organization that could address whole health in this way. While a coalition of organizations (either a private or a public–private coalition) might be able to address whole health care, responsibility would be diluted, and the coordination of efforts would be overly complex and cumbersome. There is a critical role for nongovernmental stakeholders (health system leaders, researchers, technology vendors, and others) to provide needed input and collaboration into designing the policies and payments for whole health care, and the committee concluded this could best be achieved by including these stakeholders as partners in the Center for Whole Health Innovation.
VA and HHS should lead the creation and design of the Center for Whole Health Innovation. The center could be modeled after other national centers, such as the Center for Medicare & Medicaid Innovation. The Center for Whole Health Innovation will need investments in the range of what the CMS innovation center or the Cancer Moonshot initiative receive, which will likely require congressional support. It will also need multisector participation from other whole health stakeholder agencies and organizations in addition to the people and communities they serve.
This recommendation has many similarities to the recommendation to form the Secretary’s Council on Primary Care in the National Academies’ Implementing High-Quality Primary Care report. The proposed center and the proposed council have some overlap in terms of mission, charge,
and design of whole health and primary care, respectively. However, whole health is more than high-quality primary care, and primary care has unique needs outside of whole health. The center and council will need to collaborate and build synergy with their efforts, but each will need to be independent parallel entities with unique charges.
The Center for Whole Health Innovation will need to address five specific tasks (as well as others not called out in the following list):
- Disseminate and advance the vision of whole health for the nation and how to deliver whole health care effectively and efficiently. As whole health care scales and spreads further, the Center for Whole Health Innovation can aggregate, share, and disseminate lessons learned and best practices to help systems adopt their whole health approach.
- Define how to measure and hold systems accountable for success. Measures are needed to assess the effectiveness of the delivery of whole health care and the attainment of whole health by individuals, families, and communities. These measures need to be distinctly different from current biomedical measures and should instead measure whether systems deliver whole health care’s foundational elements. Short-term measures could assess the process and delivery of care while long-term measures could focus on health outcomes.
- Ensure structures, processes, and infrastructure development to support whole health. Structures and processes that support whole health care will require experimentation with expanded interprofessional teams, new forms of inter- and intra-organizational relationships, and mechanisms for promoting their integration. The necessary infrastructure will include health information technology, workforce training and education, engagement of people and communities on whole health care, and measurement for learning to scale and spread and for accountability purposes.
- Adapt value-based payment models aligned with delivering whole health care by both public and private payers. Payment models will need to be inclusive of the entire interprofessional team and scope of whole health care services. They also need to reinforce the delivery of all five foundational elements of whole health care.
- Consider equitable allocation of resources to deliver whole health care. Because much of whole health occurs outside of conventional medical care delivery, there is a need to meaningfully invest in developing community programs and social services, especially in historically under-resourced settings with the most unmet need. National policies are needed to better allocate payment and resources across the broad spectrum of whole health services such as increased
- funding to address upstream factors affecting health, allocating more health and social care resources to the people and places in need, training the workforce needed to deliver whole health care, and improved education for all.
CONCLUSIONS
Whole health is a common good that benefits people, families, and communities. Scaling and spreading whole health care so that all can have access to needed services is a tall task and will take seismic cultural, structural, and process transformations. These include but are not limited to how to think about what it means to be healthy, how to deliver health care, who is accountable for delivering health care, and even how to measure success. Throughout the transformation process, the people, families, and communities who receive whole health care will need to be engaged as equal partners in defining health goals and the preferred strategies to reach those goals. Multisector collaboration and investment on a national and local level are needed, as is a significant reallocation of resources to ensure effective, efficient, and equitable care.
The United States has made significant national investments to address diseases and conditions, which has resulted in tremendous medical advances and innovations. However, the nation has not made similar commitments to improving the effective, efficient, and equitable delivery of care. The recommendations and approaches outlined in this report provide a roadmap for improving health, social, and community systems of care. Recent innovations in VA and in other early adopter systems of whole health care have significantly advanced the field and demonstrated the value of a whole health systems approach. Building on these advancements will ensure future success leading to better health and well-being for veterans and the nation.
















