Introduction
Nursing homes, as their very name implies, play a unique dual role in the nation’s long-term care continuum, serving as a place where people can receive needed health care and assistance with activities of daily living as well as a place they call home. For some, nursing homes serve as a temporary residence where they can recover after a hospitalization or illness. For others, it serves as their permanent home, a place where they receive care and services that should enable them to live a safe and fulfilled life. Currently, nearly 1.3 million Americans reside in more than 15,000 certified nursing homes (CDC, 2020; KFF, 2020a). Nearly 85 percent of nursing home residents are age 65 or older, and more than 40 percent are over age 85 (CMS, 2015). Aside from those nursing home residents who live there temporarily while rehabilitating from surgery or illness, most nursing home residents require assistance with activities of daily living because of chronic medical conditions or behavioral challenges, including dementia. About half of nursing home residents have Alzheimer’s or other dementias (Harris-Kojetin et al., 2019). The heterogeneity of the nursing home population contributes to persistent challenges for achieving optimal care, including the ability to provide the appropriate environment, high-quality staff training, and comprehensive quality measurement.
Long-term care is increasingly being provided in home and community-based settings (Fashaw et al., 2020), and nursing home occupancy rates are decreasing (CDC, 2017; Harrington et al., 2018; KFF, 2020b). For example, occupancy rates declined from 83.7 percent in 2009 to 80.8 percent in 2016 (Harrington et al., 2018). Occupancy rates further declined during the first year of the COVID-19 pandemic (decreasing by nearly 20 percent from 2020 to the beginning of 2021) (NIC, 2021; Paulin, 2021; Taylor and Wilson, 2021). While occupancy rates rose during 2021, they have not
yet returned to pre-pandemic rates (Berklan, 2021). In spite of this shift to community-based settings, nursing homes will likely always be needed for many reasons, including for individuals who have complex care needs, are without family or friends able to assist with care, or lack the resources to be cared for at home.
STUDY CONTEXT
Given the vulnerable state of many, if not most, nursing home residents and the large and growing number of older Americans, one would expect that the United States as a nation would ensure that nursing homes provide comprehensive, high-quality, person-centered care for the country’s aging parents, aunts and uncles, brothers and sisters, friends, and loved ones. However, the current system of nursing home care in the United States often fails to provide the supports and quality of care necessary to ensure the well-being and safety of nursing home residents—an unacceptable situation that has long been apparent to those who research, work in, or have loved ones in nursing homes. Indeed, the 1986 Institute of Medicine1 (IOM) report Improving the Quality of Care in Nursing Homes (IOM, 1986) addressed a variety of concerns related to the quality of care in nursing homes, including neglect and abuse of residents, poor quality of life, excessive cost, lack of or inconsistent regulatory oversight, lack of personal advocates for residents, and poor and unstandardized information. Thirty-five years ago, the Nursing Home Reform Act was enacted as part of the Omnibus Budget Reconciliation Act of 1987 (OBRA 87).2 As a result, the Health Care Finance Administration (now the Centers for Medicare & Medicaid Services) issued comprehensive regulations and survey processes to “ensure that residents of nursing homes receive quality care that will result in their highest practicable physical, mental, and social wellbeing.”3 Studies since the enactment of OBRA 87 have noted improvements in information on resident status, a decreased use of physical and chemical restraints, and increases in direct-care staffing (Fashaw et al., 2020; Wiener et al., 2007). However, while not all nursing homes provide substandard, unsafe, or depersonalized care, many of the concerns raised in the 1986 IOM report remain problematic today.
___________________
1 As of March 2016, the Health and Medicine Division of the National Academies of Sciences, Engineering and Medicine (National Academies) continues the consensus studies and convening activities previously carried out by the Institute of Medicine (IOM). The IOM name is used to refer to reports issued prior to July 2015.
2 Omnibus Budget Reconciliation Act of 1987, Public Law 100-203; 100th Cong., 1st Sess., (December 22, 1987).
3 Omnibus Budget Reconciliation Act of 1987, Public Law 100-203; 42 USC 1396r, 100th Cong., 1st Sess., (December 22, 1987).
The COVID-19 Pandemic
The COVID-19 pandemic and its devastating impact on nursing home residents and staff brought to the forefront the long-standing challenges in the nursing home system, such as inadequate staffing levels, poor infection control, and deficiencies that resulted in actual harm (GAO, 2003; Harrington et al., 2016, 2018; Kramer, 2021). In 2020, 42 percent of U.S. nursing homes received citations for deficiencies in infection control (KFF, 2020c), and 15 percent received citations for serious deficiencies that resulted in actual harm to a resident or put the resident at immediate risk for harm (KFF, 2020d).
Importantly, workers in nursing homes are often underappreciated, undercompensated, and underprepared for their roles in providing increasingly complex care. Robust data support the need to enhance training, salaries, and working conditions for nursing home workers, yet little progress has been made to improve the quality of these jobs (AHCA/NCAL, 2021). Again, the COVID-19 pandemic further exacerbated these preexisting shortcomings. For example, while the work of the direct-care workforce (e.g., certified nursing assistants) has commonly been referred to as physically demanding, in 2020 during the midst of the COVID-19 pandemic, the role of the nursing home worker was deemed among the most dangerous jobs in the country (Lewis, 2021). Burnout and turnover among the nursing home workforce due to the COVID-19 pandemic (which were prevalent even before the pandemic) are projected to exacerbate existing staff shortages across the country (Gandhi et al., 2021; Manchha et al., 2021).
The pandemic also highlighted the vulnerability of nursing home residents in general. The virus that causes COVID-19 (SARS-CoV-2) is particularly dangerous for individuals with underlying health conditions, especially conditions that are typical of nursing home residents. As a result, nursing home residents suffered disproportionately high rates of cases, hospitalizations, and deaths relative to the general population. For example, early in the pandemic, nursing home residents and staff accounted for 12 percent of all COVID-19 cases in the United States (Grabowski, 2020). Moreover, as of October 2021, despite nursing home residents making up less than one-half of 1 percent of the population (CDC, 2020; KFF, 2020a; U.S. Census Bureau, 2021) and just under 1.6 percent of all COVID-19 cases, they accounted for approximately 19 percent of all COVID-19 deaths (CDC, 2021a,b). The ubiquity of COVID-19 cases and deaths in nursing homes of all types (across facilities with high and low quality ratings) is indicative of a more systemic problem, one that will require systemic solutions.
Finally, the response to the COVID-19 pandemic shone a harsh light on pervasive ageism, or the undervaluing of the lives of older adults (Aronson, 2020; Carbonaro, 2020; Kendall-Taylor et al., 2020; Kilaru and Gee, 2020).
Kilaru and Gee (2020) reflected on structural ageism and noted that “complacency to the ongoing loss of life during the [COVID-19] pandemic may be the most unfortunate consequence of ageism [. . .] Ultimately, the pandemic has forced us to see how we value or devalue the lives of older adults.” Fraser and colleagues (2020) asked, “Did a pre-pandemic lack of resources for residents of [long-term care] homes exacerbate this looming crisis and our slow response?” Tied to this undervaluing of older adults is the stigma that can be associated with working in a nursing home, which contributes to persistent staffing shortages (even before the pandemic) (Beynon et al., 2020; Danilovich, 2017; Manchha et al., 2021, 2022). For family members’ perspectives, see Box 1-1.
Overall, the COVID-19 pandemic’s enormous toll on nursing home residents, families, and nursing home staff drew renewed and urgent attention to the shortfalls that continue to plague the nursing home industry, while highlighting the opportunities to ensure high-quality care for nursing home residents.
STUDY ORIGIN AND STATEMENT OF TASK
With support from a coalition of sponsors, including The John A. Hartford Foundation, The Commonwealth Fund, the Jewish Healthcare Foundation, The Sephardic Foundation on Aging, and The Fan Fox & Leslie R. Samuels Foundation, the National Academies of Sciences, Engineering, and Medicine (National Academies) formed the Committee on the Quality of Care in Nursing Homes in the fall of 2020. The sponsors charged the committee to examine how the United States delivers, finances, regulates, and measures the quality of nursing home care (see Box 1-2).
PREVIOUS WORK OF THE NATIONAL ACADEMIES
Building upon the 1986 study Improving the Quality of Care in Nursing Homes, the 2001 IOM report Improving the Quality of Long-Term Care provided a comprehensive look at the quality of care and quality of life in long-term care broadly (including nursing homes, home and community-based settings, and residential care facilities) (IOM, 2001a). The report once again raised continuing concerns about the quality, cost, and accessibility of care and the adequacy of oversight in long-term care settings, especially nursing homes. Overall, the report provided recommendations for improving external oversight, strengthening the caregiving workforce, building organizational capacity, and improving reimbursement. The report concluded:
[L]ong-term care should be consumer-centered focusing on the needs, circumstances, and preferences of people using care and involving them, to the extent possible, in planning, delivering, and evaluating care. (IOM, 2001a, pp. 248–249)
Several IOM studies focused specifically on the health care workforce. The 1996 report Nursing Staff in Hospitals and Nursing Homes made specific recommendations related to the numbers and types of nursing staff that should be present in nursing homes, key areas for training (e.g., geriatrics, occupational health and safety measures, culturally sensitive care, conflict management), and research needs (IOM, 1996). The report also examined work-related injury and stress for workers in nursing homes and
recommended screening of workers for a history of abuse and criminal records. The 2004 study Keeping Patients Safe: Transforming the Work Environment for Nurses focused on the connection between the work environment for nurses and patient safety, with a particular focus on nursing hours (IOM, 2004). The report called for improvements in nurse staffing, specifically calling for 24/7 registered nurse presence in nursing homes along with specific hours per resident day for different types of nurses. The 2008 report
Retooling for an Aging America provided recommendations to build the capacity of the health care workforce overall to care for older adults (IOM, 2008). The committee recommended education and training to enhance the competence of all types of workers in the care of older adults, including training medical residents in nursing home settings and enhancing the competence of direct-care workers. The report also called for redesigning models of care to provide comprehensive care to older adults, noting the small-home approach to nursing home care as an example of person-centered care.
More recently, the 2020 National Academies study Social Isolation and Loneliness in Older Adults found that housing status can affect levels of social isolation and loneliness (NASEM, 2020). It noted that while long-term care providers may strive to provide home-like accommodations and person-centered care, long-term care may increase social isolation and loneliness, particularly for individuals who are living far away from their loved ones, are unable to engage in meaningful social interactions, or need to share a room with someone with whom they are not compatible.
STUDY APPROACH AND SCOPE
The Committee on the Quality of Care in Nursing Homes consisted of 17 members with a broad range of expertise, including public health, gerontology/geriatrics, public policy, health care and social care providers, health equity, health information technology, health care financing and administration, nursing home regulation, nursing home quality, emergency preparedness and response, and legal issues. Appendix A provides brief biographies of the committee members and staff.
The committee deliberated during five 2- to 3-day virtual meetings and many conference calls and ad hoc meetings between November 2020 and November 2021. Additionally, the committee held six virtual public webinars and invited speakers to offer comments or make presentations to inform the committee’s deliberations. The speakers provided valuable input on a broad range of topics, including conceptualizing quality; family, resident, and clinical perspectives; industry, oversight, and regulatory perspectives (including the state survey process); issues related to staffing, culture change, equity, and nursing home leadership and ownership; quality improvement programs; and nursing home financing. The committee also established an online system for collecting narratives on resident, family, and nursing home staff experiences. Fifty-six sets of comments were submitted, and most came from the family members of nursing home residents. Quotes from these narratives are included in boxes throughout this report. Additionally, the committee completed an extensive search of the peer-reviewed literature and reviewed the gray literature, including publications by private organizations, advocacy groups, and government entities.
Overall Approach
The significant challenges to providing high-quality care in nursing homes are complex and pervasive and often extend past nursing homes themselves, reflecting challenges for long-term care in general as well as the broader health care system. Many experts have called for an entirely new system of nursing home care, which would go beyond the current realities of care delivery, regulation, financing, and quality measurement. Rebuilding an entirely new system is appealing, but the committee ultimately concluded that substantial and sustainable improvements in the quality of nursing home care require a realistic and intentional strategy that will in some areas necessitate incremental changes within the current system. Especially in areas with data and research gaps, for example, an incremental approach enables the time required to gather evidence for the best approach to achieving the committee’s vision, while at the same time increases the likelihood that unintentional consequences for nursing home residents will be identified and mitigated. Focusing only on short-term “quick fixes” also would likely not achieve the sustainable changes needed to dramatically improve the quality of care provided in nursing homes over the long term. Therefore, the committee sought to ensure that its goals and recommendations represent a coherent and integrated plan of action to achieve both short-term improvements as well as long-term objectives. The committee’s approach aligns with the statement of task, which specifically called on the committee to “develop a set of findings and recommendations to delineate a framework and general principles for improving the quality of care in today’s nursing homes” (see Box 1-2). Many of the committee’s recommendations aim to address high-level goals while allowing flexibility in how they should be implemented, while others contain greater detail about how to effectively implement the recommendations are specified. (See Chapter 10 for more on the committee’s approach to implementing its recommendations.)
Definitions and Terminology
The report uses a number of terms that absent further clarification may lead to misinterpretation. Below are some important definitions and distinctions in terminology.
Nursing Homes
While the terms “nursing home” and “skilled nursing facility” are often used interchangeably, skilled nursing facilities are designed to focus on the provision of short-term medical care after a hospital stay (although they may also provide long-term care for people with chronic illnesses). Most nursing
homes are licensed and serve as both long-term care and skilled nursing facilities. For the purposes of this report, unless otherwise noted, the committee uses the term nursing home to refer to both types of facility.
Nursing Home Residents
Nursing homes provide care to two different groups of people who have distinct care needs: short-stay individuals who require post-acute care after a hospital stay, and long-stay residents who have a more diverse range of care needs. For the purposes of this report, unless the distinction is important, the committee refers to all individuals within nursing homes as residents, while acknowledging the heterogeneity of the typical population in a nursing home that serves as both a long-term care facility and skilled nursing facility (i.e., long-stay “residents” and short-stay “patients”).
Person-Centered Care versus Person-Directed Care
Person-centered care has been defined in many ways, has no single agreed-upon definition, and is often used interchangeably with other terms such as person-directed care and patient-centered care. The 2001 IOM report Crossing the Quality Chasm defined patient-centered care as “respectful of and responsive to individual patient preferences, needs, and values and [ensures] that patient values guide all clinical decisions” (IOM, 2001b, p. 40). A 2016 literature review found 15 different descriptions of person-centered care for older adults that addressed 17 central principles or values, mostly in the domains of whole-person care, respect and value, choice, dignity, self-determination, and purposeful living (Kogan et al., 2016). Person-centered care focuses on the recipient of care and their values, preferences, goals, and abilities, rather than the efficiency and convenience of care delivery for staff (Fazio et al., 2018). In nursing home regulations, the Centers for Medicare & Medicaid Services (CMS) has specified that person-centered care means to “focus on the resident as the locus of control, and support the resident in making their own choices and having control over their daily lives.”4 Person-centered care requires, at a minimum, knowledge of the range and types of needs of nursing home residents and an assessment and care planning model that identifies, prioritizes, and addresses those needs in the context of their goals, preferences, and values.
Whereas person-centered care recognizes the goals, values, and preferences of individuals in the development of a care plan, person-directed care involves including individuals and their chosen family members as co-creators in the development of their care plans. This may be particularly
___________________
4 CMS Requirements for Long-Term Care Facilities—Definitions, 42 CFR § 483.5 (2017).
important in nursing homes where “care plans inform nearly all aspects of life” (Scales et al., 2017, p. 185). The committee recognizes person-directed care as an integral element of person-centered care in nursing homes. For the purposes of this report, the term person-centered care is used with the assumption that residents and their chosen family members are fully engaged.
Family Caregivers and Chosen Family
A variety of terms are used to describe the friends and family members who support the care of their loved one including family caregivers, informal caregivers, caregivers, and care partners. For the purposes of this report, the committee uses the term family caregiver with the understanding that family caregivers include both family members and non-family care partners (who the committee refers to as chosen family). The committee further recognizes that family caregivers may not actually provide hands-on care, but may provide support in other ways such as providing emotional support, representing the resident’s perspective and history, acting as a surrogate decision maker, and advocating for the resident’s safety and security (see more in Chapter 5). In the 2016 IOM report Families Caring for an Aging America it was said that
The term “family caregiver” should be used to reflect the diverse nature of older adults’ family and helping relationships. Some caregivers do not have a family kinship or legally defined relationship with the care recipient, but are instead partners, neighbors, or friends. Many older adults receive care from more than one family caregiver, and some caregivers may help more than one older adult. The circumstances of individual caregivers and the caregiver context are extremely variable. Family caregivers may live with, nearby, or far away from the person receiving care. Regardless, the family caregiver’s involvement is determined primarily by a personal relationship rather than by financial remuneration. The care they provide may be episodic, daily, occasional, or of short or long duration. (IOM, 2016)
Health Equity Terms
The term disparities refers to differences in care, but the term inequities recognizes “health differences that are avoidable, unnecessary, unfair and unjust” (AMA and AAMC, 2021, p. 11). Furthermore, instead of referring to cultural competence, the committee has chosen to focus on cultural humility and cultural sensitivity. Cultural competence implies a finite concept that has an end point that can be attained (largely based on the learner’s confidence and comfort, and mastery of specific knowledge) (AMA and AAMC, 2021). Cultural humility, on the other hand, recognizes the need
for lifelong learning and self-reflection to redress power imbalances and develop mutually beneficial partnerships (Tervalon and Murray-Garcia, 1998). Cultural sensitivity means that cultural norms, values, and practices are understood, respected, and accommodated in the planning and implementation of care practices (Mahmood et al., 2021; Meydanlioglu et al., 2015).
Approach to the Continuum of Long-Term Care Services
Long-term care typically refers to the provision of a wide range of services for varying lengths of time to promote healthy well-being and independence. Most long-term care facilities serve older adults and individuals with disabilities or severe/chronic illnesses (NIA, 2017). Settings for long-term care include private homes, independent living facilities, assisted living facilities, nursing homes, and skilled nursing facilities. While individuals may move among these settings during their lifetime, this committee’s charge was to focus only on the nursing home setting. However, in accordance with the statement of task, the committee does address the larger long-term care system as a contextual factor when appropriate.
Approach to Different Nursing Home Populations
Many different populations, with different care needs, goals, and lived experiences, reside in nursing homes. In particular, a significant and growing number of people under the age of 65 reside in nursing homes. Specific information about the characteristics of this population, however, is extremely limited, or outdated (see Chapter 2). For the purposes of this study, the committee primarily focused on older adults in nursing homes but asserts that its conclusions and recommendations are equally applicable for these populations, given the committee’s focus on person-centered care.
Approach to Health Equity and Disparities
Systemic failings such as neighborhood segregation, racism, and ageism have long been present in health care. These failings contribute to the poor health outcomes consistently shown for racial/ethnic minorities and those with low socioeconomic status (e.g., low household income, educational attainment), which are exacerbated by reduced access to health care and compromised quality of care. The health disadvantages due to these systemic failings and the resultant health and health care–related disparities accumulate over the life course to create inequities in patient outcomes in the long-term care system (Dannefer, 2003). The 2017 National Academies report Communities in Action: Pathways to Health Equity stated:
Health equity is the state in which everyone has the opportunity to attain full health potential and no one is disadvantaged from achieving this potential because of social position or any other socially defined circumstance. Health equity and opportunity are inextricably linked. Currently in the United States, the burdens of disease and poor health and the benefits of well-being and good health are inequitably distributed. This inequitable distribution is caused by social, environmental, economic, and structural factors that shape health and are themselves distributed unequally, with pronounced differences in opportunities for health. (NASEM, 2017, p. 1)
Health equity is generally aspirational and raises a wide range of questions. What does an equitable nursing home system generally—and a nursing home specifically—look like? What processes are needed for residents to receive care in an “equitable nursing home”? What are the barriers to an equitable nursing home system? Can we address those barriers, especially those related historical and structural racism? Do we define health equity in this context as a system where disparities across specific demographic categories (e.g., race, ethnicity, geographic location) are reduced, or a system where a demographic category does not predict poor quality nursing home care?
The committee determined early in the study process that health equity is a fundamental component of high-quality care. Rather than isolating the topic in an individual chapter, the committee decided that health equity would serve as a lens for all the topics discussed throughout the report. When an individual enters a nursing home, he or she should have the same expectations of high-quality care as any other regardless of race or ethnicity, language, gender, gender identity, or socioeconomic status. Importantly, the health equity lens was critical as the committee developed its recommendations focused on the goal of reducing disparities. That is, the committee considered how the implementation of each recommendation could affect sociodemographic groups differently or in ways that exacerbate disparities across groups.
Approach to the COVID-19 Pandemic
As noted above, the committee’s charge was to undertake a broad assessment of the quality of care in nursing homes and the factors that affect that care. While this was not a study focused on the impact of the COVID-19 pandemic on nursing homes, the committee recognized that the pandemic itself served to reveal and amplify the long-standing challenges and serious problems that exist in nursing home settings and have a direct impact on the quality of care provided. Thus, the COVID-19 pandemic served as another lens through which the committee explored the wide
range of issues affecting the quality of care in nursing homes. This report presents examples specific to the context of the COVID-19 pandemic, which serve to exemplify the challenges to providing quality, person-centered care to all nursing home residents.
Challenges of the Evidence Base
As the committee undertook the challenge of assessing the way the nation delivers, finances, regulates, and measures the quality of care in nursing homes, it quickly became evident that there were significant shortcomings in the evidence base on nursing home quality. First, the committee found a significant lack of data in many key areas, with many of the available data sources and studies quite dated; in many instances, the most recent studies on a specific topic had been conducted years or even decades earlier. Furthermore, much of the available research relies on retrospective cohort designs and is constrained by the limitations in data. Second, many sources did not distinguish among the populations studied. For example, in some studies, short-stay residents were not distinguished from long-stay residents, and studies of younger populations did not distinguish among the age groups below age 65. Moreover, many studies do not distinguish long-term care residents by setting of care (e.g., nursing home versus assisted living facility). Finally, given that this study was conducted in the midst of the COVID-19 pandemic, the committee was challenged to keep up with the inundation of information released on a daily basis—both in the popular press and the peer-reviewed literature. The committee sought to examine all sources and to prioritize the most salient research in order to inform its deliberations.
CONCEPTUAL MODEL OF NURSING HOME QUALITY
Given that the committee’s charge was to examine the quality of care in nursing homes, the committee members sought to develop a framework to help guide them in their work. Over time, scholars and professional health care organizations have developed a variety of conceptual models in an attempt to concisely define and measure nursing home quality, and, as a framework for this study, the committee created an original conceptual model of the quality of care in nursing homes based on a content analysis of existing conceptual models (or approaches) of health care quality or quality of care in nursing homes (see Box 1-3). Committee members performed multiple iterative rounds of analysis on this model, with the committee refining the model throughout the study process.
As the model depicts (see Figure 1-1), the committee’s vision of nursing home quality is that residents of nursing homes receive care in a safe
environment that honors their values and preferences, addresses goals of care, promotes equity, and assesses benefits and risks of care and treatments. However, as the committee’s evaluation of the evidence in the following chapters demonstrates, this model of quality care is not the reality in many nursing homes; rather, huge gaps in the quality of care remain despite years of research, advocacy, and regulation.
The conceptual model has three major components—inputs, nursing home care, and outcomes—and the model’s elements and the evidence supporting them are discussed throughout this report in greater detail. The model presents high-quality nursing home care as having a central focus on the nursing home residents that is person centered, culturally sensitive, respectful, and sensitive to social determinants of health. Additional core aspects of the model include that it is person directed; resident needs are met; and that it maintains dignity, maximizes independence, balances autonomy and safety, and allows for meaningful relationships.
Inputs to Nursing Home Quality
Inputs that affect nursing home care include payment and financing, national and state policy, market trends, consumer expectations, workforce, ownership and operators, the surrounding community, referring health systems, and external quality improvement supports. The committee emphasizes that equity transcends all key categories of nursing home care;
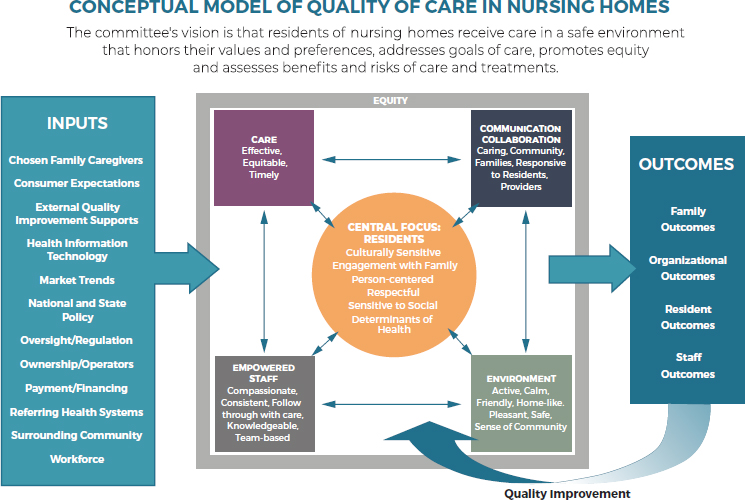
therefore, the model positions equity as surrounding nursing home care and envisioned that it must influence each of the categories.
Categories of Nursing Home Care
In addition to the central focus on residents, four other key categories in the conceptualization of high-quality nursing home care are
- Care that is effective, timely, and equitable;
- Communication that is caring and responsive to residents, families, providers, and community;
- Empowered staff who are knowledgeable, consistent, compassionate, and team based and who follow through with care; and
- An environment that is calm and active (in a way that aligns with residents’ needs), friendly, and pleasant; that has community involvement; and that is home-like.
Care
The committee envisions the “care” category to encompass elements such as addressing basic human needs, including
- Physiological needs (e.g., food, water, and rest and safety and security needs, such as being free of illness and injury);
- Social needs (e.g., companionship, family, affection); and
- Self-esteem needs (e.g., independence, meaningful activities, self-worth; and the ability to reach one’s full potential, including having optimal quality of life and meeting spiritual needs).
Care should also address individual care needs, including serious illness and end-of-life care, chronic disease, and behavioral health management (e.g., medication, treatment) with health restoration and preservation of function and comfort.
Communication
The communication category encompasses both relationships and communication. Thus the category includes fostering close relationships among residents, staff, and families; positive communication (verbal and nonverbal) with residents; staff who are open and listen to families; staff who take the time to really talk with residents; collaboration, communication, and shared decision making and care planning among staff, families, and health care providers. The category also includes coordination of care with internal and outside entities and the integration of health information technology.
Empowered Staff
The empowered staff category refers to having an effective, stable leadership involved in care. This ranges from registered nurses involved in planning and care delivery and knowledgeable, interdisciplinary staff who can meet resident basic human and behavioral health needs, to having all staff and leaders working as a team. The category also includes sensitivity to the culture of all staff, residents, and families; respect for residents’ needs, likes, and dislikes; collaboration among staff and families in working with residents; and the involvement of staff and families in care plans. This category also includes having staff in adequate numbers and consistent staff to care for residents (staff who know them well and help meet their needs); adequate supervision and training; and low staff turnover and low staff burnout.
Environment
The environment category involves issues such as a physical environment for residents and staff that is designed to be safe and secure; is odor
free and clean, with pleasant smells and sounds; and is well maintained and natural, with good lighting. Outdoor access is important, as is having community involvement; having interaction with volunteers, animals, and children; having residents engaged in age and functionally appropriate activities; and the nursing home feeling like a home, not a warehouse. Evidence of emergency preparedness is also a critical element of this category.
Outcomes of High-Quality Care
Outcomes of nursing home care include resident, family, staff, and organizational outcomes as well as outcomes related to regulation and oversight. Resident outcomes include quality of life, experience with care, satisfaction, nursing home quality measures (for both long-stay and short-stay residents), hospital admissions, health equity, and goal attainment. Family outcomes include experience with care, satisfaction, burden, and social connectedness. Staff outcomes include staff turnover and retention, staff satisfaction, and staff knowledge and competence. Organizational outcomes include publicly reported quality measures, occupancy rate, financial performance and reserves, community representation and connections, and health information technology connectivity. Oversight and regulatory outcomes include the results seen in state surveys.
Continuous Quality Improvement
Quality improvement is an important action step within the committee’s conceptual model. The nursing home setting, as is the case in all sectors of health care, has a long history of using quality improvement methods to measure the quality of care. Facilities use the results of those measurements to strive to continuously improve care by engaging with the nursing home staff, residents, and families to develop and implement improvement plans. If successful, quality improvement efforts result in anticipated improvements documented in the outcomes. If the results are not as anticipated, the iterative problem-solving process for new solutions begins.
ORGANIZATION OF THE REPORT
The committee structured its report around the components of the conceptual model. This introductory chapter has described the study context, charge to the committee, scope and methods of the study, and the conceptual model. Chapter 2 provides additional information on the landscape of the nursing home sector today. Chapter 3 examines issues related to quality measurement and quality improvement. Chapter 4 focuses on care delivery in nursing homes, while Chapter 5 examines the workforce that
supports nursing home residents. Chapter 6 addresses issues related to the safety and environment. Chapter 7 explores the financing of nursing home care. Chapter 8 addresses issues related to quality assurance, specifically, the oversight and regulation of nursing homes. Chapter 9 provides information on health information technology. Finally, Chapter 10 presents the committee’s recommendations for improving the quality of care in nursing homes.
In addition to the main report, there are five appendixes. Appendix A contains committee and staff biographies. Appendix B provides examples of successful demonstration projects in the Initiative to Reduce Avoidable Hospitalizations among Nursing Facility Residents. Appendix C contains an overview of the areas of measurement and priority areas for research included among the committee’s recommendations, and Appendix D provides a table of the committee’s recommendations organized by responsible partner. Appendix E includes a categorization of the committee’s recommendations according to an estimated implementation timeline.
CONCLUSION
Though nursing homes vary in size, type, and layout, in general they can be viewed as “complex social systems that consist of different participants, including staff, leaders, residents, and families in constantly shifting interactions” (Myhre et al., 2020). The following chapters present the evidence base for the current quality of care in nursing homes and, ultimately, the committee’s integrated set of recommendations to move the nation closer to achieving high-quality, person-centered, and equitable care for all nursing home residents, their families, and the staff who provide care for and support residents’ choices and goals.
REFERENCES
AHCA/NCAL (American Health Care Association and National Center for Assisted Living). 2021. State of the long term care industry: Survey of nursing home and assisted living providers show industry facing significant workforce crisis. https://www.ahcancal.org/News-and-Communications/Fact-Sheets/FactSheets/Workforce-Survey-September2021.pdf (accessed October 7, 2021).
AMA and AAMC (American Medical Association and Association of American Medical Colleges). 2021. Advancing health equity: Guide on language, narrative and concepts. https://www.ama-assn.org/system/files/ama-aamc-equity-guide.pdf (accessed February 6, 2022).
Aronson, L. 2020. Ageism is making the pandemic worse. https://www.theatlantic.com/culture/archive/2020/03/americas-ageism-crisis-is-helping-the-coronavirus/608905 (accessed February 7, 2022).
Berklan, J. M. 2021. Nursing home occupancy woes worse than popularly reported, industry expert says. https://www.mcknights.com/news/nursing-home-occupancy-woes-worse-than-popularly-reported-industry-expert-says (accessed February 5, 2022).
Beynon, C., R. Perkins, and L. Edelman. 2020. Breaking down stigma: Honoring nursing home staff during COVID-19. Journal of Gerontological Nursing 46(8):5.
Carbonaro, G. 2020. ‘Every life matters’: WHO chief warns against COVID-19 age discrimination. https://newseu.cgtn.com/news/2020-03-11/-Every-life-matters-WHO-warns-against-COVID-19-age-discrimination-OKDSHuH0gU/index.html (accessed February 14, 2022).
CDC (Centers for Disease Control and Prevention). 2017. Table 92. Nursing homes, beds, residents, and occupancy rates, by state: United States, selected years 1995–2016. https://www.cdc.gov/nchs/data/hus/2017/092.pdf (accessed November 19, 2021).
CDC. 2020. National Center for Health Statistics—Nursing home care. https://www.cdc.gov/nchs/fastats/nursing-home-care.htm (accessed October 16, 2020).
CDC. 2021a. COVID data tracker. https://covid.cdc.gov/covid-data-tracker/#datatracker-home (accessed June 7, 2021).
CDC. 2021b. COVID data tracker weekly review. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covidview/index.html (accessed November 12, 2021).
CMS (Centers for Medicare & Medicaid Services). 2015. Nursing home data compendium. Baltimore, MD: Centers for Medicare & Medicaid Services.
Danilovich, M. 2017. Crisis of recruitment: Stereotypes hinder staffing in geriatric service. https://medium.com/thrive-global/how-stereotypes-about-nursing-homes-can-make-aging-harder-for-everyone-51ff2d53fefd (accessed February 15, 2022).
Dannefer, D. 2003. Cumulative advantage/disadvantage and the life course: Cross-fertilizing age and social science theory. Journals of Gerontology Series B: Psychological Sciences and Social Sciences 58(6):S327–S337.
Donabedian, A. 1988. The quality of care. How can it be assessed? JAMA 260(12):1743–1948.
Fashaw, S. A., K. S. Thomas, E. McCreedy, and V. Mor. 2020. 30-year trends in nursing home composition and quality since the passage of OBRA. Journal of the American Medical Directors Association 21(2):233–239.
Fazio, S., D. Pace, J. Flinner, and B. Kallmyer. 2018. The fundamentals of person-centered care for individuals with dementia. The Gerontologist 58(S1):S10–S19.
Fraser, S., M. Lagace, B. Bongue, N. Ndeye, J. Guyot, L. Bechard, L. Garcia, V. Taler, CCNA Social Inclusion and Stigma Working Group, S. Adam, M. Beaulieu, C. D. Bergeron, V. Boudjemadi, D. Desmette, A. R. Doizzetti, S. Ethier, S. Garon, M. Gillis, M. Levasseur, M. Lortie-Lussier, P. Marier, A. Robitaille, K. Sawchuk, C. Lafontaine, and F. Tougas. 2020. Ageism and COVID-19: What does our society’s response say about us? Age Ageing 49(5):692–695.
Fulmer, T. 2018. Discovering the 4Ms: A framework for creating age-friendly health systems. https://www.johnahartford.org/blog/view/discovering-the-4ms-a-framework-for-creating-age-friendly-health-systems (accessed February 25, 2021).
Gandhi, A., H. Yu, and D. C. Grabowski. 2021. High nursing staff turnover in nursing homes offers important quality information. Health Affairs 40(3):384–391.
GAO (U.S. Government Accountability Office). 2003. Nursing home quality: Prevalence of serious problems, while declining, reinforces importance of enhanced oversight. Washington, DC: U.S. Government Accountability Office.
Grabowski, D. C. 2020. Strengthening nursing home policy for the postpandemic world: How can we improve residents’ health outcomes and experiences? New York: The Commonwealth Fund.
Harrington, C., J. F. Schnelle, M. McGregor, and S. F. Simmons. 2016. The need for higher minimum staffing standards in U.S. Nursing homes. Health services insights 9:13-19.
Harrington, C., H. Carrillo, R. Garfield, M. Musumeci, and E. Squires. 2018. Nursing facilities, staffing, residents and facility deficiencies, 2009 through 2016. https://files.kff.org/attachment/REPORT-Nursing-Facilities-Staffing-Residents-and-Facility-Deficiencies-2009-2016 (accessed February 5, 2022).
Harris-Kojetin, L., M. Sengupta, J. P. Lendon, V. Rome, R. Valverde, and C. Caffrey. 2019. Long-term care providers and services users in the United States, 2015–2016. Vital and Health Statistics, series 3, no. 43. Washington, DC: U.S. Government Publishing Office. https://www.cdc.gov/nchs/data/series/sr_03/sr03_43-508.pdf (accessed November 22, 2021).
IHI (Institute for Healthcare Improvement). 2021a. The IHI Triple Aim. http://www.ihi.org/Engage/Initiatives/TripleAim/Pages/default.aspx (accessed January 12, 2021).
IHI. 2021b. What is an age-friendly health system? http://www.ihi.org/Engage/Initiatives/Age-Friendly-Health-Systems/Pages/default.aspx (accessed November 18, 2021).
IOM (Institute of Medicine). 1986. Improving the quality of care in nursing homes. Washington, DC: National Academy Press.
IOM. 1996. Nursing staff in hospitals and nursing homes: Is it adequate? Washington, DC: National Academy Press.
IOM. 2001a. Improving the quality of long-term care. Washington, DC: National Academy Press.
IOM. 2001b. Crossing the quality chasm: A new health system for the 21st century. Washington, DC: National Academy Press.
IOM. 2004. Keeping patients safe: Transforming the work environment of nurses. Washington, DC: The National Academies Press.
IOM. 2008. Retooling for an aging America: Building the health care workforce. Washington, DC: The National Academies Press.
IOM. 2016. Families caring for an aging America. Washington, DC: The National Academies Press.
Kendall-Taylor, N., A. Neumann, and J. Schoen. 2020. Advocating for age in an age of uncertainty. https://ssir.org/articles/entry/advocating_for_age_in_an_age_of_uncertainty (accessed February 14, 2022).
KFF (Kaiser Family Foundation). 2020a. Total number of residents in certified nursing facilities. https://www.kff.org/other/state-indicator/number-of-nursing-facility-residents (accessed September 30, 2021).
KFF. 2020b. Certified nursing facility occupancy rate. https://www.kff.org/other/state-indicator/nursing-facility-occupancy-rates (accessed January 6, 2022).
KFF. 2020c. Percent of certified nursing facilities with top ten deficiencies. https://www.kff.org/other/state-indicator/percent-of-certified-nursing-facilities-with-top-ten-deficiencies-2014 (accessed September 30, 2021).
KFF. 2020d. Percent of certified nursing facilities receiving a deficiency for actual harm or jeopardy. https://www.kff.org/other/state-indicator/of-facilities-w-serious-deficiencies (accessed September 30, 2021).
Kilaru, A. S., and R. E. Gee. 2020. Structural ageism and the health of older adults. JAMA Health Forum 1(10):e201249.
Kogan, A. C., K. Wilber, and L. Mosqueda. 2016. Person-centered care for older adults with chronic conditions and functional impairment: A systematic literature review. Journal of the American Geriatrics Society 64(1):e1–e7.
Kramer, R. G. 2021. Fixing nursing homes: A fleeting opportunity. https://www.healthaffairs.org/do/10.1377/forefront.20210407.717832/full (accessed February 16, 2022).
Lewis, T. 2021. Nursing home workers had one of the deadliest jobs of 2020. https://www.scientificamerican.com/article/nursing-home-workers-had-one-of-the-deadliest-jobs-of-2020 (accessed January 6, 2022).
Mahmood, M. A., K. S. Khan, and J. R. Moss. 2021. Applying public health principles to better manage the COVID-19 pandemic: “Community participation,” “equity,” and “cultural sensitivity.” Asia Pacific Journal of Public Health 33(8):951–952.
Manchha, A. V., N. Walker, K. A. Way, D. Dawson, K. Tann, and M. Thai. 2021. Deeply discrediting: A systematic review examining the conceptualizations and consequences of the stigma of working in aged care. The Gerontologist 61(4):e129–e146.
Manchha, A. V., K. A. Way, K. Tann, and M. Thai. 2022. The social construction of stigma in aged-care work: Implications for health professionals’ work intentions. The Gerontologist. https://doi.org/10.1093/geront/gnac002.
Meydanlioglu, A., F. Arikan, and S. Gozum. 2015. Cultural sensitivity levels of university students in receiving education in health disciplines. Advances in Health Sciences Education 20:1195–1204.
Myhre, J., S. Saga, W. Malmedal, J. Ostaszkiewicz, and S. Nakrem. 2020. Elder abuse and neglect: An overlooked patient safety issue. A focus group study of nursing home leaders’ perceptions of elder abuse and neglect. BMC Health Services Research 20(1):199.
NASEM (National Academies of Sciences, Engineering, and Medicine). 2017. Communities in action: Pathways to health equity. Washington, DC: The National Academies Press.
NASEM. 2020. Social isolation and loneliness in older adults: Opportunities for the health care system. Washington, DC: The National Academies Press.
NIA (National Institute on Aging). 2017. What is long-term care? https://www.nia.nih.gov/health/what-long-term-care (accessed April 20, 2021).
NIC (National Investment Center for Seniors Housing & Care). 2021. Occupancy at U.S. skilled nursing facilities hits new low. https://www.nic.org/news-press/occupancy-at-u-s-skilled-nursing-facilities-hits-new-low (accessed January 6, 2022).
NQF (National Quality Forum). 2021. NQF. http://www.qualityforum.org (accessed February 2, 2021).
Paulin, E. 2021. Nursing homes are filled with empty beds, raising more concerns about care. https://www.aarp.org/caregiving/nursing-homes/info-2021/nursing-home-low-occupancy.html (accessed January 6, 2022).
Rantz, M. J., D. R. Mehr, L. Popejoy, M. Zwygart-Stauffacher, L. L. Hicks, V. Grando, V. S. Conn, R. Porter, J. Scott, and M. Maas. 1998. Nursing home care quality: A multidimensional theoretical model. Journal of Nursing Care Quality 12(3):30–46.
Rantz, M. J., M. Zwygart-Stauffacher, L. Popejoy, V. T. Grando, D. R. Mehr, L. L. Hicks, V. S. Conn, D. Wipke-Tevis, R. Porter, J. Bostick, M. Maas, and J. Scott. 1999. Nursing home care quality: A multidimensional theoretical model integrating the views of consumers and providers. Journal of Nursing Care Quality 14(1):16–37; quiz 85–87.
Rantz, M. J., M. Zwygart-Stauffacher, D. R. Mehr, G. F. Petroski, S. V. Owen, R. W. Madsen, M. Flesner, V. Conn, J. Bostick, R. Smith, and M. Maas. 2006. Field testing, refinement, and psychometric evaluation of a new measure of nursing home care quality. Journal of Nursing Measurement 14(2):129–148.
Rauch, J., M. Baxter, D. Quave, N. Yount, and D. Shaller. 2019. 2019 CAHPS health plan survey database, 2019 chartbook: What consumers say about their experiences with their health plans and medical care. https://cahpsdatabase.ahrq.gov/files/2019CAHPSHealthPlanChartbook.pdf (accessed February 25, 2021).
Scales, K., M. Lepore, R. A. Anderson, E. S. McConnell, Y. Song, B. Kang, K. Porter, T. Thach, and K. N. Corazzini. 2017. Person-directed care planning in nursing homes: Resident, family, and staff perspectives. Journal of Applied Gerontology 38(2):183–206.
Taylor, S., and S. Wilson. 2021. Initial observations of SNF trends data illustrates COVID-19 challenges. https://www.claconnect.com/resources/articles/2021/initial-observations-of-snf-trends-data-illustrates-covid-19-challenges (accessed January 20, 2022).
Tervalon, M., and J. Murray-Garcia. 1998. Cultural humility versus cultural competence: A critical distinction in defining physician training outcomes in multicultural education. Journal of Health Care for the Poor and Underserved 9(2):117–125.
U.S. Census Bureau. 2021. U.S. and world population clock. https://www.census.gov/popclock (accessed November 12, 2021).
Wiener, J. M., M. P. Freiman, D. Brown, and RTI International. 2007. Nursing home care quality: Twenty years after the Omnibus Budget Reconciliation Act of 1987. Durham, North Carolina: RTI International.






















