4
Systematizing Recovery Efforts to Mitigate the Next Pandemic
Without public trust in governments and science, it can be difficult for societies to overcome inequities and distrust during infectious disease epidemics and pandemics. By prioritizing community engagement and equity in efforts ranging from vaccination clinics to incident command structures, in addition to a continuous learning and improvement approach, the effects of future outbreaks can be mitigated. This chapter begins by highlighting the racial and social determinants of health (SDOH) that have become evident during the coronavirus disease 2019 (COVID-19) pandemic. Next, examples of community engagement were shared from across the world to highlight effective practices. Finally, several tools for recovery and capacity building were presented, including ensuring sustainable vaccine manufacture, creating a global pathogen monitoring network, and establishing a vaccine champion group to improve health literacy.
COMMUNITY ENGAGEMENT
Many SDOH emerged as key factors related to COVID-19 risk of exposure and severity for populations around the world. Engaging communities in a meaningful way can ensure that trust is built and existing disparities are incorporated in and accounted for within policy changes and public health measures. This section explores existing research on disparities, interventions, and case studies in community engagement.
Race, Health Disparities, and Community Engagement
Presented by Eliseo J. Pérez-Stable,
National Institute on Minority Health and Health Disparities,
National Institutes of Health
Eliseo J. Pérez-Stable, director of the National Institute on Minority Health and Health Disparities (NIMHD) at the National Institutes of Health (NIH), highlighted how racism, discrimination, SDOH, and a need for better community engagement were evident and influential during COVID-19, and how they are relevant to other present and future public health challenges.
Race and Health Disparities
Pérez-Stable explained that the existing racial, ethnic, and health disparities among Black, Latino/a/x, Indigenous, working, and disadvantaged people came to the forefront during COVID-19.1 For instance, COVID-19 has highlighted that race, ethnicity, and socioeconomic status are predictors for many negative health outcomes such as stroke and type 2 diabetes, even when controlling for other factors such as behavior (Gu et al., 2020).
More specifically, the killing of George Floyd, which coincided with the COVID-19 pandemic, raised awareness that structural racism and discrimination are still present.2 For instance, Pérez-Stable explained that the Kaiser Family Foundation Survey on Race shows that 53 percent of African Americans and 36 percent of Latinos in the United States experienced racism in the last 30 days (DiJulio et al., 2015). Pérez-Stable noted that race-related discussions and coalitions have recently increased in corporate, academic, and business organizations, creating a window of opportunity to act. He explained that currently most of the research on racism has been on an interpersonal level, but internalized and structural racism should also be addressed in research to create solutions that remove it.
NIH is currently conducting research on structural racism, both to describe it and to address it through interventions (HHS, 2021a). Furthermore, Chandy John, Ryan White Professor of Pediatric Infectious Diseases at Indiana University School of Medicine, added that structural racism should be discussed in medical and public health institutions. Laura Chanchien Parajón, deputy secretary of health at the New Mexico Department of Health, agreed that structural racism, community engagement, and empowerment are often not emphasized enough in medical school education. To allow for open, scientific, and forward-thinking discussions
___________________
1 Latinx is an emergent term used to describe gender-expansive people of Latin American origin or descent. See https://doi.org/10.2105/AJPH.2021.306238 (accessed March 10, 2022).
2 See https://www.nytimes.com/article/george-floyd.html (accessed January 24, 2022).
about racism, Pérez-Stable explained, blame and politics should be removed from the discourse. He added that leaders within an organization should take a stance against racism and initiate conversations about race within the whole organization instead of designating race discussions to a single person within an organization.
Structural and social determinants of health, rather than biological or behavioral determinants, are the cause of these disparities. Pérez-Stable noted that a combination of racism, discrimination, and an underserved health care system creates social disadvantage among certain populations, leading to a disparity in health outcomes. For example, Pérez-Stable described that observational cohort studies have shown that Black people suffer twice as much from strokes linked to high systolic blood pressure as compared to White people, adjusting for other stroke risk factors (Howard et al., 2013). A lesson from the COVID-19 pandemic has been that greater systematic policy and research attention needs to be given to the structural determinants and SDOH, such as access to affordable housing, green space and sidewalks, broadband internet access, public transportation, quality schools and education, economic and employment opportunities, public safety and criminal justice issues, and access to affordable food. Pérez-Stable explained that these factors should be seen as “factors that build health, not just create more resources for populations.” It is important, he highlighted, to conduct further research on health outcome differences between various populations. One example of such research is the Research Framework from the National Institute on Minority Health and Health Disparities (NIMHD, 2018), which emphasizes how societal, community, interpersonal, and individual factors interact with the different domains of influence (biological, behavioral, physical/built environment, and health care system).
Community Engagement
The Moderna vaccine trials, Pérez-Stable explained, elucidated that increased structure in community engagement is necessary to achieve diversity in study participation, which requires time, investments, and infrastructure.3 The Moderna vaccine trials were initially not as inclusive of underserved minority populations as leaders had hoped.4 Therefore,
___________________
3 At the time of the workshop, a vaccine to protect against COVID-19 that is made by Moderna has received emergency use authorization from the U.S. Food and Drug Administration. See https://www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/covid-19-vaccines (accessed January 24, 2022).
4 See https://www.reuters.com/article/us-health-coronavirus-vaccine-moderna-ex/exclusive-moderna-vaccine-trial-contractors-fail-to-enroll-enough-minorities-prompting-slowdown-idUSKBN26R1SP (accessed January 24, 2022).
Pérez-Stable explained, Moderna paused vaccine trial recruitment of White Americans in order to increase diversity within their trials. As a result, 37 percent of the vaccine trial participants were people of color. This is the minimum acceptable percentage for demographic representation, especially considering that greater than 50 percent of patients with COVID-19 were people of color, Pérez-Stable emphasized. The lesson learned was that a company should have a set goal for inclusive participation within their trials as well as a systematic plan on how to reach out to people, rather than assuming that individuals will volunteer. Other companies, such as NovaGen and Janssen, followed Moderna in striving for diversity and implemented Moderna’s approaches.
Another example of community engagement with vulnerable populations is the Rapid Acceleration of Diagnostics—Underserved Populations,5 funded by NIH in 2020 to create partnerships between scientists, communities, and public health departments. The national program helped distribute two million COVID-19 tests and partnered with a coordination and data collection center. Another similar example of community engagement is the Community Engagement Alliance (CEAL) initiative, which focused on inclusive research through COVID-19 awareness and communication.6 This initiative allowed academic researchers who are familiar with community engagement to partner with community organizations, health departments, and other organizations that might be interested in health and health disparities, such as the National Association for the Advancement of Colored People, as well as faith-based and advocacy-based organizations. Pérez-Stable said that CEAL could be a framework for future community-engaged research. Systematic and scientific communication are ways to gain the population’s trust in science; simply providing correct information to the public is not enough, Pérez-Stable said. Moderna’s challenge of achieving diversity indicates that one of the keys to engaging diverse communities is building trust.
Potential Interventions
There are some potential interventions within the health care system that have been shown to reduce disparities, Pérez-Stable said. Expanding access to health insurance, such as in the Affordable Care Act, would help reduce inequality. He also stated there are certain activities that are not implemented well despite the existence of public health consensus,
___________________
5 For more on the Rapid Acceleration of Diagnostics-Underserved Populations, see https://radx-up.org (accessed January 24, 2022).
6 For more on the CEAL initiative, see https://covid19community.nih.gov (accessed January 24, 2022).
such as controlling high blood pressure or diabetes, with disadvantaged groups being the most affected. Additionally, coordination of care should be improved. More specifically, health care navigators and targeted care can help individuals obtain the right care depending on their needs. Patient-centered care can be further enhanced by focusing on effective communication and cultural competence, he said, as well as creating performance measurements that help track the efficiency of equity efforts.
Finally, he advocated for increasing workforce diversity to reduce disparities. A 2018 study among graduating medical students revealed that students of underrepresented minority backgrounds were more likely to report an intent to work in underserved populations and to accept uninsured and/or Medicaid patients, after adjusting for physician specialty, gender, and debt (Garcia et al., 2018). Increasing the diversity of the health care workforce will therefore increase the number of physicians serving vulnerable populations, Pérez-Stable suggested. However, there is much work to be done. Of all medical school graduates in 2020, only 7 percent were Latino/a/x, 7 percent were African American, and less than 0.002 percent were American Indian. Beyond health care and within the research sector, only 7 percent of all NIH R01 grants, some of the most coveted and competitive awards, are given to African American and Latino/a/x principal investigators, and 14 percent of all new science, technology, engineering, and mathematics degrees are awarded to underrepresented minority scientists (AAMC, 2021).
Case Studies in Community Engagement
Various case studies in community engagement worldwide are described in the following section, including their aims, methods, challenges, and lessons learned. The initiatives described include the Penn Medicine Center vaccination clinic in Philadelphia, the NewYork-Presbyterian Hospital in New York City, the COVID-19 response of the New Mexico Department of Health, and community engagement strategies in Paraguay.
Care Equity in Philadelphia
Lauren Hahn, senior innovation manager at Penn Medicine Center for Digital Health, also highlighted the evident inequalities during COVID-19 and the need for “intentional efforts to reduce these disparities.” COVID-19 vaccination rates are associated with race and wealth, she stated. For instance, as of March 2021, only 25 percent of Black Americans in Philadelphia (whose population is 42 percent Black) are vaccinated, compared to almost 50 percent of White Americans within that same region. To close COVID-19 vaccination gaps and provide equitable
access, Hahn said that health care centers should proactively engage the community rather than expect members of the community to reach out and seek the care and information they need. To foster lasting community engagement, the Penn Medicine Center for Digital Health created a rotating community vaccine clinic that used rapid cycle innovation, proactive outreach, intentional engagement, novel workflows, and tools that were easy to use (Lee, 2021). The clinic’s success, according to Hahn, can be summarized in three guiding steps: partner, codesign, iterate.
The first key factor in the success of the Penn Medicine Center vaccination clinic was an emphasis on multidisciplinary partnerships, both from within the hospital and the community, Hahn explained. For instance, outpatient health care professionals were redirected to infectious disease and emergency preparedness. Community partnerships included collaboration with Black pastors in Philadelphia, barber shops, hair salons, community organizers, and Black-owned radio shows. The vaccine clinic also ensured that health care workers and volunteers represented the diverse makeup of the community. She noted that such collaborations with multidisciplinary members and organizations within the community helped increase trust in vaccination by bridging health care and community.
The second key factor to the clinic’s success was codesigning the clinic with community members, taking their needs into account. First, geographic barriers to access were addressed by placing vaccination clinics within the communities where they were needed. Second, technological barriers such as complicated apps and web forms were also addressed by codesigning with community stakeholders to develop no- and low-tech scheduling methods such as text (Way to Health) and call systems in different languages. Third, community engagement was encouraged by nudging patients to become vaccine ambassadors, who would be able to sign up loved ones for a vaccine appointment. Nudging the community to get vaccinated was also achieved by encouraging patients to engage on social media by posting pictures of themselves with a life-size “I got the COVID-19 vaccine” photo frame. Fourth, long postvaccine pamphlets were replaced by image-based flyers and text messages.
The vaccine clinic also wanted to avoid the long waiting times and exclusionary appointment availabilities present in other vaccination clinics, said Hahn. One solution was to prioritize patients with disabilities or elderly patients. Other solutions included organizing clinics in modules or pods that could be rearranged as necessary, conducting group rather than individual consent, and using visual tools such as “Ready” signs that indicated staff members were ready to administer a vaccine. Additionally, patient information was collected during the sign-up process to avoid filling out long registration forms at check-in during the patient’s vaccination appointment. Initially, the documentation process was conducted in Excel,
but it was subsequently digitized after determining the best documentation and scheduling method. Hahn said that these methods improved “operational efficiency and the overall experience of the clinic” by reducing wait times.
She highlighted the third key to the clinic’s success by emphasizing an iterative process, which allowed for change as feedback emerged from the community and other stakeholders. The transition from paper to digital patient documentation is one example of how the clinic improved in subsequent iterations. Additionally, patient feedback was obtained to improve the vaccination process. In summary, Hahn said that over a three-month period the clinic administered more than 7,500 vaccines to community members, 85 percent of whom self-identified as Black or Brown. There was also a 99.4 percent rate of second vaccination, and currently 56 percent of Black residents in Philadelphia are vaccinated, which is higher than many other U.S. cities with a large Black population. Following the success of this work, Hahn and her team published a guide on how to design and implement similar projects (Lee et al., 2021).
Hospital Community Partnership
Patricia Peretz, lead of the Center for Community Health Navigation (CCHN) at NewYork-Presbyterian Hospital, described two community-centered initiatives that also addressed the need to improve patient access to health care.7 CCHN was developed over the last 15 years out of the emergency department, Peretz explained. The community health workers (CHWs) program began as an effort to respond to frequent visits to the emergency department by pediatric asthma patients in northern Manhattan. The program was subsequently expanded to include not only pediatric patients but also all adult cases in branches of several New York City boroughs. The CHW program was also adapted to all emergency department patients and was called the Patient Navigator Model, which was then subsequently expanded to include inpatient cases (Garbers et al., 2016). In 2020, the CHW program was again adapted to integrate into the COVID-19 response (Peretz et al., 2020).
CHWs and patient navigators, employed by social support organizations, are embedded in the hospital health care team, Peretz explained, so they can tackle SDOH within health care services. The role of the CHWs is to collaborate with physicians and empower patients who may face barriers in obtaining health care by, for instance, ensuring that patients adhere to follow-up appointments, obtain a primary care provider, schedule
___________________
7 For more on the CCHN initiatives, see https://www.nyp.org/acn/community-programs/center-for-community-health-navigation (accessed January 24, 2022).
appointments that may be inaccessible because of digitalization, connect to financial or insurance resources, or obtain a patient-centered medical home. Needs that cannot be met directly through health care services are addressed by CHWs using a network of care, which includes partnerships with third-party organizations that provide various services such as housing, food, immigration, or domestic violence support.
Adriana Matiz, medical director of NewYork-Presbyterian Hospital’s Center for Community Health Navigation and associate professor of Pediatrics at Columbia University Medical Center, gave an example of a patient who benefited from the medical center’s CHW program. She was a recent undocumented immigrant and a mother of two children with developmental delays. The provider referred the mother to the CHW program, recommending that the mother be aided in applying for benefits. The mother identified her goals as Supplemental Nutrition Assistance Program (SNAP) enrollment and family/relationship counseling. As a result, she was referred to supporting programs including SNAP, legal services for eviction issues, and Bake Back America, and was aided in setting up her health care patient portal. Several weeks later, an emergency domestic violence incident occurred, and because the mother trusted the CHW, she called that individual. Ultimately, the police were involved, and language interpretation support was also provided. Matiz said that several lessons can be learned from this example. First, this case highlights that patients often require support in ways that are not readily visible from a single hospital visit. Second, trust is a key factor that allows CHWs to understand patients from a clinical, community, and personal perspective. Third, the CHW partnership allowed for care that addresses key SDOH instead of treating surface-level symptoms only.
Peretz reported on the success of the CHW program, saying that among adult CHW program participants from 2012 to 2021 with diabetes, 62 percent experienced decreases in their HbA1C levels,8 and 89 percent met their medication management goals. Within the pediatric asthma CHW program, hospitalizations decreased by 76 percent and emergency department visits decreased by 68 percent, she added. The patient navigator program was able to achieve 76 percent adherence to postdischarge follow-up appointments, compared to the national average of 20 to 40 percent adherence rate. CHWs also aided 6,100 patients to schedule a COVID-19 vaccine. Additionally, nearly 20,000 proactive wellness checks were conducted via phone, which consisted of asking patients what needs they had, such as food, shelter, connection to a provider, internet access, or even video chat troubleshooting to help patients connect with family.
___________________
8 Hemoglobin A1C (HbA1C) is used to measure blood glucose concentration in the management of diabetes mellitus. See https://medlineplus.gov/lab-tests/hemoglobin-a1c-hba1c-test (accessed January 24, 2022).
Peretz highlighted several essential factors to any community-based program. First, developing trust with community organizations through communication and coplanning is paramount. Second, aligning with hospital and strategic initiatives would ensure that an intervention is accepted and sustained within the community and the health care system. Third, Peretz said that employing CHWs who represent the community would increase trust in the program. Fourth, she highlighted the importance of supporting patients in increasing their familiarity and comfort level with the digitization of health care. Finally, integrating CHWs within health care as team members and within advisory boards and committees would allow for them to “offer their unique perspective and advocate on behalf of our patient populations.”
Embedding Equity into an Incident Command Structure: Lessons Learned from the New Mexico Department of Health Vaccine Team
Laura Chanchien Parajón, deputy secretary of health at the New Mexico Department of Health, introduced how public health organizations can use an incident command structure (ICS) to systematize efforts and prioritize equity. Parajón explained that as the number of available vaccines increased in New Mexico, the system became overwhelmed, resulting in challenges with internal and external communication, lack of clarity around roles, lack of systematic data collections, and an unclear chain of command as the complexity of operations outgrew the existing structure for vaccine distribution. This made it difficult to both assess equity and to implement efforts to achieve equity in the vaccine effort. With the help of the Federal Emergency Management Agency (FEMA), the New Mexico Department of Health vaccine team implemented an equity-driven ICS structure that prioritized equitable vaccine distribution. Parajón explained that ICS is a systematic management tool traditionally used in firefighting or disasters to organize resources, staff, facilities, communications, and other aspects of an emergency response. A community vaccine equity task force was part of the ICS, which ensured that underserved communities were prioritized in responses such as mobile team support.
Miranda Durham, the northwest region health officer and vaccine planning chief for the New Mexico Department of Health, explained that another important aspect of achieving equity using the ICS was establishing regular staff meetings that include data teams, CHWs, medical students, and public health professionals. During these meetings, staff identified priorities, set objectives, and developed strategies to meet the objectives; then they evaluated outcomes and subsequently identified new priorities and continued the circular process. The ICS included a functional data team, which was vital to consolidating data from various sources.
Including community feedback into the ICS was also important when developing an equitable vaccine distribution system. For instance, CHWs and medical students were able to use the Centers for Disease Control and Prevention (CDC) Rapid Community Assessment Tool in Albuquerque to identify some barriers in access to vaccines: registration app, lack of knowledge regarding whether there is vaccination fee, and confusion about vaccine transportation assistance. The community was also involved in proposing possible solutions: alternative registration methods, increased support in using the registration app, clear messages about free vaccination, paid time from work to be vaccinated, or accessible vaccination sites, especially in Latino/a/x communities. As a result, a FEMA mobile unit was mobilized in these neighborhoods to make vaccines more geographically accessible. Extended hours, walk-in services, and community outreach through CHWs were provided, along with incentives such as food bags after vaccination and communication regarding individual vaccine questions. Additionally, the data team continuously analyzed COVID-19 rates by race, region, and ethnicity, allowing interventions to be targeted and efficient.
Lessons from Paraguay
Guillermo Sequera, the general director of National Health Surveillance in the Ministry of Health and Social Welfare of Paraguay, began by describing a timeline of total COVID-19 cases in Paraguay and then discussed structural factors affecting the COVID-19 response. Sequera explained that Paraguay adopted a strict lockdown at the beginning of the COVID-19 pandemic (see Figure 4-1, period 1), thus preventing the COVID-19 surge seen in other South American countries. Deescalation of the lockdown was gradually adopted (see Figure 4-1, period 2), Sequera said. But starting January 2021, Sequera noted that the COVID-19 Gamma/P1 variant increased dramatically within the population, with an excess mortality rate of greater than 70 percent (see Figure 4-1, period 3).
Sequera discussed various factors that influence community participation in, and perception of, public health policies and interventions. He said that community engagement is usually low in Paraguay for several reasons. Health policies are highly centralized, leading communities to be seen as beneficiaries or supporters of existing policies rather than active stakeholders that shape health policy. Furthermore, lack of trust in political leadership has also eroded community willingness to engage in public health. Poverty and inequality, lack of knowledge of rights within the general population, government’s lack of recognition of minorities and diversity, and weak development of social organizations all exacerbate low community participation, Sequera added.
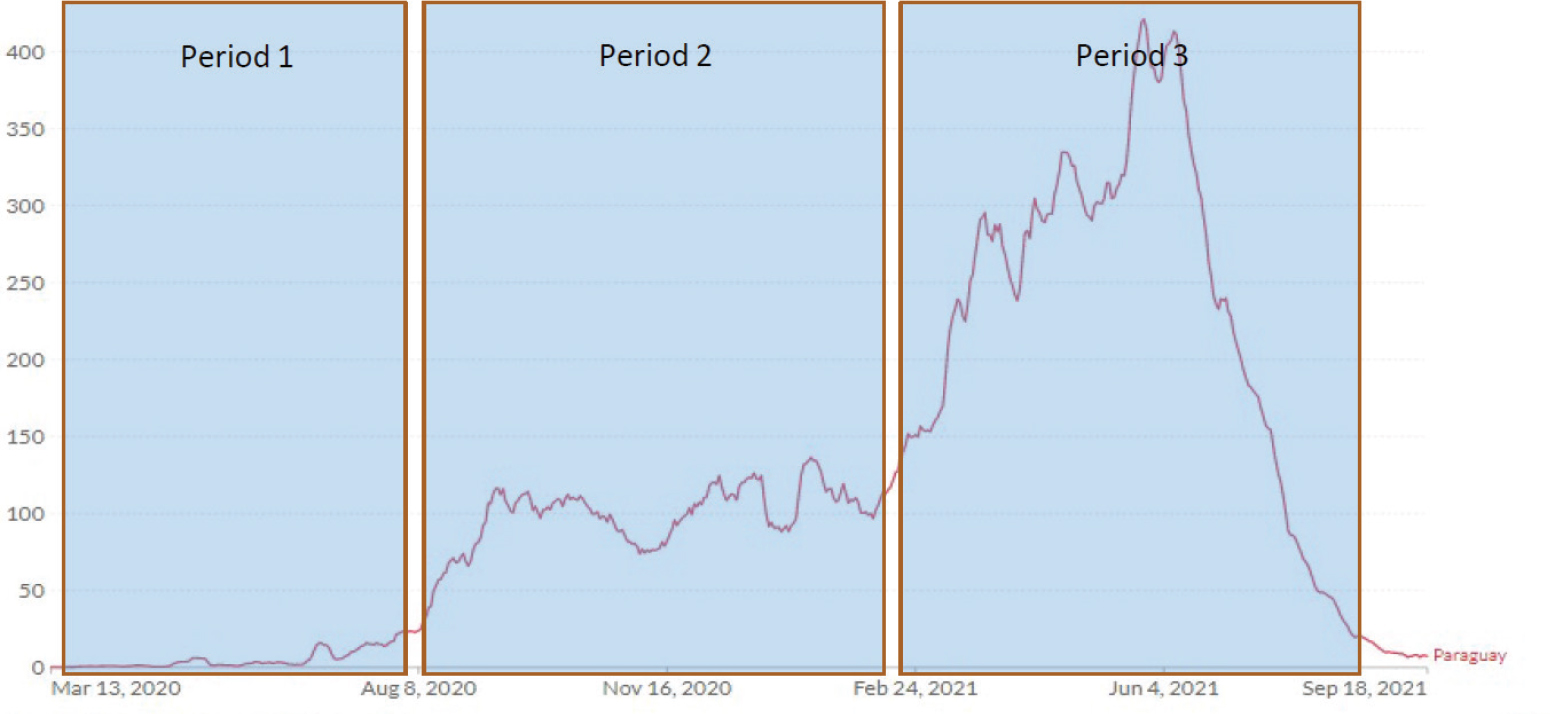
SOURCES: Guillermo Sequera presentation, September 23, 2021; Johns Hopkins University CSSE COVID-19 Data.
Next, Sequera described how political leadership and trust in authorities changed during the three periods of the COVID-19 pandemic in Paraguay, exemplifying their importance and interconnection. The low COVID-19 rates of period 1 in Paraguay led neighboring countries to have positive perceptions of Paraguay’s overall national pandemic strategy. Indeed, leadership in Paraguay had a good communication strategy, he noted. Additionally, the health ministry of Paraguay was for the first time able to have influence over broader national policy formulation. There was also increased transparency of health data within the country. Together, confident leadership, a good communication strategy, transparency, multidisciplinary policy teams, low COVID-19 rates, and international recognition of Paraguay’s success helped citizens trust government, scientific, and epidemiological information, Sequera explained. During period 3, however, the government and public health ministry were overwhelmed with COVID-19 cases. Because of geopolitical logistical concerns, Sequera said, Paraguay was also one of the last countries in the region to access available vaccines and begin mass immunization campaigns for COVID-19. These two factors eroded existing public trust and community engagement.
Another critical structural determinant that was important to address during the pandemic, Sequera added, was that of gender and caregiving roles. Unfortunately, rape and domestic violence cases increased during the lockdown in period 1 in Paraguay. Additionally, women predominantly fill caregiving roles, Sequera noted, with 70 percent of the health personnel being women, who are also caring for their children, extended family, husbands, and grieving loved ones. Sequera highlighted the importance of including women in panel discussions and policy formulations regarding grief and pandemic effects. He also warned against solely prioritizing large hospital facilities over primary care facilities, which are predominantly staffed with women, in terms of financial support and policies.
Finally, community trust and mobilization were important factors that helped individuals cope with the pandemic. Sequera explained that “we have to generate trust not only to authorities but there has to be trust [with]in the community.” For example, Sequera explained how community-organized kitchens, which were partially sponsored by the government and were seen in both wealthy and poor communities, helped promote trust within communities. These events were especially important when COVID-19 cases increased during period 3 of the pandemic because they improved communities’ social and mental health and helped members exchange medicines, ideas, and other resources. Sequera advocated for more of these types of events.
Another such event, Sequera explained, is something called polladas, which are community fundraising efforts to support individuals in need. These community mobilization efforts were quite effective in financially
helping vulnerable individuals through bake sales, raffles, and other methods. Polladas were so influential, and numerous, Sequera explained, that they were even able to put pressure on the president of Paraguay to replace members of his cabinet. They also led the government to realize the need to reform the public health system. Other community organizations, such as the Protestant and Catholic churches, were also influential in increasing community trust and reaching vulnerable and vaccine-hesitant populations. Finally, he shared that collaboration with Paraguay’s academic sector was important in transitioning the country from importing personal protective equipment to producing those products nationally.
Discussion
John asked why Paraguay saw such a rapid decrease in COVID-19 cases after period 3. Sequera said “It is probable that half of the population of the country, especially in the major cities, may have had” COVID-19, contributing to levels of immunity. Another reason could be the high vaccination rates at that point, especially among young people. John also asked how community engagement can be institutionalized, through policies and programs, for COVID-19 and other current and future health challenges. Nudging patients through behavioral design concepts is an effective method to encourage them to engage with their own communities, Hahn replied. For instance, she described how the COVID-19 vaccine scheduling app reminded patients to share information with friends and family. The app made sharing easy so patients are more likely to do it. This nudging to increase community engagement was used for COVID-19, but it can be applied to colonoscopies, annual influenza vaccines, and other health-related behaviors.
Peretz noted that community members should be included in health policy decisions as team members. Sequera agreed, explaining that if community members are not included as active stakeholders, they are less likely to support public health initiatives. Parajón emphasized the need for continuous evaluation of these community engagement efforts, noting that community engagement must happen with a proper structure, plan, data-gathering mechanism, and sufficient staff who can analyze and operationalize the data. Evaluation related to community engagement can then be used to maximize the efficiency of community outreach efforts.
In response to a question about how equity can be promoted in regions where it is not a priority, both Parajón and Hahn noted that focusing on communities would be key. Building evidence for the need for equity, and garnering support within communities would help push equity to policy agendas, they explained. Parajón suggested Paraguay’s community engagement strategy as a successful example.
AVAILABLE TOOLS FOR RECOVERY AND FUTURE CAPACITY BUILDING
Simone Blayer, global head of Chemistry, Manufacturing, Control, and Nonclinical Toxicology at PATH, discussed several areas that require attention to ensure sustainable vaccine manufacture. First, he emphasized the importance of improving workforce training globally, especially in low- and middle-income countries (LMICs). Training related to manufacture and quality control is essential, he said, for new and existing technologies. Second, Blayer highlighted the need for tech transfer hubs, which would allow for large-scale vaccine manufacturing in LMICs. Third, he noted the importance of innovation and entrepreneurial incubators. Support for innovation and tech transfer can be achieved through effective models, such as the Analytical Method Transfer guidelines. Fourth, a predictable and consistent supply chain network, especially in LMICs, can be achieved, but it requires diverse partnerships with nongovernmental organizations (NGOs), donors, and other organizations. Finally, he said, other supply chain issues that need attention when addressing vaccine manufacture sustainability are packaging, cold chain/thermostability, route and method of delivery, and waste disposal.
Joseph DeRisi, chair of the Department of Biochemistry and Biophysics at the University of California, San Francisco, and copresident of the Chan Zuckerberg Biohub, described his work on the establishment of a global emerging pathogen monitoring network as a useful “early warning radar” tool. He then listed several barriers to access in LMICs and gave suggestions on how those barriers can be overcome, including a global pathogen monitoring network. Unlike polymerase chain reaction assays that search for an expected result, etagenomic sequencing detects new and emerging pathogens without bias and hypothesis. DeRisi said that this technology can be applied to many different settings to predict emerging pathogens. The barrier to access in LMICs is not financial, but rather training, supply logistics, and data storage.
Echoing Blayer’s remarks on the importance of tech transfer, he said that simply giving equipment to scientists in LMICs is not sufficient. Instead, creating programs that train local scientists to use the technology would ensure sustainability and functionality, DeRisi said. Another barrier that scientists in LMICs face is storage of data. But because cloud storage is now accessible and relatively cheap, it is an effective solution to the data storage barrier. DeRisi said that currently, his laboratory is working to create a global emerging pathogen monitoring network, which can aid in rapid dissemination, uniformity of analysis, and increased international transparency of emerging pathogens. So far DeRisi and his team have introduced their system in 11 countries. Additionally, metagenomic sequencing was the
first to detect and sequence the whole COVID-19 genome from a tourist from China; prior to that, most of the COVID-19 data was in China.
Syra Madad, senior director of the System-wide Special Pathogens Program at New York City Health + Hospitals, discussed three challenges in communication and gave possible solutions for each. First, she said, limited health literacy in the general public means that individuals do not have the proper information to make informed decisions or do not know when or how to seek health care services, leading to higher rates of hospitalizations, emergency room visits, and vaccine hesitancy, and lower rates of preventative measure uptake. Second, Madad said that “ongoing, consistent, and reliable science and risk communication” would help health care workers and the general public to better support evidence-based public health measures. Third, Madad pointed out that public health emergencies must rely on routine and preestablished protocols rather than innovations during times of an emergency. This means that emergency response needs to be considered before an emergency, she explained. The first tool Madad presented was the Vaccine Champion Group, which trains community members on evidence-based communication strategies that they use with members of their social circle to educate them about various public health efforts. Individuals were trained on “how to break the ice in terms of starting a conversation, word choice, phrase choices, how to address misinformation and debunk myths.” This method worked particularly well, Madad explained, because it harnessed the power of social capital when trust in science is low. The second tool Madad presented addressed science and risk communication. She said that the electronic medical record (EMR) system’s patient web portal (such as MyChart) is frequently used by patients to receive test results and suggested it can be harnessed for two-way health communication. Additionally, individuals should have the ability to ask questions and engage with the EMR messages. The third tool Madad described was the Commissioned Corps of the U.S. Public Health Service, allowing public health “foot soldiers” to reach out to the most vulnerable populations and provide information about services and engage with individuals regarding public health topics.9
David Cutler, professor of applied economics in the Department of Economics at Harvard University, presented several global lessons from COVID-19. The first, Cutler explained, is the need for a nonpolitical global scientific public health organization. The challenge that the World Health Organization faces, according to Cutler, is that it is both a scientific and a political organization. Second, Cutler called for national reform of health care systems within the United States and other countries. More specifically,
___________________
9 For more on the Commissioned Corps of the U.S. Public Health Service, see https://www.usphs.gov (accessed January 24, 2022).
he called for a shift in the system toward a focus on identifying and achieving public health goals, rather than simply responding to illnesses that have already occurred. The success of such countries as Taiwan, South Korea, and Australia during COVID-19 was in part attributable to their emphasis on public health measures, Cutler explained.
Third, Cutler emphasized that inequalities should be addressed through a collective mindset because communicable diseases like COVID-19 affect the rich and poor alike. For instance, certain COVID-19 risk factors such as obesity, opioids, or smoking, which were previously thought of as problems for disadvantaged communities, are now affecting everyone: “Our health is only as good as the health of the bottom.” The interconnectedness of health on local, regional, and international levels means that increased and timely coordination and transparency between countries is necessary.
Panel Discussion
Good tools and innovations are not always effective if the environment is not receptive to those advances, said Margaret E. Kruk, professor of health systems at the Harvard T. H. Chan School of Public Health. She asked how the receptiveness to innovation seen during COVID-19 can be continued. Blayer agreed that COVID-19 has led to increased investment, financial and otherwise, in innovative technology. The unprecedented global collaboration seen during COVID-19 will be key in sustaining these investments after the pandemic, he said. DeRisi added that economic incentive is a factor that sustains receptiveness to innovation because “there’s a price to not having information,” such as new virus variants or new pathogens. Furthermore, Cutler believed that strong scientific support within public health, as seen regarding climate change, will help propel commitment to public health innovation and investment. It would also be important to incentivize multidisciplinary collaboration between public health and health care, Madad and Kruk emphasized. Madad explained that this collaboration would be better enabled by joint funding.
In response to a question about how evidence-based communication can be incorporated more in public health efforts, Madad said that communication should focus on prevention through improving health literacy. She said that this communication should not be happening only in health care facilities, but on a local and everyday level. To make communication effective, Madad highlighted the need to employ CHWs and communicators who are racially and ethnically representative of the community they are trying to reach. Additionally, Madad explained that health care is about medical interventions and connecting individuals to resources that would improve their lives. For instance, informing households of a food delivery service or isolation hotels is also an important part of public health
communication. Furthermore, Kruk added that informing the public of how their information will be used can help individuals feel safer and more willing to allow public health officials to collect their data, which can then be used for more effective public health communication and interventions.
The notion that “no one is safe until everyone is safe” is well known, but it has yet to be acted upon on an international level; many LMICs are still largely unvaccinated, Kruk said. She asked how equity can be achieved on a global scale. Cutler replied that high-income countries should view their support of LMICs not as foreign aid, but as national policy that also benefits the health of their own countries.
This page intentionally left blank.


















