5
Strategies for a Post-COVID World
While many people are eagerly awaiting the end of the coronavirus disease 2019 (COVID-19) pandemic, there is near certain agreement that this will not be the last time a novel pathogen emerges and affects the world in so many ways (Marani et al., 2021). Critical research to mitigate the effects of future outbreaks is ongoing, and there are many lessons that can be drawn from this and previous infectious disease outbreaks to inform future emergencies. This chapter begins with visions for biomedical preparedness research, public health measures, and nonpharmaceutical interventions that can be taken to improve future outcomes. It then discusses the findings and lessons from an exercise of scenario planning that was undertaken by workshop participants. This hypothetical exercise outlined a situation where a new coronavirus variant that could evade vaccine-induced immunity has emerged and is spreading through the United States.1 Finally, workshop planning members commented on the needs highlighted throughout workshop discussions and the opportunities for improved pandemic and health emergency planning to ensure the global crisis that COVID-19 brought on is not repeated.
VISIONS FOR THE FUTURE
For a broader perspective on the current pandemic and what future pandemics may hold, two speakers provided keynote presentations that
___________________
1 This scenario exercise was prepared and took place prior to the detection of the Omicron variant in November 2021.
focused on the dual approaches that could improve our society’s health and preparedness for future disease threats. The first presentation was on biomedical research, highlighting the preventive and mitigation tools being developed within that enterprise for this and future potential pathogens. The second presentation discussed public health and societal measures that can protect populations and improve outcomes the next time this type of health emergency occurs.
Pandemic Preparedness: The Biomedical Research Approach
Presented by Anthony Fauci, National Institutes of Health
Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases at the National Institutes of Health (NIH), discussed three aspects of biomedical research for pandemic preparedness: the basic research portfolio, research capacity, and countermeasure development. He pointed out that countermeasure development falls into two major buckets: vaccines and therapeutics. Vaccine development can be further separated into preparedness and response, Fauci described, and focused his remarks on preparedness, for which NIH has taken a three-part approach. The first part is the priority pathogen approach, which includes identifying and selecting priority pathogens as delineated by the World Health Organization (WHO) Research and Development blueprint for priority diseases, and then preparing for specific microbes in question. The Coalition for Epidemic Preparedness Innovation (CEPI) also has a list of priority diseases, such as Ebola, Lassa fever, and Middle East respiratory syndrome (MERS), in addition to COVID-19. Similar lists have been developed by NIH and others. The priority pathogen approach has advantages and disadvantages, as very often new challenges emerge that were not anticipated.
The second approach for vaccine development for pandemic preparedness is the platform approach, he noted, in which various vaccine technologies are developed and improved upon. This has been undertaken quite well by various actors in the field, as platforms have been perfected and applied and used for multiple different pathogens. For example, various platforms include those that use nucleic acids (e.g., for diseases such as SARS, MERS, West Nile fever), viral vectors (e.g., for diseases such as Ebola and Zika), recombinant proteins (e.g., for diseases such as influenza and respiratory syncytial virus [RSV]), and nanoparticles (e.g., for diseases such as influenza, malaria, and RSV). We have come a long way from the initial live attenuated virus approach, he noted, to now using platforms that have enhanced our ability to make an immune response.
The third approach, and the area of active research that Fauci was most excited to share, is the prototype pathogen approach, whereby scientists take
families of viruses (e.g., the genus of flaviviruses) and build on prior experiences with viruses from that family to rapidly respond to newly emergent pathogens that belong to the same family. In other words, he said, researchers use strategies and tools that were successfully applied to another virus and translate those to related virus vaccine design. This strategy employs basic virology principles, assays for preclinical and clinical settings, animal models, antigenic targets, potential immune correlates, and manufacturing strategies.
Therapeutics is the other major component of countermeasure development. In this realm, there has also been recent progress. In June 2021, the Biden administration invested $3.2 billion from the American Rescue Plan as part of the COVID-19 antiviral development strategy (HHS, 2021b). Fauci explained that this is a “whole-of-government effort, not only for COVID-19, but for future virus threats” too. This effort is referred to as the Antiviral Program for Pandemics (APP) and it “aims to catalyze the development of new medicines to combat COVID-19 and prepare for other pandemic threats.” This includes some of the known diseases and viruses that have pandemic potential, but for which few treatments exist. The approach of APP, he explained, is two-pronged and includes the development of countermeasures that are in various stages of existence (e.g., this may include the repurposing of antivirals for other diseases), as well as discovery, which expands basic science knowledge in discovering new antiviral medicines. This approach was very successful in the development of drugs for human immunodeficiency virus (HIV), which transformed the lives of millions currently living with the disease.
Fauci outlined the next steps in the APP approach, including continued engagement with manufacturers to accelerate testing and authorization of promising medicines in late-stage development, identification and evaluation of additional drug candidates for program support, and support of academia–industry partnerships that aim to discover new molecules. In conclusion, he mentioned that in September 2021, the Office of Science and Technology Policy at the White House released a $65.3 billion proposal for a program to transform the way the United States responds to pandemics (Cohen, 2021).2 This will be accomplished in part by vastly accelerating vaccine development, testing, and production. The program includes five pillars, with the first being the most relevant to countermeasure development:
- Transforming our medical defenses
- Ensuring situational awareness
- Strengthening public health systems
___________________
2 For more on this program, modeled after the Apollo space mission, see https://www.whitehouse.gov/briefing-room/statements-releases/2021/09/03/fact-sheet-biden-administration-to-transform-capabilities-for-pandemic-preparedness (accessed December 15, 2021).
- Building core capabilities
- Managing the mission
Lessons from COVID-19 and Opportunities to Improve Future Responses
Presented by Sandro Galea, Boston University School of Public Health
Galea noted that his remarks complement the biomedical research approaches outlined by Fauci and that both efforts are needed, not one over the other. Galea began by highlighting that a lot went right during COVID-19. For instance, mortality in New York decreased four-fold in the first three months after disease detection and spread in the city, which is quite remarkable for a clinical care system to learn that quickly, he pointed out, especially with the emergent nature of this disease (Horwitz et al., 2021). The most astonishing thing that has gone well in this experience has been the rapid development of effective vaccines. Two vaccines with 95 percent efficacy were developed and available to the public just eight months after clinical trials began (Ball, 2021)—this was a quantum leap advance that has been lifesaving.
While these things did go well, unfortunately, a lot also went wrong, he continued. In 2020, COVID-19 rose to become the third leading cause of death, which is extraordinary seeing as the world did not even know it existed in 2019. This demonstrates how dramatically things went wrong, and how the things that have gone wrong have done so very unevenly, Galea added. He shared a graph showing the change in life expectancy at birth by race and ethnicity, demonstrating the strikingly unequal outcomes for different populations resulting from COVID-19 (see Figure 5-1).
Galea went on to dissect why certain aspects of the COVID-19 pandemic went so wrong. He focused on two fundamental reasons, pointing out that first, there was an inequitable and unnecessary risk of even just getting COVID-19. Whether you were able to take precautions and protect yourself from others often comes down to your occupation and life and family environment, whether exposure to disease was inevitable, or whether you could easily stay home during quarantine periods. He noted that once the emergency was declared in March 2020, the wealthiest 20 percent of society in the United States stayed home much more than the poorest 20 percent.3 Additionally, he added, the more income a person has, the more ability they have to work remotely. Most people were actually unable to work remotely and safely distance themselves, and “that ability was socially, economically, and racially patterned.” Because of this, leaders and
___________________
3 See https://www.nytimes.com/interactive/2021/03/11/opinion/covid-inequality-race-gender.html (accessed February 16, 2022).
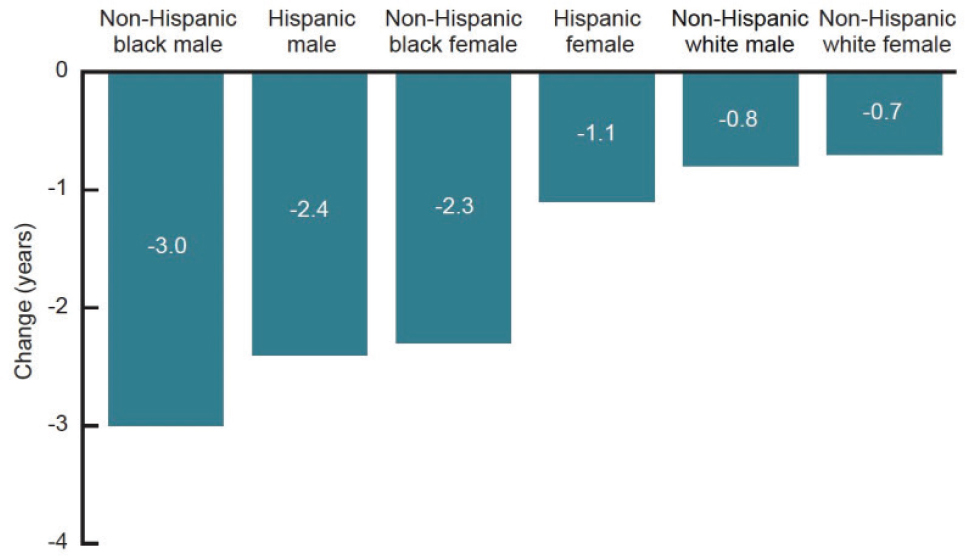
NOTES: The mortality data used in Arias et al., 2021, follow the 1997 standards from the Office of Management and Budget on Hispanic origin and race groups, which do not make a distinction between Hispanic and Latino. The term Hispanic was often used as a blanket term for this category. See https://obamawhitehouse.archives.gov/omb/fedreg_1997standards (accessed March 10, 2022).
SOURCES: Sandro Galea presentation, September 24, 2021; Arias et al., 2021.
public health authorities could not prevent a lot of people from unnecessary disease exposure.
Secondly, Galea noted, severe disease was also an inequitable risk, as demonstrated early on that those with comorbidities or other chronic conditions were more likely to suffer from severe disease. For decades in the United States, we have “underinvested in what makes us healthy,” he commented, and we have also made those investments inequitably.4 He shared data on racial income and wealth gaps between White and Black families in the United States from 1989 to 2016, saying that while White families have about 40 percent higher income than Black families on average, the gap in wealth is about 10-fold difference, with White families attaining much more wealth than Black families.5 This underinvestment and inequity,
___________________
4 See https://nam.edu/vital-directions-for-health-health-care-priorities-from-a-national-academy-of-medicine-initiative (accessed February 16, 2022).
5 See https://www.washingtonpost.com/us-policy/2019/03/14/new-explanation-stubborn-persistence-racial-wealth-gap (accessed February 16, 2022).
even before COVID-19, has resulted in the United States falling off in life expectancy, especially in comparison to other Organisation for Economic Co-operation and Development countries.6 He said this translates to a 5-year gap between the United States and countries with the highest life expectancy, so the United States is spending more but gaining less.
Leaders in government and health care sectors have continually invested in curative approaches and not preventive measures that we know can keep us healthy, and we also underinvested in measures that can specifically keep us healthy in a time of a pandemic. Much of this is because the United States does not have the infrastructure to deal with outbreaks like this, especially after years of underinvestment in public health infrastructure and surveillance.
In conclusion, Galea believed that investments in a healthy world need to be made before the next pandemic. We do not know what the disease will be, he said, so we should be investing in health across the board before then to truly mitigate the effects. He advocated for investments in a healthy world to ensure our own resiliency, which means actually investing in things like loneliness, parks, poverty, and housing. Secondly, there is a need to invest in science of consequence, where scientists can advance a comprehensive agenda to ensure that investments not only include vaccine development and biosurveillance but also create the kind of world that is robust enough to meet these types of viral threats. We need a comprehensive approach to deal with pandemic preparedness, he argued.
Matthew Zahn, Orange County Health Care Agency (California), offered that from a local public health perspective, one of the greatest difficulties has been messaging the importance of comorbidities but being careful not to blame the victims. As we move forward out of this pandemic, he asked, are there ways or opportunities to message the importance of underlying diseases without targeting the victims? Galea responded that it is incredibly important to make sure the challenge posed by underlying diseases is appropriately labeled and articulated without blaming the victim. Public health practitioners need to move away from behavioralist thinking, he said, and think more about systems and structures that individuals live within. For example, one of the primary drivers of obesity is the prevalence of calorie rich foods all around, but this has little to do with people’s behavior. One of the greatest success stories in public health has been the decline in motor vehicle deaths, he added, but this is not because people became better drivers. Instead, the creation of seatbelts and airbags and safer designs led to this change. This is the kind of world we need to build, he said, where there are healthier opportunities for everyone to live healthier lives.
___________________
6 See https://tincture.io/lets-increase-life-expectancy-in-america-in-2018-a-new-year-for-opioids-social-determinants-c82c55d85283 (accessed February 16, 2022).
STRATEGIC PLANNING
In an effort to focus the insights and emerging scientific understandings from expert discussions toward potentially applicable and operational actions in the context of real-life scenarios, the workshop incorporated a hypothetical scenario to operationalize the topics discussed over the previous workshop sessions.7 The goal of the activity was to assemble a collection of actions organized by an approximate timeline that can be informative to decision makers in this scenario. The scenario and methods for the exercise are outlined below, followed by the findings and lessons as reported by the group leaders. Zahn led and moderated the first group. Stephen J. Thomas, State University of New York Upstate Medical University, moderated the second group.
Scenario and Methods
Workshop participants were provided a narrative of a potential scenario of a new variant of SARS-CoV-2 emerging in the summer of 2023. This variant was found to primarily affect children, and there were reports of moderate to severe symptoms in many children affected. The full narrative can be found in Box 5-1.
For this exercise, participants were split into two groups and given the charge to extract key pieces of information and identify critical uncertainties, including basic knowns and unknowns of the situation. Next, they were asked to build a consequence cascade that maps out possible sequences of events once cases arrive in the jurisdiction, based on the status quo and best-guess probabilities. This exercise was meant to draw a picture of what the future could look like in the absence of intervention. Once the problems have been clearly articulated, using the consequence cascade to pick out the most likely and undesirable future states, participants generated an intervention strategy made up of discrete actions. The suggested actions were meant to address the five following goals:
- Community: Mobilize existing infrastructure and community leadership to mitigate the cost and suffering associated with an impending outbreak of the new variant.
- Budget and capacity: Efficiently budget out the unrestricted $90 million that federal and state governments have allocated for your team to spend in the next 6 months. What resources do you need to gather? What capacities do you need to generate? How are
___________________
7 See Appendices D and E for scenario outputs.
- Data: Establish relevant and reliable data-collection efforts to inform equitable resource allocation. Who needs what, and how will you know?
- Communications: Articulate an effective communication strategy that extends beyond mere messaging. What will you communicate, and how you will communicate effectively with the following audience: up and down the chain of command for the response effort, to the general public and the news media, and to different communities in your jurisdiction? How will you listen to and incorporate what you hear and learn to inform tailored solutions for particular issues raised in different communities? How will you handle uncertainty surrounding risk as information availability continues to evolve—especially before the outbreak reaches the area?
- Resilience: Build an outbreak response system that can serve as a lasting foundation for improved overall public health and outbreak security for the jurisdiction. This must include the medium-term capacity to effectively and equitably distribute the new vaccine once it becomes available, but it should also apply to longer-term and broader considerations.
you going to justify your expenditures to an oversight committee? What happens when your funds are spent?
Scenario Debrief8
Group One
Following interactive discussion and real-time mapping of the assigned tasks, Zahn shared the immediate, short-, medium-, and longer-term responses discussed by the participants in group one.9 In terms of the immediate time frame, several actions were outlined from the group discussions. First, participants in the group suggested setting up aggressive surveillance efforts for children, especially in congregate settings. Many in the group voiced the importance of having active surveillance among all age groups, including elder care settings, because this is a new variant. Second, many in the group also suggested that local governments could be given the responsibility to engage community-based organizations as soon as possible to develop strategies and responses to issues that were likely to arise, such as care for children and families. A number of participants highlighted the
___________________
8 This section describes the discussions that occurred during the breakout sessions. Statements and opinions expressed are those of individual participants and should not be construed as reflecting any group consensus.
9 For full table of strategic actions by Group One, see Appendix D.
critical importance of communication from local government and public health settings and coordinating well with community-based organizations and community partners. Third, discussions in the group brought up that hospitals and health care systems needed to enact surge protocols and identify additional staff to be prepared for shortages. One concern for many in this group was the potential for fatigue of information, hypothesizing that by 2023 the public would not want to listen to any more information about COVID-19.
Moving to the medium-term actions, the group discussed the importance of outreach and education, noting that the family dynamic would significantly change if the variant did affect children. So, in this new scenario there is now an overwhelming need for leaders and responders to have housing accessible and available for those who fall ill, where they can safely quarantine as needed, separate from their families. Many in group one also raised the need to coordinate with school districts and education departments, because if schools are closed, many children will need food and nutritional assistance. In both clinical and nonclinical settings, we need community testing on a large scale to identify new cases, participants said. It is currently still a patchwork system, but this goal needs to be achieved more systematically. The group discussions also suggested an action for the federal government, saying it can identify regulatory flexibilities that could be brought to bear to adapt health system responses as needed. This could allow for more robust access to things like personal protective equipment, monoclonal antibody therapy, vaccine rollout, and diagnostic testing. Currently, the lack of flexibility of the system and the delays in adapting to what is happening on the ground has been a continual issue, a number of group members noted.
Finally, for long-term response actions, a number of group members recommended developing testing capacity on a national level and funding and coordinating the research community to respond to misinformation. This is such a critical responsibility on the local level, he noted, and we have been relying on academic partners to help dispel myths, but they have been doing this in a volunteer role, which is difficult to sustain long term. Also, many in the group raised the need for the research community to collect, analyze, and disseminate data, especially for a novel variant.
Group Two
Stephen J. Thomas, State University of New York Upstate Medical University, moderated the second group’s exercise experience and shared the key characteristics of the future that several participants found most likely and most undesirable (which can therefore inform what mitigation strategies can be deployed to avoid this hypothetical future) (see Figure 5-2).
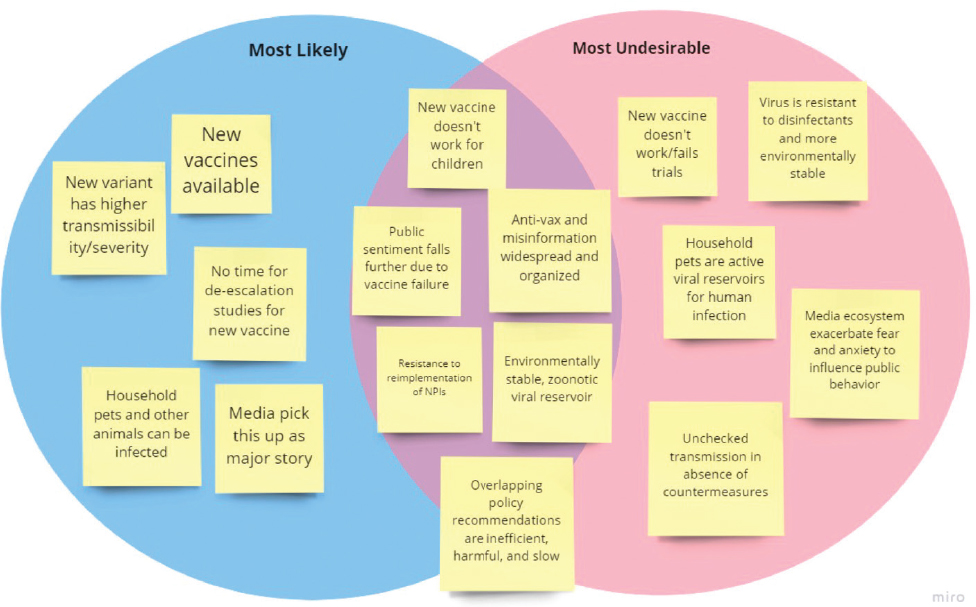
NOTE: NPI = Nonpharmaceutical intervention.
SOURCE: Stephen J. Thomas presentation, September 24, 2021.
Throughout the exercise, Thomas noted that discussion from many participants in group two focused on three main concepts:
- Disease in children: There are concerning aspects of severe outcomes in children, as well as questions about clinical attack rate, clinical severity, and epidemiology—not just in children but in all at-risk populations. They discussed whether new epidemiological trends had a basis in new pathogenesis or new mechanisms of infection or immune evasion, and how did this translate into transmission dynamics, meaning, what is the R0 of the new variant?10 Thomas also shared the group participants’ reflection on whether there is a new mechanism increasing transmission and whether it applies to increased severity and affects existing treatment strategies.
- Occurrence in a low-risk environment: The time of year indicated in the scenario, midsummer in the United States, is when most activities are primarily outdoors and not currently considered high risk. But since this genetically distinct variant seemed to have evolved in the absence of abundant transmission, there were many
___________________
10 The basic reproduction number, or R0, is a measure of the transmissibility of a pathogen. See https://wwwnc.cdc.gov/eid/article/25/1/17-1901_article (accessed January 24, 2022).
- All things communications: Several group members highlighted the importance of communication plans and advocates across many different areas. First, there is a need to effectively communicate information about an outbreak in near real time. Discussions of public health measures to disrupt the outbreak will also be a nuanced conversation because that implies that things have been stable and now people will have to return to previous measures and restart masks and distancing. How do we motivate good behavior within a community, the group discussions raised, and encourage concepts of self-advocacy? A number of participants also noted the diverse urban, semiurban, and rural environments that will all have different populations and needs.
questions on the source of the outbreak of this variant. Group two participants considered other environmental sources or zoonotic sources, and whether there were unknown viral reservoirs for persistent reintroduction back into human populations.
Next, Thomas shared some suggestions from group two for strategic actions across various time frames, similar to group one.11 He focused on two main actions that many participants deemed essential. The first, broadly, was communication. In the immediate time frame, a number of group members suggested establishing a local lead communicator. This can draw from a trusted group of local scientists, news media, religious leadership, health care professionals, or government officials. In the short term, some participants thought a two-way communication channel with the public was needed, which could use tailored messages on reimplementation of nonpharmaceutical interventions that people had maybe stopped using, as well as uncertainties around a new vaccine. In the medium and long-term time frame, many in the group suggested building and funding a communication council composed of diverse community members. This can be an enduring asset within the community to share accurate information, drawing on lots of unfortunate lessons learned throughout the pandemic—not something that is stood up and quickly dissolved when interest wanes. A second key concept was increasing real-time research and upstream surveillance, said Carolina Batista, Institute of Global Health in Barcelona. Many in the group noted an immediate need for real-time research to establish evidence and causality, identify potential animal reservoirs, and determine the stability and persistence of the viral variant.
The group discussions reiterated the need and opportunity to appropriate funds to One Health programs and biomedical preparedness in a meaningful and enduring way, so they have authority and resources to
___________________
11 For full table of proposed strategic actions for group two, see Appendix E.
execute responsibilities. One example of this broader surveillance approach is assessing wastewater, knowing that in certain areas the source of the wastewater can be tracked, and then this can be used as an early indicator to do more in-depth reflex testing. The group pointed out that there is demonstrated success with wastewater surveillance, and several participants agreed that it should be used more often as well as scaled.
Discussion
Zahn shared a question from the audience on whether there were indicators that define a successful response, and how someone can evaluate a response based on those indicators. As an initial reply, he said this is very difficult for several reasons. First, there is no easy and universal definition of success. We also fragmented our society in terms of response, he added. Local health departments are tasked with contact tracing and vaccine outreach, but there are so many social determinants of health that cannot be addressed in that way on a larger and more community-wide scale. He noted that there is not a coordinated response to this, as all the stakeholders involved have different responsibilities that are not tied together. Expanding on the community component, Batista added that successful responses are the ones that most address the needs of the community. Disparities played a key role in this pandemic, and a magnifying glass has been placed over the existing inequities in our society, she said. A successful response is the one that addresses the different needs of different communities—and not prioritizing one or the other. Essentially, being successful is agreement on the need for a coordinated response from different stakeholders.
For the next public health emergency, not necessarily pandemic, Zahn asked, what has COVID-19 taught us about the community structures, training, and engagement we need to have on an ongoing basis in order to be prepared? Lindsey Leininger, Tuck School of Business at Dartmouth felt strongly that there is a need for a much more robust digital response, including a social media ambassador and online efforts. One of our strategic failures was failing to map out the digital information environment, resource it, and attend to it, she added. In addition to keeping community relationships and empowering community health workers, this digital information mapping is necessary. Lastly, it has taught us that we need funding, Leininger said. People who have stepped up to be educators throughout the pandemic have done so for free, which is not suitable for scaling up the effort. Batista reiterated that it is important to transparently communicate the knowns and unknowns in a situation. If we are not sure what we are dealing with, then there is a need to share real-time information, and understand what is working within communities and what people’s hesitancies and concerns are.
Batista noted that people have a lot of questions and sometimes mistrust, so we need to better learn who the trusted people are in communities and empower them with training and tools to succeed. One of the problems with the reductions in local health department funding over the years, offered Zahn, is that we have outsourced much of the outreach and communication to communities to other organizations. But no matter how great the community-based organization is, they are being asked to do something beyond their role. Local health departments should be doing outreach and communications more sustainably, but the support needed has not been available.
As a final question from the audience, Zahn noted that the response plan as devised assumes no concurrent failure in the public health system, but what if the vaccine had a serious safety risk, or a therapeutic killed people because of adulteration? How would that alter the response? Thomas replied that this was a topic of discussion for group two as well, and said when it comes to preparedness, if nothing changes then nothing changes. We simply cannot put the national preparedness mission on the existing public health infrastructure, from the local level up to federal agencies, that has been defunded and hollowed out over the past decade, he stated. It already operates on a very thin margin, and continuing to take this approach will not achieve the outcome everyone desires. Instead, Thomas suggested that there should be a cross-agency federal entity that is devoted to the mission of biomedical preparedness, receives enduring appropriations to carry out this mission, and coordinates with other existing agencies. Specifically, he emphasized that layering this mission onto existing infrastructure or systems is unlikely to lead to the optimal outcome envisioned throughout this discussion.
CLOSING REMARKS
Elizabeth Hermsen, Merck & Co., commented on the far-reaching nature of the pandemic and its reverberations. It truly is a humanitarian crisis, she said, but we have the potential now to create a new future. This will require “new mechanisms, tools, and actors to take a whole-of-society approach to help address underlying issues that are necessary to support outbreak mitigation efforts.” She highlighted the increased recognition of the importance of community engagement and saw a need to redefine what is considered as expertise. Instead of coming in with determined answers, Hermsen said, health officials, researchers, and policy leaders need to colearn and cocreate solutions within communities, and put a stop to the panic-and-neglect cycle of preparedness. The lessons and progress that have been gleaned from this pandemic need to be systematized and institutionalized so they can be sustained beyond the current crisis.
Rafael Obregon, Country Representative for Paraguay at the United Nations Children’s Fund, said that one of the key objectives in planning this workshop was to elevate the dimension of equity. It has been a central theme throughout discussions, he noted, and we have heard numerous perspectives of how we can bring equity to the center of preparedness and how we can collectively address some of the underlying root causes. But this will require broadening our thinking, and he emphasized the need to move from a reactive to a proactive approach. Speakers shared exciting developments of plans to invest in these more proactive areas, such as strengthening capacities of local governments and creating public policies for communication, all in the context of equity and addressing issues holistically. It is hoped that these can come to fruition in the near future. Finally, Obregon highlighted the global nature of these events, but what has been lacking is the creation of spaces for cross-learning and sharing lessons and actions that took place in different contexts to see how they can serve the thinking and innovation needed to address these persistent challenges. He also agreed with the importance of maintaining these lessons and not losing all of the knowledge that has been gained from this current pandemic. The ongoing nature of the pandemic helps to ensure it is not lost, and it is hoped these efforts can be built on and sustained for the future. It is imperative that new efforts and investments do not fade away, he insisted.
Finally, Peter Daszak, EcoHealth Alliance, noted that COVID-19 has brought home the reason why the National Academies were asked by NIH and CDC to set up the Forum on Microbial Threats in 1996: the increasing threat of infectious diseases in a globalized world. “What’s happened with COVID-19 is that we’ve seen how connected we are” in many ways, he said. Daszak elaborated that in addition to the global interconnectedness of our modern society, we are also connected locally, between communities within cities and states, and also different social groups within these communities. People with different behaviors and risk factors within families, friends, and neighborhoods are realizing how intertwined their lives can be through the collective risk of COVID-19, and that was a really big lesson for many people. He supported the idea of bringing in additional expertise and focusing on a One Health dimension, concluding, we are not through this yet, but once we are, we need to commit to not letting this type of global emergency happen again.
This page intentionally left blank.
















