Cardiovascular Disease:
Confronting the Leading Cause of Death Worldwide
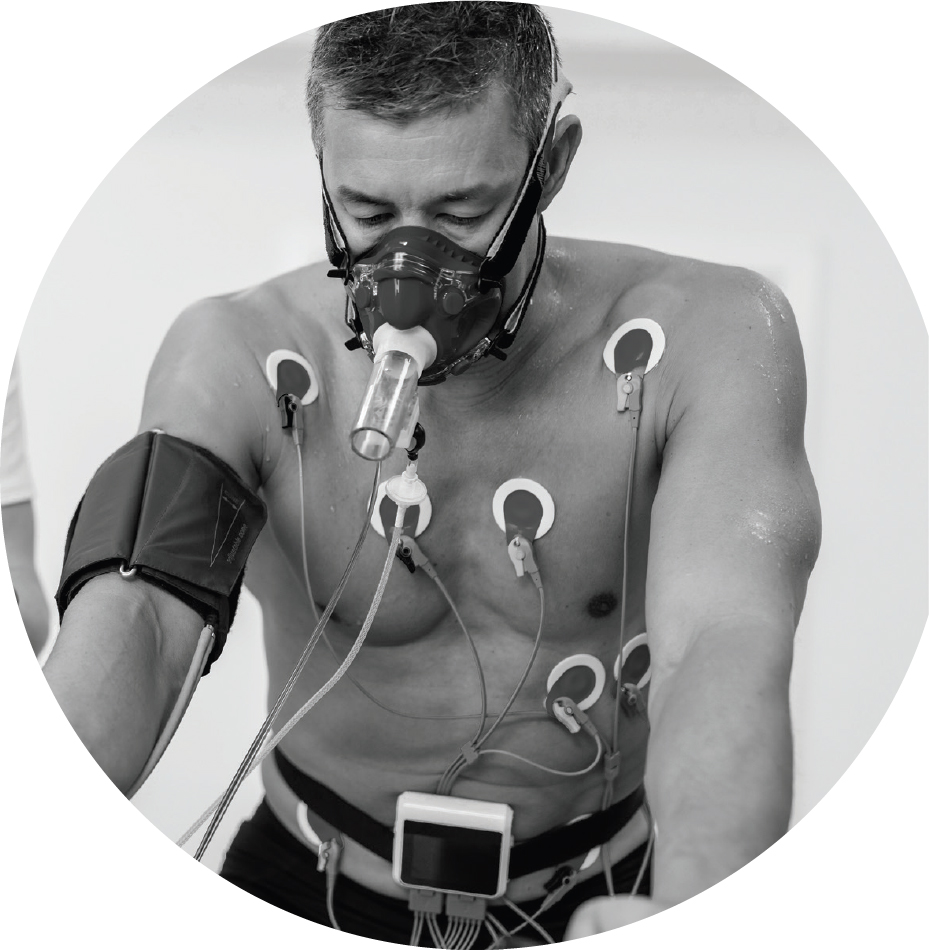
Since the 1970s, age-adjusted death rates from cardiovascular disease have plummeted by as much as 70 percent in some Western countries, largely as a result of new medicines, innovative surgical techniques and devices, and sweeping public health campaigns designed to reduce smoking and cholesterol levels. Unfortunately, the tide has turned in recent years as increasing rates of obesity and diabetes have driven cardiovascular deaths upward. Today, cardiovascular disease remains the number one killer worldwide.
1970s
Defining Cardiovascular Risk Factors
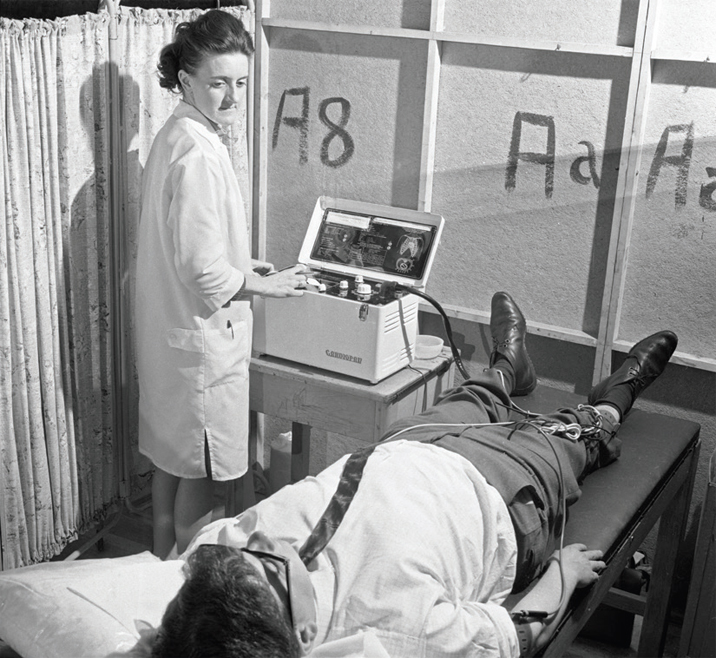
For more than half a century, the Framingham Heart Study, initiated in 1948, has provided fundamental insights into cardiovascular risk factors. By studying the lives of the residents of Framingham, Massachusetts, the study clearly showed that elevated blood pressure and cholesterol levels were associated with higher rates of heart disease, stroke, and acute myocardial infarctions or heart attacks. Identification of these risk factors has shaped public health guidelines and has led to national programs to reduce the risk of cardiovascular disease. As it has evolved into a multigenerational study of a more diverse community, the study has continued to make major contributions to understanding the leading cause of death worldwide and has spawned analogous population studies to identify the risk factors for other diseases.
1970s
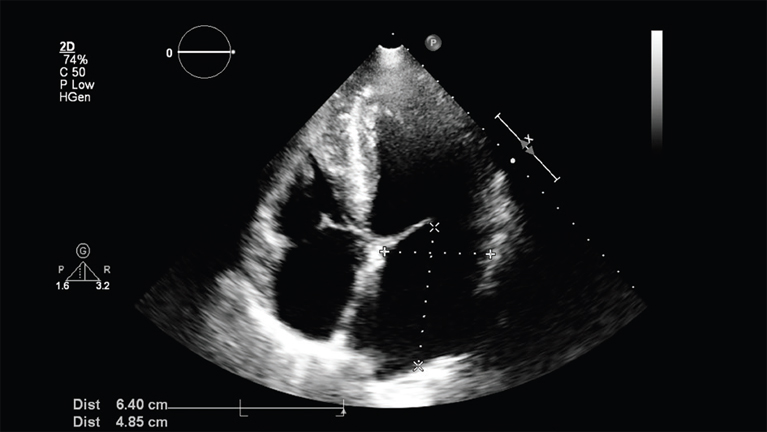
Cardiac Imaging
Four main imaging tools are used to visualize the heart and its vasculature: radiology, magnetic resonance imaging, echocardiography, and nuclear cardiology. Introduced into clinical practice in 1953, echocardiography, also known as the “virtual stethoscope,” remains the mainstream first-line modality of cardiac imaging. Readily available, portable, and specific, echocardiography allows doctors to examine cardiac anatomy and function in real time by taking an ultrasound of the heart. More than 25 million echocardiograms are performed each year throughout the world, and the procedure has prolonged and improved the lives of millions of patients.
1973
Cholesterol and Heart Disease
Though cholesterol is essential for the functioning of all organs, genetic and epidemiological studies have shown that elevated cholesterol levels can cause coronary heart disease. Scientists and the pharmaceutical industry developed a class of drugs called statins that lower cholesterol levels and reduce the frequency of heart attacks. Although the first statin was isolated in 1973, the first commercial statin, lovastatin, was not available until 1987. Since then, more statins have been approved, and studies have consistently demonstrated that their use reduces the frequency of heart attacks by 25–30 percent.
1981
The Discovery of Lifesaving Drugs
The first clinically available angiotensin-converting enzyme (ACE) inhibitor, captopril, became available in 1981 for the treatment of hypertension. By relaxing the veins and arteries, ACE inhibitors lower blood pressure and substantially reduce the risk of cardiovascular disease. As more ACE inhibitors were developed, studies showed that their use has positive effects on a wide range of diseases, including heart failure, diabetes, and kidney dysfunction.

1977
Balloons to Expand Arteries
Since 1977, when the first balloon angioplasty procedure on a coronary artery was performed, the technique has become the method of choice to treat patients with acute myocardial infarction or occluded leg arteries. During the procedure, an expandable balloon catheter is used to enlarge a collapsed artery, restoring blood flow. Advances such as drug-coated balloons offer hope for even more effective clinical applications.

1986
Scaffolding for Cardiac Vessels
In 1986, doctors implanted the first self-expanding coronary stent into a patient in Toulouse, France. Stents are used as scaffolds to prevent blood vessels from closing and to avoid restenosis in coronary surgery—a condition where scar tissue interferes with vascular flow. Developed to combat some of the problems with balloon angioplasty, stents were at first bulky and technically challenging to use, but refinements in materials and design have improved their safety and effectiveness and have led to their widespread use.
2001
Blood Pressure and Cardiovascular Disease
Many adults have a blood pressure that is somewhat elevated but not classified as high—a condition known as high-normal blood pressure. A 2001 study found that high-normal blood pressure is associated with an increased risk of cardiovascular disease, especially among people 65 and older. The study also found that people with high-normal blood pressure were more likely to suffer from a heart attack, stroke, or heart failure in 10 years than those with optimal blood pressure, emphasizing the need for people to determine early whether their risk can be reduced by lowering their blood pressure.

2010
The Hereditary Risk of Stroke
In 2010, a study determined that having a parent who suffered a stroke tripled a person’s risk of stroke, with a slightly greater risk if that parent was a father rather than a mother. This association between strokes in parents and their offspring suggests a substantial genetic contribution to the risk of stroke, though other risk factors, such as high blood pressure, obesity, and smoking, can be changed.

2010s
Precision Medicine for Cardiovascular Disease
Precision medicine could transform cardiovascular medicine by providing tailored treatments that reflect a person’s genetic background, environment, and experiences. Rather than presuming that all patients with similar symptoms share the same way of developing a disease, precision medicine bases treatments on a detailed understanding of how people’s genes interact with their environments to produce particular outcomes. Though incorporating precision medicine into clinical practice has its challenges, such as dealing with the vast amounts of data generated, it promises more individualized treatments and better outcomes.
2015
The Discovery of PCSK9 Inhibitors
The emergence of proprotein convertase subtilisin/kexin type 9 (PSCK9) inhibitors, a new class of drugs first approved in 2015, offered both an alternative and a complement to statins for treating high cholesterol. Though statins have been the cornerstone of treatment since the 1980s, many patients experience side effects or don’t fully respond. Unlike statins, PSCK9 inhibitors, which were developed following genetic studies of people with low cholesterol levels, reduce harmful cholesterol particles by binding to their receptors and destroying both the receptor and the particle. Since their introduction, PSCK9 inhibitors have consistently demonstrated remarkable efficacy in reducing the risk of cardiovascular disease.
2020s
Cardiovascular Regeneration
During a heart attack an estimated 1 billion cardiac cells can be lost, greatly increasing the risk of abnormal and life-threatening heart rhythms. Though today there is no way to replace muscle that has died after a heart attack, scientists have been using techniques at the forefront of research to explore the possibility of regenerating heart tissue. Recently, researchers have begun clinical trials that incorporate advances in stem cells, developmental biology, and biomaterials to create cells that can integrate into the living heart, creating the possibility that hearts will someday be repaired at the cellular level.

Unless current trends are reversed, more than 1 billion people will die from cardiovascular disease in the first half of the 21st century. A reduction in tobacco use, universal access to cardiovascular medications, and new tools like personalized treatments and tissue engineering could once again yield major progress against cardiovascular disease.




